Sacral Agenesis: a Pilot Whole Exome Sequencing and Copy Number Study
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Methods in and Applications of the Sequencing of Short Non-Coding Rnas" (2013)
University of Pennsylvania ScholarlyCommons Publicly Accessible Penn Dissertations 2013 Methods in and Applications of the Sequencing of Short Non- Coding RNAs Paul Ryvkin University of Pennsylvania, [email protected] Follow this and additional works at: https://repository.upenn.edu/edissertations Part of the Bioinformatics Commons, Genetics Commons, and the Molecular Biology Commons Recommended Citation Ryvkin, Paul, "Methods in and Applications of the Sequencing of Short Non-Coding RNAs" (2013). Publicly Accessible Penn Dissertations. 922. https://repository.upenn.edu/edissertations/922 This paper is posted at ScholarlyCommons. https://repository.upenn.edu/edissertations/922 For more information, please contact [email protected]. Methods in and Applications of the Sequencing of Short Non-Coding RNAs Abstract Short non-coding RNAs are important for all domains of life. With the advent of modern molecular biology their applicability to medicine has become apparent in settings ranging from diagonistic biomarkers to therapeutics and fields angingr from oncology to neurology. In addition, a critical, recent technological development is high-throughput sequencing of nucleic acids. The convergence of modern biotechnology with developments in RNA biology presents opportunities in both basic research and medical settings. Here I present two novel methods for leveraging high-throughput sequencing in the study of short non- coding RNAs, as well as a study in which they are applied to Alzheimer's Disease (AD). The computational methods presented here include High-throughput Annotation of Modified Ribonucleotides (HAMR), which enables researchers to detect post-transcriptional covalent modifications ot RNAs in a high-throughput manner. In addition, I describe Classification of RNAs by Analysis of Length (CoRAL), a computational method that allows researchers to characterize the pathways responsible for short non-coding RNA biogenesis. -

Metastatic Adrenocortical Carcinoma Displays Higher Mutation Rate and Tumor Heterogeneity Than Primary Tumors
ARTICLE DOI: 10.1038/s41467-018-06366-z OPEN Metastatic adrenocortical carcinoma displays higher mutation rate and tumor heterogeneity than primary tumors Sudheer Kumar Gara1, Justin Lack2, Lisa Zhang1, Emerson Harris1, Margaret Cam2 & Electron Kebebew1,3 Adrenocortical cancer (ACC) is a rare cancer with poor prognosis and high mortality due to metastatic disease. All reported genetic alterations have been in primary ACC, and it is 1234567890():,; unknown if there is molecular heterogeneity in ACC. Here, we report the genetic changes associated with metastatic ACC compared to primary ACCs and tumor heterogeneity. We performed whole-exome sequencing of 33 metastatic tumors. The overall mutation rate (per megabase) in metastatic tumors was 2.8-fold higher than primary ACC tumor samples. We found tumor heterogeneity among different metastatic sites in ACC and discovered recurrent mutations in several novel genes. We observed 37–57% overlap in genes that are mutated among different metastatic sites within the same patient. We also identified new therapeutic targets in recurrent and metastatic ACC not previously described in primary ACCs. 1 Endocrine Oncology Branch, National Cancer Institute, National Institutes of Health, Bethesda, MD 20892, USA. 2 Center for Cancer Research, Collaborative Bioinformatics Resource, National Cancer Institute, National Institutes of Health, Bethesda, MD 20892, USA. 3 Department of Surgery and Stanford Cancer Institute, Stanford University, Stanford, CA 94305, USA. Correspondence and requests for materials should be addressed to E.K. (email: [email protected]) NATURE COMMUNICATIONS | (2018) 9:4172 | DOI: 10.1038/s41467-018-06366-z | www.nature.com/naturecommunications 1 ARTICLE NATURE COMMUNICATIONS | DOI: 10.1038/s41467-018-06366-z drenocortical carcinoma (ACC) is a rare malignancy with types including primary ACC from the TCGA to understand our A0.7–2 cases per million per year1,2. -

Application of Microrna Database Mining in Biomarker Discovery and Identification of Therapeutic Targets for Complex Disease
Article Application of microRNA Database Mining in Biomarker Discovery and Identification of Therapeutic Targets for Complex Disease Jennifer L. Major, Rushita A. Bagchi * and Julie Pires da Silva * Department of Medicine, Division of Cardiology, University of Colorado Anschutz Medical Campus, Aurora, CO 80045, USA; [email protected] * Correspondence: [email protected] (R.A.B.); [email protected] (J.P.d.S.) Supplementary Tables Methods Protoc. 2021, 4, 5. https://doi.org/10.3390/mps4010005 www.mdpi.com/journal/mps Methods Protoc. 2021, 4, 5. https://doi.org/10.3390/mps4010005 2 of 25 Table 1. List of all hsa-miRs identified by Human microRNA Disease Database (HMDD; v3.2) analysis. hsa-miRs were identified using the term “genetics” and “circulating” as input in HMDD. Targets CAD hsa-miR-1 Targets IR injury hsa-miR-423 Targets Obesity hsa-miR-499 hsa-miR-146a Circulating Obesity Genetics CAD hsa-miR-423 hsa-miR-146a Circulating CAD hsa-miR-149 hsa-miR-499 Circulating IR Injury hsa-miR-146a Circulating Obesity hsa-miR-122 Genetics Stroke Circulating CAD hsa-miR-122 Circulating Stroke hsa-miR-122 Genetics Obesity Circulating Stroke hsa-miR-26b hsa-miR-17 hsa-miR-223 Targets CAD hsa-miR-340 hsa-miR-34a hsa-miR-92a hsa-miR-126 Circulating Obesity Targets IR injury hsa-miR-21 hsa-miR-423 hsa-miR-126 hsa-miR-143 Targets Obesity hsa-miR-21 hsa-miR-223 hsa-miR-34a hsa-miR-17 Targets CAD hsa-miR-223 hsa-miR-92a hsa-miR-126 Targets IR injury hsa-miR-155 hsa-miR-21 Circulating CAD hsa-miR-126 hsa-miR-145 hsa-miR-21 Targets Obesity hsa-mir-223 hsa-mir-499 hsa-mir-574 Targets IR injury hsa-mir-21 Circulating IR injury Targets Obesity hsa-mir-21 Targets CAD hsa-mir-22 hsa-mir-133a Targets IR injury hsa-mir-155 hsa-mir-21 Circulating Stroke hsa-mir-145 hsa-mir-146b Targets Obesity hsa-mir-21 hsa-mir-29b Methods Protoc. -

Genomic and Transcriptome Analysis Revealing an Oncogenic Functional Module in Meningiomas
Neurosurg Focus 35 (6):E3, 2013 ©AANS, 2013 Genomic and transcriptome analysis revealing an oncogenic functional module in meningiomas XIAO CHANG, PH.D.,1 LINGLING SHI, PH.D.,2 FAN GAO, PH.D.,1 JONATHAN RUssIN, M.D.,3 LIYUN ZENG, PH.D.,1 SHUHAN HE, B.S.,3 THOMAS C. CHEN, M.D.,3 STEVEN L. GIANNOTTA, M.D.,3 DANIEL J. WEISENBERGER, PH.D.,4 GAbrIEL ZADA, M.D.,3 KAI WANG, PH.D.,1,5,6 AND WIllIAM J. MAck, M.D.1,3 1Zilkha Neurogenetic Institute, Keck School of Medicine, University of Southern California, Los Angeles, California; 2GHM Institute of CNS Regeneration, Jinan University, Guangzhou, China; 3Department of Neurosurgery, Keck School of Medicine, University of Southern California, Los Angeles, California; 4USC Epigenome Center, Keck School of Medicine, University of Southern California, Los Angeles, California; 5Department of Psychiatry, Keck School of Medicine, University of Southern California, Los Angeles, California; and 6Division of Bioinformatics, Department of Preventive Medicine, Keck School of Medicine, University of Southern California, Los Angeles, California Object. Meningiomas are among the most common primary adult brain tumors. Although typically benign, roughly 2%–5% display malignant pathological features. The key molecular pathways involved in malignant trans- formation remain to be determined. Methods. Illumina expression microarrays were used to assess gene expression levels, and Illumina single- nucleotide polymorphism arrays were used to identify copy number variants in benign, atypical, and malignant me- ningiomas (19 tumors, including 4 malignant ones). The authors also reanalyzed 2 expression data sets generated on Affymetrix microarrays (n = 68, including 6 malignant ones; n = 56, including 3 malignant ones). -

Centre for Arab Genomic Studies a Division of Sheikh Hamdan Award for Medical Sciences
Centre for Arab Genomic Studies A Division of Sheikh Hamdan Award for Medical Sciences The atalogue for ransmission enetics in rabs C T G A CTGA Database PDZ Domain-Containing 2 Alternative Names The PDZD2 gene, located on the short arm of PDZD2 chromosome 5, is approximately 471 kb long with a Plakophilin-Related Armadillo Repeat Protein- coding sequence consisting of 30 exons. The gene Interacting PDZ Protein is found to be overexpressed in the plasma, frontal APIN cortex, placenta and heart. Alternative splicing of PIN1 the gene results in transcripts that encode two Activated in Prostate Cancer different isoforms of the protein. Isoform 1 of the AIPC PDZD2 protein is made up of 2839 amino acids and KIAA0300 is about 301 kDa in size. Isoform 2 of protein, which is only 280 kDa in size, is found to be Record Category expressed in the prostate. Gene locus Epidemiology in the Arab World WHO-ICD N/A to gene loci Saudi Arabia Incidence per 100,000 Live Births Wakil et al. (2016) performed a genome wide N/A to gene loci association study on 2668 Saudi patients with Coronary Artery Disease (CAD) and/or Myocardial OMIM Number Infarction (MI) and 3000 controls to identify gene 610697 loci linked to these conditions. To identify an association as being statistically significant or Mode of Inheritance suggestive, p values had to be less than 5x10-8 or N/A to gene loci 1x10-5 respectively. The PDZD2 gene carried a SNP rs32793_G that showed a suggestive Gene Map Locus association with MI [6.13E-06, OR=1.25(1.14- 5p13.3 1.37)]. -

Whole Genome and Transcriptome Sequencing of Matched Primary And
www.nature.com/scientificreports OPEN Whole genome and transcriptome sequencing of matched primary and peritoneal metastatic gastric Received: 07 April 2015 Accepted: 04 August 2015 carcinoma Published: 02 September 2015 Zhang J.1,2,*, Huang J. Y.2,3,*, Chen Y. N.1,2,*, Yuan F.4, Zhang H.5, Yan F. H.5, Wang M. J.3, Wang G.6, Su M.6, Lu G.6, Huang Y.6, Dai H.6, Ji J.1,2, Zhang J.1,2, Zhang J. N.1,2, Jiang Y. N.1,2, Chen S. J.2,3, Zhu Z. G.1,2 & Yu Y. Y.1,2 Gastric cancer is one of the most aggressive cancers and is the second leading cause of cancer death worldwide. Approximately 40% of global gastric cancer cases occur in China, with peritoneal metastasis being the prevalent form of recurrence and metastasis in advanced disease. Currently, there are limited clinical approaches for predicting and treatment of peritoneal metastasis, resulting in a 6-month average survival time. By comprehensive genome analysis will uncover the pathogenesis of peritoneal metastasis. Here we describe a comprehensive whole-genome and transcriptome sequencing analysis of one advanced gastric cancer case, including non-cancerous mucosa, primary cancer and matched peritoneal metastatic cancer. The peripheral blood is used as normal control. We identified 27 mutated genes, of which 19 genes are reported in COSMIC database (ZNF208, CRNN, ATXN3, DCTN1, RP1L1, PRB4, PRB1, MUC4, HS6ST3, MUC17, JAM2, ITGAD, IREB2, IQUB, CORO1B, CCDC121, AKAP2, ACAN and ACADL), and eight genes have not previously been described in gastric cancer (CCDC178, ARMC4, TUBB6, PLIN4, PKLR, PDZD2, DMBT1and DAB1). -

Integration of Mouse and Human Genome-Wide Association Data Identifies CK NIP4 As an Asthma Gene Robert C
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2013 Integration of mouse and human genome-wide association data identifies CK NIP4 as an asthma gene Robert C. Strunk Washington University School of Medicine in St. Louis et al Follow this and additional works at: https://digitalcommons.wustl.edu/open_access_pubs Recommended Citation Strunk, Robert C. and et al, ,"Integration of mouse and human genome-wide association data identifies KCNIP4 as an asthma gene." PLoS One.,. e56179. (2013). https://digitalcommons.wustl.edu/open_access_pubs/1395 This Open Access Publication is brought to you for free and open access by Digital Commons@Becker. It has been accepted for inclusion in Open Access Publications by an authorized administrator of Digital Commons@Becker. For more information, please contact [email protected]. Integration of Mouse and Human Genome-Wide Association Data Identifies KCNIP4 as an Asthma Gene Blanca E. Himes1,2,3*, Keith Sheppard4, Annerose Berndt5, Adriana S. Leme5, Rachel A. Myers6, Christopher R. Gignoux7, Albert M. Levin8, W. James Gauderman9, James J. Yang8, Rasika A. Mathias10, Isabelle Romieu11, Dara G. Torgerson7, Lindsey A. Roth7, Scott Huntsman7, Celeste Eng7, Barbara Klanderman3, John Ziniti1, Jody Senter-Sylvia1, Stanley J. Szefler12, Robert F. Lemanske, Jr.13, Robert S. Zeiger14, Robert C. Strunk15, Fernando D. Martinez16, Homer Boushey17, Vernon M. Chinchilli18, Elliot Israel19, David Mauger18, Gerard H. Koppelman20, Dirkje S. Postma21, Maartje A. E. Nieuwenhuis21, Judith M. Vonk22, John J. Lima23, Charles G. Irvin24, Stephen P. Peters25, Michiaki Kubo26, Mayumi Tamari26, Yusuke Nakamura27, Augusto A. Litonjua1, Kelan G. Tantisira1, Benjamin A. Raby1, Eugene R. Bleecker25, Deborah A. -

Supplementary Table 1
Supplemental Table. Genes located within 1 LOD drop range of highest observed peak from linkage analysis with percent mammographic density on chromosome 5p Gene Name GeneID Position Description LOC728411 728411 5p14.3 similar to Beta-glucuronidase precursor LOC728401 728401 5p14.3 similar to nuclear pore membrane protein 121 CDH12 1010 5p14-p13 cadherin 12, type 2 (N-cadherin 2) LOC643300 643300 5-14.3 similar to 60 kDa heat shock protein, mitochondrial precursor (Hsp60) PMCHL1 5369 5p14.3 pro-melanin-concentrating hormone-like 1 LOC391771 391771 5p14.2 similar to protein tyrosine phosphatase, non-receptor type 11 PRDM9 56979 5p14 PR domain containing 9 C5orf17 439936 5p14.2 chromosome 5 open reading frame 17 LOC503540 503540 5-14.2 fused toes homolog (mouse) pseudogene CDH10 1008 5p14-p13 cadherin 10, type 2 (T2-cadherin) LOC729826 729826 5p14.1 hypothetical protein LOC729826 MSNL1 4479 5p14.1 moesin-like 1 CDH9 1007 5p14 cadherin 9, type 2 (T1-cadherin) LOC643401 643401 5p14.1 hypothetical protein LOC643401 LOC729862 729862 5p14.1 similar to Striatin PGBD3P2 267006 5p13.3 piggyBac transposable element derived 3 pseudogene 2 HPRTP2 3254 5p13.3 hypoxanthine phosphoribosyltransferase pseudogene 2 LOC391774 391774 5p13.3 similar to ribosomal protein L19 1 Supplemental Table. Genes located within 1 LOD drop range of highest observed peak from linkage analysis with percent mammographic density on chromosome 5p (cont) Gene Name GeneID Position Description CDH6 1004 5p15.1-p14 cadherin 6, type 2, K-cadherin (fetal kidney) RNASEN 29102 5p13.3 ribonuclease III, nuclear C5orf22 55322 5p13.3 chromosome 5 open reading frame 22 PDZD2 23037 5p13.3 PDZ domain containing 2 LOC728523 728523 5p13.3 similar to ribosomal protein L9 GOLPH3 64083 5p13.3 golgi phosphoprotein 3 (coat-protein) LOC202122 202122 5p13.3 similar to ribosomal protein L27 MTMR12 54545 5p13.3 myotubularin related protein 12 ZFR 51663 5p13.3 zinc finger RNA binding protein LOC646616 646616 5p13.3 chromosome 1 open reading frame 37 pseudogene SUB1 10923 5p13.3 SUB1 homolog (S. -

Supplementary Table 1 Double Treatment Vs Single Treatment
Supplementary table 1 Double treatment vs single treatment Probe ID Symbol Gene name P value Fold change TC0500007292.hg.1 NIM1K NIM1 serine/threonine protein kinase 1.05E-04 5.02 HTA2-neg-47424007_st NA NA 3.44E-03 4.11 HTA2-pos-3475282_st NA NA 3.30E-03 3.24 TC0X00007013.hg.1 MPC1L mitochondrial pyruvate carrier 1-like 5.22E-03 3.21 TC0200010447.hg.1 CASP8 caspase 8, apoptosis-related cysteine peptidase 3.54E-03 2.46 TC0400008390.hg.1 LRIT3 leucine-rich repeat, immunoglobulin-like and transmembrane domains 3 1.86E-03 2.41 TC1700011905.hg.1 DNAH17 dynein, axonemal, heavy chain 17 1.81E-04 2.40 TC0600012064.hg.1 GCM1 glial cells missing homolog 1 (Drosophila) 2.81E-03 2.39 TC0100015789.hg.1 POGZ Transcript Identified by AceView, Entrez Gene ID(s) 23126 3.64E-04 2.38 TC1300010039.hg.1 NEK5 NIMA-related kinase 5 3.39E-03 2.36 TC0900008222.hg.1 STX17 syntaxin 17 1.08E-03 2.29 TC1700012355.hg.1 KRBA2 KRAB-A domain containing 2 5.98E-03 2.28 HTA2-neg-47424044_st NA NA 5.94E-03 2.24 HTA2-neg-47424360_st NA NA 2.12E-03 2.22 TC0800010802.hg.1 C8orf89 chromosome 8 open reading frame 89 6.51E-04 2.20 TC1500010745.hg.1 POLR2M polymerase (RNA) II (DNA directed) polypeptide M 5.19E-03 2.20 TC1500007409.hg.1 GCNT3 glucosaminyl (N-acetyl) transferase 3, mucin type 6.48E-03 2.17 TC2200007132.hg.1 RFPL3 ret finger protein-like 3 5.91E-05 2.17 HTA2-neg-47424024_st NA NA 2.45E-03 2.16 TC0200010474.hg.1 KIAA2012 KIAA2012 5.20E-03 2.16 TC1100007216.hg.1 PRRG4 proline rich Gla (G-carboxyglutamic acid) 4 (transmembrane) 7.43E-03 2.15 TC0400012977.hg.1 SH3D19 -
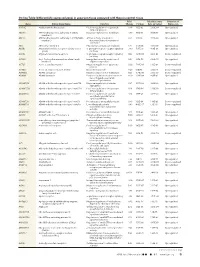
Differentially Expressed Genes in Aneurysm Tissue Compared With
On-line Table: Differentially expressed genes in aneurysm tissue compared with those in control tissue Fold False Discovery Direction of Gene Entrez Gene Name Function Change P Value Rate (q Value) Expression AADAC Arylacetamide deacetylase Positive regulation of triglyceride 4.46 1.33E-05 2.60E-04 Up-regulated catabolic process ABCA6 ATP-binding cassette, subfamily A (ABC1), Integral component of membrane 3.79 9.15E-14 8.88E-12 Up-regulated member 6 ABCC3 ATP-binding cassette, subfamily C (CFTR/MRP), ATPase activity, coupled to 6.63 1.21E-10 7.33E-09 Up-regulated member 3 transmembrane movement of substances ABI3 ABI family, member 3 Peptidyl-tyrosine phosphorylation 6.47 2.47E-05 4.56E-04 Up-regulated ACKR1 Atypical chemokine receptor 1 (Duffy blood G-protein–coupled receptor signaling 3.80 7.95E-10 4.18E-08 Up-regulated group) pathway ACKR2 Atypical chemokine receptor 2 G-protein–coupled receptor signaling 0.42 3.29E-04 4.41E-03 Down-regulated pathway ACSM1 Acyl-CoA synthetase medium-chain family Energy derivation by oxidation of 9.87 1.70E-08 6.52E-07 Up-regulated member 1 organic compounds ACTC1 Actin, ␣, cardiac muscle 1 Negative regulation of apoptotic 0.30 7.96E-06 1.65E-04 Down-regulated process ACTG2 Actin, ␥2, smooth muscle, enteric Blood microparticle 0.29 1.61E-16 2.36E-14 Down-regulated ADAM33 ADAM domain 33 Integral component of membrane 0.23 9.74E-09 3.95E-07 Down-regulated ADAM8 ADAM domain 8 Positive regulation of tumor necrosis 4.69 2.93E-04 4.01E-03 Up-regulated factor (ligand) superfamily member 11 production ADAMTS18 -

Cellular Mechanisms That Promote the Collective
CELLULAR MECHANISMS THAT PROMOTE THE COLLECTIVE MIGRATORY BEHAVIOR OF DROSOPHILA BORDER CELLS by GEORGE GIL F. ARANJUEZ Submitted in partial fulfillment of the requirements for the degree of Doctor of Philosophy Department of Genetics and Genome Sciences CASE WESTERN RESERVE UNIVERSITY August, 2015 CASE WESTERN RESERVE UNIVERSITY SCHOOL OF GRADUATE STUDIES We hereby approve the dissertation of George Gil F. Aranjuez candidate for the degree of Doctor of Philosophy. Committee Chair Dr. Helen Salz Committee Member / Mentor Dr. Jocelyn McDonald Committee Member Dr. Heather Broihier Committee Member Dr. Hua Lou Date of Defense July 7, 2015 *We also certify that written approval has been obtained for any proprietary material contained therein. 2 TABLE OF CONTENTS LIST OF TABLES ............................................................................................................ 7 LIST OF FIGURES .......................................................................................................... 8 ACKNOWLEDGEMENTS ........................................................................................... 11 ABSTRACT ..................................................................................................................... 13 CHAPTER 1. INTRODUCTION .................................................................................. 15 COLLECTIVE MIGRATION DURING NORMAL DEVELOPMENT ............. 16 Collective movement of two-dimensional cell sheets .............................. 16 Sprouting and branching involves leading -

Alsaai Udel 0060D 14351.Pdf
INVESTIGATION OF TDRD7 FUNCTION IN OCULAR LENS DEVELOPMENT by Salma Mohammed Al Saai A dissertation submitted to the Faculty of the University of Delaware in partial fulfillment of the requirements for the degree of Doctor of Philosophy in Biological Sciences Summer 2020 © 2020 Salma Mohammed Al Saai All Rights Reserved . INVESTIGATION OF TDRD7 FUNCTION IN OCULAR LENS DEVELOPMENT by Salma Mohammed Al Saai Approved: __________________________________________________________ Velia M. Fowler, Ph.D. Chair of the Department of Biological Sciences Approved: __________________________________________________________ John A. Pelesko, Ph.D. Dean of the College of Arts & Sciences Approved: __________________________________________________________ Douglas J. Doren, Ph.D. Interim Vice Provost for Graduate and Professional Education and Dean of the Graduate College I certify that I have read this dissertation and that in my opinion it meets the academic and professional standard required by the University as a dissertation for the degree of Doctor of Philosophy. Signed: __________________________________________________________ Salil A. Lachke, Ph.D. Professor in charge of dissertation I certify that I have read this dissertation and that in my opinion it meets the academic and professional standard required by the University as a dissertation for the degree of Doctor of Philosophy. Signed: __________________________________________________________ Melinda K. Duncan, Ph.D. Member of dissertation committee I certify that I have read this dissertation and that in my opinion it meets the academic and professional standard required by the University as a dissertation for the degree of Doctor of Philosophy. Signed: __________________________________________________________ Donna Woulfe, Ph.D. Member of dissertation committee I certify that I have read this dissertation and that in my opinion it meets the academic and professional standard required by the University as a dissertation for the degree of Doctor of Philosophy.