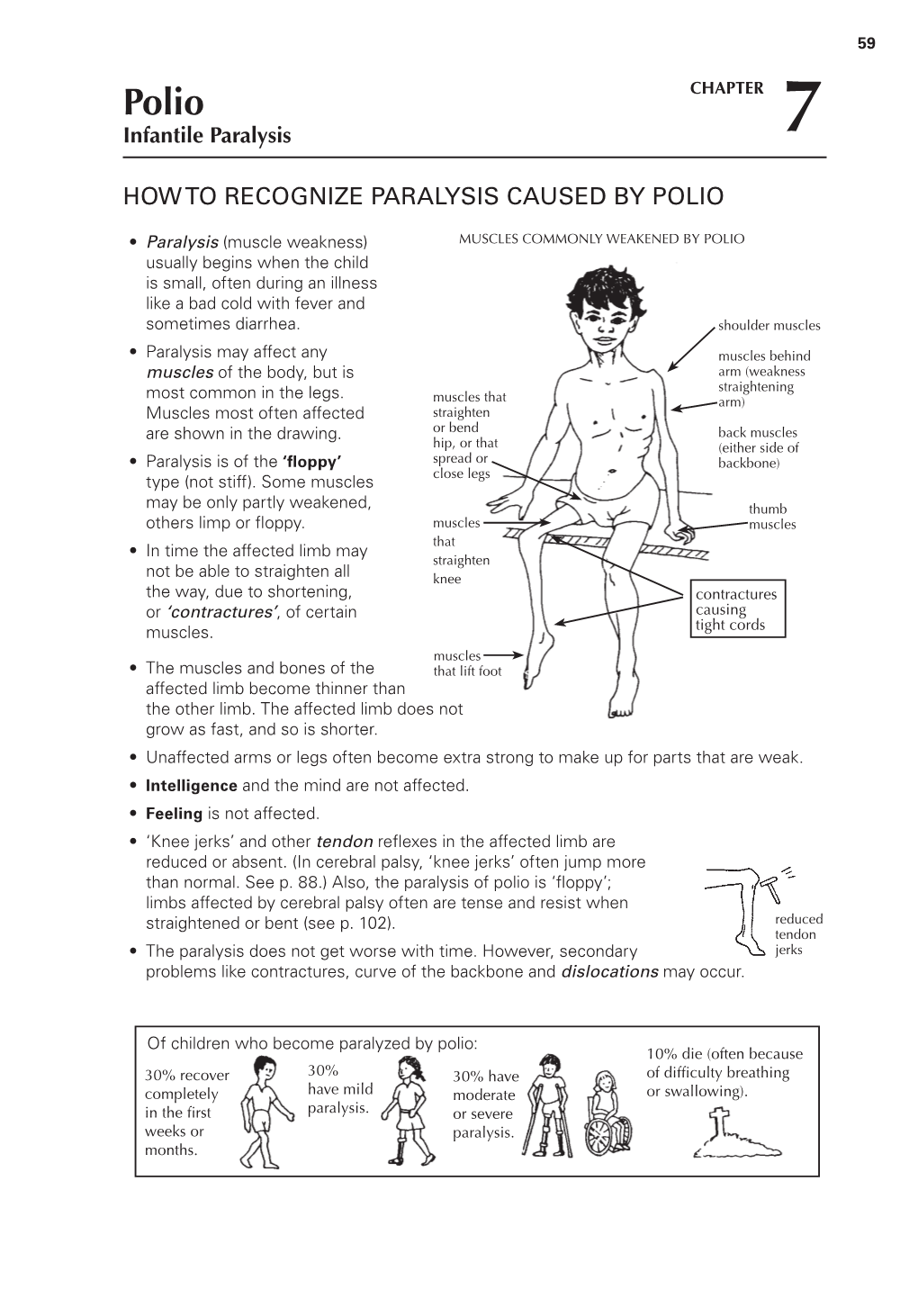
How to Recognize Paralysis Caused by Polio
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

10Neurodevelopmental Effects of Childhood Exposure to Heavy
Neurodevelopmental E¤ects of Childhood Exposure to Heavy Metals: 10 Lessons from Pediatric Lead Poisoning Theodore I. Lidsky, Agnes T. Heaney, Jay S. Schneider, and John F. Rosen Increasing industrialization has led to increased exposure to neurotoxic metals. By far the most heavily studied of these metals is lead, a neurotoxin that is particularly dangerous to the developing nervous system of children. Awareness that lead poison- ing poses a special risk for children dates back over 100 years, and there has been increasing research on the developmental e¤ects of this poison over the past 60 years. Despite this research and growing public awareness of the dangers of lead to chil- dren, government regulation has lagged scientific knowledge; legislation has been in- e¤ectual in critical areas, and many new cases of poisoning occur each year. Lead, however, is not the only neurotoxic metal that presents a danger to children. Several other heavy metals, such as mercury and manganese, are also neurotoxic, have adverse e¤ects on the developing brain, and can be encountered by children. Al- though these other neurotoxic metals have not been as heavily studied as lead, there has been important research describing their e¤ects on the brain. The purpose of the present chapter is to review the neurotoxicology of lead poisoning as well as what is known concerning the neurtoxicology of mercury and manganese. The purpose of this review is to provide information that might be of some help in avoiding repeti- tion of the mistakes that were made in attempting to protect children from the dan- gers of lead poisoning. -

Child Neurology: Hereditary Spastic Paraplegia in Children S.T
RESIDENT & FELLOW SECTION Child Neurology: Section Editor Hereditary spastic paraplegia in children Mitchell S.V. Elkind, MD, MS S.T. de Bot, MD Because the medical literature on hereditary spastic clinical feature is progressive lower limb spasticity B.P.C. van de paraplegia (HSP) is dominated by descriptions of secondary to pyramidal tract dysfunction. HSP is Warrenburg, MD, adult case series, there is less emphasis on the genetic classified as pure if neurologic signs are limited to the PhD evaluation in suspected pediatric cases of HSP. The lower limbs (although urinary urgency and mild im- H.P.H. Kremer, differential diagnosis of progressive spastic paraplegia pairment of vibration perception in the distal lower MD, PhD strongly depends on the age at onset, as well as the ac- extremities may occur). In contrast, complicated M.A.A.P. Willemsen, companying clinical features, possible abnormalities on forms of HSP display additional neurologic and MRI abnormalities such as ataxia, more significant periph- MD, PhD MRI, and family history. In order to develop a rational eral neuropathy, mental retardation, or a thin corpus diagnostic strategy for pediatric HSP cases, we per- callosum. HSP may be inherited as an autosomal formed a literature search focusing on presenting signs Address correspondence and dominant, autosomal recessive, or X-linked disease. reprint requests to Dr. S.T. de and symptoms, age at onset, and genotype. We present Over 40 loci and nearly 20 genes have already been Bot, Radboud University a case of a young boy with a REEP1 (SPG31) mutation. Nijmegen Medical Centre, identified.1 Autosomal dominant transmission is ob- Department of Neurology, PO served in 70% to 80% of all cases and typically re- Box 9101, 6500 HB, Nijmegen, CASE REPORT A 4-year-old boy presented with 2 the Netherlands progressive walking difficulties from the time he sults in pure HSP. -

Accelerating Research. Empowering Families
RESEARCH STRATEGY AND MISSION We aggressively pursue research to identify treatments and a cure for Rett syndrome. New Mecp2 female mouse model developed AMO receives FDA Orphan Drug Designation 2018 + BEYOND With your support, we can Neuren begins plans for trofinetide Phase 3 continue to blaze a trail in Rett syndrome research and family 2017 14 clinics designated empowerment to transform lives. as Rett Syndrome Clinical Research First multi-site, Centers of Excellence multi-country clinical Join us in our mission: trial begins: sarizotan • Make a donation 2015 • Coordinate a Fundraiser Clinical trial for • Participate in an Event trofinetide begins • Advocate for Rett syndrome NIH funding of the NHS begins Visit www.rettsyndrome.org or Drug screening Scout program begins call 1.800.719.8214 2014 First multi-site clinical trial Rettsyndrome.org is a 501(c)3 organization in RTT begins: NNZ-2566 (trofinetide) Accelerating dedicated to accelerating research for treatments and a cure for Rett syndrome and related disorders, 2013 while providing family empowerment. As a Established stem Research. leading organization for Rett syndrome research, cell model for Rettsyndrome.org is committed to funding high- drug screening First clinical trial quality, peer-reviewed research grants and programs. in RTT supported by Rettsyndrome.org: IGF-1 Empowering Genetic manipulation 2010 and biochemical Families. intervention improve Rett-like symptoms in a mouse model 2007 4600 Devitt Drive Cincinnati, OH 45246-1104 ‘‘ (800) 818-7388 www.rettsyndrome.org I am very thankful that Rettsyndrome.org has taken such a strong leadership role /rettsyndrome /rettsyndrome /rettsyndromeorg with advancing research. Their progress to get trofinetide to market is very exciting as it could finally be an answer to relieving some of Jill’s daily struggles. -

Hereditary Spastic Paraparesis: a Review of New Developments
J Neurol Neurosurg Psychiatry: first published as 10.1136/jnnp.69.2.150 on 1 August 2000. Downloaded from 150 J Neurol Neurosurg Psychiatry 2000;69:150–160 REVIEW Hereditary spastic paraparesis: a review of new developments CJ McDermott, K White, K Bushby, PJ Shaw Hereditary spastic paraparesis (HSP) or the reditary spastic paraparesis will no doubt Strümpell-Lorrain syndrome is the name given provide a more useful and relevant classifi- to a heterogeneous group of inherited disorders cation. in which the main clinical feature is progressive lower limb spasticity. Before the advent of Epidemiology molecular genetic studies into these disorders, The prevalence of HSP varies in diVerent several classifications had been proposed, studies. Such variation is probably due to a based on the mode of inheritance, the age of combination of diVering diagnostic criteria, onset of symptoms, and the presence or other- variable epidemiological methodology, and wise of additional clinical features. Families geographical factors. Some studies in which with autosomal dominant, autosomal recessive, similar criteria and methods were employed and X-linked inheritance have been described. found the prevalance of HSP/100 000 to be 2.7 in Molise Italy, 4.3 in Valle d’Aosta Italy, and 10–12 Historical aspects 2.0 in Portugal. These studies employed the In 1880 Strümpell published what is consid- diagnostic criteria suggested by Harding and ered to be the first clear description of HSP.He utilised all health institutions and various reported a family in which two brothers were health care professionals in ascertaining cases aVected by spastic paraplegia. The father was from the specific region. -

Cerebral Palsy the ABC's of CP
Cerebral Palsy The ABC’s of CP Toni Benton, M.D. Continuum of Care Project UNM HSC School of Medicine April 20, 2006 Cerebral Palsy Outline I. Definition II. Incidence, Epidemiology and Distribution III. Etiology IV. Types V. Medical Management VI. Psychosocial Issues VII. Aging Cerebral Palsy-Definition Cerebral palsy is a symptom complex, (not a disease) that has multiple etiologies. CP is a disorder of tone, posture or movement due to a lesion in the developing brain. Lesion results in paralysis, weakness, incoordination or abnormal movement Not contagious, no cure. It is static, but it symptoms may change with maturation Cerebral Palsy Brain damage Occurs during developmental period Motor dysfunction Not Curable Non-progressive (static) Any regression or deterioration of motor or intellectual skills should prompt a search for a degenerative disease Therapy can help improve function Cerebral Palsy There are 2 major types of CP, depending on location of lesions: Pyramidal (Spastic) Extrapyramidal There is overlap of both symptoms and anatomic lesions. The pyramidal system carries the signal for muscle contraction. The extrapyramidal system provides regulatory influences on that contraction. Cerebral Palsy Types of brain damage Bleeding Brain malformation Trauma to brain Lack of oxygen Infection Toxins Unknown Epidemiology The overall prevalence of cerebral palsy ranges from 1.5 to 2.5 per 1000 live births. The overall prevalence of CP has remained stable since the 1960’s. Speculations that the increased survival of the VLBW preemies would cause a rise in the prevalence of CP have proven wrong. Likewise the expected decrease in CP as a result of C-section and fetal monitoring has not happened. -

GBS/CIDP Foundation International
Guillain-Barré Syndrome GBS: An Acute Care Guide For Medical Professionals A publication of the GBS/CIDP Foundation International Guillain-Barré Syndrome: An Acute Care Guide For Medical Professionals A publication of the GBS/CIDP Foundation International 2012 Edition GBS/CIDP Foundation International The Holly Building 104 1/2 Forrest Avenue Narberth, PA 19072 Phone: 610.667.0131 Toll Free: 866.224.3301 Fax: 610.667.7036 [email protected] www.gbs-cidp.org Guillain-Barré Syndrome: An Acute Care Guide For Medical Professionals Contents Page Acknowledgements . i Introduction . 1 Initial Patient Evaluation . 4 Natural History of GBS: Implications for Patient Care . 6 Respiratory Complications . 8 Dysautonomia and Cardiovascular Complications . 12 Bladder, Bowel Dysfunction . 14 Metabolism: Nutrition, Hydration, Electrolytes . 14 Pain . 17 ICU Delirium . 18 Skin . 18 Musculo-Skeletal Issues, Occupational and Physical Therapy . 19 Infection . 22 Disorder Specific Treatments . 22 Appendix A. Checklist of Patient Issues to Monitor . 24 B. Diagnostic Criteria for GBS . 25 C. Prognosis . 26 References . 27 This pamphlet is provided as a service of the GBS/CIDP Foundation International Serving the medical community and patients with Guillain-Barré syndrome and related acute and chronic paralyzing disorders of the peripheral nerves. Acknowledgements Guillain-Barré syndrome (GBS) is a rare disorder. Some health professionals may not be familiar with treating it. A beautiful video by Tanya Ooraikul chronicled the superb care provided to her husband Kit during his recovery from GBS. His care at Gray Nuns Community Hospital in Edmonton, Alberta, Canada included 86 days in the intensive care unit. The video handsomely demonstrates the high quality of care that can be provided for this rare and complicated disorder in a community hospital. -
Unilateral Foot Drop: an Unusual Presentation of a More Common
DOI: 10.7860/JCDR/2017/26249.10738 Case Report Unilateral Foot Drop: An Unusual Section Presentation of a more Common Internal Medicine Disease RAMESHWAR NATH CHAURASIA1, ABHISHEK PathaK2, VIJAY nath MISHRA3, DEEPIKA JOSHI4 ABSTRACT An isolated and unilateral foot drop due to intracranial lesion is quite rare. Presenting herein a case of a 14-year-old female who complained of inability to wear and hold slipper in her left foot. Detailed neurological examination revealed left foot dorsiflexion which had 1/5 muscle power along with brisk left ankle reflex. Magnetic resonance imaging of the brain revealed multiple conglomerate inflammatory granulomas in cerebrum and cerebellum, larger one in right parasagittal region with perifocal oedema. Magnetic resonance spectrum was suggestive of tuberculoma. Her chest X-ray chest revealed milliary shadowing. She was put on anti- tubercular drugs, steroid and a prophylactic anti-epileptic drug. The dorsiflexion improved to grade 4/5 after three weeks of treatment. The motor homunculus for foot is located in parasagittal area. Therefore, in patients with foot drop, we must keep high index of suspicion for parasagittal lesions, so that prompt diagnosis and early management can be done to prevent complications and improve the quality of life of patient. Keywords: Lower motor neuron, Magnetic resonance imaging, Spastic foot drop, Tuberculoma, Upper motor neuron CASE REPORT A 14-year-old female presented with history of difficulty in walking for last three days after left foot drop. She noticed difficulty in her left foot when she was trying to wear shoes go to school. Weakness gradually progressed within next two days so much so that she was unable to hold slipper and clear the ground without tripping by her left foot. -

Epilepsy and Cerebral Palsy*
Arch Dis Child: first published as 10.1136/adc.31.155.1 on 1 February 1956. Downloaded from EPILEPSY AND CEREBRAL PALSY* BY BRIAN H. KIRMAN From the Fountain Hospital, Tooting, London (RECEIVED FOR PUBLICATION SEPTEMBER 6, 1955) The two conditions epilepsy and palsy in its Frequency of Epilepsy as a Complication many forms are amongst the earliest syndromes of Cerebral Palsy recorded in history. The association between Brissaud and Souques (1904) attempted to confine epilepsy and cerebral palsy in childhood is a matter the term 'Little's disease' to those cases not com- of everyday experience, and this association is of plicated by fits or mental defect, but Little's (1861-2) scientific interest as throwing light on the nature of own description of 63 cases refers specifically to the cerebral palsy and, more particularly, of epilepsy. complication ofconvulsions. Kinnier Wilson (1940) It is also of practical importance in view of recent refers to Little's disease not as 'an ailment of a well efforts to make more adequate provision for those defined character but a mere syndrome and a rather children with cerebral palsy who are educable. wide-ranging one at that'. Since epilepsy is also The existence of the two conditions in one child not a disease but a symptom of cerebral dysfunction constitutes a double handicap. The present ten- it is understandable that cerebral palsy and epilepsy dency in our educational system is for ever-increasing should often be encountered in the same patient. copyright. subdivision of educational 'types', and any child Kinnier Wilson states that in his experience 30% of who is difficult to fit into one of the artificial cate- cases of cerebral diplegia have fits which may be gories thus constructed is in danger of remaining general or one-sided. -

Cerebral Palsy
Cerebral Palsy Cerebral palsy encompasses a group of non-progressive and non-contagious motor conditions that cause physical disability in various facets of body movement. Cerebral palsy is one of the most common crippling conditions of childhood, dating to events and brain injury before, during or soon after birth. Cerebral palsy is a debilitating condition in which the developing brain is irreversibly damaged, resulting in loss of motor function and sometimes also cognitive function. Despite the large increase in medical intervention during pregnancy and childbirth, the incidence of cerebral palsy has remained relatively stable for the last 60 years. In Australia, a baby is born with cerebral palsy about every 15 hours, equivalent to 1 in 400 births. Presently, there is no cure for cerebral palsy. Classification Cerebral palsy is divided into four major classifications to describe different movement impairments. Movements can be uncontrolled or unpredictable, muscles can be stiff or tight and in some cases people have shaky movements or tremors. These classifications also reflect the areas of the brain that are damaged. The four major classifications are: spastic, ataxic, athetoid/dyskinetic and mixed. In most cases of cerebral palsy, the exact cause is unknown. Suggested possible causes include developmental abnormalities of the brain, brain injury to the fetus caused by low oxygen levels (asphyxia) or poor circulation, preterm birth, infection, and trauma. Spastic cerebral palsy leads to increased muscle tone and inability for muscles to relax (hypertonic). The brain injury usually stems from upper motor neuron in the brain. Spastic cerebral palsy is classified depending on the region of the body affected; these include: spastic hemiplegia; one side being affected, spastic monoplegia; a single limb being affected, spastic triplegia; three limbs being affected, spastic quadriplegia; all four limbs more or less equally affected. -
Physical Therapy & FSHD
Physical Therapy & FSHD Facioscapulohumeral Muscular Dystrophy A Guide for Patients & Physical Therapists Authors: Wendy M. King, P.T., Assistant Professor, Neurology & Shree Pandya, P.T., M.S., Assistant Professor, Neurology & Physical Medicine and Rehabilitation A publication of the FSH Society, Inc. www.fshsociety.org Table of Contents Introduction ...............................................................................4 Facioscapulohumeral Dystrophy (FSHD) .....................5 Manifestations of Impairments Related to FSHD ......5 Exercise and FSHD ...................................................................7 Hydrotherapy (Water Therapy) and FSHD ..................9 Pain and FSHD ...........................................................................9 Surgical Management of Scapular Problems ............11 Who Are Physical Therapists &What Can You Expect When You See Them? .................................12 To Physical Therapists .......................................................14 Treatment of Pain .................................................................15 Summary ...................................................................................16 References ................................................................................17 About the FSH Society .........................................................18 Contact Information .............................................................19 ‐3‐ Introduction he purpose of this guide is to assist physical T therapists and patients to develop -

Foot Drop Schema Script
CPS Foot Drop Schema Script Hi everyone - my name is Maniraj. I’m excited to narrate this Clinical Problem Solvers schema on foot drop. Foot drop is really a story about a weakness or paralysis in the muscles that dorsiflex the foot. A patient with foot drop will drag their toes while walking. To avoid tripping over their toes while walking, a patient will lift their foot higher off the ground. Since there is no dorsiflexion for a heel strike when bringing their foot down, the patient “overshoots” and slaps their foot on the ground. This is called a steppage gait. What muscles are we talking about? The main dorsiflexor muscles are the tibialis anterior and the extensors of the toes (extensor hallucis longus and extensor digitorum longus). All of these muscles are innervated by the deep peroneal nerve, which is a branch of the common peroneal nerve. The peroneal nerve itself is a terminal branch of the sciatic nerve; the other branch of the sciatic is the tibial nerve. To help anchor the nerve functions we’ll be talking about, I think it’d be beneficial to first review acronyms that can be used to memorize them. The peroneal nerve functions to evert and dorsiflex at the ankle, which can be remembered by the acronym PED. The tibial nerve functions to invert and plantarflex at the ankle, so that becomes TIP. Since the sciatic nerve is really just the bundle of peroneal & tibial nerves, you can remember the sciatic nerve functions as PED + TIP. The sciatic nerve also supplies the hamstrings, which flex the leg at the knee. -

Prescription of Foot and Ankle Orthoses for Children with Charcot–Marie–Tooth Disease: a Review of the Evidence
Narrative Review Prescription of foot and ankle orthoses for children with Charcot–Marie–Tooth disease: a review of the evidence Grant Scheffers1, Claire Hiller1, Kathryn Refshauge1, Joshua Burns1,2 1Faculty of Health Sciences, The University of Sydney, Australia, 2Institute for Neuroscience and Muscle Research, The Children’s Hospital at Westmead, Australia Background: Charcot–Marie–Tooth disease (CMT) is the most common inherited peripheral neuropathy and is associated with debilitating lower limb impairments and activity limitations. These impairments and activity limitations are potentially amendable to the prescription of orthoses, yet there is no universal, literature-based consensus to inform the decision making process of whether or not orthoses are indicated for a particular child with CMT, and if so, what type of device. Objectives: The aims of this paper were to: (1) review the lower limb impairments and activity limitations of children with CMT; (2) review the indications of commonly prescribed foot and ankle orthoses; and (3) formulate a clinical algorithm for the optimal prescription of foot and ankle orthoses for children with CMT. Major findings: We conducted a comprehensive search of the major databases and reference lists of relevant articles and books. In general, in-shoe orthoses are indicated for children with CMT and pes cavus and foot pain and/or mild balance impairments, whilst ankle-foot orthoses are indicated for children with CMT and pes cavus, foot drop, global foot and ankle muscle weakness and/or ankle equinus, and moderate-severe balance impairments and/or difficulty walking. Conclusions: A clinical algorithm is proposed to guide the prescription of foot and ankle orthoses for children with CMT.