Elements of Suffering in Myalgic Encephalomyelitis/Chronic
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

How to Talk with Your Family About Sjögren's LETTER from SSF CEO
Volume 32, Issue 10 November/December 2014 SjogrensSyndromeFoundation @MoistureSeekers LETTER FROM SSF CEO STEVEN TAYLOR his is the time of the year that we at the Sjögren’s Syndrome Foun- dation look back and give thanks to all of you who have supported Tus throughout the year! Thanks to your generous support, the SSF has continued to soar to new heights as we strive to conquer Sjögren’s. Patient care continues to be a focus of the SSF. With the develop- ment of the SSF’s Clinical Practice Guidelines for Sjögren’s, patients will eventually see standardized care in how healthcare providers treat, manage and monitor their Sjögren’s patients. This initiative marks the first time in the history of the disease that a roadmap for treating Sjögren’s has been developed. The SSF is proud to be the lead organization to make this happen for all Sjögren’s patients, and we couldn’t do it without the support of hundreds of healthcare profes- sionals who, along with the SSF staff, are researching the evidence, discussing the best continued page 2 t How to Talk With Your Family about Sjögren’s here is a growing body of evidence that rich social support networks are Timportant to overall health, immune function and healing. They improve quality of life and facilitate coping with chronic illness. Conversely, negative social interac- tions create a stress response that have the opposite effect. Support from family members and close friends can be one of the most important resources for you to draw on when dealing with Sjögren’s. -

Health by Numbers the Economic Burden of Preventable Chronic
HEALTH BY NUMBERS PUBLIC HEALTH MICHAEL FINE, MD DIRECTOR, RHODE ISLAND DEPARTMENT OF HEALTH EDITED BY SAMARA VINER-BROWN, MS The Economic Burden of Preventable Chronic Diseases in Rhode Island DEBORAH N. PEARLMAN, PhD; DARREN KAW, MPH; SOPHIE O’CONNELL, MA; YONGWEN JIANG, PhD; DONA GOLDMAN, RN, MPH 36 39 EN The Centers for Disease Control and Prevention (CDC) have a myocardial infarction; (2) coronary artery disease; (3) a identified seven chronic conditions where a comprehensive stroke; (4) asthma; (5) arthritis (defined in this questionnaire approach to prevention could save tremendous health care as rheumatoid arthritis, gout, lupus, or fibromyalgia); (6) dia- costs and reduce premature disability and death in the US. betes; and 7) high blood pressure. Adults ever diagnosed with These potentially “preventable” chronic diseases include asthma were asked if they still had asthma (current asthma). heart disease, stroke, some cancers, diabetes, arthritis,1 and The presence or absence of each condition was determined asthma.2 by a “yes” or “no” response, respectively. Women reporting In 2014, the Milken Institute study estimated the impact diabetes or high blood pressure only when pregnant were on the US economy of seven chronic diseases – cancer, excluded from these respective variables. diabetes, hypertension, stroke, heart disease, pulmonary Cardiovascular disease was based on a “yes” response to conditions, and mental illness – at $1.3 trillion annually.3 having one or more of the following diagnosed conditions: Projected costs were $28 billion more than that forecast in high blood pressure, myocardial infarction, coronary artery 2007.4 The leading drivers of health care costs were increas- disease, or a stroke. -

Seizures in Encephalitis
Neurology Asia 2008; 13 : 1 – 13 REVIEW ARTICLES Seizures in encephalitis Usha Kant Misra DM, *C T Tan MD, Jayantee Kalita DM Department of Neurology, Sanjay Gandhi PGIMS, Lucknow, India; *Department of Medicine, University of Malaya, Kuala Lumpur, Malaysia Abstract A large number of viruses can result in encephalitis. However, certain viruses are more prevalent in certain geographical regions. For example, Japanese encephalitis (JE) and dengue in South East Asia and West Nile in Middle East whereas Herpes simplex encephalitis (HSE) occurs all over the world without any seasonal or regional variation. Encephalitis can result in acute symptomatic seizures and remote symptomatic epilepsy. Risk of seizures after 20 years is 22% following encephalitis and 3% after meningitis with early seizures. Amongst the viruses, HSE is associated with most frequent and severe epilepsy. Seizures may be presenting feature in 50% because of involvement of highly epileptogenic frontotemporal cortex. Presence of seizures in HSE is associated with poor prognosis. HSE can also result in chronic and relapsing form of encephalitis and may be an aetiology factor in drug resistant epilepsy. Amongst the Flaviviruses, Japanese encephalitis is the most common and is associated with seizures especially in children. The frequency of seizures in JE is reported to be 6.9% to 46%. Associated neurocysticercosis in JE patients may aggravate the frequency and severity of seizures. Other flaviviruses such as equine, St Louis, and West Nile encephalitis can also produce seizures. In Nipah encephalitis, seizures are commoner in relapsed and late-onset encephalitis as compared to acute encephalitis (50% vs 24%). Other viruses like measles, varicella, mumps, influenza and enteroviruses may result in encephalitis and seizures. -

Progressive Multifocal Leukoencephalopathy and the Spectrum of JC Virus-Related Disease
REVIEWS Progressive multifocal leukoencephalopathy and the spectrum of JC virus- related disease Irene Cortese 1 ✉ , Daniel S. Reich 2 and Avindra Nath3 Abstract | Progressive multifocal leukoencephalopathy (PML) is a devastating CNS infection caused by JC virus (JCV), a polyomavirus that commonly establishes persistent, asymptomatic infection in the general population. Emerging evidence that PML can be ameliorated with novel immunotherapeutic approaches calls for reassessment of PML pathophysiology and clinical course. PML results from JCV reactivation in the setting of impaired cellular immunity, and no antiviral therapies are available, so survival depends on reversal of the underlying immunosuppression. Antiretroviral therapies greatly reduce the risk of HIV-related PML, but many modern treatments for cancers, organ transplantation and chronic inflammatory disease cause immunosuppression that can be difficult to reverse. These treatments — most notably natalizumab for multiple sclerosis — have led to a surge of iatrogenic PML. The spectrum of presentations of JCV- related disease has evolved over time and may challenge current diagnostic criteria. Immunotherapeutic interventions, such as use of checkpoint inhibitors and adoptive T cell transfer, have shown promise but caution is needed in the management of immune reconstitution inflammatory syndrome, an exuberant immune response that can contribute to morbidity and death. Many people who survive PML are left with neurological sequelae and some with persistent, low-level viral replication in the CNS. As the number of people who survive PML increases, this lack of viral clearance could create challenges in the subsequent management of some underlying diseases. Progressive multifocal leukoencephalopathy (PML) is for multiple sclerosis. Taken together, HIV, lymphopro- a rare, debilitating and often fatal disease of the CNS liferative disease and multiple sclerosis account for the caused by JC virus (JCV). -

Encephalitis Fact Sheet
Encephalitis Fact Sheet What is encephalitis? Encephalitis is an inflammation (irritation and swelling) of the brain tissue. It can occur as a primary illness or as a result of another illness elsewhere in the body. Frequently caused by an infection with a virus, encephalitis can be mild or severe, but severe cases are rare. Who gets encephalitis? Anyone can get encephalitis, but young children, older adults, and persons with weakened immune systems are more at risk. How is encephalitis spread? Primary encephalitis occurs when a virus directly infects the brain. Viruses that are carried by infected mosquitoes and ticks can cause primary encephalitis. Other viruses can cause an illness and then encephalitis can develop as a complication of the viral illness. When encephalitis develops after another infection, it is called post-infectious encephalitis. Post-infectious encephalitis most commonly follows a bout of chickenpox, mumps, or measles. What are the symptoms of encephalitis? Encephalitis frequently causes headache, fever, confused thinking, seizures, or problems with vision, speech, or movement. Infants and young children might have nausea, vomiting, body stiffness, constant crying, and poor feeding. How soon after exposure do symptoms appear? Encephalitis can occur within two to three weeks after a viral illness. Symptoms begin within a few days to one or two weeks after the bite from an infected mosquito. How is encephalitis diagnosed? Medical evaluation and special tests are needed to confirm the diagnosis. Anyone with a severe headache, fever, and altered mental status should seek medical care immediately. What is the treatment for encephalitis? Doctors might prescribe antiviral drugs, anti-inflammatory drugs, or other treatments for the symptoms as needed. -
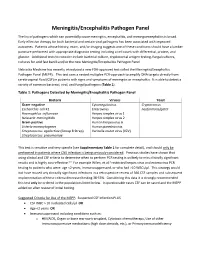
Meningitis/Encephalitis Pathogen Panel
Meningitis/Encephalitis Pathogen Panel The list of pathogens which can potentially cause meningitis, encephalitis, and meningoencephalitis is broad. Early effective therapy for both bacterial and certain viral pathogens has been associated with improved outcomes. Patients whose history, exam, and/or imaging suggests one of these conditions should have a lumber puncture performed with appropriate diagnostic testing including a cell count with differential, protein, and glucose. Additional tests to consider include bacterial culture, cryptococcal antigen testing, fungal cultures, cultures for acid fast bacilli and/or the new Meningitis/Encephalitis Pathogen Panel. Nebraska Medicine has recently introduced a new FDA-approved test called the Meningitis/Encephalitis Pathogen Panel (MEPP). This test uses a nested multiplex PCR-approach to amplify DNA targets directly from cerebrospinal fluid (CSF) in patients with signs and symptoms of meningitis or encephalitis. It is able to detect a variety of common bacterial, viral, and fungal pathogens (Table 1). Table 1: Pathogens Detected by Meningitis/Encephalitis Pathogen Panel Bacteria Viruses Yeast Gram-negative Cytomegalovirus Cryptococcus Escherichia coli K1 Enterovirus neoformans/gattii Haemophilus influenzae Herpes simplex virus 1 Neisseria meningitidis Herpes simplex virus 2 Gram-positive Human herpesvirus 6 Listeria monocytogenes Human parechovirus Streptococcus agalactiae (Group B Strep) Varicella zoster virus (VZV) Streptococcus pneumoniae This test is sensitive and very specific (see Supplementary Table 1 for complete detail), and should only be performed in patients where CNS infection is being seriously considered. Previous studies have shown that using clinical and CSF criteria to determine when to perform PCR testing is unlikely to miss clinically significant results and is highly cost-effective.1-3 For example Wilen, et al.3 restricted herpes virus and enterovirus PCR testing to patients who were: age <2 years, immunosuppressed, or who had >10 WBCs/µl. -

Digital Medicine's March on Chronic Disease
RE-IMAGINING MEDICINE COMMENTARY Digital medicine’s march on chronic disease Joseph C Kvedar, Alexander L Fogel, Eric Elenko & Daphne Zohar Digital medicine offers the possibility of continuous monitoring, behavior modification and personalized interventions at low cost, potentially easing the burden of chronic disease in cost-constrained healthcare systems. hronic disease affects approximately half surgeries—successfully addressed leading well as 86% of healthcare costs3–5. The United Cof all adult Americans, accounting for at causes of morbidity and mortality of the time States has the highest disease burden of any least seven of the ten leading causes of death (Table 1)1. In contrast, the most pressing issues developed country6. Trends in the above data and 86% of all healthcare spending. The US facing healthcare in the twenty-first century are expected to worsen in the near future. The healthcare system is ill-equipped to handle our are chronic diseases (e.g., respiratory disor- growth in chronic disease prevalence means epidemic of chronic disease. This is because ders, heart disease and diabetes), and many are that, despite increases in average life span, we most chronic disorders develop outside preventable (e.g., through smoking cessation may be experiencing a decrease in average healthcare settings, and patients with these and diet; Table 1; Fig. 1)2. The increase in the health span (the period of a person’s life spent conditions require continuous intervention prevalence of chronic disease is the primary in generally good health)7. to make the behavioral and lifestyle changes contributor to skyrocketing healthcare costs Why are we continuing to lose ground needed to effectively manage disease. -

The Lonely, Isolating, and Alienating Implications of Myalgic Encephalomyelitis/Chronic Fatigue Syndrome
healthcare Review The Lonely, Isolating, and Alienating Implications of Myalgic Encephalomyelitis/Chronic Fatigue Syndrome Samir Boulazreg 1,* and Ami Rokach 2 1 Faculty of Education, University of Western Ontario, London, ON N6A 3K7, Canada 2 Department of Psychology, York University, Toronto, ON M3J 1P3, Canada; [email protected] * Correspondence: [email protected] Received: 17 July 2020; Accepted: 11 October 2020; Published: 20 October 2020 Abstract: This article provides a narrative review on myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) through a psychosocial lens and examines how this impairment affects its sufferers during adolescence and adulthood, as well as how it impacts family caregivers and healthcare professionals’ mental health. Since there has been a lack of investigation in the literature, the primary psychosocial stressor that this review focuses on is loneliness. As such, and in an attempt to help establish a theoretical framework regarding how loneliness may impact ME/CFS, loneliness is comprehensively reviewed, and its relation to chronic illness is described. We conclude by discussing a variety of coping strategies that may be employed by ME/CFS individuals to address their loneliness. Future directions and ways with which the literature may investigate loneliness and ME/CFS are discussed. Keywords: myalgic encephalomyelitis; chronic fatigue syndrome; loneliness; psychosocial 1. The Lonely, Isolating, and Alienating Implications of ME/CFS Myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) is a debilitating neurological disorder known to produce a wide range of devastating symptoms best known to include extreme fatigue, pain, and post-exertional discomfort. Though it is thought to originate from a genetic predisposition and/or an interaction with a host of environmental factors (e.g., frequent injury), the exact precursors of this disorder are still not well-understood [1]. -

Mental Health and Chronic Diseases CDC Fact Sheet
Mental Health and Chronic Diseases Issue Brief No. 2 October 2012 Background Chronic diseases are non-communicable illnesses that are prolonged in duration, do not resolve spontaneously, and are rarely cured completely. They are the leading cause of death and disability in the United States. They cause 7 out of 10 deaths each year and are among the most preventable and treatable of all health problems (see figure below). Chronic diseases include illness such as heart disease, diabetes, cancer, and arthritis.1 Mental health disorders are medical conditions that disrupt a person's thinking, feeling, mood, ability to relate to others and daily functioning. They are medical conditions that often result in a reduced ability to cope with the routine daily activities such as going to work or raising a family. Just like chronic diseases, mental health disorders are treatable. Most people diagnosed with a serious mental health disorder can receive relief from their symptoms by following a treatment plan specifically designed for them by a trained psychologist or psychiatrist. Mental health disorders are not exclusive to those who exhibit a lack of personal strength, personality traits like being shy, or have a certain socioeconomic status. Mental health disorders include illnesses such as major depression, bipolar disorder, obsessive compulsive disorder, and post-traumatic stress disorder. One common finding is that people who suffer from a chronic disease are more likely to also suffer from depression.2 Scientists have yet to determine if having a chronic disease increases the prevalence of depression or depression increases the risk of obtaining a chronic disease. -

Chronic Health Issues
14925 Chronic Health 9/24/04 2:59 PM Page C4 Chronic Health Issues 745 Fifth Avenue, Suite 900 601 E Street, NW New York, NY 10151 Washington, DC 20049 www.dana.org www.aarp.org/nrta D17457(804) 14925 Chronic Health 9/24/04 2:59 PM Page ii f you are living with a chronic health condition, Iyou’re not alone. By some estimates, half of all Americans — 125 million people — suffer from at least one chronic condition. Almost one in four people live with more than one illness. Chronic, by definition, means long-lasting or recurring. Examples of NRTA: AARP’s Educator Community common chronic health conditions include arthritis, cancer, diabetes, Alzheimer’s disease, depression, and heart disease. This pamphlet NRTA (www.aarp.org/nrta) is AARP’s educator community. Consistent with AARP’s mission, NRTA is dedicated to enhancing the quality of life for all as we age, specifically focuses on chronic brain-related disorders, but the general guidelines through a focus on education and learning. NRTA works for positive social change in the provided may apply to any chronic condition. field of education and provides members with valuable information, advocacy, and service initiatives related to learning and education. NRTA provides national leadership through its network of affiliated retired educators’ associations in 50 states and 2,700 communities and For more than one third of Americans — some 40 million people — through its national office at the AARP headquarters in Washington, D.C. The partnership chronic illness takes the form of a brain disorder. These disorders are with the Dana Alliance for Brain Initiatives, and the Staying Sharp initiative, recognizes and explores the intimate connection between the brain, human behavior, and the ability to most commonly the result of damage to brain tissues (such as in stroke continue to learn throughout life. -

Everyday Healthy Living
Everyday Healthy Living Do you or someone in your family live with a chronic condition? Chronic diseases—such as heart disease, stroke, cancer, diabetes, asthma, and arthritis—are among the most common, costly, and preventable of all health problems in the U.S. Most households are affected by at least one chronic condition. Manage Risks With Self-Care and Lifestyle Change Daily self-care regimens and healthy lifestyle changes are essential to living with a chronic condition. From diet and physical activity to medications, self-monitoring, and other recommendations, managing chronic conditions requires a comprehensive approach to live longer, healthier and more fulfilling lives. And perhaps, healthy living is the best revenge! Living a healthy lifestyle—to either manage or prevent chronic conditions—has been shown to have significant health and economic values. A recent study showed conclusively that you could reduce your risk of diabetes, heart attack, stroke, or cancer by 80% if you would just do 4 things: Engage in regular physical activity. Not smoke. Eat a healthy diet. Avoid becoming obese. Chronic diseases are costly to individuals, families, and companies. The Centers for Disease Control and Prevention report that chronic diseases account for 75% of health care spending. According to over 114,000 members who took the Highmark Wellness Profile in 2010, 14% reported having one or two chronic conditions, costing an estimated $31,468,704 ($1,965 per person) in lost productivity (the more chronic conditions, the less productivity.) Self-care and lifestyle change can help control this alarming and costly trend. Know A Few Facts About Chronic Conditions • FACT: 7 OUT OF 10 deaths among Americans each year are from chronic diseases. -

14 Glossary of Healthcare Terms
Premera Reference Manual Premera Blue Cross 1144 GGlloossssaarryy ooff HHeeaalltthhccaarree TTeerrmmss A Accreditation: Health plan accreditation is a rigorous, comprehensive and transparent evaluation process through which the quality of the systems, processes and results that define a health plan are assessed. Acute: A condition that begins suddenly and does not last very long (e.g., broken arm). ‘acute” is the opposite of “chronic.” Acute Care: Treatment for a short-term or episodic illness or health problem. Adequacy: The extent to which a network offers the appropriate types and numbers of providers in a designated geographic distribution according to the relative availability of such providers in the area and the needs of the plan's members. Adjudication: The process of handling and paying claims. Also see Claim. Admission Notification: Hospitals routinely notify Premera of all inpatient admissions that link members to other care coordination programs, such as readmission prevention. The process includes verification of benefits and assesses any need for case management. Advance Directives: Written instructions that describe a member’s healthcare decision regarding treatment in the event of a serious medical condition which prevents the member from communicating with his/her physician; also called Living Wills. Allied Health Personnel: Specially trained and licensed (when necessary) healthcare workers other than physicians, optometrists, dentists, chiropractors, podiatrists, and nurses. Allowable: An amount agreed upon by the carrier and the practitioner as payment for covered services. Alpha Prefix: Three characters preceding the subscriber identification number on Blue Cross and/or Blue Shield plan ID cards. The alpha prefix identifies the member’s Blue Cross and/or Blue Shield plan or national account and is required for routing claims.