The Most Common Problem Facing Endurance Athletes Exercise
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Iliopsoas Tendonitis/Bursitis Exercises
ILIOPSOAS TENDONITIS / BURSITIS What is the Iliopsoas and Bursa? The iliopsoas is a muscle that runs from your lower back through the pelvis to attach to a small bump (the lesser trochanter) on the top portion of the thighbone near your groin. This muscle has the important job of helping to bend the hip—it helps you to lift your leg when going up and down stairs or to start getting out of a car. A fluid-filled sac (bursa) helps to protect and allow the tendon to glide during these movements. The iliopsoas tendon can become inflamed or overworked during repetitive activities. The tendon can also become irritated after hip replacement surgery. Signs and Symptoms Iliopsoas issues may feel like “a pulled groin muscle”. The main symptom is usually a catch during certain movements such as when trying to put on socks or rising from a seated position. You may find yourself leading with your other leg when going up the stairs to avoid lifting the painful leg. The pain may extend from the groin to the inside of the thigh area. Snapping or clicking within the front of the hip can also be experienced. Do not worry this is not your hip trying to pop out of socket but it is usually the iliopsoas tendon rubbing over the hip joint or pelvis. Treatment Conservative treatment in the form of stretching and strengthening usually helps with the majority of patients with iliopsoas bursitis. This issue is the result of soft tissue inflammation, therefore rest, ice, anti- inflammatory medications, physical therapy exercises, and/or injections are effective treatment options. -

The Textual and Visual Uses of the Literary Motif of Cross-Dressing In
The Textual and Visual Uses of the Literary Motif of Cross-Dressing in Medieval French Literature, 1200–1500 Vanessa Elizabeth Wright Submitted in accordance with the requirements for the degree of PhD in Medieval Studies University of Leeds Institute for Medieval Studies September 2019 2 The candidate confirms that the work submitted is her own and that appropriate credit has been given where reference has been made to the work of others. This copy has been supplied on the understanding that it is copyright material and that no quotation from the thesis may be published without proper acknowledgement. The right of Vanessa Elizabeth Wright to be identified as Author of this work has been asserted by her in accordance with the Copyright, Designs and Patents Act 1988. 3 Acknowledgements I would like to thank my supervisors Rosalind Brown-Grant, Catherine Batt, and Melanie Brunner for their guidance, support, and for continually encouraging me to push my ideas further. They have been a wonderful team of supervisors and it has been a pleasure to work with them over the past four years. I would like to thank my examiners Emma Cayley and Helen Swift for their helpful comments and feedback on this thesis and for making my viva a positive and productive experience. I gratefully acknowledge the funding that allowed me to undertake this doctoral project. Without the School of History and the Institute for Medieval Studies Postgraduate Research Scholarship, I would not have been able to undertake this study. Trips to archives and academic conferences were made possible by additional bursaries and fellowships from Institute for Medieval Studies, the Royal Historical Society, the Society for the Study of Medieval Languages and Literatures, the Society for Medieval Feminist Scholarship’s Foremothers Fellowship (2018), and the Society for the Study of French History. -

Wound Classification
Wound Classification Presented by Dr. Karen Zulkowski, D.N.S., RN Montana State University Welcome! Thank you for joining this webinar about how to assess and measure a wound. 2 A Little About Myself… • Associate professor at Montana State University • Executive editor of the Journal of the World Council of Enterstomal Therapists (JWCET) and WCET International Ostomy Guidelines (2014) • Editorial board member of Ostomy Wound Management and Advances in Skin and Wound Care • Legal consultant • Former NPUAP board member 3 Today We Will Talk About • How to assess a wound • How to measure a wound Please make a note of your questions. Your Quality Improvement (QI) Specialists will follow up with you after this webinar to address them. 4 Assessing and Measuring Wounds • You completed a skin assessment and found a wound. • Now you need to determine what type of wound you found. • If it is a pressure ulcer, you need to determine the stage. 5 Assessing and Measuring Wounds This is important because— • Each type of wound has a different etiology. • Treatment may be very different. However— • Not all wounds are clear cut. • The cause may be multifactoral. 6 Types of Wounds • Vascular (arterial, venous, and mixed) • Neuropathic (diabetic) • Moisture-associated dermatitis • Skin tear • Pressure ulcer 7 Mixed Etiologies Many wounds have mixed etiologies. • There may be both venous and arterial insufficiency. • There may be diabetes and pressure characteristics. 8 Moisture-Associated Skin Damage • Also called perineal dermatitis, diaper rash, incontinence-associated dermatitis (often confused with pressure ulcers) • An inflammation of the skin in the perineal area, on and between the buttocks, into the skin folds, and down the inner thighs • Scaling of the skin with papule and vesicle formation: – These may open, with “weeping” of the skin, which exacerbates skin damage. -

Calf Stretching and Strengthening Exercises
Julie Dass Injury Clinic 108 Milton Road Phone: 01234349464 Clapham Email: [email protected] Bedford MK416as Exercise plan: Patient: Date: Calf Stretches and Strengthening Mrs Julie Dass 31st Mar 2017 Exercises Eccentric calf strengthening exercise Stand with your toes on the edge of a step or a box. Hold onto something stable for support if required. We will assume the leg you are trying to strengthen is your left leg (the injured side). Lift your left leg off the step, and go onto your toes on your right leg. Now place your left foot beside the right, and place all your weight on your left leg. Drop your heels downwards below the level of the step. Use your right leg (non-injured leg) to lift yourself back to the start position. Make sure you keep your leg straight during the exercise. This exercise can help strengthen the calf muscle and may be useful for treating Achilles tendinopathy. Full squat single leg Stand on one leg, and bend your knee to the full squat (90 degrees) position. Make sure when you squat you keep the middle of your knee cap in line with the middle toes of your foot. Do not let your knee drift off to one side. Also keep your hips and pelvis level as you squat, so you go down in a straight line. Be careful not to slump forwards as you squat, maintain good posture. Always keep your foot flat on the ground, do not let your heel raise up. Video: http://youtu.be/afJNrDNonAc Full wall squat Open your legs slightly wider than shoulder width, stand with your back resting against a wall, and bend your knees to the full squat position (90 degrees). -

All About Glutes 1 Table of Contents
All About Glutes 1 Table of Contents Are You Training Your Glutes the Wrong Way? 3 • Anatomy of the Glutes 4 • Functions of the Glutes at the Hip 4 • The Shortcoming of Most Training Programs 5 • Progression and Preventing Knee Valgus 6 • Simple Solution 6 How to Identify and Correct Tight Hip Flexors 8 • What Exactly Are Tight Hip Flexors? 9 • The Hip Flexor Muscle Group 9 • Signs You Have Tight Hip Flexors 10 • What Causes Hip Tightness 10 • Stretches to Loosen up Tight Hip Flexors 10 • Exercises to Strengthen Hip Flexors 11 Pain in the Buttocks When Sitting? Tips to Prevent and Manage 12 Piriformis Syndrome • What is Piriformis Syndrome? 13 • How Does Piriformis Syndrome Happen? 13 • Special Considerations with Clients 14 • Prevention and Pain Management 14 How Do I Build the Perfect Glutes? 16 • Can’t I Just Squat and Lunge? 17 • Your Best Bets to Target the Glutes 18 • Don’t Forget the Legs 18 • Train the Glutes SPECIFICALLY 19 TABLE OF CONTENTS 800.545.4772 WWW.ISSAONLINE.EDU 2 Are You Training Your Glutes the Wrong Way? 800.545.4772 WWW.ISSAONLINE.EDU 3 UNIT ONE These days, the glutes get a lot of attention, and it’s well deserved. When you build and strengthen your glutes in the right way, they not only make your body look better, but they also increase your performance and can diminish knee pain. The problem is most people aren’t taking the best approach to training for the highest level of glute development. Anatomy of the Glutes Let’s start with a little anatomy. -

Critical Dissertations on the Origin, Antiquities, Language, Government
ExLtbkis p. KENNEDY, ANGLESEA-STREET, COLLEGE GREEN, DUBLIN. &^.i.n^ CRITICAL DISSERTATIONS O N T H E ORIGIN, ANTIQUITIES, LANGUAGE, GOVERNMENT, MANNERS, AND RELIGION, O F T H E ANTIENT CALEDONIANS, THEIR POSTERITY THE PICTS, AND THE BRITISH AND IRISH SCOTS. By JOHN MACPHERSON, D. D, Minifler of Slate, in the Isle of Sky. DUBLIN: Printed by Boulter Griersov, Printer to the King's mofl: Excellent Majcfty. mdcclxviii. TO THE HONOURABLE Charles Greville, Efq; De a r Sir, MY Father, who was the Author of the following DifTertations, would not, perhaps, have dedicated them to any man alive. He annexed, and with good reafbn, an idea of fervility to addrefles of this fort, and reckoned them the diigrace of literature. If I could not, from my foul, acquit myfelf of every felfifh view, in prefenting to you the poft- humous works of a father I tenderly loved, you would not have heard from me in this public manner. You know, my dear friend, the fincerity of my affection for you : but even that affedlion fhould not induce me to dedicate to you, had you already arrived at that eminence, in the ftate, which the abilities and fhining a 2 talents DEDICATION. talents of your early youth feem lb largely to promife, left what really is the voice of friendfhip and efteem, fhould be miftaken, by the world, for that of flattery and interefted defigns. I am on the eve of letting out for a very diftant quarter of the world : without afking your permit fion, I leave you this public tefti- mony of my regard for you, not to fecure your future favour, but to ftand as a finall proof of that attach- ment, with which I am, Dear Sir Your moft affedlionate Friend, and moft Obedient Humble Servant, John Macpherjfbn. -

GLOSSARY of MEDICAL and ANATOMICAL TERMS
GLOSSARY of MEDICAL and ANATOMICAL TERMS Abbreviations: • A. Arabic • abb. = abbreviation • c. circa = about • F. French • adj. adjective • G. Greek • Ge. German • cf. compare • L. Latin • dim. = diminutive • OF. Old French • ( ) plural form in brackets A-band abb. of anisotropic band G. anisos = unequal + tropos = turning; meaning having not equal properties in every direction; transverse bands in living skeletal muscle which rotate the plane of polarised light, cf. I-band. Abbé, Ernst. 1840-1905. German physicist; mathematical analysis of optics as a basis for constructing better microscopes; devised oil immersion lens; Abbé condenser. absorption L. absorbere = to suck up. acervulus L. = sand, gritty; brain sand (cf. psammoma body). acetylcholine an ester of choline found in many tissue, synapses & neuromuscular junctions, where it is a neural transmitter. acetylcholinesterase enzyme at motor end-plate responsible for rapid destruction of acetylcholine, a neurotransmitter. acidophilic adj. L. acidus = sour + G. philein = to love; affinity for an acidic dye, such as eosin staining cytoplasmic proteins. acinus (-i) L. = a juicy berry, a grape; applied to small, rounded terminal secretory units of compound exocrine glands that have a small lumen (adj. acinar). acrosome G. akron = extremity + soma = body; head of spermatozoon. actin polymer protein filament found in the intracellular cytoskeleton, particularly in the thin (I-) bands of striated muscle. adenohypophysis G. ade = an acorn + hypophyses = an undergrowth; anterior lobe of hypophysis (cf. pituitary). adenoid G. " + -oeides = in form of; in the form of a gland, glandular; the pharyngeal tonsil. adipocyte L. adeps = fat (of an animal) + G. kytos = a container; cells responsible for storage and metabolism of lipids, found in white fat and brown fat. -

ANTERIOR KNEE PAIN Home Exercises
ANTERIOR KNEE PAIN Home Exercises Anterior knee pain is pain that occurs at the front and center of the knee. It can be caused by many different problems, including: • Weak or overused muscles • Chondromalacia of the patella (softening and breakdown of the cartilage on the underside of the kneecap) • Inflammations and tendon injury (bursitis, tendonitis) • Loose ligaments with instability of the kneecap • Articular cartilage damage (chondromalacia patella) • Swelling due to fluid buildup in the knee joint • An overload of the extensor mechanism of the knee with or without malalignment of the patella You may feel pain after exercising or when you sit too long. The pain may be a nagging ache or an occasional sharp twinge. Because the pain is around the front of your knee, treatment has traditionally focused on the knee itself and may include taping or bracing the kneecap, or patel- la, and/ or strengthening the thigh muscle—the quadriceps—that helps control your kneecap to improve the contact area between the kneecap and the thigh bone, or femur, beneath it. Howev- er, recent evidence suggests that strengthening your hip and core muscles can also help. The control of your knee from side to side comes from the glutes and core control; that is why those areas are so important in management of anterior knee pain. The exercises below will work on a combination of flexibility and strength of your knee, hip, and core. Although some soreness with exercise is expected, we do not want any sharp pain–pain that gets worse with each rep of an exercise or any increased soreness for more than 24 hours. -

SOP DC-407 Calving Cows-Heifers
Macdonald Campus Farm Cattle Complex Standard Operating Procedure # DC-407 CALVING COWS/ HEIFERS 1. PURPOSE To facilitate comfort and ease of calving and to identify and address any complications which may arise. 2. RESPONSIBILITY 2.1 All permanent, casual and student staff 2.2 Dairy Manager and Technician 2.3 Herd Veterinarian 3. MATERIALS 3.1 Halter 3.2 Chains and handles 3.3 Pail with Endure® and warm water 3.4 Lubricating gel 3.5 Insemination gloves 3.6 Paper towel 3.7 Calf puller 3.8 Iodine 4. GENERAL 4.1 3 general stages of Calving: Stage and Time Events I – Preparatory Calf rotates to upright position Uterine contraction begins (15 minute intervals) (2 to 6 hours) Water sac expelled Cow usually lying down II – Delivery Fetus enters birth canal (30 minutes – 4 hours) Uterine contractions: (2-minute intervals) Expulsion and delivery of the calf Expulsion of the fetal membrane or placenta III – Cleaning (2 to 8 hours) 4.2 Normal delivery should be completed within 2 to 3 hours after the water sac appears in the heifers, and 1 to 2 hours in cow/heifers. If prolonged, the calf may be born dead or weak. 4.3 Most calf fatalities are caused by injuries or suffocation resulting from difficult or delayed parturition. (See Table 2: Factors Contributing to Calving Problems). 4.4 Any abnormal fetal positions must be corrected in the early stages of delivery. 4.5 Heifers and cows with small pelvic areas will likely need assistance. 4.6 If a cow has had more than one calf, the calving time may be considerably shorter. -

Thigh and Calf Discrimination in the Motor Innervation of the Chick Hindlimb Following Deletions of Limb Segments1
0270~6474/83/0306-1199$02.00/0 The Journal of Neuroscience Copyright 0 Society for Neuroscience Vol. 3, No. 6, pp. 1199-1215 Printed in U.S.A. June 1983 THIGH AND CALF DISCRIMINATION IN THE MOTOR INNERVATION OF THE CHICK HINDLIMB FOLLOWING DELETIONS OF LIMB SEGMENTS1 VIRGINIA WHITELAW** AND MARGARET HOLLYDAY$3 * Departmen,t of Biophysics and Theoretical Biology and $ Department of Pharmacological and Physiological Sciences, The University of Chicago, Chicago, Illinois 60637 Received August 11, 1982; Revised December 27, 1982; Accepted January 17, 1983 Abstract In this paper we report studies on the organization of the motor projections to chick hindlimbs lacking limb segments as a result of surgical manipulations during early embryonic development. The innervation of partial limbs, missing either a thigh or both a calf and a foot, was studied using both retrograde and orthograde horseradish peroxidase nerve-tracing techniques, as well as by serial reconstruction. In addition, [3H]thymidine autoradiography was used to characterize motoneuron production and loss. Motor organization was assessed both before and after the period of naturally occurring motoneuron death. Prior to the period of cell death, we verified by autoradiography that the organization of the motor column (i.e., motoneuron birthdates and settling patterns) was normal despite deletions of the periphery. It was also found that, initially, the entire motor column projected to the partial limbs, entering via normal crural and sciatic pathways. The proximal branching patterns of the nerves leaving the plexus were normal; however, the distal projections of the nerves which would normally serve the missing limb segment were truncated. -
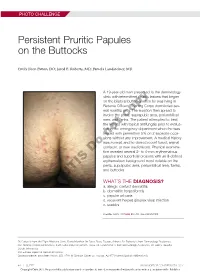
Persistent Pruritic Papules on the Buttocks
PHOTO CHALLENGE Persistent Pruritic Papules on the Buttocks Emily Ileen Patton, DO; Jared E. Roberts, MD; Pamela Landsteiner, MD A 19-year-old man presented to the dermatology clinic with intermittent pruritic lesions that began on the bilateral buttocks when he was living in Reserve Officers’ Training Corps dormitories sev- eral months prior. The eruption then spread to involve the penis, suprapubic area, periumbilical area, and flanks.copy The patient attempted to treat the lesions with topical antifungals prior to evalua- tion in the emergency department where he was treated with permethrin 5% on 2 separate occa- sionsnot without any improvement. A medical history was normal, and he denied recent travel, animal contacts, or new medications. Physical examina- Dotion revealed several 2- to 4-mm erythematous papules and superficial erosions with an ill-defined erythematous background most notable on the penis, suprapubic area, periumbilical area, flanks, and buttocks. WHAT’S THE DIAGNOSIS? CUTIS a. allergic contact dermatitis b. dermatitis herpetiformis c. papular urticaria d. recurrent herpes simplex virus infection e. scabies PLEASE TURN TO PAGE E5 FOR THE DIAGNOSIS Dr. Patton is from the Flight Medicine Clinic, Davis-Monthan Air Force Base, Tucson, Arizona. Dr. Roberts is from Dermatology Residency, San Antonio Uniformed Services Health Education Consortium, Texas. Dr. Landsteiner is from Dermatology Associates, St. Luke’s Hospital, Duluth, Minnesota. The authors report no conflict of interest. Correspondence: Emily Ileen Patton, DO, 1781 W Crimson Clover Ln, Tucson, AZ 85704 ([email protected]). E4 I CUTIS® WWW.MDEDGE.COM/DERMATOLOGY Copyright Cutis 2019. No part of this publication may be reproduced, stored, or transmitted without the prior written permission of the Publisher. -

Myofascial Pain Syndrome of Gluteus Minimus Mimicking Lumbar Radiculitis -A Case Report
Anesth Pain Med 2015; 10: 16-20 http://dx.doi.org/10.17085/apm.2015.10.1.16 ■Case Report■ Myofascial pain syndrome of gluteus minimus mimicking lumbar radiculitis -A case report- Department of Anesthesiology and Pain Medicine, Daegu Fatima Hospital, Daegu, Korea Joong-Ho Park, Kwang-Suk Shim, Young-Min Shin, Chiu Lee, Sang-Gon Lee, and Eun-Ju Kim Myofascial pain syndrome (MPS) can be characterized by pain difficult. Delays in making the correct diagnosis can result in caused by trigger points (TrPs) and fascial constrictions. Patients longer hospital stays, higher hospital fees, and unnecessary with MPS of the gluteus minimus muscles often complain of diagnostic tests and inadequate treatments. The authors have symptoms such as hip pain, especially when standing up after sitting or lying on the affected side, limping, and pain radiating down to successfully diagnosed and treated a patient with MPS of the the lower extremities. A 24-year-old female patient presenting with gluteus minimus initially diagnosed with lumbar radiculitis. motor and sensory impairments of both lower extremities was With thorough physical examination and injection of TrPs referred to our pain clinic after initially being diagnosed with lumbar radiculitis. Under the impression of MPS of the gluteus minimus under ultrasonography guidance, the patient was relieved of her muscles following through evaluation and physical examination of symptoms. We report this case to emphasize the importance of the patient, we performed trigger point injections under ultrasonography physical examination in patients presenting with symptoms guidance on the myofascial TrPs. Dramatic improvement of the suggestive of lumbar radiculitis.