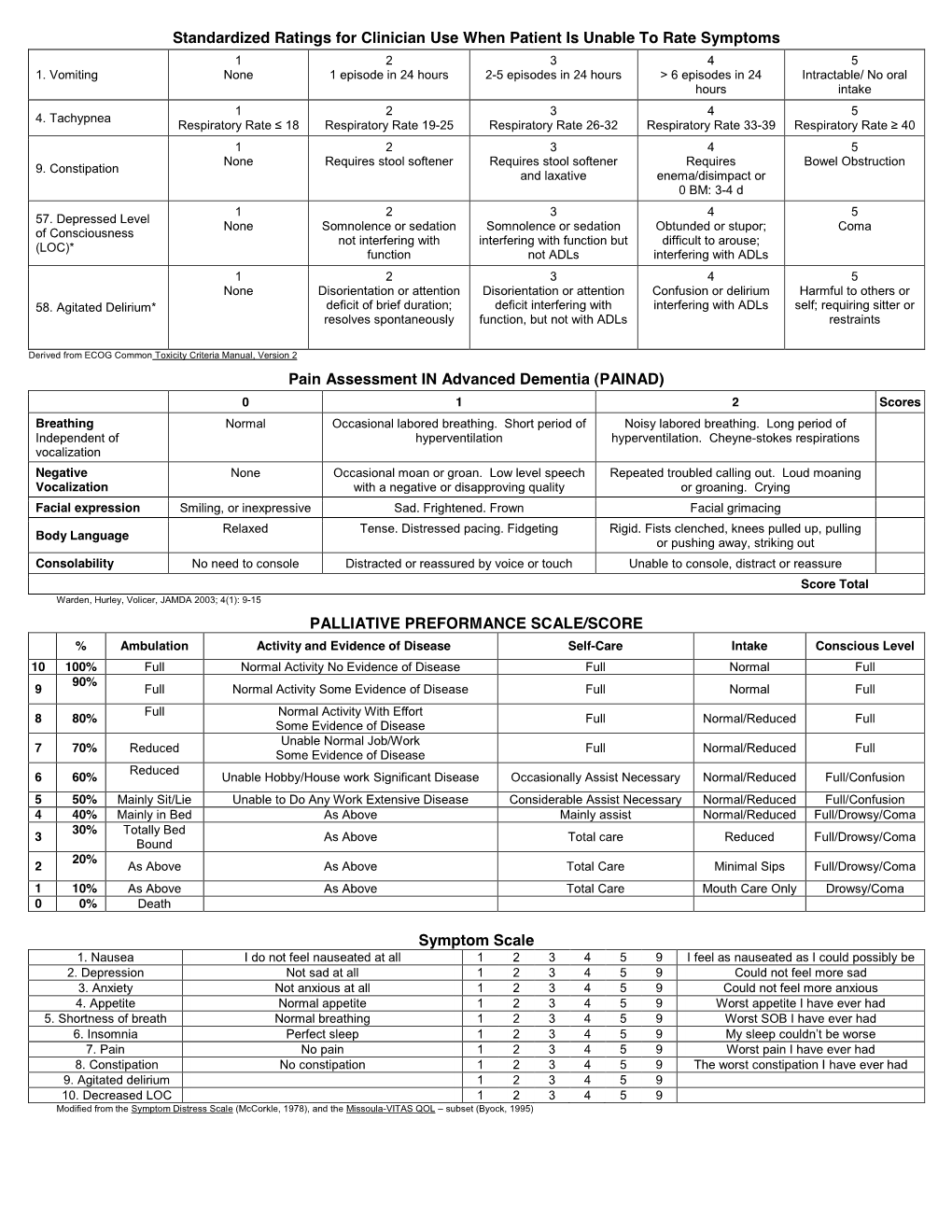
Standardized Ratings for Clinician Use When Patient Is Unable to Rate Symptoms 1 2 3 4 5 1
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Acute Stress Disorder
Trauma and Stress-Related Disorders: Developments for ICD-11 Andreas Maercker, MD PhD Professor of Psychopathology, University of Zurich and materials prepared and provided by Geoffrey Reed, PhD, WHO Department of Mental Health and Substance Abuse Connuing Medical Educaon Commercial Disclosure Requirement • I, Andreas Maercker, have the following commercial relaonships to disclose: – Aardorf Private Psychiatric Hospital, Switzerland, advisory board – Springer, book royales Members of the Working Group • Christopher Brewin (UK) Organizational representatives • Richard Bryant (AU) • Mark van Ommeren (WHO) • Marylene Cloitre (US) • Augusto E. Llosa (Médecins Sans Frontières) • Asma Humayun (PA) • Renato Olivero Souza (ICRC) • Lynne Myfanwy Jones (UK/KE) • Inka Weissbecker (Intern. Medical Corps) • Ashraf Kagee (ZA) • Andreas Maercker (chair) (CH) • Cecile Rousseau (CA) WHO scientists and consultant • Dayanandan Somasundaram (LK) • Geoffrey Reed • Yuriko Suzuki (JP) • Mark van Ommeren • Simon Wessely (UK) • Michael B. First WHO Constuencies 1. Member Countries – Required to report health stascs to WHO according to ICD – ICD categories used as basis for eligibility and payment of health care, social, and disability benefits and services 2. Health Workers – Mulple mental health professions – ICD must be useful for front-line providers of care in idenfying and treang mental disorders 3. Service Users – ‘Nothing about us without us!’ – Must provide opportunies for substanve, early, and connuing input ICD Revision Orienting Principles 1. Highest goal is to help WHO member countries reduce disease burden of mental and behavioural disorders: relevance of ICD to public health 2. Focus on clinical utility: facilitate identification and treatment by global front-line health workers 3. Must be undertaken in collaboration with stakeholders: countries, health professionals, service users/consumers and families 4. -

ICD-11 Diagnostic Guidelines Stress Disorders 2020 07 21
Pre-Publication Draft; not for citation or distribution 1 ICD-11 DIAGNOSTIC GUIDELINES Disorders Specifically Associated with Stress Note: This document contains a pre-publication version of the ICD-11 diagnostic guidelines for Disorders Specifically Associated with Stress. There may be further edits to these guidelines prior to their publication. Table of Contents DISORDERS SPECIFICALLY ASSOCIATED WITH STRESS ...................................... 2 6B40 Post-Traumatic Stress Disorder ............................................................................ 3 6B41 Complex Post-Traumatic Stress Disorder ............................................................. 8 6B42 Prolonged Grief Disorder .................................................................................... 12 6B43 Adjustment Disorder ........................................................................................... 15 6B44 Reactive Attachment Disorder ............................................................................ 17 6B45 Disinhibited Social Engagement Disorder .......................................................... 20 6B4Y Other Specified Disorders Specifically Associated with Stress ......................... 22 QE84 Acute Stress Reaction ......................................................................................... 23 © WHO Department of Mental Health and Substance Abuse 2020 Pre-Publication Draft; not for citation or distribution 2 DISORDERS SPECIFICALLY ASSOCIATED WITH STRESS Disorders Specifically Associated with Stress -

Recovery from Disorders of Consciousness: Mechanisms, Prognosis and Emerging Therapies
REVIEWS Recovery from disorders of consciousness: mechanisms, prognosis and emerging therapies Brian L. Edlow 1,2, Jan Claassen3, Nicholas D. Schiff4 and David M. Greer 5 ✉ Abstract | Substantial progress has been made over the past two decades in detecting, predicting and promoting recovery of consciousness in patients with disorders of consciousness (DoC) caused by severe brain injuries. Advanced neuroimaging and electrophysiological techniques have revealed new insights into the biological mechanisms underlying recovery of consciousness and have enabled the identification of preserved brain networks in patients who seem unresponsive, thus raising hope for more accurate diagnosis and prognosis. Emerging evidence suggests that covert consciousness, or cognitive motor dissociation (CMD), is present in up to 15–20% of patients with DoC and that detection of CMD in the intensive care unit can predict functional recovery at 1 year post injury. Although fundamental questions remain about which patients with DoC have the potential for recovery, novel pharmacological and electrophysiological therapies have shown the potential to reactivate injured neural networks and promote re-emergence of consciousness. In this Review, we focus on mechanisms of recovery from DoC in the acute and subacute-to-chronic stages, and we discuss recent progress in detecting and predicting recovery of consciousness. We also describe the developments in pharmacological and electro- physiological therapies that are creating new opportunities to improve the lives of patients with DoC. Disorders of consciousness (DoC) are characterized In this Review, we discuss mechanisms of recovery by alterations in arousal and/or awareness, and com- from DoC and prognostication of outcome, as well as 1Center for Neurotechnology mon causes of DoC include cardiac arrest, traumatic emerging treatments for patients along the entire tempo- and Neurorecovery, brain injury (TBI), intracerebral haemorrhage and ral continuum of DoC. -

Current Clinical Approach to Patients with Disorders of Consciousness
CURRENTREVIEW CLINICAL APPROA CARTICLEH TO PATIENTS WITH DISORDERS OF CONSCIOUSNESS Current clinical approach to patients with disorders of consciousness ROBSON LUIS OLIVEIRA DE AMORIM1, MARCIA MITIE NAGUMO2*, WELLINGSON SILVA PAIVA3, ALMIR FERREIRA DE ANDRADE3, MANOEL JACOBSEN TEIXEIRA4 1PhD – Assistant Physician of the Neurosurgical Emergency Unit, Division of Neurosurgery, Hospital das Clínicas, Faculdade de Medicina, Universidade de São Paulo (FMUSP), São Paulo, SP, Brazil 2Nurse – MSc Student at the Neurosurgical Emergency Unit, Division of Neurosurgery, Hospital das Clínicas, FMUSP, São Paulo, SP, Brazil 3Habilitation (BR: Livre-docência) – Professor of the Neurosurgical Emergency Unit, Division of Neurosurgery, Hospital das Clínicas, FMUSP, São Paulo, SP, Brazil 4Habilitation (BR: Livre-docência) – Full Professor of the Division of Neurosurgery, Hospital das Clínicas, FMUSP, São Paulo, SP, Brazil SUMMARY Study conducted at Hospital das Clínicas, In clinical practice, hospital admission of patients with altered level of conscious- Faculdade de Medicina, Universidade de ness, sleepy or in a non-responsive state is extremely common. This clinical con- São Paulo (FMUSP), São Paulo, SP, Brazil dition requires an effective investigation and early treatment. Performing a fo- Article received: 1/28/2015 cused and objective evaluation is critical, with quality history taking and Accepted for publication: 5/4/2015 physical examination capable to locate the lesion and define conducts. Imaging *Correspondence: and laboratory exams have played an increasingly important role in supporting Address: Av. Dr. Enéas de Carvalho Aguiar, 255, Cerqueira César clinical research. In this review, the main types of changes in consciousness are São Paulo, SP – Brazil discussed as well as the essential points that should be evaluated in the clinical Postal code: 05403-000 [email protected] management of these patients. -

Syncope: Overview and Approach to Management
SMAC01 01/21/2005 09:57 AM Page 1 1 CHAPTER 1 Syncope: Overview and approach to management Brian Olshansky, MD “near-syncope”), falling episodes, and coma are Introduction often confused with, and inappropriately labeled Syncope is a common, important medical problem as, “true” syncope. Distinction between sleeping, caused by many conditions, ranging from benign confusion, intoxication, and fainting may not be and self-limiting to chronic, recurrent, and poten- completely clear. To make matters more difficult, tially fatal causes. Unfortunately, differentiation an elderly patient, already confused, may fall and between benign and malignant causes can be diffi- pass out with only vague recall of the event. Such a cult and challenging. Even with knowledge of com- patient may even think he or she passed out when mon syndromes and conditions that cause syncope, nothing of the sort occurred. This diverse collec- and guidelines [1], an effective approach to the tion of clinical presentations perplexes the patient problem requires careful integration of clues pro- and the physician. Episodes can be difficult to define vided in the history and physical examination com- even with careful observation, and the mechanism bined with keen clinical acumen. Management of may be confusing even with extensive monitoring. this baffling problem can be frustrating, confusing, True syncope is an abrupt but transient loss of and often unrewarding. Treatment can be imposs- consciousness associated with absence of postural ible to prescribe without a clear understanding of tone followed by rapid, usually complete, recovery the cause, and treatments may be directed to risk as without the need for intervention to stop the epis- well as symptom reduction. -

Acute Stress Reaction Medical Appendix
ACUTE STRESS REACTION MEDICAL APPENDIX (including acute stress disorder, shell shock, combat fatigue) 1. Various attempts have been made to formally classify psychiatric disorders, the two major systems being: 1.1. The ICD-10 Classification of Mental and Behavioural Disorders (World Health Organisation, Geneva) is part of the 10th edition of the International Classification of Disease. This appendix follows the common abbreviation of ICD-10. It is the international system used by the majority of clinical psychiatrists in Great Britain. 1.2. The Diagnostic and Statistical Manual of Mental Disorders (fourth edition) (American Psychiatric Association Washington DC). References to it in this appendix follow the common abbreviation of DSM-IV. It is a system devised mainly by and for workers in the USA. However UK psychiatrists were consulted in its formulation. 2. The two systems above have been in existence for many years but only in their current editions have they been closely comparable. 3. This appendix discusses the clinical features and aetiology of acute stress reaction. It is generally based on the ICD-10 system with any major comparisons and distinctions with DSM-IV being discussed where relevant. The ICD-10 codes (numbers usually prefixed with F or Z) are also provided. REACTIONS TO STRESSFUL EXPERIENCES: THE NORMAL RESPONSE 4. Most people react to stress with an emotional or somatic (physical) response. These are normal reactions and do not constitute mental disorders in themselves, although some people seek help from their doctor. What is interpreted as being stressful will vary from one individual to another and the ways in which they respond vary similarly. -

Catatonia Rating Scales in Patients with Persistent Vegetative State
Original Article Catatonia Rating Scales in Patients with Persistent Vegetative State Chin-Chuen Lin, M.D.1§, Hsiang-Lan Chen, R.N.2§, Cheng-Hsien Lu, M.D., M.Sc.3, Tiao-Lai Huang, M.D.1* Departments of 1Psychiatry and 3Neurology, Kaohsiung Chang Gung Memorial Hospital and Chang Gung University College of Medicine, 2Department of Nursing, Kaohsiung Municipal Feng-Shan Hospital, Kaohsiung, Taiwan §Contributed equally as two first authors Abstract Objective: Persistent vegetative state (PVS) has similar clinical presentations with catatonia. Both PVS and catatonia can be evaluated using clinical observation and rating scales. We intended to study how catatonia rating scales perform in assessing PVS patients as compared to the standard PVS scale. Methods: Thirty residents from two nursing homes for PVS patients were evaluated with Coma Recovery Scale-Revised (CRS-R) and two catatonia rating scales (Bush–Francis Catatonia Rating Scale [BFCRS] and KANNER scale). Ten residents recovering from PVS were selected as controls, and twenty residents still meeting the criteria of PVS were selected as PVS group. Three evaluations were assessed over 6 months. We compared and analyzed the scores of each visit. The components of BFCRS and KANNER scales were also analyzed to create a simpler version for PVS patients. Results: BFCRS and KANNER scales, as well as their simplified versions, had significant correlations with CRS-R (p < 0.001 for all). This could imply that catatonia rating scales could also be used in evaluating PVS patients. Upon closer examinations of scale components, all the three scales shared components such as consciousness levels and eye movements, but BFCRS and KANNER have evaluations on rigidity and negativism, which CRS-R does not had. -

Catatonia in Major Depressive Disorder: Diagnostic Dilemma
Journal of Psychology and Clinical Psychiatry Case Report Open Access Catatonia in major depressive disorder: diagnostic dilemma. A case report Abstract Volume 10 Issue 5 - 2019 Catatonia is a complex neuropsychiatric syndrome that is often associated with psychiatric, 1 2 neurological and/or medical conditions. In order to make a diagnosis of catatonia, the Chiedozie Ojimba, Ehinor E Isidahome, clinical picture must be dominated by three or more of the following symptoms; cataplexy, Nkolika Odenigbo,1 Osaretin D Umudi,1 waxy flexibility, stupor, agitation, mutism, negativism, posturing, mannerisms, stereotypies, Olaniyi Olayinka,1 grimacing, echolalia, and echopraxia. We present a case of a 58-year-old female with no 1Department of Psychiatry, Interfaith Medical Center, USA prior psychiatric history who presented to the psychiatric emergency room with a three- 2Department of Public Health, Texas A&M School of Public week history of feeling depressed, anhedonic, hopeless, helpless, and worthless, associated Health, USA with poor sleep, poor concentration, low energy, significant weight loss due to lack of appetite, and suicidal ideations after she saw her ex-boyfriend holding hands with another Correspondence: Chiedozie Ojimba, Department of woman. Patient exhibited symptoms such as mutism, hyperextension of spine, clinching Psychiatry, Interfaith Medical Center, 1545 Atlantic Avenue of jaw, psychomotor retardation which suggested probable diagnosis of catatonia at the Brooklyn, New York 11213, USA, Tel 1-718-613-4334, Fax 1-718- 228-7907 or 718-613-4370, background of major depressive disorder nonresponding to treatment. This case report Email demonstrates the need for a high index of suspicion and early screening for catatonia in psychiatric patients given the high morbidity and mortality that is associated with this Received: September 18, 2019 | Published: September 25, condition if delayed or undiagnosed. -

The ICD-10 Classification of Mental and Behavioural Disorders
The ICD-10 Classification of Mental and Behavioural Disorders Clinical descriptions and diagnostic guidelines World Health Organization -1- Preface In the early 1960s, the Mental Health Programme of the World Health Organization (WHO) became actively engaged in a programme aiming to improve the diagnosis and classification of mental disorders. At that time, WHO convened a series of meetings to review knowledge, actively involving representatives of different disciplines, various schools of thought in psychiatry, and all parts of the world in the programme. It stimulated and conducted research on criteria for classification and for reliability of diagnosis, and produced and promulgated procedures for joint rating of videotaped interviews and other useful research methods. Numerous proposals to improve the classification of mental disorders resulted from the extensive consultation process, and these were used in drafting the Eighth Revision of the International Classification of Diseases (ICD-8). A glossary defining each category of mental disorder in ICD-8 was also developed. The programme activities also resulted in the establishment of a network of individuals and centres who continued to work on issues related to the improvement of psychiatric classification (1, 2). The 1970s saw further growth of interest in improving psychiatric classification worldwide. Expansion of international contacts, the undertaking of several international collaborative studies, and the availability of new treatments all contributed to this trend. Several national psychiatric bodies encouraged the development of specific criteria for classification in order to improve diagnostic reliability. In particular, the American Psychiatric Association developed and promulgated its Third Revision of the Diagnostic and Statistical Manual, which incorporated operational criteria into its classification system. -

Unconsciousness - First Aid: Medlineplus Medical Encyclopedia
Unconsciousness - first aid: MedlinePlus Medical Encyclopedia U.S. National Library of Medicine GO About MedlinePlus Site Map FAQs Customer Support Health Topics Drugs & Supplements Videos & Tools Espaol Home → Medical Encyclopedia → Unconsciousness - first aid Unconsciousness - first aid Unconsciousness is when a person is unable to respond to people and activities. Doctors often call this a coma or being in a comatose state. Other changes in awareness can occur without becoming unconscious. These are called altered mental status or changed mental status. They include sudden confusion, disorientation, or stupor. Unconsciousness or any other sudden change in mental status must be treated as a medical emergency. Causes Unconsciousness can be caused by nearly any major illness or injury. It can also be caused by substance (drug) and alcohol use. Choking on an object can result in unconsciousness as well. Brief unconsciousness (or fainting) is often a result from dehydration, low blood sugar, or temporary low blood pressure. It can also be caused by serious heart or nervous system problems. A doctor will determine if the affected person needs tests. Other causes of fainting include straining during a bowel movement (vasovagal syncope), coughing very hard, or breathing very fast (hyperventilating). Symptoms The person will be unresponsive (does not respond to activity, touch, sound, or other stimulation). The following symptoms may occur after a person has been unconscious: Amnesia for (not remembering) events before, during, and even after -

Altered Level of Consciousness (Aloc) & Syncope
SCHOOL HEALTH SERVICES STANDARD PROCEDURES: ALOC & SYNCOPE ALTERED LEVEL OF CONSCIOUSNESS (ALOC) & SYNCOPE (FAINTING) ALOC Altered level of consciousness (ALOC) is a state of consciousness where an individual is not as awake, alert, or able to understand or react normally. ALOC can be caused by a head injury, medicines, alcohol or drugs, dehydration, or some diseases, such as diabetes. There are different levels of ALOC, which include: Lethargic: unusual drowsiness with reduced awareness or interest in surroundings Somnolent: sleeping unless awakened by someone or something and returns to sleep when left alone Stupor: sleeping unless awakened by something done that is painful and returns to sleep when left alone Coma: look asleep but can’t be awakened at all Confusion: easily distracted and may be slow to respond, disoriented and not able to tell time and place Delirium: severe confusion and disorientation and may have delusions (belief in things that are not real) or hallucinations (sensing things that are not real). The degree of confusion may get better or worse over time. Presentation of any of these symptoms in the school setting warrants a call to EMS/9-1-1, nurse and parents immediately. Syncope Syncope (fainting) is a transient loss of consciousness accompanied by loss of postural tone due to inadequate blood supply to the brain. This loss of consciousness is usually brief. Fainting may have no medical significance, or the cause can be a serious disorder. Therefore, treat loss of consciousness as a medical emergency until the signs and symptoms are relieved and the cause is known. Typical vasovagal syncope occurs in a person in upright position with appropriate stimulus (e.g., fear or pain). -

Altered States of Consciousness Jeffrey R
Altered States of Consciousness Jeffrey R. Avner Pediatrics in Review 2006;27;331 DOI: 10.1542/pir.27-9-331 The online version of this article, along with updated information and services, is located on the World Wide Web at: http://pedsinreview.aappublications.org/content/27/9/331 Pediatrics in Review is the official journal of the American Academy of Pediatrics. A monthly publication, it has been published continuously since 1979. Pediatrics in Review is owned, published, and trademarked by the American Academy of Pediatrics, 141 Northwest Point Boulevard, Elk Grove Village, Illinois, 60007. Copyright © 2006 by the American Academy of Pediatrics. All rights reserved. Print ISSN: 0191-9601. Downloaded from http://pedsinreview.aappublications.org/ by Rachel Boykan on November 9, 2011 Article neurology Altered States of Consciousness Jeffrey R. Avner, MD* Objectives After completing this article, readers should be able to: 1. List the common causes of altered level of consciousness. Author Disclosure 2. Discuss how to differentiate medical and structural causes of altered level of Dr Avner did not consciousness. disclose any financial 3. Develop a plan for the initial phase of evaluation for an altered level of consciousness. relationships relevant 4. Recognize the importance of radiologic imaging in a child who has an altered level of to this article. consciousness. 5. Know which ingestions are likely to cause neurologic adverse effects. Definition During the course of normal interaction with one another, we observe each other’s mannerisms, responses, movements, and communications. In a sense, a person’s behavior is determined by how he or she acts or reacts to internal and external stimuli.