Atrial Fibrillation (AF) and I Was Informed That I Needed a Cardiologist to Investigate the Cause
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Sinus Rhythm, Ectopic Beats and Tachycardia Do Ectopics Matter? the FAST-TT Protocol for Fetal Tachycardia
Sinus rhythm, ectopic beats and tachycardia Do ectopics matter? The FAST-TT protocol for fetal tachycardia London 23 January 2020 Prof Julene S Carvalho Head of Brompton Centre for Fetal Cardiology Consultant Fetal and Paediatric Cardiologist Professor of Practice, Fetal Cardiology Molecular & Clinical Sciences Research Institute, SGUL Normal and abnormal rhythm Learning objectives Normal and abnormal rhythm Learning objectives • To assess the normal cardiac rhythm Normal and abnormal rhythm Learning objectives • To assess the normal cardiac rhythm • To diagnose & manage irregular rhythm Normal and abnormal rhythm Learning objectives • To assess the normal cardiac rhythm • To diagnose & manage irregular rhythm • To diagnose & manage tachycardia Abnormal rhythm Learning objectives • To assess the normal cardiac rhythm Rhythm Sinus rhythm • regular • 1 atrial : 1 ventricular activity • constant AV timing (PR interval) Sinus rhythm Sinus rhythm Sinus rhythm Sinus rhythm ‘Eye-balling’ ‘Eye-balling’ Rhythm Study of rhythm (sinus or arrhythmia) • Based on simultaneous recording of atrial and ventricular activity Fetal arrhythmias Diagnostic modalities in the fetus Simultaneous recording Ultrasound • M-mode • Pulsed wave Doppler • Tissue Doppler Fetal magnetocardiography Fetal electrocardiography Fetal arrhythmias Diagnostic modalities in the fetus Simultaneous recording Ultrasound • M-mode • Pulsed wave Doppler • Tissue Doppler Sinus rhythm M-mode echocardiography LV V RA A Sinus rhythm Pulmonary vessels Carvalho et al. Heart 2007;93:1448-53 (Epub 2006 Dec 12) Simultaneous pulmonary artery and vein Methods • At the level of the 4-chamber view • Colour flow mapping: artery and vein • Inner 2/3 of lung parenchyma • Sample volume over artery and vein • Low velocity • (Absence of fetal breathing movement) Carvalho et al. -

Atypical Presentation of Viral Myocarditis in a Young Adult Mandeep Kaur1*, Prema Bezwada2 and Ayala Rodriguez Cesar1
ISSN: 2378-3656 Kaur et al. Clin Med Rev Case Rep 2019, 6:284 DOI: 10.23937/2378-3656/1410284 Volume 6 | Issue 9 Clinical Medical Reviews Open Access and Case Reports CASE REPORT Atypical Presentation of Viral Myocarditis in a Young Adult Mandeep Kaur1*, Prema Bezwada2 and Ayala Rodriguez Cesar1 1Department of Cardiology, The Brooklyn Hospital Center, New York, USA Check for 2Department of Internal Medicine, The Brooklyn Hospital Center, New York, USA updates *Corresponding author: Mandeep Kaur, Department of Cardiology, The Brooklyn Hospital Center, New York, United States of America Abstract Case Report Convulsive Syncope can be difficult to distinguish from sei- A 32-year-old female was brought to Emergency De- zures at times. We present a young adult with cardiogenic partment after a cardiac arrest at work. As per cowork- convulsive syncope that mimic seizures. Continuous cardi- ers she suddenly collapsed and had seizure like activity. ac monitoring revealed various arrythmias during seizure like activity. She had a viral prodrome. Cardiac MRI was She was found to be pulseless, so three rounds of CPR diagnostic for myocarditis. More detailed studies for the were performed, and four shocks were delivered. Re- role of a noninvasive cardiac testing such as Cardiac MRI turn of spontaneous circulation was achieved. She re- (CMR) and newer treatment modalities such as anti-thymo- verted to full consciousness spontaneously within min- cyte immunoglobulin are required for the management of Viral Myocarditis. utes without confusion or cognitive deficits. On further enquiry she admitted a one-week history of fever and Case report: A 32-year-old female was brought to the Emergency Department after a cardiac arrest at work. -

Atropine-Induced Bigeminy by Treating Bradycardia-Dependent
maco har log P y: r O la u p c e n s Rebollar et al., Cardiovasc Pharm Open Access 2016, 5:4 a A v c o c i e d r s DOI: 10.4172/2329-6607.1000193 a s Open Access C Cardiovascular Pharmacology: ISSN: 2329-6607 Case Report OpenOpen Access Access Atropine-Induced Bigeminy by Treating Bradycardia-Dependent Ectopy Ramón Eizaga Rebollar*, María Victoria García Palacios, Javier Morales Guerrero and Luis Miguel Torres Morera Department of Anesthesiology and Reanimation, Puerta del Mar University Hospital, Spain Abstract We report the case of a 9-year-old healthy boy who underwent day-surgery herniotomy under combined general and regional anesthesia. After inhalational induction, borderline bradycardia with Premature Ventricular Contractions (PVCs) was observed in ECG tracing, which worsened despite the adequate anesthetic management to avoid and treat arrhythmogenic triggers. Subsequent diagnostic tests were performed to rule out an underlying heart disease. Thereby, we conduct a brief review of ventricular ectopy in children with structurally normal hearts, both in the clinical and perioperative setting; and finally linked to our case in order to find out the cause of the abnormal electrical activity. Keywords: Pediatrics; Anesthesia; Ectopy; Premature ventricular Echocardiogram: No structural or functional abnormalities. After contractions; Bigeminy; Atropine 2 h of uneventful stay, the patient was moved to the ward and, 12 h later, was finally discharged pending a Holter monitoring and a stress Introduction test, which finally were not carried out because of patient´s decision. Ventricular ectopy consists in extra impulses originating from an Discussion area distal to His–Purkinje system. -

Dysrhythmias
CARDIOVASCULAR DISORDERS DYSRHYTHMIAS I. BASIC PRINCIPLES OF CARDIAC CONDUCTION DISTURBANCES A. Standard ECG and rhythm strips 1. Recordings are obtained at a paper speed of 25 mm/sec. 2. The vertical axis measures distance; the smallest divisions are 1 mm ×1 mm. 3. The horizontal axis measures time; each small division is 0.04 sec/mm. B. Normal morphology Courtesy of Dr. Michael McCrea 1. P wave = atrial depolarization a. Upright in leads I, II, III, aVL, and aVF; inverted in lead aVR b. Measures <0.10 seconds wide and <3 mm high c. Normal PR interval is 0.12–0.20 seconds. 2. QRS complex = ventricular depolarization a. Measures 0.06-0.10 seconds wide b. Q wave (1) <0.04 seconds wide and <3 mm deep (2) Abnormal if it is >3 mm deep or >1/3 of the QRS complex. c. R wave ≤7.5 mm high 3. QT interval varies with rate and sex but is usually 0.33–0.42 seconds; at normal heart rates, it is normally <1/2 the preceding RR interval. 4. T wave = ventricular repolarization a. Upright in leads I, II, V3–V6; inverted in aVR b. Slightly rounded and asymmetric in configuration c. Measures ≤5 mm high in limb leads and ≤10 mm high in the chest leads 5. U wave = a ventricular afterpotential a. Any deflection after the T wave (usually low voltage) b. Same polarity as the T wave c. Most easily detected in lead V3 d. Can be a normal component of the ECG e. Prominent U waves may indicate one of the following: (1) Hypokalemia (<3 mEq/L) (2) Hypercalcemia (3) Therapy with digitalis, phenothiazines, quinidine, epinephrine, inotropic agents, or amiodarone (4) Thyrotoxicosis f. -

Arrhythmogenic Right Ventricular Dysplasia/Cardiomyopathy Involving Isolated Ventricular Septum: Case Report Veeresh Patil*, V
Scholars Journal of Applied Medical Sciences (SJAMS) ISSN 2320-6691 (Online) Sch. J. App. Med. Sci., 2014; 2(2C):699-701 ISSN 2347-954X (Print) ©Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources) www.saspublisher.com Case Report Arrhythmogenic Right Ventricular Dysplasia/Cardiomyopathy Involving Isolated Ventricular Septum: Case Report Veeresh Patil*, V. S. Prakash, Nagamalesh, Anupama.H, Satvic M Department of Cardiology, M. S. Ramaiah Medical College, Bangalore, Karnataka, India *Corresponding author Dr. Veeresh Patil Email: Abstract: Arrhythmogenic right ventricular dysplasia (ARVD) is a disorder in which normal myocardium is replaced by fibrofatty tissue. This disorder usually involves the right ventricle, but the left ventricle and septum also may be affected. Patients with ARVD are usually men younger than 35 years who complain of chest pain or rapid heart rate. In some cases, sudden cardiac death is the first presentation. Further confirmation of the diagnosis includes noninvasive studies, such as echocardiography and magnetic resonance imaging of the heart, and invasive studies such as ventricular angiography and endomyocardial biopsy. Patients with ARVD are treated initially with antiarrhythmic agents with serious consideration for automatic implantable cardioverter-defibrillator placement. We are reporting a case of arrhythmogenic Right Ventricular Dysplasia/ Cardiomyopathy involving isolated ventricular septum. Keywords: Arrhythmogenic right ventricular dysplasia/Cardiomyopathy (ARVD/C), Cardioverter-defibrillator placement, RBBB pattern INTRODUCTION medical history included type 2 diabetes mellitus since Arrhythmogenic right ventricular dysplasia (ARVD), 1 yr on oral hypoglycemic agents and Dyslipidemia also called arrhythmogenic right ventricular since 1 yr on statin therapy. His blood investigations cardiomyopathy (ARVC) or arrhythmogenic right were within normal limits. -

Iatrogenic Escape-Capture Bigeminy*
Br Heart J: first published as 10.1136/hrt.29.2.264 on 1 March 1967. Downloaded from Brit. Heart J., 1967, 29, 264.- Iatrogenic Escape-capture Bigeminy* AGUSTIN CASTELLANOS, JR., ALBERTO BUDKIN, AND LOUIS LEMBERG From the Department of Medicine (Section of Cardiology), University of Miami School of Medicine, and the Division of Electrophysiology, Jackson Memorial Hospital, Miami, Florida, U.S.A. The primary purpose of electrical pacemakers is stimulation occurred. Initiation of pacemaking on to stimulate the heart whenever the ventricular con- demand produces escape-capture bigeminy. For tractions fail for one reason or another. In addi- instance, the fourth QRS complex is conducted from tion, there has been secondary information obtained the atria with a prolonged P-R interval. The fifth through the use of electronic equipment. Most ventricular beat is an iatrogenic escape occurring important amongst the latter has been the analogy 1'24 sec. afterward. The following P waves again between natural and iatrogenic events. Artificial capture the ventricles with a long P-R. The pacemakers have proved the importance of deduc- corresponding R-R distance is only 1 18 sec., evi- tive reasoning in clinical electrocardiography. The dently shorter than the demand escape interval. purpose of the present communication is to present Hence, it discharges the artificial pacemaker. This three examples of iatrogenic escape-capture bi- could not occur with fixed rate units. Thereafter, the geminy, a previously undescribed disorder of demand pacemaker escapes again, therefore main- rhythm, which we believe stresses the role of taining the escape-capture sequence. The same electronic instruments in understanding some funda- type of arrhythmia is seen in the upper strip of Fig. -

Mitral Valve Prolapse and Sudden Cardiac Death: a Systematic Review Hui-Chen Han, MBBS; Francis J
SYSTEMATIC REVIEW AND META-ANALYSIS Mitral Valve Prolapse and Sudden Cardiac Death: A Systematic Review Hui-Chen Han, MBBS; Francis J. Ha, MBBS; Andrew W. Teh, MBBS, PhD; Paul Calafiore, MBBS; Elizabeth F. Jones, MBBS, PhD; Jennifer Johns, MBBS; Anoop N. Koshy, MBBS; David O’Donnell, MBBS; David L. Hare, MBBS, DPM; Omar Farouque, MBBS, PhD; Han S. Lim, MBBS, PhD Background-—The relationship between mitral valve prolapse (MVP) and sudden cardiac death (SCD) remains controversial. In this systematic review, we evaluate the relationship between isolated MVP and SCD to better define a potential high-risk subtype. In addition, we determine whether premortem parameters could predict SCD in patients with MVP and the incidence of SCD in MVP. Methods and Results-—Electronic searches were conducted in PubMed and Embase for all English literature articles published between 1960 and 2018 regarding MVP and SCD or cardiac arrest. We also identified articles investigating predictors of ventricular arrhythmias or SCD and cohort studies reporting SCD outcomes in MVP. From 2180 citations, there were 79 articles describing 161 cases of MVP with SCD or cardiac arrest. The median age was 30 years and 69% of cases were female. Cardiac arrest occurred during situations of stress in 47% and was caused by ventricular fibrillation in 81%. Premature ventricular complexes on Holter monitoring (92%) were common. Most cases had bileaflet involvement (70%) with redundancy (99%) and nonsevere mitral regurgitation (83%). From 22 articles describing predictors for ventricular arrhythmias or SCD in MVP, leaflet redundancy was the only independent predictor of SCD. The incidence of SCD with MVP was estimated at 217 events per 100 000 person-years. -
Dynamic J-Point Elevation Associated
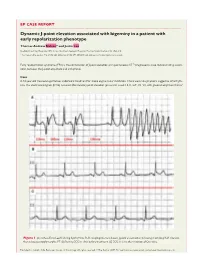
EP CASE REPORT .................................................................................................................................................... Dynamic J-point elevation associated with bigeminy in a patient with early repolarization phenotype Thomas Andrew Nelson* and Justin Lee Sheffield Teaching Hospitals NHS Trust, Northern General Hospital, Herries Road, Sheffield, S5 7AU, UK * Corresponding author. Tel: 0114 243 4343; fax: 0114 271 4084. E-mail address: [email protected] Early repolarization syndrome (ERS) is the combination of J-point elevation and spontaneous VF.1 We present a case demonstrating associ- ation between the J-point amplitude and arrhythmia. Case A 54-year-old Caucasian gentleman underwent treatment for stable angina in our institution. There were no symptoms suggestive of arrhyth- mia. The electrocardiogram (ECG) revealed inferolateral J-point elevation (present in Leads I, II, III, aVF, V5–V6, with greatest amplitude 0.2 mV Figure 1 (A) Surface ECG Lead II during dysrhythmia. R–R coupling intervals shown. J-point accentuation following short-long R–R intervals, then subsequent polymorphic VT. (B) Resting ECG in clinic before treatment. (C) ECG in clinic after initiation of Quinidine. Published on behalf of the European Society of Cardiology. All rights reserved. VC The Author 2017. For permissions, please email: [email protected]. in Lead II), notching of the S-wave and horizontal ST segments, a high-risk ER pattern.2 The corrected QT interval (Bazett’s, QTcB) was 433 ms. Coronary angiography revealed an aberrant circumflex artery arising from the right aortic sinus before coursing retroaortically. Minor disease within the left anterior descending artery (LAD) and right coronary artery was observed and a discrete stenosis in the mid-circumflex artery was stented, apparently without complication. -

Young Patient, Ventricular Tachycardia, Magnetic Resonance of the Heart and Myocarditis
HEART FAILURE Folia Cardiologica 2018 vol. 13, no. 6, pages 578–580 Copyright © 2018 Via Medica ISSN 2353–7752 Young patient, ventricular tachycardia, magnetic resonance of the heart and myocarditis Młody pacjent, częstoskurcz komorowy, rezonans magnetyczny serca i zapalenie mięśnia sercowego Filip Dybowski, Małgorzata Lelonek Department of Noninvasive Cardiology, Department of Internal Diseases and Cardiology, Medical University of Lodz, Lodz, Poland Artykuł jest tłumaczeniem pracy: Dybowski F, Lelonek M. Młody pacjent, częstoskurcz komorowy, rezonans magnetyczny serca i zapalenie mięśnia sercowego. Folia Cardiol. 2018; 13 (6): 575–577. DOI: 10.5603/FC.a2018.109 Należy cytować wersję pierwotną Abstract Here, we describe the case of a 25-year-old patient, who reported to cardiac outpatients department due to palpitations. Patient had no history of chronic diseases. We described step-by-step the diagnostic process, which allowed us to find type and cause of arrhythmia and start out effective treatment. Key words: ventricular tachycardia, myocarditis Folia Cardiologica 2018; 13, 6: 578–580 Introduction No improvement — modification of treatment A 25-year-old physician reported to the cardiac outpatient clinic because of a feeling of heart palpitations. He was not The next day, due to the severity of symptoms and his weak- treated for any chronic diseases and denied having cardiac ness, the patient came to the hospitals admission room. conditions of any kind. He stated that about 7–10 days The patient was in a stable condition, RR 130/88 mm Hg, before the visit he had a runny nose, and had not used an- HR 78/min. In ECG performed in the hospitals admission tibiotics. -

Multiple Arrhythmias in COVID-19 Patients: a Case Series
Annals of Cardiology CASE REPORT Multiple Arrhythmias in COVID-19 Patients: A Case Series Savalan Babapoor-Farrokhran1*, Zachary Port1, Deanna Gill2, Zaid Ammari1, Sumeet Mainigi1,2, and Aman Amanullah1,2 1Division of Cardiology, Department of Medicine, Einstein Medical Center, Philadelphia, USA 2Sidney Kimmel Medical College, Thomas Jefferson University, Philadelphia, USA. Abstract Extra-pulmonary manifestations of severe acute respiratory syndrome coronavirus 2 [SARS-CoV-2] infection such as cardiovascular complications have been reported and previous case reports have documented evidence of myocardial damage. Currently, very few case reports of the arrhythmias associated with Coronavirus Disease 2019 [COVID-19] exist. In this case series, we demonstrate two cases of critically ill COVID-19 patients with cardiac rhythm abnormalities that might be a direct or indirect consequence of this infection. Each of the patients experienced a variety of cardiac rhythm abnormalities. None of the patients had any record of cardiac rhythm abnormalities prior to admission. The unique point of these cases is the multiple dysrhythmias in the same patients that have not been reported previously. We demonstrated that critically ill COVID-19 patients develop different arrhythmias Open Access ranging from sinus tachycardia, bradycardia, atrial fibrillation, supraventricular tachycardia, and non-sustained ventricular tachycardia. Non-sustained Citation: Babapoor-Farrokhran S, Port Z, Gill D, Ammari Z, Mainigi S, monomorphic ventricular tachycardia was the most common arrhythmia in the two Amanullah A. Multiple Arrhythmias in cases despite normalization of electrolyte imbalances and avoidance of QTc COVID-19 Patients: A Case Series. Annals of Cardiology. 2020; 1(1):2. prolonging agents. Received: June 26, 2020 Accepted: September 30, 2020 Keywords Published: October 20, 2020 COVID-19, ventricular tachycardia, myocardial injury, intermittent bradycardia, cardiac arrhythmia, atrial fibrillation. -

Neonatal and Pediatric Guidelines for Arrhythmia Management What the Neonatal and Pediatric Critical Care Nurse Needs to Know
Neonatal and Pediatric Guidelines for Arrhythmia Management What the Neonatal and Pediatric Critical Care Nurse Needs to Know Cecilia St. George-Hyslop, M Ed, RN, CNCCP(C), The Hospital for Sick Children, Toronto, Canada Candace Morton, MSN, CPNP-PC/AC, Children’s Hospital of Wisconsin Elizabeth Daley, BA, BSN, RN, CCRN, Children’s Hospital of Los Angeles Introduction to the Problem: Arrhythmias are relatively common in the pediatric cardiac intensive care unit. Grosse-Wortmann et al studied 494 patients revealing 59% of neonates and 79% of older children have arrhythmias within 24 hrs of surgery. Of these arrhythmias, junctional ectopic tachycardia (JET) was seen in 9% of neonates and 5% of older children. Ventricular tachycardia was found in 3% of neonates and 15% of older children (Gross-Wortmann, 2010). In terms of specific arrhythmias, sinus tachycardia is the most frequently seen arrhythmia, with supraventricular tachycardia being the next most common, followed by sinus bradycardia (Hanash, 2010). Reentrant tachycardia is common in infants and children with congenital heart disease (CHD). Some arrhythmias in the early post operative period like premature atrial contraction’s (PAC’s) and premature ventricular beats (bigeminy) are usually transient and well tolerated. Others like junctional ectopic tachycardia (JET) and atrial flutter may cause significant hemodynamic instability and compromise or even sudden cardiac death. Primary arrhythmias occur in children without structural heart disease, although they may be secondary to ion channel diseases that are still being elucidated. Risk factors that predispose children for secondary arrhythmias include congenital cardiac malformations, surgical repair and scarring, long cardiopulmonary bypass times, or exposure to chronic hemodynamic stress (Brugada, 2013). -

Premature Atrial and Ventricular Contraction Detection Using Photoplethysmographic Data from a Smartwatch
sensors Article Premature Atrial and Ventricular Contraction Detection Using Photoplethysmographic Data from a Smartwatch Dong Han 1 , Syed Khairul Bashar 1 , Fahimeh Mohagheghian 1 , Eric Ding 2 , Cody Whitcomb 2 , David D. McManus 2 and Ki H. Chon 1,* 1 Department of Biomedical Engineering, University of Connecticut, Storrs, CT 06269, USA; [email protected] (D.H.); [email protected] (S.K.B.); [email protected] (F.M.) 2 Division of Cardiology, University of Massachusetts Medical School, Worcester, MA 01655, USA; [email protected] (E.D.); [email protected] (C.W.); [email protected] (D.D.M.) * Correspondence: [email protected] Received: 26 August 2020; Accepted: 30 September 2020; Published: 5 October 2020 Abstract: We developed an algorithm to detect premature atrial contraction (PAC) and premature ventricular contraction (PVC) using photoplethysmographic (PPG) data acquired from a smartwatch. Our PAC/PVC detection algorithm is composed of a sequence of algorithms that are combined to discriminate various arrhythmias. A novel vector resemblance method is used to enhance the PAC/PVC detection results of the Poincaré plot method. The new PAC/PVC detection algorithm with our automated motion and noise artifact detection approach yielded a sensitivity of 86% for atrial fibrillation (AF) subjects while the overall sensitivity was 67% when normal sinus rhythm (NSR) subjects were also included. The specificity, positive predictive value (PPV), negative predictive value (NPV) and accuracy values for the combined data consisting of both NSR and AF subjects were 97%, 81%, 94% and 92%, respectively, for PAC/PVC detection combined with our automated motion and noise artifact detection approach.