Chancroid Information for Health Care Professionals
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Parinaud's Oculoglandular Syndrome
Tropical Medicine and Infectious Disease Case Report Parinaud’s Oculoglandular Syndrome: A Case in an Adult with Flea-Borne Typhus and a Review M. Kevin Dixon 1, Christopher L. Dayton 2 and Gregory M. Anstead 3,4,* 1 Baylor Scott & White Clinic, 800 Scott & White Drive, College Station, TX 77845, USA; [email protected] 2 Division of Critical Care, Department of Medicine, University of Texas Health, San Antonio, 7703 Floyd Curl Drive, San Antonio, TX 78229, USA; [email protected] 3 Medical Service, South Texas Veterans Health Care System, San Antonio, TX 78229, USA 4 Division of Infectious Diseases, Department of Medicine, University of Texas Health, San Antonio, 7703 Floyd Curl Drive, San Antonio, TX 78229, USA * Correspondence: [email protected]; Tel.: +1-210-567-4666; Fax: +1-210-567-4670 Received: 7 June 2020; Accepted: 24 July 2020; Published: 29 July 2020 Abstract: Parinaud’s oculoglandular syndrome (POGS) is defined as unilateral granulomatous conjunctivitis and facial lymphadenopathy. The aims of the current study are to describe a case of POGS with uveitis due to flea-borne typhus (FBT) and to present a diagnostic and therapeutic approach to POGS. The patient, a 38-year old man, presented with persistent unilateral eye pain, fever, rash, preauricular and submandibular lymphadenopathy, and laboratory findings of FBT: hyponatremia, elevated transaminase and lactate dehydrogenase levels, thrombocytopenia, and hypoalbuminemia. His condition rapidly improved after starting doxycycline. Soon after hospitalization, he was diagnosed with uveitis, which responded to topical prednisolone. To derive a diagnostic and empiric therapeutic approach to POGS, we reviewed the cases of POGS from its various causes since 1976 to discern epidemiologic clues and determine successful diagnostic techniques and therapies; we found multiple cases due to cat scratch disease (CSD; due to Bartonella henselae) (twelve), tularemia (ten), sporotrichosis (three), Rickettsia conorii (three), R. -

Reportable Diseases and Conditions
KINGS COUNTY DEPARTMENT of PUBLIC HEALTH 330 CAMPUS DRIVE, HANFORD, CA 93230 REPORTABLE DISEASES AND CONDITIONS Title 17, California Code of Regulations, §2500, requires that known or suspected cases of any of the diseases or conditions listed below are to be reported to the local health jurisdiction within the specified time frame: REPORT IMMEDIATELY BY PHONE During Business Hours: (559) 852-2579 After Hours: (559) 852-2720 for Immediate Reportable Disease and Conditions Anthrax Escherichia coli: Shiga Toxin producing (STEC), Rabies (Specify Human or Animal) Botulism (Specify Infant, Foodborne, Wound, Other) including E. coli O157:H7 Scrombroid Fish Poisoning Brucellosis, Human Flavivirus Infection of Undetermined Species Shiga Toxin (Detected in Feces) Cholera Foodborne Disease (2 or More Cases) Smallpox (Variola) Ciguatera Fish Poisoning Hemolytic Uremic Syndrome Tularemia, human Dengue Virus Infection Influenza, Novel Strains, Human Viral Hemorrhagic Fever (Crimean-Congo, Ebola, Diphtheria Measles (Rubeola) Lassa, and Marburg Viruses) Domonic Acid Poisoning (Amnesic Shellfish Meningococcal Infections Yellow Fever Poisoning) Novel Virus Infection with Pandemic Potential Zika Virus Infection Paralytic Shellfish Poisoning Plague (Specify Human or Animal) Immediately report the occurrence of any unusual disease OR outbreaks of any disease. REPORT BY PHONE, FAX, MAIL WITHIN ONE (1) WORKING DAY Phone: (559) 852-2579 Fax: (559) 589-0482 Mail: 330 Campus Drive, Hanford 93230 Conditions may also be reported electronically via the California -

2012 Case Definitions Infectious Disease
Arizona Department of Health Services Case Definitions for Reportable Communicable Morbidities 2012 TABLE OF CONTENTS Definition of Terms Used in Case Classification .......................................................................................................... 6 Definition of Bi-national Case ............................................................................................................................................. 7 ------------------------------------------------------------------------------------------------------- ............................................... 7 AMEBIASIS ............................................................................................................................................................................. 8 ANTHRAX (β) ......................................................................................................................................................................... 9 ASEPTIC MENINGITIS (viral) ......................................................................................................................................... 11 BASIDIOBOLOMYCOSIS ................................................................................................................................................. 12 BOTULISM, FOODBORNE (β) ....................................................................................................................................... 13 BOTULISM, INFANT (β) ................................................................................................................................................... -

Sexually Transmitted Diseases/Infections Chancroid
Sexually Transmitted Diseases/Infections Chancroid Chancroid is a bacterial infection caused by Haemophilus ducreyi. It is spread by sexual contact and results in genital ulcers. Chancroid is a reportable genital ulcer condition that is rarely seen in North Carolina. When infection does occur, it is usually associated with sporadic outbreaks. Chancroid, as well as genital herpes and syphilis, is a risk factor in the transmission of HIV infection. Chancroid lesions may be difficult to distinguish from ulcers caused by genital herpes or syphilis. A physician must therefore diagnose the infection by excluding other diseases with similar symptoms. The combination of a painful genital ulcer and tender suppurative inguinal adenopathy suggests the diagnosis of chancroid. A probable diagnosis of chancroid, for both clinical and surveillance purposes, can be made if all of the following criteria are met: 1) the patient has one or more painful genital ulcers; 2) the patient has no evidence of T. pallidum infection by darkfield examination of ulcer exudate or by a serologic test for syphilis performed at least 7 days after onset of ulcers; 3) the clinical presentation, appearance of genital ulcers and, if present, regional lymphadenopathy are typical for chancroid; and 4) a test for HSV performed on the ulcer exudate is negative. A definitive diagnosis of chancroid requires the identification of H. ducreyi on special culture media that is not widely available from commercial sources; even when these media are used, sensitivity is less than 80 percent. No FDA- cleared PCR test for H. ducreyi is available in the United States, but such testing can be performed by clinical laboratories that have developed their own PCR test and have conducted a CLIA verification study. -

Reportable Disease Surveillance in Virginia, 2013
Reportable Disease Surveillance in Virginia, 2013 Marissa J. Levine, MD, MPH State Health Commissioner Report Production Team: Division of Surveillance and Investigation, Division of Disease Prevention, Division of Environmental Epidemiology, and Division of Immunization Virginia Department of Health Post Office Box 2448 Richmond, Virginia 23218 www.vdh.virginia.gov ACKNOWLEDGEMENT In addition to the employees of the work units listed below, the Office of Epidemiology would like to acknowledge the contributions of all those engaged in disease surveillance and control activities across the state throughout the year. We appreciate the commitment to public health of all epidemiology staff in local and district health departments and the Regional and Central Offices, as well as the conscientious work of nurses, environmental health specialists, infection preventionists, physicians, laboratory staff, and administrators. These persons report or manage disease surveillance data on an ongoing basis and diligently strive to control morbidity in Virginia. This report would not be possible without the efforts of all those who collect and follow up on morbidity reports. Divisions in the Virginia Department of Health Office of Epidemiology Disease Prevention Telephone: 804-864-7964 Environmental Epidemiology Telephone: 804-864-8182 Immunization Telephone: 804-864-8055 Surveillance and Investigation Telephone: 804-864-8141 TABLE OF CONTENTS INTRODUCTION Introduction ......................................................................................................................................1 -
Know Your Abcs: a Quick Guide to Reportable Infectious Diseases in Ohio
Know Your ABCs: A Quick Guide to Reportable Infectious Diseases in Ohio From the Ohio Administrative Code Chapter 3701-3; Effective August 1, 2019 Class A: Diseases of major public health concern because of the severity of disease or potential for epidemic spread – report immediately via telephone upon recognition that a case, a suspected case, or a positive laboratory result exists. • Anthrax • Measles • Rubella (not congenital) • Viral hemorrhagic fever • Botulism, foodborne • Meningococcal disease • Severe acute respiratory (VHF), including Ebola virus • Cholera • Middle East Respiratory syndrome (SARS) disease, Lassa fever, Marburg • Diphtheria Syndrome (MERS) • Smallpox hemorrhagic fever, and • Influenza A – novel virus • Plague • Tularemia Crimean-Congo hemorrhagic infection • Rabies, human fever Any unexpected pattern of cases, suspected cases, deaths or increased incidence of any other disease of major public health concern, because of the severity of disease or potential for epidemic spread, which may indicate a newly recognized infectious agent, outbreak, epidemic, related public health hazard or act of bioterrorism. Class B: Disease of public health concern needing timely response because of potential for epidemic spread – report by the end of the next business day after the existence of a case, a suspected case, or a positive laboratory result is known. • Amebiasis • Carbapenemase-producing • Hepatitis B (perinatal) • Salmonellosis • Arboviral neuroinvasive and carbapenem-resistant • Hepatitis C (non-perinatal) • Shigellosis -

Genital Herpes and Human Immunodeficiency Virus
Genital herpes and human immunodeficiency virus: double trouble Connie Celum,1 Ruth Levine,2 Marcia Weaver,3 & Anna Wald1 Abstract The synergistic relationship between herpes simplex virus type 2 (HSV-2) and transmission of human immunodeficiency virus (HIV) can be substantial in developing countries that have high prevalences of both viral infections. Genital herpes, most frequently caused by HSV-2, has become the leading cause of genital ulcer disease worldwide. This review of recent research on genital herpes and enhanced susceptibility to, and transmission of, HIV is part of the “Advances in HIV/AIDS research series” which endeavours to form a bridge between the research into HIV and acquired immunodeficiency syndrome (AIDS) and the practice of HIV/AIDS prevention, care and support in developing countries. Research findings have shown that being seropositive for HSV-2 can increase the risk of HIV acquisition among high-risk HIV-negative people exposed to HIV and, likewise, the infectiousness of individuals co-infected with HIV-1 and HSV-2 can increase during periods of HSV-2 reactivation. These observations have led to the initiation of several intervention trials and could ultimately lead to the setting of new priorities in public health and clinical practice. WHO has recently issued new guidelines for the syndromic management of genital ulcer disease that include antiviral treatment for lesions consistent with genital herpes. The United States Centers for Disease Control and Prevention issued updated Sexually Transmitted Diseases Treatment Guidelines in 2002 that recommended the use of type-specific serological tests for diagnosing HSV-2. Recently launched proof-of-concept, HSV-2 intervention trials in several countries will help to determine the proportion of new HIV infections that could be prevented by suppression of HSV-2, and the findings from these studies will inform those involved in setting prevention and treatment priorities and strategies in developing countries. -

Communicable Diseases Weekly Report
Communicable Diseases Weekly Report Week 08, 21 February to 27 February 2021 In summary, we report: • Chancroid – one new case in a returned traveller • Rodent-borne disease risks • Novel coronavirus 2019 (COVID-19) • Summary of notifiable conditions activity in NSW For further information see NSW Health infectious diseases page. This includes links to other NSW Health infectious disease surveillance reports and a diseases data page for a range of notifiable infectious diseases. Chancroid One case of chancroid was notified this reporting week in a traveller returning from overseas. Chancroid is an acute sexually transmitted bacterial infection that causes painful genital ulcers. The condition is now rarely seen in Australia and only one other case has been notified in NSW during the past decade. Although the incidence of chancroid is decreasing globally, it is still reported in some regions within Africa, Asia, the Caribbean and South Pacific. Chancroid genital ulcer disease is a known risk factor for the transmission of HIV. The bacterium that causes chancroid, Haemophilus ducreyi, is usually transmitted through anal, oral, or vaginal sex with an infected person. After infection, one or more ulcers (sores) develop on the genitals or around the anus. Non-genital skin infections have also been reported globally, through non-sexual skin-to-skin contact with an infected person. The ulcers are usually painful, but rarely can be asymptomatic. Swelling in the groin (due to enlarged painful lymph nodes that can liquify and develop into buboes) can also occur. Other symptoms may include pain during sexual intercourse or while urinating. An infected person can spread the infection from their genital region to other parts of their body. -

Annual Summary of Communicable Disease Reported to MDH, 2003
MINNESOTA DEPARTMENT OF HEALTH DISEASE CONTROL N EWSLETTER Volume 32, Number 4 (pages 33-52) July/August 2004 Annual Summary of Communicable Diseases Reported to the Minnesota Department of Health, 2003 Introduction Minnesota Government Data Practices do not appear in Table 2 because the Assessment is a core public health Act (Section 13.38). Provisions of the influenza surveillance system is based function. Surveillance for communi- Health Insurance Portability and on reported outbreaks rather than on cable diseases is one type of ongoing Accountability Act (HIPAA) allow for individual cases. assessment activity. Epidemiologic routine communicable disease report- surveillance is the systematic collec- ing without patient authorization. Incidence rates in this report were tion, analysis, and dissemination of calculated using disease-specific health data for the planning, implemen- Since April 1995, MDH has participated numerator data collected by MDH and a tation, and evaluation of public health as one of the Emerging Infections standardized set of denominator data programs. The Minnesota Department Program (EIP) sites funded by the derived from U.S. Census data. of Health (MDH) collects disease Centers for Disease Control and Disease incidence may be categorized surveillance information on certain Prevention (CDC) and, through this as occurring within the seven-county communicable diseases for the program, has implemented active Twin Cities metropolitan area (Twin purposes of determining disease hospital- and laboratory-based surveil- Cities metropolitan area) or outside of it impact, assessing trends in disease lance for several conditions, including (Greater Minnesota). occurrence, characterizing affected selected invasive bacterial diseases populations, prioritizing disease control and food-borne diseases. Anaplasmosis efforts, and evaluating disease preven- Human anaplasmosis (HA) is the new tion strategies. -

Disease Control Newsletter, July/August 2005
MINNESOTA DEPARTMENT OF HEALTH D ISEASE C ONTROL N EWSLETTER Volume 33, Number 4 (pages 37-56) July/August 2005 Annual Summary of Communicable Diseases Reported to the Minnesota Department of Health, 2004 Introduction private and protected under the Incidence rates in this report were Assessment is a core public health Minnesota Government Data Practices calculated using disease-specific function. Surveillance for communi Act (Section 13.38). Provisions of the numerator data collected by MDH and a cable diseases is one type of assess Health Insurance Portability and standardized set of denominator data ment. Epidemiologic surveillance is the Accountability Act (HIPAA) allow for derived from U.S. Census data. systematic collection, analysis, and routine communicable disease report Disease incidence may be categorized dissemination of health data for the ing without patient authorization. as occurring within the seven-county planning, implementation, and evalua Twin Cities metropolitan area or outside tion of health programs. The Minnesota Since April 1995, MDH has participated of it (Greater Minnesota). Department of Health (MDH) collects as an Emerging Infections Program information on certain communicable (EIP) site funded by the Centers for Anaplasmosis diseases for the purposes of determin Disease Control and Prevention (CDC) Human anaplasmosis (HA) is the new ing disease impact, assessing trends in and, through this program, has imple nomenclature for the disease formerly disease occurrence, characterizing mented active hospital- and laboratory- known as human granulocytic affected populations, prioritizing control based surveillance for several condi ehrlichiosis. HA (caused by the efforts, and evaluating prevention tions, including selected invasive rickettsia Anaplasma phagocytophilum) strategies. Prompt reporting allows bacterial diseases and food-borne is transmitted to humans by Ixodes outbreaks to be recognized in a timely diseases. -

LGV CEG June 2020
Sandyford Protocols Lymphogranuloma Venereum and Proctitis (LGV – see also Genital Ulcer Protocol) LGV must be tested in MSM with rectal symptoms and/or who are HIV positive LGV accounts for about 5% of the rectal Chlamydia detections in MSM in Glasgow. Management Confirmed cases First line: Doxycycline 100mg po bd 21 days NB warn re photosensitivity, oesophageal ulceration Second Line: Erythromycin 500 mg QDS for 21 days or Azithromycin 1g po stat followed by 1g weekly for three weeks Contact management Doxycycline 100mg po bd 21 days (Offer if sexual contact with a case of LGV within 4 weeks before onset of symptoms in index case or contact in last three months if asymptomatic LGV in an index case) Certain medications including fluconazole, macrolide and quinolone antibiotics cause QT prolongation and should not be prescribed with interacting medications. This is unlikely to be of clinical significance for stat doses but is important for longer courses. Please use BNF Interaction Checker to ensure these medications are safe to prescribe for your patient and discuss with a senior colleague if necessary. LGV epidemiology: LGV is caused by lymphotropic invasive strains of C.trachomatis (serovars L1,2,3) is now established as endemic in MSM in UK (the L2b strain is the dominant strain) Approximately 80 cases per quarter in UK Over 2000 cases to 2012 99% MSM LGV cases 8 times more likely to be HIV+ than non LGV Chlamydia cases Strong association with sex-party scene (traumatic sex, toys, fisting and enema use where shared equipment) 78% of cases are HIV+. -
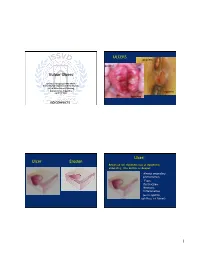
Vulvar Ulcers
ULCERS painless painful Vulvar Ulcers Lyne/e J. Margesson MD FRCPC Interna<onal Congress of Dermatology ISSVD Sister Society Mee<ng Buenos Aires, Argen<na syphilis April 14, 2017 Aphthae NO CONFLICTS Ulcer: Ulcer Erosion Result of full thickness loss of epidermis painful extending into dermis or deeper • Always secondary phenomenon • From Destruction, Necrosis, Inflammation (as in syphilis, aphthae, or tumor) 1 Erosion VULVAR ULCERS Result of loss of all or part of epidermis only ■ MULTIPLE causes spanning a variety of ages, ethnic groups, geographical regions • Result of broken vesicles, pustules or bullae ■ Differing pathologies may co-exist ■ NOT SPECIFIC ■ Classification of vulvar ulcers is difficult Vesicle or Bulla - Intraepidermal - contact dermatitis, Staph Sub epidermal - bullous disease, drug eruption Pustule: Candida, HSV Causes of Vulvar Ulcers Syndromic Approach § Used in areas where no good testing is available Infectious ulcers - commonest STIs # 1 – HSV § Lessens the dependence on laboratory tests # 2 – Syphilis (saves time and money) # 3 - Chancroid - Africa – chancroid Granuloma Inguinale - New Guinea – very rare North America § Simplifies a complex diagnostic process Non-infectious ulcers § Permits the treatment to begin immediately - Skin disorders – Aphthae, Crohn’s Disease, Trauma, cancer § STDs included are variable depending on locally prevalent STDs 2 Syndromic Protocol for Genital Ulcer Disease Commonest Causes of Vulvar Ulcers Patient complains of genital sore Infectious Non-infectious Counsel Take history and