Contraction Stress Test (Oxytocin Challenge Test) WW.04.05
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Fetal Assement Methods
12/3/2020 Fetal Assement Methods 1 up to 9% of exam 5 to 9 questions 13.00 Adjunct Fetal Surveillance Methods 10%) 13.01 Auscultation (Intermittent Auscultation- IA) 13.02 Fetal movement counting 13.03 Nonstress testing 13.04 Fetal acid base interpretation – will be covered in a separate section 13.05 Biophysical profile 13.06 Fetal Acoustic Stimulation 2 1 12/3/2020 HERE IS ONE FOR YOU!! AWW… Skin to Skin in the OR ☺ 3 Auscultation 4 2 12/3/2020 Benefits of Auscultation • Based on Random Control Trials, neonatal outcomes are comparable to those monitored with EFM • Lower CS rates • Technique is non-invasive • Widespread application is possible • Freedom of movement • Lower cost • Hands on Time and one to one support are facilitated 5 Limitation of Auscultation • Use of the Fetoscope may limit the ability to hear FHR ( obesity, amniotic fluid, pt. movement and uterine contractions) • Certain FHR patterns cannot be detected – variability and some decelerations • Some women may think IA is intrusive • Documentation is not automatic • Potential to increase staff for 1:1 monitoring • Education, practice and skill assessment of staff 6 3 12/3/2020 Auscultation • Non-electronic devices such as a Fetoscope or Stethoscope • No longer common practice in the United States though may be increasing due to patient demand • Allows listening to sounds associated with the opening and closing of ventricular valves via bone conduction • Can hear actual heart sounds 7 Auscultation Fetoscope • A Fetoscope can detect: • FHR baseline • FHR Rhythm • Detect accelerations and decelerations from the baseline • Verify an FHR irregular rhythm • Can clarify double or half counting of EFM • AWHONN, (2015), pp. -

Guidelines for Perinatal Care, 8Th Ed., Pp. 48-49, 198-205 ACOG Practice Bulletin, No 145, July 2014, Reaffirmed 2016 JOGNN, No
Guidelines for Perinatal Care, 8th ed., pp. 48-49, 198-205 ACOG Practice Bulletin, No 145, July 2014, Reaffirmed 2016 JOGNN, No. 44, pp. 683-686, 2015 Terminology and interpretation of electronic fetal monitoring tracings as defined by National Institute of Child Health and Development (NICHD) Maternal Health Competencies - Fetal Assessment & Antenatal Fetal Surveillance Fetal Heart Tones (Beginning at 10 Weeks Gestation with hand-held Doppler) 1. Review provider or standing order 2. Explain procedure and obtains patient's verbal consent 3. Perform hand hygiene prior to engaging with patient 4. Assist patient into semi-recumbent position, expose abdomen 5. Locate the point of loudest fetal heart tones and a. Palpate maternal pulse b. Utilize pulse oximetry (placed on maternal index finger) 6. Monitor maternal pulse and count fetal heart rate for 1 full minute 7. Record findings 8. Demonstrate knowledge of fetal heart rate ranges: a. Normal = 110-160 bpm b. Bradycardia = < 110 bpm c. Tachycardia = > 160 bpm 9. Demonstrate knowledge of criteria for notifying provider of concerns/findings before, during, or after assessment (per clinical policies) Fundal Height (Beginning at 12 to 14 Weeks gestation) 1. Review provider or standing order 2. Explain procedure and obtain patient's verbal consent 3. Perform hand hygiene prior to engaging with patient 4. Assist patient to semi-recumbent position, expose abdomen 5. Ensure the abdomen is soft and palpates with 2 hands to locate the uterine fundus 6. Measure from top of fundus to top of symphysis pubis using a pliable, non-elastic tape measure, keeping the tape measure in contact with the skin, and measuring along the longitudinal axis without correcting to the abdominal midline 7. -

The Empire Plan SEPTEMBER 2018 REPORTING ON
The Empire Plan SEPTEMBER 2018 REPORTING ON PRENATAL CARE Every baby deserves a healthy beginning and you can take steps before your baby is even born to help ensure a great start for your infant. That’s why The Empire Plan offers mother and baby the coverage you need. When your primary coverage is The Empire Plan, the Empire Plan Future Moms Program provides you with special services. For Empire Plan enrollees and for their enrolled dependents, COBRA enrollees with their Empire Plan benefits and Young Adult Option enrollees TABLE OF CONTENTS Five Important Steps ........................................ 2 Feeding Your Baby ...........................................11 Take Action to Be Healthy; Breastfeeding and Your Early Pregnancy ................................................. 4 Empire Plan Benefits .......................................12 Prenatal Testing ................................................. 5 Choosing Your Baby’s Doctor; New Parents ......................................................13 Future Moms Program ......................................7 Extended Care: Medical Case High Risk Pregnancy Program; Management; Questions & Answers ...........14 Exercise During Pregnancy ............................ 8 Postpartum Depression .................................. 17 Your Healthy Diet During Pregnancy; Medications and Pregnancy ........................... 9 Health Care Spending Account ....................19 Skincare Products to Avoid; Resources ..........................................................20 Childbirth Education -

Recommended Guidelines for Perinatal Care in Georgia
Section Two: Recommended Guidelines for Perinatal Care in Georgia Table of Contents Introduction to the Seventh Edition 3 Section I. Strategy for Action 4-8 Section II. Preconception and Interconception Health Care 9-10 Section III. Antepartum Care 11-15 Section IV. Intrapartum Care 16-24 Section V. Postpartum Care 25-27 Section VI. Perinatal Infections 28-30 Appendices Appendix A1. Perinatal Consultation and Transport Guidelines Georgia 31 Appendix A2. Suggested Parameters for Implementing Guidelines for Neonatal/ Maternal Transport 32-33 Appendix A3. Suggested Medical Criteria when determining the need for Consultation of Transport of the Maternal/Neonatal/Patient 34-35 Appendix A4. Perinatal Consultation/Transport Agreement 36 Appendix A5. Regional Perinatal Centers 37 Appendix B. Georgia Guidelines for Early Newborn Discharge, Minimal Criteria for Newborn Discharge, Late Preterm Discharge and Recommendation for Discharge Education Minimum Criteria for Newborn Discharge 38- 40 Appendix C. Capabilities of Health Care Providers in Hospital Delivery, Basic, Specialty and Specialty Care 41-42 Appendix D. Definitions Capabilities and Health Care Provider Types: Neonatal Levels of Care 43-44 Appendix F. Risk Identification 45 Appendix G. Maps of Georgia’s Counties Health Districts and Regions 46-50 Appendix H. Maternal and Child Health Sites 51-56 2 Introduction to the Seventh Edition This document, the Recommended Guidelines for Perinatal Care in Georgia, henceforth referred to as Guidelines, is the most comprehensive version to date. It is the culmination of work done by members and staff of the Regional Perinatal Centers and the Georgia Department of Public health (DPH), Division of Maternal & Child Health Section. This is the Third Edition under the title Recommended Guidelines for Perinatal Care in Georgia. -

OBGYN-Study-Guide-1.Pdf
OBSTETRICS PREGNANCY Physiology of Pregnancy: • CO input increases 30-50% (max 20-24 weeks) (mostly due to increase in stroke volume) • SVR anD arterial bp Decreases (likely due to increase in progesterone) o decrease in systolic blood pressure of 5 to 10 mm Hg and in diastolic blood pressure of 10 to 15 mm Hg that nadirs at week 24. • Increase tiDal volume 30-40% and total lung capacity decrease by 5% due to diaphragm • IncreaseD reD blooD cell mass • GI: nausea – due to elevations in estrogen, progesterone, hCG (resolve by 14-16 weeks) • Stomach – prolonged gastric emptying times and decreased GE sphincter tone à reflux • Kidneys increase in size anD ureters dilate during pregnancy à increaseD pyelonephritis • GFR increases by 50% in early pregnancy anD is maintaineD, RAAS increases = increase alDosterone, but no increaseD soDium bc GFR is also increaseD • RBC volume increases by 20-30%, plasma volume increases by 50% à decreased crit (dilutional anemia) • Labor can cause WBC to rise over 20 million • Pregnancy = hypercoagulable state (increase in fibrinogen anD factors VII-X); clotting and bleeding times do not change • Pregnancy = hyperestrogenic state • hCG double 48 hours during early pregnancy and reach peak at 10-12 weeks, decline to reach stead stage after week 15 • placenta produces hCG which maintains corpus luteum in early pregnancy • corpus luteum produces progesterone which maintains enDometrium • increaseD prolactin during pregnancy • elevation in T3 and T4, slight Decrease in TSH early on, but overall euthyroiD state • linea nigra, perineum, anD face skin (melasma) changes • increase carpal tunnel (median nerve compression) • increased caloric need 300cal/day during pregnancy and 500 during breastfeeding • shoulD gain 20-30 lb • increaseD caloric requirements: protein, iron, folate, calcium, other vitamins anD minerals Testing: In a patient with irregular menstrual cycles or unknown date of last menstruation, the last Date of intercourse shoulD be useD as the marker for repeating a urine pregnancy test. -

Non Stress Test – an Update Archana Mishra1* and Pikee Saxena2
Research Article Journal of Gynecology & Reproductive Medicine Non Stress Test – An Update Archana Mishra1* and Pikee Saxena2 *Corresponding author 1Assistant Professor, Department of Obstetrics and Gynecology, Archana Mishra, Assistant Professor, Department of Obstetrics VMMC & SJH, New Delhi. and Gynecology, VMMC & SJH, New Delhi, E-mail: pikeesaxena@ hotmail.com. 2Professor, Department of Obstetrics and Gynecology, LHMC & SSKH, New Delhi. Submitted: 15 Feb 2017; Accepted: 31 July 2017; Published: 09 Sep 2017 Abstract Non stress test is a time tested, convenient and reliable test of antenatal fetal surveillance. It accurately predicts those fetus that do not require acute or premature obstetric intervention and thereby prevents pregnancies from being subjected to unnecessary iatrogenic risks and avoids unnecessary medical, financial and emotional burden. The principle of non stress test is that the heart rate of a fetus with adequate oxygenation and normal neurological response will temporarily accelerate with fetal movement. Loss of reactivity is commonly associated with a fetal sleep cycle but may result from any cause of central nervous system depression, fetal acidosis or maternal drug intake and requires further evaluation for an extended period or evaluation with other techniques like biophysical profile or amniotic fluid testing or umbilical artery Doppler study as per the overall clinical scenario. A correctly performed NST, using standard technique with proper interpretation may be of great value in planning further management. Introduction rate variation, absence of foetal heart rate accelerations, and the The objective of antenatal care is to prevent adverse maternal and appearance of spontaneous late decelerations. perinatal outcome. Technological advancement and understanding of fetal physiology has enabled us to decrease perinatal mortality to Indications of Non Stress Test some extent. -

Antepartum Fetal Heart Rate Testing
Antepartum Fetal Surveillance Dr. M. Mokhtari Associate Professor of OB GYN Primary Goal The primary goal is to identify fetuses at risk of intrauterine death or neonatal complications and intervene (often by delivery) to prevent these adverse outcomes, if possible. NORMAL FETAL MOVEMENT Sonographically fetal activity can be noted as early as 7 to 8 weeks of gestation. Maternal perception of fetal movement begins around 16 to 20 weeks of gestation. The mother's first perception of fetal movement, termed "quickening," is often described as a gentle flutter . Fetal movement increases throughout day, with peak activity late at night. Kick counts ●Perception of least 10 fetal movements (FMs) over up to two hours when the mother is at rest and focused on counting ("count to 10" method) . Patients are instructed to contact within 12 hours for further evaluation if they perceive a significant and persistent reduction in fetal movement and never to wait longer than two hours if there is absent. DIFFERENTIAL DIAGNOSIS Transient decreases in fetal activity: fetal sleep states, maternal medications eg, sedatives), or maternal smoking Kick counts ●Perception of least 10 fetal movements (FMs) over up to two hours when the mother is at rest and focused on counting ("count to 10" method) . Patients are instructed to contact within 12 hours for further evaluation if they perceive a significant and persistent reduction in fetal movement and never to wait longer than two hours if there is absent. DIFFERENTIAL DIAGNOSIS Transient decreases in fetal activity: -

Glossary of Terms for Childbirth
Glossary of Terms for Childbirth Abruptio placenta (placenta abruption): Partial or complete separation of the placenta from the wall of the uterus before the baby is born. Can cause the mother to hemorrhage possibly requiring a Cesarean delivery. Asynclitic: An asynclitic birth or asynclitism refers to the position of a baby in the uterus such that the head is tilted to the side, causing the fetal head to no longer be in line with the birth canal. Most asynclitism corrects spontaneously in the progress of normal labor. Persistence of asynclitism is usually a signal of other problems with dystocia. Afterbirth: The placenta and amniotic membranes. These are expelled from the uterus during the third stage of labor. Amniocentesis: The removal of a small amount of amniotic fluid from the amniotic sac. Used to test for chromosomes, for fetal lung maturity or for amniotic infection. Amniotic sac: Thin membranes that surround the baby inside the uterus filled with amniotic fluid. Analgesia: The absence of the sense of pain without loss of consciousness. Anesthesia: The loss of body sensation. General anesthesia is loss of consciousness caused by anesthetics. Local anesthesia limits loss of sensation to one area of the body. Apgar score: A numerical evaluation of a newborn at one and five minutes after birth. Scores are based on activity (tone), pulse, grimace (reflexes), appearance (skin color) and respiration. Areola: The dark area of the breast surrounding the nipple. Birth canal: The passageway from the uterus through the vagina. Braxton-Hicks contractions: Irregular contractions that may become somewhat uncomfortable near the end of pregnancy. -

The Role of Non-Stress Test As a Method to Evaluate the Outcome of High-Risk Pregnancy: a Tertiary Care Center Experience
International Surgery Journal Singh S et al. Int Surg J. 2020 Jun;7(6):1782-1787 http://www.ijsurgery.com pISSN 2349-3305 | eISSN 2349-2902 DOI: http://dx.doi.org/10.18203/2349-2902.isj20202033 Original Research Article The role of non-stress test as a method to evaluate the outcome of high-risk pregnancy: a tertiary care center experience Shreya Singh1*, H. K. Premi2, Ranjana Gupta2 1Department of Obstetrics and Gynecology, MCH Wing, Chandauli, UP, India 2Department of Obstetrics and Gynecology, Rohilkhand Medical College and Hospital, Bareilly, UP, India Received: 12 April 2020 Revised: 27 April 2020 Accepted: 28 April 2020 *Correspondence: Dr. Shreya Singh, E-mail: [email protected] Copyright: © the author(s), publisher and licensee Medip Academy. This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. ABSTRACT Background: Non-stress test (NST) is a graphical recording of changes in fetal heart activity and uterine contraction along with fetal movement when uterus is quiescent. NST is primarily a test of fetal condition and it differs from contraction stress test which is a test of uteroplacental function. The present study aimed at evaluating the efficacy and diagnostic value of NST for antenatal surveillance in high-risk pregnancy and comparing the mode of delivery with test results. Methods: A clinical study of NST was done between November 2014 to October 2015. NST was used for their surveillance from 32 weeks of gestation and NST was recorded weekly, biweekly, on alternate days or even on daily basis depending on high risk factors and were followed up. -

Nonstress Test and Contraction Stress Test - Uptodate
2019/3/14 Nonstress test and contraction stress test - UpToDate Official reprint from UpToDate® www.uptodate.com ©2019 UpToDate, Inc. and/or its affiliates. All Rights Reserved. Nonstress test and contraction stress test Author: David A Miller, MD Section Editor: Charles J Lockwood, MD, MHCM Deputy Editor: Vanessa A Barss, MD, FACOG All topics are updated as new evidence becomes available and our peer review process is complete. Literature review current through: Feb 2019. | This topic last updated: Jan 16, 2018. INTRODUCTION Fetal health is evaluated, in part, by assessment of fetal heart rate (FHR) patterns. The primary goal is to identify fetuses at risk of intrauterine death or neonatal complications and intervene (often by delivery) to prevent these adverse outcomes, if possible. The nonstress test (NST) and the contraction stress test (CST) are used for antepartum FHR testing. An abnormal test (nonreactive NST, positive CST) is sometimes associated with adverse fetal or neonatal outcomes, while a normal test (reactive NST, negative CST) is usually associated with a neurologically intact and adequately oxygenated fetus. When interpreting these tests, the clinician needs to account for gestational age, prior results of fetal assessment, maternal conditions (including medications), and fetal condition (eg, growth restriction, anemia, arrhythmia). The NST and CST will be reviewed here. Intrapartum fetal evaluation and additional techniques for assessing fetal health are discussed separately. ● (See "Intrapartum fetal heart rate assessment".) ● (See "The fetal biophysical profile".) ● (See "Decreased fetal movement: Diagnosis, evaluation, and management".) ● (See "Doppler ultrasound of the umbilical artery for fetal surveillance".) PHYSIOLOGIC BASIS OF FETAL HEART RATE CHANGES Physiologic development of the fetal heart occurs across gestation and affects fetal heart rate (FHR) patterns. -
Prenatal Checkups and Tests
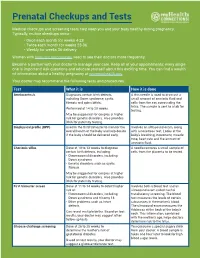
Prenatal Checkups and Tests Medical checkups and screening tests help keep you and your baby healthy during pregnancy. Typically, routine checkups occur: • Once each month for weeks 4-28 • Twice each month for weeks 28-36 • Weekly for weeks 36-delivery Women with high-risk pregnancies need to see their doctors more frequently. Become a partner with your doctor to manage your care. Keep all of your appointments: every single one is important! Ask questions and educate yourself about this exciting time. You can find a wealth of information about a healthy pregnancy at womenshealth.gov. Your doctor may recommend the following tests and procedures: Test What it is How it is done Amniocentesis Diagnoses certain birth defects, A thin needle is used to draw out a including Down syndrome, cystic small amount of amniotic fluid and fibrosis and spina bifida. cells from the sac surrounding the fetus. The sample is sent to a lab for Performed at 14 to 20 weeks. testing. May be suggested for couples at higher risk for genetic disorders. Also provides DNA for paternity testing. Biophysical profile (BPP) Used in the third trimester to monitor the Involves an ultrasound exam, along overall health of the baby and help decide with a nonstress test. Looks at the if the baby should be delivered early. baby’s breathing, movement, muscle tone, heart rate and the amount of amniotic fluid. Chorionic villus Done at 10 to 13 weeks to diagnose A needle removes a small sample of certain birth defects, including: cells from the placenta to be tested. -

HMO Benefit Guidelines Revision Date: 01/01/2019 Effective Date: 01/01/2019
Blue Shield of California Original Date: 01/01/1999 HMO Benefit Guidelines Revision Date: 01/01/2019 Effective Date: 01/01/2019 Maternity Care Benefit Coverage Prenatal and postnatal physician office visits, including prenatal diagnosis of genetic disorders of the fetus by means of diagnostic procedures in cases of high-risk pregnancy. All necessary inpatient hospital services for normal delivery, Cesarean section, complications of pregnancy and routine newborn circumcision. The Newborns and Mothers Health Protection Act of 1997 requires health plans to provide a minimum hospital stay for the mother and newborn child of 48 hours after a normal vaginal delivery. A minimum hospital stay for the mother and newborn child of 96 hours is required after a C-section unless the attending physician, in consultation with the mother, determines a shorter hospital length of stay is adequate. Note: If the mother is not covered as a subscriber or spouse by the Blue Shield HMO plan, and the newborn qualifies as a dependent of the subscriber, newborn nursery charges are eligible for coverage for the first 31 days under the subscriber’s inpatient hospital benefits, subject to standard Coordination of Benefit rules as applicable. This coverage applies regardless of whether the newborn is added to the subscriber’s plan. California law requires coverage for a follow-up visit for the mother and newborn within 48 hours of discharge when prescribed by the treating physician, if the hospital stay is less than 48 hours after a normal, vaginal delivery or less than 96 hours after a C-section. This visit shall be provided by a licensed health care provider whose scope of practice includes postpartum and newborn care.