Lentigo Maligna: Report of One Case Treated with Radium
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

Critical Evaluation of the So-Called “Junction Nevus”
View metadata, citation and similar papers at core.ac.uk brought to you by CORE provided by Elsevier - Publisher Connector CRITICAL EVALUATION OF THE SO-CALLED "JUNCTION NEVUS* S. WILLIAM BECKER, MS., M.D. The serious study of pigmented nevi was undertaken by many workers in the closing years of the 19th Century. All recognized that the microscopic picture of nevi differed from anything seen in other organs. The presence of nevus cells in both the epidermis and dermis led to concepts of origin at one or the other site, or at both sites. Dermal Origin: Demieville (1) believed that the nevus cells arose from adven- titial and endothelial cells of blood vessels. Bauer (2) and vonRecklinghausen (3) thought that the origin was from endothelium of lymph vessels rather than of blood vessels. Epidermal Origin: According to Abesser (4), Duranti, in 1871, was the first to suggest an epidermal origin of nevus cells. Kromayer (5) stated that the endo- thelium-like cells originate in the basal portion of the epidermis as "Bläschen- zellen", migrate to the dermis and develop connective tissue and elastic fibers, a change which he called "desmoplasia". Abesser (4) agreed that the cells origi- ated in the epithelium and lost their intercellular bridges, but migrated into the dermis as epithelium-like cells, and remained such. Unna (6) advanced the concept that the epithelial cells changed by losing their intercellular bridges and multiplied in groups, a process which he called "Ab- sonderung", then migrated as groups to the dermis, which he called "Abtrop- fung", thus forming pigmented nevi. -

Dermatology DDX Deck, 2Nd Edition 65
63. Herpes simplex (cold sores, fever blisters) PREMALIGNANT AND MALIGNANT NON- 64. Varicella (chicken pox) MELANOMA SKIN TUMORS Dermatology DDX Deck, 2nd Edition 65. Herpes zoster (shingles) 126. Basal cell carcinoma 66. Hand, foot, and mouth disease 127. Actinic keratosis TOPICAL THERAPY 128. Squamous cell carcinoma 1. Basic principles of treatment FUNGAL INFECTIONS 129. Bowen disease 2. Topical corticosteroids 67. Candidiasis (moniliasis) 130. Leukoplakia 68. Candidal balanitis 131. Cutaneous T-cell lymphoma ECZEMA 69. Candidiasis (diaper dermatitis) 132. Paget disease of the breast 3. Acute eczematous inflammation 70. Candidiasis of large skin folds (candidal 133. Extramammary Paget disease 4. Rhus dermatitis (poison ivy, poison oak, intertrigo) 134. Cutaneous metastasis poison sumac) 71. Tinea versicolor 5. Subacute eczematous inflammation 72. Tinea of the nails NEVI AND MALIGNANT MELANOMA 6. Chronic eczematous inflammation 73. Angular cheilitis 135. Nevi, melanocytic nevi, moles 7. Lichen simplex chronicus 74. Cutaneous fungal infections (tinea) 136. Atypical mole syndrome (dysplastic nevus 8. Hand eczema 75. Tinea of the foot syndrome) 9. Asteatotic eczema 76. Tinea of the groin 137. Malignant melanoma, lentigo maligna 10. Chapped, fissured feet 77. Tinea of the body 138. Melanoma mimics 11. Allergic contact dermatitis 78. Tinea of the hand 139. Congenital melanocytic nevi 12. Irritant contact dermatitis 79. Tinea incognito 13. Fingertip eczema 80. Tinea of the scalp VASCULAR TUMORS AND MALFORMATIONS 14. Keratolysis exfoliativa 81. Tinea of the beard 140. Hemangiomas of infancy 15. Nummular eczema 141. Vascular malformations 16. Pompholyx EXANTHEMS AND DRUG REACTIONS 142. Cherry angioma 17. Prurigo nodularis 82. Non-specific viral rash 143. Angiokeratoma 18. Stasis dermatitis 83. -
Diagnostic Pitfall of Localized Lentigo Accompanied by Post-Inflammatory
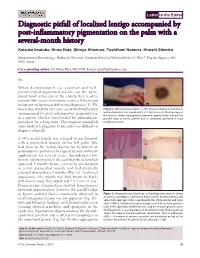
Letter to the Editor Diagnostic pitfall of localized lentigo accompanied by post-inflammatory pigmentation on the palm with a several-month history Keisuke Imafuku, Hiroo Hata, Shinya Kitamura, Toshifumi Nomura, Hiroshi Shimizu Department of Dermatology, Hokkaido University Graduate School of MedicineNorth 15, West 7, Kita-ku, Sapporo 060- 8638, Japan Corresponding author: Dr. Hiroo Hata, MD, PhD, E-mail: [email protected] Sir, When dermatologists see acquired and well- circumscribed pigmented macules on the palm, dorsal hand or forearm of the elderly, they tend to consider blue nevus, hematoma, nevus cell nevus and malignant melanoma as differential diagnoses [1]. We a b herein described the very rare case of localized lentigo Figure 1: Clinical manifestations. a. The macule is brown to dark black, accompanied by post-inflammatory pigmentation well-demarcated, flat, round and 3 x 4 mm in size. b. Dermoscopy of the macule shows homogenous brownish pigmentation without the in a patient who has been treated for palmoplanter parallel ridge or furrow pattern that is commonly observed in acral pustulosis for a long time. This eruption mimicked lentiginous lesion some kinds of lentiginous lesion and it was difficult to diagnose clinically. A 59-year-old female was referred to our hospital with a pigmented macule on her left palm. She had been to the family doctor for treatment of palmoplanter pustulosis by topical steroid ointment application for several years. According to the a history-taking interview, she said that the lesion had b appeared 5 months before referral to our hospital as a tiny pigmented macule and had gradually enlarged during those 5 months (Fig. -

Hutchinson's Melanotic Freckle
Hutchiso’s elaotic freckle Also known as Lentigo maligna What is lentigo maligna? Lentigo maligna is an early form of melanoma. In lentigo maligna the cancer cells are confined to the upper layer of the skin (epidermis). When the cancer cells spread deeper into the skin (to dermis) it is called lentigo maligna melanoma. Lentigo maligna occurs most commonly in sun damaged areas such as the face and neck in fair skinned people over the age of 60. The lesion grows slowly in size over a number of years. Melanoma is a potentially lethal disease and lentigo maligna should be diagnosed and excised as soon as possible. What causes lentigo maligna? The cause of lentigo maligna is sun exposure or solarium use. Factors that predispose a person to developing lentigo maligna or associated condition include: . chronic sun damaged/solar-induced skin damage . fair skin complexion . male gender . a personal history of non melanoma skin cancer and precancerous lesions . older individuals (those between 60 to 80 years are most commonly affected) What does lentigo maligna look like? Lentigo maligna commonly looks like a freckle, age spot, sun spot or brown patch that slowly changes shape and grows in size. The spot may be large in size, irregularly shaped with a smooth surface, and of multiple shades of brown and sometimes other colours. Thickening of part of the lesion, increasing number of colours, ulceration or bleeding can be markers that the lesion is changing into a lentigo maligna melanoma. How is lentigo maligna diagnosed? Lentigo maligna is diagnosed clinically by a dermatologist, sometimes with the help of a dermatoscope (a tool used to magnify and look closely at skin moles). -

Pigmented Contact Dermatitis and Chemical Depigmentation
18_319_334* 05.11.2005 10:30 Uhr Seite 319 Chapter 18 Pigmented Contact Dermatitis 18 and Chemical Depigmentation Hideo Nakayama Contents ca, often occurs without showing any positive mani- 18.1 Hyperpigmentation Associated festations of dermatitis such as marked erythema, with Contact Dermatitis . 319 vesiculation, swelling, papules, rough skin or scaling. 18.1.1 Classification . 319 Therefore, patients may complain only of a pigmen- 18.1.2 Pigmented Contact Dermatitis . 320 tary disorder, even though the disease is entirely the 18.1.2.1 History and Causative Agents . 320 result of allergic contact dermatitis. Hyperpigmenta- 18.1.2.2 Differential Diagnosis . 323 tion caused by incontinentia pigmenti histologica 18.1.2.3 Prevention and Treatment . 323 has often been called a lichenoid reaction, since the 18.1.3 Pigmented Cosmetic Dermatitis . 324 presence of basal liquefaction degeneration, the ac- 18.1.3.1 Signs . 324 cumulation of melanin pigment, and the mononucle- 18.1.3.2 Causative Allergens . 325 ar cell infiltrate in the upper dermis are very similar 18.1.3.3 Treatment . 326 to the histopathological manifestations of lichen pla- 18.1.4 Purpuric Dermatitis . 328 nus. However, compared with typical lichen planus, 18.1.5 “Dirty Neck” of Atopic Eczema . 329 hyperkeratosis is usually milder, hypergranulosis 18.2 Depigmentation from Contact and saw-tooth-shape acanthosis are lacking, hyaline with Chemicals . 330 bodies are hardly seen, and the band-like massive in- 18.2.1 Mechanism of Leukoderma filtration with lymphocytes and histiocytes is lack- due to Chemicals . 330 ing. 18.2.2 Contact Leukoderma Caused Mainly by Contact Sensitization . -

Unilateral Nevus of Ota with Palatal and Optic Disc
Case Report DOI: 10.7860/JCDR/2020/44666.13951 Unilateral Nevus of Ota with Palatal and Optic Section Ophthalmology Disc Pigmentation with Coincidental Preauricular Tag- A Case Report PRASANNA NAREDDY1, AMBATI DIVYA2 ABSTRACT Nevus of Ota also known as oculodermal melanosis presents as hyperpigmentation of face involving ophthalmic and maxillary branches of trigeminal nerve associated with ocular hyperpigmentation. It is due to confinement of melanocytes in the dermis. Most commonly it is unilateral but sometimes it may have bilateral presentation. Typically, it presents at birth but can also be an acquired condition. Frequently seen in Japanese and rarely in Indian subcontinent. It has more predilection towards females. Less frequently, hyperpigmentation is seen in other sites like oral mucosa, tympanum and nasal mucosa. These patients are at high risk of developing glaucoma and malignancy. The author reported a case of 12-year-old male child with unilateral pigmentation of left side face involving forehead, periorbital and cheek, along with ocular pigmentation. Hyperpigmentation of conjunctiva, iris and angles is present in left eye with intraocular pressure being normal in both eyes. Fundus showing optic disc pigmentation in the left eye with cup disc asymmetry in both eyes. Child has coexistent preauricular tag on the left side. Keywords: Congenital, Heterochromia iridis, Ocular pigmentation CASE REPORT in right eye and 14 mm of Hg in left eye. Gonioscopy revealed open A 12-year-old male child presented with complaints of abdominal angles in both eyes with hyperpigmentation of angles in the left eye. pain since 3 days to Paediatric Department where the child was admitted and further evaluation was done. -

How to Optimize Biopsy Pathology of Melanocytic Lesions
London, Dermatopathology Study Day 04.12.15 Pigmented lesions of sun-damaged skin W.J. Mooi Department of Pathology, VU university medical center, Amsterdam [email protected] Lentigo maligna Lentigo maligna • Defining combination of features: a substantial proliferation of atypical melanocytes predominantly in lentiginous arrangement, limited to the epithelial compartment of sun-damaged skin, and manifesting as a flat, impalpable hyperpigmentation, usually with irregular contours and with variations of pigmentation. • Spread into hair follicles usually present • Ascent of atypical melanocytes commonly present • Nests are absent or present • The epidermis is commonly flat and thin, but rete ridges may be present • Cellularity, ascent, nesting, degree of atypia vary within the same lesion • Lichenoid inflammatory response sometimes Lentigo maligna: some diagnostic problems • Distinction between paucicellular LM and reactive melanocytic hyperplasia in sun-damaged skin • ‘Grading’ of severity; assessment of risk of invasion: compromised by variations within the same lesion • Interpretation of small numbers of dermal melanocytes in conjunction with LM • Small dermal melanocytic naevi • Scattered isolated dermal ? pre-existent melanocytes • Lichenoid inflammatory response obscuring LM Paucicellular lentigo maligna versus reactive melanocyte hyperplasia in sun-damaged skin LENTIGO MALIGNA REACTIVE MELANOCYTIC HYPERPLASIA Lentiginous spread with or without nests Lentiginous spread only; no nests Melanocytes often directly side-to-side Melanocytes -

Vitiligo-Like Primary Cutaneous Melanoma One of the Winning Presentations Given by Dermatology Residents at the Cosmetic Surgery Forum in December 2013
RESIDENT REPORTS Vitiligo-like Primary Cutaneous Melanoma One of the winning presentations given by dermatology residents at the Cosmetic Surgery Forum in December 2013. BY HADAS SKUPSKY, MD, JENNIFER K. CHEN, MD, AND KENNETH G. LINDEN, MD melanotic melanomas comprise two percent of all melanomas. The clinical presentation is varied and may include erythematous patches, papules, or plaques.1,2 Depigmented macules and patches Ahave been described in association with both primary and metastatic melanomas. This phenomenon often represents regression of a melanoma or a side effect of melanoma- targeted immunochemotherapy. In addition, vitiligo may present at sites remotely from a melanoma.3-5 However, primary melanoma presenting as a vitiligo-like patch with- out histopathologic evidence of regression is an exceedingly rare phenomenon. To our knowledge, there is only a single Figure 1 Figure 2 report of two cases of vitiligo-like primary melanoma in situ in the literature to date.6 We herein report a case of invasive inferior shoulder with no subcutaneous nodules. She had no lentigo maligna melanoma presenting as a vitiliginous patch cervical, axillary, or supraclavicular lymphadenopathy. Biopsy of and review the possible immunopathogenesis of this lesion. the erythematous macule at the center of the patch revealed a proliferation of typical melanocytes, solitary and in irregular CASE REPORT nests, throughout the lower aspect of the epidermis and focal A 70-year-old female presented with a five-year history of an dermal invasion consistent with a lentigo maligna melanoma asymptomatic hypopigmented patch on her left upper arm. 0.2mm in depth. Biopsy of the superior aspect revealed lentigo Although the patch had initially grown slowly, the patient had maligna melanoma in situ (Figure 3). -

Dealing with Lentigo Maligna
Clinical Dealing with lentigo maligna A challenging case Daniel Mazzoni, Jim Muir more likely with larger lesions and those in higher densities with grouping, on the head and neck.1,2 follicular extension, cytological atypia and even pagetoid spread into the CASE ANSWER 2 upper epidermis. This can make the A man aged 46 years presented to a Ill-defined margins and subclinical determination of clearance of lentigo multidisciplinary team (plastic surgery, extension are common with lentigo maligna difficult.5 radiation oncology, dermatology) with a maligna and, as in this case, lead to A crucial principle is to avoid wound year-long history of a lentigo maligna on involved excision margins.3,4 closures that distort the margin until no the right ear lobe. After initial biopsy, the It can be difficult to differentiate further excisions are needed.3,6 Complex lesion had undergone two wide excisions the histopathological appearance of flaps will distort margins and make with his general practitioner (GP). Both atypical melanocytic hyperplasia seen re-excision problematic. Reconstruction excisions showed margin involvement. in sun-damaged skin from lentigo can be delayed until histopathology The GP referred the patient to a radiation maligna.5 Sun-damaged skin can confirms adequate clearance. oncologist. show features in common with lentigo Confocal microscopy can be used to The initial referral resulted in onward maligna. This includes melanocytes attempt to delineate the extent of lentigo referral to the multidisciplinary team for assessment. Examination revealed a well-healed full thickness skin graft with no clinical or dermoscopic evidence of lentigo maligna (Figure 1). -

Lentigo Maligna Melanoma and Simulants Maui January 2020 Superficial Atypical Melanocytic Proliferations
Superficial Atypical Melanocytic Proliferations II. Lentigo Maligna Melanoma and Simulants Maui January 2020 Superficial Atypical Melanocytic Proliferations • RGP Melanomas • SSM, LMM, ALM, MLM • Intermediate lesions • Dysplastic nevi, Atypical lentiginous proliferations in high CSD skin; Atypical Acral lentiginous nevi • Superficial atypical melanocytic proliferations • Pagetoid plaque-like Spitz nevi; pigmented spindle cell nevus (Reed) • Special site nevi (genital, breast, scalp, ear, flexural, etc). • Superficial atypical melanocytic proliferations of uncertain significance • Atypical/unusual/uncertain examples of all of the above Superficial Atypical Melanocytic Proliferations • RGP Melanomas • SSM, LMM, ALM, MLM • Intermediate lesions • Dysplastic nevi, Atypical lentiginous proliferations in high CSD skin; Atypical Acral lentiginous nevi • Superficial atypical melanocytic proliferations • Pagetoid plaque-like Spitz nevi; pigmented spindle cell nevus (Reed) • Special site nevi (genital, breast, scalp, ear, flexural, etc). • Superficial atypical melanocytic proliferations of uncertain significance • Atypical/unusual/uncertain examples of all of the above High CSD Melanomas and Simulants. D Elder, Maui, HI Jan 2020 Lentigo maligna melanoma Atypical lentiginous nevi/proliferations High CSD: Lentiginous Nevi and Lentigo Maligna Melanoma and Simulant(s) • Lentiginous Melanoma of Sun-Damaged Skin • LMM in situ • LMM invasive • Distinction from Dysplastic Nevi (Dysplastic Nevus-like Melanoma/Nevoid Lentigo Maligna • Lentiginous Nevi of -

Differential Diagnosis in Dermatology
Differential Diagnosis in Dermatology ZohrehTehranchi Dermatologist COMMON ACNE AND CYSTIC ACNE Rosacea Rosacea PERIORAL DERMATITIS ECZEMA/DERMATITIS Chronic irritant dermatitis Dyshidrotic eczematous dermatitis Childood atopic dermatitis Autosensitization dermatitis (“id” reaction): dermatophytid Seborrheic dermatitis PSORIASIS VULGARIS Pemphigus vulgaris BULLOUS PEMPHIGOID (BP) Pityriasis rosea small-plaque parapsoriasis Large-plaque parapsoriasis (parapsoriasis en plaques) LICHEN PLANUS (LP) GRANULOMA ANNULARE (GA) Erythema multiforme ERYTHEMA NODOSUM Actinic keratoses Bowen disease (Squamous cell carcinoma in situ) Bowen disease and invasive SCC Squamous cell carcinoma: invasive on the lip Squamous cell carcinoma, well differentiated Squamous cell carcinoma, undifferentiated Squamous cell carcinoma, advanced, well differentiated, on the hand Keratoacanthoma showing different stages of evolution BASAL CELL CARCINOMA (BCC) Basal cell carcinoma, ulcerated: Rodent ulcer A large rodent ulcer in the nuchal and Bas cell calarcinoma: sclerosing type retroauricular area extending to the temple Basal cell carcinoma, sclerosing, nodular, Superficial basal cell carcinoma: solitary lesion and multiple lesions Superficial basal cell carcinoma, invasive Basal cell carcinoma, pigmented Dysplastic nevi Superficial spreading melanoma: arising within a dysplastic nevus Congenital nevomelanocytic nevus Melanoma: arising in small CNMN Melanoma in situ: lentigo maligna Melanoma in situ, superficial spreading type Superficial spreading melanoma, vertical -

Joseph Butterfield, MD Mayo Clinic Melody Carter, MD National Institutes of Health 90 80 70 T
Joseph Butterfield, MD Mayo Clinic Melody Carter, MD National Institutes of Health Percent 50 60 70 80 90 10 20 30 40 0 Clinical o Historical • Mast cell-mediator symptoms • Less atopic disease than general population o Cutaneous • Permanent pigmented lesions with a general distribution or diffuse thickening “peau d’ orange” appearance o Other organ systems-mainly systemic disease Laboratory o Tryptase-reflects overall mast cell burden • May trend down over time and elevates with mast cell activation o Urinary metabolites-correlates with serum tryptase o Hematologic-Usually WNL; may see lymphs, PT/PTT, Plts Sonographic-Hepatosplenomegaly with systemic disease, rare lymphadenopathy Most Likely Diffuse or localized hyper-pigmented macules o Café au lait spots o Neurofibromatosis o Albright syndrome Bullous Lesions o Chronic bullous disease of childhood o Linear IgA dermatosis Solitary or multiple nodules o Congenital nevus o Juvenile Xanthogranuloma Consider No lesions o Idiopathic flushing Diffuse or localized hyper-pigmented macules o Post-inflammatory hyperpigmentation o Secondary syphilis o Chronic urticaria o Atopic dermatitis Bullous Lesions o Staphylococcus infection o Drug eruption o Incontinentia pigmenti o Bullous pemphigoid Solitary or multiple nodules Always Rule Out No lesions o Identifiable causes of anaphylaxis o Idiopathic anaphylaxis Diffuse or localized hyper-pigmented macules or papules o Secondary Syphilis o Addison’s disease o Lentigo Bullous Lesions o Bullous impetigo of infancy o Incongenta pigmenta Solitary or multiple nodules o Leukemia o Lymphoma Hypertensive spells Symptoms that improve with medications not targeting mast cell mediators or their effects: Ex: medications for anxiety or depression Seizure activity; incontinence (Delayed) problems with memory Dementia Arthritic complaints involving small joints or involving muscles.