Aminocaproic Acid Tablets, USP Rx Only
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

CSI Study Guide-Female and Male Exams
Guide for Skill Station Female & Male Exams 2019 1. Overview Students will have the opportunity to perform female and male GU exams using both mannequins and standardized patients. The female standardized patient GU exam will include the external genitalia and pelvic exam, including use of a speculum; Male GU exam will include hernia and external genitalia/testicular examination. Practice session using mannequin will include evaluation of the prostate. Also refer to the Female and Male Exam – Factsheet 2019 for additional simulation lab session instructions 2. Goal of the Procedure Accurately perform female and male GU exams using proper techniques and logical sequence, while providing for patient comfort and modesty. 3. Reference(s) Jarvis, C. (2016). Physical Examination and Health Assessment. (7th ed.). Philadelphia: Elsevier. 4. Required Reading / Review Begin by reviewing the materials from 609a Health Assessment: a. Panoptos: Week 11 Male Genitourinary System: Anus, Rectum, Prostate: Male Genital Exam Week 12 Female Genital exam b. Jarvis, C. (2016). Physical Examination and Health Assessment. Pocket Guide (7th ed.). Philadelphia: Elsevier. Use above link, then use your UA Net ID Credentials to sign into the library, then click view full text, navigate to below chapters • Chapter 17 Male Genitourinary System pp 225-236; 12 pages • Chapter 18 Female Genitourinary System pp 237-252; 16 pages • Chapter 19 Anus, Rectum, and Prostate pp 253-260; 8 pages 5. Required Procedure Competencies Professionalism 1. Present/on time 2. Prepared (readings, etc.) 3. Engaged and participated 4. Respectful of others Communication skills 1. Obtain name and age of the patient and relationship of others if present 2. -

Table of Contents
viii Contents Chapter 1. Taking the Certification Examination . 1 General Suggestions for Preparing for the Exam About the Certification Exams Chapter 2. Developmental and Behavioral Sciences . 11 Mary Jo Gilmer, PhD, MBA, RN-BC, FAAN, and Paula Chiplis, PhD, RN, CPNP Psychosocial, Cognitive, and Ethical-Moral Development Behavior Modification Physical Development: Normal Growth Expectations and Developmental Milestones Family Concepts and Issues Family-Centered Care Cultural and Spiritual Diversity Chapter 3. Communication . 23 Mary Jo Gilmer, PhD, MBA, RN-BC, FAAN, and Karen Corlett, MSN, RN-BC, CPNP-AC/PC, PNP-BC Culturally Sensitive Communication Components of Therapeutic Communication Communication Barriers Modes of Communication Patient Confidentiality Written Communication in Nursing Practice Professional Communication Advocacy Chapter 4. The Nursing Process . 33 Clara J. Richardson, MSN, RN–BC Nursing Assessment Nursing Diagnosis and Treatment Chapter 5. Basic and Applied Sciences . 49 Mary Jo Gilmer, PhD, MBA, RN-BC, FAAN, and Paula Chiplis, PhD, RN, CPNP Trauma and Diseases Processes Common Genetic Disorders Common Childhood Diseases Traction Pharmacology Nutrition Chemistry Clinical Signs Associated With Isotonic Dehydration in Infants ix Chapter 6. Educational Principles and Strategies . 69 Mary Jo Gilmer, PhD, MBA, RN-BC, FAAN, and Karen Corlett, MSN, RN-BC, CPNP-AC/PC, PNP-BC Patient Education Chapter 7. Life Situations and Adaptive and Maladaptive Responses . 75 Mary Jo Gilmer, PhD, MBA, RN-BC, FAAN, and Karen Corlett, MSN, RN-BC, CPNP-AC/PC, PNP-BC Palliative Care End-of-Life Care Response to Crisis Chapter 8. Sensory Disorders . 87 Clara J. Richardson, MSN, RN–BC Developmental Characteristics of the Pediatric Sensory System Hearing Disorders Vision Disorders Conjunctivitis Otitis Media and Otitis Externa Retinoblastoma Trauma to the Eye Chapter 9. -

Study Guide Medical Terminology by Thea Liza Batan About the Author
Study Guide Medical Terminology By Thea Liza Batan About the Author Thea Liza Batan earned a Master of Science in Nursing Administration in 2007 from Xavier University in Cincinnati, Ohio. She has worked as a staff nurse, nurse instructor, and level department head. She currently works as a simulation coordinator and a free- lance writer specializing in nursing and healthcare. All terms mentioned in this text that are known to be trademarks or service marks have been appropriately capitalized. Use of a term in this text shouldn’t be regarded as affecting the validity of any trademark or service mark. Copyright © 2017 by Penn Foster, Inc. All rights reserved. No part of the material protected by this copyright may be reproduced or utilized in any form or by any means, electronic or mechanical, including photocopying, recording, or by any information storage and retrieval system, without permission in writing from the copyright owner. Requests for permission to make copies of any part of the work should be mailed to Copyright Permissions, Penn Foster, 925 Oak Street, Scranton, Pennsylvania 18515. Printed in the United States of America CONTENTS INSTRUCTIONS 1 READING ASSIGNMENTS 3 LESSON 1: THE FUNDAMENTALS OF MEDICAL TERMINOLOGY 5 LESSON 2: DIAGNOSIS, INTERVENTION, AND HUMAN BODY TERMS 28 LESSON 3: MUSCULOSKELETAL, CIRCULATORY, AND RESPIRATORY SYSTEM TERMS 44 LESSON 4: DIGESTIVE, URINARY, AND REPRODUCTIVE SYSTEM TERMS 69 LESSON 5: INTEGUMENTARY, NERVOUS, AND ENDOCRINE S YSTEM TERMS 96 SELF-CHECK ANSWERS 134 © PENN FOSTER, INC. 2017 MEDICAL TERMINOLOGY PAGE III Contents INSTRUCTIONS INTRODUCTION Welcome to your course on medical terminology. You’re taking this course because you’re most likely interested in pursuing a health and science career, which entails proficiencyincommunicatingwithhealthcareprofessionalssuchasphysicians,nurses, or dentists. -

The Genitourinary System I
U.S. ARMY MEDICAL DEPARTMENT CENTER AND SCHOOL FORT SAM HOUSTON, TEXAS 78234-6100 THE GENITOURINARY SYSTEM I SUBCOURSE MD0579 EDITION 100 DEVELOPMENT This subcourse is approved for resident and correspondence course instruction. It reflects the current thought of the Academy of Health Sciences and conforms to printed Department of the Army doctrine as closely as currently possible. Development and progress render such doctrine continuously subject to change. ADMINISTRATION Students who desire credit hours for this correspondence subcourse must enroll in the subcourse. Application for enrollment should be made at the Internet website: http://www.atrrs.army.mil. You can access the course catalog in the upper right corner. Enter School Code 555 for medical correspondence courses. Copy down the course number and title. To apply for enrollment, return to the main ATRRS screen and scroll down the right side for ATRRS Channels. Click on SELF DEVELOPMENT to open the application; then follow the on-screen instructions. For comments or questions regarding enrollment, student records, or examination shipments, contact the Nonresident Instruction Branch at DSN 471-5877, commercial (210) 221-5877, toll-free 1-800-344-2380; fax: 210-221-4012 or DSN 471-4012, e-mail [email protected], or write to: NONRESIDENT INSTRUCTION BRANCH AMEDDC&S ATTN: MCCS-HSN 2105 11TH STREET SUITE 4191 FORT SAM HOUSTON TX 78234-5064 Be sure your social security number is on all correspondence sent to the Academy of Health Sciences. CLARIFICATION OF TERMINOLOGY When used in this publication, words such as "he," "him," "his," and "men" 'are intended to include both the masculine and feminine genders, unless specifically stated otherwise or when obvious in context. -

Medical Terminology
MEDICAL TERMINOLOGY TRI-COUNTY REGIONAL OCCUPATIONAL PROGRAM CDE COURSE 2268 CBEDS #4298 Description: This course is an introduction to medical terminology for those preparing for a health or business career such as nursing, medical secretary, ward secretary, emergency medical technician, respiratory therapist, or any other field requiring a medical vocabulary. This course articulates with the Yuba College 2+2 program, and is designed to meet the prerequisites for our ROP Vocational Nursing class and is one of the requirements for the Medical Office Services (MA) and Health Care Information Services courses. Performance Objectives: Upon completion of the Medical Terminology course, the student will understand: 1. The basic elements of a medical word. 2. Suffixes related surgical, diagnostic, symptomatic medical words. 3. Suffixes relative to medical words including adjectives, nouns, diminutives, singular and plural words. 4. Prefixes of medical words. 5. Medical words that define the human body in relation to disease processes, the four body planes, body cavities and organs, abdominopelvic regions, and demonstrating understanding of body imaging by defining terms associated with radiology, computed tomography, MRI and ultrasounds. 6. Medical words that identify the functions and body parts associated with the integumentary system. 7. Medical words that describe and define the gastrointestinal system. 8. Medical words that define and describe the respiratory system. 9. Medical words that define and describe the cardiovascular system. 10. Medical words that define and describe blood and lymphatic systems. 11. Medical words that define and describe the musculoskeletal system. 12. Medical words that define and describe the genitourinary system. 13. Medical words that define and describe the female reproductive system. -
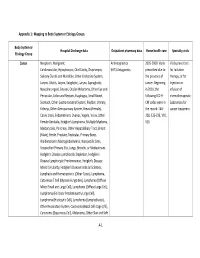
A-1 Appendix 1
Appendix 1: Mapping to Body System or Etiology Groups Body System or Hospital Discharge data Outpatient pharmacy data Home health care Specialty visits Etiology Group Cancer Neoplasm, Malignant: Antineoplastics 2005 -2009: Visits Visits prescribed Cardiovascular, Hypopharynx, Oral Cavity, Oropharynx, 5HT3 Antagonists prescribed due to for radiation Salivary Glands and Mandible, Other Endocrine System, the presence of therapy, or for Larynx, Glottis, Larynx, Subglottic, Larynx, Supraglottic, cancer. Beginning Injection or Nasopharyngeal, Sinuses, Ocular Melanoma, Other Eye and in 2010, the infusion of Periocular, Colon and Rectum, Esophagus, Small Bowel, following ICD-9- chemotherapeutic Stomach, Other Gastrointestinal System, Bladder, Urinary, CM codes were in Substances for Kidneys, Other Genitourinary System, Breast (Female), the record: 140- cancer treatment Cervix Uteri, Endometrium, Ovaries, Vagina, Vulva, Other 208, 235-239, V10, Female Genitalia, Hodgkin's Lymphoma, Multiple Myeloma, V16 Mastocytosis, Pancreas, Other Hepatobiliary Tract, Breast (Male), Penile, Prostate, Testicular, Primary Bone, Waldenstrom's Macroglobulinemia, Nonspecific Sites, Unspecified Primary Site, Lungs, Bronchi, or Mediastinum, Hodgkin's Disease Lymphocytic Depletion, Hodgkin's Disease Lymphocytic Predominance, Hodgkin's Disease Mixed Cellularity, Hodgkin's Disease Nodular Sclerosis, Lymphatic and Hematopoietic (Other Types), Lymphoma, Cutaneous T Cell (Mycosis Fungoides), Lymphoma (Diffuse Mixed Small and Large Cell), Lymphoma (Diffuse Large Cell), Lymphoma -
![The Genitourinary System (And] Instructor's Guide: the Genitourinary System](https://docslib.b-cdn.net/cover/6525/the-genitourinary-system-and-instructors-guide-the-genitourinary-system-1156525.webp)
The Genitourinary System (And] Instructor's Guide: the Genitourinary System
DOCUMENT RESUME ED 213 968 CE 031 777 TITLE The Genitourinary System (and] Instructor's Guide: The Genitourinary System. Health Occupations Education Module: Instructional Materials in Anatomy and Physiology for Pennsylvania Health Occupations Programs. INSTITUTION National Evaluation Systems, Inc., Amherst, Mass. SPONS AGENCY Pennsylvania State Dept. of Education, Harrisburg. Bureau of Vocational and Technical Education. PUB DATE atm 80 NOTE 33p.; For related documents see listing in note of CE 031 758. EDRS PRICE MF01/PCO2 Plus Postage. DESCRIPTORS ' *Allied Health Occupations Education; *Anatomy; Behaviorpl Objectives; *Individualized Instruction; *Learning Activities; Learning Modules; *Males; Medical Vocabulary; *Physiology; Postsecondary Education; Pretests Posttests; Programed Instructional Materials; Secondary Education; Self Evaluation (Individuals); Teaching Methods IDENTIFIERS *Genitourinary System; Pennsylvania ABSTRACT This module on the genitourinary system is one of 17 modules designed for individualized instruction in health occupations education programs at both the secondary and postsecondary levels. It is part of an eight-unit miniseries on anatomy, and physiology within the series of 17 modules. Following a preface which explains to the student how to use the module, the unit consists of a pretest with answers, three sections (information sheets) with their objectives (e.g., identify and describe the location and anatomical structure of the kidneys), optional activities (e.g., research the process of _____dialysi-sby an artificial kidney machine), and posttests, and a glossary of terms. Topics covered in the unit are introduction to the genitourinary system, the urinary system, and the male reproductive system. An accompanying instructor's guide Contains suggestions for using the module and answers to the posttest. (KC) *********************************************************************** * Reproductions supplied by EDRS are the best that can be made * * from the original document. -

Association of Syndactyly, Ectodermal Dysplasia, and Cleft Lip and Palate: Report of Two Sibs from Turkey
J Med Genet: first published as 10.1136/jmg.25.1.37 on 1 January 1988. Downloaded from Journal of Medical Genetics 1988, 25, 37-40 Association of syndactyly, ectodermal dysplasia, and cleft lip and palate: report of two sibs from Turkey GONUL O(UR AND MEMNUNE YUKSEL From the Institute of Child Health, University of Istanbul, (7apa/lIstanbul, Turkey. SUMMARY Two Turkish sibs, products of a second cousin marriage, with tetramelic syndactyly, ectodermal dysplasia, cleft lip and palate, renal anomalies, and mental retardation are reported. Similarities between these two brothers and previously reported cases and their mode of transmission are discussed. In 1961, Rosselli and Gulienettil reported four was said to have a cleft lip deformity. Unfortunately patients with hypohidrosis, hypotrichosis, micro- no more details were available. The family's first dontia, dystrophic nails, cleft lip and palate, deform- offspring was aborted in early pregnancy. The ities of the extremities, and malformations of the second, a healthy boy, is 11 years old. The third genitourinary system. Syndactyly was the predomi- pregnancy ended as a stillbirth but had no congenital nant digital deformity. Phenotypically normal par- malformations. The fourth and fifth children are our copyright. ents who were first cousins suggested an autosomal probands. recessive mode of inheritance in two of their cases who were sibs. In 1970, a very similar clinical CASE 1 condition was described as the EEC syndrome The older son (IV.4, fig 1) was born on 24.11.77, (ectrodactyly-ectodermal dysplasia-cleft lip/palate) weighing 2300 g, after a normal 32 week gestation. by Rudiger et a12 and Freire-Maia3 almost simul- No perinatal complications were observed. -

Unilateral Renal Agenesis in a Neonate with Congenital Diaphragmatic Hernia
Cent. Eur. J. Med. • 8(3) • 2013 • 358-361 DOI: 10.2478/s11536-013-0152-y Central European Journal of Medicine Unilateral renal agenesis in a neonate with congenital diaphragmatic hernia Case Report Kyoung Hee Han1, Kwang Sig Kim2, Jee Won Chang3, Young Don Kim1 1 Department of Pediatrics, Jeju National University Hospital, Aran 13gil 15, Jeju city, Jeju Special Self-Governing Province, 690-767, Korea 2 Department of Surgery, Jeju National University Hospital, Aran 13gil 15, Jeju city, Jeju Special Self-Governing Province, 690-767, Korea 3 Department of Thoracic Surgery, Jeju National University Hospital, Aran 13gil 15, Jeju city, Jeju Special Self-Governing Province, 690-767, Korea Received 6 December 2012; Accepted 31 January 2013 Abstract: Congenital diaphragmatic hernia (CDH) is a rare and severe disorder with a high mortality rate among infants. Unilateral renal agenesis (URA) is a relatively common congenital urinary malformation. Here, we present the case of a newborn infant with left CDH associated with ipsilateral renal agenesis. The male patient was born weighing 3.850 g through normal spontaneous vaginal delivery at 38 weeks and 6 days of gestational age at a maternity hospital. He was transferred to our neonatal intensive care unit due to respiratory distress with tachypnea, grunting and cyanosis after birth. A chest radiography indicated parts of the bowel in the thoracic cavity, consistent with CDH. Renal ultrasonography indicated no kidney structure on the left side and a 5.6 cm right kidney with normal echogenicity. Repair of the diaphragmatic hernia was performed three days after birth. Most of the colon, small bowel, stomach and spleen were located in the left pleural cavity, but the left kidney was not seen. -

EEC Syndrome and Genitourinary Anomalies: an Update Saskiazyxwvutsrqponmlkjihgfedcbazyxwvutsrqponmlkjihgfedcba M
American Journal of Medical Genetics 63:472-478 (1996) EEC Syndrome and Genitourinary Anomalies: An Update SaskiazyxwvutsrqponmlkjihgfedcbaZYXWVUTSRQPONMLKJIHGFEDCBA M. Maas, Tom P.V.M. de Jong, Paul Buss, and Raoul C.M. Hennekam Department of Pediatrics (S.M.M., R.C.M.H.) and Institute of Human Genetics (R.C.M.H.),zyxwvutsrqponmlkjihgfedcbaZYXWVUTSRQPONMLKJIHGFEDCBA Academic Medical Center, Amsterdam; Department of Pediatric Urology (T.P.V.M.d.J.),zyxwvutsrqponmlkjihgfedcbaZYXWVUTSRQPONMLKJIHGFEDCBA University Hospital for Children and Youth, “Het Wilhelmina Kinderziekenhuis.” Utrecht, The Netherlands; Institute of Medical Genetics (P.B.), University of Wales, CardifL United Kingdom We report on a large family with the ec- Structural anomalies of the genitourinary (GU) tract trodactyly, ectodermal dysplasia, clefting may also be part of the clinical spectrum of the EEC (EEC) syndrome. The clinical manifesta- syndrome. Rosselli and Gulienetti [ 19611 were probably tions in this family show great variability. the first to describe structural anomalieszyxwvutsrqponmlkjihgfedcbaZYXWVUTSRQPONMLKJIHGFEDCBA of the GU sys- Specific genitourinary anomalies were tem as an associated finding in a patient, and Preus found. The propositus with micturition and Fraser [ 19731 suggested that structural anomalies problems is discussed in detail. A dysplastic of the kidney may be an integral component of the EEC bladder epithelium might be the cause of syndrome. A summary of all GU anomalies described in these problems. A remarkable improvement patients with the EEC syndrome is provided in Table I. of the complaints was achieved upon treat- In several texts, GU anomalies are either cited as only ment with synthetic sulfonated glycos- occasional findings in EEC syndrome [Temtamy and aminoglycans. 0 1996 Wiley-Liss, Inc. -

Imaging Findings Ofneonatal Adrenal Disorders 1
J Korean Radiol Soc 1999 ; 40: 173-179 Imaging Findings ofNeonatal Adrenal Disorders 1 Hye-Kyung Yoon, M.D., Bokyung Kim Han, M.D., Min Hee Lee, M.D. In newborn infants, normal adrenal glands are characterized by a relatively thin echogenic center surrounded by a thick, hypoechoic cortical rim as seen on ultrasound (US). Various disorders involving the neonatal adrenal gland include ad renal hemorrhage, hyperplasia, cyst, Wolman’s disease, and congenital neuro blastoma. Adrenal hemorrhage is the most common cause of an adrenal mass in the neonate, though differentiation between adrenal hemorrhage and neuroblastoma is in many cases difficult. We describe characteristic US, CT and MR imaging findings in neonates with various adrenal disorders. Index words : Infants, newborn, genitourinary system Adrenal gland, abnormalities Neonatal adrenal glands are clearJy demonstrated on uJtrasound (US) using high-freguency linear or phased Normal Neonatal Adrenal Glands array transducers. The normaJ neonataJ adrenaJ gland is clearly seen on postnatal abdominal sonograms, The appearance of neonatal adrenal glands varies; consisting of an echolucent cortex and a thinner they may be lambdoid, V- or Y-shaped, and are rela echogenic centraJ med ull a. AdrenaJ hemorrhage is the tively large (1). On US, corticomeduJJ ary differen most common adrenal mass in neonates. US is used as tiation is evident, with an outer echolucent cortex and the initiaJ modaJity for diagnosing adrenaJ hemor a central echogenic line representing the medulla (Fig. rhage, the appearance -

Genitourinary System
10/27/2016 PANCE/PANRE Review Course Genitourinary System Carolyn Ducoff, PA-C Rutgers, The State University of New Jersey PANCE/PANRE Review Course Neoplastic Diseases of the GU Tract PANCE/PANRE Review Course Testicular Cancer Image Courtesy of de:Benutzer:Hasehttp://commons.wikimedia.org 1 10/27/2016 PANCE/PANRE Review Course Testicular Carcinoma • Clinical Considerations Risks: Cryptorchidism (increases risk x40!) White > African Asian Americans (+) FH (+) Personal Hx 95% are Germ Cell Tumors: Seminomas and Nonseminomas Most common neoplasm in males 15-35 yo PANCE/PANRE Review Course Testicular Cancer Signs/Symptoms Painless testicular mass or testicular enlargement, R > L side Metastatic Signs Retroperitoneal Nodes Flank Pain Mediastinum and Lung cough, chest pain, shortness of breath Brain Headaches and CNS symptoms PANCE/PANRE Review Course Testicular Carcinoma • Labs: Nonseminomas (65%) Seminomas (35%) βHCG ↑↑↑ ↑ AFP ↑ NOT ELEVATED LDH ↑↑ • Imaging Scrotal ultrasound Surveillance of mets and staging CT of the abdomen and pelvis CXR or CT of the chest MRI of the brain 2 10/27/2016 PANCE/PANRE Review Course Testicular Cancer Treatment: Radical orchiectomy for everyone Seminomas: Add XBRT +/- Chemo (cisplatin) Nonseminomas: Surveillance, May add Chemo. NOT responsive to XBRT Prognosis excellent 90-95% cure rate (71% with mets) PANCE/PANRE Review Course 2nd Most common CA 2nd most common CA death in U.S. men Public Domain Image Source: Flickr: Nelson Mandela http://commons.wikimedia.org 1 in 6 men diagnosed in lifetime Slow growing