Cases in Dermatology
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

FIG. 4A © O O Wo 2015/042110 Al III III II II III III 1 1 II III II II III III II III
(12) INTERNATIONAL APPLICATION PUBLISHED UNDER THE PATENT COOPERATION TREATY (PCT) (19) World Intellectual Property Organization International Bureau (10) International Publication Number (43) International Publication Date W O 2015/042110 A l 2 6 March 2015 (26.03.2015) P O P C T (51) International Patent Classification: (81) Designated States (unless otherwise indicated, for every A61P 37/00 (2006.01) kind of national protection available): AE, AG, AL, AM, AO, AT, AU, AZ, BA, BB, BG, BH, BN, BR, BW, BY, (21) International Application Number: BZ, CA, CH, CL, CN, CO, CR, CU, CZ, DE, DK, DM, PCT/US20 14/056021 DO, DZ, EC, EE, EG, ES, FI, GB, GD, GE, GH, GM, GT, (22) International Filing Date: HN, HR, HU, ID, IL, ΓΝ , IR, IS, JP, KE, KG, KN, KP, KR, 17 September 2014 (17.09.2014) KZ, LA, LC, LK, LR, LS, LU, LY, MA, MD, ME, MG, MK, MN, MW, MX, MY, MZ, NA, NG, NI, NO, NZ, OM, (25) Filing Language: English PA, PE, PG, PH, PL, PT, QA, RO, RS, RU, RW, SA, SC, (26) Publication Language: English SD, SE, SG, SK, SL, SM, ST, SV, SY, TH, TJ, TM, TN, TR, TT, TZ, UA, UG, US, UZ, VC, VN, ZA, ZM, ZW. (30) Priority Data: 61/880,522 20 September 2013 (20.09.2013) (84) Designated States (unless otherwise indicated, for every kind of regional protection available): ARIPO (BW, GH, (71) Applicant: CHILDREN'S MEDICAL CENTER COR¬ GM, KE, LR, LS, MW, MZ, NA, RW, SD, SL, ST, SZ, PORATION [US/US]; 55 Shattuck Street, Boston, Mas¬ TZ, UG, ZM, ZW), Eurasian (AM, AZ, BY, KG, KZ, RU, sachusetts 021 15 (US). -
Detail Report
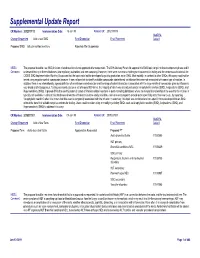
Supplemental Update Report CR Number: 2012319113 Implementation Date: 16-Jan-19 Related CR: 2012319113 MedDRA Change Requested Add a new SMQ Final Disposition Final Placement Code # Proposed SMQ Infusion related reactions Rejected After Suspension MSSO The proposal to add a new SMQ Infusion related reactions is not approved after suspension. The ICH Advisory Panel did approve this SMQ topic to go into the development phase and it Comment: underwent testing in three databases (two regulatory authorities and one company). However, there were numerous challenges encountered in testing and the consensus decision of the CIOMS SMQ Implementation Working Group was that the topic could not be developed to go into production as an SMQ. Most notably, in contrast to other SMQs, this query could not be tested using negative control compounds because it was not possible to identify suitable compounds administered via infusion that were not associated with some type of reaction. In addition, there is no internationally agreed definition of an infusion related reaction and the range of potential reactions associated with the large variety of compounds given by infusion is very broad and heterogenous. Testing was conducted on a set of around 500 terms, the majority of which was already included in Anaphylactic reaction (SMQ), Angioedema (SMQ), and Hypersensitivity (SMQ). It proved difficult to identify potential cases of infusion related reactions in post-marketing databases where the temporal relationship of the event to the infusion is typically not available. In clinical trial databases where this information is more easily available, users are encouraged to provide more specificity about the event, e.g., by reporting “Anaphylactic reaction” when it is known that this event is temporally associated with the infusion. -

Pediatric and Adolescent Dermatology
Pediatric and adolescent dermatology Management and referral guidelines ICD-10 guide • Acne: L70.0 acne vulgaris; L70.1 acne conglobata; • Molluscum contagiosum: B08.1 L70.4 infantile acne; L70.5 acne excoriae; L70.8 • Nevi (moles): Start with D22 and rest depends other acne; or L70.9 acne unspecified on site • Alopecia areata: L63 alopecia; L63.0 alopecia • Onychomycosis (nail fungus): B35.1 (capitis) totalis; L63.1 alopecia universalis; L63.8 other alopecia areata; or L63.9 alopecia areata • Psoriasis: L40.0 plaque; L40.1 generalized unspecified pustular psoriasis; L40.3 palmoplantar pustulosis; L40.4 guttate; L40.54 psoriatic juvenile • Atopic dermatitis (eczema): L20.82 flexural; arthropathy; L40.8 other psoriasis; or L40.9 L20.83 infantile; L20.89 other atopic dermatitis; or psoriasis unspecified L20.9 atopic dermatitis unspecified • Scabies: B86 • Hemangioma of infancy: D18 hemangioma and lymphangioma any site; D18.0 hemangioma; • Seborrheic dermatitis: L21.0 capitis; L21.1 infantile; D18.00 hemangioma unspecified site; D18.01 L21.8 other seborrheic dermatitis; or L21.9 hemangioma of skin and subcutaneous tissue; seborrheic dermatitis unspecified D18.02 hemangioma of intracranial structures; • Tinea capitis: B35.0 D18.03 hemangioma of intraabdominal structures; or D18.09 hemangioma of other sites • Tinea versicolor: B36.0 • Hyperhidrosis: R61 generalized hyperhidrosis; • Vitiligo: L80 L74.5 focal hyperhidrosis; L74.51 primary focal • Warts: B07.0 verruca plantaris; B07.8 verruca hyperhidrosis, rest depends on site; L74.52 vulgaris (common warts); B07.9 viral wart secondary focal hyperhidrosis unspecified; or A63.0 anogenital warts • Keratosis pilaris: L85.8 other specified epidermal thickening 1 Acne Treatment basics • Tretinoin 0.025% or 0.05% cream • Education: Medications often take weeks to work AND and the patient’s skin may get “worse” (dry and red) • Clindamycin-benzoyl peroxide 1%-5% gel in the before it gets better. -

Psoriasis, a Systemic Disease Beyond the Skin, As Evidenced by Psoriatic Arthritis and Many Comorbities
1 Psoriasis, a Systemic Disease Beyond the Skin, as Evidenced by Psoriatic Arthritis and Many Comorbities – Clinical Remission with a Leishmania Amastigotes Vaccine, a Serendipity Finding J.A. O’Daly Astralis Ltd, Irvington, NJ USA 1. Introduction Psoriasis is a systemic chronic, relapsing inflammatory skin disorder, with worldwide distribution, affects 1–3% of the world population, prevalence varies according to race, geographic location, and environmental factors (Chandran & Raychaudhuri, 2010; Christophers & Mrowietz, 2003; Farber & Nall, 1974). In Germany, 33,981 from 1,344,071 continuously insured persons in 2005 were diagnosed with psoriasis; thus the one year prevalence was 2.53% in the study group. Up to the age of 80 years the prevalence rate (range: 3.99-4.18%) was increasing with increasing age and highest for the age groups from 50 to 79 years The total rate of psoriasis in children younger than 18 years was 0.71%. The prevalence rates increased in an approximately linear manner from 0.12% at the age of 1 year to 1.2% at the age of 18 years (Schäfer et al., 2011). In France, a case-control study in 6,887 persons, 356 cases were identified (5.16%), who declared having had psoriasis during the previous 12 months (Wolkenstein et al., 2009). The prevalence of psoriasis analyzed across Italy showed that 2.9% of Italians declared suffering from psoriasis (regional range: 0.8-4.5%) in a total of 4109 individuals (Saraceno et al., 2008). The overall rate of comorbidity in subjects with psoriasis aged less than 20 years was twice as high as in subjects without psoriasis. -

Download PDF (Inglês)
Revista6Vol89ingles_Layout 1 10/10/14 11:08 AM Página 1003 WHAT IS YOUR DIAGNOSIS? 1003 s Case for diagnosis* João Roberto Antonio1 Larissa Cannizza Pacheco de Lucca1 Mariana Perez Borim1 Natália Cristina Pires Rossi1 Guilherme Bueno de Oliveira1 DOI: http://dx.doi.org/10.1590/abd1806-4841.20143156 CASE REPORT A 60-year-old woman reports a 5-year history of violaceous and intensely pruritic lesions on the dorsum and scalp, associated with a 2-year history of hair loss. She also reports decreased hair growth in the axillary and inguinal regions in the same period. Dermatological examination shows small, scaly, erythematous-violaceous, flat papules on the dorsal region; multifocal scarring alopecia areas, with smooth, bright and atrophic surface; discrete hair rarefaction in the axillary and inguinal regions; presence of longitu- FIGURE 2: dinal grooves and some depressions on the surface of Perifollicular the nail plate; no oral lesions (Figures 1 and 2). The erythema with desquamation at histopathology of the dorsal lesion is shown in figure the vertex of the 3A and that of the scalp is shown in figure 3B. scalp; cicatricial The treatment was performed using high- alopecia and potency corticoids and resulted, after three months, in smooth, bright and atrophic surface an improvement of pruritus and a slight lightening of the lesions. A FIGURE 1: B Cutaneous, erythematous- FIGURE 3: A. HE 200x. Interface dermatitis with lichenoid pattern purpuric lesions associated with dermo-epidermic detachment and lymphocytic on the infiltrate in band-like pattern in the upper dermis. B. HE 200x. dorsal region Detail of partially destroyed follicle, with perifollicular fibrosis and perivascular lymphocytic infiltrate Received on 19.09.2013. -

A Resident's Guide to Pediatric Rheumatology
A RESIDENT’S GUIDE TO PEDIATRIC RHEUMATOLOGY 4th Revised Edition - 2019 A RESIDENT’S GUIDE TO PEDIATRIC RHEUMATOLOGY This guide is intended to provide a brief introduction to basic topics in pediatric rheumatology. Each topic is accompanied by at least one up-to-date reference that will allow you to explore the topic in greater depth. In addition, a list of several excellent textbooks and other resources for you to use to expand your knowledge is found in the Appendix. We are interested in your feedback on the guide! If you have comments or questions, please feel free to contact us via email at [email protected]. Supervising Editors: Dr. Ronald M. Laxer, SickKids Hospital, University of Toronto Dr. Tania Cellucci, McMaster Children’s Hospital, McMaster University Dr. Evelyn Rozenblyum, St. Michael’s Hospital, University of Toronto Section Editors: Dr. Michelle Batthish, McMaster Children’s Hospital, McMaster University Dr. Roberta Berard, Children’s Hospital – London Health Sciences Centre, Western University Dr. Liane Heale, McMaster Children’s Hospital, McMaster University Dr. Clare Hutchinson, North York General Hospital, University of Toronto Dr. Mehul Jariwala, Royal University Hospital, University of Saskatchewan Dr. Lillian Lim, Stollery Children’s Hospital, University of Alberta Dr. Nadia Luca, Alberta Children’s Hospital, University of Calgary Dr. Dax Rumsey, Stollery Children’s Hospital, University of Alberta Dr. Gordon Soon, North York General Hospital and SickKids Hospital Northern Clinic in Sudbury, University -

Cosmetic Center May Newsletter
Cosmetic Center May Newsletter DERMATOLOGY ASSOCIATES Keratosis Pilaris May specials “KP” Very common 10 % off Sunscreen skin condition characterized by 10% off Glytone KP Products tiny, hard 20% off Laser Hair Removal bumps. Glytone and Neostrata Peels– Purchase a package of 6 and get 1 Free It can be found on the outer Purchase a Facial and Receive a Free Skin Care Starter Kit arms, thighs, and sometimes Product of the Month Procedure of the Month the buttocks Tilley Hats Facials It is caused by the buildup of Lifetime Warranty Schedule an appointment today for dead skin Waterproof & Float an hour of pampering and (keratin) around relaxation. We will use products Many Different Sizes, Styles, and the hair follicle. suitable for your skin type and Colors to Choose From KP generally condition. gets worse in the SPF 50 winter and often clears in the summer. KP is self-limiting and disappears with age. KP can be treated with products. Mother’s Day is May 10 We have several products in the Relaxing Facials & Gift Certificates make great gifts! Cosmetic Center Mini Facials for the month of May only $45 to treat and help You can also shop ONLINE at Kingsportderm.com and have the items shipped. Melanoma Awareness Month More than 1 million cases of skin cancer are diagnosed in the United States each year, making skin cancer the most common cancer in the United States. ABCDEs of Melanoma Approximately 62,480 cases of melanoma will be A. If you draw a line diagnosed each year, nearly 8,420 cases will lead to deaths. -

A New Insight on Atopic Skin Diathesis: Is It Correlated with the Severity of Melasma
A New Insight on Atopic Skin Diathesis: Is It Correlated with the Severity of Melasma Danar Wicaksono1*, Rima Mustafa2, Sri Awalia Febriana1, Kristiana Etnawati1 1 Dermatovenereology Department, Faculty of Medicine Universitas Gadjah Mada – Dr. Sardjito General Hospital, Yogyakarta-Indonesia 2 Clinical Epidemiology and Biostatistics Unit, Faculty of Medicine Universitas Gadjah Mada –Dr. Sardjito General Hospital, Yogyakarta-Indonesia Keywords: Melasma, atopic skin diathesis (ASD), MASI score, atopic dermatitis (AD) Abstract: Melasma is a macular lesion of light brown to dark on the sun-exposed area, especially on the face. Atopic Skin Diathesis (ASD) is a clinical term to describe skin atopics with previous, present or future atopic dermatitis (AD). Dennie-Morgan infraorbital folds are secondary creases in the skin below the lower eyelids with a sensitivity of 78% and a specificity of 76% to diagnose AD. Melasma skin is characterized by impaired stratum corneum integrity and a delayed barrier recovery rate. Barrier dysfunction will stimulate keratinocyte to secrete keratinocyte-derived factor, which plays role in skin pigmentation process in melasma. To analyze correlation between ASD and Melasma Area Severity Index (MASI) score in melasma patient. This study is an observational analytic study with cross sectional design. Measurement of ASD and MASI score were done in 60 subjects with melasma who went to dermatology outpatient clinic Dr. Sardjito General Hospital from July 2017 to Januari 2018. The correlation between ASD and MASI score was analyzed using Pearson correlation. The result of this study showed no significant correlation between ASD and MASI scores (r: 0.02, p: 0,85). Crude Relative Risk (RR) for Dennie-Morgan infraorbital folds and MASI score was 4 (1.01-15.87). -

COVID-19 Mrna Pfizer- Biontech Vaccine Analysis Print
COVID-19 mRNA Pfizer- BioNTech Vaccine Analysis Print All UK spontaneous reports received between 9/12/20 and 22/09/21 for mRNA Pfizer/BioNTech vaccine. A report of a suspected ADR to the Yellow Card scheme does not necessarily mean that it was caused by the vaccine, only that the reporter has a suspicion it may have. Underlying or previously undiagnosed illness unrelated to vaccination can also be factors in such reports. The relative number and nature of reports should therefore not be used to compare the safety of the different vaccines. All reports are kept under continual review in order to identify possible new risks. Report Run Date: 24-Sep-2021, Page 1 Case Series Drug Analysis Print Name: COVID-19 mRNA Pfizer- BioNTech vaccine analysis print Report Run Date: 24-Sep-2021 Data Lock Date: 22-Sep-2021 18:30:09 MedDRA Version: MedDRA 24.0 Reaction Name Total Fatal Blood disorders Anaemia deficiencies Anaemia folate deficiency 1 0 Anaemia vitamin B12 deficiency 2 0 Deficiency anaemia 1 0 Iron deficiency anaemia 6 0 Anaemias NEC Anaemia 97 0 Anaemia macrocytic 1 0 Anaemia megaloblastic 1 0 Autoimmune anaemia 2 0 Blood loss anaemia 1 0 Microcytic anaemia 1 0 Anaemias haemolytic NEC Coombs negative haemolytic anaemia 1 0 Haemolytic anaemia 6 0 Anaemias haemolytic immune Autoimmune haemolytic anaemia 9 0 Anaemias haemolytic mechanical factor Microangiopathic haemolytic anaemia 1 0 Bleeding tendencies Haemorrhagic diathesis 1 0 Increased tendency to bruise 35 0 Spontaneous haematoma 2 0 Coagulation factor deficiencies Acquired haemophilia -

Faculty Meeting August 9Th, 2011
Review of Systems is a process that includes a review of body systems. It is carried out through a series of questions regarding signs and symptoms. The Review of Systems (ROS) includes information about the following 14 systems. Constitutional: description of general appearance; growth and development, recent weight loss/gain, malaise, chills weakness, fatigue, fever, vital signs, head circumference for a baby, appetite, sleep habits, insomnia, night sweats. Integumentary: (skin and/or breast) rashes, color, sores, dryness, itching, flaking, dandruff, lumps, moles, color change, changes in hair or nails, sweating, hives, bruising, scratches, scars, swelling., acne. Eyes: vision, no change in vision, glasses or contact lenses, last eye exam, eye pain, “eye” redness, excessive tearing, double vision, blurred vision, spots, specks, flashing lights, photophobia, glaucoma, cataracts. Ears, Nose, Mouth/ Throat Ears: hearing loss, tinnitus, vertigo, earaches, ear infections, ear discharges; if hearing is decreased, use of hearing aids. Nose and sinuses: frequent colds, stuffiness’, discharge drainage, nasal itching, hay fever, nosebleeds sinusitis, sinus trouble, sinus pressure, nasal congestion, nasal discharge, nasal infection Mouth/Throat condition of teeth and gums bleeding gums dentures, (how they fit) last dental exam, dry mouth, frequent sore throats, difficulty swallowing, no posterior pharynx pain, hoarseness, sores/ulcers, hoarseness, pyorrhea. Respiratory: cough, sputum, (color, quantity) shortness of breath, pleuritic chest pain, wheezing, asthma, bronchitis, TB, emphysema, pneumonia, hemoptysis, CXR. Cardiovascular: heart trouble; high blood pressure; CV hypertension, heart murmurs, chest pain/ pressure palpitations, dyspnea, orthopnea,, rheumatic fever, paroxysmal nocturnal dyspnea, edema; past EKG or other heart tests. Peripheral Vascular; intermittent claudication, leg cramps, varicose veins, past clots in the vein, syncope, edema. -

UC Davis Dermatology Online Journal
UC Davis Dermatology Online Journal Title Proposed classification for koebner, wolf isotopic, renbok, koebner nonreaction, isotopic nonreaction & other related phenomen. Permalink https://escholarship.org/uc/item/96s656b4 Journal Dermatology Online Journal, 20(11) Authors Kannangara, Ajith P Yosipovitch, Gil Fleischer Jr., Alan B Publication Date 2014 DOI 10.5070/D32011024682 License https://creativecommons.org/licenses/by-nc-nd/4.0/ 4.0 eScholarship.org Powered by the California Digital Library University of California Volume 20 Number 11 November 2014 Commentary Proposed classification for koebner, wolf isotopic, renbok, koebner nonreaction, isotopic nonreaction & other related phenomen. Ajith P. Kannangara MD1, Gil Yosipovitch MD PhD2, Alan B. Fleischer Jr MD3 Dermatology Online Journal 20 (11): 12 1Base Hospital Balapitiya, Ministry of Health, Sri Lanka 2Department of Dermatology, Temple University School of Medicine, Philadelphia, USA 3Department of Dermatology, Wake Forest University School of Medicine; Winston-Salem, North Carolina, USA Correspondence: Ajith P. Kannangara, M.D Base Hospital Balapitiya, Ministry of Health, Sri Lanka. E-mail: [email protected] Abstract Students of skin diseases have long noted a variety of disease responses and non-responses to trauma and the presence of structural abnormalities. This article will review the series of these responses including: Koebner phenomenon, Wolf isotopic response, Renbök response, Koebner nonreaction, isotopic nonreaction, and other related skin reactions. Because most of these reported phenomena have similar morphological features the diagnosis is often made on the basis of differences in the clinical presentation. Note that some of the cutaneous reactions of similar phenomena have been described using varied nomenclature, further adding to the confusion. -

Ekbom Syndrome: a Delusional Condition of “Bugs in the Skin”
Curr Psychiatry Rep DOI 10.1007/s11920-011-0188-0 Ekbom Syndrome: A Delusional Condition of “Bugs in the Skin” Nancy C. Hinkle # Springer Science+Business Media, LLC (outside the USA) 2011 Abstract Entomologists estimate that more than 100,000 included dermatophobia, delusions of infestation, and Americans suffer from “invisible bug” infestations, a parasitophobic neurodermatitis [2••]. Despite initial publi- condition known clinically as Ekbom syndrome (ES), cations referring to the condition as acarophobia (fear of although the psychiatric literature dubs the condition “rare.” mites), ES is not a phobia, as the individual is not afraid of This illustrates the reluctance of ES patients to seek mental insects but rather convinced that they are infesting his or health care, as they are convinced that their problem is her body [3, 4]. This paper deals with primary ES, not the bugs. In addition to suffering from the delusion that bugs form secondary to underlying psychological or physiologic are attacking their bodies, ES patients also experience conditions such as drug reaction or polypharmacy [5–8]. visual and tactile hallucinations that they see and feel the While Morgellons (“the fiber disease”) is likely a compo- bugs. ES patients exhibit a consistent complex of attributes nent on the same delusional spectrum, because it does not and behaviors that can adversely affect their lives. have entomologic connotations, it is not included in this discussion of ES [9, 10]. Keywords Parasitization . Parasitosis . Dermatozoenwahn . Valuable reviews of ES include those by Ekbom [1](1938), Invisible bugs . Ekbom syndrome . Bird mites . Infestation . Lyell [11] (1983), Trabert [12] (1995), and Bak et al.