Wrvus: Do They Really Measure the Workload and Complexity of What We Do?
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Urology Scientific Session Monday, September 28, 2020
Urology Scientific Session Monday, September 28, 2020 Moderators/Panelists: Drs. Sabine Zundel, Sameh Shehata, Holger Till, Yuri Kozlov, Philipp Szavay, Eduardo Perez (S26) PNEUMOVESICOSCOPIC CORRECTION OF PRIMARY VESICOURETERAL REFLUX (VUR) IN CHILDREN. - OUR INITIAL EXPERIENCE- A. M. Benaired, Pediatric, Surgeon; H Zahaf, Pediatric, Surgeon; Military Central Hospital Purpose: Vesicoureteral reflux is a common urological abnormality predisposing risk of childhood hypertension and chronic renal failure. It is called primitive when it is due to an abnormality of the vesicoureteral junction. Different treatment approaches have been proposed a long time. Two main trends can be identified, conservative and operative approach. The main objective of our prospective study is to demonstrate the feasibility of vesicoscopic crosstrigonal ureteral reimplantation under CO2 pneumovesicum in treatment on primary vesicoureteral reflux and analyze results of this approach. Methods: A total of 60 patients underwent transvesicoscopic ureteral reimplantation (33 boys, 27 girls) by the same surgeon from Mai 2011 to Mai 2015. All patients had primary vesicoureteral reflux, and surgery was performed because of breakthrough urinary tract infection despite antibiotic prophylaxis, persistent high grade of vesicoureteral reflux especially in association with significant renal scarring, mean age at operation was 47.47 month (5 month - 12 years). Of the 60 patients, 34 had bilateral reflux and 26 had unilateral reflux. The reflux grade in the total of 94 ureters was grade IV, V in 59.57%, grade III in 35.11% and grade II in 5.32% in association with contralateral high grade vesicoureteral reflux. Our surgical methods followed those reported by Valla et al. Results: The transvesicoscopic procedure was successfully completed in all patients without perioperative complication except one case of pneumoperitoneum that required exsufflation by open laparoscopy. -

Laparoscopic Ureteral Repair in Gynaecological Surgery Carlo De Ciccoa, Anastasia Ussiab and Philippe Robert Koninckxb,C
Laparoscopic ureteral repair in gynaecological surgery Carlo De Ciccoa, Anastasia Ussiab and Philippe Robert Koninckxb,c aDepartment of Obstetrics and Gynaecology, Purpose of review University Hospital A. Gemelli, Universita` Cattolica del Sacro Cuore, bGruppo Italo-Belga, Rome, Italy and To review laparoscopic surgery in the treatment options for ureteral lesions in cDepartment of Obstetrics and Gynaecology, gynaecological surgery. University Hospital Gasthuisberg, Katholieke Recent findings Universiteit Leuven, Leuven, Belgium Laparoscopic treatment of ureteral injuries has been increasingly reported over the past Correspondence to Dr Carlo De Cicco, Department of Obstetrics and Gynaecology, University Hospital A. years. Treatment has progressively shifted from ureteroneocystostomy performed by Gemelli, Universita` Cattolica del Sacro Cuore, Largo F. laparotomy to less invasive treatment options such as ureteral stenting or dilatation in Vito 1, 00168 Rome, Italy Tel: +39 06 30155131; case of stricture, stenting under laparoscopic guidance and laparoscopic stitching of e-mail: [email protected] lacerations, laparoscopic ureteral reanastomosis or laparoscopic Current Opinion in Obstetrics and Gynecology ureteroneocystostomy for transections. Deep endometriosis surgery of an associated 2011, 23:296–300 hydronephrosis is associated with a high incidence of ureteral lesions making preoperative stenting desirable in order to facilitate the eventual repair, while avoiding the more problematic insertion of a stent after a lesion is made. The available data confirm the excellent outcome of stenting obstructive lesions. When stenting proves difficult or in case of a ureteral leakage, laparoscopic aided stenting is strongly suggested, in order to avoid further damage while permitting simultaneous repair if necessary. Laparoscopic suturing of a laceration over a stent is clearly superior to stenting only. -

Press Release Fulton County Medical Center
PRESS RELEASE FULTON COUNTY MEDICAL CENTER WELCOMES UROLOGY GROUP. MCCONNELLSBURG, PA. April 6, 2015-- (LOCAL MEDIA) Fulton County Medical Center is pleased to announce Urology of Central Pennsylvania, Inc. will be providing Urology services at Fulton County Medical Center’s Specialty Services. Urologists, R. Scott Owens, MD and Christopher P. Moyer, DO will begin seeing patients April 21, 2015. Dr. Owens, Harrisburg Native, began practicing Medicine in 1987. He has been Board Certified in Urology since 1995. His active memberships include American Medical Association, American Urological Association, PA Medical Society, Dauphin County Medical Society, and Society of Laparoscopic Surgeons. He is Vice Chairman of Surgery and Divisional Chief of Urology, Pinnacle Health. He also serves on the Board of Urology of Central PA. Clinical Interests include: Laparoscopic Surgery, Robotic Surgeries (including radical prostatectomy, partial and total nephrectomy and pyeloplasty), Female surgery/reconstruction and incontinence, Female/male bladder slings. Dr. Owens graduated from Gettysburg College with a Bachelor of Arts in Chemistry, and Penn State University College of Medicine. He completed his residency at York Hospital - Surgical, University of Illinois At Peoria - Surgical, and Medical College of Wisconsin – Urological. His activities/hobbies include tennis and golf. Christopher P. Moyer, DO became board certified in Urologic Surgery in 2002, Prostate Brachytherapy (Proseed Method) in 2002, Greenlight Laser in 2004, and Robotics in 2007. He has active memberships with the Pennsylvania Osteopathic Medical Association, American Osteopathic Association, American College of Osteopathic Surgeons, and PA Medical Society. His professional activities include Holy Spirit Health System strategic planning committee and minimal invasive committee, president (Urologic Division) American College of Osteopathic Surgeons, and board Member Urology of Central PA. -
CPT Codes Requiring Prior Authorization
CPT Codes Requiring Prior Authorization NOTE: To validate coverage by site of service, please reference the appropriate Appendices below. Services not designated as a covered service in the applicable Appendix, based on the location and type of service, are not reimbursable in accordance with the Ohio Administrative Code rules, unless prior authorization is obtained. Prior authorization is always required for non-covered or non-grouper surgical codes (codes not listed in the Appendices designated for the site of service). Site of Service Appendix Ohio Administrative Code (OAC) Physician Services Appendix DD 5101:3-1-60 Ambulatory Surgical Centers Appendix DD 5101:3-22-03 (These codes are noted in the “Current ASC Group” column of the Medicaid Fee Schedule, Appendix DD. Please reference ASC Facility Payment Rates for the ASC grouper assigned in Appendix DD.) Outpatient Hospital Surgical Services Appendix C 5101:3-2-21 Outpatient Hospital Clinic Services Appendix D 5101:3-2-21 Hospital Emergency Room Visits Appendix E 5101:3-2-21 Outpatient Hospital Ancillary Services Appendix F 5101:3-2-21 Outpatient Hospital Radiology Services Appendix G 5101:3-2-21 Outpatient Hospital Laboratory Services Appendix H 5101:3-2-21 The appropriate Medicaid Supply List and Orthotic and Prosthetic List should be referenced for prior authorization requirements regarding medical/surgical supplies, durable medical equipment, and orthotic and prosthetic services. • 5101:3-10-03 - Appendix A, Medicaid Supply List • 5101:3-10-20 - Appendix A, List of Orthotic and -

A Comparative Study Between Open and Laparoscopic Pyeloplasty
Ali Hamdan Fahad /J. Pharm. Sci. & Res. Vol. 9(10), 2017, 1961-1965 A Comparative Study between Open and Laparoscopic Pyeloplasty Ali Hamdan Fahad College of Medicine, University of Al-Qadisiyah, Iraq Abstract: Background: Historically “open pyeloplasty” has been regarded as the goldistandard for the surgicalimanagement of ureteropelvicijunctioniobstruction (UPJO). The treatment of this condition has evolved graetly over the past twenty years resulting in new surgical approaches. One of these approaches is laparoscopic pyeloplasty, this technique aimed to achieve similar results as openisurgery, with lower rates of morbidityicomplications. Aim of the study: to compare the “operative time”, “hospital stay”, analgesic use, “perioperativei complications” and “success rate” between laparoscopic and openipyeloplasty in Al Diwaniya Teaching Hospital. Patients & Methods: forty patients (26 males and 14 females) with ureteropelvic junction obstruction who had been presented to the urology ward of Al Diwaniya Teaching Hospital, were enrolled in this study. The patients included on the basisiof standard indications for PUJO repair. The patients were divided into 2 groups. Twenty patients underwent transperitonealilaparoscopic pyeloplasty and 20 patients operated upon by open surgery. We compared the “operative time”, “complications rates”, hospitalistay and “success rate” of the two groups. Results: Meanioperative time was 2 hours and 3 hours in open& laparoscopic pyeloplastyigroups, respectively. Meanihospital stay was shorter (24 hours) in the laparoscopicigroup and (48 hours) in openogroup. Mean follow-up period was 9 months. Postoperativeicomplication rates were 45 % and 55 % in laparoscopic& open pyeloplastyigroups, respectively. Successirates were 95% and 90 % for open and laparoscopic#pyeloplasty groups, respectively. Redo surgery was needed in 2 patients of laparoscopy and 1 of open surgery |groups due to recurrence of stricture. -
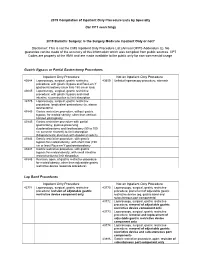

2019 Compilation of Inpatient Only Procedure Lists by Specialty
2019 Compilation of Inpatient Only Procedure Lists by Specialty (for CPT searching) 2019 Bariatric Surgery: Is the Surgery Medicare Inpatient Only or not? Disclaimer: This is not the CMS Inpatient Only Procedure List (Annual OPPS Addendum E). No guarantee can be made of the accuracy of this information which was compiled from public sources. CPT Codes are property of the AMA and are made available to the public only for non-commercial usage. Gastric Bypass or Partial Gastrectomy Procedures Inpatient Only Procedure Not an Inpatient Only Procedure 43644 Laparoscopy, surgical, gastric restrictive 43659 Unlisted laparoscopy procedure, stomach procedure; with gastric bypass and Roux-en-Y gastroenterostomy (roux limb 150 cm or less) 43645 Laparoscopy, surgical, gastric restrictive procedure; with gastric bypass and small intestine reconstruction to limit absorption 43775 Laparoscopy, surgical, gastric restrictive procedure; longitudinal gastrectomy (ie, sleeve gastrectomy) 43843 Gastric restrictive procedure, without gastric bypass, for morbid obesity; other than vertical- banded gastroplasty 43845 Gastric restrictive procedure with partial gastrectomy, pylorus-preserving duodenoileostomy and ileoileostomy (50 to 100 cm common channel) to limit absorption (biliopancreatic diversion with duodenal switch) 43846 Gastric restrictive procedure, with gastric bypass for morbid obesity; with short limb (150 cm or less) Roux-en-Y gastroenterostomy 43847 Gastric restrictive procedure, with gastric bypass for morbid obesity; with small intestine reconstruction -

Community Benefit Report Continuing Our Commitment to a Healthy Community Table of Contents
2015 Community Benefit Report Continuing Our Commitment to a Healthy Community Table of Contents To Our Community Partners and Friends: a Letter From Our President and CEO ...............1 About Children’s Hospital Los Angeles ........................................................................2 Our Commitment to the Community ............................................................................3 Community Demographics ........................................................................................4 Community Benefit Implementation Strategy .................................................................7 A Lens on Our Community’s Health ............................................................................8 Increasing Access to Health Care Resources and Information for Children, Youth and Families in our Community .......................................................................10 Raising Awareness of Pediatric Health and Related Safety and Social Issues in the Community ...................................................................................................14 Having an Impact on Reducing Obesity in Children and Youth in Our Community .....................................................................................................16 Enhancing Access to Development and Training Opportunities Targeting Youth and Young Adults in our Community ................................................................18 Achieving our Best With our Community Partners .......................................................20 -

Robotic Assisted Laproscopic Pyeloplasty
ROBOTIC ASSISTED LAPROSCOPIC PYELOPLASTY ROBOTIC ASSISTED LAPROSCOPIC PYELOPLASTY Location of Surgery: Saint John’s Health Center 2121 Santa Monica Blvd Valet parking available Hospital Phone: 310-829-5511 Patient Name: Date and Time of Surgery: Check-in Arrival Time (2 hours prior to surgery): Physician: Duration of Procedure: Approximate Total Time (arrival to discharge): Office Telephone: 310-582-7137 Office Fax: 310-582-7140 BE SURE TO ARRANGE FOR A FAMILY OR FRIEND TO DRIVE YOU HOME. IT IS RECOMMENDED THAT SOMEONE STAY WITH YOU FOR THE FIRST 24 HOURS AFTER THE PROCEDURE. John Wayne Cancer Institute | Department of Urology and Urologic Oncology | Updated 5/8/20 | Page 1 ROBOTIC ASSISTED LAPROSCOPIC PYELOPLASTY GENERAL INFORMATION Pyeloplasty is a procedure performed to correct an obstructive narrowing of the ureteropelvic junction (UPJ), an area of the upper tract collecting system just outside of the kidney. UPJ area bulging with urine, due to narrowing of ureter Urine is made in the kidney and then deposited into an upper, middle, and lower pole calyx. All three of these then merge into the renal pelvis and hilus of the kidney, which then leaves the body through the ureter to the bladder. The UPJ is the area between the renal pelvis/hilus and the ureter. This area can be narrowed congenitally (from birth), traumatically from injury, or from compression from crossing vessels that attach to the large artery the aorta. During the pyeloplasty procedure, the narrowed segment is removed and the remaining ends are re-connected. NORMAL ANATOMY John Wayne Cancer Institute | Department of Urology and Urologic Oncology | Updated 5/8/20 | Page 2 ROBOTIC ASSISTED LAPROSCOPIC PYELOPLASTY Pyeloplasty is performed robotically using the DaVinci Robot machine. -

2018 National Physician Fee Schedule Relative Value File January Release CPT Codes and Descriptions Only Are Copyright 2016 American Medical Association
2018 National Physician Fee Schedule Relative Value File January Release CPT codes and descriptions only are copyright 2016 American Medical Association. All Rights Reserved. Applicable FARS/DFARS Apply. Dental codes (D codes) are copyright 2017/17 American Dental Association. All Rights Reserved. RELEASED 12/18/2017 NON-FACILITY HCPCS MOD DESCRIPTION TOTAL MULTIPLIER TOTAL 10021 Fna w/o image 3.47 $70.00 $242.90 10022 Fna w/image 4.00 $70.00 $280.00 1003F Level of activity assess 0.00 $70.00 $0.00 10030 Guide cathet fluid drainage 16.04 $70.00 $1,122.80 10035 Perq dev soft tiss 1st imag 14.71 $70.00 $1,029.70 10036 Perq dev soft tiss add imag 12.90 $70.00 $903.00 1004F Clin symp vol ovrld assess 0.00 $70.00 $0.00 10040 Acne surgery 3.13 $70.00 $219.10 1005F Asthma symptoms evaluate 0.00 $70.00 $0.00 1006F Osteoarthritis assess 0.00 $70.00 $0.00 10060 Drainage of skin abscess 3.38 $70.00 $236.60 10061 Drainage of skin abscess 5.87 $70.00 $410.90 1007F Anti-inflm/anlgsc otc assess 0.00 $70.00 $0.00 1008F Gi/renal risk assess 0.00 $70.00 $0.00 10080 Drainage of pilonidal cyst 5.12 $70.00 $358.40 10081 Drainage of pilonidal cyst 7.68 $70.00 $537.60 1010F Severity angina by actvty 0.00 $70.00 $0.00 1011F Angina present 0.00 $70.00 $0.00 1012F Angina absent 0.00 $70.00 $0.00 10120 Remove foreign body 4.38 $70.00 $306.60 10121 Remove foreign body 7.83 $70.00 $548.10 10140 Drainage of hematoma/fluid 4.69 $70.00 $328.30 1015F Copd symptoms assess 0.00 $70.00 $0.00 10160 Puncture drainage of lesion 3.71 $70.00 $259.70 1018F Assess dyspnea not present -

INSTITUTE the for ADVANCED and MINIMALLY INVASIVE SURGERY
The INSTITUTE for ADVANCED and MINIMALLY INVASIVE SURGERY Inst for Advanced&Minimally Invasive Surgery_GC_V2_FINAL.indd 3 5/24/11 1:51 PM The ew York Methodist Hospital was one of the first surgical teaching hospitals in the United States. Its Department of I N S T I T U T E N Surgery was founded by a pioneer surgeon, Lewis S. Pilcher, who also founded the Annals of Surgery. The Hospital’s Institute for for Advanced and Minimally Invasive Surgery at New York Methodist Hospital continues a proud tradition. ADVANCED The Institute offers a range of advanced procedures involving surgical techniques that include laparoscopy, endoscopy and robotic- AND assisted surgery. Surgeons on the Institute’s panel specialize in many disease entities and areas; all of them are trained experts in advanced M I N I M A L L Y and/or minimally invasive surgical techniques. They include specialists in cardiac surgery, endovascular surgery, thoracic surgery, neurosurgery, I N V A S I V E urology, orthopedic surgery, laparoscopic surgery and podiatry. SURGERY Referrals to these specialists can be made through an individual’s primary care physician or can be requested through the Institute’s referral service. at Physicians and other health care professionals affiliated with N E W Y O R K the Institute are also available to speak to community groups on a variety of topics related to disease prevention and treatment. M E T H O D I S T Other community outreach activities of the Institute include the distribution of informational materials and screening programs. HOSPITAL -

2017 National Physician Fee Schedule Relative Value File January Release CPT Codes and Descriptions Only Are Copyright 2015 American Medical Association
2017 National Physician Fee Schedule Relative Value File January Release CPT codes and descriptions only are copyright 2015 American Medical Association. All Rights Reserved. Applicable FARS/DFARS Apply. Dental codes (D codes) are copyright 2016/16 American Dental Association. All Rights Reserved. RELEASED 11/14/2016 NON-FACILITY HCPCS MOD DESCRIPTION TOTAL MULTIPLIER TOTAL 10021 Fna w/o image 3.47 70.00 $242.90 10022 Fna w/image 4.00 70.00 $280.00 1003F Level of activity assess 0.00 70.00 $0.00 10030 Guide cathet fluid drainage 19.80 70.00 $1,386.00 10035 Perq dev soft tiss 1st imag 15.25 70.00 $1,067.50 10036 Perq dev soft tiss add imag 13.19 70.00 $923.30 1004F Clin symp vol ovrld assess 0.00 70.00 $0.00 10040 Acne surgery 2.89 70.00 $202.30 1005F Asthma symptoms evaluate 0.00 70.00 $0.00 1006F Osteoarthritis assess 0.00 70.00 $0.00 10060 Drainage of skin abscess 3.33 70.00 $233.10 10061 Drainage of skin abscess 5.86 70.00 $410.20 1007F Anti-inflm/anlgsc otc assess 0.00 70.00 $0.00 1008F Gi/renal risk assess 0.00 70.00 $0.00 10080 Drainage of pilonidal cyst 5.08 70.00 $355.60 10081 Drainage of pilonidal cyst 7.63 70.00 $534.10 1010F Severity angina by actvty 0.00 70.00 $0.00 1011F Angina present 0.00 70.00 $0.00 1012F Angina absent 0.00 70.00 $0.00 10120 Remove foreign body 4.32 70.00 $302.40 10121 Remove foreign body 7.77 70.00 $543.90 10140 Drainage of hematoma/fluid 4.63 70.00 $324.10 1015F Copd symptoms assess 0.00 70.00 $0.00 10160 Puncture drainage of lesion 3.68 70.00 $257.60 1018F Assess dyspnea not present 0.00 70.00 $0.00 -

Laparoscopic Pyeloplasty for Ureteropelvic Junctions Obstruction in Adults: 6 Years’ Experience in One Center
Hindawi BioMed Research International Volume 2017, Article ID 6743512, 4 pages https://doi.org/10.1155/2017/6743512 Research Article Laparoscopic Pyeloplasty for Ureteropelvic Junctions Obstruction in Adults: 6 Years’ Experience in One Center Rikke Søgaard Tolstrup, Marie Thue Pank, Lotte Sander, and Torben Dørflinger Department of Urology, Aalborg University Hospital, Aalborg, Denmark Correspondence should be addressed to Rikke Søgaard Tolstrup; [email protected] Received 14 October 2016; Revised 7 March 2017; Accepted 26 April 2017; Published 11 June 2017 Academic Editor: Christian Schwentner Copyright © 2017 Rikke Søgaard Tolstrup et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Objective. Ureteropelvic junction obstruction (UPJO) is a common cause of symptomatic ureteral obstruction. The aim of this study is to assess the outcome of laparoscopic pyeloplasty in patients with UPJO. Patients and Methods. Medical reports of 47 UPJO patients treated with laparoscopic pyeloplasty were retrospectively analysed. All patients were recruited from our center in the period 2004–2011. Results.Weevaluated47patients.Meanagewas36yearsandmeanhospitalstay3.6days.42(79%)ofthe patients had pain and 46 (98%) were diagnosed with hydronephrosis. 19 patients (40%) had a renal function below 40% of the affected kidney and 49% had impaired renal scan drainage. Postoperative significant improvement in pain score and renal scan drainage was found in 92% and 47% of the patients, respectively. Improvement of renal function > 10% was found in 11 patients (23%); the function remained stable in 31 patients (66%) and deteriorated > 10% in 5 patients (11%).