The Continuum Hypothesis
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Current P SYCHIATRY
Current p SYCHIATRY N ew Investigators Tips to manage and prevent discontinuation syndromes Informed tapering can protect patients when you stop a medication Sriram Ramaswamy, MD Shruti Malik, MBBS, MHSA Vijay Dewan, MD Instructor, department of psychiatry Foreign medical graduate Assistant professor Creighton University Department of psychiatry Omaha, NE University of Nebraska Medical Center Omaha, NE bruptly stopping common psychotropics New insights on psychotropic A —particularly antidepressants, benzodi- drug safety and side effects azepines, or atypical antipsychotics—can trigger a discontinuation syndrome, with: This paper was among those entered in the 2005 • rebound or relapse of original symptoms Promising New Investigators competition sponsored • uncomfortable new physical and psycho- by the Neuroleptic Malignant Syndrome Information Service (NMSIS). The theme of this year’s competition logical symptoms was “New insights on psychotropic drug safety and • physiologic withdrawal at times. side effects.” To increase health professionals’ awareness of URRENT SYCHIATRY 1 C P is honored to publish this peer- the risk of these adverse effects, this article reviewed, evidence-based article on a clinically describes discontinuation syndromes associated important topic for practicing psychiatrists. with various psychotropics and offers strategies to NMSIS is dedicated to reducing morbidity and anticipate, recognize, and manage them. mortality of NMS by improving medical and psychiatric care of patients with heat-related disorders; providing -

Doxepin Exacerbates Renal Damage, Glucose Intolerance, Nonalcoholic Fatty Liver Disease, and Urinary Chromium Loss in Obese Mice
pharmaceuticals Article Doxepin Exacerbates Renal Damage, Glucose Intolerance, Nonalcoholic Fatty Liver Disease, and Urinary Chromium Loss in Obese Mice Geng-Ruei Chang 1,* , Po-Hsun Hou 2,3, Wei-Cheng Yang 4, Chao-Min Wang 1 , Pei-Shan Fan 1, Huei-Jyuan Liao 1 and To-Pang Chen 5,* 1 Department of Veterinary Medicine, National Chiayi University, 580 Xinmin Road, Chiayi 60054, Taiwan; [email protected] (C.-M.W.); [email protected] (P.-S.F.); [email protected] (H.-J.L.) 2 Department of Psychiatry, Taichung Veterans General Hospital, 1650 Taiwan Boulevard (Section 4), Taichung 40705, Taiwan; [email protected] 3 Faculty of Medicine, National Yang-Ming University, 155 Linong Street (Section 2), Taipei 11221, Taiwan 4 School of Veterinary Medicine, National Taiwan University, 1 Roosevelt Road (Section 4), Taipei 10617, Taiwan; [email protected] 5 Division of Endocrinology and Metabolism, Show Chwan Memorial Hospital, 542 Chung-Shan Road (Section 1), Changhua 50008, Taiwan * Correspondence: [email protected] (G.-R.C.); [email protected] (T.-P.C.); Tel.: +886-5-2732946 (G.-R.C.); +886-4-7256166 (T.-P.C.) Abstract: Doxepin is commonly prescribed for depression and anxiety treatment. Doxepin-related disruptions to metabolism and renal/hepatic adverse effects remain unclear; thus, the underlying mechanism of action warrants further research. Here, we investigated how doxepin affects lipid Citation: Chang, G.-R.; Hou, P.-H.; change, glucose homeostasis, chromium (Cr) distribution, renal impairment, liver damage, and fatty Yang, W.-C.; Wang, C.-M.; Fan, P.-S.; liver scores in C57BL6/J mice subjected to a high-fat diet and 5 mg/kg/day doxepin treatment for Liao, H.-J.; Chen, T.-P. -

Olanzapine-Induced Acute Pancreatitis and New Diabetes Mellitus
Open Journal of Psychiatry, 2012, 2, 110-112 OJPsych http://dx.doi.org/10.4236/ojpsych.2012.22015 Published Online April 2012 (http://www.SciRP.org/journal/ojpsych/) Case report: Olanzapine-induced acute pancreatitis and new diabetes mellitus Erik Monasterio1*, Ruchi Bhalla2, Andrew McKean3 1Department of Psychological Medicine, University of Otago, Christchurch, New Zealand 2Hammersmith and Fulham Mental Health Unit, West London Mental Health NHS Trust, London, UK 3Hillmorton Hospital, Christchurch, New Zealand Email: *[email protected] Received 29 December 2011; revised 31 January 2012; accepted 15 February 2012 ABSTRACT criteria and required application from a psychiatrist for a patient who had been trialled unsuccessfully on risperi- The aim of this case study is to review the literature done or required treatment with olanzapine short acting and report the first published case of olanzapine-in- intra-muscular injection [4]. In June 2011, significantly duced acute pancreatitis in New Zealand. A case re- cheaper generic versions of olanzapine were introduced port of acute pancreatitis with new onset diabetes and the special authority criteria for olanzapine with- mellitus secondary to olanzapine in a 42-year-old male, drawn [5]. We aim to highlight lesser known and poten- in the absence of medical risk factors is reported. tially fatal side effects through our case report. Eleven previous case reports of olanzapine induced acute-pancreatitis were identified in the literature. A 2. CASE REPORT 42-year-old male was diagnosed with acute pancreati- tis and new diabetes mellitus induced by olanzapine. Mr. X is a 42 year old man who had come into contact Although rare, pancreatitis is associated with use of with mental health services on many occasions during some atypical antipsychotic medications. -

Efficacy of Antimanic Treatments: Meta-Analysis of Randomized, Controlled Trials
Neuropsychopharmacology (2011) 36, 375–389 & 2011 American College of Neuropsychopharmacology. All rights reserved 0893-133X/11 $32.00 www.neuropsychopharmacology.org Efficacy of Antimanic Treatments: Meta-analysis of Randomized, Controlled Trials ,1,2 2,3 4 2 Ays¸egu¨l Yildiz* , Eduard Vieta , Stefan Leucht and Ross J Baldessarini 1 2 Department of Psychiatry, Dokuz Eylu¨l University, Izmir, Turkey; Department of Psychiatry, Harvard Medical School and International Consortium for Bipolar Disorder Research and Psychopharmacology Program, McLean Division of Massachusetts General Hospital, Boston, 3 Massachusetts; Bipolar Disorders Program, Institute of Clinical Neuroscience, Hospital Clinic, University of Barcelona, IDIBAPS, CIBERSAM, 4 Barcelona, Spain; Department of Psychiatry and Psychotherapy, Klinik fu¨r Psychiatrie und Psychotherapie der TU-Mu¨nchen, Klinikum rechts der Isar, Technische Universita¨t Mu¨nchen, Mu¨nchen, Germany We conducted meta-analyses of findings from randomized, placebo-controlled, short-term trials for acute mania in manic or mixed states of DSM (III–IV) bipolar I disorder in 56 drug–placebo comparisons of 17 agents from 38 studies involving 10 800 patients. Of drugs tested, 13 (76%) were more effective than placebo: aripiprazole, asenapine, carbamazepine, cariprazine, haloperidol, lithium, olanzapine, paliperdone, quetiapine, risperidone, tamoxifen, valproate, and ziprasidone. Their pooled effect size for mania improvement (Hedges’ g in 48 trials) was 0.42 (confidence interval (CI): 0.36–0.48); pooled responder risk ratio (46 trials) was 1.52 (CI: 1.42–1.62); responder rate difference (RD) was 17% (drug: 48%, placebo: 31%), yielding an estimated number-needed-to-treat of 6 (all po0.0001). In several direct comparisons, responses to various antipsychotics were somewhat greater or more rapid than lithium, valproate, or carbamazepine; lithium did not differ from valproate, nor did second generation antipsychotics differ from haloperidol. -

Cariprazine Exhibits Anxiolytic and Dopamine D Receptor-Dependent
International Journal of Neuropsychopharmacology (2017) 20(10): 788–796 doi:10.1093/ijnp/pyx038 Advance Access Publication: May 22, 2017 Regular Research Article regular research article Cariprazine Exhibits Anxiolytic and Dopamine D3 Receptor-Dependent Antidepressant Effects in the Chronic Stress Model Vanja Duric, Mounira Banasr, Tina Franklin, Ashley Lepack, Nika Adham, Béla Kiss, István Gyertyán, Ronald S. Duman Department of Psychiatry, Yale University School of Medicine, New Haven, Connecticut (Dr Duric, Dr Banasr, Dr Franklin, Ms Lepack, and Dr Duman); Department of Physiology and Pharmacology, Des Moines University, Des Moines, Iowa (Dr Duric); Campell Family Mental Health Research Institute of CAMH, Toronto, Ontario, Canada (Dr Banasr); Department of Pharmacology, Allergan, Jersey City, New Jersey (Dr Adham); Pharmacological and Safety Research, Gedeon Richter Plc, Budapest, Hungary (Dr Kiss); MTA-SE NAP B Cognitive Translational Behavioral Pharmacology Group, Department of Pharmacology and Pharmacotherapy, Semmelweis University, Budapest, Hungary (Dr Gyertyán); Institute of Cognitive Neuroscience and Psychology, Hungarian Academy of Sciences, Budapest, Hungary (Dr Gyertyán). Correspondence: Ronald S. Duman, PhD, Professor of Psychiatry and Pharmacology, Director, Abraham Ribicoff Research Facilities, Laboratory of Molecular Psychiatry, Yale University School of Medicine, 34 Park Street, Room 308, New Haven, CT 06508 ([email protected]). Abstract Background: Cariprazine, a D3-preferring dopamine D2/D3 receptor partial agonist, is a new antipsychotic drug recently approved in the United States for the treatment of schizophrenia and bipolar mania. We recently demonstrated that cariprazine also has significant antianhedonic-like effects in rats subjected to chronic stress; however, the exact mechanism of action for cariprazine’s antidepressant-like properties is not known. -

Olanzapine and Clozapine Increase the Gabaergic Neuroactive Steroid Allopregnanolone in Rodents
Neuropsychopharmacology (2003) 28, 1–13 & 2003 Nature Publishing Group All rights reserved 0893-133X/03 $25.00 www.neuropsychopharmacology.org Olanzapine and Clozapine Increase the GABAergic Neuroactive Steroid Allopregnanolone in Rodents ,1 2,3 2 2 2,3,4 Christine E Marx* , Margaret J VanDoren , Gary E Duncan , Jeffrey A Lieberman and A Leslie Morrow 1Department of Psychiatry and Behavioral Sciences, Duke University Medical Center and Durham VA Medical Center, Durham, North Carolina, USA; 2Department of Psychiatry, University of North Carolina, Chapel Hill, North Carolina 27599, USA; 3Center for Alcohol Studies, University of 4 North Carolina, Chapel Hill, North Carolina 27599, USA; Department of Pharmacology, University of North Carolina, Chapel Hill, North Carolina 27599, USA The neuroactive steroid allopregnanolone is a potent g-aminobutyric acid type A (GABAA) receptor modulator with anxiolytic and anticonvulsant effects. Olanzapine and clozapine also have anxiolytic-like effects in behavioral models. We therefore postulated that olanzapine and clozapine would elevate allopregnanolone levels, but risperidone and haloperidol would have minimal effects. Male rats received intraperitoneal olanzapine (2.5–10.0 mg/kg), clozapine (5.0–20.0 mg/kg), risperidone (0.1–1.0 mg/kg), haloperidol (0.1–1.0 mg/ kg), or vehicle. Cerebral cortical allopregnanolone and peripheral progesterone and corticosterone levels were determined. Adrenalectomized animals were also examined. Both olanzapine and clozapine increased cerebral cortical allopregnanolone levels, but neither risperidone nor haloperidol had significant effects. Olanzapine and clozapine also increased serum progesterone and corticosterone levels. Adrenalectomy prevented olanzapine- and clozapine-induced elevations in allopregnanolone. Allopregnanolone induction may contribute to olanzapine and clozapine anxiolytic, antidepressant, and mood-stabilizing actions. -
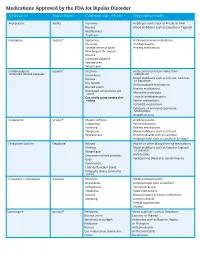
Medications Approved by the FDA for Bipolar Disorder Medication Brand Name Common Side Effects May Interact With
Medications Approved by the FDA for Bipolar Disorder Medication Brand Name Common side effects May interact with Aripiprazole Abilify® Insomnia Antidepressants such as Prozac or Paxil Nausea Mood stabilizers such as Equetro or Tegretol Restlessness Tiredness Asenapine Saphris® Sleepiness Antihypertensive medications Dizziness Antidepressants Strange sense of taste Anxiety medications Numbing of the mouth Nausea Increased appetite Feeling tired Weight gain Carbamazepine Equetro™ Dizziness Birth control pills (can make them extended release capsules Drowsiness ineffective) Mood stabilizers such as Lithium, Lamictal, Nausea or Depakote Dry mouth Anticonvulsant medications Blurred vision Anxiety medications Decreased white blood cell count Macrolide antibiotics Can rarely cause severe skin Tricyclic antidepressants rashes Cancer medications HIV/AIDS medications Cytotoxic or immunosuppressive Medications Grapefruit juice Cariprazine Vraylar® Muscle stiffness Antidepressants Indigestion Pain medications Vomiting Anxiety medications Sleepiness Mood stabilizers such as Lithium Restlessness Anticonvulsants such as Lamictal Antipsychotics such as Latuda or Seroquel Divalproex Sodium Depakote® Nausea Aspirin or other blood thinning medications Shaking Mood stabilizers such as Equetro,Tegretol, Weight gain or Lamictal Decrease in blood platelets Barbiturates Rash Cyclosporine (Neoral or Sandimmune) Pancreatitis Liver dysfunction (rare) Polycystic Ovary Syndrome (rare) Fluoxetine + Olanzapine Symbyax® Dizziness MAOI antidepressants Drowsiness Antipsychotics -

List Item Olanzapine Teva
EMA/685358/2012 EMEA/H/C/000810 EPAR summary for the public Olanzapine Teva olanzapine This is a summary of the European public assessment report (EPAR) for Olanzapine Teva. It explains how the Committee for Medicinal Products for Human Use (CHMP) assessed the medicine to reach its opinion in favour of granting a marketing authorisation and its recommendations on the conditions of use for Olanzapine Teva. What is Olanzapine Teva? Olanzapine Teva is a medicine containing the active substance olanzapine. It is available as tablets (2.5, 5, 7.5, 10, 15 and 20 mg) and as ‘orodispersible’ tablets (5, 10, 15 and 20 mg). Orodispersible tablets are tablets that dissolve in the mouth. Olanzapine Teva is a ‘generic medicine’. This means that Olanzapine Teva is similar to ‘reference medicines’ already authorised in the European Union (EU) called Zyprexa and Zyprexa Velotab. For more information on generic medicines, see the question-and-answer document here. What is Olanzapine Teva used for? Olanzapine Teva is used to treat adults with schizophrenia. Schizophrenia is a mental illness that has a number of symptoms including disorganised thinking and speech, hallucinations (hearing or seeing things that are not there), suspiciousness and delusions (mistaken beliefs). Olanzapine Teva is also effective in maintaining improvement in patients who have responded to an initial course of treatment. Olanzapine Teva is also used to treat moderate to severe manic episodes (extremely high mood) in adults. It can also be used to prevent the recurrence of these episodes (when symptoms come back) in adults with bipolar disorder (a mental illness causing alternating periods of high mood and depression) who have responded to an initial course of treatment. -
Psychotropic Drug Indications
PSYCHOTROPIC DRUG INDICATIONS (Part 1 of 2) Bipolar Disorder Mixed Generic Brand Form Mania Depression Episodes Maintenance MDD TRD PMDD Schizophrenia Others4 ATYPICAL ANTIPSYCHOTICS aripiprazole — tabs, ODT, oral √ √ √ √1 √ √ soln Abilify tabs √ √ √ √1 √ √ Abilify ext-rel IM inj √ √ Maintena Abilify tabs with √ √ √ √1 √ Mycite sensor aripiprazole Aristada ext-rel IM inj √ lauroxil Aristada ext-rel IM inj √ Initio asenapine Saphris sublingual tabs √ √ √ √ brexpiprazole Rexulti tabs √1 √ cariprazine Vraylar caps √ √ √ √ lurasidone Latuda tabs √ √ olanzapine Zyprexa tabs √ √2 √ √ √2 √ IM inj √ Zyprexa ext-rel IM inj √ Relprevv Zyprexa ODT √ √2 √ √ √2 √ Zydis quetiapine Seroquel tabs √ √ √ √ Seroquel XR ext-rel tabs √ √ √ √ √1 √ risperidone Perseris ext-rel SC inj √ Risperdal tabs, oral soln √ √ √ √ Risperdal ext-rel IM inj √ √ Consta Risperdal ODT √ √ √ √ M-tabs ziprasidone Geodon caps √ √ √1 √ IM inj √ COMBINATION ATYPICAL & SELECTIVE SEROTONIN REUPTAKE INHIBITOR olanzapine + Symbyax caps √ √ fluoxetine MONOAMINE OXIDASE INHIBITORS (MAOIs) phenelzine Nardil tabs √ selegiline EMSAM transdermal √ system tranylcypromine Parnate tabs √ SEROTONIN AND NOREPINEPHRINE REUPTAKE INHIBITORS (SNRIs) desvenlafaxine Khedezla ext-rel tabs √ Pristiq ext-rel tabs √ duloxetine Cymbalta caps √ √ levomilnacipran Fetzima ext-rel caps √ venlafaxine — scored tabs √ Effexor XR ext-rel caps √ √ SELECTIVE SEROTONIN REUPTAKE INHIBITORS (SSRIs) citalopram Celexa scored tabs √ escitalopram Lexapro scored tabs, √ √ oral soln fluoxetine — tabs, oral soln √3 √ √3 √ Prozac -

Medications to Be Avoided Or Used with Caution in Parkinson's Disease
Medications To Be Avoided Or Used With Caution in Parkinson’s Disease This medication list is not intended to be complete and additional brand names may be found for each medication. Every patient is different and you may need to take one of these medications despite caution against it. Please discuss your particular situation with your physician and do not stop any medication that you are currently taking without first seeking advice from your physician. Most medications should be tapered off and not stopped suddenly. Although you may not be taking these medications at home, one of these medications may be introduced while hospitalized. If a hospitalization is planned, please have your neurologist contact your treating physician in the hospital to advise which medications should be avoided. Medications to be avoided or used with caution in combination with Selegiline HCL (Eldepryl®, Deprenyl®, Zelapar®), Rasagiline (Azilect®) and Safinamide (Xadago®) Medication Type Medication Name Brand Name Narcotics/Analgesics Meperidine Demerol® Tramadol Ultram® Methadone Dolophine® Propoxyphene Darvon® Antidepressants St. John’s Wort Several Brands Muscle Relaxants Cyclobenzaprine Flexeril® Cough Suppressants Dextromethorphan Robitussin® products, other brands — found as an ingredient in various cough and cold medications Decongestants/Stimulants Pseudoephedrine Sudafed® products, other Phenylephrine brands — found as an ingredient Ephedrine in various cold and allergy medications Other medications Linezolid (antibiotic) Zyvox® that inhibit Monoamine oxidase Phenelzine Nardil® Tranylcypromine Parnate® Isocarboxazid Marplan® Note: Additional medications are cautioned against in people taking Monoamine oxidase inhibitors (MAOI), including other opioids (beyond what is mentioned in the chart above), most classes of antidepressants and other stimulants (beyond what is mentioned in the chart above). -

ARISTADA INITIO® Prescribing Information
HIGHLIGHTS OF PRESCRIBING INFORMATION These highlights do not include all the information needed to use ___________________ CONTRAINDICATIONS ___________________ ARISTADA INITIO® safely and effectively. See full prescribing Known hypersensitivity to aripiprazole (4). information for ARISTADA INITIO®. _______________ WARNINGS AND PRECAUTIONS _______________ ARISTADA INITIO® (aripiprazole lauroxil) extended-release injectable • Cerebrovascular Adverse Reactions in Elderly Patients with Dementia- suspension, for intramuscular use Related Psychosis: Increased incidence of cerebrovascular adverse Initial U.S. Approval: 2015 reactions (e.g., stroke, transient ischemia attack, including fatalities) (5.2). • Potential for Dosing and Medication Errors: Substitution and dispensing WARNING: INCREASED MORTALITY IN ELDERLY PATIENTS errors between ARISTADA INITIO and ARISTADA could occur. Do not WITH DEMENTIA-RELATED PSYCHOSIS substitute ARISTADA INITIO for ARISTADA (5.3). See full prescribing information for complete boxed warning. • Neuroleptic Malignant Syndrome: Manage with immediate discontinuation and close monitoring (5.4). • Elderly patients with dementia-related psychosis treated with • Tardive Dyskinesia: Discontinue if clinically appropriate (5.5). antipsychotic drugs are at an increased risk of death. (5.1) • Metabolic Changes: Monitor for hyperglycemia, dyslipidemia, and weight • ARISTADA INITIO is not approved for the treatment of patients with gain (5.6). dementia-related psychosis. (5.1) • Pathological Gambling and Other Compulsive Behaviors: -

Currently Prescribed Psychotropic Medications
CURRENTLY PRESCRIBED PSYCHOTROPIC MEDICATIONS Schizophrenia Depression Anxiety Disorders 1st generation antipsychotics: Tricyclics: Atarax (hydroxyzine) Haldol (haloperidol), *Anafranil (clomipramine) Ativan (lorazepam) Haldol Decanoate Asendin (amoxapine) BuSpar (buspirone) Loxitane (loxapine) Elavil (amitriptyline) *Inderal (propranolol) Mellaril (thioridazine) Norpramin (desipramine) Keppra (levetiracetam) Navane (thiothixene) Pamelor (nortriptyline) *Klonopin (clonazepam) Prolixin (fluphenazine), Prolixin Sinequan (doxepin) Librium (chlordiazepoxide) Decanoate Spravato (esketamine) Serax (oxazepam) Stelazine (trifluoperazine) Surmontil (trimipramine) Thorazine (chlorpromazine) *Tenormin (atenolol) Tofranil (imipramine) MEDICATIONS PSYCHOTROPIC PRESCRIBED CURRENTLY Trilafon (perphenazine) Tranxene (clorazepate) Vivactil (protriptyline) Valium (diazepam) 2nd generation antipsychotics: Zulresso (brexanolone) Vistaril (hydroxyzine) Abilify (aripiprazole) Aristada (aripiprazole) SSRIs: Xanax (alprazolam) Caplyta (lumateperone) Celexa (citalopram) *Antidepressants, especially SSRIs, are also used in the treatment of anxiety. Clozaril (clozapine) Lexapro (escitalopram) Fanapt (iloperidone) *Luvox (fluvoxamine) Geodon (ziprasidone) Paxil (paroxetine) Stimulants (used in the treatment of ADD/ADHD) Invega (paliperidone) Prozac (fluoxetine) Invega Sustenna Zoloft (sertraline) Adderall (amphetamine and Perseris (Risperidone injectable) dextroamphetamine) Latuda (lurasidone) MAOIs: Azstarys(dexmethylphenidate Rexulti (brexpiprazole) Emsam (selegiline)