Hemophagocytic Lymphohistiocytosis Gene Sequencing Panel
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Genome-Wide Rnai Screens Identify Genes Required for Ricin and PE Intoxications
Developmental Cell Article Genome-Wide RNAi Screens Identify Genes Required for Ricin and PE Intoxications Dimitri Moreau,1 Pankaj Kumar,1 Shyi Chyi Wang,1 Alexandre Chaumet,1 Shin Yi Chew,1 He´ le` ne Chevalley,1 and Fre´ de´ ric Bard1,* 1Institute of Molecular and Cell Biology, 61 Biopolis Drive, Proteos, Singapore 138673, Singapore *Correspondence: [email protected] DOI 10.1016/j.devcel.2011.06.014 SUMMARY In the lumen of the ER, these toxins are thought to interact with elements of the ER-associated degradation (ERAD) pathway, Protein toxins such as Ricin and Pseudomonas which targets misfolded proteins in the ER for degradation. exotoxin (PE) pose major public health challenges. This interaction is proposed to allow translocation to the cytosol Both toxins depend on host cell machinery for inter- without resulting in toxin degradation (Johannes and Ro¨ mer, nalization, retrograde trafficking from endosomes 2010). to the ER, and translocation to cytosol. Although Obviously, this complex set of membrane-trafficking and both toxins follow a similar intracellular route, it is membrane-translocation events involves many host proteins, some of which have already been described (Johannes and unknown how much they rely on the same genes. Ro¨ mer, 2010; Sandvig et al., 2010). Altering the function of these Here we conducted two genome-wide RNAi screens host proteins could in theory provide a toxin antidote. identifying genes required for intoxication and Consistently, inhibition of retrograde traffic by drugs such as demonstrating that requirements are strikingly Brefeldin A (Sandvig et al., 1991)(Yoshida et al., 1991) or Golgi- different between PE and Ricin, with only 13% over- cide A (Sa´ enz et al., 2009) and Retro-1 and 2 (Stechmann et al., lap. -

Non-EBV-Related Aggressive NK-Cell Leukemia: an Oncohematological Great Imitator
Case Report J Hematol. 2018;7(4):163-166 Non-EBV-Related Aggressive NK-Cell Leukemia: An Oncohematological Great Imitator Jose L. Lepe-Zunigaa, b, f, Francisco Javier Jeronimo-Lopeza, c, Jorge Gregorio Hernandez-Orantesa, d, Adriana Osiris Mendez-Cigarroaa, e Abstract Introduction Aggressive natural killer (NK)-cell leukemia (ANKL) is a very rare Ever since the expression “great imitator” was coined to re- oncohematological disease among youngsters in Latin America. Its fer to syphilis [1] and later to tuberculosis [2], the term has clinical picture imitates a variety of syndromes and diseases due to its been applied to several diseases that mimic others, making the pathophysiology. Its diagnosis is relatively simple due to the promi- real diagnosis more difficult. Pituitary apoplexy [3], cardiac nence of NK malignant cells in peripheral blood and its clinical ag- myxoma [4], lyme disease [5] and infectious mononucleosis gressiveness. In certain circumstances though, the presence of blast [6] have been so considered. In more recent times, the pre- NK cells and the natural course of the disease can be so modified by ferred great imitator has been lupus, because its clinical picture the treatment of one of the imitated diseases, especially when using can vary from predominantly hematological, to renal, hepatic, steroids, that it becomes very difficult to diagnose early in its course. neurological or dermatological in nature, challenging the cli- We present a case of a 16-year-old Mexican male who initiated symp- nician before the disease -

Immune Thrombocytopenic Purpura As Sole Manifestation And
Case Report / Olgu Sunumu DOI: 10.5578/ced.57487 • (J Pediatr Inf 2017; 11: i35-i38) Immune Thrombocytopenic Purpura As Sole Manifestation and Hemophagocytic Lypmhohistiocytosis As Sole Manifestation of Hepatitis a Virus Infection in Two Children* İmmün Trombositopenik Purpuranın Tek Bulgu Olduğu ve Hemofagositik Lenfohistiositozun Tek Bulgu Olduğu İki Çocuk Olguda Hepatit A Virüs Enfeksiyonu Zümrüt Şahbudak Bal1, Semra Şen1, Nihal Karadaş Özdemir2, Katibe Başak Yıldız1, Deniz Yılmaz Karapınar2, Fadıl Vardar1 1 Department of Pediatric Infectious Diseases, Ege University School of Medicine, Izmir, Turkey 2 Department of Hematology, Ege University School of Medicine, Izmir, Turkey * This case report was poster presented at ESPID Congress. Abstract Özet Hepatitis A virus (HAV) infection is often asymptomatic or mildly Hepatit A virüs (HAV) enfeksiyonu çocukluk çağında genellikle symptomatic in pediatric population, the severity of the disease asemptomatik ya da hafif seyirlidir, yaş arttıkça hastalığın ciddiyeti artar. increases by age. Immune-mediated extrahepatic extrahepatic Ekstrahepatik immün-aracılı bulgular ve hematolojik komplikasyonlar manifestations and hematologic complications are mainly reported genellikle yetişkinlerde, akut ve kronik hepatit B ve C enfeksiyonlarının in adults with acute and chronic hepatitis B and C. However, they are seyrinde bildirilmiştir. Çocukluk çağında oldukça nadirdir. İngilizce relatively rare in children with HAV infection. There are few available literatürde, çocuklarda hepatit A’nın otoimmün komplikasyonlarını -

Regular Article
From www.bloodjournal.org by guest on April 6, 2015. For personal use only. Regular Article IMMUNOBIOLOGY Hemophagocytic lymphohistiocytosis caused by dominant-negative mutations in STXBP2 that inhibit SNARE-mediated membrane fusion Waldo A. Spessott,1 Maria L. Sanmillan,1 Margaret E. McCormick,1 Nishant Patel,2 Joyce Villanueva,3 Kejian Zhang,4 Kim E. Nichols,5 and Claudio G. Giraudo1 1Department of Pathology and Laboratory Medicine, and 2Division of Oncology, Department of Pediatrics, The Children’s Hospital of Philadelphia, University of Pennsylvania, Philadelphia, PA; 3Division of Bone Marrow Transplant and Immune Deficiency, and 4Division of Human Genetics, Cincinnati Children’s Hospital Medical Center, Department of Pediatrics, University of Cincinnati College of Medicine, Cincinnati, OH; and 5Division of Cancer Predisposition, Department of Oncology, St. Jude Children’s Research Hospital, Memphis, TN Key Points Familial hemophagocytic lymphohistiocytosis (F-HLH) and Griscelli syndrome type 2 (GS) are life-threatening immunodeficiencies characterized by impaired cytotoxic T lymphocyte • Monoallelic STXBP2 mutations (CTL) and natural killer (NK) cell lytic activity. In the majority of cases, these disorders are affecting codon 65 impair caused by biallelic inactivating germline mutations in genes such as RAB27A (GS) and PRF1, lymphocyte cytotoxicity and UNC13D, STX11,andSTXBP2 (F-HLH). Although monoallelic (ie, heterozygous) mutations contribute to hemophagocytic have been identified in certain patients, the clinical significance and molecular mechanisms lymphohistiocytosis. by which these mutations influence CTL and NK cell function remain poorly understood. • Munc18-2R65Q/W mutant Here, we characterize 2 novel monoallelic hemophagocytic lymphohistiocytosis (HLH)- associated mutations affecting codon 65 of STXPB2, the gene encoding Munc18-2, a member proteins function in a dominant- of the SEC/MUNC18 family. -

Clinical Spectrum Ofstx1b-Related Epileptic Disorders
ARTICLE OPEN ACCESS Clinical spectrum of STX1B-related epileptic disorders Stefan Wolking, MD, Patrick May, PhD, Davide Mei, PhD, Rikke S. Møller, PhD, Simona Balestrini, PhD, Correspondence Katherine L. Helbig, MS, Cecilia Desmettre Altuzarra, MD, Nicolas Chatron, PhD, Charu Kaiwar, MD, Dr. Lerche Katharina Stohr,¨ MD, Peter Widdess-Walsh, MB, Bryce A. Mendelsohn, PhD, Adam Numis, MD, holger.lerche@ Maria R. Cilio, PhD, Wim Van Paesschen, MD, Lene L. Svendsen, MD, Stephanie Oates, MD, Elaine Hughes, MD, uni-tuebingen.de Sushma Goyal, MD, Kathleen Brown, MS, Margarita Sifuentes Saenz, MD, Thomas Dorn, MD, Hiltrud Muhle, MD, Alistair T. Pagnamenta, PhD, Dimitris V. Vavoulis, PhD, Samantha J.L. Knight, PhD, Jenny C. Taylor, PhD, Maria Paola Canevini, MD, Francesca Darra, MD, Ralitza H. Gavrilova, MD, Zoe¨ Powis, MS, Shan Tang, PhD, Justus Marquetand, MD, Martin Armstrong, PhD, Duncan McHale, PhD, Eric W. Klee, PhD, Gerhard J. Kluger, MD, Daniel H. Lowenstein, MD, Sarah Weckhuysen, PhD, Deb K. Pal, PhD, Ingo Helbig, MD, Renzo Guerrini, MD, Rhys H. Thomas, PhD, Mark I. Rees, PhD, Gaetan Lesca, PhD, Sanjay M. Sisodiya, PhD, Yvonne G. Weber, MD, Dennis Lal, PhD, Carla Marini, PhD, Holger Lerche, MD, and Julian Schubert, PhD Neurology® 2019;92:e1238-e1249. doi:10.1212/WNL.0000000000007089 Abstract Objective The aim of this study was to expand the spectrum of epilepsy syndromes related to STX1B, encoding the presynaptic protein syntaxin-1B, and establish genotype-phenotype correlations by identifying further disease- related variants. Methods We used next-generation sequencing in the framework of research projects and diagnostic testing. Clinical data and EEGs were reviewed, including already published cases. -
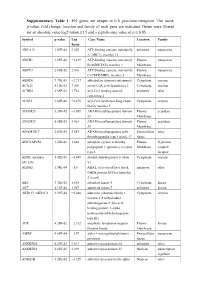
Supplementary Table 1
Supplementary Table 1. 492 genes are unique to 0 h post-heat timepoint. The name, p-value, fold change, location and family of each gene are indicated. Genes were filtered for an absolute value log2 ration 1.5 and a significance value of p ≤ 0.05. Symbol p-value Log Gene Name Location Family Ratio ABCA13 1.87E-02 3.292 ATP-binding cassette, sub-family unknown transporter A (ABC1), member 13 ABCB1 1.93E-02 −1.819 ATP-binding cassette, sub-family Plasma transporter B (MDR/TAP), member 1 Membrane ABCC3 2.83E-02 2.016 ATP-binding cassette, sub-family Plasma transporter C (CFTR/MRP), member 3 Membrane ABHD6 7.79E-03 −2.717 abhydrolase domain containing 6 Cytoplasm enzyme ACAT1 4.10E-02 3.009 acetyl-CoA acetyltransferase 1 Cytoplasm enzyme ACBD4 2.66E-03 1.722 acyl-CoA binding domain unknown other containing 4 ACSL5 1.86E-02 −2.876 acyl-CoA synthetase long-chain Cytoplasm enzyme family member 5 ADAM23 3.33E-02 −3.008 ADAM metallopeptidase domain Plasma peptidase 23 Membrane ADAM29 5.58E-03 3.463 ADAM metallopeptidase domain Plasma peptidase 29 Membrane ADAMTS17 2.67E-04 3.051 ADAM metallopeptidase with Extracellular other thrombospondin type 1 motif, 17 Space ADCYAP1R1 1.20E-02 1.848 adenylate cyclase activating Plasma G-protein polypeptide 1 (pituitary) receptor Membrane coupled type I receptor ADH6 (includes 4.02E-02 −1.845 alcohol dehydrogenase 6 (class Cytoplasm enzyme EG:130) V) AHSA2 1.54E-04 −1.6 AHA1, activator of heat shock unknown other 90kDa protein ATPase homolog 2 (yeast) AK5 3.32E-02 1.658 adenylate kinase 5 Cytoplasm kinase AK7 -

Primary Splenic Histiocytic Sarcoma Complicated with Prolonged
Yamada et al. Diagnostic Pathology 2012, 7:143 http://www.diagnosticpathology.org/content/7/1/143 CASE REPORT Open Access Primary splenic histiocytic sarcoma complicated with prolonged idiopathic thrombocytopenia and secondary bone marrow involvement: a unique surgical case presenting with splenomegaly but non-nodular lesions Sohsuke Yamada1*, Takashi Tasaki11, Naoko Satoh1,2, Atsunori Nabeshima1, Shohei Kitada1,3, Hirotsugu Noguchi1, Kozue Yamada4, Morishige Takeshita4 and Yasuyuki Sasaguri1 Abstract: A 67-year-old Japanese female was followed up due to prolonged idiopathic thrombocytopenia with non-response to steroid therapy for 4 years, but recent progressive pancytopenia, hypo-albuminemia, and hypo-γ-globulinemia were presented. An abdominal CT scan revealed heterogeneously enhanced splenomegaly without any nodular lesions. A splenectomy was performed, and gross examination showed markedly hyperemic red pulp, weighing 760 g, accompanied by multiple foci of peripheral anemic infarction. Surprisingly, microscopic findings exhibited a diffuse proliferation of medium-sized to large tumor cells having pleomorphic nuclei, prominent nucleoli, and abundant eosinophilic cytoplasm, predominantly within the sinuses and cords of the red pulp, which occasionally displayed conspicuous hemophagocytosis and vascular permeation. In immunohistochemistry, these atypical cells were specifically positive for CD68 (KP-1), CD163, and lysozyme, which was consistent with histiocytic sarcoma (HS) of the spleen. Subsequently, section from the aspiration of bone marrow showed infiltration of the neoplastic cells associated with erythrophagocytosis 2 months after the operation, but never before it. Therefore, primary splenic HS presenting with secondary bone marrow involvement was conclusively diagnosed. Since early diagnosis and treatment are necessary for the HS patients with poor outcomes, splenic HS should be considered as a differential diagnosis in cases with chronic thrombocytopenia and splenomegaly. -

Syntaxin Binding Mechanism and Disease-Causing Mutations In
Syntaxin binding mechanism and disease-causing PNAS PLUS mutations in Munc18-2 Yvonne Hackmanna, Stephen C. Grahama,1,2, Stephan Ehlb, Stefan Höningc, Kai Lehmbergd, Maurizio Aricòe, David J. Owena, and Gillian M. Griffithsa,2 aCambridge Institute for Medical Research, University of Cambridge Biomedical Campus, University of Cambridge, Cambridge CB2 0XY, United Kingdom; bCentre of Chronic Immunodeficiency, 79106 Freiburg, Germany; cInstitute for Biochemistry I and Center for Molecular Medicine Cologne, University of Cologne, 50931 Cologne, Germany; dDepartment of Paediatric Haematology and Oncology, University Medical Center Hamburg Eppendorf, 20246 Hamburg, Germany; and ePediatric Hematology Oncology Network, Istituto Toscana Tumori, 50139 Florence, Italy Edited* by Peter Cresswell, Yale University School of Medicine, New Haven, CT, and approved October 11, 2013 (received for review July 18, 2013) Mutations in either syntaxin 11 (Stx11) or Munc18-2 abolish Munc18-2 belongs to the Sec1/Munc18-like (SM) protein cytotoxic T lymphocytes (CTL) and natural killer cell (NK) cytotox- family, whose members are all ∼600 residues long and are in- icity, and give rise to familial hemophagocytic lymphohistiocytosis volved in regulation of SNARE-mediated membrane fusion (FHL4 or FHL5, respectively). Although Munc18-2 is known to events (9, 10). The two closest homologs of Munc18-2 are interact with Stx11, little is known about the molecular mecha- Munc18-1, which is crucial for neurotransmitter secretion in nisms governing the specificity of this interaction or how in vitro neurons (11, 12), and Munc18-3, which is more widely expressed IL-2 activation leads to compensation of CTL and NK cytotoxicity. and is involved in Glut4 translocation (13). -

Secondary Hemophagocytic Lymphohistiocytosis in Post-COVID-19 Patients: a Report of Two Cases
Open Access Case Report DOI: 10.7759/cureus.17328 Secondary Hemophagocytic Lymphohistiocytosis in Post-COVID-19 Patients: A Report of Two Cases Pranjal Kalita 1 , Devina Laishram 1 , Biswajit Dey 1 , Jaya Mishra 1 , Bhupen Barman 2 , Himesh Barman 3 1. Pathology, North Eastern Indira Gandhi Regional Institute of Health and Medical Sciences, Shillong, IND 2. Internal Medicine, North Eastern Indira Gandhi Regional Institute of Health and Medical Sciences, Shillong, IND 3. Paediatrics, North Eastern Indira Gandhi Regional Institute of Health and Medical Sciences, Shillong, IND Corresponding author: Biswajit Dey, [email protected] Abstract Hemophagocytic lymphohistiocytosis (HLH) is a disease that can affect both children and adults. HLH can be categorized as primary or secondary. Secondary HLH (sHLH) may be secondary to various viral infections. Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) virus infection is a pandemic with multi- system involvement. HLH in COVID-19 positive patients is a recognized entity. However, in post-COVID-19 patients who have recovered and are negative by serological tests and reverse transcription-polymerase chain reaction test may present with sHLH due to dysregulation of the immune system. We highlight this unusual finding of post-COVID-19 sHLH in two cases, who were diagnosed by the new revised H-score. Categories: Infectious Disease, Hematology Keywords: covid-19, secondary hemophagocytic lymphohistiocytosis, immune system, sars-cov-2, bone marrow Introduction Hemophagocytic lymphohistiocytosis (HLH) is a lethal disorder of varying etiology and encompasses a wide range of diseases. Familial HLH (FHLH) and immune-related HLH constitute the primary HLH spectrum whereas infections, drug-related and transplantation, malignancies, and macrophage activation syndrome (MAS) constitute the secondary HLH (sHLH) spectrum [1]. -

Mapping Transmembrane Binding Partners for E-Cadherin Ectodomains
SUPPLEMENTARY INFORMATION TITLE: Mapping transmembrane binding partners for E-cadherin ectodomains. AUTHORS: Omer Shafraz 1, Bin Xie 2, Soichiro Yamada 1, Sanjeevi Sivasankar 1, 2, * AFFILIATION: 1 Department of Biomedical Engineering, 2 Biophysics Graduate Group, University of California, Davis, CA 95616. *CORRESPONDING AUTHOR: Sanjeevi Sivasankar, Tel: (530)-754-0840, Email: [email protected] Figure S1: Western blots a. EC-BioID, WT and Ecad-KO cell lysates stained for Ecad and tubulin. b. HRP-streptavidin staining of biotinylated proteins eluted from streptavidin coated magnetic beads incubated with cell lysates of EC-BioID with (+) and without (-) exogenous biotin. c. C-BioID, WT and Ecad-KO cell lysates stained for Ecad and tubulin. d. HRP-streptavidin staining of biotinylated proteins eluted from streptavidin coated magnetic beads incubated with cell lysates of C-BioID with (+) and without (-) exogenous biotin. (+) Biotin (-) Biotin Sample 1 Sample 2 Sample 3 Sample 4 Sample 1 Sample 2 Sample 3 Sample 4 Percent Percent Percent Percent Percent Percent Percent Percent Gene ID Coverage Coverage Coverage Coverage Coverage Coverage Coverage Coverage CDH1 29.6 31.4 41.1 36.5 10.8 6.7 28.8 29.1 DSG2 26 14.6 45 37 0.8 1.9 1.6 18.7 CXADR 30.2 26.2 32.7 27.1 0.0 0.0 0.0 6.9 EFNB1 24.3 30.6 24 30.3 0.0 0.0 0.0 0.0 ITGA2 16.5 22.2 30.1 33.4 1.1 1.1 5.2 7.2 CDH3 21.8 9.7 20.6 25.3 1.3 1.3 0.0 0.0 ITGB1 11.8 16.7 23.9 20.3 0.0 2.9 8.5 5.8 DSC3 9.7 7.5 11.5 13.3 0.0 0.0 2.6 0.0 EPHA2 23.2 31.6 31.6 30.5 0.8 0.0 0.0 5.7 ITGB4 21.8 27.8 33.1 30.7 0.0 1.2 3.9 4.4 ITGB3 23.5 22.2 26.8 24.7 0.0 0.0 5.2 9.1 CDH6 22.8 18.1 28.6 24.3 0.0 0.0 0.0 9.1 CDH17 8.8 12.4 20.7 18.4 0.0 0.0 0.0 0.0 ITGB6 12.7 10.4 14 17.1 0.0 0.0 0.0 1.7 EPHB4 11.4 8.1 14.2 16.3 0.0 0.0 0.0 0.0 ITGB8 5 10 15 17.6 0.0 0.0 0.0 0.0 ITGB5 6.2 9.5 15.2 13.8 0.0 0.0 0.0 0.0 EPHB2 8.5 4.8 9.8 12.1 0.0 0.0 0.0 0.0 CDH24 5.9 7.2 8.3 9 0.0 0.0 0.0 0.0 Table S1: EC-BioID transmembrane protein hits. -

Intravascular Large B-Cell Lymphoma
CLINICAL MEDICINE Intravascular Large B-cell Lymphoma Associated with Systemic and Central Nervous System Hemophagocytic Lymphohistiocytosis: A Case Report Aradhana Verma1; Akanksha Sharma, MD2; Ryan Robetorye, MD3; Alyx Porter, MD2; Talal Hilal, MD4 Perm J 2020;24:19.105 E-pub: 12/06/2019 https://doi.org/10.7812/TPP/19.105 ABSTRACT represents up to one-fourth of second- Introduction: We present a case of an ary HLH cases. Among these, the most Asian variant of intravascular large B-cell common are hematologic malignancies, lymphoma associated with systemic and especially T-cell/natural killer-cell lym- central nervous system hemophagocytic phoma or leukemia. In the Asian variant lymphohistiocytosis (HLH) with multiple of IVLBCL, about 25% of patients can neurologic manifestations. present with a broad range of neurologic Case Presentation: A 68-year-old, symptoms, including seizures, strokes, and previously healthy, Korean woman pre- cognitive deficits that can serve as impor- sented with a 4-week history of fever and tant clues toward the diagnosis.2 IVLBCL weight loss. She had pancytopenia with can prove to be a diagnostic challenge for neutropenia, a ferritin level of 5030 μg/L, clinicians and pathologists if the presenta- and elevated liver enzyme levels. Bone tion is subtle or nonspecific, but it should marrow, liver biopsy specimens, and be considered when a secondary cause of cerebrospinal fluid demonstrated hemo- HLH is not detected. phagocytosis. The patient was treated with the HLH-2004 protocol, but her dis- CASE PRESENTATION Figure 1. Axial cut of fluid-attenuated inversion ease relapsed 3 months later. A repeated Presenting Concerns recovery sequence of the brain magnetic resonance liver biopsy specimen confirmed the imaging demonstrates T2 hyperintensity (arrow) in A 68-year-old Korean woman came to the left occipital region. -

Aggressive NK Cell Leukemia with Hemophagocyticlymphohistiocytosis
ISSN 2572-9578 SciO p Forschene n HUB for Sc i e n t i f i c R e s e a r c h Journal of Clinical and Laboratory Medicine Case Report Volume: 2.2 Open Access Received date: 21 Aug 2017; Accepted date: 19 Aggressive NK Cell Leukemia with Hemophagocytic Sep 2017; Published date: 25 Sep 2017. Lymphohistiocytosis: A Case Report Citation: K Nogi, H Tashiro, K Kawasugi , M Matsuzawa, T Osawa,et al. (2017) Aggressive Kimiko Nogi1, Haruko Tashiro 2, Kazuo Kawasugi 3, Mayumi Matsuzawa1, Takeshi NK Cell Leukemia with Hemophagocytic Osawa1, Ryohei Toyooka1, Taiji Furukawa4 and Naoki Shirafuji2* Lymphohistiocytosis: A Case Report. J Clin Lab Med 2(2): doi http://dx.doi.org/10.16966/2572-9578.116 1Department of Central Laboratory, Teikyo University School of Medicine 2-11-1 Kaga, Itabashi-ku, Tokyo 173-8606, Japan Copyright: © 2017 Nogi K, et al. This is an 2 open-access article distributed under the terms Department of Internal Medicine, Teikyo University School of Medicine 2-11-1 Kaga, Itabashi- of the Creative Commons Attribution License, ku, Tokyo 173-8606, Japan which permits unrestricted use, distribution, and 3Department of Medical Technology, Teikyo University School of Medicine 2-11-1 Kaga, reproduction in any medium, provided the original Itabashi-ku, Tokyo 173-8606, Japan author and source are credited. 4Department of Laboratory Medicine, Teikyo University School of Medicine 2-11-1 Kaga, Itabashi-ku, Tokyo 173-8606, Japan *Corresponding author: Dr. Naoki Shirafuji, Department of Internal Medicine, Teikyo University School of Medicine 2-11-1, Kaga, Itabashi-ku, Tokyo 173-8606 Japan, Tel: +81-3-3964-1211; E-mail: [email protected] Abstract Hemophagocytic lymphohistiocytosis (HLH) is a hyper inflammatory condition caused by a highly stimulated and defective inflammatory response.