What Science Reveals About Fetal Pain 2017 Edition
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Hysteroscopy with Dilation and Curretage (D & C)
501 19th Street, Trustees Tower FORT SANDERS WOMEN’S SPECIALISTS 1924 Pinnacle Point Way Suite 401, Knoxville Tn 37916 P# 865-331-1122 F# 865-331-1976 Suite 200, Knoxville Tn 37922 Dr. Curtis Elam, M.D., FACOG, AIMIS, Dr. David Owen, M.D., FACOG, Dr. Brooke Foulk, M.D., FACOG Dr. Dean Turner M.D., FACOG, ASCCP, Dr. F. Robert McKeown III, M.D., FACOG, AIMIS, Dr. Steven Pierce M.D., Dr. G. Walton Smith, M.D., FACOG, Dr. Susan Robertson, M.D., FACOG HYSTEROSCOPY WITH DILATION AND CURRETAGE (D & C) Please read and sign the following consent form when you feel that you completely understand the surgical procedure that is to be performed and after you have asked all of your questions. If you have any further questions or concerns, please contact our office prior to your procedure so that we may clarify any pertinent issues. Definition: HysterosCopy is an outpatient procedure that allows your doctor direct visualization of the inside of the uterine cavity (womb) by inserting a thin lighted telescope (hysteroscope) through the vagina (birth canal) and cervix, without making an abdominal incision. This procedure enables your doctor to examine the lining of the uterus, look for polyps, fibroids, scar tissue, blockages of the fallopian tubes, and abnormal partitions. In addition, this procedure allows your doctor to remove or surgically treat many of the abnormalities seen. Dilation and Curettage (D&C) allows your doctor to take a sample of the tissue that lines your uterus (endometrium) and/or to remove polyps, fibroid tumors, or hyperplasia. Suction D&C is used in cases of miscarriage. -

Do Nothing, Do Something, Aspirate: Management of Early Pregnancy
Disclosure Do Nothing, Do Something, • I train providers in Nexplanon insertion and removal Aspirate: • I do not receive any honoraria for this Management Of Early Pregnancy Loss Sarah Prager, MD, MAS Department of Obstetrics and Gynecology University of Washington Objectives Nomenclature By the end of this workshop participants will be able to: Early Pregnancy Loss/Failure (EPL/EPF) Spontaneous Abortion (SAb) 1. Understand diagnosis of early pregnancy loss (EPL) Miscarriage 2. Describe EPL management options in a clinic or the ED. 3. Describe the uterine evacuation procedure using These are all used interchangeably! the manual uterine aspirator (MUA). 4. Demonstrate the use of MUA for uterine Manual Uterine Aspiration/Aspirator (MUA) evacuation using papayas as simulation models. Manual Vacuum Aspiration/Aspirator (MVA) 5. Express an awareness of their own values related Uterine Evacuation to pregnancy and EPL management. Suction D&C/D&C/dilation and curettage Background Imperfect obstetrics: most don’t continue • Early Pregnancy Loss (EPL) is the most common complication of early pregnancy • 8–20% clinically recognized pregnancies • 13–26% all pregnancies • ~ 800,000 EPLs each year in the US • 80% of EPLs occur in 1st trimester • Many women with EPL first contact medical care through the emergency room Brown S, Miscarriage and its associations. Sem Repro Med. 1 Samantha Risk Factors for EPL • Age • 26 yo G2P1 presents to the • Prior SAb emergency room with vaginal • Smoking bleeding after a positive • Alcohol home pregnancy test. An • Caffeine (controversial) ultrasound shows a CRL of • Maternal BMI <18.5 or >25 7mm but no cardiac activity. • Celiac disease (untreated) • She wants to know why this • Cocaine happened. -

Dilation and Curettage (D&C) Consent Form
Dilation and Curettage (D&C) Consent Form Patient Name: ____________________________________________ Date of Birth: __________ Guardian Name (if applicable): ________________________________ Patient ID: ___________ Washington State law guarantees that you have both the right and the obligation to make decisions regarding your health care. Your physician can provide you with the necessary information and advice, but as a member of the health care team, you must participate in the decision making process. This form acknowledges your consent to treatment recommended by your physician. 1 MY PROCEDURE I hereby give my consent for Dr. or/and his/her associates to perform a Dilation and Curettage upon me. I understand the procedure is to be performed at the First Hill Surgery Center. This has been recommended to me by my physician in order to diagnose or treat dysfunctional uterine bleeding, menorrhagia (heavy menstrual bleeding) increased endometrial thickness, uterine polyps, and/or miscarriage. I understand that the procedure or treatment can be described as follows: The cervix is mechanically dilated and the lining of the uterus is either scraped or suctioned to remove tissue for possible biopsy. This procedure is routinely done in an outpatient surgery center and typically takes 15-20 minutes to complete. General anesthesia or sedation may be required for this procedure and will be administered by a qualified anesthesiologist. Your anesthesiologist will be available to discuss this further with you on the day of your procedure. 2 MY BENEFITS Some potential benefits of this procedure include: Removing tissue from the uterus may temporarily relieve abnormal bleeding lining; removing tissue for biopsy of the uterine lining; resolution of failed pregnancy. -

The Effects of Alcohol in Newborns Efeitos Do Álcool No Recém-Nascido
REVIEW The effects of alcohol in newborns Efeitos do álcool no recém-nascido Maria dos Anjos Mesquita* ABSTRACT alcoólicas leva a prejuízos individuais, para a sua família e para The purpose of this article was to present a review of the effects toda a sociedade. Apesar disso, a dificuldade do seu diagnóstico e of alcohol consumption by pregnant mothers on their newborn. a inexperiência dos profissionais de saúde faz com que o espectro Definitions, prevalence, pathophysiology, clinical features, diagnostic dessas lesões seja pouco lembrado e até desconhecido. As lesões criteria, follow-up, treatment and prevention were discussed. A causadas pela ação do álcool no concepto são totalmente prevenidas search was performed in Medline, LILACS, and SciELO databases se a gestante não consumir bebidas alcoólicas durante a gestação. using the following terms: “fetus”, “newborn”, “pregnant woman”, Assim, é fundamental a detecção das mulheres consumidoras “alcohol”, “alcoholism”, “fetal alcohol syndrome”, and “alcohol- de álcool durante a gravidez e o desenvolvimento de programas related disorders”. Portuguese and English articles published from específicos de alerta sobre as consequências do álcool durante a 2000 to 2009 were reviewed. The effects of alcohol consumed by gestação e amamentação. pregnant women on newborns are extremely serious and occur frequently; it is a major issue in Public Health worldwide. Fetal alcohol Descritores: Bebidas alcoólicas/efeitos adversos; Feto; Recém-nascido; spectrum disorders cause harm to individuals, their families, and the Síndrome alcoólica fetal; Transtornos relacionados ao uso de álcool entire society. Nevertheless, diagnostic difficulties and inexperience of healthcare professionals result in such damage, being remembered rarely or even remaining uncovered. -

Model for Teaching Cervical Dilation and Uterine Curettage
Model for Teaching Cervical Dilation and Uterine Curettage Linda J. Gromko, MD, and Sam C. Eggertsen, MD Seattle, W a s h in g to n t least 15 percent of clinically recognizable pregnan METHODS A cies terminate in fetal loss, with the majority occur ring in the first trimester.1 Cervical dilation and uterine The fabric model was developed under the guidance of curettage (D&C) is frequently important in the manage physicians at the University of Washington Department ment of early pregnancy loss to control bleeding and re of Family Medicine and is commercially available.* The duce the risk of infection. D&Cs are also done for thera model, designed to approximate a 10-week last-menstrual- peutic first trimester abortions in family practice settings. period-sized uterus, is supported by elastic “ligaments” Resident experience may vary greatly, and some may feel on a wooden frame (Figure 1). A standard Graves spec inadequately trained in this procedure. The initial use of ulum can be inserted into the “vagina,” permitting vi gynecologic instruments (ie, tenaculum, sound, dilators, sualization of a cloth cervix. After placement of a tena curette) can feel awkward to the learner, and extensive culum onto the cervix, a paracervical block can be verbal tutoring may be discomfiting to the awake patient. demonstrated and the uterus sounded. Progressive dilation Training on a model can reduce these problems. After with Pratt or Denniston dilators follows: a drawstring al gaining basic skills on a model, the resident can focus on lows for the cervix to retain each successive degree of di gaining additional skills and refining technique during pa lation. -

FASD Effects of Alcohol on a Fetus
EFFECTS OF ALCOHOL ON A FETUS “Of all the substances of abuse (including cocaine, heroin, and marijuana), alcohol produces by far the most serious neurobehavioral effects in the fetus.” —Institute of Medicine Report to Congress, 19961 Prenatal exposure to alcohol can damage a fetus at any time, causing problems that persist throughout the individual’s life. There is no known safe level of alcohol use in pregnancy. WHAT IS THE SCOPE OF THE PROBLEM? identified in virtually every part of the body, including the brain, face, eyes, ears, heart, kidneys, and bones. No Alcohol is one of the most dangerous teratogens, which single mechanism can account for all the problems that are substances that can damage a developing fetus.1 Every alcohol causes. Rather, alcohol sets in motion many time a pregnant woman has a drink, her unborn child processes at different sites in the developing fetus: has one, too. Alcohol, like carbon monoxide from cigarettes, passes easily through the placenta from the • Alcohol can trigger cell death in a number of ways, mother's bloodstream into her baby's blood (See Figure causing different parts of the fetus to develop abnormally. 1)—and puts her fetus at risk of having a fetal alcohol • Alcohol can disrupt the way nerve cells develop, travel spectrum disorder (FASD). The blood alcohol level to form different parts of the brain, and function. (BAC) of the fetus becomes equal to or greater than the blood alcohol level of the mother. Because the fetus • By constricting the blood vessels, alcohol interferes with cannot break down alcohol the way an adult can, its BAC blood flow in the placenta, which hinders the delivery 2 remains high for a longer period of time. -

Dilation and Curettage (D&C)
Fact Sheet From ReproductiveFacts.org The Patient Education Website of the American Society for Reproductive Medicine Dilation and Curettage (D&C) This fact sheet was developed in collaboration with The Society of Reproductive Surgeons “Dilation and curettage” (D&C) is a short surgical as intestines, bladder, or blood vessels, are injured. If procedure that removes tissue from your uterus (womb). any of these organs are injured, they must be repaired You may need this procedure if you have unexplained with surgery. However, if no other organs have been or abnormal bleeding, or if you have delivered a baby injured, long-term complications from a perforation are and placental tissue remains in your womb. D&C also is extremely rare and the uterus heals on its own. performed to remove pregnancy tissue remaining from can occur after a D&C. If you are not a miscarriage or an abortion. Infections pregnant at the time of your D&C, this complication How is the procedure done? is extremely rare. However, 10% of women who were D&C can be done in a doctor’s office or in the hospital. pregnant before their D&C can get an infection, usually You may be given medications to relax you or to put you within 1 week of the procedure. It may be related to a to sleep for a short time. Your doctor will slowly widen sexually transmitted infection or due to normal bacteria the opening to your uterus (cervix). Opening your cervix that pass from the vagina into the uterus during or can cause cramping. -
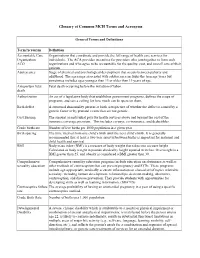
Glossary of Common MCH Terms and Acronyms
Glossary of Common MCH Terms and Acronyms General Terms and Definitions Term/Acronym Definition Accountable Care Organizations that coordinate and provide the full range of health care services for Organization individuals. The ACA provides incentives for providers who join together to form such ACO organizations and who agree to be accountable for the quality, cost, and overall care of their patients. Adolescence Stage of physical and psychological development that occurs between puberty and adulthood. The age range associated with adolescence includes the teen age years but sometimes includes ages younger than 13 or older than 19 years of age. Antepartum fetal Fetal death occurring before the initiation of labor. death Authorization An act of a legislative body that establishes government programs, defines the scope of programs, and sets a ceiling for how much can be spent on them. Birth defect A structural abnormality present at birth, irrespective of whether the defect is caused by a genetic factor or by prenatal events that are not genetic. Cost Sharing The amount an individual pays for health services above and beyond the cost of the insurance coverage premium. This includes co-pays, co-insurance, and deductibles. Crude birth rate Number of live births per 1000 population in a given year. Birth spacing The time interval from one child’s birth until the next child’s birth. It is generally recommended that at least a two-year interval between births is important for maternal and child health and survival. BMI Body mass index (BMI) is a measure of body weight that takes into account height. -

If You Are Pregnant: INFORMATION on FETAL DEVELOPMENT, ABORTION and ALTERNATIVES August 2019
If You Are Pregnant: INFORMATION ON FETAL DEVELOPMENT, ABORTION AND ALTERNATIVES August 2019 IF YOU ARE PREGNANT: INFORMATION ON FETAL DEVELOPMENT, ABORTION AND ALTERNATIVES If You Are Pregnant: Information on Fetal Development, Abortion and Alternatives Resources used by the Minnesota Department of Health for this publication are Human Embryology and Developmental Biology, Fifth Edition, 2014; Larsen’s Human Embryology, Fifth Edition, 2014; The Developing Human, 10th Edition, 2016; and In the Womb, 2006. The photographs in this booklet are credited to Lennart Nilsson/TT Images and are used by permission; except for week 38 copyright Minnesota Department of Health. The illustrations found throughout this booklet were created by Peg Gerrity, Houston, Texas. Copyright: http://www.peggerrity.com. Minnesota Department of Health Division of Child and Family Health PO Box 64882 St. Paul, MN 55164-0882 651-201-3580 Women's Right to Know (https://www.health.state.mn.us/people/wrtk/index.html) Upon request, this material will be made available in an alternative format such as large print, Braille or audio recording. Printed on recycled paper. 2 IF YOU ARE PREGNANT: INFORMATION ON FETAL DEVELOPMENT, ABORTION AND ALTERNATIVES Contents If You Are Pregnant: INFORMATION ON FETAL DEVELOPMENT, ABORTION AND ALTERNATIVES............................................................................................................................. 1 Introduction ............................................................................................................................... -

A B C Pregnancy Terms and Definitions
Pregnancy Terms and Definitions Obstetrics & Gynecology A After pains or afterbirth pains: Contractions of the uterus that occur after your baby is born, as the uterus returns to its normal size. This may cause cramping for a few days, especially if this is not your first baby or if you are nursing. Amniocentesis: the removal of a sample of amniotic fluid by means of a needle inserted through the mother’s abdominal wall; used for genetic and biochemical analysis of the baby. Amniotic fluid: the liquid surrounding and protecting the baby within the amniotic sac throughout pregnancy. Amniotic sac: the membrane within the uterus that contains the baby and the amniotic fluid. Analgesic: Medication that relieves or reduces pain. Anesthesia: Loss of feeling. There are three ways of doing this: general, local and epidural. Anesthesiologist: A doctor who specializes in the use of anesthesia. Anesthetist: A registered nurse who has special training in anesthesia. Apgar score rating: A system to evaluate the health of your baby immediately after birth. The score can be zero to 10, based on appearance and color, pulse, reflexes, activity and respiration. B Baby blues: A mild depression many women feel in the first few weeks after birth. Braxton-Hicks contractions: Mild, usually painless contractions that occur during the entire pregnancy, but are only felt from the 5th month on. Breech birth: Baby is born feet or buttocks first. C Cephalopelvic disproprition (CPD): Baby’s head is too large for the mother’s pelvic bones. Cervix: the neck of the uterus; Pap smears are taken from the cervix. -

Alcohol Abuse in Pregnant Women: Effects on the Fetus and Newborn, Mode of Action and Maternal Treatment
Int. J. Environ. Res. Public Health 2010, 7, 364-379; doi:10.3390/ijerph7020364 OPEN ACCESS International Journal of Environmental Research and Public Health ISSN 1660-4601 www.mdpi.com/journal/ijerph Review Alcohol Abuse in Pregnant Women: Effects on the Fetus and Newborn, Mode of Action and Maternal Treatment Asher Ornoy 1,* and Zivanit Ergaz 1,2 1 Laboratory of Teratology, The Institute of Medical Research Israel Canada, Hadassah Medical School and Hospital, The Hebrew University of Jerusalem, Ein Kerem, P.O. Box 12271, Jerusalem, 91120, Israel; E-Mail: [email protected] 2 Department of Neonatology, Hadassah Medical School and Hospital, Hadassah Medical Center, Hebrew University, P.O. Box 24035, Jerusalem, 91240, Israel * Author to whom correspondence should be addressed; E-Mail: [email protected]; Tel.: +972-50-624-2125. Received: 16 December 2009 / Accepted: 22 January 2010 / Published: 27 January 2010 Abstract: Offspring of mothers using ethanol during pregnancy are known to suffer from developmental delays and/or a variety of behavioral changes. Ethanol, may affect the developing fetus in a dose dependent manner. With very high repetitive doses there is a 6–10% chance of the fetus developing the fetal alcoholic syndrome manifested by prenatal and postnatal growth deficiency, specific craniofacial dysmorphic features, mental retardation, behavioral changes and a variety of major anomalies. With lower repetitive doses there is a risk of "alcoholic effects" mainly manifested by slight intellectual impairment, growth disturbances and behavioral changes. Binge drinking may impose some danger of slight intellectual deficiency. It is advised to offer maternal abstinence programs prior to pregnancy, but they may also be initiated during pregnancy with accompanying close medical care. -

The Political and Moral Battle Over Late-Term Abortion
CROSSING THE LINE: THE POLITICAL AND MORAL BATTLE OVER LATE-TERM ABORTION Rigel C. Oliverit "This is an emotional,distorted debate. We are using the lives ofa few women to create divisions across this country... -Senator Patty Murray' I. INTRODUCTION The 25 years following the Supreme Court's landmark decision in Roe v. Wade2 have seen a tremendous amount of social and political activism on both sides of the abortion controversy. Far from settling the issue of a woman's constitutional right to an abortion, the Roe decision galvanized pro-life and pro- choice groups and precipitated many small "battles" in what many on both sides view to be a "war" between fetal protection and women's access to reproductive choice. These battles have occurred at the judicial, grassroots, and political levels, with each side gaining and losing ground. Pro-life activists staged a nation-wide campaign of clinic protests, which led to Congress's 1994 enactment of the Federal Access to Clinic Entrances law creating specific civil and criminal penalties for violence outside of abortion clinics.3 State legislatures imposed limitations on the right to abortion, including mandatory waiting periods and requirements for parental or spousal notification. Many of these limitations were then challenged before the Supreme Court, which struck down or upheld them according to the "undue burden" standard of review articulated in PlannedParenthood of Southeastern Pennsylvania v. Casey.4 Recent developments have shifted the focus of conflict from clinic entrances and state regulation of abortion access to the abortion procedures themselves. The most controversial procedures include RU-486--the "abortion drug"-and a particular late term surgical procedure called intact dilation and extraction ("D&X")-more popularly known as "partial-birth abortion." The controversy surrounding the D&X procedure escalated dramatically in June of 1995, when both houses of Congress first introduced legislation to ban the procedure.