Apolipoprotein M Attenuates Doxorubicin Cardiotoxicity by Regulating Transcription Factor EB
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Decreased Plasma Concentrations of Apolipoprotein M in Sepsis And
Kumaraswamy et al. Critical Care 2012, 16:R60 http://ccforum.com/content/16/2/R60 RESEARCH Open Access Decreased plasma concentrations of apolipoprotein M in sepsis and systemic inflammatory response syndromes Sunil B Kumaraswamy1, Adam Linder2, Per Åkesson2 and Björn Dahlbäck1* Abstract Introduction: Apolipoprotein M (apoM) is present in 5% of high-density lipoprotein (HDL) particles in plasma. It is a carrier of sphingosine-1-phosphate (S1P), which is important for vascular barrier protection. The aim was to determine the plasma concentrations of apoM during sepsis and systemic inflammatory response syndrome (SIRS) and correlate them to levels of apolipoprotein A-I (apoA1), apolipoprotein B (apoB), HDL-, and low-density lipoprotein (LDL)-cholesterol. Methods: Plasma samples from patients with (1), severe sepsis with shock (n = 26); (2), severe sepsis without shock (n = 44); (3), sepsis (n = 100); (4), infections without SIRS (n = 43); and (5) SIRS without infection (n = 20) were analyzed. The concentrations of apoM, apoA1, and apoB were measured with enzyme-linked immunosorbent assays (ELISAs). Total, HDL-, and LDL-cholesterol concentrations were measured with a commercial HDL/LDL cholesterol test. Results: ApoM concentrations correlated negatively to acute-phase markers. Thus, apoM behaved as a negative acute-phase protein. Decreased values were observed in all patient groups (P < 0.0001), with the most drastic decreases observed in the severely sick patients. ApoM levels correlated strongly to those of apoA1, apoB, HDL, and LDL cholesterol. The HDL and LDL cholesterol levels were low in all patient groups, as compared with controls (P < 0.0001), in particular, HDL cholesterol. ApoA1 and apoB concentrations were low only in the more severely affected patients. -

Systematic Genetic Analysis of the MHC Region Reveals Mechanistic
RESEARCH ARTICLE Systematic genetic analysis of the MHC region reveals mechanistic underpinnings of HLA type associations with disease Matteo D’Antonio1,2†, Joaquin Reyna2,3†, David Jakubosky3,4, Margaret KR Donovan4,5, Marc-Jan Bonder6, Hiroko Matsui1, Oliver Stegle6, Naoki Nariai2‡, Agnieszka D’Antonio-Chronowska1,2, Kelly A Frazer1,2* 1Institute for Genomic Medicine, University of California, San Diego, San Diego, United States; 2Department of Pediatrics, Rady Children’s Hospital, University of California, San Diego, San Diego, United States; 3Biomedical Sciences Graduate Program, University of California, San Diego, La Jolla, United States; 4Bioinformatics and Systems Biology Graduate Program, University of California, San Diego, San Diego, United States; 5Department of Biomedical Informatics, University of California, San Diego, San Diego, United States; 6European Molecular Biology Laboratory, European Bioinformatics Institute, Cambridge, United Kingdom Abstract The MHC region is highly associated with autoimmune and infectious diseases. Here we conduct an in-depth interrogation of associations between genetic variation, gene expression and disease. We create a comprehensive map of regulatory variation in the MHC region using WGS from 419 individuals to call eight-digit HLA types and RNA-seq data from matched iPSCs. Building on this regulatory map, we explored GWAS signals for 4083 traits, detecting colocalization for 180 *For correspondence: disease loci with eQTLs. We show that eQTL analyses taking HLA type haplotypes into account [email protected] have substantially greater power compared with only using single variants. We examined the † These authors contributed association between the 8.1 ancestral haplotype and delayed colonization in Cystic Fibrosis, equally to this work postulating that downregulation of RNF5 expression is the likely causal mechanism. -

1 Characterizing the Emergence of Liver and Gallbladder
bioRxiv preprint doi: https://doi.org/10.1101/718775; this version posted July 30, 2019. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. Page 1 Characterizing the Emergence of Liver and Gallbladder from the Embryonic Endoderm through Single-Cell RNA-Seq Tianhao Mu1,2,3,4§, Liqin Xu5,6,7§, Yu Zhong5,6,8§, Xinyu Liu4,9§, Zhikun Zhao5,6, Chaoben Huang3, Xiaofeng Lan3, Chengchen Lufei4,9, Yi Zhou4,9, Yixun Su1,3, Luang Xu9, Miaomiao Jiang5,6, Hongpo Zhou5,6, Xinxin Lin5,6, Liang Wu5,6, Siqi Peng5,6, Shiping Liu5,6, Susanne Brix7, Michael Dean10, Norris R. Dunn11, Kenneth S. Zaret12, Xin-Yuan Fu1,2,3,4,9,13*& Yong Hou5,6* 1 Department of Biochemistry, YLL School of Medicine, National University of Singapore, Singapore 119615, Singapore. 2 Laboratory of Human Diseases and Immunotherapies, West China Hospital, Sichuan University, Chengdu 610041, China. 3 Department of Biology, Southern University of Science and Technology, Shenzhen 518055, China. 4 GenEros Biopharma, Hangzhou 310018, China. 5 BGI-Shenzhen, Shenzhen 518083, China. 6 China National GeneBank, BGI-Shenzhen, Shenzhen 518120, China. 7 Department of Biotechnology and Biomedicine, Technical University of Denmark, Soltofts Plads, 2800 Kongens Lyngby, Denmark. 8 School of Biology and Biological Engineering, South China University of Technology, Guangzhou 510006, China. 1 bioRxiv preprint doi: https://doi.org/10.1101/718775; this version posted July 30, 2019. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. -

(LCN) Gene Family, Including Evidence the Mouse Mup Cluster Is Result of an “Evolutionary Bloom” Georgia Charkoftaki1, Yewei Wang1, Monica Mcandrews2, Elspeth A
Charkoftaki et al. Human Genomics (2019) 13:11 https://doi.org/10.1186/s40246-019-0191-9 REVIEW Open Access Update on the human and mouse lipocalin (LCN) gene family, including evidence the mouse Mup cluster is result of an “evolutionary bloom” Georgia Charkoftaki1, Yewei Wang1, Monica McAndrews2, Elspeth A. Bruford3, David C. Thompson4, Vasilis Vasiliou1* and Daniel W. Nebert5 Abstract Lipocalins (LCNs) are members of a family of evolutionarily conserved genes present in all kingdoms of life. There are 19 LCN-like genes in the human genome, and 45 Lcn-like genes in the mouse genome, which include 22 major urinary protein (Mup)genes.TheMup genes, plus 29 of 30 Mup-ps pseudogenes, are all located together on chromosome (Chr) 4; evidence points to an “evolutionary bloom” that resulted in this Mup cluster in mouse, syntenic to the human Chr 9q32 locus at which a single MUPP pseudogene is located. LCNs play important roles in physiological processes by binding and transporting small hydrophobic molecules —such as steroid hormones, odorants, retinoids, and lipids—in plasma and other body fluids. LCNs are extensively used in clinical practice as biochemical markers. LCN-like proteins (18–40 kDa) have the characteristic eight β-strands creating a barrel structure that houses the binding-site; LCNs are synthesized in the liver as well as various secretory tissues. In rodents, MUPs are involved in communication of information in urine-derived scent marks, serving as signatures of individual identity, or as kairomones (to elicit fear behavior). MUPs also participate in regulation of glucose and lipid metabolism via a mechanism not well understood. -

Supporting Information
Supporting Information Poulogiannis et al. 10.1073/pnas.1009941107 SI Materials and Methods Loss of Heterozygosity (LOH) Analysis of PARK2. Seven microsatellite Bioinformatic Analysis of Genome and Transcriptome Data. The markers (D6S1550, D6S253, D6S305, D6S955, D6S980, D6S1599, aCGH package in R was used to identify significant DNA copy and D6S396) were amplified for LOH analysis within the PARK2 number (DCN) changes in our collection of 100 sporadic CRCs locus using primers that were previously described (8). (1) (Gene Expression Omnibus, accession no. GSE12520). The MSP of the PARK2 Promoter. CpG sites within the PARK2 promoter aCGH analysis of cell lines and liver metastases was derived region were detected using the Methprimer software (http://www. from published data (2, 3). Chromosome 6 tiling-path array- urogene.org/methprimer/index.html). Methylation-specificand CGH was used to identify the smallest and most frequently al- control primers were designed using the Primo MSP software tered regions of DNA copy number change on chromosome 6. (http://www.changbioscience.com/primo/primom.html); bisulfite An integrative approach was used to correlate expression pro- modification of genomic DNA was performed as described pre- files with genomic copy number data from a SNP array from the viously (9). All tumor DNA samples from primary CRC tumors same tumors (n = 48) (4) (GSE16125), using Pearson’s corre- (n = 100) and CRC lines (n = 5), as well as those from the leukemia lation coefficient analysis to identify the relationships between cell lines KG-1a (acute myeloid leukemia, AML), U937 (acute DNA copy number changes and gene expression of those genes lymphoblastic leukemia, ALL), and Raji (Burkitt lymphoma, BL) SssI located within the small frequently altered regions of DCN were screened as part of this analysis. -
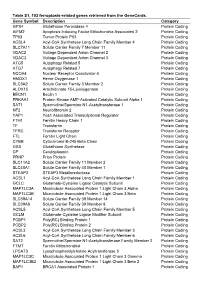
Table S1. 103 Ferroptosis-Related Genes Retrieved from the Genecards
Table S1. 103 ferroptosis-related genes retrieved from the GeneCards. Gene Symbol Description Category GPX4 Glutathione Peroxidase 4 Protein Coding AIFM2 Apoptosis Inducing Factor Mitochondria Associated 2 Protein Coding TP53 Tumor Protein P53 Protein Coding ACSL4 Acyl-CoA Synthetase Long Chain Family Member 4 Protein Coding SLC7A11 Solute Carrier Family 7 Member 11 Protein Coding VDAC2 Voltage Dependent Anion Channel 2 Protein Coding VDAC3 Voltage Dependent Anion Channel 3 Protein Coding ATG5 Autophagy Related 5 Protein Coding ATG7 Autophagy Related 7 Protein Coding NCOA4 Nuclear Receptor Coactivator 4 Protein Coding HMOX1 Heme Oxygenase 1 Protein Coding SLC3A2 Solute Carrier Family 3 Member 2 Protein Coding ALOX15 Arachidonate 15-Lipoxygenase Protein Coding BECN1 Beclin 1 Protein Coding PRKAA1 Protein Kinase AMP-Activated Catalytic Subunit Alpha 1 Protein Coding SAT1 Spermidine/Spermine N1-Acetyltransferase 1 Protein Coding NF2 Neurofibromin 2 Protein Coding YAP1 Yes1 Associated Transcriptional Regulator Protein Coding FTH1 Ferritin Heavy Chain 1 Protein Coding TF Transferrin Protein Coding TFRC Transferrin Receptor Protein Coding FTL Ferritin Light Chain Protein Coding CYBB Cytochrome B-245 Beta Chain Protein Coding GSS Glutathione Synthetase Protein Coding CP Ceruloplasmin Protein Coding PRNP Prion Protein Protein Coding SLC11A2 Solute Carrier Family 11 Member 2 Protein Coding SLC40A1 Solute Carrier Family 40 Member 1 Protein Coding STEAP3 STEAP3 Metalloreductase Protein Coding ACSL1 Acyl-CoA Synthetase Long Chain Family Member 1 Protein -

Imputed Gene Associations Identify Replicable Trans-Acting Genes Enriched in Transcription Pathways and Complex Traits
bioRxiv preprint doi: https://doi.org/10.1101/471748; this version posted November 19, 2018. The copyright holder for this preprint (which was not certified by peer review) is the author/funder, who has granted bioRxiv a license to display the preprint in perpetuity. It is made available under aCC-BY-ND 4.0 International license. Imputed gene associations identify replicable trans-acting genes enriched in transcription pathways and complex traits Heather E. Wheeler1,2,3, , Sally Ploch1, Alvaro N. Barbeira4, Rodrigo Bonazzola4, Alireza Fotuhi Siahpirani5, Ashis Saha6, Alexis Battle6,7, Sushmita Roy8, and Hae Kyung Im4, 1Department of Biology, Loyola University Chicago, Chicago, IL 2Department of Computer Science, Loyola University Chicago, Chicago, IL 3Department of Public Health Sciences, Stritch School of Medicine, Loyola University Chicago, Maywood, IL 4Section of Genetic Medicine, Department of Medicine, University of Chicago, Chicago, IL 5Department of Computer Sciences, University of Wisconsin-Madison, Madison, WI 6Department of Computer Science, Johns Hopkins University, Baltimore, MD 7Department of Biomedical Engineering, Johns Hopkins University, Baltimore, MD 8Department of Biostatistics and Medical Informatics, University of Wisconsin-Madison, Madison, WI Regulation of gene expression is an important mechanism SNPs associated with gene expression in cis, typically mean- through which genetic variation can affect complex traits. A ing SNPs within 1 Mb of the target gene. Because effect sizes substantial portion of gene expression variation can be ex- are large enough, around 100 samples in the early eQTL stud- plained by both local (cis) and distal (trans) genetic variation. ies could detect replicable associations in the reduced multi- Much progress has been made in uncovering cis-acting expres- ple testing space of cis-eQTLs (1–3). -

17Β-Estradiol Regulates the Expression of Apolipoprotein M Through
Wei et al. Lipids in Health and Disease (2017) 16:66 DOI 10.1186/s12944-017-0458-x RESEARCH Open Access 17β-estradiol regulates the expression of apolipoprotein M through estrogen receptor α-specific binding motif in its promoter Jiang Wei1, Yang Yu1, Guang-hua Luo1, Yue-hua Feng1, Yuan-ping Shi1, Jun Zhang1, Qin-feng Mu1, Miao-mei Yu1, Li-li Pan1, Maria Berggren-Söderlund3, Peter Nilsson-Ehle3, Xiao-ying Zhang2 and Ning Xu3* Abstract Background: We have previously demonstrated that estrogen could significantly enhance expression of apolipoprotein M (apoM), whereas the molecular basis of its mechanism is not fully elucidated yet. To further investigate the mechanism behind the estrogen induced up-regulation of apoM expression. Results: Our results demonstrated either free 17β-estradiol (E2) or membrane-impermeable bovine serum albumin-conjugated E2 (E2-BSA) could modulate human apoM gene expression via the estrogen receptor alpha (ER-α) pathway in the HepG2 cells. Moreover, experiments with the luciferase activity analysis of truncated apoM promoters could demonstrate that a regulatory region (from-1580 to −1575 bp (−GGTCA-)) upstream of the transcriptional start site of apoM gene was essential for the basal transcriptional activity that regulated by the ER-α. With the applications of an electrophoresis mobility shift assay and a chromatin immunoprecipitation assay, we could successfully identify a specific ER-α binding element in the apoM promoter region. Conculsion: In summary, the present study indicates that 17β-estradiol induced up-regulation of apoM in HepG2 cells is through an ER-α-dependent pathway involving ER-α binding element in the promoter of the apoM gene. -

Original Article Changes in Inflammatory Factors in SV40MES13 Mesangial Cells After Silencing Apom Gene
Int J Clin Exp Pathol 2020;13(6):1451-1456 www.ijcep.com /ISSN:1936-2625/IJCEP0098732 Original Article Changes in inflammatory factors in SV40MES13 mesangial cells after silencing ApoM gene Jiongjiong Liu1*, Yang Zhang3*, Xiao Zhang2, Shuchang Zhang3, Yunfei Hu3, Lizhuo Wang3, Jialin Gao3, Yao Zhang3 Departments of 1International Medical Services, 2Pediatric Surgery, The First Affiliated Hospital of USTC-Divsion of Life Sciences and Medicine, University of Sciences and Technology of China, Hefei 230001, China; 3Anhui Province Key Laboratory of Biological Macro-Molecules Research, Wannan Medical College, Wuhu 241001, China. *Equal contributors. Received June 20, 2019; Accepted September 17, 2019; Epub June 1, 2020; Published June 15, 2020 Abstract: Objective: Inflammation is an important process in the occurrence and development of nephropathy, and ApoM is closely related to inflammation. This article aims to investigate the inflammatory changes of SV40 MES13 cells after ApoM gene silencing by western blot and to explore the relationship between ApoM and inflammation. Methods: Control group glomerular mesangial cells (SV40 MES13), and the same cells after adding a small inter- fering RNA silencing ApoM gene for 24 h were observed under a microscope and photographed. After extracting the protein western blot was used to explore the associated inflammation of IL-6, P-Jak2, Erk, TNF-α, P-JNK, IKKβ, P-p38, IκBα, P-IKKα/β, NF-κB and P-NF-κB expression. Results: Western blot showed that ApoM gene was success- fully silenced in SV40 MES13 cells after adding small interfering RNA. The decrease of inflammatory factors IL-6 and P-Jak2 in Jak/Stat pathway was statistically significant. -

Plasma Protein Expression Profiles, Cardiovascular Disease, And
www.nature.com/scientificreports OPEN Plasma protein expression profles, cardiovascular disease, and religious struggles among South Asians in the MASALA study Long H. Ngo1,2,3*, M. Austin Argentieri4,5, Simon T. Dillon1,2, Blake Victor Kent4,6, Alka M. Kanaya7,8, Alexandra E. Shields1,4,8 & Towia A. Libermann1,2,8 Blood protein concentrations are clinically useful, predictive biomarkers of cardiovascular disease (CVD). Despite a higher burden of CVD among U.S. South Asians, no CVD-related proteomics study has been conducted in this sub-population. The aim of this study is to investigate the associations between plasma protein levels and CVD incidence, and to assess the potential infuence of religiosity/ spirituality (R/S) on signifcant protein-CVD associations, in South Asians from the MASALA Study. We used a nested case–control design of 50 participants with incident CVD and 50 sex- and age-matched controls. Plasma samples were analyzed by SOMAscan for expression of 1305 proteins. Multivariable logistic regression models and model selection using Akaike Information Criteria were performed on the proteins and clinical covariates, with further efect modifcation analyses conducted to assess the infuence of R/S measures on signifcant associations between proteins and incident CVD events. We identifed 36 proteins that were signifcantly expressed diferentially among CVD cases compared to matched controls. These proteins are involved in immune cell recruitment, atherosclerosis, endothelial cell diferentiation, and vascularization. A fnal multivariable model found three proteins (Contactin-5 [CNTN5], Low afnity immunoglobulin gamma Fc region receptor II-a [FCGR2A], and Complement factor B [CFB]) associated with incident CVD after adjustment for diabetes (AUC = 0.82). -

Integrated Bioinformatics Analysis of Apolipoprotein M in Thyroid Cancer
Integrated bioinformatics analysis of apolipoprotein M in thyroid cancer jiang wei Soochow University https://orcid.org/0000-0002-0943-3705 Yang Yu Soochow University Jun. Zhang Soochow University Ning Xu Lunds Universitet Guanghua Luo ( [email protected] ) https://orcid.org/0000-0001-8339-2828 Research article Keywords: ApoM, Thyroid cancer, Diagnosis, Biomarker, Prognosis Posted Date: December 19th, 2019 DOI: https://doi.org/10.21203/rs.2.19323/v1 License: This work is licensed under a Creative Commons Attribution 4.0 International License. Read Full License Page 1/16 Abstract Background Throid cancer is one of the most common cancer worldwide and its mechanism of development remains elusive.Apolipoprotein M (ApoM) is associated with lipid metabolism, inammation and atherosclerosis, but the prognostic value of apoM in thyroid cancer has not been well studied. Methods In this study, transcriptional expression, survival, gene ontology and networks of apoM in patients with thyroid cancer were analyzed using integrated bioinformatics tools including UALCAN, GEO, LinkedOmics, GeneMANIA, STRING, CircNET and KOBAS. Results Results indicated that ApoM is decreased in thyroid cancer tissues and is therefore negatively associated with malignant clinicopathological parameters. However, Kaplan-Meier analyses showed that ApoM expression is not an independent and signicant prognostic factor for overall survival in thyroid cancer. LinkedOmics Conclusions These results indicate that integrated bioinformatics analysis provide valuable information on apoM expression and potential regulatory networks in thyroid cancer. This information will be crucial in understanding the role of apoM in thyroid carcinogenesis. Background Thyroid cancer is the most common endocrine malignancy and presents in four differentiation types; anaplastic carcinoma, medullary carcinoma, follicular carcinoma and papillary carcinoma [1]. -

Endothelium-Protective Sphingosine-1-Phosphate Provided by HDL-Associated Apolipoprotein M
Endothelium-protective sphingosine-1-phosphate provided by HDL-associated apolipoprotein M Christina Christoffersena,1, Hideru Obinatab,1, Sunil B. Kumaraswamyc, Sylvain Galvanib, Josefin Ahnströmc, Madhumati Sevvanad, Claudia Egerer-Sieberd, Yves A. Mullerd, Timothy Hlab,2, Lars B. Nielsena,e,2, and Björn Dahlbäckc,2 aDepartment of Clinical Biochemistry, Rigshospitalet, 2100 Copenhagen, Denmark; bCenter for Vascular Biology, Department of Pathology and Laboratory Medicine, Weill Cornell Medical College, Cornell University, New York, NY 10065; cWallenberg Laboratory, Department of Laboratory Medicine, Skåne University Hospital, Lund University, SE 20502 Malmö, Sweden; dDepartment of Biology, Friedrich-Alexander-University Erlangen-Nuremberg, D-91052 Erlangen, Germany; and eDepartment of Biomedical Sciences, University of Copenhagen, 2100 Copenhagen, Denmark Edited* by John A. Glomset, University of Washington, Seattle, WA, and approved May 4, 2011 (received for review February 25, 2011) Protection of the endothelium is provided by circulating sphingo- Indeed, r-apoM expressed in Escherichia coli was found to co- sine-1-phosphate (S1P), which maintains vascular integrity. We crystallize with myristic acid (19), illustrating that apoM can bind show that HDL-associated S1P is bound specifically to both human lipid compounds with fatty acid side chains, and in vitro binding and murine apolipoprotein M (apoM). Thus, isolated human experiments demonstrated that S1P displaced the myristic acid − ApoM+ HDL contained S1P, whereas ApoM HDL did not. More- with an IC of 0.90 μM (19). We demonstrate here that apoM is −/− 50 over, HDL in Apom mice contains no S1P, whereas HDL in trans- the carrier of S1P in HDL, mediating vasoprotective actions on genic mice overexpressing human apoM has an increased S1P the endothelium.