Philip Shihua Li
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Wrvus: Do They Really Measure the Workload and Complexity of What We Do?
wRVUs: Do They Really Measure the Workload and Complexity Of What We Do? Raj S. Pruthi MD MHA FACS Rhodes Distinguished Professor and Chair Department of Urology The University of North Carolina at Chapel Hill INTRODUCTION Productivity-based Compensation • InCreasing use of wRVU in employed Compensation models • 2007 (16%) à 2016 (> 60%) • Use of benChmarked data (MGMA, AMGA, SC) to determine compensation/produCtivity ($/wRVU) • e.g. AMGA $441,836 / 7649 = $57.76/wRVU 2 INTRODUCTION wRVU • RBRVS - Developed for HCFA by Hsaio et al (1986-92) • Passed in 1989 -- implemented in 1992 INTRODUCTION Work RVU x Work GPCI + Practice Expense RVU x PE GPCI Conversion Payment = x FaCtor Rate + Malpractice RVU x MP GPCI GPCI = geographiC praCtiCe Cost index INTRODUCTION • RVUs à metric of physician productivity • RVUs : CPT code 405 urologiCal serviCes 22 383 Work = Time x Intensity INTRODUCTION Work 100 units INTRODUCTION • RVU assignments initially made in consultation with nominees from various medical specialties • Quarterly adjustments based on survey data • Zero sum game INTRODUCTION Changes to Work RVUs RUC Summary of Recommendation INTRODUCTION Who Gets Surveys? • Respondents seleCted by AUA by random sampling • May be sub-speCialty, e.g. prosthetiCs • May be general, e.g. cysto with dilation • Private praCtiCe (small & large), hospital-based, and aCademiC • Need at least 30-50 responses -- ideally >100 responses INTRODUCTION • Subjective methodology linked with compensation • Accurate measure of surgical complexity? workload? effort? time? -

Urology Scientific Session Monday, September 28, 2020
Urology Scientific Session Monday, September 28, 2020 Moderators/Panelists: Drs. Sabine Zundel, Sameh Shehata, Holger Till, Yuri Kozlov, Philipp Szavay, Eduardo Perez (S26) PNEUMOVESICOSCOPIC CORRECTION OF PRIMARY VESICOURETERAL REFLUX (VUR) IN CHILDREN. - OUR INITIAL EXPERIENCE- A. M. Benaired, Pediatric, Surgeon; H Zahaf, Pediatric, Surgeon; Military Central Hospital Purpose: Vesicoureteral reflux is a common urological abnormality predisposing risk of childhood hypertension and chronic renal failure. It is called primitive when it is due to an abnormality of the vesicoureteral junction. Different treatment approaches have been proposed a long time. Two main trends can be identified, conservative and operative approach. The main objective of our prospective study is to demonstrate the feasibility of vesicoscopic crosstrigonal ureteral reimplantation under CO2 pneumovesicum in treatment on primary vesicoureteral reflux and analyze results of this approach. Methods: A total of 60 patients underwent transvesicoscopic ureteral reimplantation (33 boys, 27 girls) by the same surgeon from Mai 2011 to Mai 2015. All patients had primary vesicoureteral reflux, and surgery was performed because of breakthrough urinary tract infection despite antibiotic prophylaxis, persistent high grade of vesicoureteral reflux especially in association with significant renal scarring, mean age at operation was 47.47 month (5 month - 12 years). Of the 60 patients, 34 had bilateral reflux and 26 had unilateral reflux. The reflux grade in the total of 94 ureters was grade IV, V in 59.57%, grade III in 35.11% and grade II in 5.32% in association with contralateral high grade vesicoureteral reflux. Our surgical methods followed those reported by Valla et al. Results: The transvesicoscopic procedure was successfully completed in all patients without perioperative complication except one case of pneumoperitoneum that required exsufflation by open laparoscopy. -

Laparoscopic Ureteral Repair in Gynaecological Surgery Carlo De Ciccoa, Anastasia Ussiab and Philippe Robert Koninckxb,C
Laparoscopic ureteral repair in gynaecological surgery Carlo De Ciccoa, Anastasia Ussiab and Philippe Robert Koninckxb,c aDepartment of Obstetrics and Gynaecology, Purpose of review University Hospital A. Gemelli, Universita` Cattolica del Sacro Cuore, bGruppo Italo-Belga, Rome, Italy and To review laparoscopic surgery in the treatment options for ureteral lesions in cDepartment of Obstetrics and Gynaecology, gynaecological surgery. University Hospital Gasthuisberg, Katholieke Recent findings Universiteit Leuven, Leuven, Belgium Laparoscopic treatment of ureteral injuries has been increasingly reported over the past Correspondence to Dr Carlo De Cicco, Department of Obstetrics and Gynaecology, University Hospital A. years. Treatment has progressively shifted from ureteroneocystostomy performed by Gemelli, Universita` Cattolica del Sacro Cuore, Largo F. laparotomy to less invasive treatment options such as ureteral stenting or dilatation in Vito 1, 00168 Rome, Italy Tel: +39 06 30155131; case of stricture, stenting under laparoscopic guidance and laparoscopic stitching of e-mail: [email protected] lacerations, laparoscopic ureteral reanastomosis or laparoscopic Current Opinion in Obstetrics and Gynecology ureteroneocystostomy for transections. Deep endometriosis surgery of an associated 2011, 23:296–300 hydronephrosis is associated with a high incidence of ureteral lesions making preoperative stenting desirable in order to facilitate the eventual repair, while avoiding the more problematic insertion of a stent after a lesion is made. The available data confirm the excellent outcome of stenting obstructive lesions. When stenting proves difficult or in case of a ureteral leakage, laparoscopic aided stenting is strongly suggested, in order to avoid further damage while permitting simultaneous repair if necessary. Laparoscopic suturing of a laceration over a stent is clearly superior to stenting only. -

Glickman Urological & Kidney Institute
Glickman Urological & Kidney Institute Graphic design and photography were provided by Cleveland Clinic’s Center for Medical Art and Photography. © The Cleveland Clinic Foundation 2017 9500 Euclid Avenue, Cleveland, OH 44195 clevelandclinic.org 2016 Outcomes 17-OUT-426 108374_CCFBCH_17OUT426_acg.indd 1-3 8/31/17 3:02 PM Measuring Outcomes Promotes Quality Improvement Clinical Trials Cleveland Clinic is running more than 2200 clinical trials at any given time for conditions including breast and liver cancer, coronary artery disease, heart failure, epilepsy, Parkinson disease, chronic obstructive pulmonary disease, asthma, high blood pressure, diabetes, depression, and eating disorders. Cancer Clinical Trials is a mobile app that provides information on the more than 200 active clinical trials available to cancer patients at Cleveland Clinic. clevelandclinic.org/cancertrialapp Healthcare Executive Education Cleveland Clinic has programs to share its expertise in operating a successful major medical center. The Executive Visitors’ Program is an intensive, 3-day behind-the-scenes view of the Cleveland Clinic organization for the busy executive. The Samson Global Leadership Academy is a 2-week immersion in challenges of leadership, management, and innovation taught by Cleveland Clinic leaders, administrators, and clinicians. Curriculum includes coaching and a personalized 3-year leadership development plan. clevelandclinic.org/executiveeducation Consult QD Physician Blog A website from Cleveland Clinic for physicians and healthcare professionals. Discover the latest research insights, innovations, treatment trends, and more for all specialties. consultqd.clevelandclinic.org Social Media Cleveland Clinic uses social media to help caregivers everywhere provide better patient care. Millions of people currently like, friend, or link to Cleveland Clinic social media — including leaders in medicine. -

The History of Microsurgery in Urological Practice
Chen-1 The History of Microsurgery in Urological Practice Mang L. Chen1, Gregory M. Buncke2 and Paul J. Turek3 1G.U. Recon, San Francisco, CA, 94114 2The Buncke Clinic, San Francisco, CA 94114 3The Turek Clinic, Beverly Hills, CA 90210 Correspondence to: Mang Chen, MD G.U. Recon 45 Castro St, Suite 111 San Francisco, CA 94114 Tel: 415-481-3980 Email: [email protected] Chen-2 Abstract Operative microscopy spans all surgical disciplines, allowing human dexterity to perform beyond direct visual limitations. Microsurgery started in otolaryngology, became popular in reconstructive microsurgery, and was then adopted in urology. Starting with reproductive tract reconstruction of the vas and epididymis, microsurgery in urology now extends to varicocele repair, sperm retrieval, penile transplantation and free flap phalloplasty. By examining the peer reviewed and lay literature this review discusses the history of microsurgery and its subsequent development as a subspecialty in urology. Keywords: urology, microsurgery, phalloplasty, vasovasostomy, varicocelectomy Chen-3 I. Introduction Microsurgery has been instrumental to surgical advances in many medical fields. Otolaryngology, ophthalmology, gynecology, hand and plastic surgery have all embraced the operating microscope to minimize surgical trauma and scar and to increase patency rates of vessels, nerves and tubes. Urologic adoption of microsurgery began with vasectomy reversals, testis transplants, varicocelectomies and sperm retrieval and has now progressed to free flap phalloplasties and penile transplantation. In this review, we describe the origins of microsurgery, highlight the careers of prominent microsurgeons, and discuss current use applications in urology. II. Birth of Microsurgery 1) Technology The birth of microsurgery followed from an interesting marriage of technology and clinical need. -

Examining Male Infertility
C O Examining Male Infertility N T I N U Susanne Quallich I N G n increasing number of Problems of male infertility can seem like minor issues within the couples seek evaluation larger realm of urology. But many male infertility diagnoses can be and treatment for infer- successfully treated, allowing the couple to conceive naturally or E tility, especially as more with minimal medical assistance. Some patients presenting with male D Acouples delay childbearing in infertility can have more significant disease. Treatments for male U order to establish their careers. A infertility will continue to progress, and as an increasing number of male factor alone is the cause of couples seek infertility services, the need to provide basic informa- C infertility in up to 20% of infer- tion grows as well. A tile couples and a contributing factor in another 30% to 40% of T all couples presenting for infertil- reproductive technologies. influence on overall male develop- I ity evaluations (American It is common to recommend ment and growth. Spermatogenesis O Urological Association [AUA] & an infertility evaluation in couples is driven by testosterone production N American Society for Reproduc- with a history of unprotected in the Leydig cells of the testes. tive Medicine (ASRM), 2001a; intercourse for at least 12 months Under the influence of luteinizing ASRM, 2004). Problems with without a pregnancy and with hormone (LH) and follicle-stimulat- infertility affect approximately 6.1 attempts to time intercourse with ing hormone (FSH), which are million people in the United ovulation, although this length of released from the anterior pituitary, States, or roughly 10% of the time can be shortened as the the testes begin to produce sperm in reproductive-age population. -

Robotic Surgery for Male Infertility
Robotic Surgery for Male Infertility Annie Darves-Bornoz, MD, Evan Panken, BS, Robert E. Brannigan, MD, Joshua A. Halpern, MD, MS* KEYWORDS Robotic surgical procedures Infertility Male Vasovasostomy Varicocele KEY POINTS Robotic-assisted approaches to male infertility microsurgery have potential practical benefits including reduction of tremor, 3-dimensional visualization, and decreased need for skilled surgical assistance. Several small, retrospective studies have described robotic-assisted vasectomy reversal with com- parable clinical outcomes to the traditional microsurgical approach. Few studies have described application of the robot to varicocelectomy, testicular sperm extrac- tion, and spermatic cord denervation. The use of robotic-assistance for male infertility procedures is evolving, and adoption has been limited. Rigorous studies are needed to evaluate outcomes and cost-effectiveness. INTRODUCTION with intraperitoneal and pelvic surgery. On the other hand, many of the theoretic and practical ad- Up to 15% of couples have infertility, with approx- 1,2 vantages offered by the robotic approach are imately 50% of cases involving a male factor. A highly transferrable to surgery for male infertility: substantial proportion of men with subfertility have surgically treatable and even reversible etiologies, High quality, 3-dimensional visualization is such as a varicocele or vasal obstruction. The essential for any microsurgical procedure. introduction of the operating microscope revolu- Improved surgeon ergonomics are always desir- tionized the field of male infertility, dramatically able, particularly given the surgeon morbidity improving visualization of small, complex associated with microsurgery.3 anatomic structures. The technical precision Filtering of physiologic tremor can improve pre- afforded has improved operative outcomes across cision during technically demanding micro- the board. -

Microsurgical Denervation of Spermatic Cord for Chronic Idiopathic Orchialgia: Long-Term Results from an Institutional Experience
Original Article pISSN: 2287-4208 / eISSN: 2287-4690 World J Mens Health 2019 January 37(1): 78-84 https://doi.org/10.5534/wjmh.180035 Microsurgical Denervation of Spermatic Cord for Chronic Idiopathic Orchialgia: Long-Term Results from an Institutional Experience Rajeev Chaudhari, Satyadeo Sharma , Shahil Khant, Krutik Raval Department of Urology, Ruby Hall Clinic, Pune, India Purpose: Chronic testicular pain remains an important challenge for urologists. At present there are many treatment modali- ties available for chronic orchialgia. Some patients remain in pain despite a conservative treatment. Microsurgical denerva- tion of spermatic cord appears to be successful in relieving pain in patients who fail conservative management. We assessed the long-term efficacy, complications and patient perceptions of microsurgical denervation of the spermatic cord in the treat- ment of chronic orchialgia. Materials and Methods: A prospective study was conducted from January 2007 to January 2016 which included men with testicular pain of >3 months duration, failure of conservative management, persistent of pain for >3 months after treating the underlying cause. Total 48 patients with 62 testicular units (14 bilateral) showed the response to spermatic cord block and underwent microsurgical denervation of spermatic cord. Results: Out of 62 testicular units (14 bilateral) which were operated, complete 2 years follow-up data were available for 38 testicular units. Out of these 38 units, 31 units (81.57%) had complete pain relief, 4 units (10.52%) had partial pain, and 3 units (7.89%) were non-responders. Complications were superficial wound infection in 3 units (4.83%), hydrocele in 2 units (3.22%), subcutaneous seroma in 2 units (3.22%), and an incisional hematoma in 1 unit (1.61%) out of 62 operated testicu- lar units. -

Urology Supplemental Guide
Supplemental Guide for Urology Supplemental Guide: Urology April 2020 1 Supplemental Guide for Urology TABLE OF CONTENTS Introduction .................................................................................................................................... 3 Patient Care .................................................................................................................................... 4 Patient Evaluation ........................................................................................................................ 4 Peri-Procedural Care .................................................................................................................... 6 Endoscopic Procedures ............................................................................................................... 8 Open Procedures ......................................................................................................................... 9 Minimally Invasive Procedures (Laparoscopic and Robotic) ..................................................... 10 Office-Based Procedures ........................................................................................................... 12 Medical Knowledge ...................................................................................................................... 14 Clinical Medical Knowledge........................................................................................................ 14 Clinical Reasoning ..................................................................................................................... -

The Acute Scrotum 12 Module 2
Department of Urology Medical Student Handbook INDEX Introduction 1 Contact Information 3 Chairman’s Welcome 4 What is Urology? 5 Urology Rotation Overview 8 Online Teaching Videos 10 Required Readings 11 Module 1. The Acute Scrotum 12 Module 2. Adult Urinary Tract Infections (UTI) 22 Module 3. Benign Prostatic Hyperplasia (BPH) 38 Module 4. Erectile Dysfunction (ED) 47 Module 5. Hematuria 56 Module 6. Kidney Stones 64 Module 7. Pediatric Urinary Tract Infections (UTI) 77 Module 8. Prostate Cancer: Screening and Management 88 Module 9. Urinary Incontinence 95 Module 10. Male Infertility 110 Urologic Abbreviations 118 Suggested Readings 119 Evaluation Process 121 Mistreatment/Harassment Policy 122 Research Opportunities 123 INTRODUCTION Hello, and welcome to Urology! You have chosen a great selective during your Surgical and Procedural Care rotation. Most of the students who take this subspecialty course enjoy themselves and learn more than they thought they would when they signed up for it. During your rotation you will meet a group of urologists who are excited about their medical specialty and feel privileged to work in it. Urology is a rapidly evolving technological specialty that requires surgical and diagnostic skills. Watch the video “Why Urology?” for a brief introduction to the field from the American Urological Association (AUA). https://youtu.be/kyvDMz9MEFA Urology at UW Urology is a specialty that treats patients with many different kinds of problems. At the UW you will see: patients with kidney problems including kidney cancer -

Press Release Fulton County Medical Center
PRESS RELEASE FULTON COUNTY MEDICAL CENTER WELCOMES UROLOGY GROUP. MCCONNELLSBURG, PA. April 6, 2015-- (LOCAL MEDIA) Fulton County Medical Center is pleased to announce Urology of Central Pennsylvania, Inc. will be providing Urology services at Fulton County Medical Center’s Specialty Services. Urologists, R. Scott Owens, MD and Christopher P. Moyer, DO will begin seeing patients April 21, 2015. Dr. Owens, Harrisburg Native, began practicing Medicine in 1987. He has been Board Certified in Urology since 1995. His active memberships include American Medical Association, American Urological Association, PA Medical Society, Dauphin County Medical Society, and Society of Laparoscopic Surgeons. He is Vice Chairman of Surgery and Divisional Chief of Urology, Pinnacle Health. He also serves on the Board of Urology of Central PA. Clinical Interests include: Laparoscopic Surgery, Robotic Surgeries (including radical prostatectomy, partial and total nephrectomy and pyeloplasty), Female surgery/reconstruction and incontinence, Female/male bladder slings. Dr. Owens graduated from Gettysburg College with a Bachelor of Arts in Chemistry, and Penn State University College of Medicine. He completed his residency at York Hospital - Surgical, University of Illinois At Peoria - Surgical, and Medical College of Wisconsin – Urological. His activities/hobbies include tennis and golf. Christopher P. Moyer, DO became board certified in Urologic Surgery in 2002, Prostate Brachytherapy (Proseed Method) in 2002, Greenlight Laser in 2004, and Robotics in 2007. He has active memberships with the Pennsylvania Osteopathic Medical Association, American Osteopathic Association, American College of Osteopathic Surgeons, and PA Medical Society. His professional activities include Holy Spirit Health System strategic planning committee and minimal invasive committee, president (Urologic Division) American College of Osteopathic Surgeons, and board Member Urology of Central PA. -
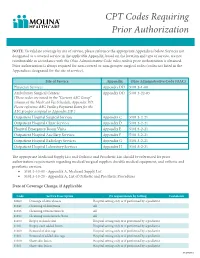
CPT Codes Requiring Prior Authorization
CPT Codes Requiring Prior Authorization NOTE: To validate coverage by site of service, please reference the appropriate Appendices below. Services not designated as a covered service in the applicable Appendix, based on the location and type of service, are not reimbursable in accordance with the Ohio Administrative Code rules, unless prior authorization is obtained. Prior authorization is always required for non-covered or non-grouper surgical codes (codes not listed in the Appendices designated for the site of service). Site of Service Appendix Ohio Administrative Code (OAC) Physician Services Appendix DD 5101:3-1-60 Ambulatory Surgical Centers Appendix DD 5101:3-22-03 (These codes are noted in the “Current ASC Group” column of the Medicaid Fee Schedule, Appendix DD. Please reference ASC Facility Payment Rates for the ASC grouper assigned in Appendix DD.) Outpatient Hospital Surgical Services Appendix C 5101:3-2-21 Outpatient Hospital Clinic Services Appendix D 5101:3-2-21 Hospital Emergency Room Visits Appendix E 5101:3-2-21 Outpatient Hospital Ancillary Services Appendix F 5101:3-2-21 Outpatient Hospital Radiology Services Appendix G 5101:3-2-21 Outpatient Hospital Laboratory Services Appendix H 5101:3-2-21 The appropriate Medicaid Supply List and Orthotic and Prosthetic List should be referenced for prior authorization requirements regarding medical/surgical supplies, durable medical equipment, and orthotic and prosthetic services. • 5101:3-10-03 - Appendix A, Medicaid Supply List • 5101:3-10-20 - Appendix A, List of Orthotic and