Liver Changes Associated with Cholecystitis
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

Print This Article
International Surgery Journal Lew D et al. Int Surg J. 2021 May;8(5):1575-1578 http://www.ijsurgery.com pISSN 2349-3305 | eISSN 2349-2902 DOI: https://dx.doi.org/10.18203/2349-2902.isj20211831 Case Report Acute gangrenous appendicitis and acute gangrenous cholecystitis in a pregnant patient, a difficult diagnosis: a case report David Lew, Jane Tian*, Martine A. Louis, Darshak Shah Department of Surgery, Flushing Hospital Medical Center, Flushing, New York, USA Received: 26 February 2021 Accepted: 02 April 2021 *Correspondence: Dr. Jane Tian, E-mail: [email protected] Copyright: © the author(s), publisher and licensee Medip Academy. This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License, which permits unrestricted non-commercial use, distribution, and reproduction in any medium, provided the original work is properly cited. ABSTRACT Abdominal pain is a common complaint in pregnancy, especially given the physiological and anatomical changes that occur as the pregnancy progresses. The diagnosis and treatment of common surgical pathologies can therefore be difficult and limited by the special considerations for the fetus. While uncommon in the general population, concurrent or subsequent disease processes should be considered in the pregnant patient. We present the case of a 36 year old, 13 weeks pregnant female who presented with both acute appendicitis and acute cholecystitis. Keywords: Appendicitis, Cholecystitis, Pregnancy, Pregnant INTRODUCTION population is rare.5 Here we report a case of concurrent appendicitis and cholecystitis in a pregnant woman. General surgeons are often called to evaluate patients with abdominal pain. The differential diagnosis list must CASE REPORT be expanded in pregnant woman and the approach to diagnosing and treating certain diseases must also be A 36 year old, 13 weeks pregnant female (G2P1001) adjusted to prevent harm to the fetus. -

A Drug-Induced Cholestatic Pattern
Review articles Hepatotoxicity: A Drug-Induced Cholestatic Pattern Laura Morales M.,1 Natalia Vélez L.,1 Octavio Germán Muñoz M., MD.2 1 Medical Student in the Faculty of Medicine and Abstract the Gastrohepatology Group at the Universidad de Antioquia in Medellín, Colombia Although drug induced liver disease is a rare condition, it explains 40% to 50% of all cases of acute liver 2 Internist and Hepatologist at the Hospital Pablo failure. In 20% to 40% of the cases, the pattern is cholestatic and is caused by inhibition of the transporters Tobon Uribe and in the Gastrohepatology Group at that regulate bile synthesis. This reduction in activity is directly or indirectly mediated by drugs and their me- the Universidad de Antioquia in Medellín, Colombia tabolites and/or by genetic polymorphisms and other risk factors of the patient. Its manifestations range from ......................................... biochemical alterations in the absence of symptoms to acute liver failure and chronic liver damage. Received: 30-01-15 Although there is no absolute test or marker for diagnosis of this disease, scales and algorithms have Accepted: 26-01-16 been developed to assess the likelihood of cholestatic drug induced liver disease. Other types of evidence are not routinely used because of their complexity and cost. Diagnosis is primarily based on exclusion using circumstantial evidence. Cholestatic drug induced liver disease has better overall survival rates than other patters, but there are higher risks of developing chronic liver disease. In most cases, the patient’s condition improves when the drug responsible for the damage is removed. Hemodialysis and transplantation should be considered only for selected cases. -

April Is IBS Awareness Month
4/19/2021 Irritable Bowel Syndrome (IBS) in Women: Today’s approach Kathryn Hutchins, MD Assistant Professor University of Nebraska Medical Center Division of Gastroenterology & Hepatology Irritable Bowel Syndrome • No disclosures April is IBS awareness month Objectives Define Irritable Bowel Syndrome (IBS) including its subtypes Describe the current criteria and diagnostic approach for IBS Discuss the management approach to IBS 1 4/19/2021 Clinical Scenarios • 18 y/o female reports longstanding history of GI troubles. She comes to clinic because she is having bouts of diarrhea. Diarrhea is most often when she is nervous or stressed. Diarrhea is more common in the days prior to having her period. Imodium helps to slow the diarrhea • 38 y/o female reports bloating and discomfort most days and especially after eating. She reports having a bowel movement once every 3‐4 days and typically stools are small balls. Bowel movements alleviate bloating. When she travels, she is especially miserable with constipation and bloating. • 41 y/o female with 2 year history of RUQ abdominal pain and frequent loose stools. Gallbladder removed years earlier for different symptoms. Evaluation has included EGD, colonoscopy, endoscopic ultrasound, ERCP x 2 with stent placement and subsequent removal. Countless appointment with evaluations in 3 different states. Irritable Bowel Syndrome defined • IBS is one of the functional gastrointestinal disorders (FGID). Functional bowel disorders (FBD) are FGID of the lower GI tract. • The FGID are also referred to disorder of the brain –gut interaction (DBGI). • IBS is a common of disorders of the brain –gut axis • Chronic symptoms of abdominal pain, bloating, diarrhea, and constipation • No identified structural or lab abnormality to account for recurring symptoms*** Gastroenterology 2020;158:1262–1273 Disorders of the Brain –Gut Interaction Functional Gastrointestinal Disorders Functional Bowel Disorders 2 4/19/2021 How common and who does it affect Clinical visits • 12% of primary care visits. -

A Rare Hepatic Manifestation of Systemic Lupus Erythematosus
Cholestatic hepatitis in SLE Cholestatichepatitis:ararehepaticmanifestationof systemiclupuserythematosus WHChow,MSLam,WKKwan,WFNg Systemic lupus erythematosus is a multi-system inflammatory disease. The clinical manifestations are diverse. Hepatic manifestation is a rarely seen complication of systemic lupus erythematosus. We report a case of complication of systemic lupus erythematosus presenting as cholestatic hepatitis in a 56-year- old Chinese woman. The cholestatic hepatitis progressed as part of the lupus activity and responded to steroid therapy. HKMJ 1997;3:331-4 Key words: Hepatitis; Cholestasis; Lupus erythematosus, systemic; Liver Introduction of body weight and had had a poor appetite. She was a non-drinker and had no long term drug history. Systemic lupus erythematosus (SLE) is a multi- system inflammatory disease associated with the A general examination showed her to be jaundiced, development of auto-antibodies to a variety of self- pale, and dyspnoeic with an elevated body tempera- antigens. The clinical manifestations of SLE are ture of 38.2°C. Chest examination demonstrated coarse diverse. In 1982, the American Rheumatism Associa- crackles heard over both lung fields. Other parts of tion (ARA) published revised criteria for the classifi- the examination were unremarkable. There was 2+ cation of SLE.1 For a diagnosis of SLE, individuals proteinuria in the mid-stream urine but the culture should have four or more of the following features: for organisms was negative. Investigations revealed a malar rash, discoid rash, photosensitivity, oral ulcers, normochromic, normocytic anaemia (haemoglobin 9.4 non-erosive arthritis, pleuritis or pericarditis, renal g/dL [normal range, 11.5-15.5 g/dL]) with normal disorder, seizures or psychosis, haematological white cell and differential counts. -

Clinical Management of Gastroesophageal Reflux Disease
Osteopathic Family Physician (2011) 3, 58-65 Clinical management of gastroesophageal reflux disease Renata Jarosz, DO,a Thomas G. Zimmerman, DO, FACOFP,b Daniel Van Arsdale, DOc From aStanford Hospital Physical Medicine and Rehabilitation Residency Program, Redwood City, CA, bSouth Nassau Family Medicine, Oceanside, NY, and cSouthampton Hospital, Southampton, NY. KEYWORDS: Gastroesophageal reflux disease (GERD) is a common problem that occurs in both adult and pediatric Gastroesophageal; populations and can significantly degrade patients’ quality of life and lead to life-threatening complications. Reflux; A prudent course of management in a patient with classic GERD symptoms would be to empirically Disease; prescribe lifestyle modifications and a proton pump inhibitor (PPI) for six to eight weeks. Osteopathic GERD; manipulative treatment may also be a useful adjunct. If the patient is unable to afford a PPI, a histamine Current; type-2 receptor antagonist may be substituted (although they are much less effective). If resolution of Treatment; symptoms occurs, the therapeutic response can confirm the diagnosis of uncomplicated GERD. If the patient Diagnosis; has recurrent or intractable symptoms, the next step would be to order pH monitoring, manometry, or Management; endoscopic evaluation of the esophagus and stomach (esophagogastroduodenoscopy [EGD]). If there are Osteopathic; any atypical symptoms such as persistent cough, asthma, melena, sore throat, or hoarse voice, EGD should Manipulative; be ordered immediately. Patients with chronic esophagitis or extra-esophageal symptoms who have failed Treatment; (or refused) medical management should consider fundoplication. OMT; © 2011 Elsevier Inc. All rights reserved. Barrett; Medical; Medications Gastroesophageal reflux disease (GERD) is a common evaluate and manage GERD. Table 1 outlines some key points problem that occurs in both adult and pediatric populations in of information for readers to consider. -

Primary Biliary Cholangitis: a Brief Overview Justin S
REVIEW Primary Biliary Cholangitis: A Brief Overview Justin S. Louie,* Sirisha Grandhe,* Karen Matsukuma,† and Christopher L. Bowlus* Primary biliary cholangitis (PBC), previously referred to supported by the higher concordance of PBC in monozy- as primary biliary cirrhosis, is the most common chronic gotic compared with dizygotic twins.4 In addition, certain cholestatic autoimmune disease affecting adults in the human leukocyte antigen haplotypes have been associ- United States.1 It is characterized by a hallmark serologic ated with PBC, as well as variants at loci along the inter- signature, antimitochondrial antibody (AMA), and specific leukin-12 (IL-12) immunoregulatory pathway (IL-12A and bile duct pathology with progressive intrahepatic duct de- IL-12RB2 loci).5 struction leading to cholestasis. PBC is potentially fatal and can have both intrahepatic and extrahepatic complications. PATHOGENESIS EPIDEMIOLOGY The primary disease mechanism in PBC is thought to be T cell lymphocyte–mediated injury against intralobu- PBC affects all races and ethnicities; however, it is best lar biliary epithelial cells. This causes progressive destruc- studied in the Caucasian population. The condition pre- tion and eventual disappearance of the intralobular bile dominantly affects women older than 40 years, with a ducts. Molecular mimicry has been proposed as the ini- female/male ratio of 9:1.2 Although the incidence of PBC tiating event in the loss of tolerance primarily to mito- appears to be stable, the overall prevalence of the disease chondrial pyruvate dehydrogenase complex, E2, during is increasing.3 An individual’s genetic susceptibility, epige- which exogenous antigens evoke an immune response netic factors, and certain environmental triggers seem to that recognizes an endogenous (self) antigen inciting an play important roles. -

Gallbladder Disease in the Aged Patient- a Comprehensive Diagnosis and Treatment Approach
Review Article Adv Res Gastroentero Hepatol Volume 8 Issue 1 - November 2017 Copyright © All rights are reserved by Zvi Perry DOI: 10.19080/ARGH.2017.08.555730 Gallbladder Disease in the Aged Patient- A Comprehensive Diagnosis and Treatment Approach Sharon Ziskind1, Uri Netz2, Udit Gibor2, ShaharAtias2, Leonid Lantsberg2 and Zvi H Perry1,2* 1Soroka University Medical Center, Israel 2Department of Epidemiology and Health Management, Ben-Gurion University of the Negev, Israel Submission: September 01, 2017; Published: November 22, 2017 *Corresponding author: Zvi Perry, MD, MA, Surgical Ward A, Soroka University Medical Center PO Box 151, Beer-Sheva 64101, Israel, Tel: +972-8-6400610; Fax: +972-8-6477633; Email: Abstract The improvements in life expectancy combined with aging of the baby boomer generation will result in a rapid increase in the population older than 65 years in the next few decades, and thus an increase in the need to take care of elderly patients. The authors of this chapter were born and raised in Israel, a country in which due to the holocaust and the fact it was a young nation, was not accustomed to elderly patients. But, in the last decade the percentage of patients older than 65 has crossed the 10% mark of the entire population and we were forced to learn elderly patients and the know how in treating them is not the same as the 30 years old patient. It is important to do so, because It is expected and to find ways to care and treat older patients. As the saying in pediatrics, that a child is not a small adult, the same rule applies seemingly to that by 2030 one in five people will be older than 65 years, with the most rapidly growing segment of this older population being persons older than 85. -

Gastroesophageal Reflux Disease
The new england journal of medicine clinical practice Gastroesophageal Reflux Disease Peter J. Kahrilas, M.D. This Journal feature begins with a case vignette highlighting a common clinical problem. Evidence supporting various strategies is then presented, followed by a review of formal guidelines, when they exist. The article ends with the author’s clinical recommendations. A 53-year-old man, who is otherwise healthy and has a 20-year history of occasional heartburn, reports having had worsening heartburn for the past 12 months, with daily symptoms that disturb his sleep. He reports having had no dysphagia, gastroin- testinal bleeding, or weight loss and in fact has recently gained 20 lb (9 kg). What would you advise regarding his evaluation and treatment? The Clinical Problem From the Division of Gastroenterology, Gastroesophageal reflux disease is the most common gastrointestinal diagnosis re- Feinberg School of Medicine, Chicago. Ad- corded during visits to outpatient clinics.1 In the United States, it is estimated that dress reprint requests to Dr. Kahrilas at the Feinberg School of Medicine, 676 St. Clair 14 to 20% of adults are affected, although such percentages are at best approxima- St., Suite 1400, Chicago, IL 60611-2951, tions, given that the disease has a nebulous definition and that such estimates are or at [email protected]. based on the prevalence of self-reported chronic heartburn.2 A current definition of N Engl J Med 2008;359:1700-7. the disorder is “a condition which develops when the ref lux of stomach contents causes Copyright © 2008 Massachusetts Medical Society. troublesome symptoms (i.e., at least two heartburn episodes per week) and/or complications.”3 Several extraesophageal manifestations of the disease are well rec- ognized, including laryngitis and cough (Table 1). -
Cholecystitis
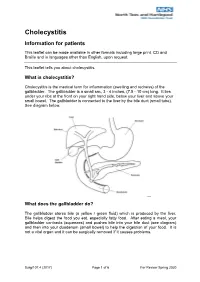
Cholecystitis Information for patients This leaflet can be made available in other formats including large print, CD and Braille and in languages other than English, upon request. This leaflet tells you about cholecystitis. What is cholecystitis? Cholecystitis is the medical term for inflammation (swelling and redness) of the gallbladder. The gallbladder is a small sac, 3 - 4 inches, (7.5 - 10 cm) long. It lies under your ribs at the front on your right hand side, below your liver and above your small bowel. The gallbladder is connected to the liver by the bile duct (small tube). See diagram below. What does the gallbladder do? The gallbladder stores bile (a yellow / green fluid) which is produced by the liver. Bile helps digest the food you eat, especially fatty food. After eating a meal, your gallbladder contracts (squeezes) and pushes bile into your bile duct (see diagram) and then into your duodenum (small bowel) to help the digestion of your food. It is not a vital organ and it can be surgically removed if it causes problems. Surg/107.4 (2017) Page 1 of 6 For Review Spring 2020 Cholecystitis What causes cholecystitis? Inflammation of the gallbladder is often caused when gallstones irritate the gallbladder and sometimes cause an infection. Gallstones are formed in the gallbladder or bile duct and develop when bile forms crystals. Over time these crystals become hardened and eventually grow into stones but they do not always cause problems. However, gallstones can cause: jaundice. If the stones move from your gallbladder and block your bile duct jaundice can occur. -

Progress Report Cholestasis and Lesions of the Biliary Tract in Chronic Pancreatitis
Gut: first published as 10.1136/gut.19.9.851 on 1 September 1978. Downloaded from Gut, 1978, 19, 851-857 Progress report Cholestasis and lesions of the biliary tract in chronic pancreatitis The occurrence of jaundice in the course of chronic pancreatitis has been recognised since the 19th century" 2. But in the early papers it is uncertain whether the cases were due to acute, acute relapsing, or to chronic pan- creatitis, or even to pancreatic cancer associated with pancreatitis or benign ampullary stenosis. With the introduction of endoscopic retrograde cholangiopancreato- graphy (ERCP), there has been a renewed interest in the biliary complica- tions of chronic pancreatitis (CP). However, papers published recently by endoscopists have generally neglected the cholangiographic aspect of the lesions and are less precise and less well documented than papers published just after the second world war, following the introduction of manometric cholangiography3-5. Furthermore, the description of obstructive jaundice due to chronic pancreatitis, classical 20 years ago, seems to have been forgotten until the recent papers. Radiological aspects of bile ducts in chronic pancreatitis http://gut.bmj.com/ If one limits the subject to primary diseases of the pancreas, particularly chronic calcifying pancreatitis (CCP)6, excluding chronic pancreatitis secondary to benign ampullary stenosis7, cancer obstructing the main pancreatic duct8 9 and acute relapsing pancreatitis secondary to gallstones'0 radiological aspect of the main bile duct" is type I the most.common on September 25, 2021 by guest. Protected copyright. choledocus (Figure). This description has been repeatedly confirmed'2"13. It is a long stenosis of the intra- or retropancreatic part of the main bile duct. -

The Spectrum of Gallbladder Disease
The Spectrum of Gallbladder Disease Rebecca Kowalski, M.D. October 18, 2017 Overview A (brief) history of gallbladder surgery Anatomy Anatomical variations Physiology Pathophysiology Diagnostic imaging of the gallbladder Natural history of cholelithiasis Case presentations of the spectrum of gallstone disease Summary History of Gallbladder Surgery Gallbladder Surgery: A Relatively Recent Change Prior to the late 1800s, doctors treated gallbladder disease with a cholecystostomy, due to the fear that removing the organ would kill patients Carl Johann August Langenbuch (director of the Lazarus Hospital in Berlin, Germany) practiced on a cadaver to remove the gallbladder, and in 1882, performed a cholecystectomy on a patient. He was discharged after 6 weeks in the hospital https://en.wikipedia.org/wiki/Carl_Langenbuch By 1897 over 100 cholecystectomies had been performed Gallbladder Surgery: A Relatively Recent Change In 1985, Erich Mühe removed a patient’s gallbladder laparoscopically in Germany Erich Muhe https://openi.nlm.ni h.gov/detailedresult. php?img=PMC30152 In 1987, Philippe Mouret (a 44_jsls-2-4-341- French gynecologic surgeon) g01&req=4 performed a laparoscopic cholecystectomy In 1992, the National Institutes of Health (NIH) created guidelines for laparoscopic cholecystectomy in the United Philippe Mouret States, essentially transforming https://www.pinterest.com surgical practice /pin/58195020154734720/ Anatomy and Abnormal Anatomy http://accesssurgery.mhmedical.com/content.aspx?bookid=1202§ionid=71521210 http://www.slideshare.net/pryce27/rsna-final-2 http://www.slideshare.net/pryce27/rsna-final-2 http://www.slideshare.net/pryce27/rsna-final-2 Physiology a http://www.nature.com/nrm/journal/v2/n9/fig_tab/nrm0901_657a_F3.html Simplified overview of the bile acid biosynthesis pathway derived from cholesterol Lisa D. -

An Update on the Management of Cholestatic Liver Diseases
Clinical Medicine 2020 Vol 20, No 5: 513–6 CME: HEPATOLOGY An update on the management of cholestatic liver diseases Authors: Gautham AppannaA and Yiannis KallisB Cholestatic liver diseases are a challenging spectrum of autoantibodies though may be performed in cases of diagnostic conditions arising from damage to bile ducts, leading to doubt, suspected overlap syndrome or co-existent liver pathology build-up of bile acids and inflammatory processes that cause such as fatty liver. injury to cholangiocytes and hepatocytes. Primary biliary cholangitis (PBC) and primary sclerosing cholangitis (PSC) are ABSTRACT the two most common cholestatic disorders. In this review we Key points detail the latest guidelines for the diagnosis and management of patients with these two conditions. Ursodeoxycholic acid can favourably alter the natural history of primary biliary cholangitis in a majority of patients, given at the appropriate dose of 13–15 mg/kg/day. Primary biliary cholangitis Primary biliary cholangitis (PBC) is a chronic autoimmune liver Risk stratification is of paramount importance in the disorder characterised by immune-mediated destruction of management of primary biliary cholangitis to identify epithelial cells lining the intrahepatic bile ducts, resulting in patients with suboptimal response to ursodeoxycholic acid persistent cholestasis and, in some patients, a progression to and poorer long-term prognosis. Alkaline phosphatase cirrhosis if left untreated. The exact mechanisms remain unclear >1.67 times the upper limit of normal and a bilirubin above but are most likely a result of exposure to environmental factors in the normal range indicate high-risk disease and suboptimal a genetically susceptible individual.1 The majority of patients are treatment response.