Molecular Signatures of Colon Cancer-Associated Fibroblasts
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Sonic Hedgehog-Gli1 Signaling and Cellular Retinoic Acid Binding Protein 1 Gene Regulation in Motor Neuron Differentiation and Diseases
International Journal of Molecular Sciences Article Sonic Hedgehog-Gli1 Signaling and Cellular Retinoic Acid Binding Protein 1 Gene Regulation in Motor Neuron Differentiation and Diseases Yu-Lung Lin y, Yi-Wei Lin y, Jennifer Nhieu y, Xiaoyin Zhang and Li-Na Wei * Department of Pharmacology, University of Minnesota, Minneapolis, MN 55455, USA; [email protected] (Y.-L.L.); [email protected] (Y.-W.L.); [email protected] (J.N.); [email protected] (X.Z.) * Correspondence: [email protected]; Tel.: +1-612-6259402 Contributed equally. y Received: 29 April 2020; Accepted: 7 June 2020; Published: 9 June 2020 Abstract: Cellular retinoic acid-binding protein 1 (CRABP1) is highly expressed in motor neurons. Degenerated motor neuron-like MN1 cells are engineered by introducing SODG93A or AR-65Q to model degenerated amyotrophic lateral sclerosis (ALS) or spinal bulbar muscular atrophy neurons. Retinoic acid (RA)/sonic hedgehog (Shh)-induced embryonic stem cells differentiation into motor neurons are employed to study up-regulation of Crabp1 by Shh. In SODG93A or AR-65Q MN1 neurons, CRABP1 level is reduced, revealing a correlation of motor neuron degeneration with Crabp1 down-regulation. Up-regulation of Crabp1 by Shh is mediated by glioma-associated oncogene homolog 1 (Gli1) that binds the Gli target sequence in Crabp10s neuron-specific regulatory region upstream of minimal promoter. Gli1 binding triggers chromatin juxtaposition with minimal promoter, activating transcription. Motor neuron differentiation and Crabp1 up-regulation are both inhibited by blunting Shh with Gli inhibitor GANT61. Expression data mining of ALS and spinal muscular atrophy (SMA) motor neurons shows reduced CRABP1, coincided with reduction in Shh-Gli1 signaling components. -

Cell Line-Dependent Variability of Coordinate Expression of P75ntr and CRABP1 and Modulation of Effects of Fenretinide on Neuroblastoma Cells
Hindawi Publishing Corporation Oxidative Medicine and Cellular Longevity Volume 2016, Article ID 7568287, 8 pages http://dx.doi.org/10.1155/2016/7568287 Research Article Cell Line-Dependent Variability of Coordinate Expression of p75NTR and CRABP1 and Modulation of Effects of Fenretinide on Neuroblastoma Cells Yaoli Pu Yang, Simeng Wang, Xingguo Li, and Nina F. Schor Department of Pediatrics, University of Rochester School of Medicine and Dentistry, Rochester, NY 14642, USA Correspondence should be addressed to Nina F. Schor; nina [email protected] Received 10 September 2015; Revised 18 October 2015; Accepted 22 October 2015 Academic Editor: Giuseppe Filomeni Copyright © 2016 Yaoli Pu Yang et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Neuroblastoma is a childhood neural crest tumor. Fenretinide, a retinoic acid analogue, induces accumulation of mitochondrial reactive oxygen species and consequent apoptosis in neuroblastoma cells. The p75 neurotrophin receptor (p75NTR) enhances the antineuroblastoma cell efficacy of fenretinide in vitro. We examined the role of the retinoid binding protein, CRABP1, in p75NTR- mediated potentiation of the efficacy of fenretinide. Knockdown and overexpression, respectively, of either p75NTR or CRABP1 were effected in neuroblastoma cell lines using standard techniques. Expression was determined by qRT-PCR and confirmed atthe protein level by Western blot. Metabolic viability was determined by Alamar blue assay. While protein content of CRABP1 correlated roughly with that of p75NTR in the three neuroblastoid or epithelioid human neuroblastoma cell lines studied, manipulation of p75NTR expression resulted in cell line-dependent, variable change in CRABP1 expression. -
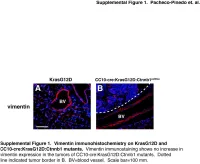
Supplemental Figure 1. Vimentin
Double mutant specific genes Transcript gene_assignment Gene Symbol RefSeq FDR Fold- FDR Fold- FDR Fold- ID (single vs. Change (double Change (double Change wt) (single vs. wt) (double vs. single) (double vs. wt) vs. wt) vs. single) 10485013 BC085239 // 1110051M20Rik // RIKEN cDNA 1110051M20 gene // 2 E1 // 228356 /// NM 1110051M20Ri BC085239 0.164013 -1.38517 0.0345128 -2.24228 0.154535 -1.61877 k 10358717 NM_197990 // 1700025G04Rik // RIKEN cDNA 1700025G04 gene // 1 G2 // 69399 /// BC 1700025G04Rik NM_197990 0.142593 -1.37878 0.0212926 -3.13385 0.093068 -2.27291 10358713 NM_197990 // 1700025G04Rik // RIKEN cDNA 1700025G04 gene // 1 G2 // 69399 1700025G04Rik NM_197990 0.0655213 -1.71563 0.0222468 -2.32498 0.166843 -1.35517 10481312 NM_027283 // 1700026L06Rik // RIKEN cDNA 1700026L06 gene // 2 A3 // 69987 /// EN 1700026L06Rik NM_027283 0.0503754 -1.46385 0.0140999 -2.19537 0.0825609 -1.49972 10351465 BC150846 // 1700084C01Rik // RIKEN cDNA 1700084C01 gene // 1 H3 // 78465 /// NM_ 1700084C01Rik BC150846 0.107391 -1.5916 0.0385418 -2.05801 0.295457 -1.29305 10569654 AK007416 // 1810010D01Rik // RIKEN cDNA 1810010D01 gene // 7 F5 // 381935 /// XR 1810010D01Rik AK007416 0.145576 1.69432 0.0476957 2.51662 0.288571 1.48533 10508883 NM_001083916 // 1810019J16Rik // RIKEN cDNA 1810019J16 gene // 4 D2.3 // 69073 / 1810019J16Rik NM_001083916 0.0533206 1.57139 0.0145433 2.56417 0.0836674 1.63179 10585282 ENSMUST00000050829 // 2010007H06Rik // RIKEN cDNA 2010007H06 gene // --- // 6984 2010007H06Rik ENSMUST00000050829 0.129914 -1.71998 0.0434862 -2.51672 -

Detailed Review Paper on Retinoid Pathway Signalling
1 1 Detailed Review Paper on Retinoid Pathway Signalling 2 December 2020 3 2 4 Foreword 5 1. Project 4.97 to develop a Detailed Review Paper (DRP) on the Retinoid System 6 was added to the Test Guidelines Programme work plan in 2015. The project was 7 originally proposed by Sweden and the European Commission later joined the project as 8 a co-lead. In 2019, the OECD Secretariat was added to coordinate input from expert 9 consultants. The initial objectives of the project were to: 10 draft a review of the biology of retinoid signalling pathway, 11 describe retinoid-mediated effects on various organ systems, 12 identify relevant retinoid in vitro and ex vivo assays that measure mechanistic 13 effects of chemicals for development, and 14 Identify in vivo endpoints that could be added to existing test guidelines to 15 identify chemical effects on retinoid pathway signalling. 16 2. This DRP is intended to expand the recommendations for the retinoid pathway 17 included in the OECD Detailed Review Paper on the State of the Science on Novel In 18 vitro and In vivo Screening and Testing Methods and Endpoints for Evaluating 19 Endocrine Disruptors (DRP No 178). The retinoid signalling pathway was one of seven 20 endocrine pathways considered to be susceptible to environmental endocrine disruption 21 and for which relevant endpoints could be measured in new or existing OECD Test 22 Guidelines for evaluating endocrine disruption. Due to the complexity of retinoid 23 signalling across multiple organ systems, this effort was foreseen as a multi-step process. -

Supplementary Table 1: Adhesion Genes Data Set
Supplementary Table 1: Adhesion genes data set PROBE Entrez Gene ID Celera Gene ID Gene_Symbol Gene_Name 160832 1 hCG201364.3 A1BG alpha-1-B glycoprotein 223658 1 hCG201364.3 A1BG alpha-1-B glycoprotein 212988 102 hCG40040.3 ADAM10 ADAM metallopeptidase domain 10 133411 4185 hCG28232.2 ADAM11 ADAM metallopeptidase domain 11 110695 8038 hCG40937.4 ADAM12 ADAM metallopeptidase domain 12 (meltrin alpha) 195222 8038 hCG40937.4 ADAM12 ADAM metallopeptidase domain 12 (meltrin alpha) 165344 8751 hCG20021.3 ADAM15 ADAM metallopeptidase domain 15 (metargidin) 189065 6868 null ADAM17 ADAM metallopeptidase domain 17 (tumor necrosis factor, alpha, converting enzyme) 108119 8728 hCG15398.4 ADAM19 ADAM metallopeptidase domain 19 (meltrin beta) 117763 8748 hCG20675.3 ADAM20 ADAM metallopeptidase domain 20 126448 8747 hCG1785634.2 ADAM21 ADAM metallopeptidase domain 21 208981 8747 hCG1785634.2|hCG2042897 ADAM21 ADAM metallopeptidase domain 21 180903 53616 hCG17212.4 ADAM22 ADAM metallopeptidase domain 22 177272 8745 hCG1811623.1 ADAM23 ADAM metallopeptidase domain 23 102384 10863 hCG1818505.1 ADAM28 ADAM metallopeptidase domain 28 119968 11086 hCG1786734.2 ADAM29 ADAM metallopeptidase domain 29 205542 11085 hCG1997196.1 ADAM30 ADAM metallopeptidase domain 30 148417 80332 hCG39255.4 ADAM33 ADAM metallopeptidase domain 33 140492 8756 hCG1789002.2 ADAM7 ADAM metallopeptidase domain 7 122603 101 hCG1816947.1 ADAM8 ADAM metallopeptidase domain 8 183965 8754 hCG1996391 ADAM9 ADAM metallopeptidase domain 9 (meltrin gamma) 129974 27299 hCG15447.3 ADAMDEC1 ADAM-like, -

Human Oxygen Sensing May Have Origins in Prokaryotic Elongation Factor Tu Prolyl-Hydroxylation
Human oxygen sensing may have origins in prokaryotic elongation factor Tu prolyl-hydroxylation John S. Scottia, Ivanhoe K. H. Leunga,1,2, Wei Gea,b,1, Michael A. Bentleyc, Jordi Papsd, Holger B. Kramere, Joongoo Leea, WeiShen Aika, Hwanho Choia, Steinar M. Paulsenc,3, Lesley A. H. Bowmanf, Nikita D. Loika,4, Shoichiro Horitaa,e, Chia-hua Hoa,5, Nadia J. Kershawa,6, Christoph M. Tangf, Timothy D. W. Claridgea, Gail M. Prestonc, Michael A. McDonougha, and Christopher J. Schofielda,7 aChemistry Research Laboratory, Department of Chemistry, University of Oxford, Oxford OX1 3TA, United Kingdom; bChinese Academy of Medical Sciences, Beijing 100005, China; cDepartment of Plant Sciences, University of Oxford, Oxford OX1 3RB, United Kingdom; dDepartment of Zoology, University of Oxford, Oxford OX1 3PS, United Kingdom; eDepartment of Physiology, Anatomy, and Genetics, University of Oxford, Oxford OX1 3QX, United Kingdom; and fDepartment of Pathology, University of Oxford, Oxford OX1 3RE, United Kingdom Edited by Gregg L. Semenza, The Johns Hopkins University School of Medicine, Baltimore, MD, and approved August 5, 2014 (received for review May 30, 2014) The roles of 2-oxoglutarate (2OG)-dependent prolyl-hydroxylases Results in eukaryotes include collagen stabilization, hypoxia sensing, and Pseudomonas spp. Contain a Functional PHD. To investigate the role translational regulation. The hypoxia-inducible factor (HIF) sensing of a putative PHD homolog in Pseudomonas aeruginosa (PPHD), system is conserved in animals, but not in other organisms. How- we initially characterized a PPHD insertional mutant strain. ever, bioinformatics imply that 2OG-dependent prolyl-hydroxy- Metabolic screening studies revealed that the PPHD mutant strain lases (PHDs) homologous to those acting as sensing components displays impaired growth in the presence of iron chelators (e.g., for the HIF system in animals occur in prokaryotes. -

Human Induced Pluripotent Stem Cell–Derived Podocytes Mature Into Vascularized Glomeruli Upon Experimental Transplantation
BASIC RESEARCH www.jasn.org Human Induced Pluripotent Stem Cell–Derived Podocytes Mature into Vascularized Glomeruli upon Experimental Transplantation † Sazia Sharmin,* Atsuhiro Taguchi,* Yusuke Kaku,* Yasuhiro Yoshimura,* Tomoko Ohmori,* ‡ † ‡ Tetsushi Sakuma, Masashi Mukoyama, Takashi Yamamoto, Hidetake Kurihara,§ and | Ryuichi Nishinakamura* *Department of Kidney Development, Institute of Molecular Embryology and Genetics, and †Department of Nephrology, Faculty of Life Sciences, Kumamoto University, Kumamoto, Japan; ‡Department of Mathematical and Life Sciences, Graduate School of Science, Hiroshima University, Hiroshima, Japan; §Division of Anatomy, Juntendo University School of Medicine, Tokyo, Japan; and |Japan Science and Technology Agency, CREST, Kumamoto, Japan ABSTRACT Glomerular podocytes express proteins, such as nephrin, that constitute the slit diaphragm, thereby contributing to the filtration process in the kidney. Glomerular development has been analyzed mainly in mice, whereas analysis of human kidney development has been minimal because of limited access to embryonic kidneys. We previously reported the induction of three-dimensional primordial glomeruli from human induced pluripotent stem (iPS) cells. Here, using transcription activator–like effector nuclease-mediated homologous recombination, we generated human iPS cell lines that express green fluorescent protein (GFP) in the NPHS1 locus, which encodes nephrin, and we show that GFP expression facilitated accurate visualization of nephrin-positive podocyte formation in -

Role of Cellular Retinoic Acid Binding Protein 2
Airway biology Dysregulation of elastin expression by fibroblasts in Thorax: first published as 10.1136/thx.2007.093302 on 11 July 2008. Downloaded from pulmonary emphysema: role of cellular retinoic acid binding protein 2 L Plantier,1,2,3 C Rochette-Egly,4 D Goven,1 A Boutten,1,5 M Bonay,1,6 G Lese`che,3,7 M Fournier,2,3 B Crestani,1,2,3 J Boczkowski1,8 1 INSERM U700, Hoˆpital Bichat, ABSTRACT in the lung is a stimulus for the alveologenesis 2 Paris, France; Services de Background: All-trans retinoic acid (ATRA) stimulates phase of lung development3; secondly, all-trans Pneumologie, Hoˆpital Bichat, elastin synthesis by lung fibroblasts and induces alveolar retinoic acid (ATRA) induces the expression of Assistance Publique-Hoˆpitaux de 4 Paris, Paris, France; 3 Universite´ regeneration in animal models of pulmonary emphysema. elastin in lung fibroblasts ; thirdly, vitamin A Paris 7, UFR me´dicale Denis However, ATRA treatment has had disappointing results deficiency leads to an emphysema-like phenotype Diderot, Faculte´Bichat, Paris, in human emphysema. It was hypothesised that a defect in the lung of adult rats5; finally, the systemic 4 France; Institut de Ge´ne´tique in the ATRA signalling pathway contributes to the defect administration of ATRA has been reported to et de Biologie Mole´culaire et Cellulaire, Strasbourg, France; of alveolar repair in the human emphysematous lung. abrogate elastase induced emphysema in adult rats 5 Service de Biochimie A, Hoˆpital Methods: Fibroblasts were cultured from the lung of 10 and mice.67 Retinoic acid exerts its effects by Bichat, Assistance Publique- control subjects and eight patients with emphysema. -

ADAMTS1, CRABP1, and NR3C1 Identified As
Cellular Oncology 28 (2006) 259–272 259 IOS Press ADAMTS1, CRABP1,andNR3C1 identified as epigenetically deregulated genes in colorectal tumorigenesis Guro E. Lind a, Kristine Kleivi b,∗, Gunn I. Meling c, Manuel R. Teixeira d, Espen Thiis-Evensen e, Torleiv O. Rognum f and Ragnhild A. Lothe a,g,∗∗ a Department of Cancer Prevention, Institute for Cancer Research, Rikshospitalet-Radiumhospitalet Medical Centre, Oslo, Norway b Department of Genetics, Institute for Cancer Research, Rikshospitalet-Radiumhospitalet Medical Centre, Oslo, Norway c Surgical Department, Faculty Division Akershus University Hospital, University of Oslo, Oslo, Norway d Department of Genetics, Portuguese Oncology Institute, Porto, Portugal e Medical Department, Rikshospitalet-Radiumhospitalet Medical Centre, Oslo, Norway f Institute of Forensic Medicine, Institute for Cancer Research, Rikshospitalet-Radiumhospitalet Medical Centre, Oslo, Norway g Department of Molecular Biosciences, University of Oslo, Oslo, Norway Abstract. Background: Gene silencing through CpG island hypermethylation is a major mechanism in cancer development. In the present study, we aimed to identify and validate novel target genes inactivated through promoter hypermethylation in colorectal tumor development. Methods: With the use of microarrays, the gene expression profiles of colon cancer cell lines before and after treatment with the demethylating agent 5-aza-2 -deoxycytidine were identified and compared. The expression of the responding genes was compared with microarray expression data of primary colorectal carcinomas. Four of these down- regulated genes were subjected to methylation-specific PCR, bisulphite sequencing, and quantitative gene expression analysis using tumors (n = 198), normal tissues (n = 44), and cell lines (n = 30). Results: Twenty-one genes with a CpG island in their promoter responded to treatment in cell lines, and were simultaneously down-regulated in primary colorectal carcinomas. -

Osteogenesis Imperfecta Types I-XI Implications for the Neonatal Nurse Jody Womack , RNC-NIC, NNP-BC, MS
Ksenia Zukowsky, PhD, APRN, NNP-BC ❍ Section Editor Beyond the Basics 3.0 HOURS Continuing Education Osteogenesis Imperfecta Types I-XI Implications for the Neonatal Nurse Jody Womack , RNC-NIC, NNP-BC, MS ABSTRACT Osteogenesis imperfecta (OI), also called “brittle bone disease,” is a rare heterozygous connective tissue disorder that is caused by mutations of genes that affect collagen. Osteogenesis imperfecta is characterized by decreased bone mass, bone fragility, and skin hyperlaxity. The phenotype present is determined according to the mutation on the affected gene as well as the type and location of the mutation. Osteogenesis imperfecta is neither preventable nor treatable. Osteogenesis imperfecta is classified into 11 types to date, on the basis of their clinical symptoms and genetic components. This article discusses the definition of the disease, the classifications on the basis of its clinical features, incidence, etiology, and pathogenesis. In addition, phenotype, natural history, diagnosis and manage- ment of this disease, recurrence risk, and, most importantly, the implications for the neonatal nurse and management for the family are discussed. Key Words: brittle bone disease , COL1A1 , COL1A2 , collagen disorders , osteogenesis imperfecta steogenesis imperfecta (OI) is a rare connec- is imperative to help the patient and the parents car- tive tissue disorder that is caused by muta- ing for infants born with OI. tions of genes that affect collagen. 1-4 Collagen O is the major protein of connective tissues, which is the REVIEW OF LITERATURE framework of bones. When collagen is not function- ing properly or there is lack of collagen in the tissue, Osteogenesis imperfecta was thought to have affected bones break easily. -

Primepcr™Assay Validation Report
PrimePCR™Assay Validation Report Gene Information Gene Name cellular retinoic acid binding protein I Gene Symbol Crabp1 Organism Mouse Gene Summary Description Not Available Gene Aliases AI326249, Crabp-1, CrabpI, Rbp-5 RefSeq Accession No. NC_000075.6, NT_039474.8 UniGene ID Mm.34797 Ensembl Gene ID ENSMUSG00000032291 Entrez Gene ID 12903 Assay Information Unique Assay ID qMmuCID0018468 Assay Type SYBR® Green Detected Coding Transcript(s) ENSMUST00000034830 Amplicon Context Sequence CTGTGCGCACCACGGAGATCAACTTCAAGGTCGGAGAGGGCTTCGAGGAGGAG ACAGTGGACGGACGCAAATGCAGGAGTTTACCCACGTGGGAGAATGAGAACAA GATTCACTGCACACAGACACTTCTTGAGGGGGATGGCCCTAAAA Amplicon Length (bp) 120 Chromosome Location 9:54765585-54768456 Assay Design Intron-spanning Purification Desalted Validation Results Efficiency (%) 96 R2 0.999 cDNA Cq 19.04 cDNA Tm (Celsius) 84.5 gDNA Cq 43.1 Specificity (%) 100 Information to assist with data interpretation is provided at the end of this report. Page 1/4 PrimePCR™Assay Validation Report Crabp1, Mouse Amplification Plot Amplification of cDNA generated from 25 ng of universal reference RNA Melt Peak Melt curve analysis of above amplification Standard Curve Standard curve generated using 20 million copies of template diluted 10-fold to 20 copies Page 2/4 PrimePCR™Assay Validation Report Products used to generate validation data Real-Time PCR Instrument CFX384 Real-Time PCR Detection System Reverse Transcription Reagent iScript™ Advanced cDNA Synthesis Kit for RT-qPCR Real-Time PCR Supermix SsoAdvanced™ SYBR® Green Supermix Experimental Sample qPCR Mouse Reference Total RNA Data Interpretation Unique Assay ID This is a unique identifier that can be used to identify the assay in the literature and online. Detected Coding Transcript(s) This is a list of the Ensembl transcript ID(s) that this assay will detect. -

Proteoglycan Form and Function: a Comprehensive Nomenclature of Proteoglycans
HHS Public Access Author manuscript Author ManuscriptAuthor Manuscript Author Matrix Biol Manuscript Author . Author manuscript; Manuscript Author available in PMC 2016 May 06. Published in final edited form as: Matrix Biol. 2015 March ; 42: 11–55. doi:10.1016/j.matbio.2015.02.003. Proteoglycan form and function: A comprehensive nomenclature of proteoglycans Renato V. Iozzo1 and Liliana Schaefer2 1Department of Pathology, Anatomy and Cell Biology and the Cancer Cell Biology and Signaling Program, Kimmel Cancer Center, Sidney Kimmel Medical College at Thomas Jefferson University, Philadelphia, PA 19107, USA 2Pharmazentrum Frankfurt/ZAFES, Institut für Allgemeine Pharmakologie und Toxikologie, Klinikum der Goethe-Universität Frankfurt am Main, Frankfurt am Main, Germany Abstract We provide a comprehensive classification of the proteoglycan gene families and respective protein cores. This updated nomenclature is based on three criteria: Cellular and subcellular location, overall gene/protein homology, and the utilization of specific protein modules within their respective protein cores. These three signatures were utilized to design four major classes of proteoglycans with distinct forms and functions: the intracellular, cell-surface, pericellular and extracellular proteoglycans. The proposed nomenclature encompasses forty-three distinct proteoglycan-encoding genes and many alternatively-spliced variants. The biological functions of these four proteoglycan families are critically assessed in development, cancer and angiogenesis, and in various acquired and genetic diseases where their expression is aberrant. Keywords Proteoglycan; Glycosaminoglycan; Cancer growth; Angiogenesis; Growth factor modulation Introduction It has been nearly 20 years since the original publication of a comprehensive classification of proteoglycan gene families [1]. For the most part, these classes have been widely accepted. However, a broad and current taxonomy of the various proteoglycan gene families and their products is not available.