Milia: a Review and Classification
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
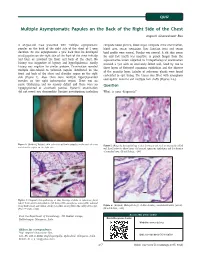
Multiple Asymptomatic Papules on the Back of the Right Side of the Chest Angoori Gnaneshwar Rao
QUIZ Multiple Asymptomatic Papules on the Back of the Right Side of the Chest Angoori Gnaneshwar Rao A 43-year-old male presented with multiple asymptomatic complete blood picture, blood sugar, complete urine examination, papules on the back of the right side of the chest of 1 year blood urea, serum creatinine, liver function tests and serum duration. He was asymptomatic a year back then he developed lipid profile were normal. Fundus was normal. A slit skin smear small papules on the right side of the front of the chest initially for acid fast bacilli was negative. A punch biopsy from the and later on involved the front and back of the chest. No representative lesion subjected to histopathological examination history was suggestive of leprosy and hyperlipidemias. Family revealed a cyst with an intricately folded wall, lined by two to history was negative for similar problem. Examination revealed three layers of flattened squamous epithelium and the absence multiple skin-colored to yellowish papules distributed on the of the granular layer. Lobules of sebaceous glands were found front and back of the chest and shoulder region on the right embedded in cyst lining. The lumen was filled with amorphous side [Figure 1]. Also, there were multiple hyperpigmented eosinophilic material and multiple hair shafts [Figures 2-4]. macules on the right infrascapular region. There was no nerve thickening and no sensory deficit and there were no Question hypopigmented or anesthetic patches. Systemic examination did not reveal any abnormality. Routine investigations including What is your diagnosis? (Original) Multiple skin-colored to yellowish papules on the back of chest Figure 1: Figure 2: (Original) Histopathology of skin showing a cyst with an intricately folded and shoulder region on the right side wall lined by two to three layers of flattened squamous epithelium and the absence of granular layer. -

Neonatal Dermatology Review
NEONATAL Advanced Desert DERMATOLOGY Dermatology Jennifer Peterson Kevin Svancara Jonathan Bellew DISCLOSURES No relevant financial relationships to disclose Off-label use of acitretin in ichthyoses will be discussed PHYSIOLOGIC Vernix caseosa . Creamy biofilm . Present at birth . Opsonizing, antibacterial, antifungal, antiparasitic activity Cutis marmorata . Reticular, blanchable vascular mottling on extremities > trunk/face . Response to cold . Disappears on re-warming . Associations (if persistent) . Down syndrome . Trisomy 18 . Cornelia de Lange syndrome PHYSIOLOGIC Milia . Hard palate – Bohn’s nodules . Oral mucosa – Epstein pearls . Associations . Bazex-Dupre-Christol syndrome (XLD) . BCCs, follicular atrophoderma, hypohidrosis, hypotrichosis . Rombo syndrome . BCCs, vermiculate atrophoderma, trichoepitheliomas . Oro-facial-digital syndrome (type 1, XLD) . Basal cell nevus (Gorlin) syndrome . Brooke-Spiegler syndrome . Pachyonychia congenita type II (Jackson-Lawler) . Atrichia with papular lesions . Down syndrome . Secondary . Porphyria cutanea tarda . Epidermolysis bullosa TRANSIENT, NON-INFECTIOUS Transient neonatal pustular melanosis . Birth . Pustules hyperpigmented macules with collarette of scale . Resolve within 4 weeks . Neutrophils Erythema toxicum neonatorum . Full term . 24-48 hours . Erythematous macules, papules, pustules, wheals . Eosinophils Neonatal acne (neonatal cephalic pustulosis) . First 30 days . Malassezia globosa & sympoidalis overgrowth TRANSIENT, NON-INFECTIOUS Miliaria . First weeks . Eccrine -

Basal Cell Carcinoma: Topical Therapy Versus Surgical Treatment
Journal of the Saudi Society of Dermatology & Dermatologic Surgery (2012) 16,41–51 King Saud University Journal of the Saudi Society of Dermatology & Dermatologic Surgery www.ksu.edu.sa www.jssdds.org www.sciencedirect.com REVIEW ARTICLE Basal cell carcinoma: Topical therapy versus surgical treatment Khalifa E. Sharquie a,*, Adil A. Noaimi b,1 a Scientific Council of Dermatology and Venereology, Iraqi Board for Medical Specializations, Iraq b Department of Dermatology and Venereology, College of Medicine, University of Baghdad, Iraq Received 1 November 2011; revised 7 June 2012; accepted 7 June 2012 Available online 6 July 2012 KEYWORDS Abstract Basal cell carcinoma (BCC) is a non-melanoma skin cancer and is one of the commonest Basal cell carcinoma; malignancies of the skin encountered in daily clinical practice. It derives from non-keratinizing cells Topical therapy of BCC by that originate in the basal layer of the epidermis. It accounts for approximately 75% of all skin can- podophylline; cer in the world, and 53.2% in Iraqi patients. Generally, most BCC cases are sporadic, but it may Surgical treatment also appear in genetic disorders such as Gorlin’s syndrome, Rombo’s syndrome, and xeroderma pigmentosa (XP). If left untreated, BCC will continue to invade locally and may result in substantial tissue damage that compromises function and cosmetic look. Metastasis is an extremely rare event. The tumor characteristically develops on sun-exposed skin of lighter-skinned individuals. There are two main modalities of therapy including topical like: Imiquimod, 5-fluorouracil (5- FU), photodynamic therapy (PDT), radiation therapy (RT), topical & intralesional zinc sulfate and topical 25% podophylline. -

Northwestern University, October 2003
CHICAGO DERMATOLOGICAL SOCIETY CASE # 1 Presented by James Swan, M.D., Mary Martini, M.D. and Keren Horn, M.D. Department of Dermatology, Feinberg School of Medicine, Northwestern University HISTORY OF PRESENT ILLNESS This 45 year-old Caucasian male presented for a problem-focused exam of a right upper extremity lesion. However, complete physical exam revealed peri-orbital slate-gray hyperpigmentation as well as generalized bronze hyperpigmentation in sun-exposed areas, prompting questions regarding these abnormalities. Other abnormalities in pigment included approximately 10 café au lait macules, nearly all greater than 1.5cm in size. Axillary freckling was also noted. Review of systems was positive for migraine headaches, arthritis, decreased libido and fatigue (the patient sleeps greater than 12 hours each night without feeling refreshed). PAST MEDICAL HISTORY Right orbital tumor status post excision 2001 Depression MEDICATIONS Depakote Remeron ALLERGIES Amoxicillin (angioedema) FAMILY HISTORY Brother with the same pigmentation anomalies. Both his father and his sister died of liver cancer; his sister passed away at 40 years of age. SOCIAL HISTORY The patient does not drink alcohol and has smoked one pack of cigarettes per day for the past 30 years. He is on disability due to “depression” and exhaustion which make it unable for him to sustain an eight hour work day. PHYSICAL EXAM There is peri-orbital slate-gray hyperpigmentation as well as generalized bronze hyperpigmentation in sun-exposed areas. In addition, the patient has approximately 10 café au lait macules, nearly all greater than 1.5cm in size. Axillary freckling is also noted, and there are protuberances of the left elbow and right knee. -

2016 Essentials of Dermatopathology Slide Library Handout Book
2016 Essentials of Dermatopathology Slide Library Handout Book April 8-10, 2016 JW Marriott Houston Downtown Houston, TX USA CASE #01 -- SLIDE #01 Diagnosis: Nodular fasciitis Case Summary: 12 year old male with a rapidly growing temple mass. Present for 4 weeks. Nodular fasciitis is a self-limited pseudosarcomatous proliferation that may cause clinical alarm due to its rapid growth. It is most common in young adults but occurs across a wide age range. This lesion is typically 3-5 cm and composed of bland fibroblasts and myofibroblasts without significant cytologic atypia arranged in a loose storiform pattern with areas of extravasated red blood cells. Mitoses may be numerous, but atypical mitotic figures are absent. Nodular fasciitis is a benign process, and recurrence is very rare (1%). Recent work has shown that the MYH9-USP6 gene fusion is present in approximately 90% of cases, and molecular techniques to show USP6 gene rearrangement may be a helpful ancillary tool in difficult cases or on small biopsy samples. Weiss SW, Goldblum JR. Enzinger and Weiss’s Soft Tissue Tumors, 5th edition. Mosby Elsevier. 2008. Erickson-Johnson MR, Chou MM, Evers BR, Roth CW, Seys AR, Jin L, Ye Y, Lau AW, Wang X, Oliveira AM. Nodular fasciitis: a novel model of transient neoplasia induced by MYH9-USP6 gene fusion. Lab Invest. 2011 Oct;91(10):1427-33. Amary MF, Ye H, Berisha F, Tirabosco R, Presneau N, Flanagan AM. Detection of USP6 gene rearrangement in nodular fasciitis: an important diagnostic tool. Virchows Arch. 2013 Jul;463(1):97-8. CONTRIBUTED BY KAREN FRITCHIE, MD 1 CASE #02 -- SLIDE #02 Diagnosis: Cellular fibrous histiocytoma Case Summary: 12 year old female with wrist mass. -

Pili Torti: a Feature of Numerous Congenital and Acquired Conditions
Journal of Clinical Medicine Review Pili Torti: A Feature of Numerous Congenital and Acquired Conditions Aleksandra Hoffmann 1 , Anna Wa´skiel-Burnat 1,*, Jakub Z˙ ółkiewicz 1 , Leszek Blicharz 1, Adriana Rakowska 1, Mohamad Goldust 2 , Małgorzata Olszewska 1 and Lidia Rudnicka 1 1 Department of Dermatology, Medical University of Warsaw, Koszykowa 82A, 02-008 Warsaw, Poland; [email protected] (A.H.); [email protected] (J.Z.);˙ [email protected] (L.B.); [email protected] (A.R.); [email protected] (M.O.); [email protected] (L.R.) 2 Department of Dermatology, University Medical Center of the Johannes Gutenberg University, 55122 Mainz, Germany; [email protected] * Correspondence: [email protected]; Tel.: +48-22-5021-324; Fax: +48-22-824-2200 Abstract: Pili torti is a rare condition characterized by the presence of the hair shaft, which is flattened at irregular intervals and twisted 180◦ along its long axis. It is a form of hair shaft disorder with increased fragility. The condition is classified into inherited and acquired. Inherited forms may be either isolated or associated with numerous genetic diseases or syndromes (e.g., Menkes disease, Björnstad syndrome, Netherton syndrome, and Bazex-Dupré-Christol syndrome). Moreover, pili torti may be a feature of various ectodermal dysplasias (such as Rapp-Hodgkin syndrome and Ankyloblepharon-ectodermal defects-cleft lip/palate syndrome). Acquired pili torti was described in numerous forms of alopecia (e.g., lichen planopilaris, discoid lupus erythematosus, dissecting Citation: Hoffmann, A.; cellulitis, folliculitis decalvans, alopecia areata) as well as neoplastic and systemic diseases (such Wa´skiel-Burnat,A.; Zółkiewicz,˙ J.; as cutaneous T-cell lymphoma, scalp metastasis of breast cancer, anorexia nervosa, malnutrition, Blicharz, L.; Rakowska, A.; Goldust, M.; Olszewska, M.; Rudnicka, L. -

Differential Diagnosis of the Scalp Hair Folliculitis
Acta Clin Croat 2011; 50:395-402 Review DIFFERENTIAL DIAGNOSIS OF THE SCALP HAIR FOLLICULITIS Liborija Lugović-Mihić1, Freja Barišić2, Vedrana Bulat1, Marija Buljan1, Mirna Šitum1, Lada Bradić1 and Josip Mihić3 1University Department of Dermatovenereology, 2University Department of Ophthalmology, Sestre milosrdnice University Hospital Center, Zagreb; 3Department of Neurosurgery, Dr Josip Benčević General Hospital, Slavonski Brod, Croatia SUMMARY – Scalp hair folliculitis is a relatively common condition in dermatological practice and a major diagnostic and therapeutic challenge due to the lack of exact guidelines. Generally, inflammatory diseases of the pilosebaceous follicle of the scalp most often manifest as folliculitis. There are numerous infective agents that may cause folliculitis, including bacteria, viruses and fungi, as well as many noninfective causes. Several noninfectious diseases may present as scalp hair folli- culitis, such as folliculitis decalvans capillitii, perifolliculitis capitis abscendens et suffodiens, erosive pustular dermatitis, lichen planopilaris, eosinophilic pustular folliculitis, etc. The classification of folliculitis is both confusing and controversial. There are many different forms of folliculitis and se- veral classifications. According to the considerable variability of histologic findings, there are three groups of folliculitis: infectious folliculitis, noninfectious folliculitis and perifolliculitis. The diagno- sis of folliculitis occasionally requires histologic confirmation and cannot be based -
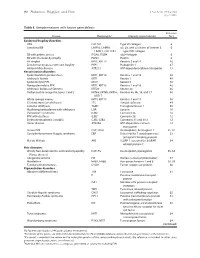

Table I. Genodermatoses with Known Gene Defects 92 Pulkkinen
92 Pulkkinen, Ringpfeil, and Uitto JAM ACAD DERMATOL JULY 2002 Table I. Genodermatoses with known gene defects Reference Disease Mutated gene* Affected protein/function No.† Epidermal fragility disorders DEB COL7A1 Type VII collagen 6 Junctional EB LAMA3, LAMB3, ␣3, 3, and ␥2 chains of laminin 5, 6 LAMC2, COL17A1 type XVII collagen EB with pyloric atresia ITGA6, ITGB4 ␣64 Integrin 6 EB with muscular dystrophy PLEC1 Plectin 6 EB simplex KRT5, KRT14 Keratins 5 and 14 46 Ectodermal dysplasia with skin fragility PKP1 Plakophilin 1 47 Hailey-Hailey disease ATP2C1 ATP-dependent calcium transporter 13 Keratinization disorders Epidermolytic hyperkeratosis KRT1, KRT10 Keratins 1 and 10 46 Ichthyosis hystrix KRT1 Keratin 1 48 Epidermolytic PPK KRT9 Keratin 9 46 Nonepidermolytic PPK KRT1, KRT16 Keratins 1 and 16 46 Ichthyosis bullosa of Siemens KRT2e Keratin 2e 46 Pachyonychia congenita, types 1 and 2 KRT6a, KRT6b, KRT16, Keratins 6a, 6b, 16, and 17 46 KRT17 White sponge naevus KRT4, KRT13 Keratins 4 and 13 46 X-linked recessive ichthyosis STS Steroid sulfatase 49 Lamellar ichthyosis TGM1 Transglutaminase 1 50 Mutilating keratoderma with ichthyosis LOR Loricrin 10 Vohwinkel’s syndrome GJB2 Connexin 26 12 PPK with deafness GJB2 Connexin 26 12 Erythrokeratodermia variabilis GJB3, GJB4 Connexins 31 and 30.3 12 Darier disease ATP2A2 ATP-dependent calcium 14 transporter Striate PPK DSP, DSG1 Desmoplakin, desmoglein 1 51, 52 Conradi-Hu¨nermann-Happle syndrome EBP Delta 8-delta 7 sterol isomerase 53 (emopamil binding protein) Mal de Meleda ARS SLURP-1 -

A Deep Learning System for Differential Diagnosis of Skin Diseases
A deep learning system for differential diagnosis of skin diseases 1 1 1 1 1 1,2 † Yuan Liu , Ayush Jain , Clara Eng , David H. Way , Kang Lee , Peggy Bui , Kimberly Kanada , ‡ 1 1 1 Guilherme de Oliveira Marinho , Jessica Gallegos , Sara Gabriele , Vishakha Gupta , Nalini 1,3,§ 1 4 1 1 Singh , Vivek Natarajan , Rainer Hofmann-Wellenhof , Greg S. Corrado , Lily H. Peng , Dale 1 1 † 1, 1, 1, R. Webster , Dennis Ai , Susan Huang , Yun Liu * , R. Carter Dunn * *, David Coz * * Affiliations: 1 G oogle Health, Palo Alto, CA, USA 2 U niversity of California, San Francisco, CA, USA 3 M assachusetts Institute of Technology, Cambridge, MA, USA 4 M edical University of Graz, Graz, Austria † W ork done at Google Health via Advanced Clinical. ‡ W ork done at Google Health via Adecco Staffing. § W ork done at Google Health. *Corresponding author: [email protected] **These authors contributed equally to this work. Abstract Skin and subcutaneous conditions affect an estimated 1.9 billion people at any given time and remain the fourth leading cause of non-fatal disease burden worldwide. Access to dermatology care is limited due to a shortage of dermatologists, causing long wait times and leading patients to seek dermatologic care from general practitioners. However, the diagnostic accuracy of general practitioners has been reported to be only 0.24-0.70 (compared to 0.77-0.96 for dermatologists), resulting in over- and under-referrals, delays in care, and errors in diagnosis and treatment. In this paper, we developed a deep learning system (DLS) to provide a differential diagnosis of skin conditions for clinical cases (skin photographs and associated medical histories). -

The Comparison of Blood Lipid Profile in Patients with and Without Androgenetic Alopecia
ORIGINAL ARTICLE DOI: 10.4274/jtad.galenos.2020.76486 J Turk Acad Dermatol 2020;14(1):12-18 The Comparison of Blood Lipid Profile in Patients with and Without Androgenetic Alopecia Tuğba Akın, Zekayi Kutlubay, Özge Aşkın Istanbul University-Cerrahpasa, Cerrahpasa Faculty of Medicine, Department of Dermatology, Istanbul, Turkey ABSTRACT Background: Androgenetic alopecia (AGA) is the most common cause of hair loss in both sexes. In several studies investigating the relationship between AGA and dyslipidemia, conflicting results have been reported. In this study, we aimed to compare serum triglyceride (TG) and high- density lipoprotein (HDL) cholesterol levels that one of the criteria of metabolic syndrome in male patients with and without AGA. Materials and Methods: The study group was consisted of 40 patients who had 2 and higher AGA. The control group was consisted of 40 patients aged who had no AGA at the clinical examination or who had stage 1 AGA. Fasting serum TG and HDL cholesterol levels were compared between study and control groups. Results: The mean serum TG values in the study group were 89.60; the mean serum TG values in the control group were 85.40. There was no statistical difference in serum TG values between the two groups (p<0.005). The number of patients with serum TG value ≥150 mg/dL was 5 (12.5%) in the study group and 3 (7.5%) in the control group; however, this difference was not statistically significant too (p<0.005). Mean serum HDL cholesterol levels in the study group were 52.67; the mean serum HDL cholesterol values in the control group were 52.62. -

Follicular Atrophoderma and Pseudopelade Associated with Chondrodystrophia Calcificans Congenita* Helen Ollendorff Curth, M.D
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Elsevier - Publisher Connector FOLLICULAR ATROPHODERMA AND PSEUDOPELADE ASSOCIATED WITH CHONDRODYSTROPHIA CALCIFICANS CONGENITA* HELEN OLLENDORFF CURTH, M.D. In 1943 Miescher (1) reported peculiar atrophic changes of the skin of body and scalp in a 7 year old Swiss girl. There were spots of atrophic alopecia on the scalp, and on the extremities and trunk irregular zones in which dimple-like depressions were found at the place of follicular orifices. The child was very small and had thoracic kyphoscoliosis, lumbar lordosis, luxation of the right hip, a considerably shortened right leg, and a moderately shortened left arm. Five years earlier, Burckhardt (2) has described the skeletal condition of the same child, then 2 years old, as chondrodystrophia foetalis calcarea. In the Eng- lish speaking countries this disease is called chondrodystrophia calcificans congenita, chondro- osseous dystrophy with punctate epiphyseal dysplasia, or similar variations. Several cases of this newly described syndrome of cutaneous and skeletal changes have lately been seen in New York. REPORT OF CA5E5 1. C. S. (3), an 8 year old Jewish girl, was hora in the United States. The parents of the child were horn in Poland. They have three children, of whom the patient is the second. The father, mother, a sister aged 10, and a brother aged 5, are small hut do not present the characteristic cutaneous or skeletal changes to he described. The mother was well during her second pregnancy. The child was horn spontaneously at full term. Immediately after birth the mother noticed that large parts of the scalp and body were covered by red crusts, some tiny, others confluent and forming large adherent masses. -
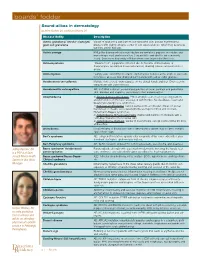

Boards' Fodder
boards’ fodder Sound-alikes in dermatology by Jeffrey Kushner, DO, and Kristen Whitney, DO Disease Entity Description Actinic granuloma/ Annular elastolytic Variant of granuloma annulare on sun-damaged skin; annular erythematous giant cell granuloma plaques with slightly atrophic center in sun-exposed areas, which may be precipi- tated by actinic damage. Actinic prurigo PMLE-like disease with photodistributed erythematous papules or nodules and hemorrhagic crust and excoriation. Conjunctivitis and cheilitis are commonly found. Seen more frequently in Native Americans (especially Mestizos). Actinomycetoma “Madura Foot”; suppurative infection due to Nocaria, Actinomadura, or Streptomyces resulting in tissue tumefaction, draining sinuses and extrusion of grains. Actinomycosis “Lumpy Jaw”; Actinomyces israelii; erythematous nodules at the angle of jaw leads to fistulous abscess that drain purulent material with yellow sulfur granules. Acrokeratosis verruciformis Multiple skin-colored, warty papules on the dorsal hands and feet. Often seen in conjunction with Darier disease. Acrodermatitis enteropathica AR; SLC39A4 mutation; eczematous patches on acral, perineal and periorificial skin; diarrhea and alopecia; secondary to zinc malabsorption. Atrophoderma 1) Atrophoderma vermiculatum: Pitted atrophic scars in a honeycomb pattern around follicles on the face; associated with Rombo, Nicolau-Balus, Tuzun and Braun-Falco-Marghescu syndromes. 2) Follicular atrophoderma: Icepick depressions at follicular orifices on dorsal hands/feet or cheeks; associated with Bazex-Dupré-Christol and Conradi- Hünermann-Happle syndromes. 3) Atrophoderma of Pasini and Pierini: Depressed patches on the back with a “cliff-drop” transition from normal skin. 4) Atrophoderma of Moulin: Similar to Pasini/Pierini, except lesions follow the lines of Blaschko. Anetoderma Localized area of flaccid skin due to decreased or absent elastic fibers; exhibits “buttonhole” sign.