Fingolimod (Gilenya)
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Glatiramer Acetate
Clinical Policy: Glatiramer Acetate (Copaxone, Glatopa) Reference Number: CP.PHAR.252 Effective Date: 09.01.16 Last Review Date: 05.20 Coding Implications Line of Business: Commercial, HIM, Medicaid Revision Log See Important Reminder at the end of this policy for important regulatory and legal information. Description Glatiramer acetate (Copaxone®, Glatopa®) is a polypeptide. FDA Approved Indication(s) Copaxone and Glatopa are indicated for the treatment of patients with relapsing forms of multiple sclerosis (MS), to include clinically isolated syndrome, relapsing-remitting disease, and active secondary progressive disease, in adults. Policy/Criteria Provider must submit documentation (such as office chart notes, lab results or other clinical information) supporting that member has met all approval criteria. It is the policy of health plans affiliated with Centene Corporation® that Copaxone and Glatopa are medically necessary when the following criteria are met: I. Initial Approval Criteria A. Multiple Sclerosis (must meet all): 1. Diagnosis of one of the following (a, b, or c): a. Clinically isolated syndrome; b. Relapsing-remitting MS; c. Secondary progressive MS; 2. Prescribed by or in consultation with a neurologist; 3. Age ≥ 18 years; 4. If request is for brand Copaxone, member has experienced clinically significant adverse effects to generic glatiramer (including Glatopa) or has contraindication(s) to its excipients; 5. Glatiramer is not prescribed concurrently with other disease modifying therapies for MS (see Appendix D); 6. Dose does not exceed 20 mg per day (1 prefilled syringe per day) or 40 mg three times per week (3 prefilled syringes per week). Approval duration: Medicaid/HIM – 6 months Commercial – 6 months or to the member’s renewal date, whichever is longer B. -

The Change of Fingolimod Patient Profiles Over Time
Journal of Personalized Medicine Article The Change of Fingolimod Patient Profiles over Time: A Descriptive Analysis of Two Non-Interventional Studies PANGAEA and PANGAEA 2.0 Tjalf Ziemssen 1,* and Ulf Schulze-Topphoff 2 1 Zentrum für Klinische Neurowissenschaften, Universitätsklinikum Carl Gustav Carus, D-01307 Dresden, Germany 2 Novartis Pharma GmbH, D-90429 Nuremberg, Germany; [email protected] * Correspondence: [email protected] Abstract: (1) Background: Fingolimod (Gilenya®) was the first oral treatment for patients with relapsing-remitting multiple sclerosis (RRMS). Since its approval, the treatment landscape has changed enormously. (2) Methods: Data of PANGAEA and PANGAEA 2.0, two German real-world studies, were descriptively analysed for possible evolution of patient profiles and treatment behavior. Both are prospective, multi-center, non-interventional, long-term studies on fingolimod use in RRMS in real life. Data of 4229 PANGAEA patients (recruited 2011–2013) and 2441 PANGAEA 2.0 patients (recruited 2015–2018) were available. Baseline data included demographics, RRMS characteristics and disease severity. (3) Results: The mean age of PANGAEA and PANGAEA 2.0 patients was similar (38.8 vs. 39.2 years). Patients in PANGAEA 2.0 had shorter disease duration (7.1 vs. 8.2 years) and fewer relapses in the year before baseline (1.2 vs. 1.6). Disease severity at baseline estimated by Citation: Ziemssen, T.; EDSS and SDMT was lower in PANGAEA 2.0 patients compared to PANGAEA (EDSS difference Schulze-Topphoff, U. The Change of 1.0 points; SDMT difference 3.3 points). (4) Conclusions: The results hint at an influence of changes in Fingolimod Patient Profiles over the treatment guidelines and the label on fingolimod patients profiles over time. -

Medical Review(S) Clinical Review
CENTER FOR DRUG EVALUATION AND RESEARCH APPLICATION NUMBER: 22-527 MEDICAL REVIEW(S) CLINICAL REVIEW Application Type NDA Application Number 22-527 Priority or Standard P Submit Date 12-21-2009 Received Date 12-21-2009 PDUFA Goal Date 9-21-2010 Division / Office FDA/ODE1 Reviewer Name Heather D. Fitter Review Completion Date August 26, 2010 Established Name Fingolimod (Proposed) Trade Name Gilenya Therapeutic Class S1P receptor modulator Applicant Novartis Formulation(s) Oral tablets Dosing Regimen 0.5 mg Indication(s) To reduce the frequency of relapses and delay the progression of disability in relapsing MS Intended Population(s) Relapsing Multiple Sclerosis Template Version: March 6, 2009 Clinical Review Heather D. Fitter, M.D. NDA 22-527 Fingolimod Table of Contents 1 RECOMMENDATIONS/RISK BENEFIT ASSESSMENT......................................... 7 1.1 Recommendation on Regulatory Action ............................................................. 7 1.2 Risk Benefit Assessment.................................................................................... 8 2 INTRODUCTION AND REGULATORY BACKGROUND ........................................ 8 2.1 Product Information ............................................................................................ 9 2.2 Table of Currently Available Treatments for the Proposed Indication................. 9 2.3 Availability of Proposed Active Ingredient in the United States ........................ 12 2.4 Important Safety Issues with Consideration to Related Drugs......................... -

Clinical Policy: Interferon Beta-1B (Betaseron, Extavia)
Clinical Policy: Interferon Beta-1b (Betaseron, Extavia) Reference Number: CP.CPA.331 Effective Date: 06.01.18 Last Review Date: 05.19 Coding Implications Line of Business: Commercial Revision Log See Important Reminder at the end of this policy for important regulatory and legal information. Description Interferon beta-1b (Betaseron®, Extavia®) is an amino acid glycoprotein. FDA Approved Indication(s) Betaseron and Extavia are indicated for the treatment of patients with relapsing forms of multiple sclerosis (MS), to include clinically isolated syndrome, relapsing-remitting disease, and active secondary progressive disease, in adults. Policy/Criteria Provider must submit documentation (such as office chart notes, lab results or other clinical information) supporting that member has met all approval criteria. It is the policy of health plans affiliated with Centene Corporation® that Betaseron and Extavia are medically necessary when the following criteria are met: I. Initial Approval Criteria A. Multiple Sclerosis (must meet all): 1. Diagnosis of one of the following (a, b, or c): a. Clinically isolated syndrome (CIS); b. Relapsing-remitting MS (RRMS); c. Secondary progressive MS (SPMS); 2. Prescribed by or in consultation with a neurologist; 3. Age ≥ 12 years; 4. For Extavia requests, member meets one of the following (a or b): a. If RRMS and age ≥ 18 years: Failure of two of the following at up to maximally indicated doses, unless contraindicated or clinically significant adverse effects are experienced: Aubagio®, Tecfidera®, Gilenya™, Avonex®, Betaseron®, Plegridy®, glatiramer, Copaxone®, Glatopa®, or Rebif®; b. If CIS or SPMS: Failure of two of the following at up to maximally indicated doses, unless contraindicated or clinically significant adverse effects are experienced: Avonex, Betaseron, Plegridy, or Rebif; *Prior authorization is required for all disease modifying therapies for MS 5. -

Comparative Clinical and Cost-Effectiveness of Drug
Table 46: Univariate Sensitivity Analysis Regarding Cost of Relapse Cost per relapse = $1,405 Grima et al.74 ICUR versus Treatment Total Cost Total QALYs glatiramer Sequential ICUR acetate Glatiramer acetate $288,507 11.272 Ref Ref (Copaxone) Interferon beta-1b $299,930 11.376 $109,519 $109,519 (Extavia) Dimethyl fumarate $332,772 11.442 $261,092 $503,474 (Tecfidera) Natalizumab (Tysabri) $459,081 11.580 $554,068 $913,177 Dominated treatments Dominated by interferon Interferon beta-1b $313,300 11.376 $237,687 beta-1b 250 mcg (Betaseron) (Extavia) Dominated by interferon Interferon beta-1a 22 beta-1b 250 mcg $316,087 11.187 Dominated mcg (Rebif) (Extavia) and glatiramer acetate Dominated by interferon Interferon beta-1a beta-1b 250 mcg $319,267 11.167 Dominated (Avonex) (Extavia) and glatiramer acetate Dominated by interferon beta-1b 250 mcg Interferon beta-1a 44 $344,575 11.262 Dominated (Extavia), glatiramer mcg (Rebif) acetate and dimethyl fumarate Dominated by dimethyl Fingolimod (Gilenya) $389,409 11.422 $673,157 fumarate Cost per relapse = $6,402 Karampampa et al.75 Glatiramer acetate $311,927 11.272 Ref Ref (Copaxone) Interferon beta-1b $323,995 11.376 $115,694 $115,694 (Extavia) Dimethyl fumarate $353,243 11.442 $243,695 $448,383 (Tecfidera) Natalizumab (Tysabri) $475,615 11.580 $531,700 $884,714 Dominated treatments Dominated by interferon Interferon beta-1b $337,364 11.395 $243,863 beta-1b 250 mcg (Betaseron) (Extavia) Dominated by interferon Interferon beta-1a 22 beta-1b 250 mcg $340,051 11.190 Dominated mcg (Rebif) (Extavia) -
Analysis of Changes in Disease Modifying Treatment in The
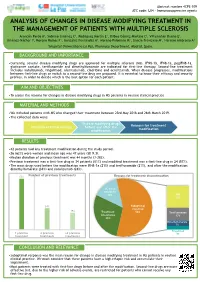
Abstract number 4CPS-109 ATC code: L04 - Immunosuppressive agents ANALYSIS OF CHANGES IN DISEASE MODIFYING TREATMENT IN THE MANAGEMENT OF PATIENTS WITH MULTIPLE SCLEROSIS Arancón Pardo A1, Sobrino Jiménez C1, Rodríguez Martín E1, Bilbao Gómez-Martino C1, Villamañán Bueno E1, Jiménez-Nácher I1, Moreno Ramos F1, González Fernández A1, Moreno Palomino M1, García-Trevijano M1, Herrero Ambrosio A1 1Hospital Universitario La Paz, Pharmacy Department, Madrid, Spain. BACKGROUND AND IMPORTANCE •Currently, several disease modifying drugs are approved for multiple sclerosis (MS). IFNβ-1b, IFNβ-1a, pegIFNβ-1a, glatiramer acetate, teriflunomide and dimethylfumarate are indicated for first-line therapy. Second-line treatment includes natalizumab, fingolimod, alemtuzumab, cladribine and ocrelizumab. When disease progresses, modifications between first-line drugs or switch to a second-line drug are proposed. It is essential to know their efficacy and security profiles, in order to decide which is the best option for each patient. AIM AND OBJECTIVES •To assess the reasons for changes in disease modifying drugs in MS patients in routine clinical practice. MATERIAL AND METHODS •We included patients with MS who changed their treatment between 23rd May 2018 and 26th March 2019. •The collected data were: Disease modifying drugs Reasons for treatment Duration of initial therapy before and after the modification modification RESULTS •42 patients had any treatment modification during the study period. •26 (62%) were women and mean age was 47 years (SD 9.3). •Median duration of previous treatment was 44 months (3-282). •Previous treatment was a first-line drug in 34 patients (81%) and modified treatment was a first-line drug in 24 (57%). -

Patient Focused Disease State and Assistance Programs
Patient Focused Disease State and Assistance Programs Medication Medication Toll-free Brand (Generic) Website number Additional Resources Allergy/Asthma Xolair (omalizumab) xolair.com 1-866-4-XOLAIR lung.org Cardiovascular Pradaxa (dabigatran) pradaxa.com 877-481-5332 heart.org Praluent (alirocumab) praluent.com 844-PRALUENT thefhfoundation.org Repatha (evolocumab) repatha.com 844-REPATHA Tikosyn (dofetilide) tikosyn.com 800-879-3477 Crohn’s Disease Cimzia (certolizumab pegol) cimzia.com 866-4-CIMZIA crohnsandcolitis.com Humira (adalimumab) humira.com 800-4-HUMIRA crohnsforum.com Stelara (ustekinumab) stelarainfo.com 877-STELARA Dermatology Cosentyx (secukinumab) cosentyx.com 844-COSENTYX psoriasis.org Dupixent (dupilumab) dupixent.com 844-DUPIXENT nationaleczema.org Enbrel (etanercept) enbrel.com 888-4-ENBREL Humira (adalimumab) humira.com 800-4-HUMIRA Otezla (apremilast) otezla.com 844-4-OTEZLA Stelara (ustekinumab) stelarainfo.com 877-STELARA Taltz (ixekizumab) taltz.com 800-545-5979 Hematology Aranesp (darbepoetin alfa) aranesp.com 805-447-1000 chemocare.com Granix (filgrastim) granixrx.com 888-4-TEVARX hematology.org Jadenu (deferasirox) jadenu.com 888-282-7630 Neulasta (pegfilgrastim) neulasta.com 800-77-AMGEN Neupogen (filgrastim) neupogen.com 800-77-AMGEN Nivestym (filgrastim) nivestym.com 800-879-3477 Zarxio (filgrastim) zarxio.com 800-525-8747 Zytiga (abiraterone) zytiga.com 800-JANSSEN Hepatitis B Baraclude (entecavir) baraclude.com 800-321-1335 cdc.gov Viread (tenofovir disoproxil viread.com 800-GILEAD-5 hepb.org fumarate) -

COMPARISON of the WHO ATC CLASSIFICATION & Ephmra/Intellus Worldwide ANATOMICAL CLASSIFICATION
COMPARISON OF THE WHO ATC CLASSIFICATION & EphMRA/Intellus Worldwide ANATOMICAL CLASSIFICATION: VERSION June 2019 2 Comparison of the WHO ATC Classification and EphMRA / Intellus Worldwide Anatomical Classification The following booklet is designed to improve the understanding of the two classification systems. The development of the two systems had previously taken place separately. EphMRA and WHO are now working together to ensure that there is a convergence of the 2 systems rather than a divergence. In order to better understand the two classification systems, we should pay attention to the way in which substances/products are classified. WHO mainly classifies substances according to the therapeutic or pharmaceutical aspects and in one class only (particular formulations or strengths can be given separate codes, e.g. clonidine in C02A as antihypertensive agent, N02C as anti-migraine product and S01E as ophthalmic product). EphMRA classifies products, mainly according to their indications and use. Therefore, it is possible to find the same compound in several classes, depending on the product, e.g., NAPROXEN tablets can be classified in M1A (antirheumatic), N2B (analgesic) and G2C if indicated for gynaecological conditions only. The purposes of classification are also different: The main purpose of the WHO classification is for international drug utilisation research and for adverse drug reaction monitoring. This classification is recommended by the WHO for use in international drug utilisation research. The EphMRA/Intellus Worldwide classification has a primary objective to satisfy the marketing needs of the pharmaceutical companies. Therefore, a direct comparison is sometimes difficult due to the different nature and purpose of the two systems. -

The Real-World Patient Experience of Fingolimod and Dimethyl Fumarate
Wicks et al. BMC Res Notes (2016) 9:434 DOI 10.1186/s13104-016-2243-8 BMC Research Notes RESEARCH ARTICLE Open Access The real‑world patient experience of fingolimod and dimethyl fumarate for multiple sclerosis Paul Wicks1* , Lawrence Rasouliyan2, Bo Katic1, Beenish Nafees3, Emuella Flood3 and Rahul Sasané4 Abstract Background: Oral disease-modifying therapies offer equivalent or superior efficacy and greater convenience versus injectable options. Objectives: To compare patient-reported experiences of fingolimod and dimethyl fumarate. Methods: Adult relapsing-remitting multiple sclerosis patients treated with fingolimod or dimethyl fumarate were recruited from an online patient community and completed an online survey about treatment side effects, discon- tinuation, and satisfaction. Results: 281 patients in four groups completed the survey: currently receiving fingolimod (CF, N 61), currently receiving dimethyl fumarate (CDMF, N 129), discontinued fingolimod (DF, N 32) and discontinued= dimethyl fuma- rate (DDMF, N 59). Reasons for treatment= switch were to take oral treatment =(CF: 63.3 %, CDMF: 61.8 %), side effects of prior medication= (CF: 67.3 %, CDMF: 44.1 %) and lack of effectiveness of prior medication (CF: 38.8 %, CDMF: 31.4 %). Main reasons for discontinuation were side effects (DF: 46.9 %, DDMF: 67.8 %) and lack of effectiveness (DF: 25.0 %, DDMF: 15.3 %). CDMF patients had an increased risk of abdominal pain, flushing, diarrhea, and nausea. Treatment satisfaction was highest among CF patients followed by CDMF, DF, and then DDMF patients. Conclusions: Discontinuation was driven by experience of side effects. Patients currently taking dimethyl fumarate were more likely to experience a side effect versus patients currently taking fingolimod. -

Gilenya, INN-Fingolimod
24 September 2015 EMA/CHMP/549382/2015 Committee for Medicinal Products for Human Use (CHMP) Assessment report Gilenya International non-proprietary name: FINGOLIMOD Procedure No. EMEA/H/C/002202/II/0034 Note Variation assessment report as adopted by the CHMP with all information of a commercially confidential nature deleted. 30 Churchill Place ● Canary Wharf ● London E14 5EU ● United Kingdom Telephone +44 (0)20 3660 6000 Facsimile +44 (0)20 3660 5555 Send a question via our website www.ema.europa.eu/contact An agency of the European Union © European Medicines Agency, 2015. Reproduction is authorised provided the source is acknowledged. Table of contents 1. Background information on the procedure .............................................. 5 1.1. Type II variation .................................................................................................. 5 1.2. Steps taken for the assessment of the product ......................................................... 6 2. Scientific discussion ................................................................................ 6 2.1. Introduction......................................................................................................... 6 2.2. Non-clinical aspects .............................................................................................. 8 2.2.1. Ecotoxicity/environmental risk assessment ........................................................... 8 2.2.2. Conclusion on the non-clinical aspects ............................................................... -

Beta Interferons and Glatiramer Acetate for Treatment of Multiple Sclerosis
Clinical Criteria Subject: Beta Interferons and Glatiramer Acetate for Treatment of Multiple Sclerosis Document #: ING-CC-0014 Publish Date: 01/01/201909/23/2019 Status: Revised Last Review Date: 08/17/201808/16/2019 Table of Contents Overview Coding References Clinical criteria Document history Overview This document addresses the use of beta interferon agents and glatiramer acetate agents, injectable disease modifying therapies approved by the Food and Drug Administration (FDA) to treat relapsing forms of multiple sclerosis. Interferon beta-1a agents: • Avonex (interferon beta-1a) • Plegridy (peginterferon beta-1a) • Rebif (interferon beta-1a) Interferon beta-1b agents: • Betaseron (interferon beta-1b) • Extavia (interferon beta-1b) Glatiramer acetate agents: • Copaxone (glatiramer acetate) • Glatopa (glatiramer acetate) Multiple sclerosis is an autoimmune inflammatory demyelinating disease of the central nervous system. Common symptoms of the disease include fatigue, numbness, coordination and balance problems, bowel and bladder dysfunction, emotional and cognitive changes, spasticity, vision problems, dizziness, sexual dysfunction and pain. Multiple sclerosis can be subdivided into four phenotypes: clinically isolated syndrome (CIS), relapsing remitting (RRMS), primary progressive (PPMS) and secondary progressive (SPMS). Relapsing multiple sclerosis (RMS) is a general term for all relapsing forms of multiple sclerosis including CIS, RRMS and active SPMS. The treatment goal for multiple sclerosis is to prevent relapses and progressive worsening of the disease. Currently available disease- modifying therapies (DMT) are most effective for the relapsing-remitting form of multiple sclerosis and less effective for secondary progressive decline. DMT include injectable agents, infusion therapies and oral agents. The American Academy of Neurology (AAN) guidelines suggest starting disease-modifying therapy in individuals with relapsing forms of multiple sclerosis with recent clinical relapses or MRI activity. -

Pathophysiology and Imaging Diagnosis of Demyelinating Disorders
brain sciences Pathophysiology and Imaging Diagnosis of Demyelinating Disorders Edited by Evanthia Bernitsas Printed Edition of the Special Issue Published in Brain Sciences www.mdpi.com/journal/brainsci Pathophysiology and Imaging Diagnosis of Demyelinating Disorders Special Issue Editor Evanthia Bernitsas MDPI • Basel • Beijing • Wuhan • Barcelona • Belgrade Special Issue Editor Evanthia Bernitsas Wayne State University School of Medicine USA Editorial Office MDPI St. Alban-Anlage 66 Basel, Switzerland This edition is a reprint of the Special Issue published online in the open access journal Brain Sciences (ISSN 2076-3425) in 2017 (available at: http://www.mdpi.com/journal/brainsci/special issues/ multiple sclerosis demyelinating). For citation purposes, cite each article independently as indicated on the article page online and as indicated below: Lastname, F.M.; Lastname, F.M. Article title. Journal Name Year, Article number, page range. First Edition 2018 ISBN 978-3-03842-943-2 (Pbk) ISBN 978-3-03842-944-9 (PDF) Articles in this volume are Open Access and distributed under the Creative Commons Attribution (CC BY) license, which allows users to download, copy and build upon published articles even for commercial purposes, as long as the author and publisher are properly credited, which ensures maximum dissemination and a wider impact of our publications. The book taken as a whole is c 2018 MDPI, Basel, Switzerland, distributed under the terms and conditions of the Creative Commons license CC BY-NC-ND (http://creativecommons.org/licenses/by-nc-nd/4.0/). Table of Contents About the Special Issue Editor ...................................... v Preface to ”Pathophysiology and Imaging Diagnosis of Demyelinating Disorders” ......