Variability of the Lateral Ligamentous Complex of the Knee
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

June 3, 2016 Karen B. Desalvo, M.D., M.P.H., M.Sc. Acting Assistant
June 3, 2016 Karen B. DeSalvo, M.D., M.P.H., M.Sc. Acting Assistant Secretary Department of Health and Human Services Office of the National Coordinator for Health Information Technology Attention: RFI Regarding Assessing Interoperability for MACRA 330 C Street, SW, Room 7025A Washington, DC 20201 Subject: Office of the National Coordinator for Health Information Technology; Medicare Access and CHIP Reauthorization Act of 2015; Request for Information Regarding Assessing Interoperability for MACRA Dear Acting Assistant Secretary DeSalvo: The American Association of Orthopaedic Surgeons (AAOS) and orthopaedic specialty societies, representing over 18,000 board-certified orthopaedic surgeons, appreciate the opportunity to provide comments on the Request for Information Regarding Assessing Interoperability for MACRA by the Office of the National Coordinator (ONC) for Health Information Technology, and published in the Federal Register on April 8, 2016. The AAOS has been committed to working with ONC in the adoption of electronic health records. As surgical specialists, we have unique Health Information Technology (HIT) needs and respectfully offer some suggestions to improve interoperability to better reflect the needs of our surgical specialists and their patients and accelerate HIT adoption in the future by orthopaedic surgeons. The AAOS thanks ONC in advance for its solicitation and consideration of the following comments and concerns. We have structured our comments in the order that ONC is soliciting public feedback in the RFI document referenced above. Scope of Measurement: Defining Interoperability and Population The focus of measurement should not be limited to “meaningful Electronic Health Records (EHR) users,” as defined (e.g., eligible professionals, eligible hospitals, and CAHs that attest to meaningful use of certified EHR technology under CMS’ Medicare and Medicaid EHR Incentive Programs), and their exchange partners. -

Avulsion of the Anterior Lateral Meniscal Root Secondary to Tibial Eminence Fracture
Avulsion of the Anterior Lateral Meniscal Root Secondary to Tibial Eminence Fracture Publish date: May 8, 2018 Authors: Travis J. Menge, MD Jorge Chahla, MD Justin J. Mitchell, MD Chase S. Dean, MD and Robert F. LaPrade, MD Author Affiliation | Disclosures Authors’ Disclosure Statement: Dr. LaPrade reports that he receives royalties and is a paid consultant for Smith and Nephew, Arthrex, and Össur. Dr. Menge reports that he is a paid consultant for Smith and Nephew. Dr. Mitchell reports that he has received educational and grant support from Arthrex, Smith and Nephew, and DJO, LLC. The other authors report no actual or potential conflict of interest in relation to this article. Dr. Menge is an Orthopaedic and Sports Medicine Surgeon, Spectrum Health Medical Group, Grand Rapids, Michigan. Dr. Mitchell is an Orthopaedic and Sports Medicine Surgeon, Gundersen Health System, La Crosse, Wisconsin. Dr. Chahla is a Clinical Fellow, Cedars Sinai Kerlan Jobe Institute, Santa Monica, California. Dr. Dean is an Orthopaedic Surgical Resident, University of Colorado Hospital, Denver, Colorado. Dr. LaPrade is an Orthopaedic Complex Knee and Sports Medicine Surgeon, and Chief Medical Officer and Co-Director of the Sports Medicine Fellowship, Steadman Philippon Research Institute, The Steadman Clinic, Vail, Colorado. Address correspondence to: Robert F. LaPrade MD, PhD, Steadman Philippon Research Institute, The Steadman Clinic, 181 West Meadow Drive, Suite 400, Vail, Colorado 81657 (email, [email protected]). Am J Orthop. 2018;47(5). Copyright Frontline Medical Communications Inc. 2018. All rights reserved. Take-Home Points Root tears of all meniscal attachments have been described. A comprehensive anatomic understanding of the meniscal roots is of utmost importance to suspect root lesions. -

ACR Appropriateness Criteria® Acute Trauma to the Knee
Revised 2019 American College of Radiology ACR Appropriateness Criteria® Acute Trauma to the Knee Variant 1: Adult or child 5 years of age or older. Fall or acute twisting trauma to the knee. No focal tenderness, no effusion, able to walk. Initial imaging. Procedure Appropriateness Category Relative Radiation Level Radiography knee May Be Appropriate ☢ Bone scan with SPECT or SPECT/CT knee Usually Not Appropriate ☢☢☢ CT knee with IV contrast Usually Not Appropriate ☢ CT knee without and with IV contrast Usually Not Appropriate ☢ CT knee without IV contrast Usually Not Appropriate ☢ MR arthrography knee Usually Not Appropriate O MRA knee without and with IV contrast Usually Not Appropriate O MRA knee without IV contrast Usually Not Appropriate O MRI knee without and with IV contrast Usually Not Appropriate O MRI knee without IV contrast Usually Not Appropriate O US knee Usually Not Appropriate O Variant 2: Adult or child 5 years of age or older. Fall or acute twisting trauma to the knee. One or more of the following: focal tenderness, effusion, inability to bear weight. Initial imaging. Procedure Appropriateness Category Relative Radiation Level Radiography knee Usually Appropriate ☢ Bone scan with SPECT or SPECT/CT knee Usually Not Appropriate ☢☢☢ CT knee with IV contrast Usually Not Appropriate ☢ CT knee without and with IV contrast Usually Not Appropriate ☢ CT knee without IV contrast Usually Not Appropriate ☢ MR arthrography knee Usually Not Appropriate O MRA knee without and with IV contrast Usually Not Appropriate O MRA knee without IV contrast Usually Not Appropriate O MRI knee without and with IV contrast Usually Not Appropriate O MRI knee without IV contrast Usually Not Appropriate O US knee Usually Not Appropriate O ACR Appropriateness Criteria® 1 Acute Trauma to the Knee Variant 3: Adult or skeletally mature child. -

Hip, Knee Joints and Ankle Joints
Hip, knee joints and ankle joints Musculoskeletal block- Anatomy-lecture 18 Editing file Color guide : Only in boys’ slides in Green Only in girls’ slides in Purple Objectives Important in Red Doctor’s notes in Blue Extra information in Grey ✓ List the type & articular surfaces of hip joint , knee joint and ankle joint. ✓ Describe the ligaments of hip joints and ankle joint. ✓ Describe movements of hip joint, knee joint and ankle joint. ✓ Describe the capsule of knee joint, its extra- & intra-capsular ligaments. ✓ List important bursae in relation to knee joint. ✓ Apply Hilton’s law about nerve supply of knee joints. ● Type: a synovial, ball & socket joint The Hip Joint ● Articular surfaces: -acetabulum of hip (pelvic bone) Ligaments: -head of the femur Intracapsular Extracapsular Transverse Ligament Iliofemoral Pubofemoral Ischiofemoral Acetabular labrum acetabular of femoral ligament ligament ligament ligament head -Fibro-cartilaginous Converts Carries -Y shaped - Antero- inferior -Posterior to collar acetabular notch vessels to -Anterior to to joint joint -Attached to margins into foramen head of joint of acetabulum → (acetabular foramen) femur -Limits -Limits -Limits medial increases its depth through which the extension abduction and rotation for better retaining acetabular vessels lateral rotation of head of femur pass Pictures in the following slide Intracapsular Extracapsular Movements Hip Dislocations Congenital • More common in girls and Medial Lateral associated with inability to adduct Flexion Extension Abduction Adduction -

The ITB Conundrum
TRAINING DOCTOR’S ORDERS impingement syndrome, otherwise known The ITB as a painful ITB. Upon learning the diagno- sis, the patient often responds, “I hate this stu- Conundrum pid ITB.” As my mom taught me, it’s never good to By Jordan D. Metzl, M.D. hate. Rather, a better course is to understand and fix the problem. The iliotibial band (ITB) is a thick tendon that connects the tensor fas- cia lata muscle—which starts on the outside of he scenario goes something like this: the hip—to the outside part of the tibia, the A triathlete comes walking into the major bone in the lower leg. The ITB cross- T office with a confused look on his face. es two joints, the hip and the knee, and helps “Doc, here’s the deal,” he says. “My knee is control the angle of the lower leg with run- fine when I walk into your office, it’s fine when ning. It can also cause a pain in the hip called I’m walking around town, but after 10 minutes trochanteric bursitis, a pinching on the outside of running, it’s killing me!” of the hip joint. In the knee, a tight ITB caus- “Where does it hurt?” I ask. “It’s here, just es a similar pinching. on the outside of my knee, where the bone So what actually causes the pain in ITB bumps out just above my knee,” he says. “After impingement syndrome? There is a little flu- I’ve run for 10 minutes, it starts to feel as id filled sack called a bursa that sits between the though someone is jabbing the outside of my tendon and the outside of the femur bone, knee with a needle.” Hearing this much of the area called the lateral femoral condyle in the story, even before the physical exam or the knee and the greater trochanter in the X-rays, I am almost always ready to make hip. -

Femur Tibia Fibula Patella Lateral Meniscus Medial Meniscus Anterior
3213 Eastlake Ave E, Suite A, Seattle, WA 98102 4300 198th Street SW, Lynnwood, WA 98036 Anatomy of the Knee Overview The knee is the body's largest joint. It's the place Femur where three bones meet: the tibia, the femur and the patella. The knee is a "hinge" joint. It allows the leg to bend in one direction only. Let's take a closer look at the main parts of the knee's anatomy. Patella Bones The base of the knee is formed by the tibia. This bone, also called the "shinbone," is the large bone of the lower leg. The smaller bone of the lower leg, called the "fibula," connects to the tibia just below the knee. It is not part of the joint. Above this is the Tibia femur, which is also known as the "thighbone." This is the longest, largest and heaviest bone of the body. The patella, commonly called the "kneecap," Fibula covers and protects the front of the knee joint. Articular Cartilage Within the knee, the surfaces of the bones are covered with a layer of articular cartilage. This tough, smooth tissue protects the bones. It allows them to glide smoothly as the knee flexes and Articular extends. Cartilage Menisci Between the tibia and femur are two thick pads called "menisci." Each one individually is called a "meniscus." These are made of cartilage. They act Anterior Posterior as cushions for the two rounded protrusions on the Cruciate Cruciate end of the femur, which are called the "condyles." Ligament Ligament Cruciate Ligaments The tibia and the femur are connected to each Lateral Medial other by a pair of strong bands of tissue called Meniscus Meniscus "cruciate ligaments." The anterior cruciate ligament is commonly called the "ACL." The posterior cruciate ligament is commonly called the "PCL." These ligaments cross each other like an X in the center of the knee. -
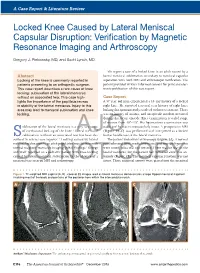
Locked Knee Caused by Lateral Meniscal Capsular Disruption: Verification by Magnetic Resonance Imaging and Arthroscopy
A Case Report & Literature Review G. J. Pinkowsky and S. Lynch Locked Knee Caused by Lateral Meniscal Capsular Disruption: Verification by Magnetic Resonance Imaging and Arthroscopy Gregory J. Pinkowsky, MD, and Scott Lynch, MD We report a case of a locked knee in an adult caused by a Abstract lateral meniscal subluxation secondary to meniscal capsular Lockingf o the knee is commonly reported in separation with both MRI and arthroscopic verification. The patients presenting to an orthopedic surgeon. patient provided written informed consent for print and elec- This case report describes a rare cause of knee tronic publication of this case report. locking: subluxation of the lateral meniscus without an associated tear. This case high- Case Report lights the importance of the popliteus recess A 57-year-old man experienced a 10-day history of a locked in stability of the lateral meniscus. Injury to this right knee. He reported a several year history of right knee area may lead to meniscal subluxation and knee locking that spontaneously resolved without treatment. There locking. was no history of trauma, and no specific incident occurred during this recent episode. Knee examination revealed range of motion from 10°-115°. His ligamentous examination was ubluxation of the lateral meniscus is a very rare cause stable and he was neurovascularly intact. A preoperative MRI of mechanical locking of the knee.1 LateralAJO meniscal (Figure 1A-C) was performed and interpreted as a locked S subluxation without an associated tear has been de- bucket handle tear of the lateral meniscus. scribed in several case reports.1-3 Locking caused by lateral The patient underwent arthroscopy (Figure 2A). -

Intraosseous Bioplasty for a Subchondral Cyst in the Lateral Condyle of Femur
Journal of Clinical Medicine Brief Report Intraosseous Bioplasty for a Subchondral Cyst in the Lateral Condyle of Femur Anish G.R. Potty 1,2,3, Ashim Gupta 1,4,5,6 , Hugo C. Rodriguez 1,2 , Ian W. Stone 2 and Nicola Maffulli 7,8,9,* 1 South Texas Orthopaedic Research Institute, Laredo, TX 78045, USA; [email protected] (A.G.R.P.); [email protected] (A.G.); [email protected] (H.C.R.) 2 School of Osteopathic Medicine, University of the Incarnate Word, San Antonio, TX 78209, USA; [email protected] 3 Laredo Sports Medicine Clinic, Laredo, TX 78041, USA 4 Department of Psychology, Illinois Wesleyan University, Bloomington, IL 61701, USA 5 Future Biologics, Lawrenceville, GA 30043, USA 6 BioIntegrate, Lawrenceville, GA 30043, USA 7 Department of Musculoskeletal Disorders, School of Medicine and Surgery, University of Salerno, 84084 Fisciano, Italy 8 Barts and the London School of Medicine and Dentistry, Centre for Sports and Exercise Medicine, Queen Mary University of London, London E1 4DG, UK 9 School of Pharmacy and Bioengineering, Keele University Faculty of Medicine, Stoke on Trent ST4 7QB, UK * Correspondence: n.maff[email protected] Received: 7 April 2020; Accepted: 4 May 2020; Published: 6 May 2020 Abstract: Several conditions can lead to the development of a subchondral cyst. The mechanism by which the cysts form, their location, and their severity depend on the underlying pathology, although the exact pathogenesis is not fully elucidated. Treatment options vary according to the location of the cyst, with less invasive procedures such as calcium phosphate cement injection to a joint arthroplasty when there is an extensive cyst in communication with the joint space. -

Species - Domesticus (Chicken) to Mammals (Human Being)
Int. J. LifeSc. Bt & Pharm. Res. 2013 Sunil N Tidke and Sucheta S Tidke, 2013 ISSN 2250-3137 www.ijlbpr.com Vol. 2, No. 4, October 2013 © 2013 IJLBPR. All Rights Reserved Research Paper MORPHOLOGY OF KNEE JOINT - CLASS- AVES - GENUS - GALLUS, - SPECIES - DOMESTICUS (CHICKEN) TO MAMMALS (HUMAN BEING) Sunil N Tidke1* and Sucheta S Tidke2 *Corresponding Author: Sunil N Tidke [email protected] In the present investigation, a detailed comparison is made between the human knee and the knee of chicken (Gallus domesticus), with the object of determining similarities or variation of structure and their possible functional significance, if any special attention has been paid to bone taking part in joint, the surrounding muscles and tendons, which play an important part in stabilizing these joints, the form and attachments of the intraarticular menisci, which have been credited with the function of ensuring efficient lubrication throughout joints movement, and to the ligaments, the function of which is disputed. Keywords: Bony articular part, Intra capsular and extra capsular structure and Muscular changes INTRODUCTION patella. A narrow groove on the lateral condyle of femur articulate with the head of the fibula and The manner in which the main articulations of intervening femoro fibular disc. The tibia has a the vertebrate have become variously modified enormous ridge and crest for the insertion of the in relation to diverse function has been patellar tendon and origin of the extensor muscle. investigated by many workers, notably, Parsons The cavity of the joint communicates above and (1900) and Haines (1942). The morphology of the below the menisci with the central part of joint knee joint of human has been studied in great around the cruciate ligament. -

Gross Anatomy of the Lower Limb. Knee and Ankle Joint. Walking
Gross anatomy of the lower limb. Knee and ankle joint. Walking. Sándor Katz M.D.,Ph.D. Knee joint type: trochoginglimus (hinge and pivot) Intracapsular ligaments: • Anterior cruciate lig. • Posterior cruciate lig. • Transverse lig. • Posterior meniscofemoral .lig. Medial meniscus: C- shaped. Lateral meniscus: almost a complete ring. Knee joint Extracapsular ligaments. Tibial collateral lig. is broader and fuses with the articular capsule and medial meniscus. Fibular collateral lig. is cord-like and separates from the articular capsule. Knee joint - extracapsular ligaments Knee joint - bursae Knee joint - movements • Flexion: 120-130° • Hyperextension: 5° • Voluntary rotation: 50-60° • Terminal rotation: 10° Ankle (talocrural) joint type: hinge Talocrural joint - medial collateral ligament Medial collateral = deltoid ligament Tibionavicular part (1) (partly covers the anterior tibiotalar part) Tibiocalcaneal part (2-3) Posterior tibiotalar part (4) Medial process (6) Sustentaculum tali (7) Tendon of tibialis posterior muscles (9) Talocrural joint - lateral collateral ligament Lateral collateral ligament Anterior talofibular ligament (5, 6) Calcaneofibular ligament (10) Lateral malleolus (1) Tibia (2) Syndesmosis tibiofibularis (3, 4) Talus (7) Collum tali (8) Caput tali (9) Interosseous talocalcaneal ligament (11) Cervical ligament (12) Talonavicular ligament (13) Navicular bone (14) Lateral collateral ligament Posterior talofibular ligament (5) Fibula (1) Tibia (2) Proc. tali, tuberculum laterale (3) Proc. tali, tuberculum mediale (11) Tendo, musculus felxor hallucis longus (8) Lig. calcaneofibulare (12) Tendo, musculus peroneus brevis (13) Tendo, musculus peroneus longus (14) Art. subtalaris (15) Talocrural joint - movements Dorsiflexion: 15° Plantarfelxion: 40° Talotarsal joint (lower ankle joint): talocalcaneonavicular joint and subtalar joint Bony surfaces: anterior and middle talar articular surfaces and head of the talus + anterior and middle calcaneal articular surfaces, navicular. -

Lab Activity 9
Lab Activity 9 Appendicular Skeleton Martini Chapter 8 Portland Community College BI 231 Appendicular Skeleton • Upper & Lower extremities • Shoulder Girdle • Pelvic Girdle 2 Humerus 3 Humerus: Proximal End Greater tubercle Lesser tubercle Head: Above the epiphyseal line Anatomical Neck Surgical neck Intertubercular groove Anterior Medial Posterior4 Deltoid Tuberosity 5 Radial Groove 6 Trochlea (Distal Humerus) Anterior Posterior Anterior Posterior 7 Capitulum (Distal Humerus) Anterior Posterior Anterior Posterior 8 Olecranon Fossa (Distal Humerus) Anterior Posterior Anterior Posterior 9 Medial Epicondyle (Distal Humerus) Anterior Posterior Anterior Posterior 10 Lateral Epicondyle (Distal Humerus) Anterior Posterior Anterior Posterior 11 Radial Fossa (Distal Humerus) Anterior Posterior Anterior Posterior 12 Coronoid Fossa (Distal Humerus) Anterior Posterior Anterior Posterior 13 Lateral Supracondylar Ridge (Distal Humerus) Anterior Posterior Anterior Posterior 14 Medial Supracondylar Ridge (Distal Humerus) Anterior Posterior Anterior Posterior 15 Humerus: Distal End/Anterior Medial Lateral Supracondylar Supracondylar Ridge Ridge Coronoid Fossa Radial fossa Lateral Medial Epicondyle Epicondyle Capitulum Trochlea 16 Humerus: Distal End/Posterior Olecranon Fossa Medial Epicondyle Lateral Epicondyle Trochlea 17 Radius • “Rotates” • On the thumb side of the forearm 18 Radius: Head 19 Radial Tuberosity 20 Ulnar Notch of the Radius 21 Ulnar Notch of the Radius 22 Radius: Interosseous Ridge 23 Styloid Process of the Radius 24 Radius Distal Anterior -

Meniscus Tear Handout 503-293-0161
® ® Sports Injury medIcIne depArTmenT 9250 SW Hall Blvd., Tigard, OR 97223 Meniscus Tear Handout 503-293-0161 WHAT IS IT? The meniscus is a C-shaped piece of cartilage in the knee that cushions and acts as a shock absorber between your thigh bone (femur) and shin bone (tibia). You have both an inner (medial) and outer (lateral) meniscus that help distribute the forces in the knee when you are weight-bearing. Meniscal tears can occur when the knee is forcefully twisted, sustains a direct blow, deep squatting or during activities that require changing directions. As we age, this cartilage begins to lose elasticity and can easily be torn without any type of trauma. Meniscal (Cartilage) Tear Lateral meniscus (torn) Femur (thighbone) Top view Tibia (shinbone) Medical meniscus Front view of knee WHAT ARE THe SYMPTOMS? Pain and swelling are the most common signs of an injury to your meniscus. If the tear occurs from a sudden injury, you may feel/hear a pop at the time of the injury. Swelling after the injury can often gradually increase over a 1-2 day period. You may also feel like your knee is “locked” where you are unable to move it through the full range of motion. If your tear is more of a chronic degenerative tear, you may just have symptoms of pain, swelling & stiffness off and on based on your activity level. WHy DOES IT HURT? At first it just hurts because of the fresh injury and swelling. Later it hurts when you move your knee and the torn pieces get caught between the bones and pull on the meniscus.