Comments on Patient Protection and Affordable Care Act; Exchange Program Integrity
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Memo to the Biden Administration Transition Team
Memo to the Biden Administration Transition Team From: Trish Riley, National Academy for State Health Policy Executive Director Re: State-based marketplace strategies for insurance market stabilization and improvement Nov. 20, 2020 The National Academy for State Health Policy (NASHP), in close consultation with executives from state-based health insurance marketplaces (SBMs), has developed a list of priority actions that may: ● Lower costs and bring stability to individual and small group health insurance markets; ● Improve access to health insurance coverage; and/or ● Improve consumer experience when purchasing small group or individual market coverage. NASHP is home to the State Health Exchange Leadership Network, a consortium of state leaders and staff dedicated to operation of the SBMs. This list draws upon the experience of SBM leaders who have spent the past decade building and operating successful platforms for the procurement of health insurance coverage. These recommendations reflect NASHP’s collective discussions with SBM leaders, but do not reflect consensus across all SBMs. States value flexibility to design their programs to meet local needs and circumstances. For additional information specific to each state, please see Appendix A, which includes references to comments submitted by SBMs in response to various policy changes. We have also included the contact information for SBM executives who can provide additional information specific to their states. NASHP is ready to provide any additional information that may be helpful as you deliberate critically important issues related to health care coverage. Thank you for your time and consideration. Sincerely, Trish Riley Executive Director National Academy for State Health Policy 2 Monument Square, Suite 910, Portland ME 04101 1233 20th St NW, Suite 303, Washington, DC 20036 Phone: (207) 837-4815 State-Based Marketplace Recommended Areas for Priority Administrative Action in 2021 I. -

236Th & 237Th Legislative Health Committee Report
THE NEW YORK STATE SENATE STANDING COMMITTEE ON HEALTH 236TH-237TH LEGISLATIVE SESSION REPORT _________________________________ SENATOR KEMP HANNON CHAIRMAN REPORT OF THE NEW YORK STATE SENATE STANDING COMMITTEE ON HEALTH 236th & 237th LEGISLATIVE SESSION Senator Kemp Hannon, Chairman Senator Gustavo Rivera, Ranking Member Committee Members Senator Greg Ball Senator Velmanette Montogmery Senator Hugh T. Farley Senator Ted O’ Brien Senator Simcha Felder Senator Jose Peralta Senator Martin J. Golden Senator Diane J. Savino Senator Ruth Hassell- Thompson Senator Jose M. Serrano Senator Brad Hoylman Senator James L. Seward Senator William J. Larkin, Jr. Senator Catharine M. Young Senator Jack M. Martins Committee Staff Kristin Sinclair, Committee Director Alison Kane, Counsel to the Chairman Beth Kempter, Committee Clerk Room 420 New York State Capitol Albany, NY 12247 TABLE OF CONTENTS Executive Summary .........................................................................................................................1 Health Chapters ................................................................................................................................2 Patient Safety & Rights ........................................................................................................2 Health Care Facilities..........................................................................................................3 Health Care Professionals ...................................................................................................6 -

What Explains 2018'S Marketplace Enrollment Rates?
U.S. Health Reform—Monitoring and Impact What Explains 2018’s Marketplace Enrollment Rates? June 2018 By Rachel A. Burton, Rebecca A. Peters, Erik Wengle, Caroline Elmendorf, and Joshua Aarons Support for this research was provided by the Robert Wood Johnson Foundation. The views expressed here do not necessarily reflect the views of the Foundation. With support from the Robert Wood Johnson Foundation (RWJF), the Urban Institute is undertaking a comprehensive monitoring and tracking project to examine the implementation and effects of health reform. The project began in May 2011 and will take place over several years. The Urban Institute will document changes to the implementation of national health reform to help states, researchers and policymakers learn from the process as it unfolds. Reports that have been prepared as part of this ongoing project can be found at www.rwjf.org and www.healthpolicycenter.org. SUMMARY In the months leading up to the 2018 open enrollment kept grandmothered off-marketplace plans because period for health insurance marketplaces, members of premiums for these plans have grown at slower rates Congress made several efforts to repeal and replace the than marketplace premiums have. Affordable Care Act (ACA). Also, the federal government stopped reimbursing insurers for cost-sharing reductions The size of premium tax credits. Rhode Island, (CSRs) for eligible marketplace enrollees with incomes below Washington, and Louisiana maximized their premium 250 percent of the federal poverty level (FPL); cut funding tax credits by “silver-loading”—that is, directing insurers for enrollment assisters and marketplace advertising; to only increase silver plan premiums to account for and shortened the default open enrollment period for the cancelation of federal CSR payments. -

August 25, 2021 NEW YORK FORWARD/REOPENING
September 24, 2021 NEW YORK FORWARD/REOPENING GUIDANCE & INFORMATIONi FEDERAL UPDATES: • On August 3, 2021, the Centers for Disease Control and Prevention (CDC) issued an extension of the nationwide residential eviction pause in areas experiencing substantial and high levels of community transmission levels of SARS-CoV-2, which is aligned with the mask order. The moratorium order, that expires on October 3, 2021, allows additional time for rent relief to reach renters and to further increase vaccination rates. See: Press Release ; Signed Order • On July 27, 2021, the Centers for Disease Control and Prevention (CDC) updated its guidance for mask wearing in public indoor settings for fully vaccinated people in areas where coronavirus transmission is high, in response to the spread of the Delta Variant. The CDC also included a recommendation for fully vaccinated people who have a known exposure to someone with suspected or confirmed COVID-19 to be tested 3-5 days after exposure, and to wear a mask in public indoor settings for 14 days or until they receive a negative test result. Further, the CDC recommends universal indoor masking for all teachers, staff, students, and visitors to schools, regardless of vaccination status See: https://www.cdc.gov/coronavirus/2019- ncov/vaccines/fully-vaccinated-guidance.html • The CDC on Thursday, June 24, 2021 announced a one-month extension to its nationwide pause on evictions that was executed in response to the pandemic. The moratorium that was scheduled to expire on June 30, 2021 is now extended through July 31, 2021 and this is intended to be the final extension of the moratorium. -

Coronavirus Resource Guide for Residents and Businesses
Coronavirus Resource Guide For Residents & Businesses Compliments of: The Office of Suffolk County Legislator William R. Spencer, MD 18th District 224 Wall Street, Suite 303 Huntington, NY 11743 (631) 854-4500 Updated: 4/14/2021 2 Message from Legislator Spencer… Dear Neighbor, The COVID-19 pandemic has turned our lives upside down and the greater effects of this crisis have impacted all of us in numerous ways - emotionally, physically and economically. As we emerge from this crisis after more than a year of facing a pandemic, we see that the collective efforts and sacrifices made by many have led to a flattening of the curve, and now, with vaccination efforts ramping up across the country there is hope that we will one day return to a semblance of normalcy. Many Suffolk residents and businesses will be coping with the effects of COVID-19 for the foreseeable future. In an effort to help constituents navigate the ever-changing landscape and the numerous support services available across multiple levels of government, my office has put together the enclosed resource guide. It is my hope that this comprehensive list can help point you in the right direction during this difficult time. Please continue practicing social distancing and following all of the CDC recommended precautionary measures to prevent the spread of the virus. Check up on your family, friends, and neighbors, and remember to thank our health care workers, first responders, and essential employees on the frontlines. If you know of someone in need of support, feel free to refer him or her to my office, we are here to provide assistance. -

Consumer Decisionmaking in the Health Care Marketplace
Research Report Consumer Decisionmaking in the Health Care Marketplace Erin Audrey Taylor, Katherine Grace Carman, Andrea Lopez, Ashley N. Muchow, Parisa Roshan, Christine Eibner C O R P O R A T I O N For more information on this publication, visit www.rand.org/t/rr1567 Library of Congress Cataloging-in-Publication Data is available for this publication. ISBN: 978-0-8330-9505-3 Published by the RAND Corporation, Santa Monica, Calif. © Copyright 2016 RAND Corporation R® is a registered trademark. Limited Print and Electronic Distribution Rights This document and trademark(s) contained herein are protected by law. This representation of RAND intellectual property is provided for noncommercial use only. Unauthorized posting of this publication online is prohibited. Permission is given to duplicate this document for personal use only, as long as it is unaltered and complete. Permission is required from RAND to reproduce, or reuse in another form, any of its research documents for commercial use. For information on reprint and linking permissions, please visit www.rand.org/pubs/permissions.html. The RAND Corporation is a research organization that develops solutions to public policy challenges to help make communities throughout the world safer and more secure, healthier and more prosperous. RAND is nonprofit, nonpartisan, and committed to the public interest. RAND’s publications do not necessarily reflect the opinions of its research clients and sponsors. Support RAND Make a tax-deductible charitable contribution at www.rand.org/giving/contribute www.rand.org Preface For this report, researchers conducted a literature review to better understand how consumers make choices about health insurance enrollment and to assess how website design can influence choice when consumers select plans online. -

Health Insurance Exchange Operations Chart
Health Insurance Exchange Operations Chart *Chart updated June 12, 2015 Allison Wils As states continue to refine the operations of their health insurance exchanges, regardless of the exchange type (state-based exchange, state partnership exchange, or federally facilitated marketplace), it's helpful to compare and contrast operational resources. This chart contains each state's resources and forms for three distinct, and fundamentally important, areas of exchange operation: applications, appeals, and taxes. With links directly to the states' forms and guides related to these issue areas, this chart serves as a one-stop resource library for those interested in developing new, or revising old, versions of applications, appeals, and tax resources. Like all State Refor(u)m research, this chart is a collaborative effort with you, the user. Know of something we should add to this compilation? Your feedback is central to our ongoing, real-time analytical process, so tell us in a comment, or email [email protected] with your suggestions. State Application Forms & Guides Appeal Forms & Guides Tax Guides IRS: Form 1095-A Health Insurance Marketplace Statement IRS: Instructions for Form 1095-A Health Insurance Marketplace Statement IRS: Form 8962 Premium Tax Credit IRS: Form 8965 Health Coverage Federally-Facilitated Marketplaces Healthcare.gov: Appeal Request Exemptions Healthcare.gov: Application for (FFM) & State Partnership Form for Wyoming Marketplace (SPM) States (AK, Health Coverage & Help Paying IRS: Instructions for Form 8965 AL, AR, AZ, DE, FL, GA, IA, IL, IN, Costs Healthcare.gov: Appeal Request Health Coverage Exemptions KS, LA, ME, MI, MS, MO, MT, NC, Form for Select States (Group 1) Healthcare.gov: Instructions to IRS: Affordable Care Act Tax ND, NE, NH, NJ, OH, OK, PA, SC, Help You Complete Your Provisions SD, TN, TX, UT, VA, WA, WV, and Healthcare.gov: Appeal Request Application for Health Coverage Form for Select States (Group 2) WY) IRS: Pub. -

Getting Into Gear for 2014: an Early Look at Branding and Marketing of New Health Insurance Marketplaces
September 2013 | Issue Brief Getting into Gear for 2014: An Early Look at Branding and Marketing of New Health Insurance Marketplaces As of September 2013, states and the federal government are on the eve of their October 1st launch of open enrollment for the new Health Insurance Marketplaces, where consumers will be able to shop for and purchase private coverage and potentially receive subsidies to lower the cost of that coverage. Achieving adequate enrollment through these Marketplaces will be important for fulfilling the Affordable Care Act’s (ACA’s) goal of reducing the nation’s uninsured rate. Moreover, sufficient enrollment, particularly among young and healthy individuals, will be important for ensuring the financial sustainability of the Marketplaces over time. Recognizing the importance of enrollment, the federal government and the 17 states operating State-based Marketplaces have invested resources and conducted extensive consumer research to inform the branding and marketing campaigns for their Marketplaces. Based on a review of publicly available materials as of September 2013, this brief provides an examination of the Marketplace branding strategies, websites, and marketing materials, providing insight into how consumers will be introduced to the Marketplaces and some of the key messages and approaches the Marketplaces will utilize to encourage individuals to enroll. BACKGROUND The ACA seeks to reduce the number of uninsured through two key coverage expansions: the creation of new Health Insurance Marketplaces and an expansion in Medicaid eligibility. The Health Insurance Marketplaces will provide consumers with a choice of qualified health plans, offering similar benefits, so they can select the one that best meets their needs. -
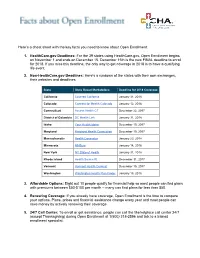
Facts About Open Enrollment
Here’s a cheat sheet with the key facts you need to know about Open Enrollment: 1. HealthCare.gov Deadlines: For the 39 states using HealthCare.gov, Open Enrollment begins on November 1 and ends on December 15. December 15th is the new FINAL deadline to enroll for 2018. If you miss this deadline, the only way to get coverage in 2018 is to have a qualifying life event. 2. Non-HealthCare.gov Deadlines: Here’s a rundown of the states with their own exchanges, their websites and deadlines: State State Based Marketplace Deadline for 2018 Coverage California Covered California January 31, 2018 Colorado Connect for Health Colorado January 12, 2018 Connecticut Access Health CT December 22, 2017 District of Columbia DC Health Link January 31, 2018 Idaho Your Health Idaho December 15, 2017 Maryland Maryland Health Connection December 15, 2017 Massachusetts Health Connector January 23, 2018 Minnesota MNSure January 14, 2018 New York NY State of Health January 31, 2018 Rhode Island Health Source RI December 31, 2017 Vermont Vermont Health Connect December 15, 2017 Washington Washington Health Plan Finder January 15, 2018 3. Affordable Options: Eight out 10 people qualify for financial help so most people can find plans with premiums between $50-$100 per month -- many can find plans for less than $50. 4. Renewing Coverage: If you already have coverage, Open Enrollment is the time to compare your options. Plans, prices and financial assistance change every year and most people can save money by actively renewing their coverage. 5. 24/7 Call Center: To enroll or get assistance, people can call the Marketplace call center 24/7 (except Thanksgiving) during Open Enrollment at 1(800) 318-2596 and talk to a trained enrollment specialist. -

NY State of Health Comments on HHS Notice of Benefit and Payment Parameters for 2021
NY State of Health Comments on HHS Notice of Benefit and Payment Parameters for 2021 NY State of Health, the State’s Official Health Plan Marketplace submits the following comments on the proposed regulations for 45 CFR Parts 146, 149, 155, 156, and 158; Patient Protection and Affordable Care Act; HHS Notice of Benefit and Payment Parameters for 2021; Notice Requirement for Non-Federal Governmental Plans [CMS-9916-P]. D. Part 155 - Exchange Establishment Standards and Other Related Standards Under the Affordable Care Act 1. Verification Process Related to Eligibility for Insurance Affordability Programs • Proposed Rule With regard to Exchange requirements to verify applicant eligibility or enrollment in employer sponsored coverage, the proposed rule adopts a new alternative approach to replace the current procedures in § 155.320(d)(4)(i), under which an Exchange may design its verification process based on the Exchange’s assessment of risk for inappropriate eligibility or payment for APTC or CSRs. As HHS continues to explore the best options for verification of employer-sponsored coverage, it notes that it will not take enforcement action against Exchanges that do not perform random sampling for plan years 2020 and 2021. • NY State of Health Comments NY State of Health supports continued state flexibility on employer-sponsored coverage verification, including through approved alternative procedures. In addition, NY State of Health encourages Federal efforts to make available to states a reliable data source for this purpose. 2. Eligibility -

Standardized Plan
Standardizing Health Plan Benefit Design in the Individual Market: Opportunities and Implications Sabrina Corlette and Chiquita Brooks-LaSure November 6, 2019 A grantee of the Robert Wood Johnson Foundation www.shvs.org About State Health and Value Strategies State Health and Value Strategies (SHVS) assists states in their efforts to transform health and health care by providing targeted technical assistance to state officials and agencies. The program is a grantee of the Robert Wood Johnson Foundation, led by staff at Princeton University’s Woodrow Wilson School of Public and International Affairs. The program connects states with experts and peers to undertake health care transformation initiatives. By engaging state officials, the program provides lessons learned, highlights successful strategies, and brings together states with experts in the field. Learn more at www.shvs.org. Questions? Email Heather Howard at [email protected]. Support for this webinar was provided by the Robert Wood Johnson Foundation. The views expressed here do not necessarily reflect the views of the Foundation. State Health & Value Strategies | 3 About Georgetown’s Center on Health Insurance Reforms (CHIR) • A team of experts on private health insurance and health reform • Conduct research and policy analysis, provide technical assistance to federal and state policymakers, regulators, and consumer advocates • Based at Georgetown University’s McCourt School of Public Policy • Learn more at https://chir.georgetown.edu/ State Health & Value Strategies | 4 About Manatt Health Manatt Health integrates legal and consulting expertise to better serve the complex needs of clients across the healthcare system. Combining legal excellence, first-hand experience in shaping public policy, sophisticated strategy insight, and deep analytic capabilities, we provide uniquely valuable professional services to the full range of health industry players. -

American Rescue Plan: Frequently Asked Questions (April 15, 2021)
American Rescue Plan: Frequently Asked Questions (April 15, 2021) I. Enhanced Federal Financial Assistance 1. Who is eligible for financial assistance through the American Rescue Plan and when will it be available through NY State of Health? Enhanced tax credits are available to lower and moderate income New Yorkers now and to higher income New Yorkers starting in June. If you were already eligible for financial help, this new higher financial assistance is available now. Log back into your NY State of Health account and check if you are eligible for the new financial assistance. If you were previously told that you were not eligible for financial help because your income is too high, you may be eligible for it starting in June. 2. I already get financial assistance to lower my monthly premium. Will my premiums go down with this new federal assistance? Most likely, yes. Unless your premium after tax credits is already $0, you will be eligible for additional financial assistance. Existing enrollees who were already eligible for tax credits can access the American Rescue Plan enhanced tax credits now. Low and moderate-income individuals (income up to $51,040 for an individual and $104,800 for a family of four) who were previously eligible for tax credits are now eligible for higher tax credits. These individuals can update their tax credit amounts by logging into their NY State of Health account and increasing their tax credit amount or by calling Customer Service (1-855-355-5777) now. Here’s a video of how to increase your tax credit amount: https://info.nystateofhealth.ny.gov/arpavideo.