Management of Acute Cholecystitis and Acute Cholangitis in Emergency Setting
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Print This Article
International Surgery Journal Lew D et al. Int Surg J. 2021 May;8(5):1575-1578 http://www.ijsurgery.com pISSN 2349-3305 | eISSN 2349-2902 DOI: https://dx.doi.org/10.18203/2349-2902.isj20211831 Case Report Acute gangrenous appendicitis and acute gangrenous cholecystitis in a pregnant patient, a difficult diagnosis: a case report David Lew, Jane Tian*, Martine A. Louis, Darshak Shah Department of Surgery, Flushing Hospital Medical Center, Flushing, New York, USA Received: 26 February 2021 Accepted: 02 April 2021 *Correspondence: Dr. Jane Tian, E-mail: [email protected] Copyright: © the author(s), publisher and licensee Medip Academy. This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. ABSTRACT Abdominal pain is a common complaint in pregnancy, especially given the physiological and anatomical changes that occur as the pregnancy progresses. The diagnosis and treatment of common surgical pathologies can therefore be difficult and limited by the special considerations for the fetus. While uncommon in the general population, concurrent or subsequent disease processes should be considered in the pregnant patient. We present the case of a 36 year old, 13 weeks pregnant female who presented with both acute appendicitis and acute cholecystitis. Keywords: Appendicitis, Cholecystitis, Pregnancy, Pregnant INTRODUCTION population is rare.5 Here we report a case of concurrent appendicitis and cholecystitis in a pregnant woman. General surgeons are often called to evaluate patients with abdominal pain. The differential diagnosis list must CASE REPORT be expanded in pregnant woman and the approach to diagnosing and treating certain diseases must also be A 36 year old, 13 weeks pregnant female (G2P1001) adjusted to prevent harm to the fetus. -

Increased Risk and Case Fatality Rate of Pyogenic Liver Abscess in Patients with Liver Cirrhosis: a Gut: First Published As 10.1136/Gut.48.2.260 on 1 February 2001
260 Gut 2001;48:260–263 Increased risk and case fatality rate of pyogenic liver abscess in patients with liver cirrhosis: a Gut: first published as 10.1136/gut.48.2.260 on 1 February 2001. Downloaded from nationwide study in Denmark I Mølle, A M Thulstrup, H Vilstrup, H T Sørensen Abstract in case reports, and most often in patients with Background—Patients with liver cirrhosis iron overload.9–12 In a few case series of patients are at increased risk of serious bacterial with pyogenic liver abscesses, the prevalence of infections carrying a high case fatality liver cirrhosis was 0.9–13%,257and the preva- rate. Case reports have suggested an lence of chronic alcoholism was more than association between liver cirrhosis and 10% in other studies.413 pyogenic liver abscess. To determine if liver cirrhosis is a risk factor Aims—To estimate the risk and case fatal- for liver abscess, we estimated the incidence ity rate of pyogenic liver abscess in Danish rate and 30 day case fatality rate of pyogenic patients with liver cirrhosis compared liver abscess in a nationwide cohort of patients with the background population. with liver cirrhosis referring to the entire Methods—Identification of all patients Danish population. with liver cirrhosis and pyogenic liver abscess over a 17 year period in the Methods National Registry of Patients. Information STUDY POPULATION AND DATA SOURCES on death was obtained from the Danish Denmark has approximately 5.2 million inhab- Central Person Registry. itants. Admission, stay, and treatment in Dan- Results—We identified 22 764 patients ish public hospitals are free. -

Diagnosis and Treatment of Perianal Crohn Disease: NASPGHAN Clinical Report and Consensus Statement
CLINICAL REPORT Diagnosis and Treatment of Perianal Crohn Disease: NASPGHAN Clinical Report and Consensus Statement ÃEdwin F. de Zoeten, zBrad A. Pasternak, §Peter Mattei, ÃRobert E. Kramer, and yHoward A. Kader ABSTRACT disease. The first description connecting regional enteritis with Inflammatory bowel disease is a chronic inflammatory disorder of the perianal disease was by Bissell et al in 1934 (2), and since that time gastrointestinal tract that includes both Crohn disease (CD) and ulcerative perianal disease has become a recognized entity and an important colitis. Abdominal pain, rectal bleeding, diarrhea, and weight loss consideration in the diagnosis and treatment of CD. Perianal characterize both CD and ulcerative colitis. The incidence of IBD in the Crohn disease (PCD) is defined as inflammation at or near the United States is 70 to 150 cases per 100,000 individuals and, as with other anus, including tags, fissures, fistulae, abscesses, or stenosis. autoimmune diseases, is on the rise. CD can affect any part of the The symptoms of PCD include pain, itching, bleeding, purulent gastrointestinal tract from the mouth to the anus and frequently will include discharge, and incontinence of stool. perianal disease. The first description connecting regional enteritis with perianal disease was by Bissell et al in 1934, and since that time perianal INCIDENCE AND NATURAL HISTORY disease has become a recognized entity and an important consideration in the Limited pediatric data describe the incidence and prevalence diagnosis and treatment of CD. Perianal Crohn disease (PCD) is defined as of PCD. The incidence of PCD in the pediatric age group has been inflammation at or near the anus, including tags, fissures, fistulae, abscesses, estimated to be between 13.6% and 62% (3). -

Descriptive Study Regarding the Etiological Factors Responsible for Secondary Bacterial Peritonitis in Patients Admitted in a Te
International Journal of Health Sciences and Research Vol.10; Issue: 7; July 2020 Website: www.ijhsr.org Original Research Article ISSN: 2249-9571 Descriptive Study Regarding the Etiological Factors Responsible for Secondary Bacterial Peritonitis in Patients Admitted in a Tertiary Care Hospital in Trans Himalayan Region Raj Kumar1, Rahul Gupta2, Anjali Sharma3, Rajesh Chaudhary4 1MS General Surgery, Civil Hospital Baijnath, Himachal Pradesh 2MD Community Medicine, District Programme Officer, Health and Family Welfare, Himachal Pradesh 3Resident Doctor, Department of Microbiology, DRPGMC Kangra at Tanda, Himachal Pradesh 4MS General Surgery, Civil Hospital Nagrota Bagwan, Himachal Pradesh Corresponding Author: Rahul Gupta ABSTRACT Peritonitis is an inflammation of the peritoneum. Primary peritonitis which is spontaneous bacterial peritonitis, Secondary peritonitis due to infection from intraabdominal source or spillage of its contents and Tertiary peritonitis which is recurrent or reactivation of secondary peritonitis. The present study was aimed to determine the etiology of generalized secondary peritonitis among the patients admitted in Department of General Surgery, Dr RPGMC Kangra at Tanda. This descriptive observational study was conducted in the department of surgery Dr. Rajendra Prasad Government Medical College Kangra at Tanda consisting of patients having acute generalised secondary peritonitis presented in emergency department or Surgery outdoor patient department over a period of one year from December 2016 through November 2017. The most common etiology of generalized secondary peritonitis in our patients was peptic ulcer disease (77.13%) followed by perforated appendicitis (9.8%). Etiological factors of secondary generalised peritonitis have a different pattern in different geographical regions. Peptic ulcer disease remains the commonest etiology of secondary peritonitis in India followed by enteric perforation which is in contrast to the western studies where appendicular and colon perforations are more common. -

Acute Onset Flank Pain-Suspicion of Stone Disease (Urolithiasis)
Date of origin: 1995 Last review date: 2015 American College of Radiology ® ACR Appropriateness Criteria Clinical Condition: Acute Onset Flank Pain—Suspicion of Stone Disease (Urolithiasis) Variant 1: Suspicion of stone disease. Radiologic Procedure Rating Comments RRL* CT abdomen and pelvis without IV 8 Reduced-dose techniques are preferred. contrast ☢☢☢ This procedure is indicated if CT without contrast does not explain pain or reveals CT abdomen and pelvis without and with 6 an abnormality that should be further IV contrast ☢☢☢☢ assessed with contrast (eg, stone versus phleboliths). US color Doppler kidneys and bladder 6 O retroperitoneal Radiography intravenous urography 4 ☢☢☢ MRI abdomen and pelvis without IV 4 MR urography. O contrast MRI abdomen and pelvis without and with 4 MR urography. O IV contrast This procedure can be performed with US X-ray abdomen and pelvis (KUB) 3 as an alternative to NCCT. ☢☢ CT abdomen and pelvis with IV contrast 2 ☢☢☢ *Relative Rating Scale: 1,2,3 Usually not appropriate; 4,5,6 May be appropriate; 7,8,9 Usually appropriate Radiation Level Variant 2: Recurrent symptoms of stone disease. Radiologic Procedure Rating Comments RRL* CT abdomen and pelvis without IV 7 Reduced-dose techniques are preferred. contrast ☢☢☢ This procedure is indicated in an emergent setting for acute management to evaluate for hydronephrosis. For planning and US color Doppler kidneys and bladder 7 intervention, US is generally not adequate O retroperitoneal and CT is complementary as CT more accurately characterizes stone size and location. This procedure is indicated if CT without contrast does not explain pain or reveals CT abdomen and pelvis without and with 6 an abnormality that should be further IV contrast ☢☢☢☢ assessed with contrast (eg, stone versus phleboliths). -

PERFORATED PEPTIC ULCER. Patient Usually Experiences
Postgrad Med J: first published as 10.1136/pgmj.12.134.470 on 1 December 1936. Downloaded from 470 POST-GRADUATE MEDICAL JOURNAL December, 1936 PERFORATED PEPTIC ULCER. By RONALD W. RAVEN, F.R.C.S. (Assistant Surgeon to T'he French Hospital, Assistant Surgeon to The Gordon Hospital for Rectal Diseases and Swrgical Registrar to The Royal Cancer Hospital.) INTRODUCTION. Peptic ulceration is a crippling disease judged from the stand-point of morbidity, and is also dangerous to life on account of serious complications, such as haemorrhage or perforation which may supervene during the course of the disease. These complications may occur in any patient and there are no criteria which will indicate whether or not an ulcer will bleed or perforate. When the treatment of peptic ulceration is under review it must be remembered that from 20 to 30 per cent. of these ulcers perforate. In a large series of cases I found that the incidence of perforation was 27 per cent. It is thus essential that patients suffering with peptic ulcer should be kept under continuous careful observation. Unfortunately, however, a small percentage of patients give no previous history of the peptic ulcer syndrome and perforation of the ulcer is the first indication of its presence. Recently, when considering the role of surgery in the treatment of chronic peptic ulcer, Joll stated that there has been a rise in the incidence of perforation as a complication of peptic ulcer since medical treatment has become systematized in the treatment of this disease. It must also be remembered that medical treat- Protected by copyright. -

Pregnancy and the Biliary Tract
MINI-REVIEW Pregnancy and the biliary tract Tuvia Gilat MD, Fred Konikoff MD T Gilat, F Konikoff. Pregnancy and the biliary tract. Can J Gas- Grossesse et voies biliaires troenterol 2000;14(Suppl D):55D-59D. Pregnancy induces many physiological changes, some of which may have patho- RÉSUMÉ : La grossesse donne lieu à de nombreux changements physiolo- logical results. In population studies, gallstones were found in giques, dont certains peuvent avoir des conséquences pathologiques. Des 6.5% to 8.4% of nulliparous women, and in 18.4% to 19.3% of études démographiques ont révélé la présence de calculs biliaires chez 6,5 à women with two to three or more pregnancies. In women followed 8,4 % des femmes nullipares et chez 18,4 à 19,3 % des femmes ayant eu au throughout pregnancy, neoformation of gallstones was documented moins deux grossesses. Chez des femmes qui ont été suivies pendant toute in 3% to 8.1% depending on the population. Some 20% to 30% of la grossesse, la néoformation de calculs biliaires a été objectivée chez 3 à these gallstones redissolve postpartum. The frequency of biliary col- 8,1 % des patientes selon la population étudiée. Quelque 20 à 30 % de ces ic during pregnancy is controversial, and the recommended thera- calculs biliaires se dissolvent après l’accouchement. La fréquence de la co- lique hépatique pendant la grossesse est controversée, et on recommande peutic approach during pregnancy is conservative. When essential, une démarche thérapeutique traditionnelle pendant la grossesse. Lors- invasive procedures are relatively well tolerated, preferably during qu’elles sont essentielles, les interventions effractives sont bien tolérées, de the second trimester. -
Pancreatic Disorders in Inflammatory Bowel Disease
Submit a Manuscript: http://www.wjgnet.com/esps/ World J Gastrointest Pathophysiol 2016 August 15; 7(3): 276-282 Help Desk: http://www.wjgnet.com/esps/helpdesk.aspx ISSN 2150-5330 (online) DOI: 10.4291/wjgp.v7.i3.276 © 2016 Baishideng Publishing Group Inc. All rights reserved. MINIREVIEWS Pancreatic disorders in inflammatory bowel disease Filippo Antonini, Raffaele Pezzilli, Lucia Angelelli, Giampiero Macarri Filippo Antonini, Giampiero Macarri, Department of Gastro- acute pancreatitis or chronic pancreatitis has been rec enterology, A.Murri Hospital, Polytechnic University of Marche, orded in patients with inflammatory bowel disease (IBD) 63900 Fermo, Italy compared to the general population. Although most of the pancreatitis in patients with IBD seem to be related to Raffaele Pezzilli, Department of Digestive Diseases and Internal biliary lithiasis or drug induced, in some cases pancreatitis Medicine, Sant’Orsola-Malpighi Hospital, 40138 Bologna, Italy were defined as idiopathic, suggesting a direct pancreatic Lucia Angelelli, Medical Oncology, Mazzoni Hospital, 63100 damage in IBD. Pancreatitis and IBD may have similar Ascoli Piceno, Italy presentation therefore a pancreatic disease could not be recognized in patients with Crohn’s disease and ulcerative Author contributions: Antonini F designed the research; Antonini colitis. This review will discuss the most common F and Pezzilli R did the data collection and analyzed the data; pancreatic diseases seen in patients with IBD. Antonini F, Pezzilli R and Angelelli L wrote the paper; Macarri G revised the paper and granted the final approval. Key words: Pancreas; Pancreatitis; Extraintestinal mani festations; Exocrine pancreatic insufficiency; Ulcerative Conflictofinterest statement: The authors declare no conflict colitis; Crohn’s disease; Inflammatory bowel disease of interest. -

Necrotizing Pancreatitis and Gas Forming Organisms
JOP. J Pancreas (Online) 2016 Nov 08; 17(6):649-652. CASE REPORT Necrotizing Pancreatitis and Gas Forming Organisms Theadore Hufford, Terrence Lerner Metropolitan Group Hospitals Residency in General Surgery, University of Illinois, United States ABSTRACT Context Acute Pancreatitis is a common disease of the gastrointestinal tract that accounts for thousands of hospital admissions in the United States every year. Severe acute necrotic pancreatitis has a high mortality rate if left untreated, and always requires surgical intervention. The timing of surgical intervention is of importance. Here we present a case of a patient with severe necrotizing pancreatitis with possible gas producing bacteria in the retroperitoneum shown on imaging and cultures. Case Report The patient is a Seventy- two-year old male presenting to the emergency department with complaining of severe epigastric pain for the past 48 hours. The labs and clinical symptoms were consistent with pancreatitis. However, the imaging showed necrotic pancreatitis that required immediate intervention. During the course of six weeks, the patient underwent numerous surgical procedures to debride the necrotic pancreas. The patient was ultimately clinically stable to be discharged and transferred to a skilled-nursing facility, but returned 3 days later with a post- surgical wound infection vs. Conclusion The patient ultimately expired 7 days after his second admission to the hospital due to multi-organ failure secondary to sepsis. anastomotic leak with enterocutaneous fistula. INTRODUCTION has proven to decrease mortality by about 40% in most cases [6]. Finding the cause of the infection is of the Acute Pancreatitis (AP) is a common disease of the utmost importance in necrotizing pancreatitis cases. -

The Clinical Analysis of Acute Pancreatitis in Colorectal Cancer Patients Undergoing Chemotherapy After Operation
Journal name: OncoTargets and Therapy Article Designation: Original Research Year: 2015 Volume: 8 OncoTargets and Therapy Dovepress Running head verso: Ji et al Running head recto: Analysis of acute pancreatitis in colorectal cancer patients open access to scientific and medical research DOI: http://dx.doi.org/10.2147/OTT.S88857 Open Access Full Text Article ORIGINAL RESEARCH The clinical analysis of acute pancreatitis in colorectal cancer patients undergoing chemotherapy after operation Yanlei Ji1 Abstract: Acute pancreatitis is a rare complication in postoperative colorectal cancer patients Zhen Han2 after FOLFOX6 (oxaliplatin + calcium folinate +5-FU [5-fluorouracil]) chemotherapy. In this Limei Shao1 paper, a total of 62 patients with gastrointestinal cancer were observed after the burst of acute Yunling Li1 pancreatitis. Surgery of the 62 cases of colorectal cancer patients was completed successfully. Long Zhao1 But when they underwent FOLFOX6 chemotherapy, five patients got acute pancreatitis (8.06%), Yuehuan Zhao1 four (6.45%) had mild acute pancreatitis, and one (1.61%) had severe acute pancreatitis, of which two were males (3.23%) and three females (4.84%). No patients (0.00%) had acute pancreatitis 1 Department of Special Diagnosis, on the 1st day after chemotherapy; one patient (1.61%) got it in the first 2 and 3 days after Shandong Cancer Hospital and Institute, Jinan, People’s Republic chemotherapy; and three others (4.83%) got it in the first 4 days after chemotherapy. In the 2 For personal use only. of China; Department of Internal 62 patients with malignant tumors, the body mass index (BMI) was less than 18 (underweight) in Medicine, Jinan Second People’s six of them, with two cases of acute pancreatitis (33.33%); the BMI was 18–25 (normal weight) Hospital, Jinan, People’s Republic of China in 34 cases, with one case (2.94%) of acute pancreatitis; the BMI was 25–30 (overweight) in 13 cases, with 0 cases (0.00%) of acute pancreatitis; and the BMI was $30 (obese) in nine patients, with two cases of acute pancreatitis (22.22%). -

Study of Calculus Pancreatitis
STUDY OF CALCULUS PANCREATITIS Dissertation Submitted for MS Degree (Branch I) General Surgery April 2011 The Tamilnadu Dr.M.G.R.Medical University Chennai – 600 032. MADURAI MEDICAL COLLEGE, MADURAI. CERTIFICATE This is to certify that this dissertation titled “STUDY OF CALCULUS PANCREATITIS” submitted by DR.P.K.PRABU to the faculty of General Surgery, The Tamilnadu Dr. M.G.R. Medical University, Chennai in partial fulfillment of the requirement for the award of MS degree Branch I General Surgery, is a bonafide research work carried out by him under our direct supervision and guidance from October 2008 to October 2010. DR. M.GOPINATH, M.S., Pro. A.SANKARAMAHALINGAM M.S, PROFESSOR AND HEAD, PROFESSOR, DEPARTMENT OF GENERAL SURGERY, DEPARTMENT OF GENERAL SURGERY, MADURAI MEDICAL COLLEGE, MADURAI MEDICAL COLLEGE, MADURAI. MADURAI. DECLARATION I, DR.P.K.PRABU solemnly declare that the dissertation titled “STUDY OF CALCULUS PANCREATITIS” has been prepared by me. This is submitted to The Tamilnadu Dr. M.G.R. Medical University, Chennai, in partial fulfillment of the regulations for the award of MS degree (Branch I) General Surgery. Place: Madurai DR. P.K.PRABU Date: ACKNOWLEDGEMENT At the very outset I would like to thank Dr.A.EDWIN JOE M.D.,(FM) the Dean Madurai Medical College and Dr.S.M.SIVAKUMAR M.S., (General Surgery) Medical Superintendent, Government Rajaji Hospital, Madurai for permitting me to carryout this study in this Hospital. I wish to express my sincere thanks to my Head of the Department of Surgery Prof.Dr.M.GOPINATH M.S., and Prof.Dr.MUTHUKRISHNAN M.Ch., Head of the Department of Surgical Gastroenterology for his unstinted encouragement and valuable guidance during this study. -
Cholecystitis
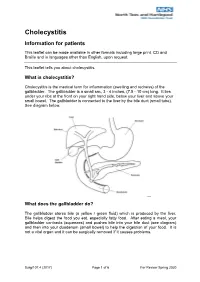
Cholecystitis Information for patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. This leaflet tells you about cholecystitis. What is cholecystitis? Cholecystitis is the medical term for inflammation (swelling and redness) of the gallbladder. The gallbladder is a small sac, 3 - 4 inches, (7.5 - 10 cm) long. It lies under your ribs at the front on your right hand side, below your liver and above your small bowel. The gallbladder is connected to the liver by the bile duct (small tube). See diagram below. What does the gallbladder do? The gallbladder stores bile (a yellow / green fluid) which is produced by the liver. Bile helps digest the food you eat, especially fatty food. After eating a meal, your gallbladder contracts (squeezes) and pushes bile into your bile duct (see diagram) and then into your duodenum (small bowel) to help the digestion of your food. It is not a vital organ and it can be surgically removed if it causes problems. Surg/107.4 (2017) Page 1 of 6 For Review Spring 2020 Cholecystitis What causes cholecystitis? Inflammation of the gallbladder is often caused when gallstones irritate the gallbladder and sometimes cause an infection. Gallstones are formed in the gallbladder or bile duct and develop when bile forms crystals. Over time these crystals become hardened and eventually grow into stones but they do not always cause problems. However, gallstones can cause: jaundice. If the stones move from your gallbladder and block your bile duct jaundice can occur.