A Step-By-Step Guide to Placement of the LAP-BAND Adjustable Gastric Banding System
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Laparoscopic Nissen Fundoplication Description
OhioHealth Mansfield Laparoscopic Nissen Fundoplication Laparoscopic Nissen Fundoplication is a surgical procedure intended to cure Esophagus gastroesophageal reflux disease (GERD). Reflux disease is a disorder of the lower esophageal sphincter (the circular muscle at the base of the esophagus that serves as a barrier between the esophagus and stomach). When the LES malfunctions, acidic stomach contents are able to inappropriately reflux into the esophagus causing undesirable symptoms. The laparoscopic Nissen Esophageal Fundoplication involves wrapping a small portion of the stomach around the sphincter junction between the esophagus and stomach to augment the function of the Tightened LES. The operation effectively cures GERD with recurrence rates ranging from hiatus 5-10 percent over the life of the patient. Patients who experience a recurrence can be treated medically or undergo a redo laparoscopic Nissen Fundoplication. The most common postoperative side effect of a laparoscopic Nissen Fundoplication is gas bloating. A small percentage of patients (10-20 percent) will not be able to belch or vomit after surgery. Some patients may experience temporary difficult swallowing after surgery. Some patients may experience intermittent episodes of “dumping syndrome” due to Vagus nerve irritation or Top of stomach being excessive acid production in the stomach. wrapped around esophagus Patients are typically on a modified diet for a few weeks after surgery to allow time for healing of the surgical repair and recovery of the function of the esophagus and stomach. Top of stomach fully wrapped around esophagus and sutured Nissen fundoplication © OhioHealth Inc. 2018. All rights reserved. Laparoscopic. 05/18.. -

Adjustable Gastric Banding
7 Review Article Page 1 of 7 Adjustable gastric banding Emre Gundogdu, Munevver Moran Department of Surgery, Medical School, Istinye University, Istanbul, Turkey Contributions: (I) Conception and design: All authors; (II) Administrative support: All authors; (III) Provision of study materials or patients: All authors; (IV) Collection and assembly of data: All authors; (V) Data analysis and interpretation: All authors; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Emre Gündoğdu, MD, FEBS. Assistant Professor of Surgery, Department of Surgery, Medical School, Istinye University, Istanbul, Turkey. Email: [email protected]; [email protected]. Abstract: Gastric banding is based on the principle of forming a small volume pouch near the stomach by wrapping the fundus with various synthetic grafts. The main purpose is to limit oral intake. Due to the fact that it is a reversible surgery, ease of application and early results, the adjustable gastric band (AGB) operation has become common practice for the last 20 years. Many studies have shown that the effectiveness of LAGB has comparable results with other procedures in providing weight loss. Early studies have shown that short term complications after LAGB are particularly low when compared to the other complicated procedures. Even compared to RYGB and LSG, short-term results of LAGB have been shown to be significantly superior. However, as long-term results began to emerge, such as failure in weight loss, increased weight regain and long-term complication rates, interest in the procedure disappeared. The rate of revisional operations after LAGB is rapidly increasing today and many surgeons prefer to convert it to another bariatric procedure, such as RYGB or LSG, for revision surgery in patients with band removed after LAGB. -

OBESITY SURGERY: INDICATIONS, TECHNIQUES, WEIGHTLOSS and POSSIBLE COMPLICATIONS - Review Article
REFERENCES: 1. Makauchi M, Mori T, Gunven P, et 3. Belghiti J, Noun R, Malafosse R, et T, Sauvanet A. Portal triad clamping or al. Safety of hemihepatic vascular occlusion al. Continuous versus intermittent portal hepatic vascular exclusion for major liver during resection of the liver. Surg Gynecol triad clamping for liver resection. A resection. A controlled study. Ann Surg. Obstet 1989; 130:824–831. controlled study. Ann Surg 1999; 229:369 1996 Aug; 224(2):155-61 2. Wobbes T, Bemelmans BLH, –375. 6. PE Clavien, S Yadav, d. Syndram, R. Kuypers JHC, et al. Risk of postoperative 4. J.R. Hiatt J.Gabbay,R W. Busuttil. Bently. Protective Effects of Ischemic septic complications after abdominal Surgical Anatomy of the Hepatic Arteries Preconditioning for Liver Resection surgery treatment in relation to in 1000 Cases. Ann Surg.1994 Vol. 220, Performed Under Inflow Occlusion in preoperative blood transfusion. Surg No. 1, 50-52 Humans. Ann Surg Vol. 232, No. 2, 155– Gynecol Obstet 1990; 171: 5. Belghiti J, Noun R, Zante E, Ballet 162 Corresponding author: Ludmil Marinov Veltchev, MD PhD Mobile: +359 876 259 685 E-mail: [email protected] Journal of IMAB - Annual Proceeding (Scientific Papers) 2009, book 1 OBESITY SURGERY: INDICATIONS, TECHNIQUES, WEIGHTLOSS AND POSSIBLE COMPLICATIONS - Review article Ludmil M. Veltchev Fellow, Master’s Program in Hepatobiliary Pancreatic Surgery, Henri Bismuth Hepatobiliary Institute, 12-14, avenue Paul Vaillant-Couturier, 94804 Villejuif Cedex SUMMARY type of treatment is the only one leading to a lasting effect. In long-term perspective, the conservative treatment Basically, two mechanisms allow the unification of all of obesity is always doomed to failure and only the surgical known methods into three categories: method allows reducing obesity. -

Nissen Fundoplication & Hiatal Hernia Repairs
Post-Operative Instructions Laparoscopic Nissen Fundoplication (or Hiatal Hernia Repair) Description of the Operation We will be doing a laparoscopic Nissen (or Toupet) fundoplication for you. Any hiatal hernia will also be repaired at the time of surgery. A fundoplication involves wrapping a portion of your stomach around your esophagus. This creates a valve-like mechanism to stop reflux of stomach juices into your esophagus (and to prevent a hiatal hernia from recurring). We’ll close your skin with tiny pieces of tape or transparent glue. Be prepared to spend one night in the hospital, although you might not need to, depending on how you feel after surgery. Your Recovery Vigorous straining (or prolonged vomiting) too soon after surgery can damage your diaphragm muscle before the stitches in it have had a chance to heal. This can cause your stomach to move out of position (a hiatal hernia) and the operation to fail or even require re-operation. Almost everybody experiences constant, dull chest, neck or shoulder discomfort when waking up from surgery. It usually fades within a day or two, sometimes longer. Because your operation will be performed laparoscopically, your discomfort will probably resolve before your diaphragm has finished healing. You should avoid heavy-lifting and any activity that causes you to strain and “get red in the face” for at least a month to let the diaphragm heal. You should be able to return to work or usual activities (except for the heavy-lifting) within a few days to a few weeks, depending on the activities. You may resume showering the day after surgery. -

Medical Policy Bariatric Surgery
Medical Policy Bariatric Surgery Subject: Bariatric Surgery Background: Morbid obesity (also called clinically severe obesity) is a serious health condition that can interfere with basic physical functions such as breathing or walking and reduce life expectancy. Individuals who are morbidly obese are at greater risk for serious medical complications including hypertension, coronary artery disease, type 2 diabetes mellitus, sleep apnea, gastroesophageal reflux disease and osteoarthritis. While the immediate cause of obesity is caloric intake that persistently exceeds caloric output, a limited number of cases may also be caused by illnesses such as hypothyroidism, Cushing's disease, and hypothalamic lesions. Nonsurgical strategies for achieving weight loss and weight maintenance (e.g., caloric restriction, increased physical activity, behavioral modification) are recommended for most overweight and obese persons. Bariatric (weight loss) surgery is a major surgical intervention and is indicated for adults and adolescents who have completed bone growth and are morbidly obese. Bariatric surgery procedures modify the anatomy of the gastrointestinal tract and cause weight loss by restricting the amount of food the stomach can hold, causing malabsorption of nutrients. Bariatric procedures can often cause hormonal and metabolic changes that result from gastric and intestinal surgery. Contraindications for bariatric surgeries include cardiac complications, significant respiratory dysfunction, non- compliance with medical treatment, psychological disorders that a psychologist/psychiatrist determines are likely to exacerbate or interfere with long-term management, significant eating disorders, and severe hiatal hernia/gastroesophageal reflux. Authorization: Prior authorization is required for bariatric surgeries provided to members enrolled in commercial (HMO, POS, PPO) products. Bariatric procedures can only be done at fully accredited centers. -

Gastroparesis and Dumping Syndrome: Current Concepts and Management
Journal of Clinical Medicine Review Gastroparesis and Dumping Syndrome: Current Concepts and Management Stephan R. Vavricka 1,2,* and Thomas Greuter 2 1 Center of Gastroenterology and Hepatology, CH-8048 Zurich, Switzerland 2 Department of Gastroenterology and Hepatology, University Hospital Zurich, CH-8091 Zurich, Switzerland * Correspondence: [email protected] Received: 21 June 2019; Accepted: 23 July 2019; Published: 29 July 2019 Abstract: Gastroparesis and dumping syndrome both evolve from a disturbed gastric emptying mechanism. Although gastroparesis results from delayed gastric emptying and dumping syndrome from accelerated emptying of the stomach, the two entities share several similarities among which are an underestimated prevalence, considerable impairment of quality of life, the need for a multidisciplinary team setting, and a step-up treatment approach. In the following review, we will present an overview of the most important clinical aspects of gastroparesis and dumping syndrome including epidemiology, pathophysiology, presentation, and diagnostics. Finally, we highlight promising therapeutic options that might be available in the future. Keywords: gastroparesis; dumping syndrome; pathophysiology; clinical presentation; treatment 1. Introduction Gastroparesis and dumping syndrome both evolve from a disturbed gastric emptying mechanism. While gastroparesis results from significantly delayed gastric emptying, dumping syndrome is a consequence of increased flux of food into the small bowel [1,2]. The two entities share several important similarities: (i) gastroparesis and dumping syndrome are frequent, but also frequently overlooked; (ii) they affect patient’s quality of life considerably due to possibly debilitating symptoms; (iii) patients should be taken care of within a multidisciplinary team setting; and (iv) treatment should follow a step-up approach from dietary modifications and patient education to pharmacological interventions and, finally, surgical procedures and/or enteral feeding. -

Laparoscopic Adjustable Gastric Band As a Revision Surgery for Failed Vertical Gastric Sleeve Or Roux-En-Y Gastric Bypass
Lincey Alexida, Xiaohua Qi, Patrick B. Asdell, José M. Martínez Landrón, Samarth B. Patel, Faustino Allongo. Frederick Tiesenga. Laparoscopic Adjustable Gastric Band as a Revision Surgery for Failed Vertical Gastric Sleeve or Roux-en-Y Gastric Bypass. IAIM, 2017; 4(12): 37-42. Original Research Article Laparoscopic Adjustable Gastric Band as a Revision Surgery for Failed Vertical Gastric Sleeve or Roux-en-Y Gastric Bypass Lincey Alexida1*, Xiaohua Qi2, Patrick B. Asdell3, José M. Martínez Landrón4, Samarth B. Patel5, Faustino Allongo6, Frederick Tiesenga7 14th year Medical Student, Saint James School of Medicine, 1480 Renaissance Drive, Suite 300, Park Ridge, IL 60068, USA 23rd year Medical Student, Saint James School of Medicine, 1480 Renaissance Drive, Suite 300, Park Ridge, IL 60068, USA 33rd year Medical Student, Saint James School of Medicine, 1480 Renaissance Drive, Suite 300, Park Ridge, IL 60068, USA 44th year Medical Student, American University of St. Vincent, 17950 Preston Rd #420, Dallas, TX 75252 53rd year medical student, Saint James School of Medicine, 1480 Renaissance Drive, Suite 300, Park Ridge, IL 60068, USA 63rd year medical student, Windsor University School of Medicine, 332 S Austin Blvd #2E, Oak Park Il, 60304 7 Medical Doctor, Department of Surgery, West Suburban Medical Center, 1950 N Harlem Ave, Elmwood Park, IL 60707, USA *Corresponding author email: [email protected] International Archives of Integrated Medicine, Vol. 4, Issue 12, December, 2017. Copy right © 2017, IAIM, All Rights Reserved. Available online at http://iaimjournal.com/ ISSN: 2394-0026 (P) ISSN: 2394-0034 (O) Received on: 02-11-2017 Accepted on: 16-11-2017 Source of support: Nil Conflict of interest: None declared. -

Laparoscopic Surgery for Gastro-Esophageal Acid Reflux
Best Practice & Research Clinical Gastroenterology 28 (2014) 97–109 Contents lists available at ScienceDirect Best Practice & Research Clinical Gastroenterology 8 Laparoscopic surgery for gastro-esophageal acid reflux disease Marlies P. Schijven, MD, PhD, MHSc, Assistant Professor of Surgery *, Suzanne S. Gisbertz, MD, PhD, Assistant Professor of Surgery, Mark I. van Berge Henegouwen, MD, PhD, Assistant Professor of Surgery Department of Surgery, Academic Medical Centre, PO Box 22660, 1100 DD Amsterdam, The Netherlands abstract Keywords: Systematic review Gastro-esophageal reflux disease is a troublesome disease for Reflux many patients, severely affecting their quality of life. Choice of Toupet treatment depends on a combination of patient characteristics and Nissen fl GERD preferences, esophageal motility and damage of re ux, symptom GORD severity and symptom correlation to acid reflux and physician Gastro-esophageal reflux disease preferences. Success of treatment depends on tailoring treatment Endoluminal modalities to the individual patient and adequate selection of Fundoplication treatment choice. PubMed, Embase, The Cochrane Database of Laparoscopy Systematic Reviews, and the Cumulative Index to Nursing and Proton pump inhibitors Allied Health Literature (CINAHL) were searched for systematic Anti-reflux procedures reviews with an abstract, publication date within the last five years, in humans only, on key terms (laparosc* OR laparoscopy*) AND (fundoplication OR reflux* OR GORD OR GERD OR nissen OR toupet) NOT (achal* OR pediat*). Last search was performed on July 23nd and in total 54 articles were evaluated as relevant from this search. The laparoscopic Toupet fundoplication is the therapy of choice for normal-weight GERD patients qualifying for laparo- scopic surgery. No better pharmaceutical, endoluminal or surgical alternatives are present to date. -

Gastrocolic Fistulae
View metadata, citation and similar papers at core.ac.uk REVIEW brought to you by CORE provided by Elsevier - Publisher Connector International Journal of Surgery 10 (2012) 129e133 Contents lists available at SciVerse ScienceDirect International Journal of Surgery journal homepage: www.theijs.com Review Gastrocolic fistulae; From Haller till nowadays Michael Stamatakos a,*, Ioannis Karaiskos b, Ioannis Pateras b, Ioannis Alexiou c, Charikleia Stefanaki d, Konstantinos Kontzoglou c a Generasl Surgeon, N. Athinaion M.D., Hospital, Athens, Greece b 1st Department of Surgery, Medical School, University of Athens, Laikon General Hospital, Athens, Greece c 2nd Department of Propaedeutic Surgery, Medical School, University of Athens, Laikon General Hospital, Athens, Greece d Medic. Athens, Greece article info abstract Article history: Gastrocolic Fistula is, in the majority of cases the pathological communication between stomach and Received 5 April 2011 transverse colon, because cases involved with the small intestine, pancreas and skin have been also Received in revised form documented, even though are rare. It occurs mostly in adults, but they can be present to infants, as well, as 14 February 2012 a result of congenital abnormalities or iatrogenic procedures (i.e. migration of PEG tube that placed before). Accepted 15 February 2012 In the Western Countries, the most common cause is the adenocarcinoma of the colon, while in Japan, Available online 20 February 2012 adenocarcinoma of the stomach is the most frequent cause. It seldom appears, as a complication of a benign peptic ulcer, in Crohn’s disease and as a result of significant intake of steroids or NSAIDs. Keywords: fi Gastrocolic fistula The typical symptoms of a gastrocolic stula are abdominal pain, nausea-vomiting, diarrhea and Colocutaneous fistula weight loss. -

TAR and Non-Benefit List: Codes 40000 Thru 49999 Page Updated: January 2021
tar and non cd4 1 TAR and Non-Benefit List: Codes 40000 thru 49999 Page updated: January 2021 Surgery Digestive System Note: Refer to the TAR and Non-Benefit: Introduction to List in this manual for more information about the categories of benefit restrictions. Lips Excision Code Description Benefit Restrictions 40490 Biopsy of lip Assistant Surgeon services not payable Other Procedures Code Description Benefit Restrictions 40799 Unlisted procedure, lips Requires TAR, Primary Surgeon/ Provider Vestibule of Mouth Incision Code Description Benefit Restrictions 40800 Drainage of abscess/cyst, mouth, simple Assistant Surgeon services not payable 40801 Drainage of abscess/cyst, mouth, complicated Assistant Surgeon services not payable 40804 Removal of embedded foreign body, mouth, simple Assistant Surgeon services not payable 40805 Removal of embedded foreign body, mouth, Assistant Surgeon complicated services not payable 40806 Incision labial frenum Non-Benefit Excision Code Description Benefit Restrictions 40808 Biopsy, vestibule of mouth Assistant Surgeon services not payable 40810 Excision of lesion mucosa/submucosa, mouth, without Non-Benefit repair Part 2 – TAR and Non-Benefit List: Codes 40000 thru 49999 tar and non cd4 2 Page updated: January 2021 Excision (continued) Code Description Benefit Restrictions 40812 Excision of lesion mucosa/submucosa, mouth, simple Assistant Surgeon repair services not payable 40816 Excision of lesion, mouth, mucosa/submucosa, Assistant Surgeon complex services not payable 40819 Excision of frenum, labial -
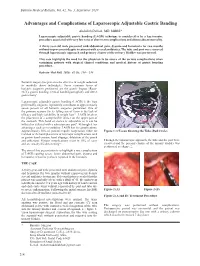
Advantages and Complications of Laparoscopic Adjustable Gastric Banding
Bahrain Medical Bulletin, Vol. 42, No. 3, September 2020 Advantages and Complications of Laparoscopic Adjustable Gastric Banding Abdullah Dalboh, MD, MBBS* Laparoscopic adjustable gastric banding (LAGB) technique is considered to be a less invasive procedure associated with very low rates of short-term complications and almost absent mortality. A thirty-year-old male presented with abdominal pain, dysuria and hematuria for two months without improvement despite treatment with several antibiotics. The tube and port were removed through laparoscopic approach and primary closure of the urinary bladder was performed. This case highlights the need for the physician to be aware of the serious complications when examining patients with atypical clinical conditions and medical history of gastric banding procedure. Bahrain Med Bull 2020; 42 (3): 214 - 215 Bariatric surgery has proven to be effective in weight reduction in morbidly obese individuals. Some common forms of bariatric surgeries performed are the gastric bypass (Roux- en-Y), gastric banding, vertical banded gastroplasty and sleeve gastrectomy1. Laparoscopic adjustable gastric banding (LAGB) is the least preferred by surgeons; it presently contributes to approximately seven percent of all bariatric surgeries performed. One of the primary reasons for its falling out of favor is the lack of efficacy and high variability in weight loss2,3. LAGB involves the placement of a compressible device on the upper part of the stomach. This band or device is adjustable as it can be inflated or deflated with a subcutaneous port4. Although it has advantages such as reversibility, LAGB has its complications. Approximately 50% of patients require reoperation either for Figure 1: CT-scan Showing the Tube (Red Circle) revision of the band placement or for major complications such as gastric band erosion, band slippage, dilatation of the pouch and adhesions. -

Maestro Rechargeable System
® Maestro Rechargeable System Instructions for Use CAUTION: Federal Law restricts this device to sale by or on the order of a physician. Copyright 2015 by EnteroMedics Inc., St. Paul, Minnesota All rights reserved EnteroMedics, VBLOC and Maestro are registered trademarks of EnteroMedics Inc. The Maestro System is protected under U.S., European, Japanese and Australian Patents, and patent applications. Subject to Pat. Nos.: AU2004209978; AU2009245845; AU2006280277; AU2006280278; AU2008226689; AU2008259917; AU2011265519; US 7,167,750; US 7,672,727; US 7,822,486; US 7,917,226; US 8,010,204; US 8,068,918; US 8,103,349; US 8,140,167; US 8,483,830; US 8,483,838; US 8,521,299; US 8,532,787; US 8,538,542; US 8,825,164; JP 5486588; EP 1601414; EP 1603634; EP 1922109; and EP1922111 For use in a method covered by Pat. Nos.: AU2009231601; US 7,489,969; US 7,729,771; US 7,613,515; US 7,844,338; US 8,046,085; US 8,538,533 Maestro® Rechargeable System P01392-001 Rev J System Instructions for Use Table of Contents 1. INDICATIONS FOR USE .................................................................................................................... 4 2. CONTRAINDICATIONS ..................................................................................................................... 5 3. WARNINGS ..................................................................................................................................... 6 4. PRECAUTIONS ................................................................................................................................