Deep Tendon Reflex: the Tools and Original Article Techniques
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Correlation of Electrodiagnostic and Clinical Findings in Unilateral S1 Radiculopathy
Neurol. Croat. Vol. 65, 1-4, 2016 Correlation of electrodiagnostic and clinical findings in unilateral S1 radiculopathy Seyed Mansoor Rayegani, Navid Rahimi, Elham Loni, Shahram Rahimi Dehgolan, Leyla Sedighipour ABSTRACT – Objectives: Lumbosacral radiculopathy is a challenging diagnosis and electrodiagnostic study (EDX) is a good complementary test to magnetic resonance imaging (MRI). Physical examination, MRI and electrodiagnosis have different diagnostic value in this regard. MRI can provide anatomical evidence and is 3 useful in choosing the treatment procedure, but it may also yield false-positive results. In this study, we as- 1-4, 2016 Number sessed the correlation of clinical and EDX findings in patients with L5-S1 disc herniation on MRI.Methods: EDX was performed in 87 patients referred for clinical and MRI diagnosis of S1 radiculopathy. The consist- ency of EDX results with MRI and clinical findings was evaluated by Pearson 2χ -test and odds ratio. Results: Disc protrusion was present in 58% and disc extrusion in 42% of patients. Physical examination revealed absent Achilles reflex in 83% and decreased S1 dermatome sensation in 65% of patients. In this study, EDX sensitivity was about 92%. The highest consistency between EDX parameters and physical examination find- ings was recorded between absent H-reflex and decreased Achilles reflex (OR=6.20; p=0.014), but there was no significant consistency between H-reflex and either muscular weakness or straight leg raising test result (p>0.05). There was no relationship between the type of disc herniation on MRI and H-reflex either. There was correlation between H-reflex abnormalities and absent ankle reflex in patients with unilateral L5-S1 disc herniation on MRI. -

Theoretical Part Recruitment and Summation in Skeletal Muscle
name number study group Theoretical part Recruitment and summation in skeletal muscle Myography and electromyography Myography is a method for recording skeletal muscle contractions. On the contrary, electromyography (EMG) is a method registering the electric activity produced by skeletal muscle. Muscle fibre Each individual skeletal muscle cell (or myocyte or fiber) contains a dense parallel array of smaller, cylindrical elements called myofibrils that have the diameter of a Z disk (Figure 1). Each of these myofibrils comprises repeating units, or sarcomeres, that consist of smaller interdigitating filaments called myofilaments. These myofilaments come in two types, thick filaments composed primarily of myosin and thin filaments composed primarily of actin. The sarcomere extends from one Z disk to another. Sarcomeres stacked end to end make up a myofibril. The repeating sarcomeres are most highly organized within skeletal and cardiac muscle and impart a striped appearance. Thin filaments are 5 to 8 nm in diameter and, in striated muscle, 1 μm in length. In striated muscle, the thin filaments are tethered together at one end, where they project from a dense disk known as the Z disk. The Z disk is oriented perpendicular to the axis of the muscle fibre; thin filaments project from both its faces. Not only do Z disks tether the thin filaments of a single myofibril together, but connections between the Z disks also tether each myofibril to its neighbours. These interconnections align the sarcomeres and give skeletal and, to a lesser extent, cardiac muscle its striated appearance. The thick filaments are 10 nm in diameter and, in striated muscle, 1.6 μm in length. -

Level Diagnosis of Cervical Compressive Myelopathy: Signs, Symptoms, and Lesions Levels
Elmer Press Original Article J Neurol Res • 2013;3(5):135-141 Level Diagnosis of Cervical Compressive Myelopathy: Signs, Symptoms, and Lesions Levels Naoki Kasahata ficult to accurately localize the lesion before radiographic Abstract diagnosis. However, neurological level diagnosis of spinal cord is important for accurate lesion-specific level diagnosis, Background: To elucidate signs and symptoms corresponding to patients’ treatment, avoiding diagnostic error, differential di- each vertebral level for level-specific diagnoses. agnosis, and especially for accurate level diagnosis of other nonsurgical myelopathies. Moreover, level diagnosis should Methods: We studied 106 patients with cervical compressive my- be considered from multiple viewpoints. Therefore, we in- elopathy. Patients who showed a single compressive site on mag- tend to make level diagnosis of myelopathy more accurate. netic resonance imaging (MRI) were selected, and signs, symp- Previously, lesion-specific level diagnoses by determin- toms, and the levels of the MRI lesions were studied. ing a sensory disturbance area or location of numbness in Results: Five of 12 patients (41.7%) with C4-5 intervertebral level the hands had the highest accuracy [1, 2]. Previous stud- lesions showed decreased or absent biceps and brachioradialis re- ies reported that C3-4 intervertebral level lesions showed flexes, while 4 of these patients (33.3%) showed generalized hyper- increased or decreased biceps reflexes, deltoid weakness, reflexia. In comparison, 5 of 24 patients (20.8%) with C5-6 inter- and sensory disturbance of arms or forearms [1, 3, 4], while vertebral level lesions showed decreased or absent triceps reflexes; C4-5 intervertebral level lesions showed decreased biceps however, 9 of these patients (37.5%) showed decreased or absent reflexes, biceps weakness, and sensory disturbance of hands biceps and brachioradialis reflexes. -
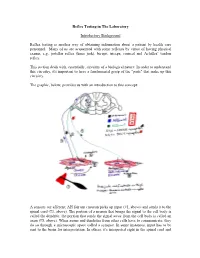
Reflex Testing in the Laboratory
Reflex Testing in The Laboratory Introductory Background Reflex testing is another way of obtaining information about a patient by health care personnel. Many of us are acquainted with some reflexes by virtue of having physical exams, e.g., patellar reflex (knee jerk), biceps, triceps, corneal and Achilles’ tendon reflex. This section deals with, essentially, circuitry of a biological nature. In order to understand this circuitry, it's important to have a fundamental grasp of the "parts" that make up this circuitry. The graphic, below, provides us with an introduction to this concept: A sensory (or afferent; AH fair unt) neuron picks up input (#1, above) and sends it to the spinal cord (#3, above). The portion of a neuron that brings the signal to the cell body is called the dendrite; the portion that sends the signal away from the cell body is called an axon (#5, above). When axons and dendrites from other cells have to communicate, they do so through a microscopic space called a synapse. In some instances, input has to be sent to the brain for interpretation. In others, it's interpreted right in the spinal cord and signals are sent out (motor or efferent; EE fair unt) to the effector organ. In simple stretch reflexes, only two neurons are involved: sensory and motor, graphic, above. In this figure, a stretch reflex is illustrated. The way it works is in this manner: 1) a tendon is stimulated (in this illustration by a reflex hammer), 2) the spindle (blue coil in the diagram) detects this stimulus and sends the input to the cord, 3) the information crosses one synapse (mono-synaptic) to a motor neuron that sends output to the spindle (green coil in diagram) and the muscle contracts. -

In the Name of God the Compassionate and the Merciful
In the Name of God the Compassionate and the Merciful Cutaneomuscular Reflexes in the Lower Limbs in Man A Thesis Submitted for the Degree of Doctor of Philosophy in the Faculty of Medicine by Hossein-Bagheri BSc and MSc in Physiotherapy April 1995 Division of Neuroscience and Biomedical Systems, Institute of Biomedical Life Sciences, University of Glasgow ProQuest Number: 11007741 All rights reserved INFORMATION TO ALL USERS The quality of this reproduction is dependent upon the quality of the copy submitted. In the unlikely event that the author did not send a com plete manuscript and there are missing pages, these will be noted. Also, if material had to be removed, a note will indicate the deletion. uest ProQuest 11007741 Published by ProQuest LLC(2018). Copyright of the Dissertation is held by the Author. All rights reserved. This work is protected against unauthorized copying under Title 17, United States C ode Microform Edition © ProQuest LLC. ProQuest LLC. 789 East Eisenhower Parkway P.O. Box 1346 Ann Arbor, Ml 48106- 1346 g la s s o w r DNivEfiajr? library Dedicated to my wife and children Dedicated to my father who passed away during my Ph.D course i Contents Page List of contents i List of figures vi List of tables ix Abbreviations xi Acknowledgement xiii Declaration and list of publications xiv Summary xv 1. Introduction 1 1.1 General history 1 1.2 Techniques for identifying spinal reflexes 3 Monosynaptic testing 3 H-reflex 3 Spinal proprioceptive reflexes 4 Single motor unit EMG recording 4 Peristimulus time histogram 5 Surface -
Caregiver-Handbook-06-Health-1
Health Communicable Diseases What is a Communicable Disease? A communicable disease is one that is spread from one person to another through a variety of ways that include: contact with blood and bodily fluids, breathing in an airborne virus, or by having contact with a little bug called lice. For the most part, communicable diseases are spread through viruses and bacteria that live in blood and body fluids. For instance, hepatitis and human immunodeficiency virus (HIV) are examples of infections that can be carried in blood and bodily fluids. On the other hand, tuberculosis is an airborne disease. A person with tuberculosis (TB) can spread tiny germs that float in the air if they cough or sneeze without covering their nose or mouth. And, there are some communicable diseases like head lice that are caused by a live lice bug that is spread by using an infected comb or wearing a hat that is infested with lice. For more information about how to reduce potential exposure to communicable diseases, see Section 7. Let’s take a closer look at some communicable diseases. Page 6-2 - 53 - Head Lice How is Head Lice Spread? Head lice can infest people of all ages and economic standing. Head to head contact or simple exchange of hats, clothing, combs and other personal items can lead to the transmission of lice from one person to another. Head lice are contagious. If someone you know has head lice, do not panic. Caregiving Tips: 1. Inspect for Lice and Nits Using a magnifying glass and natural light, carefully examine hair, scalp, sideburns, eyebrows, beards and mustaches of all household members for lice and their eggs, called “nits.” Nits, which are yellowish-white in color and oval shaped, can be easier to locate than lice. -

The Phenomenon of Multiple Stretch Reflexes
Henry Ford Hospital Medical Journal Volume 34 Number 1 Article 6 3-1986 The Phenomenon of Multiple Stretch Reflexes Robert D. Teasdall Follow this and additional works at: https://scholarlycommons.henryford.com/hfhmedjournal Part of the Life Sciences Commons, Medical Specialties Commons, and the Public Health Commons Recommended Citation Teasdall, Robert D. (1986) "The Phenomenon of Multiple Stretch Reflexes," Henry Ford Hospital Medical Journal : Vol. 34 : No. 1 , 31-36. Available at: https://scholarlycommons.henryford.com/hfhmedjournal/vol34/iss1/6 This Article is brought to you for free and open access by Henry Ford Health System Scholarly Commons. It has been accepted for inclusion in Henry Ford Hospital Medical Journal by an authorized editor of Henry Ford Health System Scholarly Commons. The Phenomenon of Multiple Stretch Reflexes Robert D. Teasdall, MD* Multiple stretch reflexes occur in muscles adjacent to or remote from the tap. The response may be ipsilateral or bilateral. These reflexes are encountered not only in normal subjects with brisk stretch reflexes but particularly in patients with lesions of the upper motor neuron. The concussion obtained by the blow is conducted along bone to muscle. Muscle spindles are stimulated, and in this manner independent stretch reflexes are produced in these muscles. This mechanism is responsible for the phenomenon of multiple stretch reflexes. The thorax and pelvis play important roles in the contralateral responses by transmitting these mechanical events across the midline. (Henry FordHosp Med J 1986;34:31-6) ontraction of muscles remote from the site of f)ercussion is Head and neck Cencountered in patients with brisk stretch reflexes. -

Clinical Tests and Differential Diagnosis of Cervical Spondylotic Myelopathy 39
Clinical Tests and Differential Diagnosis of Cervical 05 Spondylotic Myelopathy Jesus Lafuente Introduction MRI, and clinical symptoms is essential for a correct diagnosis. Anterior-posterior width Cervical spondylotic myelopathy (CSM) is reduction, cross-sectional evidence of cord a disabling disease caused by a combina- compression, obliteration of the subarach- tion of mechanical compression and vascu- noid space, and signal intensity changes to lar compromise of the spinal cord. It is the the cord found on MR imaging are consid- most common cause of spinal dysfunction ered the most appropriate parameters for in older patients.1 The onset is often insidi- confirmation of a spinal cord compression ous with long periods of episodic, stepwise myelopathy.4 In some occasions when the progression and may present with different diagnosis is still not clear, the use of other symptoms from one patient to another.2 CSM studies could help, such as diagnostic elec- is a clinical diagnosis that may involve broad- trophysiology and cerebrospinal fluid (CSF) based gait disturbances first, associated with examination. weakness of the legs, and then spasticity.3 As spinal cord degeneration progresses, lower motor neuron findings in the upper extremi- Clinical Tests ties, such as loss of strength, atrophy, and CSM is the most common cause of spinal difficulty in fine finger movements, may cord dysfunction in the world. A meticu- present.3 Additional clinical findings may lous physical examination of patients with include: neck stiffness, shoulder pain, pares- cervical pathology can relatively make the thesia in one or both arms or hands, radicu- distinction between radiculopathy or mye- lopathy, a positive Hoffman and/or Babinski lopathy easy. -

LETTERS to the EDITOR Calf Muscle Hypertrophy
Clinical Neuropathology, Vol. 37 – No. 3/2018 – Letters to the editor 146 LETTERS TO THE EDITOR sias in the right foot and continuous calf pain. Routine blood tests, including sedimentation rate, C-reactive protein, eosinophil count, Calf muscle hypertrophy thyroid hormones, liver enzymes, and cry- following S1 radiculopathy: ocrit were within normal ranges. ANA-ENA screening and search for neurotrophic vi- Letter A stress disorder caused by ruses were negative. Serum creatine kinase ©2018 Dustri-Verlag Dr. K. Feistle hyperactivity with variable (CK) was increased (520 UI/L). ISSN 0722-5091 response to treatment Needle electromyography (EMG) showed DOI 10.5414/NP301093 e-pub: February 16, 2018 marked abnormalities consisting of continu- Nila Volpi1,2, Federica Ginanneschi1,2, ous complex repetitive discharges (CRDs), Alfonso Cerase1,3, Salvatore Francesco polyphasic motor unit potentials with reduced Carbone4, Margherita Aglianò1, voluntary recruitment in the right gastroc- Paola Lorenzoni1, Matteo Bellini3, nemius muscle. EMG recordings of right Sabina Bartalini2, Giovanni Di Pietro5, tibialis anterior, quadriceps femoris, gluteus and Alessandro Rossi1,2 maximum, and adductor magnus muscles were unremarkable. 1Department of Medical, Surgical, and Magnetic resonance imaging (MRI) (Fig- Neurological Sciences, University of ure 1) showed a volume increase of right leg Siena, 2Unit of Neurology and Clinical posterior muscles, more evident on soleus Neurophysiology, 3Unit of Neuroradiology, and medial gastrocnemius, with intrafascial 4Unit of Diagnostic Imaging, and edema and mild hypervascularization of hy- 5Unit of Neurosurgery, University pertrophic muscles. Hospital Santa Maria alle Scotte, Lumbosacral spinal MRI and computed Siena, Italy tomography (Figure 1) evidenced diffuse de- generative disease of the lumbar spine and a L5-S1 right paramedian posterior disc herni- Sir, – Neurogenic focal muscle hyper- ation compressing the ipsilateral S1 radicular trophy (NMH) is a rare event in different sheath and S1 nerve root. -

REFLEXES the Stretch Reflex Physiological Stretch Reflex Are Present in a Healthy Individual
REFLEXES The stretch reflex Physiological stretch reflex are present in a healthy individual. The evocation of reflex: by tapping of neurological hammer on the respective tendon The tapping: only one reasonably strong, painless, fast, accurate The muscle groups, that are investigated: relaxed The position and the grip: the best one position and one grip for the examination of all reflexes on the limb Reinforcement maneuvers to improve the evoking: • Placing the therapist's fingers on the tendon (stretching) and tapping on the fingers • Jendrassik's maneuver - clinch the hands together and try to break away or the patient to clench their teeth or the isometric contraction on the opposite limb = on the basis of the phenomenon of irradiation • A distraction: eg. calculation: from 100 gradually subtract 7 • Change positions: in lying supine the response is the lowest, in sitting or standing the excitability of the central nervous system increases and the responses are higher Response: Normoreflexia = the muscle contraction with an adequate motion Hyperreflexia = increased response, muscle contraction with significantly large movement = response even with slight tapping of hammer = the reflex zone (area of inducing) is extended beyond the tendon = in central paresis, in disorders of the extrapyramidal system, in cerebellar lesions with pendulum movements Hyporeflexia = the decreased response (only contraction happens but not to move), necessary sharper tap and reinforcement maneuver Areflexia = no response = in peripheral paresis Rate the reflex -

Correlation of Electrodiagnostic and Clinical Findings
ORIGINAL ARTICLE Correlation of Electrodiagnostic and Clinical Findings in Unilateral S1 Radiculopathy Seyed Mansoor Rayegani1,2, Seyed Ahmad Raeissadat1,3, Elham Loni4, Navid Rahimi1,2, Shahram Rahimi-Dehgolan5, Leyla Sedighipour1,2 1 Department of Physical Medicine and Rehabilitation, Physical Medicine and Rehabilitation Research Center, Shahid Beheshti University of Medical Sciences, Tehran, Iran 2 Shohada Hospital, Shahid Beheshti University of Medical Sciences, Tehran, Iran 3 Clinical Development Research Center, Shahid Modarres Hospital, Shahid Beheshti University of Medical Sciences, Tehran, Iran. 4 Department of Physical Medicine and Rehabilitation, University of Social Welfare and Rehabilitation Sciences, Tehran, Iran 5Department of Physical Medicine and Rehabilitation, School of Medicine, Tehran University of Medical Sciences, Tehran, Iran Received: 20 Jan. 2018; Accepted: 15 Dec. 2018 Abstract- Lumbosacral radiculopathy is a challenging diagnosis, and Electrodiagnostic study (EDX) is a good complementary test for Magnetic Resonance Imaging (MRI). Physical examination, MRI and electrodiagnosis have different diagnostic values in this regard. MRI can provide anatomical evidence and is useful in choosing a treatment process, but it could also have false positive results. In this study, we assessed the correlation of clinical and electrodiagnostic findings in patients with positive MRI findings for S1 radiculopathy. EDX was performed for 87 patients referred with clinical and MRI diagnosis of S1 radiculopathy. The consistency between EDX results, MRI, and clinical findings were evaluated by Pearson chi 2 and odds ratio. Fifty-eight percent of patients had disc protrusion, and 42% had extrusion. Physical examination revealed absent Achilles reflex in 83% and decreased S1 dermatome sensation in 65%. In this study, EDX sensitivity was about 92%. -

Testing the Reflexes
Page 1 of 6 ESSENTIALS Testing the reflexes 1 2 A J Lees neurologist , Brian Hurwitz former general practitioner 1The National Hospital, Queen Square, London WC1N 3BG, UK; 2King’s College London, London WC2B 6LE, UK with muscles via the nerve roots, plexuses, peripheral nerves, What you need to know and neuromuscular junction) and an upper motor neurone lesion • Tendon reflex testing allows lower and upper motor neurone lesions to (due to damage upstream from the anterior horn cell, including be distinguished reliably the corticospinal tracts, the brain stem, and motor cortex). This • Interpret reflexes alongside a clinical history and any abnormalities of distinction is the first stage in locating the site of neurological power, tone, and sensation found on examination damage. • Reflex testing is essential if you suspect spinal cord and cauda equina compression, acute cervical or lumbar disc compression, or acute There are situations where all the neurological symptoms occur inflammatory demyelinating polyradiculoneuropathy above the neck (such as bulbar symptoms due to motor neurone disease) where reflex testing is also essential. Eliciting the deep tendon reflexes is a vital component of Box 1 lists some clinical scenarios where testing the deep tendon medical assessments in general practice (where 9% of medical reflexes is discriminatory when coming to a diagnosis. problems are believed to be neurological in origin1) and in hospital (where 10-20% of admissions have a primary Box 1: Presentations in general practice where tendon reflex