“SMART” STUDY District Umerkot Sindh, Pakistan
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

(Ppr) Infection in Sindh Province of Pakistan- a One Year Study
ALI ET AL (2019), FUUAST J.BIOL., 9(1): 149-157 PREVALENCE OF PESTE DES PETITS RUMINANTS (PPR) INFECTION IN SINDH PROVINCE OF PAKISTAN- A ONE YEAR STUDY SYED NOMAN ALI1,2, SHAHID ALI KHAN3, MASOOD VANDIAR4, RIASAT WASEE ULLAH5AND SHAHANA UROJ KAZMI6 1Livestock Department, Government of the Sindh 2Department of Agriculture & Agribusiness Management, University of Karachi, Pakistan. 3Food and Agriculture Organization of the United Nations, Islamabad Pakistan. ([email protected]). 4Central Veterinary Diagnostics Laboratory, Tando Jam. ([email protected]) 5Veterinary Research Institute, Lahore ([email protected]) 6Department of Microbiology and Immunology, Dadabhoy University (DIHE) & the University of Karachi, Pakistan ([email protected]) Corresponding author email: [email protected] الخہص وموجدہۺررسیچۺاپاتسکنۺےکۺوصہبۺدنسھۺںیمۺرکبویںۺاورۺڑیھبوںۺںیمۺاپےئۺوایلۺامیبریۺاکاٹ (PPR) یکۺوموجدیگ،ۺاابسبۺاورۺرٹنکولۺرکےنۺےکۺاکرۺآدمۺرطےقیۺولعممۺرکےنۺےکۺ ےئلۺیکۺیئگۺےہ۔ۺسجۺےکۺدورانۺایسۺامیبریۺیکۺ۷۴۸ۺۺوابء (Outbreaks)اکۺاجزئہۺایلۺایگۺوجۺوصہبۺدنسھۺےکۺ۹۲ۺںیمۺےسۺ۶۲االضعۺںیمۺاپیئۺیئگۺبسۺےسۺزایدہۺوابءۺ۱۵.۷۲ۺدصیفۺایٹمریۺعلضۺ ںیمۺاورۺبسۺےسۺمکۺرعےصۺیکۺوابءۺرمعۺوکٹۺعلضۺںیمۺراکیرڈۺیکۺیئگۺوجۺہکۺ ۵ۺدنۺیھتۺاسۺےکۺالعوہۺےبملۺرعہصۺیکۺامیبریۺﻻڑاکہنۺںیمۺاپیئۺیئگۺوجہک ۶۲ۺدنۺیھت۔ۺۺامیبریۺیکۺاشنوینںۺںیمۺمسجۺےکۺ درہجۺرحاتۺںیمۺااضہفF ۶ .۷۰۱ےسF ۲ .۲۰۱راکیرڈۺایکۺایگ۔ۺآوھکنںۺیکۺوسزش،ۺآوھکنںۺاورۺانکۺےسۺاگڑیۺرموطتب،ۺاھکیسنۺاورۺدتسۺاپےئۺےئگ،ۺہنمۺںیمۺوسمڑوںۺرپۺﻻلۺوسنجۺ ےکۺاشننۺےکۺاسھتۺزابنۺاورۺاگولںۺرپۺیھبۺوسنجۺاورۺزمخۺےکۺاشننۺاپےئۺےئگ۔ ELISAےکۺےجیتنۺرپ ANOVA -

National Plantation Drive QUICK FACTS Cities and Villages
level of air pollution in the National Plantation Drive QUICK FACTS cities and villages. Pakistan is one of the youngest and fastest Duration: 2020 - 2021 Implementing partners: Daraz Pakistan , Shan Foods developing countries of the world. Pvt Limited Karachi is among the most polluted cities in the Location: Karachi, Sindh world. The air of the city is polluted with high Funding partners: Daraz Pakistan, Shan Foods levels of lead and cadmium that pose a grave [email protected] risk to public health, says a recent study that also points out that the average concentration of these trace metals found in residential areas of Karachi is higher than those found in Delhi and Beijing. In another environmental study, the research team has found that Karachi, Pakistan, holds the world’s title for ozone. Of the nearly 300 measurements collected over 1 year, roughly a third exceeded what the researchers considered a “harmful” threshold for ozone, which can lead to smog. UNAP is planning a project of plantation and forestation in the province of Sindh. It will be a contribution to SDG 13 (Climate Action) which aims to conserve and restore the use of terrestrial ecosystems such as forests, wetlands, drylands and mountains by 2020. Halting deforestation is also vital to mitigating the impact of climate change. It calls for action to reduce the high Page | 1 UNAP partners with people at all levels of society to help build nations that can withstand crisis, and drive and sustain the kind of growth that improves the quality of life for everyone. Programme Outputs • Considering the land and forest situation in Sindh, especially the urban area of Karachi, a plantation project is planned to improve the environment and ecosystem of Karachi and Umerkot District, which is currently under the threat of a major environment threatening factor: air By 2020, ensure the conservation, pollution. -

Weekly Field Epidemiology Report
Federal Disease Surveillance and Response Unit Field Epidemiology & Disease Surveillance Division National Institute of Health (NIH) Islamabad WEEKLY FIELD EPIDEMIOLOGY REPORT Volume 2 Issue 48 Nov 25 - Dec 01, 2019 Date: December 12, 2019 Provincial Technical Officers and fellows of FELTP PDSRUs/RDSRUs. In week 48 of 2019, no new case was assigned at the Disease Surveillance, Response Units reported. (DSRU’s) are working with provincial, and district health Diphtheria Surveillance: authorities on event based disease surveillance and During 2018 total 464 suspected cases of Diphtheria were outbreak response. reported. Total 544 cases reported in 2019 including 11 new DSRUs are sharing the disease surveillance data, case reported last week. outbreak reports and activities of FELTP fellows to the Dengue Surveillance: Federal Disease Surveillance and Response Unit In 2018 total 3204 Dengue cases were reported, from Sindh (FDSRU) at the Field Epidemiology and Disease (2088) while in 2019 total 24,336 cases have been reported Surveillance Division (FEDSD) National Institute of so far. In week 48, 2019, Punjab (62), KP (11), Baluchistan Health (NIH) Islamabad on weekly basis. (45), No report received from KP Merged Areas, ICT, KP, Sindh & AJK. Inside Issues Page No. CCHF Surveillance: Diphtheria /Dengue/ CCHF Surveillance 1 XDR/MDR-Typhoid Surveillance Karachi / In 2018 total 63 CCHF (suspected and confirmed) cases 1-5 Hyderabad Sindh were reported from DSRUs and 75 cases have been reported TVC campaign Sind and AEFI Surveillance 5-6 in 2019. -

RELIEF AREA VISIT to PAKISTAN 13Th – 26Th JUNE 2013 1
RELIEF AREA VISIT TO PAKISTAN 13th – 26th JUNE 2013 1. Introduction and acknowledgements The Anglican Alliance brings together development, relief and advocacy across the Anglican Communion. We were established as an initiative of the Archbishop of Canterbury and the Anglican Communion, starting our operations in January 2011 with a series of global consultations with partner Churches and agencies. These consultations identified capacity- building as the priority in our relief work. The provision of training schemes and tools would be developed with local Churches and agencies working with communities in disaster-prone areas. Furthermore, it was decided that one focus for this work should be on the preparedness stage, aimed at mobilising Churches and communities to take preventive measures before disasters strike. For the last three monsoon seasons Pakistan has been severely affected by heavy rain and floods. The Diocese of Hyderabad was particularly hard-hit in 2011. It covers Sindh Province, excluding Karachi which forms its own diocese. Unusual rain patterns and unpredictable weather conditions have made people fear that floods might come at any time during the year. Furthermore, there is a poor weather forecast for the 2013 monsoon season. To encourage the communities to be prepared before the oncoming monsoons, the Alliance engaged in a collaborative process to produce a resource that could be used by the community for discussion and mobilisation in preparation for flooding. Through consultation we developed a large cloth book, measuring approximately 1m2, made from a very durable and high quality nylon fabric (made from recycled plastic bottles). Drawing from more high level publications, we developed a series of brightly-coloured, culturally-appropriate drawings, with simple messaging and discussion points written in Urdu on alternate pages. -

PESA-DP-Hyderabad-Sindh.Pdf
Rani Bagh, Hyderabad “Disaster risk reduction has been a part of USAID’s work for decades. ……..we strive to do so in ways that better assess the threat of hazards, reduce losses, and ultimately protect and save more people during the next disaster.” Kasey Channell, Acting Director of the Disaster Response and Mitigation Division of USAID’s Office of U.S. Foreign Disas ter Ass istance (OFDA) PAKISTAN EMERGENCY SITUATIONAL ANALYSIS District Hyderabad August 2014 “Disasters can be seen as often as predictable events, requiring forward planning which is integrated in to broader de velopment programs.” Helen Clark, UNDP Administrator, Bureau of Crisis Preven on and Recovery. Annual Report 2011 Disclaimer iMMAP Pakistan is pleased to publish this district profile. The purpose of this profile is to promote public awareness, welfare, and safety while providing community and other related stakeholders, access to vital information for enhancing their disaster mitigation and response efforts. While iMMAP team has tried its best to provide proper source of information and ensure consistency in analyses within the given time limits; iMMAP shall not be held responsible for any inaccuracies that may be encountered. In any situation where the Official Public Records differs from the information provided in this district profile, the Official Public Records should take as precedence. iMMAP disclaims any responsibility and makes no representations or warranties as to the quality, accuracy, content, or completeness of any information contained in this report. Final assessment of accuracy and reliability of information is the responsibility of the user. iMMAP shall not be liable for damages of any nature whatsoever resulting from the use or misuse of information contained in this report. -

PAKISTAN-SINDH August 2019 – Projection Until December 2019 Report # 0001 | Issued in September 2019
IPC ACUTE MALNUTRITION ANALYSIS PAKISTAN-SINDH August 2019 – Projection until December 2019 Report # 0001 | Issued in September 2019 Key Figures August 2019 SAM* 365,209 Number of cases 1,000,458 MAM* Number of 6-59 months children acutely 635,249 Number of cases malnourished IN NEED OF TREATMENT GAM* 1,000,458 Number of cases How Severe, How Many and When – Acute malnutrition is a major public health problem in all the 8 drought affected districts in the Sindh province. Two districts in the province have extremely critical levels (IPC AMN Phase 5) of acute malnutrition– i.e. about every third child in these districts is suffering from acute malnutrition. Six other districts have critical levels (IPC AMN Phase 4) of acute malnutrition. Although the 6 districts are classified as in IPC AMN Phase 4, 2 of them have acute malnutrition closer to IPC AMN Phase 5. Where – Among the 8 drought affected districts notified by Govt. of Sindh in 2018, the districts with extremely critical levels of acute malnutrition are namely Tharparkar and Umerkot. Six other districts such as Jamshoro, Kambar Shahdadkot, Badin, Dadu, Sanghar, and Thatta are classified as being in IPC AMN Phase 4. Of these 6 districts, 2 of them, i.e. Kambar Shahdadkot and Badin, have acute malnutrition levels very close to IPC AMN Phase 5. Why – The major factors contributing to acute malnutrition include very poor quality and quantity of food, high food insecurity, poor sanitation coverage, and high incidence of low birthweight. Additionally, exclusive breastfeeding and access to safe drinking water are also of concern in several districts. -

Acute Malnutrition Situation in Jamshoro, Tharparkar and Umerkot Districts in Sindh
Acute Malnutrition Situation in Jamshoro, Tharparkar and Umerkot Districts in Sindh Results of IPC Acute Malnutrition Analysis IPC Global Partners With the support of OBJECTIVES OF IPC ACUTE MALNUTRITION ANALYSIS IN SINDH . Classify the areas (Jamshoro, Umerkot and Tharparkar) based on the prevalence of acute malnutrition . Identify major contributing factors to acute malnutrition . Provide actionable knowledge by consolidating wide-ranging evidence on acute malnutrition and contributing factors for response planning METHODS AND PROCESS (1) • Globally, three scales of IPC classification are being used at present: . IPC for Acute Food Insecurity (IPC AFI), . IPC for Chronic Food Insecurity (IPC CFI) and . IPC for Acute Malnutrition (IPC AMN) • Outcome indicator for IPC AMN: GAM by WHZ (Weight for Height) or GAM by MUAC of children age 6-59 months • 5 phases in IPC AMN METHODS & PROCESSES (2) • The data on outcome indicator GAM (MUAC) was taken from Livelihood and Food Security Assessment (LFSA) conducted in April/May 2017. • For other indicators/contributing factors, – SMART nutrition surveys conducted by UNICEF and partners in the targeted districts, – LFSA, MICS, PSLM, and other national surveys were used as the main sources of information in the analysis. • Experts and analysts on nutrition, health and food security from Pakistan with the support from IPC Global (Rome) and Regional (Bangkok) team carried out the analysis • The experts were representatives of . Sindh Govt (Planning & Development Department, Nutrition Support Program, PDMA, Bureau of Statistics, Livestock Department); . Federal Government (Ministry of Planning, Development & Reform, Ministry of National Food Security & Research, Pakistan Agriculture Research Centre); . UN organizations (FAO, WFP, UNICEF, WHO); and . -

Organizational Presence in Union Councils of Sindh - ER - Floods 2011
Organizational presence in Union Councils of Sindh - ER - Floods 2011 Gilgit Baltistan China ! ! ! ! ! ! ! ! ! !! ! ! !! Khyber Pakhtun! khwa !! ! ! Azad Kashmi!r! Disputed Territory Afghanistan Fata ! 4 Punjab Tangwani Kashmore Thul Balochistan Kashmore India Jacobabad Jacobabad Iran Ubauro Kanhdkot Sindh Shikarpur Garhi Khairo Khanpur (Shikarpur) Ghotki Arabian sea Shahdadkot Shikarpur Qubo Saeed Khan Lakhi Daharki Garhi Yasin Pano Aqil Miro Khan Ghotki Ratodero Sukkur Mirpur Mathelo Kingri Qambar Shahdadkot Rohri Kambar Ali Khan Larkana Khairpur Khangarh Larkana Gambat Warah Bakrani Sukkur Kot Diji Salehpat Dokri Sobodhero Mehar Khairpur Nathan Shah Kandiaro Mirwah Ghulam Shah Bagrani Saeedpur Bhiria Naushahro Feroze Dadu Dadu Naushahro Feroze Faiz Ganj Khairpur Moro Nara Johi Kazi Ahmed Daur Shaheed Benazirabad Nawabshah Sehwan Sinjhoro Barhoon Sakrand Shahdadpur Sanghar Ashgarabad Sinjhoro Sindh Jaffar Khan Laghari Kurkali Jhatia Jhol Khipro Hala Manik ThaheemSyes Sughatullah Shaheed Manjhand Khori Tando Adam Sanghar Hatungo Matiari Jan Nawaz Ali Jamshoro Jhando Mari Matiari Dassori Khahi Mirabad Mirpur Khas Pithoro Thano Bula Khan Kotri Shadi pali Pithoro Saabho Qasimabad Tando Allah Yar Tando Allah Yar Umerkot Hyderabad City Hyderabad Sanjar Chang Dengan Dad Jarwar Samaro Umerkot Hyderabad Kot Ghulam Muhammad Latifabad MMirir pImuamr B uKx Hhadai Bsux Burgury padhario Tando Muhammad Khan Saeed Khan Lund Digri Chachro Matli Sufan Shah Kunri Mulakatyar Mir Khuda Buksh Saeed Matto Lakhat Tando Jan Mohammad Karachi City Thatta Malir -

COVID-19 EMERGENCY RESPONSE Daily Situation Report
COVID-19 EMERGENCY RESPONSE Daily Situation Report- April 13, 2020 Sindh Rural Support Organizaiton (SRSO) SRSO Complex, Shikarpur Road, Sukkur (Sindh), Pakistan, Ph.#: 071-56271820 Website: www.srso.org.pk Daily Situation Report – April 13, 2020 All the cities of Sindh are locked down. Daily wagers faced much difficulties to meet their ends. In such a pandemic and lockdown situation poor people of the community cannot afford their basic needs of life. In this situation, the Community didn’t leave alone to the poor daily wagers and elderly people of their communities. SRSO through representatives of community institutions (CIs) and staff are responding COVID-19 emergency within its outreach areas through Community Savings, Ration and Vegetables Distribution, Linkages Development, Identification of deserving HHs, delivering awareness sessions on precautionary measures to fight COVID-19 and Registration of needy and poor families under the Govt. of Pakistan Ehsaas Emergency Cash Programme. Households and individuals are being supported with Cash, Ration and capitalizing LSO linkages for relief activities in their concerned areas. SRSO well trained human capital is engaged in Government relief activities through identification of deserving beneficiaries, distribution of ration bags, conducting awareness sessions on preventive measures to combat COVID-19 SRSO is also facilitating the Government of Sindh in the identification of deserving families and distribution of food items in most needy households. SRSO outreach and scale of response -

Sindh Flood 2011 - Union Council Ranking - Tharparkar District
PAKISTAN - Sindh Flood 2011 - Union Council Ranking - Tharparkar District Union council ranking exercise, coordinated by UNOCHA and UNDP, is a joint effort of Government and humanitarian partners Community Restoration Food Education in the notified districts of 2011 floods in Sindh. Its purpose is to: SANGHAR SANGHAR SANGHAR Parno Gadro Parno Gadro Parno Gadro Identify high priority union councils with outstanding needs. Pirano Pirano Pirano Jo Par Jo Par Jo Par Facilitate stackholders to plan/support interventions and divert INDIA INDIA INDIA UMERKOT UMERKOT Tar Ahmed Tar Ahmed UMERKOT Tar Ahmed Mithrio Mithrio Mithrio resources where they are most needed. Charan Charan Charan MATIARI Sarianghiar MATIARI Sarianghiar MATIARI Sarianghiar Provide common prioritization framework to clusters, agencies Vejhiar Chachro Vejhiar Chachro Vejhiar Chachro Kantio Hirar Tardos Kantio Hirar Tardos Kantio Hirar Tardos Mithrio Mithrio Mithrio and donors. Chelhar Charan Chelhar Charan Chelhar Charan Satidero Satidero Satidero First round of this exercise is completed from February - March Mohrano Islamkot Mohrano Islamkot Mohrano Islamkot Mithrio Singaro Tingusar Mithrio Singaro Tingusar Mithrio Singaro Tingusar Bhitaro Bhatti Bhitaro Bhatti Bhitaro Bhatti BADIN Joruo BADIN Joruo BADIN Joruo 2012. Khario Harho Khario Harho Khario Harho Khetlari Ghulam Nagarparkar Khetlari Ghulam Nagarparkar Khetlari Ghulam Nagarparkar Shah Shah Shah Malanhori Mithi Malanhori Mithi Malanhori Mithi Virawah Virawah Virawah Sobhiar Vena Sobhiar Vena Sobhiar Vena Pithapur -

Sindh Province - Flood Analysis (Flood Extent from 27 August 2010 to 07 September 2010)
Pakistan Floods: Sindh Province - Flood Analysis (Flood Extent from 27 August 2010 to 07 September 2010) Kashmore Taluka Thul Taluka Kashmore PUNJAB Jacobabad Taluka Kandhkot Taluka BALOCHISTAN Jaccobabad Ubauro Taluka Shikarpur Taluka Garhi Khairo Taluka Khanpur Taluka Ghotki Taluka Shikarpur Lakhi Taluka Garhi Yasin Taluka Shahdad Kot Taluka Pano Aqil Taluka Ghotki Daharki Taluka Miro Khan Taluka Sukkur Taluka Ratodero Taluka Kambar Ali Khan Taluka Mirpur Mathelo Taluka Kingri Taluka Rohri Taluka Qambar Shahdad kot Larkana Taluka Khairpur Taluka Khangarh Taluka Larkana Gambat Taluka Hamal Lake Warah Taluka Sukkur Dokri Taluka Kot Diji Taluka Salehpat Taluka Sobho Dero Taluka Mehar Taluka An estimated 7 million people are affected Khairpur Nathan Shah Taluka Kandiaro Taluka Mirwah Taluka 19 districts and 7,277 villages are affected. 1,098,720 houses are damaged Bhiria Taluka 199 deaths and 1,072 injuries are reported Naushahro Feroze (Source: NDMA, PDMA, GBDMA, FDMA as of 13092010) Dadu Khairpur Faiz Ganj Taluka Naushahro Feroze Taluka Dadu Taluka Moro Taluka Nara Taluka Johi Taluka Manchar Lake Daulat Pur Taluka Nawabshah Taluka Flood Water entered Jhanagar ! ! S.Banazirabad and Bajara towns as Manchar lake brusted as of 13 Sep 2010 Sehwan Taluka SINDH (UNOCHA Sit Rep # 24) Sakrand Taluka Shahdadpur Taluka Sanghar Taluka Water Supplies to Shewan tehsil I N D I A was cut down due to possible Sinjhoro Taluka contamination as of 13 Sep 2010 Sanghar Hala Taluka (UNOCHA Sit Rep # 24). Khipro Taluka Tando Adam Taluka Matiari Jam Nawaz -
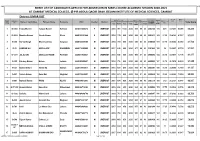
District: UMAR KOT MERIT LIST of CANDIDATES APPLIED FOR
MBBS MERIT LIST OF CANDIDATES APPLIED FOR ADMISSION IN MBBS COURSE ACADEMIC SESSION 2020-2021 SESSION 2020-2021 AT GAMBAT MEDICAL COLLEGE, @ PIR ABDUL QADIR SHAH JEELANI INSTITUTE OF MEDICAL SCIENCES, GAMBAT District: UMAR KOT Int. Adj. Matric Matric O / Level Inter A / Level MDCAT Merit GIMS FILE Test ROLL MDCAT Test 40% 10% Name of Candidates Fathers Name Surname CNIC Gender District B B Test Total Score NO# NO. Obt Inter NUMBER 50% o Year Marks Total o Year Grade Marks Marks % Aa Aa 1 G-1482 Tooba Muneer Tarique Muneer Kahloon 4430333488214 F UMERKOT g2016 951 1100 g2020 938 85 A1 2402160 170 42.5 34.1091 8.6455 85.255 a a B B 2 G-1083 Manisha Kumari Vinesh Kumar Khatri 4440122391488 F UMERKOT I2018 745 850 I 2020 985 90 A1 2903411 149 37.25 35.8182 8.7647 81.833 S S M M 3 G-306 Harmat Singh Ghansham Das Sangrasi 4440122265385 M UMERKOT i2018 709 850 i 2020 980 89 A1 4900548 151 37.75 35.6364 8.3412 81.728 r r B B 4 G-91 KAMRAN ALI ABDUL AZIZ RAHIMOON 4440176905885 M UMERKOT I2017 698 850 I 2020 971 88 A1 3307849 152 38 35.3091 8.2118 81.521 S S B B 5 G-1277 JALAL DIN ABDULLAH KHAN PATHAN 4440411925627 M UMERKOT I2018 656 850 I 2020 960 87 A1 4900692 155 38.75 34.9091 7.7176 81.377 S S M M 6 G-300 Pardeep Kumar Mohan Lohana 4440392509487 M UMERKOT i2018 716 850 i 2020 995 90 A1 4900052 147 36.75 36.1818 8.4235 81.355 r r B B 7 G-327 Bashir Ahmed Sardar Ali Samejo 4440135929031 M UMERKOT I2018 655 850 I 2020 954 87 A1 2904607 155 38.75 34.6909 7.7059 81.147 S S B B 8 G-547 Suresh Kumar Rano Mal Meghwar 4440118625881 M UMERKOT I2018 672