Educational Workshop
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Medical Review(S) Clinical Review
CENTER FOR DRUG EVALUATION AND RESEARCH APPLICATION NUMBER: 200327 MEDICAL REVIEW(S) CLINICAL REVIEW Application Type NDA Application Number(s) 200327 Priority or Standard Standard Submit Date(s) December 29, 2009 Received Date(s) December 30, 2009 PDUFA Goal Date October 30, 2010 Division / Office Division of Anti-Infective and Ophthalmology Products Office of Antimicrobial Products Reviewer Name(s) Ariel Ramirez Porcalla, MD, MPH Neil Rellosa, MD Review Completion October 29, 2010 Date Established Name Ceftaroline fosamil for injection (Proposed) Trade Name Teflaro Therapeutic Class Cephalosporin; ß-lactams Applicant Cerexa, Inc. Forest Laboratories, Inc. Formulation(s) 400 mg/vial and 600 mg/vial Intravenous Dosing Regimen 600 mg every 12 hours by IV infusion Indication(s) Acute Bacterial Skin and Skin Structure Infection (ABSSSI); Community-acquired Bacterial Pneumonia (CABP) Intended Population(s) Adults ≥ 18 years of age Template Version: March 6, 2009 Reference ID: 2857265 Clinical Review Ariel Ramirez Porcalla, MD, MPH Neil Rellosa, MD NDA 200327: Teflaro (ceftaroline fosamil) Table of Contents 1 RECOMMENDATIONS/RISK BENEFIT ASSESSMENT ......................................... 9 1.1 Recommendation on Regulatory Action ........................................................... 10 1.2 Risk Benefit Assessment.................................................................................. 10 1.3 Recommendations for Postmarketing Risk Evaluation and Mitigation Strategies ........................................................................................................................ -

Severe Sepsis Tipsheet
Severe Sepsis Tipsheet SEVERE SEPSIS A, B, and C of the following must be met within 6 hours of each other. A. Documentation of a suspected infection. There may be reference to “possible infection,” “suspect infection,” “rule out infection,” or similar documentation. B. TWO or more manifestations of systemic infection according to the Systemic Inflammatory Response Syndrome (SIRS) criteria, which are: • Temperature > 38.3 C or < 36.0 C (> 100.9 F or < 96.8 F) • Heart rate (pulse) > 90 • Respiration > 20 per minute • White blood cell count > 12,000 or < 4,000 or > 10% bands C. Organ dysfunction, evidenced by any one of the following: • Systolic blood pressure (SBP) < 90 mmHg, or mean arterial pressure < 65 mmHg, or a systolic blood pressure decrease of more than 40 mmHg. Physician/APN/PA documentation must be present in the medical record indicating a > 40 mmHg decrease in SBP has occurred and is related to infection, severe sepsis or septic shock and not other causes. • Acute respiratory failure as evidenced by a new need for invasive or non-invasive mechanical ventilation. To use acute respiratory failure as a sign of organ dysfunction there must be: • Documentation of acute respiratory failure AND • Documentation the patient is on mechanical ventilation • Invasive mechanical ventilation requires an endotracheal or tracheostomy tube. Non-invasive mechanical ventilation may be referred to as BiPAP or CPAP. • New need for mechanical ventilation indicates the patient was not using the same type of mechanical ventilation prior to the current acute respiratory failure. • Use the time at which there is documentation the patient has both acute respiratory failure and is on mechanical ventilation. -
Below Are the CLSI Breakpoints for Selected Bacteria. Please Use Your Clinical Judgement When Assessing Breakpoints
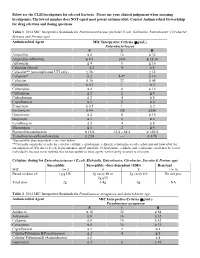
Below are the CLSI breakpoints for selected bacteria. Please use your clinical judgement when assessing breakpoints. The lowest number does NOT equal most potent antimicrobial. Contact Antimicrobial Stewardship for drug selection and dosing questions. Table 1: 2014 MIC Interpretive Standards for Enterobacteriaceae (includes E.coli, Klebsiella, Enterobacter, Citrobacter, Serratia and Proteus spp) Antimicrobial Agent MIC Interpretive Criteria (g/mL) Enterobacteriaceae S I R Ampicillin ≤ 8 16 ≥ 32 Ampicillin-sulbactam ≤ 8/4 16/8 ≥ 32/16 Aztreonam ≤ 4 8 ≥ 16 Cefazolin (blood) ≤ 2 4 ≥ 8 Cefazolin** (uncomplicated UTI only) ≤ 16 ≥ 32 Cefepime* ≤ 2 4-8* ≥ 16 Cefotetan ≤ 16 32 ≥ 64 Ceftaroline ≤ 0.5 1 ≥ 2 Ceftazidime ≤ 4 8 ≥ 16 Ceftriaxone ≤ 1 2 ≥ 4 Cefpodoxime ≤ 2 4 ≥ 8 Ciprofloxacin ≤ 1 2 ≥ 4 Ertapenem ≤ 0.5 1 ≥ 2 Fosfomycin ≤ 64 128 ≥256 Gentamicin ≤ 4 8 ≥ 16 Imipenem ≤ 1 2 ≥ 4 Levofloxacin ≤ 2 4 ≥ 8 Meropenem ≤ 1 2 ≥ 4 Piperacillin-tazobactam ≤ 16/4 32/4 – 64/4 ≥ 128/4 Trimethoprim-sulfamethoxazole ≤ 2/38 --- ≥ 4/76 *Susceptibile dose-dependent – see chart below **Cefazolin can predict results for cefaclor, cefdinir, cefpodoxime, cefprozil, cefuroxime axetil, cephalexin and loracarbef for uncomplicated UTIs due to E.coli, K.pneumoniae, and P.mirabilis. Cefpodoxime, cefinidir, and cefuroxime axetil may be tested individually because some isolated may be susceptible to these agents while testing resistant to cefazolin. Cefepime dosing for Enterobacteriaceae ( E.coli, Klebsiella, Enterobacter, Citrobacter, Serratia & Proteus spp) Susceptible Susceptible –dose-dependent (SDD) Resistant MIC </= 2 4 8 >/= 16 Based on dose of: 1g q12h 1g every 8h or 2g every 8 h Do not give 2g q12 Total dose 2g 3-4g 6g NA Table 2: 2014 MIC Interpretive Standards for Pseudomonas aeruginosa and Acinetobacter spp. -

Antibacterial Drug Usage Analysis
Department of Health and Human Services Public Health Service Food and Drug Administration Center for Drug Evaluation and Research Office of Surveillance and Epidemiology Drug Use Review Date: April 5, 2012 To: Edward Cox, M.D. Director Office of Antimicrobial Products Through: Gerald Dal Pan, M.D., MHS Director Office of Surveillance and Epidemiology Laura Governale, Pharm.D., MBA Deputy Director for Drug Use Division of Epidemiology II Office of Surveillance and Epidemiology Hina Mehta, Pharm.D. Drug Use Data Analysis Team Leader Division of Epidemiology II Office of Surveillance and Epidemiology From: Tracy Pham, Pharm.D. Drug Use Data Analyst Division of Epidemiology II Office of Surveillance and Epidemiology Drug Name(s): Systemic Antibacterial Drug Products Application Type/Number: Multiple Applicant/sponsor: Multiple OSE RCM #: 2012-544 **This document contains proprietary drug use data obtained by FDA under contract. The drug use data/information in this document has been cleared for public release.** 1 EXECUTIVE SUMMARY The Division of Epidemiology II is providing an update of the drug utilization data in terms of number of kilograms or international units of selected systemic antibacterial drug products sold from manufacturers to various retail and non-retail channels of distribution for years 2010-2011 as a surrogate for nationwide antibacterial drug use in humans. Propriety drug use databases licensed by the FDA were used to conduct this analysis. Data findings are as follows: During years 2010 and 2011, the majority of kilograms of selected systemic antibacterial drug products sold were to outpatient retail pharmacy settings. Approximately 3.28 million kilograms of selected systemic antibacterial drug products were sold during year 2010, and around 3.29 million kilograms were sold during year 2011. -

Consideration of Antibacterial Medicines As Part Of
Consideration of antibacterial medicines as part of the revisions to 2019 WHO Model List of Essential Medicines for adults (EML) and Model List of Essential Medicines for children (EMLc) Section 6.2 Antibacterials including Access, Watch and Reserve Lists of antibiotics This summary has been prepared by the Health Technologies and Pharmaceuticals (HTP) programme at the WHO Regional Office for Europe. It is intended to communicate changes to the 2019 WHO Model List of Essential Medicines for adults (EML) and Model List of Essential Medicines for children (EMLc) to national counterparts involved in the evidence-based selection of medicines for inclusion in national essential medicines lists (NEMLs), lists of medicines for inclusion in reimbursement programs, and medicine formularies for use in primary, secondary and tertiary care. This document does not replace the full report of the WHO Expert Committee on Selection and Use of Essential Medicines (see The selection and use of essential medicines: report of the WHO Expert Committee on Selection and Use of Essential Medicines, 2019 (including the 21st WHO Model List of Essential Medicines and the 7th WHO Model List of Essential Medicines for Children). Geneva: World Health Organization; 2019 (WHO Technical Report Series, No. 1021). Licence: CC BY-NC-SA 3.0 IGO: https://apps.who.int/iris/bitstream/handle/10665/330668/9789241210300-eng.pdf?ua=1) and Corrigenda (March 2020) – TRS1021 (https://www.who.int/medicines/publications/essentialmedicines/TRS1021_corrigenda_March2020. pdf?ua=1). Executive summary of the report: https://apps.who.int/iris/bitstream/handle/10665/325773/WHO- MVP-EMP-IAU-2019.05-eng.pdf?ua=1. -

Management of Penicillin and Beta-Lactam Allergy
Management of Penicillin and Beta-Lactam Allergy (NB Provincial Health Authorities Anti-Infective Stewardship Committee, September 2017) Key Points • Beta-lactams are generally safe; allergic and adverse drug reactions are over diagnosed and over reported • Nonpruritic, nonurticarial rashes occur in up to 10% of patients receiving penicillins. These rashes are usually not allergic and are not a contraindication to the use of a different beta-lactam • The frequently cited risk of 8 to 10% cross-reactivity between penicillins and cephalosporins is an overestimate based on studies from the 1970’s that are now considered flawed • Expect new intolerances (i.e. any allergy or adverse reaction reported in a drug allergy field) to be reported after 0.5 to 4% of all antimicrobial courses depending on the gender and specific antimicrobial. Expect a higher incidence of new intolerances in patients with three or more prior medication intolerances1 • For type-1 immediate hypersensitivity reactions (IgE-mediated), cross-reactivity among penicillins (table 1) is expected due to similar core structure and/or major/minor antigenic determinants, use not recommended without desensitization • For type-1 immediate hypersensitivity reactions, cross-reactivity between penicillins (table 1) and cephalosporins is due to similarities in the side chains; risk of cross-reactivity will only be significant between penicillins and cephalosporins with similar side chains • Only type-1 immediate hypersensitivity to a penicillin manifesting as anaphylaxis, bronchospasm, -

Antibiotic Use for Sepsis in Neonates and Children: 2016 Evidence Update
Antibiotic Use for Sepsis in Neonates and Children: 2016 Evidence Update Aline Fuchsa, Julia Bielickia,b, Shrey Mathurb, Mike Sharlandb, Johannes N. Van Den Ankera,c a Paediatric Pharmacology and Pharmacometrics, University Children's Hospital Basel, Basel, Switzerland b Paediatric Infectious Disease Research Group, Institute for Infection and Immunity, St George's University of London, London, United Kingdom c Division of Clinical Pharmacology, Children’s National Health System, Washington, DC, USA WHO-Reviews 1 TABLE OF CONTENTS 1. INTRODUCTION ............................................................................................................................... 3 1.1. Aims ......................................................................................................................................... 3 1.2. Background ............................................................................................................................. 3 1.2.1. Definition and diagnosis ................................................................................................. 3 Neonatal Sepsis ............................................................................................................................... 3 Paediatric Sepsis ............................................................................................................................. 4 Community versus hospital acquired sepsis .................................................................................. 5 1.2.2. Microbiology .................................................................................................................. -

Comparative Activity of Newer Antibiotics Against Gram-Negative Bacilli
CONTRIBUTION • Comparative activity of newer antibiotics against gram-negative bacilli CYNTHIA C. KNAPP, MS AND JOHN A. WASHINGTON, MD • The in vitro activities of cefoperazone, cefotaxime, ceftriaxone, ceftazidime, azlocillin, mezlocillin, piperacillin, ticarcillin/clavulanate, aztreonam, imipenem, and ciprofloxacin were concurrently deter- mined against over 1,000 isolates of gram-negative bacilli from clinical specimens of patients at the Cleve- land Clinic. Cephalosporins, penicillins, and aztreonam were active against species of Enterobacteriaceae other than Citrobacter freundii, Enterobacter aerogenes, and Enterobacter cloacae. Ceftazidime was the most active cephalosporin against Pseudomonas aeruginosa. Against the Enterobacteriaceae, the rank order of activity of penicillins was ticarcillin/clavulanate > piperacillin > mezlocillin > azlocillin. Against P. aer- uginosa, the rank order of activity of penicillins was piperacillin > ticarcillin/clavulanate > azlocillin > mezlocillin. Aztreonam was less active v P. aeruginosa than ceftazidime, cefoperazone, or piperacillin. The most active antimicrobials against all isolates tested were imipenem and ciprofloxacin. • INDEX TERMS: ANTIBIOTICS, LACTAM; GRAM-NEGATIVE BACTERIA • CLEVE CLIN J MED 1989; 56:161-166 HE RECENT introduction of ciprofloxacin for and penicillins, as well as the monobactam, aztreonam, clinical use follows closely a period of active re- and the carbapenem, imipenem.1-3 search in and development of expanded spec- We compared the susceptibility of more than 1,000 trum p-lactam antibiotics, including cephalo- clinical bacterial isolates to four expanded spectrum Tsporins, penicillins, monobactams, and carbapenems. cephalosporins (cefoperazone, cefotaxime, ceftriaxone, Although numerous published studies compare the ac- and ceftazidime), four expanded spectrum penicillins tivity of ciprofloxacin with other quinolones, only a (azlocillin, mezlocillin, piperacillin, and ticarcil- limited number of studies compare the activity of ci- lin/clavulanate), aztreonam, imipenem, and ciproflox- acin. -

Evaluation of Pharmacodynamic Interactions Between Telavancin
Infect Dis Ther DOI 10.1007/s40121-016-0121-2 ORIGINAL RESEARCH Evaluation of Pharmacodynamic Interactions Between Telavancin and Aztreonam or Piperacillin/ Tazobactam Against Pseudomonas aeruginosa, Escherichia coli and Methicillin-Resistant Staphylococcus aureus Juwon Yim . Jordan R. Smith . Katie E. Barber . Jessica A. Hallesy . Michael J. Rybak Received: May 2, 2016 Ó The Author(s) 2016. This article is published with open access at Springerlink.com ABSTRACT Methods: In vitro one-compartment PK/PD models were run over 96 h simulating TLV Introduction: In clinical trials comparing 10 mg/kg every 48 h, ATM 500 mg every 8 h telavancin (TLV) with vancomycin for and PTZ continuous infusion 13.5 g over 24 h treatment of hospital-acquired pneumonia, alone and in combination against P. aeruginosa, TLV demonstrated lower clinical cure rates E. coli and methicillin-resistant S. aureus than vancomycin in patients who had mixed (MRSA). The efficacy of antimicrobials was gram-positive and -negative infections and were evaluated by plotting time-kill curves and concomitantly treated with either aztreonam calculating the reduction in log10 cfu/ml over (ATM) or piperacillin/tazobactam (PTZ). Here, 96 h. we investigated therapeutic interactions Results: Against both MRSA strains, TLV was between TLV and ATM or PTZ in an in vitro rapidly bactericidal at 4 h and maintained its pharmacokinetic/pharmacodynamic (PK/PD) activity over 96 h with no observed antagonism model under simulated reduced renal function by either ATM or PTZ. PTZ maintained conditions. bacteriostatic and bactericidal activities against Enhanced content To view enhanced content for this E. coli ATCC 25922 and clinical strain R1022 at article go to http://www.medengine.com/Redeem/ 96 h, whereas both strains regrew as soon as 22E4F0603737CC9F. -

Ceftaroline in Complicated Skin and Skin-Structure Infections
Infection and Drug Resistance Dovepress open access to scientific and medical research Open Access Full Text Article REVIEW Ceftaroline in complicated skin and skin-structure infections Paul O Hernandez1 Abstract: Ceftaroline is an advanced-generation cephalosporin antibiotic recently approved by Sergio Lema2 the US Food and Drug Administration for the treatment of complicated skin and skin-structure Stephen K Tyring3 infections (cSSSIs). This intravenous broad-spectrum antibiotic exerts potent bactericidal activity Natalia Mendoza2,4 by inhibiting bacterial cell wall synthesis. A high affinity for the penicillin-binding protein 2a (PBP2a) of methicillin-resistant Staphylococcus aureus (MRSA) makes the drug especially 1University of Texas School of Medicine at San Antonio, beneficial to patients with MRSA cSSSIs. Ceftaroline has proved in multiple well-conducted San Antonio, TX, 2Woodhull clinical trials to have an excellent safety and efficacy profile. In adjusted doses it is also recom- Medical and Mental Health Center, mended for patients with renal or hepatic impairment. Furthermore, the clinical effectiveness Brooklyn, NY, 3Department of Dermatology, University of Texas and high cure rate demonstrated by ceftaroline in cSSSIs, including those caused by MRSA Health Science Center at Houston, and other multidrug-resistant strains, warrants its consideration as a first-line treatment option 4 Houston, TX, USA; Department of for cSSSIs. This article reviews ceftaroline and its pharmacology, efficacy, and safety data to Dermatology, El -

Ertapenem Or Ticarcillin/Clavulanate for the Treatment of Intra-Abdominal Infections Or Acute Pelvic Infections in Pediatric Patients
The American Journal of Surgery 194 (2007) 367–374 Clinical surgery–American Ertapenem or ticarcillin/clavulanate for the treatment of intra-abdominal infections or acute pelvic infections in pediatric patients Albert E. Yellin, M.D.a,*, Jeffrey Johnson, M.D.b, Iliana Higareda, M.D.c, Blaise L. Congeni, M.D.d, Antonio C. Arrieta, M.D.e, Doreen Fernsler, B.S.f, Joseph West, Ph.D.f, Richard Gesser, M.D.f aDepartment of Surgery, Keck School of Medicine of the University of Southern California, 1200 N State St, Rm 9610, Los Angeles, CA 90033, USA bDepartment of Pediatrics, Keck School of Medicine of the University of Southern California, 1240 N Mission Rd, L902, Los Angeles, CA 90089-9300, USA cHospital Civil de Guadalajara, Hospital 278, 4420 El Retiro St, Guadalajara, Jalisco Mexico dAkron Children’s Hospital, Division of Infectious Diseases, Locust Professional Bldg, 300 Locust St, Ste 4, Akron, OH 44308-1062, USA eChildren’s Hospital of Orange County, Pediatric Infectious Diseases, 455 South Main Street, Orange, CA 92868, USA fMerck Research Laboratories, Merck & Co., Inc., 126 East Lincoln Avenue, Rahway, NJ 07065, USA Manuscript received June 20, 2006; revised manuscript January 20, 2007 Abstract Background: Ertapenem, a group I carbapenem antibiotic, has been shown to be safe and effective in treating adults with complicated intra-abdominal (cIAI) or acute pelvic infection (API). This study evaluated ertapenem for treating these infections in children. Methods: In an open-label study, children aged 2 to 17 years with cIAI or API were randomized 3:1 to receive ertapenem or ticarcillin/clavulanate. -

Real-World Use of Telavancin in the Treatment of Osteomyelitis
Diagnostic Microbiology and Infectious Disease 95 (2019) 185–190 Contents lists available at ScienceDirect Diagnostic Microbiology and Infectious Disease journal homepage: www.elsevier.com/locate/diagmicrobio Real-world use of telavancin in the treatment of osteomyelitis Louis D. Saravolatz a,⁎, Kerry O. Cleveland b, Khalid Rikabi c, Ali Hassoun d, Joseph Reilly e, Leonard B. Johnson a, Cedric Spak f, Sharon Valenti a, Susan Szpunar a a Ascension-St John Hospital and Wayne State University School of Medicine, Grosse Pointe Woods, Michigan, USA b University of Tennessee, Mephis Tennessee, USA c Geographic Medicine Services of Biloxi, Biloxi, Mississippi, USA d Alabama Infectious Diseases Center, Huntsville, Alabama, USA e AtlantiCare Regional Medical Center, Pomona, NJ, USA f North Texas Disease Consultants, Dallas, Texas, USA article info abstract Article history: This is a retrospective analysis of patients with osteomyelitis who received telavancin at some time during their Received 30 November 2018 treatment course. The primary outcome was the percent of patients cured or improved at the end of telavancin Received in revised form 17 May 2019 therapy (EOTT). The secondary outcome was the percent of patients cured or improved three months after dis- Accepted 18 May 2019 continuation of telavancin therapy. There were 32 cases of osteomyelitis with methicillin-resistant Staphylococ- Available online 28 May 2019 cus aureus identified in 17 (56.7%), methicillin-sensitive Staphylococcus aureus 2(6.6%), coagulase negative Keywords: staphylococci 6 (20.0%) and other pathogens, 5 (16.7%). At EOTT, 87.5% of patients had their osteomyelitis Telavancin cured and 94.6% had the infection cured at three months after telavancin was completed.