If You Have a Gastrointestinal Carcinoid Tumor
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Recent Advances in Radiological and Radionuclide Imaging and Therapy
European Journal of Endocrinology (2004) 151 15–27 ISSN 0804-4643 REVIEW Recent advances in radiological and radionuclide imaging and therapy of neuroendocrine tumours Gregory Kaltsas, Andrea Rockall1, Dimitrios Papadogias, Rodney Reznek1 and Ashley B Grossman Departments of Endocrinology and 1Academic Radiology, St Bartholomew’s Hospital, London ECIA 7BE, UK (Correspondence should be addressed to Ashley B Grossman, Department of Endocrinology, St Bartholomew’s Hospital, London EC1A 7BE, UK; Email: [email protected]) Abstract Neuroendocrine tumours (NETs) constitute a heterogeneous group of tumours that are able to express cell membrane neuroamine uptake mechanisms and/or specific receptors, such as somatostatin receptors, which can be of great value in the localization and treatment of these tumours. Scintigra- phy with 111In-pentetreotide has become one of the most important imaging investigations in the initial identification and staging of gastro-enteropancreatic (GEP) tumours, whereas helical computed tomography (CT), magnetic resonance imaging (MRI), endoscopic and/or peri-operative ultrason- ography are used for the precise localization of GEPs and in monitoring their response to treatment. Scintigraphy with 123I-MIBG (meta-iodobenzylguanidine) is sensitive in the identification of chromaf- fin cell tumours, although scintigraphy with 111In-pentetreotide may also have a role in the localiz- ation of malignant chromaffin cell tumours and medullary thyroid carcinoma; for further localization and monitoring of the response to treatment both CT and MRI are used with high diagnostic accu- racy. More recently, positron emission tomography (PET) scanning is being increasingly used for the localization of NETs, particularly when other imaging modalities have failed, although its precise role and utility remain to be defined. -

Yale New Haven Health- Nuclear Medicine Octreotide Imaging Exam
Yale New Haven Hospital Department of Radiology and Biomedical Imaging NewHaven Nuclear Medicine- Octreotide Scan Health Pre-exam Information and Instructions Thank you for choosing Yale New Haven Hospital We are looking forward to providing you with exceptional care. Your doctor has ordered an Octreotide scan. This is an imaging test that is used for localization of primary and metastatic neuroendocrine tumors bearing somatostatin receptors. This exam consists of 3 appointments over two days. Yale New Haven Hospital Preparation for this Exam: Before Arriving for Your Exam Please arrive 15 minutes early to check in. Children accompanying patients during visits: o Unfortunately, we cannot routinely supervise your children during your imaging study. We believe that you are best served when we can provide 100% of our attention to you. Therefore, we encourage you to make childcare arrangements or to bring a responsible adult with you to supervise your children. There are no pre-exam instructions. The injection for this exam is specifically ordered for you and is very expensive, if you are unable to keep your appointment or have any questions, please call us at 203-688-1011 option 7. Wear loose comfortable clothing, since you will need to lie still for a period of time. We want to make your waiting time as pleasant as possible. Consider bringing your favorite magazine, book or music player to help you pass the time. Please leave your jewelry and valuables at home. After Arriving Upon arrival, a technologist will explain your procedure and answer any questions you may have. ATTENTION Females (ages 10 to 55) To ensure Radiation Safety, the following is YNHH Policy on pregnancy test for this Radiology exam. -

Use of DOTATATE PET/CT Scan in the Diagnosis and Staging Of
WJOESWJOES DOTATATE10.5005/jp-journals-10002-1231 PET/CT in Thymic Carcinoid CASE REPORT Use of DOTATATE PET/CT Scan in the Diagnosis and Staging of Thymic Atypical Carcinoid Tumor in a Patient with Secondary ACTH-dependent Cushing Syndrome: Look Twice and Cut Once 1John Agzarian, 2Hisham Quandeel, 3Irina Bancos, 4Geoffrey B Johnson, 5Stephen C Scharf, 6Geoffrey B Thompson 7Joanne Yi, 8Xiaotun Zhang, 9K Robert Shen ABSTRACT Keywords: DOTATATE, Mediastinal, Positron emission tomog- raphy, Thymic carcinoid. Neuroendocrine thymic tumors represent the least common type of primary thymic tumor with a prevalence of 2 to 5%. We How to cite this article: Agzarian J, Quandeel H, Bancos I, present a case of locally advanced thymic atypical carcinoid Johnson GB, Scharf SC, Thompson GB, Yi J, Zhang X, Shen KR. tumor diagnosed incidentally while investigating progressive Use of DOTATATE PET/CT Scan in the Diagnosis and Staging of Thymic Atypical Carcinoid Tumor in a Patient with Second- Cushing syndrome. Computed tomography (CT) scan demon- ary ACTH-dependent Cushing Syndrome: Look Twice and Cut strated a large 2.9 cm exophytic thyroid nodule and a 2.0 cm Once. World J Endoc Surg 2018;10(2):127-133. anterior mediastinal mass. Biopsy of the thyroid nodule demon- strated benign thyroid tissue, and octreotide scan revealed avid Source of support: Nil uptake in the right thyroid lobe with minimal uptake in the thymic Conflict of interest: None tumor. 68Gallium-1,4,7,10-tetraazacyclododecane-N,N′,N″N′″- tetraacetic acid-D-Phe1,Tyr 3-octreotate (Ga-68 DOTATATE) positron emission tomography (PET)/CT scan showed intense INTRODUCTION uptake in the thyroid gland followed by a moderate amount of activity in the anterior mediastinal mass. -

Octreotide Imaging
Nuclear Medicine Patient Information Octreotide Imaging . A radioactive tracer will be administered through the IV. Welcome to VCU Health Nuclear Medicine. We are . An image will be taken 4 hours after your located in the Gateway Building, 2nd floor, 1200 East injection. Marshall Street. Our hours of operation are Monday . You may go on with normal activities in between through Friday, 7 am to 5 pm. Advanced scheduling is the injection and scan (eat and drink as normal). required for all nuclear medicine exams. Please review . You will lie down while the camera takes pictures the following information about your test. Please call of your whole body for 30 minutes. (804) 828-6828 to schedule your test or if you have any . The images will be checked for quality by our questions about your nuclear medicine exam. Physician and more pictures may be needed. Day 2 - 3 What is it? . You will lie down while the camera takes pictures Imaging of tumors bearing somatostatin receptors. of your whole body and possibly a SPECT (360 degree picture of your body) for 1 – 2 hours. 3. Why are you having this test? . The images will be checked for quality by our An Octreotide scan is used for localization of primary and Physician and more pictures may be needed. metastatic neuroendocrine tumors bearing somatostatin receptors. Neuroendocrine relates to the interaction 6. After Care Information between the nervous system and the glands that produce • You may return to all your normal activities. the hormones (endocrine system). This may include, but • Most of the radioactive tracer leaves your body not limited to: carcinoid tumors, neuroendocrine tumors. -

Acr Practice Parameter for the Performance of Gallium-68 Dotatate Pet/Ct for Neuroendocrine Tumors
The American College of Radiology, with more than 30,000 members, is the principal organization of radiologists, radiation oncologists, and clinical medical physicists in the United States. The College is a nonprofit professional society whose primary purposes are to advance the science of radiology, improve radiologic services to the patient, study the socioeconomic aspects of the practice of radiology, and encourage continuing education for radiologists, radiation oncologists, medical physicists, and persons practicing in allied professional fields. The American College of Radiology will periodically define new practice parameters and technical standards for radiologic practice to help advance the science of radiology and to improve the quality of service to patients throughout the United States. Existing practice parameters and technical standards will be reviewed for revision or renewal, as appropriate, on their fifth anniversary or sooner, if indicated. Each practice parameter and technical standard, representing a policy statement by the College, has undergone a thorough consensus process in which it has been subjected to extensive review and approval. The practice parameters and technical standards recognize that the safe and effective use of diagnostic and therapeutic radiology requires specific training, skills, and techniques, as described in each document. Reproduction or modification of the published practice parameter and technical standard by those entities not providing these services is not authorized. Adopted 2018 (Resolution 32)* ACR PRACTICE PARAMETER FOR THE PERFORMANCE OF GALLIUM-68 DOTATATE PET/CT FOR NEUROENDOCRINE TUMORS PREAMBLE This document is an educational tool designed to assist practitioners in providing appropriate radiologic care for patients. Practice Parameters and Technical Standards are not inflexible rules or requirements of practice and are not intended, nor should they be used, to establish a legal standard of care1. -
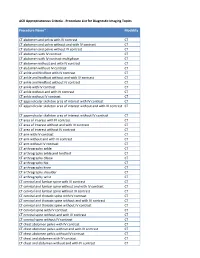
Standard Procedure List – AC Diagnostic Topics
ACR Appropriateness Criteria - Procedure List for Diagnostic Imaging Topics Procedure Name* Modality CT abdomen and pelvis with IV contrast CT CT abdomen and pelvis without and with IV contrast CT CT abdomen and pelvis without IV contrast CT CT abdomen with IV contrast CT CT abdomen with IV contrast multiphase CT CT abdomen without and with IV contrast CT CT abdomen without IV contrast CT CT ankle and hindfoot with IV contrast CT CT ankle and hindfoot without and with IV contrast CT CT ankle and hindfoot without IV contrast CT CT ankle with IV contrast CT CT ankle without and with IV contrast CT CT ankle without IV contrast CT CT appendicular skeleton area of interest with IV contrast CT CT appendicular skeleton area of interest without and with IV contrast CT CT appendicular skeleton area of interest without IV contrast CT CT area of interest with IV contrast CT CT area of interest without and with IV contrast CT CT area of interest without IV contrast CT CT arm with IV contrast CT CT arm without and with IV contrast CT CT arm without IV contrast CT CT arthrography ankle CT CT arthrography ankle and hindfoot CT CT arthrography elbow CT CT arthrography hip CT CT arthrography knee CT CT arthrography shoulder CT CT arthrography wrist CT CT cervical and lumbar spine with IV contrast CT CT cervical and lumbar spine without and with IV contrast CT CT cervical and lumbar spine without IV contrast CT CT cervical and thoracic spine with IV contrast CT CT cervical and thoracic spine without and with IV contrast CT CT cervical and thoracic spine -

Diagnostic Nuclear Medicine Investigations in the Management of Thyroid Cancer Susan E.M
27 Diagnostic Nuclear Medicine Investigations in the Management of Thyroid Cancer Susan E.M. Clarke Introduction cancer, computed tomography (CT) will detect macroscopic lung metastases, brain and liver metastases, and magnetic resonance imaging Whilst radionuclide imaging of the thyroid has (MRI) has proven sensitivity for detecting long been used in the management of patients marrow involvement. with thyroid cancer, its proven role is the subject Although 131I iodine has been used for over 50 of discussion. 131I iodine has a clearly estab- years to image and treat thyroid cancer, it is in lished place in the imaging and treatment of his- the last 20 years that there has been the devel- tologically proven differentiated papillary and opment of many new radiopharmaceuticals follicular thyroid cancer but the role of radio- that are now being used to image patients with nuclide imaging in diagnosis remains con- thyroid cancer. Whilst many of these remain of troversial. Similarly, in patients with medullary research interest only, 18fluorodeoxyglucose thyroid cancer, radionuclide imaging is utilized (18FDG) is rapidly becoming established as a very variably. It is in the centers where there is valuable agent in patients with 131I iodine scan a close collaboration between the thyroid onco- negative disease. logy service and the nuclear medicine depart- Whilst radionuclide imaging is a comple- ment that the contribution of radionuclide mentary imaging technique to other anatomical imaging is most frequently recognized. imaging methods, it has two main advantages. Diagnostic nuclear medicine techniques may The first is the provision of whole-body infor- be used in the detection of metastatic spread mation that facilitates accurate staging at to the skeleton. -

(MIBG) Scintigraphy in Malignant Pheochromocytoma
HUMAN STUDIES Comparison of Radiolabeled Octreotide and Meta-Iodobenzylguanidine (MIBG) Scintigraphy in Malignant Pheochromocytoma Florence Tenenbaum, Jean Lumbroso, Martin Schlumberger, AgnèsMure, Pierre F. Plouin, Bernard Caillou and Claude Parmentier Service de MédecineNucléaireand Service d'Histopathologie, Institut Gustave-Roussy, Vdlejuif, France; and Service d'Hypertension, Hôpital Broussais, Paris, France sympathetic paraganglia (para-aortic paragangliomas or ex Methods: The resultsof in vivo somatostatinscintigraphywere tra-adrenal pheochromocytomas). correlated with those of MIBG from 14 patients, aged 22-66 yr, Malignant behavior characterized by local invasion or by with metastatic pheochromocytoma (10 patients), malignant the presence of chromaffin tissue in sites where it is nor paraganglioma (3 patients) and metastatic ganglioneuroblas- mally absent, i.e., bone, liver and lung occurs in about 10% toma (1 patient). Twelve patients had elevated catecholamine of pheochromocytomas and more frequently in para-aortic excretion. A dynamic study and serial whole-body scans (4-48 paragangliomas (28%-42%) (1-4). The malignancy must hr) were obtained after injection of 130-187 MBq of111In-DTPA- be distinguished from a multicentric disease which is pos Phe-1-octreotide. When indicated, SPECT imaging was done. sible with this kind of tumor. More than 40% of the patients The results were compared to MIBG scans obtained after a do not have métastasesat the time of initial surgery, but diagnostic or a therapeutic dose. Results: Three patients with more than 20 tumor sites on MIBG scans had only 1-9 sites on métastasesare discovered during prolonged follow-up by 111ln-octreotide scintigraphy. Two patients had no MIBG uptake combining urinary measurement of catecholamines and de but one had lung uptake on octreotide scintigraphy. -

Somatostatin-Receptor Scintigraphy in Primary Breast Cancer
Somatostatin-receptor scintigraphy in primary breast cancer Summary Introduction Somatostatin-receptor (SS-R) scintigraphy successfully Somatostatin receptors (SS-R) have been found in shows primary cancers and distant metastases in most neuroendocrine tumours (carcinoids, islet cell tumours, patients with carcinoids, islet cells tumours, and paragangliomas) as well as in meningiomas.1-5 Studies also paragangliomas. Previous in-vitro studies indicated that show SS-Rs in some primary breast cancers,6-9 probably of somatostatin receptors are present in human breast cancers. neuroendocrine origin.8 Antiproliferative effects of We report positive scintigraphy with [111In-DTPA-D-Phe1]- somatostatin analogues have been reported on the growth of breast-cancer cell lines and octreotide in 39 of 52 primary breast cancers (75%). Parallel experimental cancers, including We a new in-vitro autoradiography with [125I-Tyr3]-octreotide of 30 of explants.lO.l1 recently introduced technique in which cancers could be shown in after these showed a corresponding somatostatin-receptor status SS-R-positive vivo, giving radionuclide-labelled somatostatin in 28. Significantly more invasive ductal cancers could be analogue followed by gamma-camera scintigraphy.12-16 In the shown than invasive lobular carcinomas (85% vs 56%; present study we investigated this technique in primary p<0·05). Also the number of T2 cancers which were shown cancers and metastates of 50 patients with breast cancer, was higher than T1 (86% vs 61%; p<0·05). Imaging of the and compared its value in the detection of recurrent disease axillae showed non-palpable cancer-containing lymphnodes in with the serum markers CEA and CA 15-3, which are 4 of 13 with patients subsequently histologically-proven commonly used for this purpose. -

Octreotide Scan
Octreotide Scan Tell your doctor if you are pregnant or breastfeeding. You have scheduled an Octreotide™ study. This study uses a small amount of radioactive material. The level of radioactivity used is extremely low and has no side effects. How do I prepare for my study? • Discontinue taking Somatostatin® 24-48 hours before injection. Discontinue radiation therapy. • Notify your physician if you have a cold or the flu. What will happen during my study? This is a 2 part study. Part 1: We will inject a small amount of radioactive material into a vein in your arm. Part 2 (24 hours later): • We will position you on an imaging table, under a special detector called a gamma camera. The camera will be close to the part of your body being imaged. The camera does not produce any radiation and will not cause any pain or discomfort. • You may also receive a CT scan as part of the imaging procedure to help your doctors read the study. • Sometimes additional imaging is required 48 hours after the injection. Department of Radiology - 1 - Disclaimer: This document contains information and/or instructional materials developed by the University of Michigan Health System (UMHS) for the typical patient with your condition. It may include links to online content that was not created by UMHS and for which UMHS does not assume responsibility. It does not replace medical advice from your health care provider because your experience may differ from that of the typical patient. Talk to your health care provider if you have any questions about this document, your condition or your treatment plan. -

The 2010 Gastrointestinal Cancers Symposium General Session IV: Prevention, Screening and Diagnosis
The 2010 Gastrointestinal Cancers Symposium General Session IV: Prevention, Screening and Diagnosis Abstract #125: The role of octreotide imaging in detecting neuroendocrine tumors (NETS) in 2010: Do we still need it? Speaker: Diane Reidy‐Lagunes, MD – Memorial Sloan Kettering Cancer Center Introduction • The goal of the presentation is to understand the relative utility of CT or MRI (morphologic imaging) and octreotide scan (functional imaging) to detect disease in patients with neuroendocrine tumors. • Many patients in the preoperative/postoperative metastatic setting are actually getting both of these imaging modalities and it is unclear if there is an incremental benefit of using both modalities in detecting neuroendocrine tumors. Background – Neuroendocrine Tumors and Octreotide • Neuroendocrine tumors (NETs) are uncommon tumors that express the neuroendocrine markers synaptophysin and chromogranin. • Per SEER data presented by Dr. Yao the incidence of NETs is increasing. Their prevalence is also increasing as patients live longer with the disease. • Well differentiated NETs typically express somatostatin receptors. • Octreotide is an eight amino analogue of the 14‐amino acid regulatory hormone somatostatin. It binds to tumor cells that have predominantly type 2, 3, 5 somatostatin receptors (SSRT). Octreotide Scan (aka OctreoScanTM) – Background • A diagnostic nuclear medicine imaging modality utilizing an octreotide molecule linked via a chelator to Indium. • Injected and binds to predominantly SSRT 2, 3, 5 when delivered to the cell surface. • Radioactivity is internalized into the cell via endocytosis and a gamma camera takes pictures of tumors to evaluate extent of disease. Comparison of Radiation Exposure and Cost • An Octreotide scan’s radiation exposure is similar to that of a CT scan. -

Recommendations for Medical Imaging Procedures
Recommendations for medical imaging procedures Recommendation by the German Commission on Radiological Protection Adopted at the 300th SSK meeting on 27 June 2019 For many decades, diagnostic imaging has been an indispensable tool of ensure referral guidelines modern medicine to clarify diagnostic questions, thus allowing for the for medical imaging, taking planning of appropriate individual treatments. Some examination methods into account the radiation such as X-ray or nuclear medical diagnostics involve ionising radiation or doses, are available to the radioactive substances. In view of the radiological exposure involved in referrers. such procedures, physicians must consider carefully whether a different The Federal Environment diagnostic method with less or no radiation exposure, such as ultrasound Ministry, being responsible for radiological protection, has for many years or magnetic resonance procedures, might not be at least equally well advocated keeping the number of applications involving radiation suited for a specific patient. Therefore the Recommendations for medical exposure as low as possible. There is constant enhancement of imaging procedures address first of all physicians referring patients for diagnostic procedures and therefore these recommendations are further diagnostics. The goal is to avoid unnecessary radiation exposure reviewed and updated on a regular basis. while achieving the same level of diagnostic accuracy. I would like to thank the German Commission on Radiological Protection, the The recommendations list the most suitable imaging procedures for various medical associations involved and in particular the working group under various diagnostic questions. However, physicians must still provide in the chair of Professor Reinhard Loose for their work. each individual case the justifying indication for the selected examination method and document it.