Differential Diagnosis in Dermatology
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Dermatology DDX Deck, 2Nd Edition 65
63. Herpes simplex (cold sores, fever blisters) PREMALIGNANT AND MALIGNANT NON- 64. Varicella (chicken pox) MELANOMA SKIN TUMORS Dermatology DDX Deck, 2nd Edition 65. Herpes zoster (shingles) 126. Basal cell carcinoma 66. Hand, foot, and mouth disease 127. Actinic keratosis TOPICAL THERAPY 128. Squamous cell carcinoma 1. Basic principles of treatment FUNGAL INFECTIONS 129. Bowen disease 2. Topical corticosteroids 67. Candidiasis (moniliasis) 130. Leukoplakia 68. Candidal balanitis 131. Cutaneous T-cell lymphoma ECZEMA 69. Candidiasis (diaper dermatitis) 132. Paget disease of the breast 3. Acute eczematous inflammation 70. Candidiasis of large skin folds (candidal 133. Extramammary Paget disease 4. Rhus dermatitis (poison ivy, poison oak, intertrigo) 134. Cutaneous metastasis poison sumac) 71. Tinea versicolor 5. Subacute eczematous inflammation 72. Tinea of the nails NEVI AND MALIGNANT MELANOMA 6. Chronic eczematous inflammation 73. Angular cheilitis 135. Nevi, melanocytic nevi, moles 7. Lichen simplex chronicus 74. Cutaneous fungal infections (tinea) 136. Atypical mole syndrome (dysplastic nevus 8. Hand eczema 75. Tinea of the foot syndrome) 9. Asteatotic eczema 76. Tinea of the groin 137. Malignant melanoma, lentigo maligna 10. Chapped, fissured feet 77. Tinea of the body 138. Melanoma mimics 11. Allergic contact dermatitis 78. Tinea of the hand 139. Congenital melanocytic nevi 12. Irritant contact dermatitis 79. Tinea incognito 13. Fingertip eczema 80. Tinea of the scalp VASCULAR TUMORS AND MALFORMATIONS 14. Keratolysis exfoliativa 81. Tinea of the beard 140. Hemangiomas of infancy 15. Nummular eczema 141. Vascular malformations 16. Pompholyx EXANTHEMS AND DRUG REACTIONS 142. Cherry angioma 17. Prurigo nodularis 82. Non-specific viral rash 143. Angiokeratoma 18. Stasis dermatitis 83. -

Skin Diseases in Wrestling
Skin conditions in wrestling – how to prevent Krisztián Gáspár, MD, PhD Assistant professor University of Debrecen Faculty of Medicine Department of Dermatology Debrecen, Hungary Disclosure • Presenter: Krisztián Gáspár • I have the Relationships with commercial interests: – Advisory Board/Speakers Bureau: none – Funding (Grants/Honoraria): none – Research/Clinical Trials: Eli Lilly, Novartis, Pfizer, Janssen, Sanofi, Abbvie – Speaker/Consulting Fees: Eli Lilly, Novartis, Janssen, Sanofi, Abbvie • None to disclose regarding this presentation Objectives • Normal and impaired skin barrier • Atopic dermatitis – model for understanding barrier • Skin diseases in wrestling • Treatments • Prevention techniques in skin infections Skin barrier Danger model: ”The basic function of immune system is not to distinct between self and non-self, but to recognize danger” Polly Matzinger, PhD, Immunologist, NIH In order to avoid or prevent a loss on the mat you need a good defense – The same is true for skin (an active defense) Skin barrier functions Physicochemical barrier and immunological barrier – in close morphological and functional connection Physicochemical barrier Immunological barrier (SIS) Stratum corneum: corneocytes • Epidermis, dermis Stratum granulosum: keratinocytes • Keratinocytes, dendritic cells, T cells Cornified envelop , structural proteins • Defensins, cytokines, chemokines (filaggrin) Lipid layer, proteases, protease inhibitors, defensins Tight junctions, corneodesmosomes Physicochemical barrier Genetics Environmental factors -

Vesicular and Ulcerative Dermatopathy Resembling Superficial Necrolytic Dermatitis in Captive Black Rhinoceroses (Diceros Bicornis)
Vet Path01 353 1-42 (1998) Vesicular and Ulcerative Dermatopathy Resembling Superficial Necrolytic Dermatitis in Captive Black Rhinoceroses (Diceros bicornis) L. MUNSON, J. W. KOEHLER, J. E. WILKINSON, AND R. E. MILLER Department of Pathology, College of Veterinary Medicine, University of Tennessee,Knoxville, TN (LM, JWK, JEW); and Department of Animal Health, St. Louis Zoological Park, St. Louis, MO (REM) Abstract. The histopathology, clinical presentation, and epidemiology of a cutaneous and oral mucosal disease affecting 40 black rhinoceroses (Diceros bicomis) at 21 zoological parks (50% of the captive US population) were investigated. Twenty-seven biopsies were examined from recent lesions, and clinical infor- mation was available from 127 episodes.The cutaneous lesions began as plaques that progressedto vesicles, bullae, or ulcers. Lesions waxed and waned in individual cases.Lesions were predominantly bilaterally sym- metrical, affecting pressurepoints, coronary bands, tips of the ears and tail, and along the lateral body wall and dorsum. Oral lesions were first noticed as ulcers and were present on the lateral margins of the tongue, palate, and mucocutaneousjunctions of the lips. All recent lesions had similar histopathologic findings of prominent acanthosis,hydropic degenerationof keratinocytes in the stratum spinosum,spongiosis, intraepithelial vesicles, and parakeratosiswithout dermal inflammation. Chronic lesions were ulcerated. No pathogens were identified by culture or electron microscopy. Most episodescoincided with stressevents -
Diagnostic Pitfall of Localized Lentigo Accompanied by Post-Inflammatory
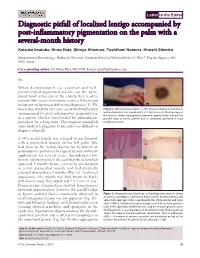
Letter to the Editor Diagnostic pitfall of localized lentigo accompanied by post-inflammatory pigmentation on the palm with a several-month history Keisuke Imafuku, Hiroo Hata, Shinya Kitamura, Toshifumi Nomura, Hiroshi Shimizu Department of Dermatology, Hokkaido University Graduate School of MedicineNorth 15, West 7, Kita-ku, Sapporo 060- 8638, Japan Corresponding author: Dr. Hiroo Hata, MD, PhD, E-mail: [email protected] Sir, When dermatologists see acquired and well- circumscribed pigmented macules on the palm, dorsal hand or forearm of the elderly, they tend to consider blue nevus, hematoma, nevus cell nevus and malignant melanoma as differential diagnoses [1]. We a b herein described the very rare case of localized lentigo Figure 1: Clinical manifestations. a. The macule is brown to dark black, accompanied by post-inflammatory pigmentation well-demarcated, flat, round and 3 x 4 mm in size. b. Dermoscopy of the macule shows homogenous brownish pigmentation without the in a patient who has been treated for palmoplanter parallel ridge or furrow pattern that is commonly observed in acral pustulosis for a long time. This eruption mimicked lentiginous lesion some kinds of lentiginous lesion and it was difficult to diagnose clinically. A 59-year-old female was referred to our hospital with a pigmented macule on her left palm. She had been to the family doctor for treatment of palmoplanter pustulosis by topical steroid ointment application for several years. According to the a history-taking interview, she said that the lesion had b appeared 5 months before referral to our hospital as a tiny pigmented macule and had gradually enlarged during those 5 months (Fig. -

Dyshidrotic Eczema
University of Calgary PRISM: University of Calgary's Digital Repository Cumming School of Medicine Cumming School of Medicine Research & Publications 2014-09-16 Dyshidrotic eczema Leung, Alexander K.C.; Barankin, Benjamin; Hon, Kam Lun Enliven Archive Leung AK, Barankin B, Hon KL (2014) Dyshidrotic Eczema. Enliven: Pediatr Neonatol Biol 1(1): 002. http://hdl.handle.net/1880/50267 journal article Downloaded from PRISM: https://prism.ucalgary.ca Research Article www.enlivenarchive.org Enliven: Pediatrics and Neonatal Biology Dyshidrotic Eczema Alexander K. C. Leung1*, Benjamin Barankin2, and Kam Lun Hon3 1Clinical Professor of Pediatrics, University of Calgary, Pediatric Consultant, Alberta Children’s Hospital 2Medical Director and Founder, Toronto Dermatology Centre 3Professor of Pediatrics, Chinese University of Hong Kong * Corresponding author: Alexander K. C. Leung, MBBS, FRCPC, FRCP Citation: Leung AK, Barankin B, Hon KL (2014) Dyshidrotic Eczema. (UK & Irel), FRCPCH, FAAP, Clinical Professor of Pediatrics, University Enliven: Pediatr Neonatol Biol 1(1): 002. of Calgary, Pediatric Consultant, Alberta Children’s Hospital, Canada, Tel: Copyright:@ 2014 Dr. Alexander K. C. Leung. This is an Open Access (403) 230-3322; Fax: (403) 230-3322; E-mail: [email protected] article published and distributed under the terms of the Creative Commons th Received Date: 14 August 2014 Attribution License, which permits unrestricted use, distribution and th Accepted Date: 10 September 2014 reproduction in any medium, provided the original author and source are th Published Date: 16 September 2014 credited. Abstract Dyshidrotic eczema, also known as dyshidrotic dermatitis or pompholyx, is characterized by pruritic, tense, deep-seated vesicles mainly on the palms and lateral surfaces of the fingers. -

PLENARY SESSION ABSTRACTS Theme: IMMUNITY and AUTOIMMUNITY
PLENARY SESSION ABSTRACTS Theme: IMMUNITY AND AUTOIMMUNITY State-of-the-Art Address Supporting Review What’s new in autoimmune blistering diseases? Epithelial, immune cell and microbial cross- D. F. MURRELL talk in homeostasis and atopic dermatitis Department of Dermatology, St George Hospital, and T. KOBAYASHI UNSW Faculty of Medicine, Sydney, New South Wales, Laboratory for Innate Immune Systems, RIKEN Center Australia for Integrative Medical Sciences (IMS), Yokohama, There are several blistering diseases which occur natu- Japan rally in other species as well as in humans; for example, Skin is a complex and dynamic ecosystem, wherein the pemphigus occurs naturally in dogs and horses and the epithelial cells, immune cells and microbiota engage in inherited blistering disease, epidermolysis bullosa, also active dialogues and maintain barrier integrity and occurs in dogs. Several new validated scoring systems functional immunity. Alterations of the peaceful coexis- to measure the severity of autoimmune blistering dis- tence with the resident microbiota, referred to as dys- ease (AIBD) have been developed which assist in biosis, lead to dysregulation of host immunity. It has demonstrating efficacy of new treatments, such as the been long debated whether the dysbiosis in the skin of Pemphigus Disease Area Index (PDAI) for pemphigus atopic dermatitis is merely a consequence of chronic and Bullous Pemphigoid Disease Area Index (BPDAI) skin inflammation or whether it is actively involved in for pemphigoid. Pemphigus is due to autoantibodies to driving skin inflammation. Microbiome analysis by 16S desmogleins 1 and 3 in human pemphigus foliaceus and rRNA sequencing in humans and dogs with atopic der- vulgaris and desmocollin1 in canine pemphigus foli- matitis showed the shifts in microbial diversity repre- aceus, generated by the late onset activation of the sented by increased proportion of Staphylococcus spp. -

Hutchinson's Melanotic Freckle
Hutchiso’s elaotic freckle Also known as Lentigo maligna What is lentigo maligna? Lentigo maligna is an early form of melanoma. In lentigo maligna the cancer cells are confined to the upper layer of the skin (epidermis). When the cancer cells spread deeper into the skin (to dermis) it is called lentigo maligna melanoma. Lentigo maligna occurs most commonly in sun damaged areas such as the face and neck in fair skinned people over the age of 60. The lesion grows slowly in size over a number of years. Melanoma is a potentially lethal disease and lentigo maligna should be diagnosed and excised as soon as possible. What causes lentigo maligna? The cause of lentigo maligna is sun exposure or solarium use. Factors that predispose a person to developing lentigo maligna or associated condition include: . chronic sun damaged/solar-induced skin damage . fair skin complexion . male gender . a personal history of non melanoma skin cancer and precancerous lesions . older individuals (those between 60 to 80 years are most commonly affected) What does lentigo maligna look like? Lentigo maligna commonly looks like a freckle, age spot, sun spot or brown patch that slowly changes shape and grows in size. The spot may be large in size, irregularly shaped with a smooth surface, and of multiple shades of brown and sometimes other colours. Thickening of part of the lesion, increasing number of colours, ulceration or bleeding can be markers that the lesion is changing into a lentigo maligna melanoma. How is lentigo maligna diagnosed? Lentigo maligna is diagnosed clinically by a dermatologist, sometimes with the help of a dermatoscope (a tool used to magnify and look closely at skin moles). -

Pigmented Contact Dermatitis and Chemical Depigmentation
18_319_334* 05.11.2005 10:30 Uhr Seite 319 Chapter 18 Pigmented Contact Dermatitis 18 and Chemical Depigmentation Hideo Nakayama Contents ca, often occurs without showing any positive mani- 18.1 Hyperpigmentation Associated festations of dermatitis such as marked erythema, with Contact Dermatitis . 319 vesiculation, swelling, papules, rough skin or scaling. 18.1.1 Classification . 319 Therefore, patients may complain only of a pigmen- 18.1.2 Pigmented Contact Dermatitis . 320 tary disorder, even though the disease is entirely the 18.1.2.1 History and Causative Agents . 320 result of allergic contact dermatitis. Hyperpigmenta- 18.1.2.2 Differential Diagnosis . 323 tion caused by incontinentia pigmenti histologica 18.1.2.3 Prevention and Treatment . 323 has often been called a lichenoid reaction, since the 18.1.3 Pigmented Cosmetic Dermatitis . 324 presence of basal liquefaction degeneration, the ac- 18.1.3.1 Signs . 324 cumulation of melanin pigment, and the mononucle- 18.1.3.2 Causative Allergens . 325 ar cell infiltrate in the upper dermis are very similar 18.1.3.3 Treatment . 326 to the histopathological manifestations of lichen pla- 18.1.4 Purpuric Dermatitis . 328 nus. However, compared with typical lichen planus, 18.1.5 “Dirty Neck” of Atopic Eczema . 329 hyperkeratosis is usually milder, hypergranulosis 18.2 Depigmentation from Contact and saw-tooth-shape acanthosis are lacking, hyaline with Chemicals . 330 bodies are hardly seen, and the band-like massive in- 18.2.1 Mechanism of Leukoderma filtration with lymphocytes and histiocytes is lack- due to Chemicals . 330 ing. 18.2.2 Contact Leukoderma Caused Mainly by Contact Sensitization . -

Tinea Capitis 2014 L.C
BJD GUIDELINES British Journal of Dermatology British Association of Dermatologists’ guidelines for the management of tinea capitis 2014 L.C. Fuller,1 R.C. Barton,2 M.F. Mohd Mustapa,3 L.E. Proudfoot,4 S.P. Punjabi5 and E.M. Higgins6 1Department of Dermatology, Chelsea & Westminster Hospital, Fulham Road, London SW10 9NH, U.K. 2Department of Microbiology, Leeds General Infirmary, Leeds LS1 3EX, U.K. 3British Association of Dermatologists, Willan House, 4 Fitzroy Square, London W1T 5HQ, U.K. 4St John’s Institute of Dermatology, Guy’s and St Thomas’ NHS Foundation Trust, St Thomas’ Hospital, Westminster Bridge Road, London SE1 7EH, U.K. 5Department of Dermatology, Hammersmith Hospital, 150 Du Cane Road, London W12 0HS, U.K. 6Department of Dermatology, King’s College Hospital, Denmark Hill, London SE5 9RS, U.K. 1.0 Purpose and scope Correspondence Claire Fuller. The overall objective of this guideline is to provide up-to- E-mail: [email protected] date, evidence-based recommendations for the management of tinea capitis. This document aims to update and expand Accepted for publication on the previous guidelines by (i) offering an appraisal of 8 June 2014 all relevant literature since January 1999, focusing on any key developments; (ii) addressing important, practical clini- Funding sources cal questions relating to the primary guideline objective, i.e. None. accurate diagnosis and identification of cases; suitable treat- ment to minimize duration of disease, discomfort and scar- Conflicts of interest ring; and limiting spread among other members of the L.C.F. has received sponsorship to attend conferences from Almirall, Janssen and LEO Pharma (nonspecific); has acted as a consultant for Alliance Pharma (nonspe- community; (iii) providing guideline recommendations and, cific); and has legal representation for L’Oreal U.K. -

A Retrospective Study of Idiopathic Ulcerative Dermatitis in Mice with a C57BL/6 Background
Journal of the American Association for Laboratory Animal Science Vol 45, No 6 Copyright 2006 November 2006 by the American Association for Laboratory Animal Science Pages 8-12 Reports A Retrospective Study of Idiopathic Ulcerative Dermatitis in Mice with a C57BL/6 Background Robin J Kastenmayer,* Michele A Fain, and Kathy A Perdue Idiopathic ulcerative dermatitis is a well-recognized disease in C57BL mice and related strains. This disease manifests as a pruritic dermatitis with resulting self-mutilation, dermal ulceration, necrosis, and fibrosis. Ulcerative dermatitis has the ability to confound ongoing research by causing systemic pathologic changes, such as lymphadenopathy and splenomegaly. Although various treatments have been described, none has been curative consistently; therefore, minimizing negative effects on research through prevention of disease is ideal. To identify etiologic factors, we conducted a 2-y retrospective study of 1352 mice with a C57BL/6 genetic background; these mice demonstrated an overall prevalence of 4.1% and a seasonal effect with a peak incidence during midsummer. Corroborating previous studies, our study revealed a disease predilection for female mice. In contrast to prior reports, the disease prevalence was greatest in 10- to 16-mo-old mice. In addition, mice with a C57BL/6 background that were deficient in the gene for inducible nitric oxide synthase had a 50% disease incidence, suggesting a potential animal model for further characterizing the pathogenesis, prevention, and treatment of ulcerative dermatitis. Abbreviations: iNOS, inducible nitric oxide synthase; UD, ulcerative dermatitis Idiopathic ulcerative dermatitis (UD) with pruritus is a Allentown, NJ) with corncob bedding (Harlan Teklad, Madison, common condition in C57BL mice, especially C57BL/6J mice. -

Allergic Contact Dermatitis Handout
#30: ALLERGIC CONTACT DERMATITIS PATIENT PERSPECTIVES Allergic contact dermatitis Contact dermatitis is an itchy rash that is caused by something touching (contacting) your skin. The rash is usually red, bumpy, and itchy. Sometimes there are blisters filled with fluid. THERE ARE TWO TYPES OF CONTACT DERMATITIS: COMMON FORMS OF ALLERGIC CONTACT DERMATITIS: 1. Some things that contact skin are very irritating and will cause a rash in most people. This rash is called irritant contact dermatitis. Examples are acids, soaps, cold weather, and friction. » ALLERGIC CONTACT DERMATITIS TO HOMEMADE SLIME 2. Some things that touch your skin give you a rash because you are allergic to them. This rash is called allergic contact dermatitis. » Slime is a homemade gooey These are items that do not bother everyone’s skin. They only substance that many young people cause a rash in people who are allergic to those items. make and play with. » There are several recipes for making WHAT ARE COMMON CAUSES OF ALLERGIC slime. Common ingredients include CONTACT DERMATITIS IN CHILDREN AND boric acid, contact lens solution, WHERE ARE THEY FOUND? laundry detergent, shaving cream, and school glue. Many ingredients » Homemade slime: often irritation (irritant contact dermatitis) being used can cause irritation results from soap or detergent but can have allergic contact (“irritant contact dermatitis”) and some dermatitis to glues and other ingredients can cause allergic contact dermatitis. » Plants: poison ivy, poison oak, poison sumac » Children playing with slime may get » Metals (especially nickel): snaps, jewelry, an itchy rash on their hands. There belt buckles, electronics, toys can be blisters, flaking, peeling, and cracking. -

Infectious ID Reaction Case Report
EMERGENCY MEDICINE ISSN 2379-4046 http://dx.doi.org/10.17140/EMOJ-3-133 Open Journal Case Report Infectious ID Reaction *Corresponding author Larry B. Mellick, MD 1 1 2* Department of Emergency Medicine CPT. Katherine D. Percy, DO ; Lt. Col. Massimo D. Federico, MD ; Larry B. Mellick, MD Augusta University Health Sciences Campus 1 AF-1020, 1120 15th Street Department of Emergency Medicine, Carl R. Darnall Army Medical Center, 36000 Darnall Augusta, Georgia 30912, USA Loop, Fort Hood, TX 76544, USA E-mail: [email protected] 2Department of Emergency Medicine, Augusta University, Health Sciences Campus, AF-1020, 1120 15th Street, Augusta, Georgia 30912, USA Volume 3 : Issue 1 Article Ref. #: 1000EMOJ3133 CHIEF COMPLAINT Article History Redness and swelling to left leg. Received: December 9th, 2016 Accepted: February 16th, 2017 HISTORY OF PRESENT ILLNESS Published: February 17th, 2017 An otherwise healthy 7-year-old male presented to the emergency department complaining of a pruritic, red rash with that had increased in area over 7 days. The rash reportedly began Citation as a localized lesion on his left lower extremity and developed a secondary diffuse rash over Percy KD, Federico MD, Mellick LB. In- the trunk and upper extremities after the initial ED encounter. During the initial emergency fectious ID reaction. Emerg Med Open department visit he was prescribed diphenhydramine and topical hydrocortisone with minimal J. 2017; 3(1): 14-15. doi: 10.17140/ relief. He denied any known environmental or allergen exposures or asthma history suggesting EMOJ-3-133 atopic dermatitis, or new exposures to medications. The patient and his parent also denied fever, lymphadenopathy, or any respiratory signs and symptoms.