The Indications for Toe Transfer After ''Minor
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Metatarsalgia
just the symptoms. What can I expect from treatment? With a proper diagnosis, and a well-rounded treatment plan including orthotics, the prog- nosis is excellent. With Sole Supports™ foot or- thotics you can expect either a dramatic loss The Truth About . of pain within the first weeks of use or a more gradual reduction of symptoms, depending Metatarsalgia on how long the problem has existed, normal body weight or how well you follow other ther- For more information and a apeutic regimens prescribed by your provider. professional consultation regarding Did you know that, with Sole whether Sole Supports may be Supports, metatarsal pads are rarely helpful for you, please contact the needed? following certified Sole Supports practitioner: What is it? Metatarsalgia is a term used to describe a pain- ful foot condition in the area just before the Arch Flattened small toes (more commonly referred to as the ball of the foot). The condition is characterized by pain and inflammation on the sole in the region of the metatarsal heads, which are the ends of the long bones in your foot. The joint This handout provides a general overview on this capsule or tendons may also be inflamed. topic and may not apply to everyone. To find out if this handout applies to you and to get more infor- mation on this subject, consult with your certified Sole Supports practitioner. Arch Restored The pain is generally aggravated by putting ments but your doctor is likely to recommend pressure off the metatarsals should also be pressure (as in walking) through the ball of a conservative approach first including: followed. -

Wound Classification
Wound Classification Presented by Dr. Karen Zulkowski, D.N.S., RN Montana State University Welcome! Thank you for joining this webinar about how to assess and measure a wound. 2 A Little About Myself… • Associate professor at Montana State University • Executive editor of the Journal of the World Council of Enterstomal Therapists (JWCET) and WCET International Ostomy Guidelines (2014) • Editorial board member of Ostomy Wound Management and Advances in Skin and Wound Care • Legal consultant • Former NPUAP board member 3 Today We Will Talk About • How to assess a wound • How to measure a wound Please make a note of your questions. Your Quality Improvement (QI) Specialists will follow up with you after this webinar to address them. 4 Assessing and Measuring Wounds • You completed a skin assessment and found a wound. • Now you need to determine what type of wound you found. • If it is a pressure ulcer, you need to determine the stage. 5 Assessing and Measuring Wounds This is important because— • Each type of wound has a different etiology. • Treatment may be very different. However— • Not all wounds are clear cut. • The cause may be multifactoral. 6 Types of Wounds • Vascular (arterial, venous, and mixed) • Neuropathic (diabetic) • Moisture-associated dermatitis • Skin tear • Pressure ulcer 7 Mixed Etiologies Many wounds have mixed etiologies. • There may be both venous and arterial insufficiency. • There may be diabetes and pressure characteristics. 8 Moisture-Associated Skin Damage • Also called perineal dermatitis, diaper rash, incontinence-associated dermatitis (often confused with pressure ulcers) • An inflammation of the skin in the perineal area, on and between the buttocks, into the skin folds, and down the inner thighs • Scaling of the skin with papule and vesicle formation: – These may open, with “weeping” of the skin, which exacerbates skin damage. -

PE2260 Five-Finger Exercise
The Five-Finger Exercise The 5-finger exercise is helpful for relaxation and calming your system. It does not take long, but can help you feel much more peaceful and relaxed and help you feel better about yourself. Try it any time you feel tension. What are the steps to the 5-finger exercise? On one hand, touch your thumb to your index finger. Think back to a time you felt tired after exercise or some other fun physical activity. Touch your thumb to your middle finger. Go back to a time when you had a loving experience. You might recall a loving day with your family or a good friend, a warm hug from a parent or a time you had a really good conversation with someone. Touch your thumb to your ring finger. Remember the nicest compliment anyone ever gave you. Try to accept it now fully. When you do this, you are showing respect for the person who said it. You are really paying them a compliment in return. Touch your thumb to your little finger. Go back in your mind to the most beautiful and relaxing place you have ever been. Spend some time thinking of being there. To Learn More Free Interpreter Services • Adolescent Medicine • In the hospital, ask your nurse. 206-987-2028 • From outside the hospital, call the toll-free Family Interpreting Line, • Ask your healthcare provider 1-866-583-1527. Tell the interpreter • seattlechildrens.org the name or extension you need. Seattle Children’s offers interpreter services for Deaf, hard of hearing or non-English speaking patients, family members and legal representatives free of charge. -

Female Pelvic Relaxation
FEMALE PELVIC RELAXATION A Primer for Women with Pelvic Organ Prolapse Written by: ANDREW SIEGEL, M.D. An educational service provided by: BERGEN UROLOGICAL ASSOCIATES N.J. CENTER FOR PROSTATE CANCER & UROLOGY Andrew Siegel, M.D. • Martin Goldstein, M.D. Vincent Lanteri, M.D. • Michael Esposito, M.D. • Mutahar Ahmed, M.D. Gregory Lovallo, M.D. • Thomas Christiano, M.D. 255 Spring Valley Avenue Maywood, N.J. 07607 www.bergenurological.com www.roboticurology.com Table of Contents INTRODUCTION .................................................................1 WHY A UROLOGIST? ..........................................................2 PELVIC ANATOMY ..............................................................4 PROLAPSE URETHRA ....................................................................7 BLADDER .....................................................................7 RECTUM ......................................................................8 PERINEUM ..................................................................9 SMALL INTESTINE .....................................................9 VAGINAL VAULT .......................................................10 UTERUS .....................................................................11 EVALUATION OF PROLAPSE ............................................11 SURGICAL REPAIR OF PELVIC PROLAPSE .....................15 STRESS INCONTINENCE .........................................16 CYSTOCELE ..............................................................18 RECTOCELE/PERINEAL LAXITY .............................19 -

Mallet Finger Advice Information for Patients Page 2 This Information Leaflet Is for People Who Have Had a Mallet Finger Injury
Oxford University Hospitals NHS Trust Emergency Department Mallet finger advice Information for patients page 2 This information leaflet is for people who have had a mallet finger injury. It describes the injury, symptoms and treatment. What is a mallet finger? A mallet finger is where the end joint of the finger bends towards the palm and cannot be straightened. This is usually caused by an injury to the end of the finger which has torn the tendon that straightens the finger. Sometimes a flake of bone may have been pulled off from where the tendon should be attached to the end bone. An X-ray will show whether this has happened. In either case, without the use of this tendon the end of your finger will remain bent. What are the symptoms? • pain • swelling • inability to straighten the tip of your finger. page 3 How is it treated? Your finger will be placed in a plastic splint to keep it straight. The end joint will be slightly over extended (bent backwards). The splint must be worn both day and night for 6 to 8 weeks. This allows the two ends of the torn tendon or bone to stay together and heal. The splint will be taped on, allowing you to bend the middle joint of your finger. The splint should only be removed for cleaning (see below). Although you can still use your finger, you should keep your hand elevated (raised) in a sling for most of the time, until the doctor sees you in the outpatient clinic. This will help to reduce any swelling and pain. -

Palm Reading
Palm Reading Also known as palmistry or chiromancy, palm reading is practiced all over the world with roots in Indian astrology and gypsy fortune-telling. The objective is to evaluate a person’s character and aspects of their life by studying the palm of their hand. There is no substantiate evidence of correlation between palm features and psychological traits; palm reading is for entertainment purposes. Getting Started Which hand to read? There are two main practices: For males, the left hand is what you’re born with, and the right is what you’ve accumulated throughout your life. For females, it’s the opposite. Your dominant hand (the hand you use most often) determines your future and your other, non-dominant hand, is used to determine the past or hidden traits Take these into consideration when choosing which hand to read. Reading the Primary Lines of your Hand 1. Interpret the Heart Line This line is believed to indicate emotional stability, romantic perspectives, depression, and cardiac health. Begins below the index finger = content with love life Begins below the middle finger = selfish when it comes to love Begins in-between the middle and index fingers = caring and understanding Is straight and short = less interest in romance Touches life line = heart is broken easily Is long and curvy = freely expresses emotions and feelings Is straight and parallel to the head line = good handle on emotions Is wavy = many relationships, absence of serious relationships Circle on the line = sad or depressed Broken line = emotional trauma 2. Examine the Head Line This line represents learning style, communication style, intellectualism, and thirst for knowledge. -
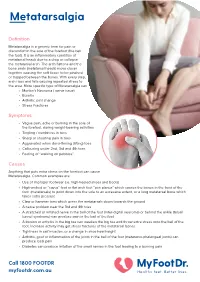
Metatarsalgia
Metatarsalgia Definition Metatarsalgia is a generic term for pain or discomfort in the sole of the forefoot (the ball of the foot). It is an inflammatory condition of the metatarsal heads due to a drop or collapse of the metatarsal arch. The arch flattens and the bone ends (metatarsal heads) move closer together causing the soft tissue to be pinched or trapped between the bones. With every step, the arch rises and falls causing repeated stress to the area. More specific type of Metatarsalgia can be: • Morton’s Neuroma ( nerve issue) • Bursitis • Arthritic joint change • Stress Fractures Symptoms • Vague pain, ache or burning in the sole of the forefoot, during weight-bearing activities • Tingling / numbness in toes • Sharp or shooting pain in toes • Aggravated when dorsi-flexing (lifting) toes • Callousing under 2nd, 3rd and 4th toes • Feeling of “walking on pebbles” Causes Anything that puts extra stress on the forefoot can cause Metatarsalgia. Common examples are: • Use of improper footwear (i.e. high-heeled shoes and boots) • High-arched or “cavus” foot or flat arch feet “pes planus” which causes the bones in the front of the foot (metatarsals) to point down into the sole to an excessive extent, or a long metatarsal bone which takes extra pressure • Claw or hammer toes which press the metatarsals down towards the ground • A nerve problem near the 3rd and 4th toes • A stretched or irritated nerve in the ball of the foot (inter-digital neuroma) or behind the ankle (tarsal tunnel syndrome) can produce pain in the ball of the foot • A bunion or arthritis in the big toe can weaken the big toe and throw extra stress onto the ball of the foot. -

Treatment of Spastic Foot Deformities
TREATMENT OF SPASTIC FOOT DEFORMITIES penn neuro-orthopaedics service Table of Contents OVERVIEW Severe loss of movement is often the result of neurological disorders, Overview .............................................................. 1 such as stroke or brain injury. As a result, ordinary daily activities Treatment ............................................................. 2 such as walking, eating and dressing can be difficult and sometimes impossible to accomplish. Procedures ........................................................... 4 The Penn Neuro-Orthopaedics Service assists patients with Achilles Tendon Lengthening .........................................4 orthopaedic problems caused by certain neurologic disorders. Our Toe Flexor Releases .....................................................5 team successfully treats a wide range of problems affecting the limbs including foot deformities and walking problems due to abnormal Toe Flexor Transfer .......................................................6 postures of the foot. Split Anterior Tibialis Tendon Transfer (SPLATT) ...............7 This booklet focuses on the treatment of spastic foot deformities The Extensor Tendon of the Big Toe (EHL) .......................8 under the supervision of Keith Baldwin, MD, MSPT, MPH. Lengthening the Tibialis Posterior Tendon .......................9 Care After Surgery .................................................10 Notes ..................................................................12 Pre-operative right foot. Post-operative -

Stretching and Positioning Regime for Upper Limb
Information for patients and visitors Stretching and Positioning Regime for Upper Limb Physiotherapy Department This leaflet has been designed to remind you of the exercises you Community & Therapy Services have been taught, the correct techniques and who to contact with any queries. For more information about our Trust and the services we provide please visit our website: www.nlg.nhs.uk Information for patients and visitors Muscle Tone Muscle tone is an unconscious low level contraction of your muscles while they are at rest. The purpose of this is to keep your muscles primed and ready to generate movement. Several neurological causes may change a person’s muscle tone to increase or decrease resulting in a lack of movement. Over time, a lack of movement can cause stiffness, pain, and spasticity. In severe cases this may also lead to contractures. Spasticity Spasticity can be defined as a tightening or stiffness of the muscle due to increased muscle tone. It can interfere with normal functioning. It can also greatly increase fatigue. However, exercise, properly done, is vital in managing spasticity. The following tips may prove helpful: • Avoid positions that make the spasticity worse • Daily stretching of muscles to their full length will help to manage the tightness of spasticity, and allow for optimal movement • Moving a tight muscle to a new position may result in an increase in spasticity. If this happens, allow a few minutes for the muscles to relax • When exercising, try to keep head straight • Sudden changes in spasticity may -

How to Self-Bandage Your Leg(S) and Feet to Reduce Lymphedema (Swelling)
Form: D-8519 How to Self-Bandage Your Leg(s) and Feet to Reduce Lymphedema (Swelling) For patients with lower body lymphedema who have had treatment for cancer, including: • Removal of lymph nodes in the pelvis • Removal of lymph nodes in the groin, or • Radiation to the pelvis Read this resource to learn: • Who needs self-bandaging • Why self-bandaging is important • How to do self-bandaging Disclaimer: This pamphlet is for patients with lymphedema. It is a guide to help patients manage leg swelling with bandages. It is only to be used after the patient has been taught bandaging by a clinician at the Cancer Rehabilitation and Survivorship (CRS) Clinic at Princess Margaret Cancer Centre. Do not self-bandage if you have an infection in your abdomen, leg(s) or feet. Signs of an infection may include: • Swelling in these areas and redness of the skin (this redness can quickly spread) • Pain in your leg(s) or feet • Tenderness and/or warmth in your leg(s) or feet • Fever, chills or feeling unwell If you have an infection or think you have an infection, go to: • Your Family Doctor • Walk-in Clinic • Urgent Care Clinic If no Walk-in clinic is open, go to the closest hospital Emergency Department. 2 What is the lymphatic system? Your lymphatic system removes extra fluid and waste from your body. It plays an important role in how your immune system works. Your lymphatic system is made up of lymph nodes that are linked by lymph vessels. Your lymph nodes are bean-shaped organs that are found all over your body. -

Hammer Toe Information Sheet
Fitter Feet For Life Hammer toe information sheet. (ref. A15) A hammer toe is a deformity of the first small toe joint with in toes. (proximal inter-phalangeal joint) This deformity can occur in the second, third, fourth or fifth (relatively rare) toes, causing it to be permanently bent, resembling a hammer. This abnormality can create pressure on the foot when wearing shoes and cause discomfort and problems walking. The joints themselves can be arthritic and painful. There is a choice of different procedures to straighten a hammer toe. This information sheet has been written to help you choose which procedure is best for you. Fig 1 Hammer toe . Fig 2 Arthrodesis with K wires . Fig 3. Smart toe implant An arthrodesis is a surgical procedure to treat hammer toes. The deformed joint is fully removed and the apposing bone ends fused together in a corrected position. The joint will no longer move. The joint closer to the end of the toe will still move. The joint where the toe joins the foot will also continue to move. 1 Fitter Feet For life. 34 North Street. London SW40HD 0207 627 4901 Fitter Feet For Life 1. K-Wire Arthrodesis. Traditionally hammer toe correction is performed by arthrodesis surgery using K-Wires. The procedure is successful in most cases and has been performed for many years. The deformed joint is removed and the bone ends are secured together with a K-wire which protrudes though the tip of the toe. The foot must be kept dry, dressed and the k-wire protected in a post operative shoe for six weeks after the operation. -

Comparison of the Upper and Lower Limbs-A Phylogenetic Concept
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-ISSN: 2279-0853, p-ISSN: 2279-0861.Volume 14, Issue 8 Ver. I (Aug. 2015), PP 14-16 www.iosrjournals.org Comparison of the Upper and Lower Limbs-A Phylogenetic Concept Dr.Vandana Sinam1, Dr.Thonthon Daimei2, I Deven Singh3, N Damayanti Devi4 1.Medical officer,2. Senior Resident,3. Assistant Proffessor,4. Professor and Head, Department of Anatomy Regional Institute of Medical Sciences, Imphal, Manipur Abstract: The upper and lower limbs of the human body are phylogenetically homologues of the forelimbs and hind limbs of the quadrupeds. Primates started lifting of the forelimbs off the ground for various functional adaptations as evolution progressed and this led to the deviation of the forelimbs from lower limbs. With the gradual diversification of the functions, morphological evolution of the two limbs follows closely leading to the differences in upper and the lower limbs in the human. Since the inception of the Anatomy as one of the curriculum in medical subjects, the anatomical position has been termed as one that the body stand erect with the eyes looking straight forward and the two upper limbs hanging by the side of the body with the palm facing forward. Therefore in this position the upper limb looked forward with the palm also accordingly faced forward too whilst with the thumb on the lateral side whilst in the lower limb, the big toe which is homologous to the thumb, is placed on the medial side. The anatomical position in the upper limb is not normally a comfortable position as it is kept in this position with effort.