Schizophrenia and Public Health
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

First Episode Psychosis an Information Guide Revised Edition
First episode psychosis An information guide revised edition Sarah Bromley, OT Reg (Ont) Monica Choi, MD, FRCPC Sabiha Faruqui, MSc (OT) i First episode psychosis An information guide Sarah Bromley, OT Reg (Ont) Monica Choi, MD, FRCPC Sabiha Faruqui, MSc (OT) A Pan American Health Organization / World Health Organization Collaborating Centre ii Library and Archives Canada Cataloguing in Publication Bromley, Sarah, 1969-, author First episode psychosis : an information guide : a guide for people with psychosis and their families / Sarah Bromley, OT Reg (Ont), Monica Choi, MD, Sabiha Faruqui, MSc (OT). -- Revised edition. Revised edition of: First episode psychosis / Donna Czuchta, Kathryn Ryan. 1999. Includes bibliographical references. Issued in print and electronic formats. ISBN 978-1-77052-595-5 (PRINT).--ISBN 978-1-77052-596-2 (PDF).-- ISBN 978-1-77052-597-9 (HTML).--ISBN 978-1-77052-598-6 (ePUB).-- ISBN 978-1-77114-224-3 (Kindle) 1. Psychoses--Popular works. I. Choi, Monica Arrina, 1978-, author II. Faruqui, Sabiha, 1983-, author III. Centre for Addiction and Mental Health, issuing body IV. Title. RC512.B76 2015 616.89 C2015-901241-4 C2015-901242-2 Printed in Canada Copyright © 1999, 2007, 2015 Centre for Addiction and Mental Health No part of this work may be reproduced or transmitted in any form or by any means electronic or mechanical, including photocopying and recording, or by any information storage and retrieval system without written permission from the publisher—except for a brief quotation (not to exceed 200 words) in a review or professional work. This publication may be available in other formats. For information about alterna- tive formats or other CAMH publications, or to place an order, please contact Sales and Distribution: Toll-free: 1 800 661-1111 Toronto: 416 595-6059 E-mail: [email protected] Online store: http://store.camh.ca Website: www.camh.ca Disponible en français sous le titre : Le premier épisode psychotique : Guide pour les personnes atteintes de psychose et leur famille This guide was produced by CAMH Publications. -

Do the Lifetime Prevalence and Prognosis of Schizophrenia Differ Among World Regions? Cheryl Lynn Smith
Claremont Colleges Scholarship @ Claremont CMC Senior Theses CMC Student Scholarship 2018 Do the Lifetime Prevalence and Prognosis of Schizophrenia Differ Among World Regions? Cheryl Lynn Smith Recommended Citation Smith, Cheryl Lynn, "Do the Lifetime Prevalence and Prognosis of Schizophrenia Differ Among World Regions?" (2018). CMC Senior Theses. 1978. http://scholarship.claremont.edu/cmc_theses/1978 This Open Access Senior Thesis is brought to you by Scholarship@Claremont. It has been accepted for inclusion in this collection by an authorized administrator. For more information, please contact [email protected]. Do the Lifetime Prevalence and Prognosis of Schizophrenia Differ Among World Regions? A Thesis Presented by Cheryl Lynn Smith To the Keck Science Department Of Claremont McKenna, Pitzer, and Scripps Colleges In partial fulfillment of The degree of Bachelor of Arts Senior Thesis in Human Biology 04/23/2018 LIFETIME PREVALENCE AND PROGNOSIS OF SCHIZOPHRENIA 1 Table of Contents Abstract …………………………………………………………...……………………… 2 1. Introduction………………………………………………...…………...……………… 3 2. Background Information ……………………………...……………………………….. 5 2.1 Historical Background of Schizophrenia ……………………....…………… 5 2.2 Lifetime Prevalence of Schizophrenia …………………………...…..……… 12 2.3 Prognosis in People with Schizophrenia ……………....………...…..……… 13 3. Methods …………………………………………...……………………..……………. 17 4. Results ……………………………………………...…………………….…….…….... 18 5. Discussion ……………………………………………...……………………………… 24 6. Acknowledgements …………………………………………...………………………. -

Resource Document on Social Determinants of Health
APA Resource Document Resource Document on Social Determinants of Health Approved by the Joint Reference Committee, June 2020 "The findings, opinions, and conclusions of this report do not necessarily represent the views of the officers, trustees, or all members of the American Psychiatric Association. Views expressed are those of the authors." —APA Operations Manual. Prepared by Ole Thienhaus, MD, MBA (Chair), Laura Halpin, MD, PhD, Kunmi Sobowale, MD, Robert Trestman, PhD, MD Preamble: The relevance of social and structural factors (see Appendix 1) to health, quality of life, and life expectancy has been amply documented and extends to mental health. Pertinent variables include the following (Compton & Shim, 2015): • Discrimination, racism, and social exclusion • Adverse early life experiences • Poor education • Unemployment, underemployment, and job insecurity • Income inequality • Poverty • Neighborhood deprivation • Food insecurity • Poor housing quality and housing instability • Poor access to mental health care All of these variables impede access to care, which is critical to individual health, and the attainment of social equity. These are essential to the pursuit of happiness, described in this country’s founding document as an “inalienable right.” It is from this that our profession derives its duty to address the social determinants of health. A. Overview: Why Social Determinants of Health (SDOH) Matter in Mental Health Social determinants of health describe “the causes of the causes” of poor health: the conditions in which individuals are “born, grow, live, work, and age” that contribute to the development of both physical and psychiatric pathology over the course of one’s life (Sederer, 2016). The World Health Organization defines mental health as “a state of well-being in which every individual realizes his or her own potential, can cope with the normal stresses of life, can work productively and fruitfully, and is able to make a contribution to her or his community” (World Health Organization, 2014). -

Spanish Clinical Language and Resource Guide
SPANISH CLINICAL LANGUAGE AND RESOURCE GUIDE The Spanish Clinical Language and Resource Guide has been created to enhance public access to information about mental health services and other human service resources available to Spanish-speaking residents of Hennepin County and the Twin Cities metro area. While every effort is made to ensure the accuracy of the information, we make no guarantees. The inclusion of an organization or service does not imply an endorsement of the organization or service, nor does exclusion imply disapproval. Under no circumstances shall Washburn Center for Children or its employees be liable for any direct, indirect, incidental, special, punitive, or consequential damages which may result in any way from your use of the information included in the Spanish Clinical Language and Resource Guide. Acknowledgements February 2015 In 2012, Washburn Center for Children, Kente Circle, and Centro collaborated on a grant proposal to obtain funding from the Hennepin County Children’s Mental Health Collaborative to help the agencies improve cultural competence in services to various client populations, including Spanish-speaking families. These funds allowed Washburn Center’s existing Spanish-speaking Provider Group to build connections with over 60 bilingual, culturally responsive mental health providers from numerous Twin Cities mental health agencies and private practices. This expanded group, called the Hennepin County Spanish-speaking Provider Consortium, meets six times a year for population-specific trainings, clinical and language peer consultation, and resource sharing. Under the grant, Washburn Center’s Spanish-speaking Provider Group agreed to compile a clinical language guide, meant to capture and expand on our group’s “¿Cómo se dice…?” conversations. -

Bipolar Disorder in ADULTS the Disorder, Its Treatment and Prevention
Bipolar lidelse hos voksne, engelsk Information about BIPOLAR DISORDER IN ADULTS The disorder, its treatment and prevention Psykiatri og Social psykinfomidt.dk CONTENTS 03 What is bipolar disorder? 04 What causes bipolar disorder? 06 What are the symptoms of bipolar disorder? 09 How is bipolar disorder diagnosed? 10 Different progressions and modes of expression 11 How can bipolar disorder be treated and prevented? 14 What can you do to help yourself if you have bipolar disorder? 16 What can your loved ones do? Bipolar affective disorder (the term we will use in this publication is “bipolar disorder”) is a serious mental disorder. When a person has bipolar disorder, knowledge of the illness is important. The more you know, the better you can handle and prevent the illness and its consequences. This brochure describes the illness as well as options for its treatment and prevention. It is mainly intended for people being treated for bipolar disorder by the psychiatric service in Region Midtjylland. We hope this brochure will help you and your loved ones to learn more about the diagnosis of bipolar disorder. Kind regards The psychiatric service in Region Midtjylland Tingvej 15, 8800 Viborg Tel.: 7841 0000 Bipolar disorder in adults WHAT IS BIPOLAR DISORDER? Bipolar disorder is a mental illness lot in terms of reducing the progression characterised by episodes of mania, of symptoms and decreasing the hypomania (a mild form of mania), psychological and social costs to the depression and/or mixed state (a state individual and the family. where manic and depressive symptoms coexist or occur in rapid succession). -

Eating Disorders: About More Than Food
Eating Disorders: About More Than Food Has your urge to eat less or more food spiraled out of control? Are you overly concerned about your outward appearance? If so, you may have an eating disorder. National Institute of Mental Health What are eating disorders? Eating disorders are serious medical illnesses marked by severe disturbances to a person’s eating behaviors. Obsessions with food, body weight, and shape may be signs of an eating disorder. These disorders can affect a person’s physical and mental health; in some cases, they can be life-threatening. But eating disorders can be treated. Learning more about them can help you spot the warning signs and seek treatment early. Remember: Eating disorders are not a lifestyle choice. They are biologically-influenced medical illnesses. Who is at risk for eating disorders? Eating disorders can affect people of all ages, racial/ethnic backgrounds, body weights, and genders. Although eating disorders often appear during the teen years or young adulthood, they may also develop during childhood or later in life (40 years and older). Remember: People with eating disorders may appear healthy, yet be extremely ill. The exact cause of eating disorders is not fully understood, but research suggests a combination of genetic, biological, behavioral, psychological, and social factors can raise a person’s risk. What are the common types of eating disorders? Common eating disorders include anorexia nervosa, bulimia nervosa, and binge-eating disorder. If you or someone you know experiences the symptoms listed below, it could be a sign of an eating disorder—call a health provider right away for help. -
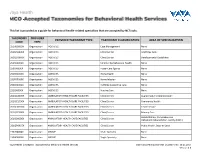
This List Is Provided As a Guide for Behavioral Health-Related Specialties That Are Accepted by Nctracks
This list is provided as a guide for behavioral health-related specialties that are accepted by NCTracks. TAXONOMY PROVIDER PROVIDER TAXONOMY TYPE TAXONOMY CLASSIFICATION AREA OF SPECIALIZATION CODE TYPE 251B00000X Organization AGENCIES Case Management None 261QA0600X Organization AGENCIES Clinic/Center Adult Day Care 261QD1600X Organization AGENCIES Clinic/Center Developmental Disabilities 251S00000X Organization AGENCIES Community/Behavioral Health None 253J00000X Organization AGENCIES Foster Care Agency None 251E00000X Organization AGENCIES Home Health None 251F00000X Organization AGENCIES Home Infusion None 253Z00000X Organization AGENCIES In-Home Supportive Care None 251J00000X Organization AGENCIES Nursing Care None 261QA3000X Organization AMBULATORY HEALTH CARE FACILITIES Clinic/Center Augmentative Communication 261QC1500X Organization AMBULATORY HEALTH CARE FACILITIES Clinic/Center Community Health 261QH0100X Organization AMBULATORY HEALTH CARE FACILITIES Clinic/Center Health Service 261QP2300X Organization AMBULATORY HEALTH CARE FACILITIES Clinic/Center Primary Care Rehabilitation, Comprehensive 261Q00000X Organization AMBULATORY HEALTH CARE FACILITIES Clinic/Center Outpatient Rehabilitation Facility (CORF) 261QP0905X Organization AMBULATORY HEALTH CARE FACILITIES Clinic/Center Public Health, State or Local 193200000X Organization GROUP Multi-Specialty None 193400000X Organization GROUP Single-Specialty None Vaya Health | Accepted Taxonomies for Behavioral Health Services Claims and Reimbursement | Content rev. 10.01.2017 Version -

The Clinical Presentation of Psychotic Disorders Bob Boland MD Slide 1
The Clinical Presentation of Psychotic Disorders Bob Boland MD Slide 1 Psychotic Disorders Slide 2 As with all the disorders, it is preferable to pick Archetype one “archetypal” disorder for the category of • Schizophrenia disorder, understand it well, and then know the others as they compare. For the psychotic disorders, the diagnosis we will concentrate on will be Schizophrenia. Slide 3 A good way to organize discussions of Phenomenology phenomenology is by using the same structure • The mental status exam as the mental status examination. – Appearance –Mood – Thought – Cognition – Judgment and Insight Clinical Presentation of Psychotic Disorders. Slide 4 Motor disturbances include disorders of Appearance mobility, activity and volition. Catatonic – Motor disturbances • Catatonia stupor is a state in which patients are •Stereotypy • Mannerisms immobile, mute, yet conscious. They exhibit – Behavioral problems •Hygiene waxy flexibility, or assumption of bizarre • Social functioning – “Soft signs” postures as most dramatic example. Catatonic excitement is uncontrolled and aimless motor activity. It is important to differentiate from substance-induced movement disorders, such as extrapyramidal symptoms and tardive dyskinesia. Slide 5 Disorders of behavior may involve Appearance deterioration of social functioning-- social • Behavioral Problems • Social functioning withdrawal, self neglect, neglect of • Other – Ex. Neuro soft signs environment (deterioration of housing, etc.), or socially inappropriate behaviors (talking to themselves in -

Schizophrenia
Schizophrenia The upcoming fifth edition of the Diagnostic and Statistical Manual of Mental Disorders (DSM-5) makes several key changes to the category of schizophrenia and highlights for future study an area that could be critical for early detection of this often debilitating condition. Changes to the Diagnosis Schizophrenia is characterized by delusions, hallucinations, disorganized speech and behavior, and other symptoms that cause social or occupational dysfunction. For a diagnosis, symptoms must have been present for six months and include at least one month of active symptoms. DSM-5 raises the symptom threshold, requiring that an individual exhibit at least two of the specified symptoms. (In the manual’s previous editions, that threshold was one.) Additionally, the diagnostic criteria no longer identify subtypes. Subtypes had been defined by the predominant symptom at the time of evaluation. But these were not helpful to clinicians because patients’ symptoms often changed from one subtype to another and presented overlapping subtype symptoms, which blurred distinc- tions among the five subtypes and decreased their validity. Some of the subtypes are now specifiers to help provide further detail in diagnosis. For example, catatonia (marked by motor immobility and stupor) will be used as a specifier for schizophrenia and other psychotic conditions such as schizoaffec- tive disorder. This specifier can also be used in other disorder areas such as bipolar disorders and major depressive disorder. Area for Further Study Attenuated psychosis syndrome is included in Section III of the new manual; conditions listed there require further research before their consideration as formal disorders. This potential category would identify a person who does not have a full-blown psychotic disorder but exhibits minor versions of relevant symptoms. -

Schizophrenia Clinical Practice Guidelines
Royal Australian and New Zealand College of Psychiatrists clinical practice guidelines for the management of schizophrenia and related disorders Cherrie Galletly1,2,3, David Castle4, Frances Dark5, Verity Humberstone6, Assen Jablensky7, Eóin Killackey8,9, Jayashri Kulkarni10,11, Patrick McGorry8,9,12, Olav Nielssen13 and Nga Tran14,15 Abstract Objectives: This guideline provides recommendations for the clinical management of schizophrenia and related disorders for health professionals working in Australia and New Zealand. It aims to encourage all clinicians to adopt best practice principles. The recommendations represent the consensus of a group of Australian and New Zealand experts in the management of schizophrenia and related disorders. This guideline includes the management of ultra-high risk syndromes, first-episode psychoses and prolonged psychoses, including psychoses associated with substance use. It takes a holistic approach, addressing all aspects of the care of people with schizophrenia and related disorders, not only correct diagnosis and symptom relief but also optimal recovery of social function. Methods: The writing group planned the scope and individual members drafted sections according to their area of interest and expertise, with reference to existing systematic reviews and informal literature reviews undertaken for this guideline. In addition, experts in specific areas contributed to the relevant sections. All members of the writing group reviewed the entire document. The writing group also considered relevant international -

Association Between Schizophrenia Polygenic Score and Psychotic Symptoms In
bioRxiv preprint doi: https://doi.org/10.1101/528802; this version posted January 26, 2019. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY 4.0 International license. Association between schizophrenia polygenic score and psychotic symptoms in Alzheimer’s disease: meta-analysis of 11 cohort studies. Byron Creese1,2*, Evangelos Vassos3*, Sverre Bergh2,4,5*, Lavinia Athanasiu6,7, Iskandar Johar8,2, Arvid Rongve9,10,,2, Ingrid Tøndel Medbøen5,11, Miguel Vasconcelos Da Silva1,8,2, Eivind Aakhus4, Fred Andersen12, Francesco Bettella6,7 , Anne Braekhus5,11,13, Srdjan Djurovic10,14, Giulia Paroni16, Petroula Proitsi17, Ingvild Saltvedt18,19, Davide Seripa16, Eystein Stordal20,21, Tormod Fladby22,23, Dag Aarsland2,8,24, Ole A. Andreassen6,7, Clive Ballard1,2*, Geir Selbaek4,5,25*, on behalf of the AddNeuroMed consortium and the Alzheimer's Disease Neuroimaging Initiative** 1. University of Exeter Medical School, Exeter, UK 2. Norwegian, Exeter and King's College Consortium for Genetics of Neuropsychiatric Symptoms in Dementia 3. Social Genetic and Developmental Psychiatry Centre, Institute of Psychiatry, Psychology and Neuroscience, King's College London 4. Research centre of Age-related Functional Decline and Disease, Innlandet Hospital Trust, Pb 68, Ottestad 2312, Norway 5. Norwegian National Advisory Unit on Ageing and Health, Vestfold Hospital Trust, Tønsberg, Norway 6. NORMENT, Institute of Clinical Medicine, University of Oslo, Oslo, Norway. 7. NORMENT, Division of Mental Health and Addiction, Oslo University Hospital, Oslo, Norway 8. Department of Old Age Psychiatry, Institute of Psychiatry, Psychology and Neuroscience, King's College London 9. -

Psychotic Symptoms in Post Traumatic Stress Disorder: a Case Illustration and Literature Review
CASE REPORT SA Psych Rev 2003;6: 21-24 Psychotic symptoms in post traumatic stress disorder: a case illustration and literature review Adekola O Alao, Laura Leso, Mantosh J Dewan, Erika B Johnson Department of Psychiatry, State University of New York, Syracuse, NY, USA ABSTRACT Posttraumatic stress disorder (PTSD) is a condition being increasingly recognized. The diagnosis is based on the re-experiencing of a traumatic event. There have been reports of the presence of psychotic symptoms in some cases of PTSD. This may represent in- creased severity or a different diagnostic clinical entity. It has also been suggested that psychotic symptoms may be over-represented in the Hispanic population. In this manuscript, we describe a case to illustrate this relationship and we review the current literature on the relationship of psychotic symptoms among PTSD patients. The implications regarding diagnosis, treatment, and prognosis are discussed. Keywords: Psychosis; PTSD; Trauma; Hallucinations; Delusions; Posttraumatic stress disorder. INTRODUCTION the best of our knowledge is the first report of psychotic symp- Posttraumatic stress disorder (PTSD) is a psychiatric illness for- toms in a non-veteran adult with PTSD. mally recognized with the publication of the third edition of the Diagnostic and Statistical Manual of the American Psychiatric CASE ILLUSTRATION Association in 1980.1 Re-experiencing of traumatic events as A 37 year-old gentleman was admitted to a state university hos- recurrent unpleasant images, nightmares, and intrusive feelings pital inpatient setting after alerting his wife of his suicidal is a core characteristic of PTSD.2 Most PTSD research has oc- thoughts and intent to slit his throat with a kitchen knife.