Rehabilitation of Proximal Humerus & Clavicular Fractures
Total Page:16
File Type:pdf, Size:1020Kb

Load more
Recommended publications
-

Body Mechanics As the Rotator Cuff Gether in a Cuff-Shape Across the Greater and Lesser Tubercles the on Head of the Humerus
EXPerT CONTENT Body Mechanics by Joseph E. Muscolino | Artwork Giovanni Rimasti | Photography Yanik Chauvin Rotator Cuff Injury www.amtamassage.org/mtj WORKING WITH CLieNTS AFFecTED BY THIS COmmON CONDITION ROTATOR CUFF GROUP as the rotator cuff group because their distal tendons blend and attach to- The four rotator cuff muscles are gether in a cuff-shape across the greater and lesser tubercles on the head of the supraspinatus, infraspinatus, the humerus. Although all four rotator cuff muscles have specific concen- teres minor, and subscapularis (Fig- tric mover actions at the glenohumeral (GH) joint, their primary functional ure 1). These muscles are described importance is to contract isometrically for GH joint stabilization. Because 17 Before practicing any new modality or technique, check with your state’s or province’s massage therapy regulatory authority to ensure that it is within the defined scope of practice for massage therapy. the rotator cuff group has both mover and stabilization roles, it is extremely functionally active and therefore often physically stressed and injured. In fact, after neck and low back conditions, the shoulder is the most com- Supraspinatus monly injured joint of the human body. ROTATOR CUFF PATHOLOGY The three most common types of rotator cuff pathology are tendinitis, tendinosus, and tearing. Excessive physi- cal stress placed on the rotator cuff tendon can cause ir- ritation and inflammation of the tendon, in other words, tendinitis. If the physical stress is chronic, the inflam- matory process often subsides and degeneration of the fascial tendinous tissue occurs; this is referred to as tendinosus. The degeneration of tendinosus results in weakness of the tendon’s structure, and with continued Teres minor physical stress, whether it is overuse microtrauma or a macrotrauma, a rotator cuff tendon tear might occur. -

Midshaft Clavicle Fracture
You have a Midshaft Clavicle Fracture This is a break to the middle of your collar bone. Healing: It normally takes 6-12 weeks to heal, but symptoms can continue for 3-6 months. Smoking will slow down your healing. We would advise that you stop smoking while your fracture heals. Talk to your GP or go to www.smokefree.nhs.uk for more information. Pain and Swelling: Your shoulder may be swollen and you will have some pain. Taking pain medication and using ice or cold packs will help. More information is on the next page. Wearing your sling: Use your sling for 3 weeks. You can take it off to wash, dress and do your exercises. It does not need to be worn at night. Exercise and activity: It is important to start gentle exercises straight away to prevent stiffness. You will find pictures and instructions for your exercises below. You should not do any heavy lifting or overhead movement for the first 6 weeks. Follow up: You will see a shoulder specialist 3 weeks after your injury. They may do another x-ray to check the position of your fracture. They will explain the next stage of your rehabilitation. If you have not received your appointment letter within 1 week, please contact us. Contact us: If you are concerned about your symptoms, are unable to follow this rehabilitation plan or notice pain other than at your shoulder, please contact the Virtual Fracture Clinic. Updated 9th June 2021 Caring for your injury: Weeks 1-3 Remember to use your sling for the first 3 weeks. -

Comparison of Four Different Internal Fixation Methods in the Treatment of Distal Clavicle Fractures
EXPERIMENTAL AND THERAPEUTIC MEDICINE 19: 451-458, 2020 Comparison of four different internal fixation methods in the treatment of distal clavicle fractures LIANG LI*, HONGXIAO WU*, PEICHAO JIANG, XIAOCHUAN HAN, SHIYUAN CHEN and XUEZHONG YU Department of Orthopaedics, Dongying People's Hospital, Dongying, Shandong 257091, P.R. China Received March 15, 2019; Accepted August 8, 2019 DOI: 10.3892/etm.2019.8233 Abstract. This study compared the clinical efficacy of four of shoulder pain, an increase in the range of motion of the internal fixation methods in the treatment of distal clavicle shoulder, and a reduction in complications, and thus, are pref- fractures, in an effort to guide appropriate selection and erable for the early functional recovery of limbs. application in the clinic. Eighty‑four patients with distal clav- icle‑comminuted fractures were treated with a distal clavicle Introduction anatomic plate (group A), clavicular hook plate (group B), double‑plate vertical fixation (group C), or T‑shaped steel Due to its subcutaneous location, clavicle is one of the bones plate internal fixation (group D). The Constant‑Murley scoring that are most frequently fractured in the upper body due to car system was used to evaluate the shoulder joint function. The accidents and sports trauma. The incidence of distal clavicle fracture healing time, VAS, and postoperative complications fractures accounts for 12‑21% of all clavicular fractures (1). were compared and analyzed among the four groups. According Distal clavicle fractures are typically attributed to a direct to the Constant‑Murley evaluation standard, the excellent and blow to the point of the shoulder or a fall on an outstretched good rates of the four groups were 94.4, 73.1, 95 and 80% hand. -

Bone Limb Upper
Shoulder Pectoral girdle (shoulder girdle) Scapula Acromioclavicular joint proximal end of Humerus Clavicle Sternoclavicular joint Bone: Upper limb - 1 Scapula Coracoid proc. 3 angles Superior Inferior Lateral 3 borders Lateral angle Medial Lateral Superior 2 surfaces 3 processes Posterior view: Acromion Right Scapula Spine Coracoid Bone: Upper limb - 2 Scapula 2 surfaces: Costal (Anterior), Posterior Posterior view: Costal (Anterior) view: Right Scapula Right Scapula Bone: Upper limb - 3 Scapula Glenoid cavity: Glenohumeral joint Lateral view: Infraglenoid tubercle Right Scapula Supraglenoid tubercle posterior anterior Bone: Upper limb - 4 Scapula Supraglenoid tubercle: long head of biceps Anterior view: brachii Right Scapula Bone: Upper limb - 5 Scapula Infraglenoid tubercle: long head of triceps brachii Anterior view: Right Scapula (with biceps brachii removed) Bone: Upper limb - 6 Posterior surface of Scapula, Right Acromion; Spine; Spinoglenoid notch Suprspinatous fossa, Infraspinatous fossa Bone: Upper limb - 7 Costal (Anterior) surface of Scapula, Right Subscapular fossa: Shallow concave surface for subscapularis Bone: Upper limb - 8 Superior border Coracoid process Suprascapular notch Suprascapular nerve Posterior view: Right Scapula Bone: Upper limb - 9 Acromial Clavicle end Sternal end S-shaped Acromial end: smaller, oval facet Sternal end: larger,quadrangular facet, with manubrium, 1st rib Conoid tubercle Trapezoid line Right Clavicle Bone: Upper limb - 10 Clavicle Conoid tubercle: inferior -
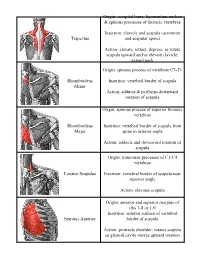
Trapezius Origin: Occipital Bone, Ligamentum Nuchae & Spinous Processes of Thoracic Vertebrae Insertion: Clavicle and Scapul
Origin: occipital bone, ligamentum nuchae & spinous processes of thoracic vertebrae Insertion: clavicle and scapula (acromion Trapezius and scapular spine) Action: elevate, retract, depress, or rotate scapula upward and/or elevate clavicle; extend neck Origin: spinous process of vertebrae C7-T1 Rhomboideus Insertion: vertebral border of scapula Minor Action: adducts & performs downward rotation of scapula Origin: spinous process of superior thoracic vertebrae Rhomboideus Insertion: vertebral border of scapula from Major spine to inferior angle Action: adducts and downward rotation of scapula Origin: transverse precesses of C1-C4 vertebrae Levator Scapulae Insertion: vertebral border of scapula near superior angle Action: elevates scapula Origin: anterior and superior margins of ribs 1-8 or 1-9 Insertion: anterior surface of vertebral Serratus Anterior border of scapula Action: protracts shoulder: rotates scapula so glenoid cavity moves upward rotation Origin: anterior surfaces and superior margins of ribs 3-5 Insertion: coracoid process of scapula Pectoralis Minor Action: depresses & protracts shoulder, rotates scapula (glenoid cavity rotates downward), elevates ribs Origin: supraspinous fossa of scapula Supraspinatus Insertion: greater tuberacle of humerus Action: abduction at the shoulder Origin: infraspinous fossa of scapula Infraspinatus Insertion: greater tubercle of humerus Action: lateral rotation at shoulder Origin: clavicle and scapula (acromion and adjacent scapular spine) Insertion: deltoid tuberosity of humerus Deltoid Action: -

Complications Associated with Clavicular Fracture
NOR200061.qxd 9/11/09 1:23 PM Page 217 Complications Associated With Clavicular Fracture George Mouzopoulos ▼ Emmanuil Morakis ▼ Michalis Stamatakos ▼ Mathaios Tzurbakis The objective of our literature review was to inform or- subclavian vein, due to its stable connection with the thopaedic nurses about the complications of clavicular frac- clavicle via the cervical fascia, can also be subjected to ture, which are easily misdiagnosed. For this purpose, we injuries (Casbas et al., 2005). Damage to the internal searched MEDLINE (1965–2005) using the key words clavicle, jugular vein, the suprascapular artery, the axillary, and fracture, and complications. Fractures of the clavicle are usu- carotid artery after a clavicular fracture has also been ally thought to be easily managed by symptomatic treatment reported (Katras et al., 2001). About 50% of injuries to the subclavian arteries are in a broad arm sling. However, it is well recognized that not due to fractures of the clavicle because the proximal all clavicular fractures have a good outcome. Displaced or part is dislocated superiorly by the sternocleidomas- comminuted clavicle fractures are associated with complica- toid, causing damage to the vessel (Sodhi, Arora, & tions such as subclavian vessels injury, hemopneumothorax, Khandelwal, 2007). If no injury happens during the ini- brachial plexus paresis, nonunion, malunion, posttraumatic tial displacement of the fractured part, then it is un- arthritis, refracture, and other complications related to os- likely to happen later, because the distal segment is dis- teosynthesis. Herein, we describe what the orthopaedic nurse placed downward and forward due to shoulder weight, should know about the complications of clavicular fractures. -

Evaluation of Humeral and Glenoid Bone Deformity in Glenohumeral Arthritis 5
Evaluation of Humeral and Glenoid Bone Deformity 1 in Glenohumeral Arthritis Brian F. Grogan and Charles M. Jobin Introduction glenoid bone wear helps the surgeon formulate a successful treatment plan and surgical goals Glenohumeral arthritis is the sequela of a vari- to address the pathoanatomy and improve the ety of pathologic shoulder processes, most durability of shoulder arthroplasty. The evalu- commonly degenerative osteoarthritis, but may ation of humeral and glenoid bone deformity also be secondary to post-traumatic conditions, in glenohumeral arthritis has profound surgical inflammatory arthritis, rotator cuff tear arthrop- implications and is fundamental to successful athy, and postsurgical conditions most com- shoulder arthroplasty. monly post-capsulorrhaphy arthritis. Patients with glenohumeral arthritis commonly demon- strate patterns of bony deformity on the glenoid Glenoid Deformity in Osteoarthritis and humerus that are caused by the etiology of the arthritis. For example, osteoarthritis com- Glenoid deformity and glenohumeral subluxation monly presents with posterior glenoid wear, are commonly seen in the setting of primary osteo- secondary glenoid retroversion, and posterior arthritis of the glenohumeral joint. The glenoid humeral head subluxation, while inflammatory wear tends to occur posteriorly and may be best arthritis routinely causes concentric glenoid viewed on axial radiographs or computed tomog- wear with central glenoid erosion. A thorough raphy (CT) axial images. Glenoid erosion, as first history and physical, as well as laboratory and characterized by Walch, is noted to be either central radiographic workup, are keys to understanding or posterior, with varying degrees of wear and pos- the etiology of arthritis and understanding the terior subluxation of the humerus [1, 2] (Fig. -

Avulsion Fracture of Brachioradialis Muscle Origin: an Exceedingly Rare Entity: a Case Report
10-039_OA1 8/13/16 5:34 PM Page 50 Malaysian Orthopaedic Journal 2016 Vol 10 No 2 Behera G, et al http://dx.doi.org/10.5704/MOJ.1607.010 Avulsion Fracture of Brachioradialis Muscle Origin: An Exceedingly Rare Entity: A Case Report Behera G, DNB, Balaji G, MS Ortho, Menon J, MRCS (Edin.), Sharma D, MCH, Komuravalli VK, DNB Jawaharlal Institute of Postgraduate Medical Education and Research (JIPMER), Puducherry, India Date of submission: March 2016 Date of acceptance: June 2016 ABSTRACT lateral supracondylar ridge just proximal to the lateral epicondyle. He had restriction of active terminal elbow Avulsion fracture of the brachioradialis origin at its proximal extension by 10 degrees with near normal active elbow attachment on the lateral supracondylar ridge of the distal flexion, pronation and supination. Active flexion and humerus is exceedingly rare, and only two cases have been extension at wrist were painful along with the painful reported in the literature so far. In this article, we present a terminal elbow extension. There was significant pain at the 38 years old patient who sustained a closed avulsion fracture lateral distal humerus when active elbow flexion against of the lateral supracondylar ridge of left humerus at the resistance was performed in the mid-pronated position of the proximal attachment of brachioradialis following a fall forearm. There was no distal neurovascular deficit. backwards on outstretched hand after being struck by a lorry from behind while riding on a two-wheeler (motorcycle). He Antero-posterior (AP) plain radiograph of the left elbow was managed with above elbow plaster for four weeks showed a fracture of the lateral distal humerus at the followed by elbow and wrist mobilization. -

Humerus Fracture
Portsmouth Hospitals NHS Trust Virtual Fracture Clinic Patient information Humerus Fracture Specialist Support This leaflet can be made available in another language, large print or another format. Please speak to the Virtual Fracture Clinic who can advise you Humerus VFC DCR leaflet 18 5871.indd 1 12/12/2018 09:42:15 This information leaflet follows up your recent conversation with the Fracture Clinic, where your case was reviewed by an orthopaedic Consultant (Bone specialist). You have sustained a fracture (break) to your Humerus (upper arm bone). The Virtual Fracture Clinic letter will detail where the fracture is. This is a very painful injury due to muscle spasms and the bone ends moving. Regular painkillers will be required during your healing stage to aid recovery. The treatment centre you attended will have provided you with a type of sling called a “collar and cuff”. This is the correct type of sling initially for this type of injury. This should be worn at all times. If you are worried that you are unable to follow this rehabilitation plan, or have any questions, then please contact us by using the contact numbers on the front of this leaflet. Healing: It takes approximately 12 weeks to heal. To fully resolve can take up to 1 year. Pain and This can be a painful injury. You are likely to swelling: experience significant swelling & bruising that can track down your chest, arm and into your hand. Take regular painkillers and ensure regular movement of fingers wrist and elbow. You may find it easier to sleep in an upright position. -

Medial Clavicle Fracture Dislocation Surgically Treated: Case Report Miguel Frias*, Renato Ramos, Marco Bernardes, Tiago Pinheiro Torres and Pedro Lourenço
ISSN: 2469-5777 Frias et al. Trauma Cases Rev 2018, 4:066 DOI: 10.23937/2469-5777/1510066 Volume 4 | Issue 2 Trauma Cases and Reviews Open Access CASE REPORT Medial Clavicle Fracture Dislocation Surgically Treated: Case Report Miguel Frias*, Renato Ramos, Marco Bernardes, Tiago Pinheiro Torres and Pedro Lourenço Centro Hospitalar de Vila Nova de Gaia/Espinho, Portugal *Corresponding author: Miguel Frias, Centro Hospitalar de Vila Nova de Gaia/Espinho, Porto, Portugal Check for updates injury to the trachea and esophagus and the possibility Abstract of pneumothorax [7]. The medial clavicle fracture is a rare injury and almost all the times conservatively treated. Therefore, the number of Although rare, such injuries require rapid diagnosis operations reported in the literature are limited. Posterior followed by effective treatment to avoid future dislocation can result in serious complications and such complications [8]. Specifically, periarticular and injuries require rapid diagnosis followed by effective treat- ment to avoid future complications. The present case re- intraarticular fractures remain a therapeutic challenge: ports a case of a 33-year-old healthy man that was involved The medial fragment is too small to stabilize with in a high-fall, being diagnosed with a rare displaced medi- common linear implants, and bending forces that occur al clavicular fracture associated with an unstable posterior during shoulder motion are disproportionately high lateral fragment dislocation surgically treated. Imagiological images and intraoperative photographs are presented. The [9]. Indications for surgery have traditionally included authors collected this case in order to report this rare and open fractures, soft-tissue damage, or neurovascular complex injury. -
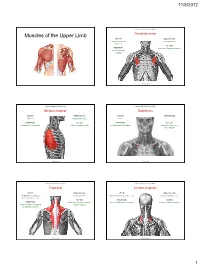
Muscles of the Upper Limb.Pdf
11/8/2012 Muscles Stabilizing Pectoral Girdle Muscles of the Upper Limb Pectoralis minor ORIGIN: INNERVATION: anterior surface of pectoral nerves ribs 3 – 5 ACTION: INSERTION: protracts / depresses scapula coracoid process (scapula) (Anterior view) Muscles Stabilizing Pectoral Girdle Muscles Stabilizing Pectoral Girdle Serratus anterior Subclavius ORIGIN: INNERVATION: ORIGIN: INNERVATION: ribs 1 - 8 long thoracic nerve rib 1 ---------------- INSERTION: ACTION: INSERTION: ACTION: medial border of scapula rotates scapula laterally inferior surface of scapula stabilizes / depresses pectoral girdle (Lateral view) (anterior view) Muscles Stabilizing Pectoral Girdle Muscles Stabilizing Pectoral Girdle Trapezius Levator scapulae ORIGIN: INNERVATION: ORIGIN: INNERVATION: occipital bone / spinous accessory nerve transverse processes of C1 – C4 dorsal scapular nerve processes of C7 – T12 ACTION: INSERTION: ACTION: INSERTION: stabilizes / elevates / retracts / upper medial border of scapula elevates / adducts scapula acromion / spine of scapula; rotates scapula lateral third of clavicle (Posterior view) (Posterior view) 1 11/8/2012 Muscles Stabilizing Pectoral Girdle Muscles Moving Arm Rhomboids Pectoralis major (major / minor) ORIGIN: INNERVATION: ORIGIN: INNERVATION: spinous processes of C7 – T5 dorsal scapular nerve sternum / clavicle / ribs 1 – 6 dorsal scapular nerve INSERTION: ACTION: INSERTION: ACTION: medial border of scapula adducts / rotates scapula intertubucular sulcus / greater tubercle flexes / medially rotates / (humerus) adducts -

Use of an Absorbable Plate in the Management of a Clavicle Fracture in an Adolescent
A Case Report & Literature Review Use of an Absorbable Plate in the Management of a Clavicle Fracture in an Adolescent Eric W. Edmonds, MD was successfully used to manage delayed union of a Abstract displaced and shortened clavicle fracture. The patient Management of clavicle fractures continues to evolve. provided written informed consent for print and elec- Indications for operative management seem to be tronic publication of this case report. expanding, particularly in athletic youth. Surgical inter- vention has potential complications, many associated ASE EPORT with use of metal implants. To my knowledge, this case C R report is the first to describe use of a biodegradable A right-handed, 17-year-old girl injured her left shoulder implant. The subcutaneous position of the clavicle makes and right wrist in a fall from a mountain bike. Initial it ideal for fixation with a biodegradable implant in which management at an outside emergency department con- no second surgery is required for implant removal. sisted of a simple sling for a left midshaft clavicle fracture (Figure 1) and a volar wrist splint for a right comminuted intra-articular distal radius fracture. One day later, the he shoulder, the most mobile joint in the body, patient received a univalved short arm cast with appro- is prone to instability and injury. Due to the priate molding and underwent computed tomography for subcutaneous and relatively anterior location, the intra-articular fracture. No tenting of the skin over and because its thin midshaft lacks muscular the clavicle was noted during this visit to our facility. Tand ligamentous support, the clavicle is a common injury Sixteen days after injury, the distal radius fracture site.