Concomitant Gallstone Disease Was Associated with a Worse Prognosis in Non-Cirrhotic Patients with Primary Biliary Cholangitis
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Umbilical Hernia with Cholelithiasis and Hiatal Hernia
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Springer - Publisher Connector Yamanaka et al. Surgical Case Reports (2015) 1:65 DOI 10.1186/s40792-015-0067-8 CASE REPORT Open Access Umbilical hernia with cholelithiasis and hiatal hernia: a clinical entity similar to Saint’striad Takahiro Yamanaka*, Tatsuya Miyazaki, Yuji Kumakura, Hiroaki Honjo, Keigo Hara, Takehiko Yokobori, Makoto Sakai, Makoto Sohda and Hiroyuki Kuwano Abstract We experienced two cases involving the simultaneous presence of cholelithiasis, hiatal hernia, and umbilical hernia. Both patients were female and overweight (body mass index of 25.0–29.9 kg/m2) and had a history of pregnancy and surgical treatment of cholelithiasis. Additionally, both patients had two of the three conditions of Saint’s triad. Based on analysis of the pathogenesis of these two cases, we consider that these four diseases (Saint’s triad and umbilical hernia) are associated with one another. Obesity is a common risk factor for both umbilical hernia and Saint’s triad. Female sex, older age, and a history of pregnancy are common risk factors for umbilical hernia and two of the three conditions of Saint’s triad. Thus, umbilical hernia may readily develop with Saint’s triad. Knowledge of this coincidence is important in the clinical setting. The concomitant occurrence of Saint’s triad and umbilical hernia may be another clinical “tetralogy.” Keywords: Saint’s triad; Cholelithiasis; Hiatal hernia; Umbilical hernia Background of our knowledge, no previous reports have described the Saint’s triad is characterized by the concomitant occur- coexistence of umbilical hernia with any of the three con- rence of cholelithiasis, hiatal hernia, and colonic diverticu- ditions of Saint’s triad. -

Cirrhosis of Liver Is a Risk Factor for Gallstone Disease
International Journal of Research in Medical Sciences Shirole NU et al. Int J Res Med Sci. 2017 May;5(5):2053-2056 www.msjonline.org pISSN 2320-6071 | eISSN 2320-6012 DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20171841 Original Research Article Cirrhosis of liver is a risk factor for gallstone disease Nikhil U. Shirole*, Sudhir J. Gupta, Dharmesh K. Shah, Nitin R. Gaikwad, Tushar H. Sankalecha, Harit G. Kothari Department of Gastroenterology, Government Medical College and Super-speciality Hospital, Nagpur, Maharashtra, India Received: 07 February 2017 Revised: 22 March 2017 Accepted: 24 March 2017 *Correspondence: Dr. Nikhil U. Shirole, E-mail: [email protected] Copyright: © the author(s), publisher and licensee Medip Academy. This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. ABSTRACT Background: Gallstones are common clinical finding in general population. Mean prevalence rate in Indian population is 4-5%. The prevalence of gallstones is found to be high in cirrhotic patients compared to the general population in some western studies. Cause of this increased prevalence however is not known. Aim of the study was to evaluate prevalence of the gall stones in the cirrhotic patients, assess risk factors in cirrhotic patients and clinical presentation. Methods: This is the cross sectional observational study, included cirrhotic patients (compensated or decompensated). Risk factors for gallstone formation (age, gender and diabetes mellitus), characteristics of liver cirrhosis (etiology, Child Turcotte Pugh class, hypersplenism and varices) and clinical presentation were assessed in all cirrhotic patients with gallstones. -

April Is IBS Awareness Month
4/19/2021 Irritable Bowel Syndrome (IBS) in Women: Today’s approach Kathryn Hutchins, MD Assistant Professor University of Nebraska Medical Center Division of Gastroenterology & Hepatology Irritable Bowel Syndrome • No disclosures April is IBS awareness month Objectives Define Irritable Bowel Syndrome (IBS) including its subtypes Describe the current criteria and diagnostic approach for IBS Discuss the management approach to IBS 1 4/19/2021 Clinical Scenarios • 18 y/o female reports longstanding history of GI troubles. She comes to clinic because she is having bouts of diarrhea. Diarrhea is most often when she is nervous or stressed. Diarrhea is more common in the days prior to having her period. Imodium helps to slow the diarrhea • 38 y/o female reports bloating and discomfort most days and especially after eating. She reports having a bowel movement once every 3‐4 days and typically stools are small balls. Bowel movements alleviate bloating. When she travels, she is especially miserable with constipation and bloating. • 41 y/o female with 2 year history of RUQ abdominal pain and frequent loose stools. Gallbladder removed years earlier for different symptoms. Evaluation has included EGD, colonoscopy, endoscopic ultrasound, ERCP x 2 with stent placement and subsequent removal. Countless appointment with evaluations in 3 different states. Irritable Bowel Syndrome defined • IBS is one of the functional gastrointestinal disorders (FGID). Functional bowel disorders (FBD) are FGID of the lower GI tract. • The FGID are also referred to disorder of the brain –gut interaction (DBGI). • IBS is a common of disorders of the brain –gut axis • Chronic symptoms of abdominal pain, bloating, diarrhea, and constipation • No identified structural or lab abnormality to account for recurring symptoms*** Gastroenterology 2020;158:1262–1273 Disorders of the Brain –Gut Interaction Functional Gastrointestinal Disorders Functional Bowel Disorders 2 4/19/2021 How common and who does it affect Clinical visits • 12% of primary care visits. -

Clinical Management of Gastroesophageal Reflux Disease
Osteopathic Family Physician (2011) 3, 58-65 Clinical management of gastroesophageal reflux disease Renata Jarosz, DO,a Thomas G. Zimmerman, DO, FACOFP,b Daniel Van Arsdale, DOc From aStanford Hospital Physical Medicine and Rehabilitation Residency Program, Redwood City, CA, bSouth Nassau Family Medicine, Oceanside, NY, and cSouthampton Hospital, Southampton, NY. KEYWORDS: Gastroesophageal reflux disease (GERD) is a common problem that occurs in both adult and pediatric Gastroesophageal; populations and can significantly degrade patients’ quality of life and lead to life-threatening complications. Reflux; A prudent course of management in a patient with classic GERD symptoms would be to empirically Disease; prescribe lifestyle modifications and a proton pump inhibitor (PPI) for six to eight weeks. Osteopathic GERD; manipulative treatment may also be a useful adjunct. If the patient is unable to afford a PPI, a histamine Current; type-2 receptor antagonist may be substituted (although they are much less effective). If resolution of Treatment; symptoms occurs, the therapeutic response can confirm the diagnosis of uncomplicated GERD. If the patient Diagnosis; has recurrent or intractable symptoms, the next step would be to order pH monitoring, manometry, or Management; endoscopic evaluation of the esophagus and stomach (esophagogastroduodenoscopy [EGD]). If there are Osteopathic; any atypical symptoms such as persistent cough, asthma, melena, sore throat, or hoarse voice, EGD should Manipulative; be ordered immediately. Patients with chronic esophagitis or extra-esophageal symptoms who have failed Treatment; (or refused) medical management should consider fundoplication. OMT; © 2011 Elsevier Inc. All rights reserved. Barrett; Medical; Medications Gastroesophageal reflux disease (GERD) is a common evaluate and manage GERD. Table 1 outlines some key points problem that occurs in both adult and pediatric populations in of information for readers to consider. -

Gallbladder Disease in the Aged Patient- a Comprehensive Diagnosis and Treatment Approach
Review Article Adv Res Gastroentero Hepatol Volume 8 Issue 1 - November 2017 Copyright © All rights are reserved by Zvi Perry DOI: 10.19080/ARGH.2017.08.555730 Gallbladder Disease in the Aged Patient- A Comprehensive Diagnosis and Treatment Approach Sharon Ziskind1, Uri Netz2, Udit Gibor2, ShaharAtias2, Leonid Lantsberg2 and Zvi H Perry1,2* 1Soroka University Medical Center, Israel 2Department of Epidemiology and Health Management, Ben-Gurion University of the Negev, Israel Submission: September 01, 2017; Published: November 22, 2017 *Corresponding author: Zvi Perry, MD, MA, Surgical Ward A, Soroka University Medical Center PO Box 151, Beer-Sheva 64101, Israel, Tel: +972-8-6400610; Fax: +972-8-6477633; Email: Abstract The improvements in life expectancy combined with aging of the baby boomer generation will result in a rapid increase in the population older than 65 years in the next few decades, and thus an increase in the need to take care of elderly patients. The authors of this chapter were born and raised in Israel, a country in which due to the holocaust and the fact it was a young nation, was not accustomed to elderly patients. But, in the last decade the percentage of patients older than 65 has crossed the 10% mark of the entire population and we were forced to learn elderly patients and the know how in treating them is not the same as the 30 years old patient. It is important to do so, because It is expected and to find ways to care and treat older patients. As the saying in pediatrics, that a child is not a small adult, the same rule applies seemingly to that by 2030 one in five people will be older than 65 years, with the most rapidly growing segment of this older population being persons older than 85. -

Gastroesophageal Reflux Disease
The new england journal of medicine clinical practice Gastroesophageal Reflux Disease Peter J. Kahrilas, M.D. This Journal feature begins with a case vignette highlighting a common clinical problem. Evidence supporting various strategies is then presented, followed by a review of formal guidelines, when they exist. The article ends with the author’s clinical recommendations. A 53-year-old man, who is otherwise healthy and has a 20-year history of occasional heartburn, reports having had worsening heartburn for the past 12 months, with daily symptoms that disturb his sleep. He reports having had no dysphagia, gastroin- testinal bleeding, or weight loss and in fact has recently gained 20 lb (9 kg). What would you advise regarding his evaluation and treatment? The Clinical Problem From the Division of Gastroenterology, Gastroesophageal reflux disease is the most common gastrointestinal diagnosis re- Feinberg School of Medicine, Chicago. Ad- corded during visits to outpatient clinics.1 In the United States, it is estimated that dress reprint requests to Dr. Kahrilas at the Feinberg School of Medicine, 676 St. Clair 14 to 20% of adults are affected, although such percentages are at best approxima- St., Suite 1400, Chicago, IL 60611-2951, tions, given that the disease has a nebulous definition and that such estimates are or at [email protected]. based on the prevalence of self-reported chronic heartburn.2 A current definition of N Engl J Med 2008;359:1700-7. the disorder is “a condition which develops when the ref lux of stomach contents causes Copyright © 2008 Massachusetts Medical Society. troublesome symptoms (i.e., at least two heartburn episodes per week) and/or complications.”3 Several extraesophageal manifestations of the disease are well rec- ognized, including laryngitis and cough (Table 1). -
Cholecystitis
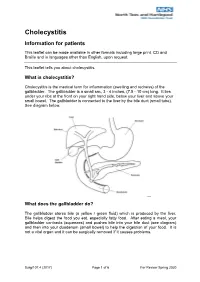
Cholecystitis Information for patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. This leaflet tells you about cholecystitis. What is cholecystitis? Cholecystitis is the medical term for inflammation (swelling and redness) of the gallbladder. The gallbladder is a small sac, 3 - 4 inches, (7.5 - 10 cm) long. It lies under your ribs at the front on your right hand side, below your liver and above your small bowel. The gallbladder is connected to the liver by the bile duct (small tube). See diagram below. What does the gallbladder do? The gallbladder stores bile (a yellow / green fluid) which is produced by the liver. Bile helps digest the food you eat, especially fatty food. After eating a meal, your gallbladder contracts (squeezes) and pushes bile into your bile duct (see diagram) and then into your duodenum (small bowel) to help the digestion of your food. It is not a vital organ and it can be surgically removed if it causes problems. Surg/107.4 (2017) Page 1 of 6 For Review Spring 2020 Cholecystitis What causes cholecystitis? Inflammation of the gallbladder is often caused when gallstones irritate the gallbladder and sometimes cause an infection. Gallstones are formed in the gallbladder or bile duct and develop when bile forms crystals. Over time these crystals become hardened and eventually grow into stones but they do not always cause problems. However, gallstones can cause: jaundice. If the stones move from your gallbladder and block your bile duct jaundice can occur. -

The Spectrum of Gallbladder Disease
The Spectrum of Gallbladder Disease Rebecca Kowalski, M.D. October 18, 2017 Overview A (brief) history of gallbladder surgery Anatomy Anatomical variations Physiology Pathophysiology Diagnostic imaging of the gallbladder Natural history of cholelithiasis Case presentations of the spectrum of gallstone disease Summary History of Gallbladder Surgery Gallbladder Surgery: A Relatively Recent Change Prior to the late 1800s, doctors treated gallbladder disease with a cholecystostomy, due to the fear that removing the organ would kill patients Carl Johann August Langenbuch (director of the Lazarus Hospital in Berlin, Germany) practiced on a cadaver to remove the gallbladder, and in 1882, performed a cholecystectomy on a patient. He was discharged after 6 weeks in the hospital https://en.wikipedia.org/wiki/Carl_Langenbuch By 1897 over 100 cholecystectomies had been performed Gallbladder Surgery: A Relatively Recent Change In 1985, Erich Mühe removed a patient’s gallbladder laparoscopically in Germany Erich Muhe https://openi.nlm.ni h.gov/detailedresult. php?img=PMC30152 In 1987, Philippe Mouret (a 44_jsls-2-4-341- French gynecologic surgeon) g01&req=4 performed a laparoscopic cholecystectomy In 1992, the National Institutes of Health (NIH) created guidelines for laparoscopic cholecystectomy in the United Philippe Mouret States, essentially transforming https://www.pinterest.com surgical practice /pin/58195020154734720/ Anatomy and Abnormal Anatomy http://accesssurgery.mhmedical.com/content.aspx?bookid=1202§ionid=71521210 http://www.slideshare.net/pryce27/rsna-final-2 http://www.slideshare.net/pryce27/rsna-final-2 http://www.slideshare.net/pryce27/rsna-final-2 Physiology a http://www.nature.com/nrm/journal/v2/n9/fig_tab/nrm0901_657a_F3.html Simplified overview of the bile acid biosynthesis pathway derived from cholesterol Lisa D. -

Biliary Tract Microbiota: a New Kid on the Block of Liver Diseases?
European Review for Medical and Pharmacological Sciences 2020; 24: 2750-2775 Biliary tract microbiota: a new kid on the block of liver diseases? A. NICOLETTI1, F.R. PONZIANI2, E. NARDELLA1, G. IANIRO2, A. GASBARRINI1, L. ZILERI DAL VERME2 1Internal Medicine, Gastroenterology and Hepatology, Fondazione Policlinico Universitario Agostino Gemelli IRCCS, Università Cattolica del Sacro Cuore, Rome, Italy 2Internal Medicine, Gastroenterology and Hepatology, Fondazione Policlinico Universitario Agostino Gemelli IRCCS, Rome, Italy Abstract. – The microbiome plays a crucial man body1,2. Indeed, a resident microbiota has recent- role in maintaining the homeostasis of the or- ly been described in several human environments ganism. Recent evidence has provided novel previously described as devoid of microorganisms, insights for understanding the interaction be- such as the urinary tract and the stomach3-9. Even tween the microbiota and the host. However, the 10 vast majority of such studies have analyzed the healthy placenta hosts microbial communities . interactions taking place in the intestinal tract. Bile has traditionally been considered sterile The biliary tree has traditionally been consid- under normal conditions11-14. ered sterile under normal conditions. However, The physical and chemical features of bile and the advent of metagenomic techniques has re- its antimicrobial activity were supposed to create vealed an unexpectedly rich bacterial communi- a hostile environment for bacteria. Moreover, the ty in the biliary tract. Associations between specific microbiolog- difficulty in collecting bile samples, coupled with ical patterns and inflammatory biliary diseases the lack of sensibility of culture techniques in and cancer have been recently described. Hence, detecting microbes in low-charge samples, sus- biliary dysbiosis may be a primary trigger in the tained this hypothesis for a long time. -

Pathogenesis of Gall Stones in Crohn's Disease
94 Gutl994;35:94-97 Pathogenesis ofgall stones in Crohn's disease: an alternative explanation Gut: first published as 10.1136/gut.35.1.94 on 1 January 1994. Downloaded from R Hutchinson, P N M Tyrrell, D Kumar, J A Dunn, J K W Li, R N Allan Abstract that other factors are necessary for gall stone The increased prevalence of gall stones in formation including nucleation factors and gall Crohn's disease is thought to be related to bladder stasis.78 depletion of the bile salt pool due either to Clinically we noted a high incidence of gall terminal ileal disease or after ileal resection. stones in patients with Crohn's disease but there This study was designed to examine whether was no obvious correlation with terminal ileal this hypothesis is correct and explore alterna- disease, which suggested that gall stones were tive explanations. Two hundred and fifty one not necessarily attributable to the disturbance in randomly selected patients (156 females, 95 the enterohepatic circulation of bile salts. We males, mean age 45 years) were interviewed therefore surveyed a large number of patients and screened by ultrasonography to determine with Crohn's disease to determine the prevalence the prevalence ofgall stones in a large popula- of gall stones and the risk factors for their tion of patients with Crohn's disease. Sixty development. nine (28%) patients had gall stones proved by ultrasonography (n=42), or had had chole- cystectomy for gail stone disease (n=27). The Patients and methods risk factors for the development of gall stones Two hundred and fifty one consecutive patients including sex, age, site, and duration of with Crohn's disease attending the inflammatory disease, and previous intestinal resection were bowel disease clinic were studied and clinical examined by multivariate analysis. -

Diagnosis and Management of Primary Sclerosing Cholangitis
AASLD PRACTICE GUIDELINES Diagnosis and Management of Primary Sclerosing Cholangitis Roger Chapman,1 Johan Fevery,2 Anthony Kalloo,3 David M. Nagorney,4 Kirsten Muri Boberg,5 Benjamin Shneider,6 and Gregory J. Gores7 Preamble classification used by the Grading of Recommendation This guideline has been approved by the American Asso- Assessment, Development, and Evaluation (GRADE) ciation for the Study of Liver Diseases and represents the workgroup with minor modifications (Table 1).3 The position of the Association. These recommendations pro- strength of recommendations in the GRADE system are vide a data-supported approach. They are based on the classified as strong (class 1) or weak (class 2). The quality following: (1) formal review and analysis of the recently- of evidence supporting strong or weak recommendations published world literature on the topic (Medline search); is designated by one of three levels: high (level A), mod- (2) American College of Physicians Manual for Assessing erate (level B), or low-quality (level C). Health Practices and Designing Practice Guidelines1; (3) guideline policies, including the AASLD Policy on the Definition and Diagnosis Development and Use of Practice Guidelines and the Definitions. Primary sclerosing cholangitis (PSC) is a American Gastroenterological Association Policy State- chronic, cholestatic liver disease characterized by inflam- ment on Guidelines2; and (4) the experience of the au- mation and fibrosis of both intrahepatic and extrahepatic thors in the specified topic. bile ducts,4 leading to the formation of multifocal bile Intended for use by physicians, these recommenda- duct strictures. PSC is likely an immune mediated, pro- tions suggest preferred approaches to the diagnostic, ther- gressive disorder that eventually develops into cirrhosis, apeutic and preventative aspects of care. -

Enterogastric Reflux Mimicking Gallbladder Disease: Detection, Quantitation and Potential Significance
Enterogastric Reflux Mimicking Gallbladder Disease: Detection, Quantitation and Potential Significance Alberto J. Arroyo, J. Bradley Burns, Wayne A. Huyghe, Ann E. Dollman and Yogesh P. Patel Department of Nuclear Medicine, Division of Radiology, St. Vincent Mercy Medical Center, Toledo; and Department of Radiology, Medical College of Ohio, Toledo, Ohio enterogastric reflux during such studies performed to evaluate Objective: Visualization of enterogastric reflux (EGR) may gallbladder (GB) disease (2). Gastric reflux may damage the be present during hepatobiliary imaging. Reflux of bile may gastric mucosa, alter its function and cause such symptoms as damage the gastric mucosa, altering its function, and cause epigastric and postprandial pain, intermittent vomiting of such symptoms as epigastric pain, heartburn, nausea, inter- mittent vomiting and abdominal fullness. These symptoms bilious contents, heartburn, nausea and abdominal fullness (3). also are associated with gallbladder disease. The aim of this These symptoms are associated also with GB disease. study was to quantitate the EGR index (EGRI) and to The role of bile and pancreatic enzymes in the pathogenesis determine if a difference exists in normal and abnormal of dyspeptic symptoms and mucosal lesions of the stomach and responses using standard cholecystokinin (CCK)-augmented esophagus has been extensively investigated (4). Questions hepatobiliary imaging. persist including whether the presence of bile in the stomach is Methods: This study used 129 patients. LAO dynamic data a physiologic phenomenon, and what amount of bile the ϫ on a 128 128 matrix at a rate of 1 frame/min were obtained. stomach can tolerate without pathologic or clinical manifesta- After the gallbladder ejection fraction (GBEF) was deter- tions (5).