Implications of New Understandings of Gliomas in Children and Adults with NF1: Report of a Consensus Conference
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Central Nervous System Tumors General ~1% of Tumors in Adults, but ~25% of Malignancies in Children (Only 2Nd to Leukemia)
Last updated: 3/4/2021 Prepared by Kurt Schaberg Central Nervous System Tumors General ~1% of tumors in adults, but ~25% of malignancies in children (only 2nd to leukemia). Significant increase in incidence in primary brain tumors in elderly. Metastases to the brain far outnumber primary CNS tumors→ multiple cerebral tumors. One can develop a very good DDX by just location, age, and imaging. Differential Diagnosis by clinical information: Location Pediatric/Young Adult Older Adult Cerebral/ Ganglioglioma, DNET, PXA, Glioblastoma Multiforme (GBM) Supratentorial Ependymoma, AT/RT Infiltrating Astrocytoma (grades II-III), CNS Embryonal Neoplasms Oligodendroglioma, Metastases, Lymphoma, Infection Cerebellar/ PA, Medulloblastoma, Ependymoma, Metastases, Hemangioblastoma, Infratentorial/ Choroid plexus papilloma, AT/RT Choroid plexus papilloma, Subependymoma Fourth ventricle Brainstem PA, DMG Astrocytoma, Glioblastoma, DMG, Metastases Spinal cord Ependymoma, PA, DMG, MPE, Drop Ependymoma, Astrocytoma, DMG, MPE (filum), (intramedullary) metastases Paraganglioma (filum), Spinal cord Meningioma, Schwannoma, Schwannoma, Meningioma, (extramedullary) Metastases, Melanocytoma/melanoma Melanocytoma/melanoma, MPNST Spinal cord Bone tumor, Meningioma, Abscess, Herniated disk, Lymphoma, Abscess, (extradural) Vascular malformation, Metastases, Extra-axial/Dural/ Leukemia/lymphoma, Ewing Sarcoma, Meningioma, SFT, Metastases, Lymphoma, Leptomeningeal Rhabdomyosarcoma, Disseminated medulloblastoma, DLGNT, Sellar/infundibular Pituitary adenoma, Pituitary adenoma, -

Cerebellar Anaplastic Astrocytoma in Adult Patients: 15 Consecutive Cases from a Single Institution and Literature Review
medRxiv preprint doi: https://doi.org/10.1101/2020.09.09.20188938; this version posted September 14, 2020. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted medRxiv a license to display the preprint in perpetuity. All rights reserved. No reuse allowed without permission. Cerebellar anaplastic astrocytoma in adult patients: 15 consecutive cases from a single institution and literature review Artem Belyaev1, Dmitry Usachev1, Marina Ryzhova1, Gleb Gulida1, Vasilisa Skvortsova2,3, Igor Pronin1, Grigory Kobiakov1. 1 Burdenko Neurosurgery Center, 4th Tverskaya-Yamskaya, 16, Moscow, 125047, Russia 2 Wellcome Trust Centre for Neuroimaging, University College London, London, United Kingdom; 3 Max Planck University College London Centre for Computational Psychiatry and Ageing Research, London, United Kingdom; Abstract: Adult cerebellar anaplastic astrocytomas (cAA) are rare entities and their clinical and genetic appearances are still ill defined. Previously, malignant gliomas of the cerebellum were combined and reviewed together (cAA and cerebellar glioblastomas (cGB), that could have possibly affected overall results. We present characteristics of 15 adult patients with cAA and compared them to a series of 45 patients with a supratentorial AA (sAA). The mean age at cAA diagnosis was 39.3 years (range 19-72). A history of neurofibromatosis type I was noted in 1 patient (6.7%). An IDH-1 mutation was identified in 6/15 cases and a methylated MGMT promoter in 5/15 cases. Patients in study and control groups were matched in age, sex and IDH- 1 mutation status. Patients in a study group tended to have a more frequent multifocal presentation at diagnosis (13% vs. -
A Case of Intramedullary Spinal Cord Astrocytoma Associated with Neurofibromatosis Type 1
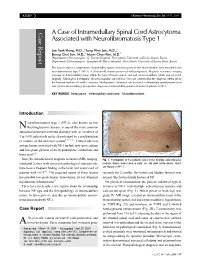
KISEP J Korean Neurosurg Soc 36 : 69-71, 2004 Case Report A Case of Intramedullary Spinal Cord Astrocytoma Associated with Neurofibromatosis Type 1 Jae Taek Hong, M.D.,1 Sang Won Lee, M.D.,1 Byung Chul Son, M.D.,1 Moon Chan Kim, M.D.2 Department of Neurosurgery,1 St. Vincent Hospital, The Catholic University of Korea, Suwon, Korea Department of Neurosurgery,2 Kangnam St. Mary's Hospital, The Catholic University of Korea, Seoul, Korea The authors report a symptomatic intramedullary spinal cord astrocytoma in the thoracolumbar area associated with neurofibromatosis type 1 (NF-1). A 38-year-old woman presented with paraparesis. Magnetic resonance imaging revealed an intramedullary lesion within the lower thoracic spinal cord and conus medullaris, which was removed surgically. Pathological investigation showed anaplastic astrocytoma. This case confirms that the diagnosis criteria set by the National Institute of Health Consensus Development Conference can be useful to differentiate ependymoma from astrocytoma when making a preoperative diagnosis of intramedullary spinal cord tumor in patients of NF-1. KEY WORDS : Astrocytoma·Intramedullary cord tumor·Neurofibromatosis. Introduction eurofibromatosis type 1 (NF-1), also known as von N Recklinghausen's disease, is one of the most common autosomal dominant inherited disorders with an incidence of 1 in 3,000 individuals and is characterized by a predisposition to tumors of the nervous system5,6,12,16). Central nervous system lesions associated with NF-1 include optic nerve glioma and low-grade gliomas of the hypothalamus, cerebellum and brain stem6,10). Since the introduction of magnetic resonance(MR) imaging, Fig. 1. Photograph of the patient's back shows multiple subcutaneous incidental lesions with uncertain pathological characteristic nodules (black arrow) and a cafe-au-lait spot (white arrow), which have been a frequent finding in the brain and spinal cord of are typical of NF-1. -

Astrocytoma: a Hormone-Sensitive Tumor?
International Journal of Molecular Sciences Review Astrocytoma: A Hormone-Sensitive Tumor? Alex Hirtz 1, Fabien Rech 1,2,Hélène Dubois-Pot-Schneider 1 and Hélène Dumond 1,* 1 Université de Lorraine, CNRS, CRAN, F-54000 Nancy, France; [email protected] (A.H.); [email protected] (F.R.); [email protected] (H.D.-P.-S.) 2 Université de Lorraine, CHRU-Nancy, Service de Neurochirurgie, F-54000 Nancy, France * Correspondence: [email protected]; Tel.: +33-372746115 Received: 29 October 2020; Accepted: 27 November 2020; Published: 30 November 2020 Abstract: Astrocytomas and, in particular, their most severe form, glioblastoma, are the most aggressive primary brain tumors and those with the poorest vital prognosis. Standard treatment only slightly improves patient survival. Therefore, new therapies are needed. Very few risk factors have been clearly identified but many epidemiological studies have reported a higher incidence in men than women with a sex ratio of 1:4. Based on these observations, it has been proposed that the neurosteroids and especially the estrogens found in higher concentrations in women’s brains could, in part, explain this difference. Estrogens can bind to nuclear or membrane receptors and potentially stimulate many different interconnected signaling pathways. The study of these receptors is even more complex since many isoforms are produced from each estrogen receptor encoding gene through alternative promoter usage or splicing, with each of them potentially having a specific role in the cell. The purpose of this review is to discuss recent data supporting the involvement of steroids during gliomagenesis and to focus on the potential neuroprotective role as well as the mechanisms of action of estrogens in gliomas. -

Epidemiology and Survival of Patients with Brainstem Gliomas: a Population-Based Study Using the SEER Database
ORIGINAL RESEARCH published: 11 June 2021 doi: 10.3389/fonc.2021.692097 Epidemiology and Survival of Patients With Brainstem Gliomas: A Population-Based Study Using the SEER Database † † Huanbing Liu 1 , Xiaowei Qin 1 , Liyan Zhao 2, Gang Zhao 1* and Yubo Wang 1* 1 Department of Neurosurgery, First Hospital of Jilin University, Changchun, China, 2 Department of Clinical Laboratory, Second Hospital of Jilin University, Changchun, China Background: Brainstem glioma is a primary glial tumor that arises from the midbrain, Edited by: pons, and medulla. The objective of this study was to determine the population-based Yaohua Liu, epidemiology, incidence, and outcomes of brainstem gliomas. Shanghai First People’s Hospital, China Methods: The data pertaining to patients with brainstem gliomas diagnosed between Reviewed by: 2004 and 2016 were extracted from the SEER database. Descriptive analyses were Kristin Schroeder, conducted to evaluate the distribution and tumor-related characteristics of patients with Duke Cancer Institute, United States Gerardo Caruso, brainstem gliomas. The possible prognostic indicators were analyzed by Kaplan-Meier University Hospital of Policlinico G. curves and a Cox proportional hazards model. Martino, Italy *Correspondence: Results: The age-adjusted incidence rate was 0.311 cases per 100,000 person-years Gang Zhao between 2004 and 2016. A total of 3387 cases of brainstem gliomas were included in our [email protected] study. Most of the patients were white and diagnosed at 5-9 years of age. The most Yubo Wang [email protected] common diagnosis confirmed by histological review was ependymoma/anaplastic †These authors have contributed ependymoma. The median survival time was 24 months. -

Malignant CNS Solid Tumor Rules
Malignant CNS and Peripheral Nerves Equivalent Terms and Definitions C470-C479, C700, C701, C709, C710-C719, C720-C725, C728, C729, C751-C753 (Excludes lymphoma and leukemia M9590 – M9992 and Kaposi sarcoma M9140) Introduction Note 1: This section includes the following primary sites: Peripheral nerves C470-C479; cerebral meninges C700; spinal meninges C701; meninges NOS C709; brain C710-C719; spinal cord C720; cauda equina C721; olfactory nerve C722; optic nerve C723; acoustic nerve C724; cranial nerve NOS C725; overlapping lesion of brain and central nervous system C728; nervous system NOS C729; pituitary gland C751; craniopharyngeal duct C752; pineal gland C753. Note 2: Non-malignant intracranial and CNS tumors have a separate set of rules. Note 3: 2007 MPH Rules and 2018 Solid Tumor Rules are used based on date of diagnosis. • Tumors diagnosed 01/01/2007 through 12/31/2017: Use 2007 MPH Rules • Tumors diagnosed 01/01/2018 and later: Use 2018 Solid Tumor Rules • The original tumor diagnosed before 1/1/2018 and a subsequent tumor diagnosed 1/1/2018 or later in the same primary site: Use the 2018 Solid Tumor Rules. Note 4: There must be a histologic, cytologic, radiographic, or clinical diagnosis of a malignant neoplasm /3. Note 5: Tumors from a number of primary sites metastasize to the brain. Do not use these rules for tumors described as metastases; report metastatic tumors using the rules for that primary site. Note 6: Pilocytic astrocytoma/juvenile pilocytic astrocytoma is reportable in North America as a malignant neoplasm 9421/3. • See the Non-malignant CNS Rules when the primary site is optic nerve and the diagnosis is either optic glioma or pilocytic astrocytoma. -

Rehabilitation of Adult Patients with Primary Brain Tumors: a Narrative Review
brain sciences Review Rehabilitation of Adult Patients with Primary Brain Tumors: A Narrative Review Parth Thakkar 1, Brian D. Greenwald 2,* and Palak Patel 1 1 Rutgers Robert Wood Johnson Medical School, Piscataway, NJ 08854, USA; [email protected] (P.T.); [email protected] (P.P.) 2 JFK Johnson Rehabilitation Institute, Edison, NJ 08820, USA * Correspondence: [email protected] Received: 22 May 2020; Accepted: 25 July 2020; Published: 29 July 2020 Abstract: Rehabilitative measures have been shown to benefit patients with primary brain tumors (PBT). To provide a high quality of care, clinicians should be aware of common challenges in this population including a variety of medical complications, symptoms, and impairments, such as headaches, seizures, cognitive deficits, fatigue, and mood changes. By taking communication and family training into consideration, clinicians can provide integrated and patient-centered care to this population. This article looks to review the current literature in outpatient and inpatient rehabilitation options for adult patients with PBTs as well as explore the role of the interdisciplinary team in providing survivorship care. Keywords: primary brain tumor; neuro-oncology; brain cancer; rehabilitation 1. Introduction About 80,000 people in the United States are diagnosed with a primary brain tumor (PBT) every year [1]. PBTs vary widely in their clinical presentations and can carry devastating prognoses for patients. The average survival rate for patients with malignant brain tumors is 35%, and the five-year survival rate for glioblastoma multiforme, the most common form of primary malignant brain tumor in adults, is 5.6%. There are an estimated 700,000 Americans living with a PBT, of which approximately 70% are benign and 30% are malignant [2]. -

Information Sheet 4: High-Grade Glioma Brain Tumours and Treatment Options
Information Sheet 4: High-Grade Glioma brain tumours and treatment options This information document on high grade brain tumours simply provides a basis for discussion with the healthcare professionals with whom you are in contact. It should not in any way be used as a substitute for professional care. What is a Glioma? There are nearly 100 different types of brain tumours. Most primary brain tumours develop from the cells that support the nerve cells of the brain. These are called glial cells. So a tumour of glial cells is given the collective name of a glioma. About half of all primary brain tumours are gliomas. Low-grade or high-grade? Brain tumours are put into groups according to how fast they are likely to grow. There are four groups, called Grades 1–4. The cells are examined under a microscope, and the more normal they look, the more slowly the brain tumour is likely to develop and the lower the grade. The more abnormal the cells look, the more quickly the brain tumour is likely to grow and the higher the grade. You may have been told you have a benign tumour or a malignant tumour. Low-grade tumours are generally regarded as benign and high-grade as malignant. Malignant So, generally speaking, malignant means that: The tumour is relatively fast growing It may come back after surgery, even if completely removed It may spread to other parts of the brain or spinal cord It cannot just be treated with surgery and will need further treatments, such as radiotherapy or chemotherapy, to try to stop it from returning. -

Primary Intracranial Neoplasms in Man Comprise from 2 to 5 Per Cent of All Tumors in the Body
THE AMERICAN JOURNAL OF PATHOLOGY VOLUME XXXI JANUARY-FEBRUARY, I955 NUMBER x THE NATURE OF GLIOMAS AS REVEALED BY ANIMAL EXPERIMENTATION * H. M. ZnMMERMAN, M.D. From the Laboratory Division, Montej ore Hospital, New York 67, N.Y. Primary intracranial neoplasms in man comprise from 2 to 5 per cent of all tumors in the body. Of these neoplasms, somewhat less than half belong to the glioma group. The latter comprises at least seven universally recognized, distinctive types as well as a number of related subtypes. The major types are: astrocytoma, astroblas- toma, ependymoma, gioblastoma multiforme, medulloblastoma, oligo- dendroglioma, and spongioblastoma polare. To the subtypes belong, among others, the ependymoblastomas, ganglioneuromas, and me- dullo-epitheliomas. The problem of identification and classification of tumors of the glioma variety has not been simple, mainly for two reasons. One is that neurosurgical pathology is still in that early developmental stage which is preoccupied with descriptive morphology and with finding new tumor types to classify. Thus it is still considered somewhat of an achievement to have divided the astrocytoma into the piloid, fibril- lary, and protoplasmic types, even though the histogenesis and biologic behavior of this tumor does not seem to warrant such subclassification. The other is that a vastly complicated terminology has developed which has greatly discouraged students in this field. The concept is also current that a battery of complicated and difficult staining techniques is essential for the identification of the various gliomas. The general pathologist has shunned the field of neurosurgical pathology because of his belief in the almost insurmountable complexity of the intra- cranial neoplasms. -

Clinical Applications of PET in Brain Tumors*
CONTINUING EDUCATION Clinical Applications of PET in Brain Tumors* Wei Chen Department of Molecular and Medical Pharmacology, David Geffen School of Medicine, UCLA, Los Angeles, California; and Department of Radiology, Kaiser Permanente Woodland Hills Medical Center, Woodland Hills, California PET-guided biopsy. The article discusses the clinical course Malignant gliomas and metastatic tumors are the most common and treatment of the tumors; clinical issues pertinent to brain tumors. Neuroimaging plays a significant role clinically. In neuroimaging; the benefits and limitations of the current low-grade tumors, neuroimaging is needed to evaluate recurrent gold standard, MRI; the role of the established PET tracer disease and to monitor anaplastic transformation into high-grade 18F-FDG; and the potential of PET tracers alternative to tumors. In high-grade and metastatic tumors, the imaging chal- 18 18 lenge is to distinguish between recurrent tumor and treatment- F-FDG, such as amino acid tracers, with emphasis on F- induced changes such as radiation necrosis. The current clinical labeled amino acid tracers. gold standard, MRI, provides superior structural detail but poor specificity in identifying viable tumors in brain treated with sur- EPIDEMIOLOGY AND CLASSIFICATION OF GLIOMAS 18 gery, radiation, or chemotherapy. F-FDG PET identifies ana- According to the classification of the World Health Orga- plastic transformation and has prognostic value. The sensitivity nization (WHO), gliomas are of 3 main types—astrocytomas, and specificity of 18F-FDG in evaluating recurrent tumor and treatment-induced changes can be improved significantly by oligodendrogliomas, and mixed oligoastrocytomas—which coregistration with MRI and potentially by delayed imaging 3–8 can usually be distinguished by their histologic features (2). -

Involvement of the Olfactory Apparatus by Gliomas
CLINICAL REPORT HEAD & NECK Involvement of the Olfactory Apparatus by Gliomas X. Wu, Y. Li, C.M. Glastonbury, and S. Cha ABSTRACT SUMMARY: The olfactory bulbs and tracts are central nervous system white matter tracts maintained by central neuroglia. Although rare, gliomas can originate from and progress to involve the olfactory apparatus. Through a Health Insurance Portability and Accountability Act–compliant retrospective review of the institutional teaching files and brain MR imaging reports spanning 10 years, we identified 12 cases of gliomas involving the olfactory bulbs and tracts, including 6 cases of glioblastoma, 2 cases of ana- plastic oligodendroglioma, and 1 case each of pilocytic astrocytoma, diffuse (grade II) astrocytoma, anaplastic astrocytoma (grade III), and diffuse midline glioma. All except the pilocytic astrocytoma occurred in patients with known primary glial tumors else- where. Imaging findings of olfactory tumor involvement ranged from well-demarcated enhancing masses to ill-defined enhancing infiltrative lesions to nonenhancing masslike FLAIR signal abnormality within the olfactory tracts. Familiarity with the imaging find- ings of glioma involvement of the olfactory nerves is important for timely diagnosis and treatment of recurrent gliomas and to dis- tinguish them from other disease processes. ABBREVIATIONS: GBM ¼ glioblastoma multiforme; TMZ ¼ temozolomide; EGFR ¼ epidermal growth factor receptor; IDH1 ¼ Isocitrate dehydrogenase 1; MGMT ¼ O6-methylguanine methyltransferase he olfactory bulbs and tracts are central nervous system white bulbs and tracts and to differentiate them from other masses of Tmatter tracts extending directly to the cerebrum, maintained the anterior cranial fossa. by a combination of specialized olfactory ensheathing cells and central neuroglia, including astrocytes and oligodendrocytes.1 As Case Series a result, gliomas can rarely originate from and progress to involve – the olfactory apparatus. -

Sudden Death Due to Primary Intracranial Neoplasms. a Forensic Autopsy Study
ANTICANCER RESEARCH 26: 2463-2466 (2006) Sudden Death due to Primary Intracranial Neoplasms. A Forensic Autopsy Study THEODORE VOUGIOUKLAKIS1, ANTIGONY MITSELOU1 and NIKI J. AGNANTIS2 Departments of 1Forensic Pathology and 2Pathology, Medical School, University of Ioannina, Ioannina, Greece Abstract. Although most fatal tumors are diagnosed well young adults aged 20 to 39 years, representing the third before a patient’s death, occasionally forensic pathologists leading cancer-related death in the past two decades (6). encounter cases in which the presence of a primary tumor of As a result of increasingly widespread access to modern the central nervous system had not been suspected prior to and sensitive imaging technology, such as computed death. A search for cases of sudden death due to intracranial tomography (CT) and magnetic resonance imaging, sudden tumors from a total of 1985 autopsies from the archives of the death due to undiagnosed intracranial neoplasms probably Department of Forensic Pathology, University of Ioannina, accounts for fewer cases in forensic autopsy series (6, 7). In Greece, in the period 1998-2005, was undertaken. Two such this article, two patients, whose sudden demise could be cases in which a medico-legal autopsy had disclosed brain directly attributed to the effects of a previously augmented tumors were found. The first case was a 34-year-old man who intracranial pressure due to acute and severe hemorrhage had been found unconscious in bed, and died a few hours after of a brain tumor, comprising a glioblastoma grade WHO- hospitalization. His autopsy had revealed a 7-cm glioblastoma IV and an astrocytoma grade WHO-III respectively, are at the level of the third ventricle.