Children and Their Vision
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
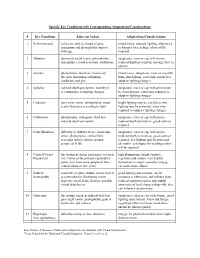
Specific Eye Conditions with Corresponding Adaptations/Considerations
Specific Eye Conditions with Corresponding Adaptations/Considerations # Eye Condition Effect on Vision Adaptations/Considerations 1 Achromotopsia colors are seen as shades of grey, tinted lenses, reduced lighting, alternative nystagmus and photophobia improve techniques for teaching colors will be with age required 2 Albinism decreased visual acuity, photophobia, sunglasses, visor or cap with a brim, nystagmus, central scotomas, strabismus reduced depth perception, moving close to objects 3 Aniridia photophobia, field loss, vision may tinted lenses, sunglasses, visor or cap with fluctuate depending on lighting brim, dim lighting, extra time required to conditions and glare adapt to lighting changes 4 Aphakia reduced depth perception, inability to sunglasses, visor or cap with a brim may accommodate to lighting changes be worn indoors, extra time required to adapt to lighting changes 5 Cataracts poor color vision, photophobia, visual bright lighting may be a problem, low acuity fluctuates according to light lighting may be preferred, extra time required to adapt to lighting changes 6 Colobomas photophobia, nystagmus, field loss, sunglasses, visor or cap with a brim, reduced depth perception reduced depth perception, good contrast required 7 Color Blindness difficulty or inability to see colors and sunglasses, visor or cap with a brim, detail, photophobia, central field reduced depth perception, good contrast scotomas (spotty vision), normal required, low lighting may be preferred, peripheral fields alternative techniques for teaching colors -

Hereditary Reversion Pigmentation of the Eyelids with Heterochromia of the Iris
874 LEE MASTEN FRANCIS enucleated. The following report on the Other cells were round with hyper- specimen was submitted from the New chromatic nuclei; while scattered thruout York State Institute for the Study of the tumor were large deeply staining Malignant Diseases: cells with one or two nuclei but free from The gross appearance of a cross sec- pigment. There were apparently two tion of the eye shows a tumor lying in types of pigmented cells, the one a large the lower temporal quadrant of the eye, irregular cell with long protoplasmic evidently springing from the choroid processes densely filled with fine yellow- near the margin of the optic disc. This ish granules, evidently chromatophores. tumor measured 15x10 mm. and was The other type of pigmented cell was a slightly nodular irregular ovoid tumor. evidently a tumor cell of the type men- The surface appeared smooth, was dark tioned above but containing fewer gran- gray in color and was of a soft consist- ules than the chromatophores. Thruout ency. The retina was markedly detached the tumor were small areas of hemor- and contained a clear serous fluid. Cross rhage and between the cells could be section of the tumor mass showed a demonstrated here and there, free pig- deeply pigmented homogeneous surface. ment granules. Microscopically, the tumor varied as From this picture, we would make a to the cellular constituents. There were diagnosis of malignant melanoma, fre- areas showing many pigment cells and quently called melanosarcoma, but by other areas almost free from the same. some authorities considered as melanotic The tumor was very vascular showing many fine capillaries around which in carcinoma. -

A Patient & Parent Guide to Strabismus Surgery
A Patient & Parent Guide to Strabismus Surgery By George R. Beauchamp, M.D. Paul R. Mitchell, M.D. Table of Contents: Part I: Background Information 1. Basic Anatomy and Functions of the Extra-ocular Muscles 2. What is Strabismus? 3. What Causes Strabismus? 4. What are the Signs and Symptoms of Strabismus? 5. Why is Strabismus Surgery Performed? Part II: Making a Decision 6. What are the Options in Strabismus Treatment? 7. The Preoperative Consultation 8. Choosing Your Surgeon 9. Risks, Benefits, Limitations and Alternatives to Surgery 10. How is Strabismus Surgery Performed? 11. Timing of Surgery Part III: What to Expect Around the Time of Surgery 12. Before Surgery 13. During Surgery 14. After Surgery 15. What are the Potential Complications? 16. Myths About Strabismus Surgery Part IV: Additional Matters to Consider 17. About Children and Strabismus Surgery 18. About Adults and Strabismus Surgery 19. Why if May be Important to a Person to Have Strabismus Surgery (and How Much) Part V: A Parent’s Perspective on Strabismus Surgery 20. My Son’s Diagnosis and Treatment 21. Growing Up with Strabismus 22. Increasing Signs that Surgery Was Needed 23. Making the Decision to Proceed with Surgery 24. Explaining Eye Surgery to My Son 25. After Surgery Appendix Part I: Background Information Chapter 1: Basic Anatomy and Actions of the Extra-ocular Muscles The muscles that move the eye are called the extra-ocular muscles. There are six of them on each eye. They work together in pairs—complementary (or yoke) muscles pulling the eyes in the same direction(s), and opposites (or antagonists) pulling the eyes in opposite directions. -

Understanding Corneal Blindness
Understanding Corneal Blindness The cornea copes very well with minor injuries or abrasions. If the highly sensitive cornea is scratched, healthy cells slide over quickly and patch the injury before infection occurs and vision is affected. If the scratch penetrates the cornea more deeply, however, the healing process will take longer, at times resulting in greater pain, blurred vision, tearing, redness, and extreme sensitivity to light. These symptoms require professional treatment. Deeper scratches can also cause corneal scarring, resulting in a haze on the cornea that can greatly impair vision. In this case, a corneal transplant may be needed. Corneal Diseases and Disorders that May Require a Transplant Corneal Infections. Sometimes the cornea is damaged after a foreign object has penetrated the tissue, such as from a poke in the eye. At other times, bacteria or fungi from a contaminated contact lens can pass into the cornea. Situations like these can cause painful inflammation and corneal infections called keratitis. These infections can reduce visual clarity, produce corneal discharges, and perhaps erode the cornea. Corneal infections can also lead to corneal scarring, which can impair vision and may require a corneal transplant. Fuchs' Dystrophy. Fuchs' Dystrophy occurs when endothelial cells gradually deteriorate without any apparent reason. As more endothelial cells are lost over the years, the endothelium becomes less efficient at pumping water out of the stroma (the middle layers of the cornea). This causes the cornea to swell and distort vision. Eventually, the epithelium also takes on water, resulting in pain and severe visual impairment. Epithelial swelling damages vision by changing the cornea's normal curvature, and causing a sightimpairing haze to appear in the tissue. -

WSPOS Worldwide Webinar 16: Amblyopia - How and When
Answers to Audience Questions - WSPOS Worldwide Webinar 16: Amblyopia - How and When WWW 16 Panellists Anna Horwood Celeste Mansilla David Granet Krista Kelly Lionel Kowal Susan Cotter Yair Morad Anna Horwood (AH), Celeste Mansilla (CM), Krista Kelly (KK), Lionel Kowal (LK), Susan Cotter (SC), Yair Morad (YM) 1. How do you maintain attained iso visual acuity after successful amblyopia treatment? AH: Intermittent monitoring. If they have regressed previously, I might carry on very intermittent occlusion (an hour or two a week) until I was sure it was stable. CM: With gradual and controlled reduction of the treatment, for example: if the patient had 1 hour of patch per day, I leave it with 1 hour 3 times a week during a month. I do a check and if the visual acuity was maintained, I lower patches to 2 times a week. I keep checking and going down like this until I suspend the treatment. If at any time I detect worsening visual acuity, I return to the previous treatment. SC: Best way is attainment of normal binocular vision. I do not worry about ansiometropic amblyopes who have random dot stereopsis post-treatment. If have constant unilateral strabismus, I can do some limited part-time patching, decreasing patching dosage over time given no regression of VA. YM: repeat examination every 6 months. If I see regression, I will prescribe patching for 30 min a day. 2. How do you plan for very dense amblyopes? AH: I very rarely see them because, with screening, they are picked up early and usually do well. -

Hyperopia Hyperopia
Hyperopia Hyperopia hyperopia hyperopia • Farsightedness, or hyperopia, • Farsightedness occurs if your eyeball is too as it is medically termed, is a short or the cornea has too little curvature, so vision condition in which distant objects are usually light entering your eye is not focused correctly. seen clearly, but close ones do • Its effect varies greatly, depending on the not come into proper focus. magnitude of hyperopia, the age of the individual, • Approximately 25% of the the status of the accommodative and general population is hyperopic (a person having hyperopia). convergence system, and the demands placed on the visual system. By Judith Lee and Gretchyn Bailey; reviewed by Dr. Vance Thompson; Flash illustration by Stephen Bagi 1. Cornea is too flap. hyperopia • In theory, hyperopia is the inability to focus and see the close objects clearly, but in practice many young hyperopics can compensate the weakness of their focusing ability by excessive use of the accommodation functions of their eyes. Hyperopia is a refractive error in • But older hyperopics are not as lucky as them. By which parallel rays of light aging, accommodation range diminishes and for 2. Axial is too short. entering the eye reach a focal older hyperopics seeing close objects becomes point behind the plane of the retina, while accommodation an impossible mission. is maintained in a state of relaxation. 1 Amplitude of Accommodation hyperopia Maximum Amplitude= 25-0.4(age) • An emmetropic eye for reading and other near Probable Amplitude= 18.5-.3(age) work, at distance of 16 in (40cm), the required amount of acc. -

Orthoptic Department Information Sheet
Are there any complications? Keratoconus is a rare condition where the cornea becomes thinner and cone shaped. This results in increasingly large amounts of astigmatism resulting in poor vision which is not fully corrected by glasses. Contact numbers Keratoconus usually requires contact lenses Orthoptist: for clear vision, and may eventually result in needing surgery on the cornea. St Richard’s A Keratometer is an instrument sometimes 01243 831499 used to measure the curvature of the cornea. By focusing a circle of light on the Southlands cornea and measuring its reflection, it is 01273 446077 possible to tell the exact curvature of the cornea’s surface. A more sophisticated procedure called corneal topography may be done in some cases to get an even more detailed idea of Orthoptic Department the shape of the cornea. Information Sheet We are committed to making our publications as accessible as possible. If you need this document in an alternative format, for example, large print, Braille or a language other than Astigmatism English, please contact the Communications Office by email: [email protected] St Richard’s Hospital or speak to a member of the department. Spitalfield Lane Chichester West Sussex PO19 6SE www.westernsussexhospitals.nhs.uk Southlands Hospital Department: Orthoptics Upper Shoreham Road Issue date: March 2018 Shoreham-by-Sea Review date: March 2020 West Sussex BN43 6TQ Leaflet Ref: ORT03 This leaflet is intended to answer some of What are the signs and symptoms? These eye drops stop the eyes from the questions of patients or carers of Children are good at adapting to blurred focussing for a few hours so that the patients diagnosed with astigmatism under vision and will often not show any signs of Optometrist can get an accurate reading. -

Surgical Options in Managing Convergent Strabismus Fixus Related to High Myopia
Ophthalmol Ina 2015;41(2):107-115 107 Case Report Surgical Options in Managing Convergent Strabismus Fixus Related to High Myopia Jessica Zarwan, Gusti G Suardana, Anna P Bani Department of Ophthalmology, Faculty of Medicine, Indonesia University Cipto Mangunkusumo Hospital, Jakarta ABSTRACT Background: Convergent strabismus fixus is a condition in which one or both eyes are anchored in extreme adduction. This condition is caused by superotemporal herniation of the enlarged globe from the muscle cone through the space between the superior and lateral rectus muscle. It is commonly related to high myopia. Recently, transposition type procedure which unite the superior and lateral rectus muscles were proposed as the treatment of choice in this condition. However, there is no clear consensus regarding the best surgical procedure in convergent strabismus fixus. This case series reported three rare cases of convergent strabismus fixus related to high myopia and highlight the option of surgical procedure that can be done in these cases. Case Illustration: Three patients presented with convergent strabismus fixus of both eyes with history of bilateral high myopia since childhood. All patients showed Krimsky tests of >95∆ET preoperatively, with medial displacement of superior rectus and inferior displacement of lateral rectus of both eyes in all patients on orbital imaging. The bilateral Yokoma procedure both resulted in an orthophoric postoperative result with marked improvement in abduction and elevation. The hemi-Jensen also showed a significant improvement of over than 60∆ on the operated eye, resorting it to a central position during primary gaze. Conclusion: Convergent strabismus fixus is a rare condition and frequently associated with high myopia. -

Strabismus, Amblyopia & Leukocoria
Strabismus, Amblyopia & Leukocoria [ Color index: Important | Notes: F1, F2 | Extra ] EDITING FILE Objectives: ➢ Not given. Done by: Jwaher Alharbi, Farrah Mendoza. Revised by: Rawan Aldhuwayhi Resources: Slides + Notes + 434 team. NOTE: F1& F2 doctors are different, the doctor who gave F2 said she is in the exam committee so focus on her notes Amblyopia ● Definition Decrease in visual acuity of one eye without the presence of an organic cause that explains that decrease in visual acuity. He never complaints of anything and his family never noticed any abnormalities ● Incidence The most common cause of visual loss under 20 years of life (2-4% of the general population) ● How? Cortical ignorance of one eye. This will end up having a lazy eye ● binocular vision It is achieved by the use of the two eyes together so that separate and slightly dissimilar images arising in each eye are appreciated as a single image by the process of fusion. It’s importance 1. Stereopsis 2. Larger field If there is no coordination between the two eyes the person will have double vision and confusion so as a compensatory mechanism for double vision the brain will cause suppression. The visual pathway is a plastic system that continues to develop during childhood until around 6-9 years of age. During this time, the wiring between the retina and visual cortex is still developing. Any visual problem during this critical period, such as a refractive error or strabismus can mess up this developmental wiring, resulting in permanent visual loss that can't be fixed by any corrective means when they are older Why fusion may fail ? 1. -

Blue Light and Your Eyes
Blue Light and Your Eyes What is blue light? 211 West Wacker Drive, Suite 1700 Sunlight is made up of red, orange, yellow, green, blue, indigo and Chicago, Illinois 60606 violet light. When combined, it becomes the white light we see. 800.331.2020 Each of these has a different energy and wavelength. Rays on the PreventBlindness.org red end have longer wavelengths and less energy. On the other end, blue rays have shorter wavelengths and more energy. Light that looks white can have a large blue component, which can expose the eye to a higher amount of wavelength from the blue end of the spectrum. Where are you exposed to blue light? The largest source of blue light is sunlight. In addition, there are many other sources: • Fluorescent light • CFL (compact fluorescent light) bulbs • LED light • Flat screen LED televisions • Computer monitors, smart phones, and tablet screens Blue light exposure you receive from screens is small compared to the amount of exposure from the sun. And yet, there is concern over the long-term effects of screen exposure because of the close proximity of the screens and the length of time spent looking at them. According to a recent NEI-funded study, children’s eyes absorb more blue light than adults from digital device screens. This publication is copyrighted. This sheet may be reproduced—unaltered in hard print (photocopied) for educational purposes only. The Prevent Blindness name, logo, telephone number and copyright information may not be omitted. Electronic reproduction, other reprint, excerption or use is not permitted without written consent. -

Astigmatism Astigmatism Is One of the Most Common Vision Problems, But
Astigmatism Astigmatism is one of the most common vision problems, but most people don't know what it is. Many people are relieved to learn that astigmatism is not an eye disease. Like nearsightedness and farsightedness, astigmatism is a type of refractive error – a condition related to the shape and size of the eye that causes blurred vision. In addition to blurred vision, uncorrected astigmatism can cause headaches, eyestrain and make objects at all distances appear distorted. Astigmatism signs and symptoms If you have only a small amount of astigmatism, you may not notice it at all, or you may have only mildly blurred or distorted vision. But even small amounts of uncorrected astigmatism can cause headaches, fatigue and eyestrain over time. Astigmatism usually develops in childhood. A study at the Ohio State University School of Optometry found that more than 28% of schoolchildren have astigmatism. Children may be even more unaware of the condition than adults, and they may also be less likely to complain of blurred or distorted vision. But astigmatism can cause problems that interfere with learning, so it's important to have your child’s eyes examined at regular intervals during their school years. What causes astigmatism? Usually, astigmatism is caused by an irregularshaped cornea, the clear front surface of the eye. In astigmatism, the cornea isn’t perfectly round, but instead is more football or eggshaped. In some cases, astigmatism may be caused by an irregularshaped lens inside the eye. In most astigmatic eyes, the irregular shape of the cornea or lens causes light rays to form two distorted images in the back of the eye, rather than a single clear one. -

Eyemed Blue Light
BLUE LIGHT: FREQUENTLY ASKED QUESTIONS From ZZZs to disease, the blue light battle is on It’s indisputable: our eyes are overexposed to digital devices like never before. And in the background hides potentially harmful blue light that may affect our sleep, or even cause long-term vision issues. But, here’s some good news — you can act now to potentially minimize vision issues later with advanced lens filtering technology formulated to guard your eyes. Q: WHAT IS BLUE LIGHT? A: Blue light is a natural part of the light spectrum visible to the human eye; it can come from fluorescent lighting, electronic screens, and of course, the sun. By day, blue light can be associated with boosted mood and attention, but by night, it can be a culprit of interrupted sleep. 1 Q: HOW DOES BLUE LIGHT INTERRUPT SLEEP? A: Researchers know that exposure to light at night suppresses the secretion of melatonin, a hormone that tells us when it is time to sleep. And an extended lack of deep sleep has been linked to depression and a decline in the body’s ability to fight off certain diseases. 1 Q: CAN BLUE LIGHT EXPOSURE CAUSE LONG-TERM DAMAGE TO MY EYESIGHT? A: In addition to disrupting sleep, blue light has been found to contribute to retinal stress, which could lead to an early onset of age-related macular degeneration (AMD).2 Macular degeneration deteriorates healthy cells within the macula, creating a loss of central vision that may impact reading, writing, driving, color perception and other cognitive functions. In serious cases, blindness can occur.