Title Page 1 Exploration of the Clinical Effect of Modified Peroneal Nerve
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
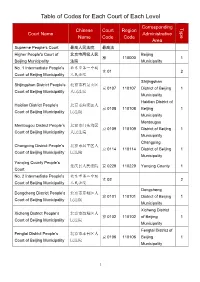
Table of Codes for Each Court of Each Level
Table of Codes for Each Court of Each Level Corresponding Type Chinese Court Region Court Name Administrative Name Code Code Area Supreme People’s Court 最高人民法院 最高法 Higher People's Court of 北京市高级人民 Beijing 京 110000 1 Beijing Municipality 法院 Municipality No. 1 Intermediate People's 北京市第一中级 京 01 2 Court of Beijing Municipality 人民法院 Shijingshan Shijingshan District People’s 北京市石景山区 京 0107 110107 District of Beijing 1 Court of Beijing Municipality 人民法院 Municipality Haidian District of Haidian District People’s 北京市海淀区人 京 0108 110108 Beijing 1 Court of Beijing Municipality 民法院 Municipality Mentougou Mentougou District People’s 北京市门头沟区 京 0109 110109 District of Beijing 1 Court of Beijing Municipality 人民法院 Municipality Changping Changping District People’s 北京市昌平区人 京 0114 110114 District of Beijing 1 Court of Beijing Municipality 民法院 Municipality Yanqing County People’s 延庆县人民法院 京 0229 110229 Yanqing County 1 Court No. 2 Intermediate People's 北京市第二中级 京 02 2 Court of Beijing Municipality 人民法院 Dongcheng Dongcheng District People’s 北京市东城区人 京 0101 110101 District of Beijing 1 Court of Beijing Municipality 民法院 Municipality Xicheng District Xicheng District People’s 北京市西城区人 京 0102 110102 of Beijing 1 Court of Beijing Municipality 民法院 Municipality Fengtai District of Fengtai District People’s 北京市丰台区人 京 0106 110106 Beijing 1 Court of Beijing Municipality 民法院 Municipality 1 Fangshan District Fangshan District People’s 北京市房山区人 京 0111 110111 of Beijing 1 Court of Beijing Municipality 民法院 Municipality Daxing District of Daxing District People’s 北京市大兴区人 京 0115 -

Studies on the Space Matching Relationship Between Self-Service
2019 2nd International Workshop on Advances in Social Sciences (IWASS 2019) Studies on the Space Matching Relationship between Self-Service Banking Outlets and Tourism Supporting Factors in Tourist Cities-Taking Central Downtown of Hohhot City as an Example Wei Zhang1,2, Zhaoxiang Qin1 1Tourism College of Inner Mongolia Normal University, Hohhot, Inner Mongolia, 010022, China 2Collage of Earth and Environmental Science, Lanzhou University, Lanzhou, Gansu, 730000, China Keywords: Tourist city, Self-service banking outlets, Tourism supporting factor, Central downtown of hohhot Abstract: With the central downtown of Hohhot, a tourist city, as an example, kernel density estimation method and the buffer analysis method were used to inspect the space matching relationship between service scope of self-service banking outlets and the tourist reception facilities. Analysis results show that there exists a certain gap between the service scope of self-service banking outlets and the matching with tourist reception facilities, and tourists’ economic behaviors during travelling are limited. Therefore, it is necessary to build a tourist demand oriented urban tourism consumption service supply system with the participation and collaboration of multiple subjects including government, market, and enterprises. 1. Introduction With the development of urban tourism, self-service banking outlets have started to extend their service objects. Tourists as an important component of tourism city have injected new vigor into the development of urban financial industry. In 2018, Hohhot with permanent resident population of 3 million received a total of 30.574 million tourists, whish is far higher that of the number of local residents. According to the author's investigation in Hohhot, despite of the convenience of the development of electronic payment for tourists' tourism consumption, tourists have small and fast banking financial activities of varying degrees during travelling. -

Corporate Information
THIS DOCUMENT IS IN DRAFT FORM, INCOMPLETE AND SUBJECT TO CHANGE AND THAT THE INFORMATION MUST BE READ IN CONJUNCTION WITH THE SECTION HEADED “WARNING” ON THE COVER OF THIS DOCUMENT. CORPORATE INFORMATION Registered office Windward 3 Regatta Office Park P.O. Box 1350 Grand Cayman KY1-1108 Cayman Islands Principal place of business in Unit 2413A, 24/F Hong Kong Lippo Centre Tower One 89 Queensway Admiralty Hong Kong Principal place of business in The Fifth Farm the PRC Shengle Economic Park Helinger County Hohhot Inner Mongolia PRC Company’s website https://www.mengshu.cn/ (information contained in this website does not form part of this document) Joint Company Secretaries Ms. Bai Xueying (白雪瑩女士) The Fifth Farm Shengle Economic Park Helinger County Hohhot City Inner Mongolia PRC Mr. Chen Kun (陳坤先生) Solicitor Unit 2413A, 24/F Lippo Centre Tower One 89 Queensway Admiralty Hong Kong Authorised representatives (for the Ms. Tie Ying (鐵英女士) purpose of the Listing Rules) No. 1202, Unit 3, No. 1 Upper Building Dianli Jia Yuan Saihan District Hohhot Inner Mongolia PRC −64− THIS DOCUMENT IS IN DRAFT FORM, INCOMPLETE AND SUBJECT TO CHANGE AND THAT THE INFORMATION MUST BE READ IN CONJUNCTION WITH THE SECTION HEADED “WARNING” ON THE COVER OF THIS DOCUMENT. CORPORATE INFORMATION Mr. Chen Kun (陳坤先生) Solicitor Unit 2413A, 24/F Lippo Centre Tower One 89 Queensway Admiralty Hong Kong Audit committee Ms. Ge Xiaoping (葛曉萍) (Chairman) Mr. Sun Baoping (孫保平) Ms. Hao Chunhong (郝春虹) Remuneration committee Mr. Sun Baoping (孫保平) (Chairman) Ms. Ge Xiaoping (葛曉萍) Ms. Cui Hanzhang (崔含章) Nomination committee Mr. -

2.12 Inner Mongolia Autonomous Region Inner Mongolia Hengzheng
2.12 Inner Mongolia Autonomous Region Inner Mongolia Hengzheng Industrial Group Co., Ltd., affiliated to the Inner Mongolia Autonomous Region Prison Administration Bureau, has 26 prison enterprises Legal representative of the prison company: Xu Hongguang, Chairman of Inner Mongolia Hengzheng Industrial Group Co., Ltd. His official positions in the prison system: Communist Party Committee Member and Deputy Director of the Ministry of Justice of the Inner Mongolia Autonomous Region; Deputy Secretary of the Party Committee and Director of the Inner Mongolia Autonomous Region Prison Administration Bureau.1 Business areas: Metal processing; machinery manufacturing; production of building materials; real estate; wood processing; garment manufacturing; agricultural production, agricultural and livestock product processing and related consulting services2 The Inner Mongolia Autonomous Region Prison Administration Bureau is the functional organization of Inner Mongolia government in charge of prison-related work in the province. There are 22 units within the province’s prison system. The province’s direct-subordinate prison system has 960,000 mu of land and 22 prison enterprises, which are mainly engaged in machinery manufacturing, production of building materials and coals, garment processing and food production.3 Address: 3 Xinhua West Street, Hohhot City, Inner Mongolia Autonomous Region No. Company Name of the Legal Person Legal Registered Business Scope Company Notes on the Prison Name Prison, to which and representative/Title Capital Address the Company Shareholder(s) Belongs 1 Inner Inner Mongolia Inner Mongolia Xu Hongguang 44.17 Metal processing; Machinery 3 Xinhua West Inner Mongolia Autonomous Region Prison Mongolia Autonomous Hengzheng Chairman of Inner million manufacturing; Production of Street, Hohhot, Administration Bureau is the functional Hengzheng Region Prison Industrial Mongolia Hengzheng yuan building materials; Real estate; Inner Mongolia organization of Inner Mongolia government Industrial Administration Group Co., Ltd. -

Global Offering
中國聖牧有機奶業有限公司 CHINA SHENGMU ORGANIC MILK LIMITED MILK ORGANIC SHENGMU CHINA CHINA SHENGMU ORGANIC MILK LIMITED 中國聖牧有機奶業有限公司 (Incorporated in the Cayman Islands with limited liability) Stock Code: 1432 Global CHINA SHENGMU ORGANIC MILK LIMITED 中國聖牧有機奶業有限公司 Offering Joint Sponsors Joint Global Coordinators, Joint Bookrunners and Joint Lead Managers Joint Bookrunners and Joint Lead Managers (In alphabetical order) ShengMu_IPO_G01J(24mm)_05.indd 1 14年6月25日 下午2:29 IMPORTANT IMPORTANT: If you are in any doubt about any of the contents of this prospectus, you should obtain independent professional advice. CHINA SHENGMU ORGANIC MILK LIMITED 中國聖牧有機奶業有限公司 (Incorporated in the Cayman Islands with limited liability) Global Offering Total number of Offer Shares under the : 444,800,000 Shares (subject to the Global Offering Over-allotment Option) Number of Hong Kong Public Offer Shares : 44,480,000 Shares (subject to adjustment) Number of International Offer Shares : 400,320,000 Shares (subject to adjustment and the Over-allotment Option) Offer Price : Not more than HK$2.95 per Share and expected to be not less than HK$2.39 per Share, plus brokerage of 1%, SFC transaction levy of 0.003% and Hong Kong Stock Exchange trading fee of 0.005% (payable in full on application and subject to refund on final pricing) Nominal value : HK$0.00001 per Share Stock code : 1432 Joint Sponsors, Joint Global Coordinators, Joint Bookrunners and Joint Lead Managers Joint Bookrunners and Joint Lead Managers (in alphabetical order) Hong Kong Exchanges and Clearing Limited, The Stock Exchange of Hong Kong Limited and Hong Kong Securities Clearing Company Limited take no responsibility for the contents of this prospectus, make no representation as to its accuracy or completeness and expressly disclaim any liability whatsoever for any loss howsoever arising from or in reliance upon the whole or any part of the contents of this prospectus. -

Minimum Wage Standards in China August 11, 2020
Minimum Wage Standards in China August 11, 2020 Contents Heilongjiang ................................................................................................................................................. 3 Jilin ............................................................................................................................................................... 3 Liaoning ........................................................................................................................................................ 4 Inner Mongolia Autonomous Region ........................................................................................................... 7 Beijing......................................................................................................................................................... 10 Hebei ........................................................................................................................................................... 11 Henan .......................................................................................................................................................... 13 Shandong .................................................................................................................................................... 14 Shanxi ......................................................................................................................................................... 16 Shaanxi ...................................................................................................................................................... -

47052-002: Low-Carbon District Heating Project in Hohhot in Inner
Environmental Impact Assessment Project Number: 47052 July 2014 People’s Republic of China: Low Carbon District Heating Project in Hohhot in Inner Mongolia Autonomous Region Prepared by Hohhot City Development Investment and Operation Company and Hohhot Chengfa Heating Company for Asian Development Bank This is a document of the borrower. The views expressed herein do not necessarily represent those of ADB’s Board of Directors, Management, or staff, and may be preliminary in nature. CURRENCY EQUIVALENTS (as of 25 June 2014) Currency unit – Yuan (CNY) CNY1.00 = $ 0.1603 $1.00 = CNY 6.2402 ABBREVIATIONS ADB Asian Development Bank AP Affected Person ASL Above Sea Level CEMS Continuous Emissions Monitoring System CHP Combined Heat and Power CNY Chinese Yuan CSEMP Construction Site Environmental Management Plan EA Executing Agency EHS Environment, Health and Safety EHSS Environment, Health and Safety Specialist EHSU Environment, Health and Safety Unit EIA Environmental Impact Assessment EMoP Environmental Monitoring Plan EMP Environmental Management Plan EMS Environmental Monitoring Station EPB Environmental Protection Bureau FGD Flue-Gas Desulfurization FSR Feasibility Study Report GDP Gross Domestic Product GHG Green House Gas GIMAR Government of Inner Mongolia Autonomous Region GIP Good International Practice GRM Grievance Redress Mechanism HCDIO Hohhot City Development Investment and Operation Company HDPE High Density Polyethylene HES Heat Exchange Station HH Household HSP Heat Supply Plant IA Implementing Agency IEE Initial Environmental -

Cdm Afforestation Project Environmental and Social
(Research Institute of Forest Ecology, Environment and Protection, China Academy of Forestry) EIB (European Investment Bank) CDM AFFORESTATION PROJECT IMAR (Inner Mongolia Autonomous Region) ENVIRONMENTAL AND SOCIAL IMPACT ASSESSMENT September, 2008 2 # Dongxiaofu, Haidian Distinct Beijing, P.R. China EIB Loan CDM Afforestation Project ESIA report Project Name: European Investment Bank Loan Clean Development Mechanism Afforestation Project Commission Unit: Inner Mongolia Forestry Administration, PRC (IMFA) Project Director: Fu Yaping ESIA Team Members: Fu Yaping Research Institute of Forest Ecology, Environment and Protection, CAF Li Yu Research Institute of Forest Ecology, Environment and Protection, CAF Li Xingchun Research Institute of Forest Ecology, Environment and Protection, CAF Xiao Wenfa Research Institute of Forest Ecology, Environment and Protection, CAF Zhang Yongan Research Institute of Forest Ecology, Environment and Protection, CAF Ma Zuoli Research Institute of Forest Ecology, Environment and Protection, CAF Bai Liping Research Institute of Forest Ecology, Environment and Protection, CAF Wang Jiangling North China Electric Power University Xin Jing North China Electric Power University Du Xianyuan North China Electric Power University Liu Jianlin North China Electric Power University Gao Qian North China Electric Power University Wang Lili Beijing Normal University Chen Jie Forestry Survey and Design Academy of IMAR Lv Xin Forestry Survey and Design Academy of IMAR RIFFEEP September, 2008 EIB Loan CDM Afforestation Project -

Inner Mongolia Autonomous Region Environment Improvement Project
Environmental Monitoring Report Project Number: 40634-013 April 2017 PRC: Inner Mongolia Autonomous Region Environment Improvement Project Prepared by Inner Mongolia Project Management Office and Energy and Environment Development Research Center This report has been submitted to ADB by the Inner Mongolia Project Management Office and EED and is made publicly available in accordance with ADB’s public communications policy (2005). It does not necessarily reflect the views of ADB. This environmental monitoring report is a document of the borrower. The views expressed herein do not necessarily represent those of ADB's Board of Directors, Management, or staff, and may be preliminary in nature. Your attention is directed to the “terms of use” section on ADB’s website. In preparing any country program or strategy, financing any project, or by making any designation of or reference to a particular territory or geographic area in this document, the Asian Development Bank does not intend to make any judgments as to the legal or other status of any territory or area. Environmental Monitoring Report (July – Dec. 2016) Project Number: Loan_No.2658-PRC April 2017 PRC: Inner Mongolia Autonomous Region Environmental Improvement Project (Phase II) Submit by: Inner Mongolia Autonomous Region PMO Prepared by: Energy and Environmental Development Research Center The Project Leading Group Office of the ADB Loan Inner Mongolia Autonomous Region GovernmentThe views expressed submitted herein the are report those to ofthe the ADB, consultant and issued and do in not accordance necessarily withrepresent the ADB's those of ADB’s Environmentalmembers, Board Safeguard of Directors, Policies Management, (2009). or This staff, report and may may be not preliminary reflect the in nature. -

Annual Report 2019 Contents
Stock Code: 360 ANNUAL REPORT 2019 CONTENTS Corporate Information 2 Management Discussion and Analysis 3 Profiles of the Directors and Senior Management 15 Corporate Governance Report 18 Environmental, Social and Governance Report 29 Report of the Directors 37 Independent Auditor’s Report 53 Consolidated Statement of Profit or Loss and Other Comprehensive Income 60 Consolidated Statement of Financial Position 62 Consolidated Statement of Changes in Equity 64 Consolidated Statement of Cash Flows 65 Notes to the Consolidated Financial Statements 67 Financial Summary 176 Annual Report 2019 New Focus Auto Tech Holdings Limited 1 CORPORATE INFORMATION Directors Legal Advisers Executive Director Paul Hastings Tong Fei (appointed with effect from 1 July 2019) 21-22/F, Bank of China Tower 1 Garden Road Non-executive Directors Hong Kong Wang Zhenyu Zhang Jianxing (Acting Chairman with effect from Principal Share Registrar and 1 July 2019) Transfer Office SMP Partner (Cayman) Limited Independent Non-executive Directors 3rd Floor, Royal Bank House Hu Yuming 24 Shedden Road Lin Lei George Town Zhang Xiaoya Grand Cayman KY1-1110 Cayman Islands Company Secretary Liu Xiao Hua Branch Share Registrar and Transfer Office in Hong Kong Registered Office Computershare Hong Kong Investor Services Cricket Square Limited Hutchins Drive 17M/F, Hopewell Centre P.O. Box 2681 183 Queen’s Road East Grand Cayman KY1-1111 Wan Chai Cayman Islands Hong Kong Principal Place of Business in Hong Kong Stock Code 5/F, 180 Hennessy Road 360 Wan Chai Hong Kong Website https://www.nfa360.com -

China Mengshu Ecological Group Company Limited 中國蒙樹生態集團有限公司 (Incorporated in the Cayman Islands with Limited Liability)
The Stock Exchange of Hong Kong Limited and the Securities and Futures Commission take no responsibility for the contents of this Application Proof, make no representation as to its accuracy or completeness and expressly disclaim any liability whatsoever for any loss howsoever arising from or in reliance upon the whole or any part of the contents of this Application Proof. Application Proof of China Mengshu Ecological Group Company Limited 中國蒙樹生態集團有限公司 (Incorporated in the Cayman Islands with limited liability) WARNING The publication of this Application Proof is required by The Stock Exchange of Hong Kong Limited (the “Stock Exchange”)/the Securities and Futures Commission (the “Commission”) solely for the purpose of providing information to the public in Hong Kong. This Application Proof is in draft form. The information contained in it is incomplete and is subject to change which can be material. By viewing this document, you acknowledge, accept and agree with China Mengshu Ecological Group Company Limited (the “Company”), its sponsor, advisers or member of the underwriting syndicate that: (a) this document is only for the purpose of providing information about the Company to the public in Hong Kong and not for any other purposes. No investment decision should be based on the information contained in this document; (b) the publication of this document or supplemental, revised or replacement pages on the Stock Exchange’s website does not give rise to any obligation of the Company, its sponsor, advisers or members of the underwriting -

Corporate Information
THIS DOCUMENT IS IN DRAFT FORM, INCOMPLETE AND SUBJECT TO CHANGE AND THAT THE INFORMATION MUST BE READ IN CONJUNCTION WITH THE SECTION HEADED “WARNING” ON THE COVER OF THIS DOCUMENT. CORPORATE INFORMATION Registered office PO Box 309 3day CI (i) App1A-6 Ugland House Grand Cayman, KY1-1104 Cayman Islands Principal place of business in Room 606-607 App1A-6 S.342(1)(a)(v) Hong Kong 6/F, China Merchants Building 3day CI (i) 152-155 Connaught Road Central, Hong Kong Headquarters and principal place of Food Industry Park, Deng Kou County App1A-29(2) App1A-43 business in China Bayannur City App1A-6 3day CI (i) Inner Mongolia Autonomous Region PRC Joint company secretaries Mr. LI Yundong (李運動) LR8.17 App1A-42 Flat 3 of Unit 1 App1A-3 LR19.05(2) Tower 2 of Dianlier Company Dormitory 3day CI (ii) Yinxindong Road Yinxin District, Hohhot City Inner Mongolia Autonomous Region PRC Mr. AU Wai Keung (區偉強) (HKICPA) 3day CI (iii) Flat C, 4/F, Blk 6 Pokfulam Gardens Pokfulam, Hong Kong Authorized representative(s) Mr. CUI Ruicheng (崔瑞成) LR19.05(2)(a) 3day CI (ii) Flat 4 of Unit 5 Tower 4 of Caoyuanmingzhu Hailaerxi Road Huimin District, Hohhot City Inner Mongolia Autonomous Region PRC Mr. AU Wai Keung (區偉強) Flat C, 4/F, Blk 6 Pokfulam Gardens Pokfulam, Hong Kong Audit committee Ms. GE Xiaoping (葛曉萍) (Chairman) 3day CI (iv) Mr. LI Changqing (李長青) Mr. CUI Guiyong (崔桂勇) Remuneration committee Mr. WONG Kun Kau (黃灌球)(Chairman) 3day CI (iv) Mr. LI Changqing (李長青) Mr. SUN Qian (孫謙) —81— THIS DOCUMENT IS IN DRAFT FORM, INCOMPLETE AND SUBJECT TO CHANGE AND THAT THE INFORMATION MUST BE READ IN CONJUNCTION WITH THE SECTION HEADED “WARNING” ON THE COVER OF THIS DOCUMENT.