Cervical Spinal Stenosis
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Diapositiva 1
Thoracic Cage and Thoracic Inlet Professor Dr. Mario Edgar Fernández. Parts of the body The Thorax Is the part of the trunk betwen the neck and abdomen. Commonly the term chest is used as a synonym for thorax, but it is incorrect. Consisting of the thoracic cavity, its contents, and the wall that surrounds it. The thoracic cavity is divided into 3 compartments: The central mediastinus. And the right and left pulmonary cavities. Thoracic Cage The thoracic skeleton forms the osteocartilaginous thoracic cage. Anterior view. Thoracic Cage Posterior view. Summary: 1. Bones of thoracic cage: (thoracic vertebrae, ribs, and sternum). 2. Joints of thoracic cage: (intervertebral joints, costovertebral joints, and sternocostal joints) 3. Movements of thoracic wall. 4. Thoracic cage. Thoracic apertures: (superior thoracic aperture or thoracic inlet, and inferior thoracic aperture). Goals of the classes Identify and describe the bones of the thoracic cage. Identify and describe the joints of thoracic cage. Describe de thoracic cage. Describe the thoracic inlet and identify the structures passing through. Vertebral Column or Spine 7 cervical. 12 thoracic. 5 lumbar. 5 sacral 3-4 coccygeal Vertebrae That bones are irregular, 33 in number, and received the names acording to the position which they occupy. The vertebrae in the upper 3 regions of spine are separate throughout the whole of life, but in sacral anda coccygeal regions are in the adult firmly united in 2 differents bones: sacrum and coccyx. Thoracic vertebrae Each vertebrae consist of 2 essential parts: An anterior solid segment: vertebral body. The arch is posterior an formed of 2 pedicles, 2 laminae supporting 7 processes, and surrounding a vertebral foramen. -

Cervical Fusion
Medical Coverage Policy Effective Date ............................................. 6/15/2021 Next Review Date ....................................... 6/15/2022 Coverage Policy Number .................................. 0527 Cervical Fusion Table of Contents Related Coverage Resources Overview .............................................................. 1 Acupuncture Coverage Policy ................................................... 1 Bone, Cartilage and Ligament Graft Substitutes General Background ............................................ 4 Bone Growth Stimulators: Electrical (Invasive, Medicare Coverage Determinations .................... 9 Noninvasive), Ultrasound Coding/Billing Information .................................... 9 Discography Intervertebral Disc (IVD) Prostheses References ........................................................ 11 Intraoperative Monitoring Lumbar Fusion for Spinal Instability and Degenerative Disc Conditions, Including Sacroiliac Fusion Minimally Invasive Intradiscal/Annular Procedures and Trigger Point Injections INSTRUCTIONS FOR USE The following Coverage Policy applies to health benefit plans administered by Cigna Companies. Certain Cigna Companies and/or lines of business only provide utilization review services to clients and do not make coverage determinations. References to standard benefit plan language and coverage determinations do not apply to those clients. Coverage Policies are intended to provide guidance in interpreting certain standard benefit plans administered by Cigna Companies. -
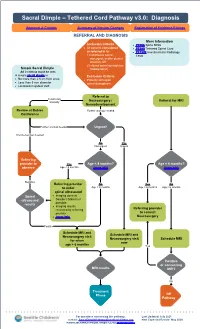
Sacral Dimple – Tethered Cord Pathway V3.0: Diagnosis
Sacral Dimple – Tethered Cord Pathway v3.0: Diagnosis Approval & Citation Summary of Version Changes Explanation of Evidence Ratings REFERRAL AND DIAGNOSIS More Information Inclusion Criteria • PE056 Spina Bifida • All patients considered • PE589 Tethered Spinal Cord or referred in for • PE1999 Anesthesia for Radiology 1) cutaneous sacral, Tests coccygeal, and/or gluteal anomaly OR 2) closed spinal dysraphism Simple Sacral Dimple (radiographic) All 3 criteria must be met. A simple sacral dimple is: Exclusion Criteria • No more than 2.5 cm from anus • Patients with open • Less than 5 mm diameter spinal dysraphism • Localized in gluteal cleft Referral to Cutaneous anomaly Neurosurgery / Referral for MRI Neurodevelopment Review at Babies Further workup needed Conference Further workup needed Urgent? No intervention needed No Yes Not urgent Urgent Referring provider to Yes Age < 4 months? Age < 6 months? observe Age < 4 months (more info) (more info) Negative Referring provider No Yes No to order Age ≥ 4 months Age < 6 months Age ≥ 6 months spinal ultrasound Spinal • Imaging done at ultrasound Seattle Children’s if results possible • Imaging results reviewed by referring Referring provider provider to consult • (more info) Neurosurgery Positive Schedule MRI and Schedule MRI and Neurosurgery visit Neurosurgery visit Schedule MRI for when now age > 6 months Yes Positive or concerning MRI results MRI? No Treatment Phase Off Pathway For questions concerning this pathway, Last Updated: July 2021 contact: [email protected] -

Anatomy of the Spine
12 Anatomy of the Spine Overview The spine is made of 33 individual bones stacked one on top of the other. Ligaments and muscles connect the bones together and keep them aligned. The spinal column provides the main support for your body, allowing you to stand upright, bend, and twist. Protected deep inside the bones, the spinal cord connects your body to the brain, allowing movement of your arms and legs. Strong muscles and bones, flexible tendons and ligaments, and sensitive nerves contribute to a healthy spine. Keeping your spine healthy is vital if you want to live an active life without back pain. Spinal curves When viewed from the side, an adult spine has a natural S-shaped curve. The neck (cervical) and low back (lumbar) regions have a slight concave curve, and the thoracic and sacral regions have a gentle convex curve (Fig. 1). The curves work like a coiled spring to absorb shock, maintain balance, and allow range of motion throughout the spinal column. The muscles and correct posture maintain the natural spinal curves. Good posture involves training your body to stand, walk, sit, and lie so that the least amount of strain is placed on the spine during movement or weight-bearing activities. Excess body weight, weak muscles, and other forces can pull at the spine’s alignment: • An abnormal curve of the lumbar spine is lordosis, also called sway back. • An abnormal curve of the thoracic spine is Figure 1. (left) The spine has three natural curves that form kyphosis, also called hunchback. an S-shape; strong muscles keep our spine in alignment. -

Delayed Diagnosis of Tandem Spinal Stenosis: a Retrospective Institutional Review
International Journal of Spine Surgery, Vol. 13, No. 3, 2019, pp. 283–288 https://doi.org/10.14444/6038 ÓInternational Society for the Advancement of Spine Surgery Delayed Diagnosis of Tandem Spinal Stenosis: A Retrospective Institutional Review AMIT BHANDUTIA, MD, LUKE BROWN, MD, MBA, ALYSA NASH, MD, IAN BUSSEY, MD, MARK SHASTI, MD, EUGENE KOH, MD, PHD, KELLEY BANAGAN, MD, STEVEN LUDWIG, MD, DANIEL GELB, MD Department of Orthopaedics, University of Maryland Medical Center, Baltimore, Maryland ABSTRACT Background: Tandem spinal stenosis (TSS) is defined as simultaneous spinal stenosis in the cervical, thoracic, and/or lumbar regions and may present with both upper and lower motor neuron symptoms, neurogenic claudication, and gait disturbance. Current literature has focused mainly on the prevalence of TSS and treatment methods, while the incidence of delayed TSS diagnosis is not well defined. The purpose of this study was to determine the incidence of delayed TSS diagnosis at our institution and describe the clinical characteristics commonly observed in their particular presentation. Methods: Following institutional review board approval, an institutional billing database review was performed for patients who underwent a spinal decompression procedure between 2006 and 2016. Thirty-three patients who underwent decompression on 2 separate spinal regions within 1 year were included for review. Patients with delayed diagnosis of TSS following the first surgery were differentiated from those with preoperative diagnosis of TSS. Results: TSS requiring surgical decompression occurred in 33 patients, with the incidence being 2.06% in this cohort. Fifteen patients received a delayed diagnosis after the first surgical decompression (45%) and were found to have a longer interval between decompressions (7.6 6 2.1 months versus 4.01 6 3 months, P ¼ .0004). -

Protocols Full Document
STATE OF RHODE ISLAND WORKERS’ COMPENSATION COURT MEDICAL ADVISORY BOARD PROTOCOLS Approved by the Medical Advisory Board Rhode Island Workers’ Compensation Court John Parziale, MD Robert M. Ferrieri Chair Chief Judge Workers’ Compensation Court Sheila G. Mitchell, RN, BSN Medical Advisory Board Administrator Effective: 1/28/2020 1 TABLE OF CONTENTS YEAR PROTCOL WAS LAST REVIEWED . 3 PREFACE. 4 CARPAL TUNNEL SYNDROME . 5 CERVICAL MUSCULOLIGAMENTOUS INJURY (Sprain/Strain) . 8 HERNIATED CERVICAL DISC . 11 PROTOCOLS FOR INJURIES TO THE EYE . 15 PROTOCOL FOR THE EVALUATION AND MANAGEMENT OF ACUTE SHOULDER INJURIES . 26 PROTOCOL FOR THE MANAGEMENT OF ACUTE INJURIES TO THE KNEE . 29 LOW BACK MUSCULOLIGAMENTOUS INJURY (SPRAIN/STRAIN). 33 HERNIATED LUMBAR DISC. 36 LUMBAR FUSION.. 40 TRAUMATIC BRAIN INJURY.(formerly Post Traumatic Headache) . 42 CHRONIC REGIONAL PAIN SYNDROME (formerly Symp. Dyst.). 47 THORACIC OUTLET SYNDROME . 51 PROTOCOLS FOR INJURIES TO THE FOOT AND ANKLE. 54 WORKERS COMP. PROTOCOLS WHEN PRIMARY INJURY IS PSYCHIATRIC/PSYCHOLOGICAL. 69 OUTPATIENT PHYSICAL AND OCCUPATIONAL THERAPY PROTOCOL GUIDELINES. 84 ACOUSTIC TRAUMA. 91 INTERVENTIONAL PAIN MANAGEMENT TREATMENT PROTOCOL . 95 WORK HARDENING PROTOCOLS . 113 PROTOCOL FOR THE MANAGEMENT OF HERNIAS . .. 118 ACUPUNCTURE.. 123 TEMPOROMANDIBULAR JOINT DISORDERS.. 126 ACUTE HAND INJURY PROTOCOLS.. 131 PHARMACEUTICAL PROTOCOLS . 144 CONTACT DERMATITIS PROTOCOL. 145 CUBITAL TUNNEL SYNDROME.. 147 RADIAL TUNNEL SYNDROME . 150 SPINAL COLUMN STIMULATORS . 153 ANTERIOR CRUCIATE RUPTURES . 155 HEARING LOSS PROTOCOL . 157 INITIAL VOCATIONAL ASSESSMENT PROTOCOL GUIDELINES. 159 HIERARCHY OF VOCATIONAL REHABILITATION. 161 OCCUPATIONAL HEARING IMPAIRMENT TREATMENT PROTOCOL . 162 DIAGNOSIS AND INITIAL TREATMENT OF OCCUPATIONAL ASTHMA . 166 CHRONIC NONINTERVENTIONAL, NONCANCER PAIN PROTOCOL . 174 2 YEAR PROTOCOL WAS LAST REVIEWED PREFACE CARPAL TUNNEL SYNDROME . -

Vertebral Column
Vertebral Column • Backbone consists of Cervical 26 vertebrae. • Five vertebral regions – Cervical vertebrae (7) Thoracic in the neck. – Thoracic vertebrae (12) in the thorax. – Lumbar vertebrae (5) in the lower back. Lumbar – Sacrum (5, fused). – Coccyx (4, fused). Sacrum Coccyx Scoliosis Lordosis Kyphosis Atlas (C1) Posterior tubercle Vertebral foramen Tubercle for transverse ligament Superior articular facet Transverse Transverse process foramen Facet for dens Anterior tubercle • Atlas- ring of bone, superior facets for occipital condyles. – Nodding movement signifies “yes”. Axis (C2) Spinous process Lamina Vertebral foramen Transverse foramen Transverse process Superior articular facet Odontoid process (dens) •Axis- dens or odontoid process is body of atlas. – Pivotal movement signifies “no”. Typical Cervical Vertebra (C3-C7) • Smaller bodies • Larger spinal canal • Transverse processes –Shorter – Transverse foramen for vertebral artery • Spinous processes of C2 to C6 often bifid • 1st and 2nd cervical vertebrae are unique – Atlas & axis Typical Cervical Vertebra Spinous process (bifid) Lamina Vertebral foramen Inferior articular process Superior articular process Transverse foramen Pedicle Transverse process Body Thoracic Vertebrae (T1-T12) • Larger and stronger bodies • Longer transverse & spinous processes • Demifacets on body for head of rib • Facets on transverse processes (T1-T10) for tubercle of rib Thoracic Vertebra- superior view Spinous process Transverse process Facet for tubercle of rib Lamina Superior articular process -

The Spinal Canal in Cervical Spondylosis
J Neurol Neurosurg Psychiatry: first published as 10.1136/jnnp.26.2.166 on 1 April 1963. Downloaded from J. Neurol. Neurosurg. Psychiat., 1963, 26, 166 The spinal canal in cervical spondylosis A. R. CHRISPIN AND F. LEES From the Departments of Diagnostic Radiology and Neurology, St. Bartholomew's Hospital, London Cervical spondylosis was defined by Brain (1948), by the canal size with one of the patient's own para- Brain, Northfield, and Wilkinson (1952), and by meters in the region, namely, the size of the bodies of Frykholm (1951). Its essential features are protrusion the cervical vertebrae. This method eliminates geo- of the annulus fibrosus and changes in the adjacent metrical errors of radiographic projection and avoids vertebral margins. The size of the cervical spinal the difficulties in measuring the varying antero- canal may play a major part in the neurological posterior diameters of the irregular canal. manifestations of cervical spondylosis. The antero-posterior diameters of the cervical canal in 200 normal adults were measured by Boijsen METHOD (1954). Wolf, Khilnani, and Malis (1956) in a similar study found that the antero-posterior diameter at the The routinely taken lateral radiograph ofthecervicalspine first cervical vertebra varied 16 to be examined is placed on a horizontally positioned from mm. to more viewing box. A piece of blank developed x-ray film is than 30 mm. and from C.4 to C.7 varied from 12 mm. then placed over the radiograph. A careful tracing using Protected by copyright. to 22 mm. The average antero-posterior diameter a sharp film-marking pencil is then made. -

Review Laminectomy for Cervical Myelopathy
Spinal Cord (2003) 41, 317–327 & 2003 International Spinal Cord Society All rights reserved 1362-4393/03 $25.00 www.nature.com/sc Review Laminectomy for cervical myelopathy NE Epstein*,1,2,3,4 1The Albert Einstein College of Medicine, Bronx, NY, USA; 2The North Shore-Long Island Jewish Health System, Manhasset, NY, USA; 3New Hyde Park, NY, USA; 4Winthrop University Hospital, Mineola, NY, USA Study design: Cervical laminectomy with or without fusion, or laminoplasty, successfully address congenital or acquired stenosis, multilevel spondylosis, ossification of the posterior longitudinal ligament (OPLL), and ossification of the yellow ligament (OYL). To optimize surgical results, however, these procedures should be applied to carefully selected patients. Objectives: To determine the clinical, neurodiagnostic, appropriate posterior cervical approaches to be employed in patients presenting with MR- and CT-documented multilevel cervical disease. To limit perioperative morbidity, dorsal decompressions with or without fusions should be performed utilizing awake intubation and positioning and continuous intraoperative somatosensory- evoked potential monitoring. Setting: United States of America. Methods: The clinical, neurodiagnostic, and varied dorsal decompressive techniques employed to address pathology are reviewed. Techniques, including laminectomy, laminoforaminotomy, and laminoplasty are described. Where preoperative dynamic X-rays document instability, simultaneous fusions employing wiring or lateral mass plate/screw or rod/screw techniques may be employed. Nevertheless, careful patient selection remains one of the most critical factors to operative success as older individuals with prohibitive comorbidities or fixed long-term neurological deficits should not undergo these procedures. Results: Short- and long-term outcomes following dorsal decompressions with or without fusions vary. Those with myelopathy over 65 years of age often do well in the short-term, but demonstrate greater long-term deterioration. -

Spinal Stenosis.Pdf
Spinal Stenosis Overview Spinal stenosis is the narrowing of your spinal canal and nerve root canal along with the enlargement of your facet joints. Most commonly it is caused by osteoarthritis and your body's natural aging process, but it can also develop from injury or previous surgery. As the spinal canal narrows, there is less room for your nerves to branch out and move freely. As a result, they may become swollen and inflamed, which can cause pain, cramping, numbness or weakness in your legs, back, neck, or arms. Mild to moderate symptoms can be relieved with medications, physical therapy and spinal injections. Severe symptoms may require surgery. Anatomy of the spinal canal To understand spinal stenosis, it is helpful to understand how your spine works. Your spine is made of 24 moveable bones called vertebrae. The vertebrae are separated by discs, which act as shock absorbers preventing the vertebrae from rubbing together. Down the middle of each vertebra is a hollow space called the spinal canal that contains the spinal cord, spinal nerves, ligaments, fat, and blood vessels. Spinal nerves exit the spinal canal through the intervertebral foramen (also called the nerve root canal) to branch out to your body. Both the spinal and nerve root canals are surrounded by bone and ligaments. Bony changes can narrow the canals and restrict the spinal cord or nerves (see Anatomy of the Spine). What is spinal stenosis? Spinal stenosis is a degenerative condition that happens gradually over time and refers to: • narrowing of the spinal and nerve root canals • enlargement of the facet joints • stiffening of the ligaments • overgrowth of bone and bone spurs (Figure 1) Figure 1. -

Ultrasonographic Evaluation of the Sacrococcyx and Spinal Canal In
http:// ijp.mums.ac.ir Original Arti cle (Pages: 6267-6274) Ultrasonographic Evaluation of the Sacrococcyx and Spinal Canal in Children with Constipation Seyed Ali Alamdaran1, Mohammad Taghi Pourhoseini1, Seyed Ali Jafari2, Reza Shojaeian3, 1Ali Feyzi1, *Masoud Pezeshki Rad 1, 4 1 Department of Radiology, Faculty of Medicine, Mashhad University of Medical Sciences, Mashhad, Iran. 2 Department of Pediatrics, Faculty of Medicine, Mashhad University of Medical Sciences, Mashhad, Iran. 3 Department of Pediatric Surgery, Faculty of Medicine, Mashhad University of Medical Sciences, Mashhad, Iran. 4 Surgical Oncology Research Center, Mashhad University of Medical Sciences, Mashhad, Iran. Abstract Background The occult neurological disorders are an important cause of constipation in children. This study aimed to evaluate the spinal canal and lumbosacral by ultrasound in pediatric constipation to better identifying neurological causes of constipation. Materials and Methods In this case-control study, 100 children with constipation (age range 1 to 14 years) without previously known chronic illness referred to the Radiology Department of the Mashhad Pediatric Dr. Sheikh Hospital were selected. After recording clinical data, the patients were undergone sacral and spinal cord ultrasound examinations and the results were compared with the control group (healthy children with transient illness (otherwise constipation or urinary disorders) who had referred to radiology department for sonographic examination). Results The mean age of patients was 6 ± 3.3 years old. The tethered cord and occult intrasacral meningocele were observed in 2% of patients group. Spina bifida was found in 64% patients, and 31% control subjects with significant difference (P = 0.009). About one third of cases with spina bifida were found in lumbar L5 vertebra, and another two third were in high sacral vertebrae (S1 or S2). -

C1 Stenosis – an Easily Missed Cause for Cervical Myelopathy
Neurospine 2019;16(3):456-461. Neurospine https://doi.org/10.14245/ns.1938200.100 pISSN 2586-6583 eISSN 2586-6591 Review Article C1 Stenosis – An Easily Missed Cause Corresponding Author for Cervical Myelopathy Andrei Fernandes Joaquim 1 2 3 2 https://orcid.org/0000-0003-2645-0483 Andrei Fernandes Joaquim , Griffin Baum , Lee A. Tan , K. Daniel Riew 1Neurosurgery Division, Department of Neurology, State University of Campinas (UNICAMP), Campinas-SP, Neurosurgery Division, Department of Brazil Neurology, State University of Campinas 2Department of Orthopedic Surgery, Columbia University, New York, NY, USA 3 (UNICAMP), Campinas, Brazil Department of Neurosurgery, University of California San Francisco, San Francisco, CA, USA E-mail: [email protected] Received: June 13, 2019 C1 stenosis is often an easily missed cause for cervical myelopathy. The vast majority of cer- Revised: July 16, 2019 vical myelopathy occurs in the subaxial cervical spine. The cervical canal is generally largest Accepted: July 17, 2019 at C1/2, explaining the relatively rare incidence of neurological deficits in patients with odon- toid fractures. However, some subjects have anatomical anomalies of the atlas, which may cause stenosis and result in clinical symptoms similar to subaxial cord compression. Isolat- ed pure atlas hypoplasia leading to stenosis is quite rare and may be associated with other This is an Open Access article distributed under anomalies, such as atlas clefts or transverse ligament calcification. It may also be more com- the terms of the Creative Commons Attribution monly associated with syndromic conditions such as Down or Turner syndrome. Although Non-Commercial License (http://creativecom- mons.org/licenses/by-nc/4.0/) which permits the diagnosis can be easily made with a cervical magnetic resonance imaging, the C3/2 spi- unrestricted non-commercial use, distribution, nolaminar test using a lateral cervical plain radiograph is a useful and sensitive tool for screen- and reproduction in any medium, provided the ing.