Heidenhain's Syndrome) by A
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Diseases/Symptoms Reported to Be Associated with Lyme Disease
Diseases/Symptoms Reported to be Associated with Lyme Disease Abdominal pseudo-eventration Abdominal wall weakness Acrodermatitis chronica atrophicans (ACA) Acute Acral Ischemia Acute conduction disorders Acute coronary syndrome Acute exogenous psychosis Acute febrile illness Acute hemiparesis Acute ischaemic pontine stroke Acute meningitis Acute myelo-meningo-radiculitis Acute myelitis Acute pediatric monoarticular arthritis Acute peripheral facial palsy Acute perimyocarditis Acute posterior multifocal placoid pigment epitheliopathy (APMPPE) Acute pyogenic arthritis Acute reversible diffuse conduction system disease Acute septic arthritis Acute severe encephalitis Acute transitory auriculoventricular block Acute transverse myelitis Acute urinary retention Acquired Immune Deficiency Syndrome (AIDS) Algodystrophy Allergic conditions Allergic conjunctivitis Alopecia Alzheimer’s Disease Amyotrophic lateral sclerosis (ALS - Lou Gehrig's Disease) Amyotrophy Anamnesis Anetoderma Anorexia nervosa Anterior optic neuropathy Antepartum fever Anxiety Arrhythmia Arthralgia Arthritis Asymmetrical hearing loss Ataxic sensory neuropathy Atraumatic spontaneous hemarthrosis Atrioventricular block Attention Deficit Disorder (ADD) Attention Deficit Hyperactivity Disorder (ADHD) Back pain without radiculitis Bannwarth’s Syndrome Behcet's disease Bell’s Palsy Benign cutaneous lymphocytoma Benign lymphocytic infiltration (Jessner-Kanof) Bilateral acute confluent disseminated choroiditis Bilateral carpal tunnel syndrome Bilateral facial nerve palsy Bilateral -

55400-Neuropathdementiav5
08/11/2019 Bodian silver method Neuropathology of the Dementia Spectrum Charles Duyckaerts Escourolle Neuropathology Lab Alzheimer-Prion team ICM Pitié-Salpêtrière Senile plaquePitié-Salpêtrière Neurofibrillary tangle 12 Aβ accumulation + tauopathy = Alzheimer disease (please note: no neuronal loss in criteria) Pitié-Salpêtrière Pitié-Salpêtrière 34 1 08/11/2019 BRAAK STAGES : tau pathology THAL PHASES : Aβ pathology I II 1 23 III IV 4 5 V VI Braak and Braak. Acta Neuropathol 1991 Thal et al. Neurology 2002 Pitié-Salpêtrière Pitié-Salpêtrière 56 Pick’s circumscribed atrophy Pitié-Salpêtrière α-synuclein IHC Pitié-Salpêtrière 78 2 08/11/2019 Dementia (~1920) Alzheimer disease Pick disease (Pick circumscribed atrophy) Alzheimer A (1911) Uber eigenartige Krankheitsfälle des späteren Alters. Zentralblatt Gesam Neurol Psychiat 4: 356- Pitié-Salpêtrière Pitié-Salpêtrière 385 910 Pick disease Pick disease (Pick body disease) is also a tauopathy Tau IHC Pitié-Salpêtrière Pitié-Salpêtrière 11 12 3 08/11/2019 Fronto-temporal dementia with 1- behavioral changes 2- semantic dementia 3- progressive non-fluent aphasia Pick disease (with Pick bodies) « Pick without Pick body » R. Escourolle. 1957 & S. Brion Type C of Tissot, Constantinidis & Richard, 1975 Previously « Atypical Pick disease » Knopman DS, Mastri AR, Frei WH, Sung JH, Rustan T (1990) Dementia lacking distinctive histologic feature: a common non-Alzheimer degenerative dementia. Neurology 40: 251-256 Pitié-Salpêtrière Pitié-Salpêtrière 13 14 Mutations in the tau gene in frontotemporal dementia -

Case Report Reversible Cortical Blindness and Convulsions with Cyclosporin a Toxicity in a Patient Undergoing Allogeneic Peripheral Stem Cell Transplantation
Bone Marrow Transplantation, (1997) 20, 793–795 1997 Stockton Press All rights reserved 0268–3369/97 $12.00 Case report Reversible cortical blindness and convulsions with cyclosporin A toxicity in a patient undergoing allogeneic peripheral stem cell transplantation B Madan and SA Schey Department of Haematology, Guy’s Hospital, London, UK Summary: one course each of MACE (mitozantrone on days 1, 3 and 5, cytosine arabinoside on days 1–10, etoposide on days 1– A 40-year-old woman underwent allogeneic peripheral 5) and ICE (idarubicin on days 1 and 2, cytosine arabino- blood stem cell transplantation for relapsed AML-M6. side on days 1–3, etoposide on days 1–3). She achieved She developed graft-versus-host disease on day +15 complete remission after her first induction but relapsed post-transplant, for which she was treated with cyclo- within 1 month of completion of ICE chemotherapy. In sporin A and methyl prednisolone. On day +19 she March 1996 she was given mitoxantrone, cytosine arabino- developed cortical blindness, headache and convulsions side and PSC-833 (a cyclosporin D analogue) as per relapse which were associated with white matter changes on protocol and achieved complete remission. In July 1996, MRI scanning of the head and elevated cyclosporin A she received an allogeneic peripheral stem cell transplant levels. A diagnosis of cyclosporin A encephalopathy was from her HLA-identical sister following conditioning with made and cyclosporin A was discontinued. Her vision cyclophosphamide and total body irradiation. She received recovered completely after 48 h and the other symptoms cyclosporin A as prophylaxis for graft-versus-host disease. -

Cortical Blindness: Etiology, Diagnosis, and Prognosis
Cortical Blindness: Etiology, Diagnosis, and Prognosis Michael S. Aldrich, MD," Anthony G. Alessi, MD," Roy W. Beck, MD,$ and Sid Gilman, MDI We examined 15 patients with cortical blindness, reviewed the records of 10 others, and compared these 25 patients to those in previous studies of cortical blindness. Although cerebrovascular disease was the most common cause in ow series, surgery, particularly cardiac surgery, and cerebral angiography were also major causes. Only 3 patients denied their blindness, although 4 others were unaware of their visual loss. Electroencephalograms (EEGs) were performed during the period of blindness in 20 patients and all recordings were abnormal, with absent alpha rhythm. Visual evoked potentials recorded during blindness were abnormal in 15 of 19 patients, but did not correlate with the severity of visual loss or with outcome. Bioccipital lucencies were found in computed tomographic (CT) scans of 14 patients; none of the 14 regained good vision. Recovery of vision was poor in all 8 patients who had a spontaneous stroke, but fair or good in 11 of the other 17 patients. Prognosis was best in patients under the age of 40 years, in those without a history of hypertension or diabetes mellitus, and in those without associated cognitive, language, or memory impair- ments. We conclude that (1) the prognosis in cortical blindness is poor when caused by stroke; (2) EEGs are more useful than visual evoked potentials for diagnosis; and (3) bioccipital abnormalities shown on CT scan are associated with a poor prognosis. Aldrich MS, Alessi AG, Beck RW, Gilman S: Cortical blindness: etiology, diagnosis, and prognosis. -

Bilateral Cortical Blindness Due to Bilateral Occipital Infarcts Without Anosognosia
Journal of Neurology & Stroke Bilateral Cortical Blindness due to Bilateral Occipital Infarcts without Anosognosia Abstract Case Report Bilateral cortical blindness refers to the total loss of vision in the presence of Volume 4 Issue 1- 2016 normal pupillary reflexes and in the absence of Ophthalmological disease resulting from bilateral lesions of the striate cortex in the occipital lobes. In most cases, these patients deny their blindness and their behavior is as if they have an intact vision. We report the case of an 84-year-old man with bilateral cortical blindness resulting from bilateral occipital lobe infarcts. The patient presented this infrequent clinical condition after acute bilateral infarction of the occipital 1First Propedeutic Department of Internal Medicine, lobes possibly due to cardiac embolism resulting from atrial fibrillation of Aristotle University of Thessaloniki, Greece unknown duration. Subcutaneous administration of low molecular weight heparin 2First Department of Neurology, Aristotle University of in therapeutic doses resulted in neurological improvement in the first four days. Thessaloniki, Greece Interestingly, the visual symptoms were complicated neither by anosognosia 3First Department of Ophthalmology, Aristotle University of nor by memory impairment. Cortical blindness and Anton’s syndrome should Thessaloniki, Greece be considered in patients with atypical visual loss and evidence of occipital lobe 4Department of Radiology, Aristotle University of injury. Cerebrovascular disease could be the background -

THE CLINICAL ASSESSMENT of the PATIENT with EARLY DEMENTIA S Cooper, J D W Greene V15
J Neurol Neurosurg Psychiatry: first published as 10.1136/jnnp.2005.081133 on 16 November 2005. Downloaded from THE CLINICAL ASSESSMENT OF THE PATIENT WITH EARLY DEMENTIA S Cooper, J D W Greene v15 J Neurol Neurosurg Psychiatry 2005;76(Suppl V):v15–v24. doi: 10.1136/jnnp.2005.081133 ementia is a clinical state characterised by a loss of function in at least two cognitive domains. When making a diagnosis of dementia, features to look for include memory Dimpairment and at least one of the following: aphasia, apraxia, agnosia and/or disturbances in executive functioning. To be significant the impairments should be severe enough to cause problems with social and occupational functioning and the decline must have occurred from a previously higher level. It is important to exclude delirium when considering such a diagnosis. When approaching the patient with a possible dementia, taking a careful history is paramount. Clues to the nature and aetiology of the disorder are often found following careful consultation with the patient and carer. A focused cognitive and physical examination is useful and the presence of specific features may aid in diagnosis. Certain investigations are mandatory and additional tests are recommended if the history and examination indicate particular aetiologies. It is useful when assessing a patient with cognitive impairment in the clinic to consider the following straightforward questions: c Is the patient demented? c If so, does the loss of function conform to a characteristic pattern? c Does the pattern of dementia conform to a particular pattern? c What is the likely disease process responsible for the dementia? An understanding of cognitive function and its anatomical correlates is necessary in order to ascertain which brain areas are affected. -

Patients with Cortical Blindness Who Do Not Have Any Residual Functional Vision, Talking Devices Can Be Given, I.E
Title: Reading Ability spared in a case of Acquired Cortical Blindness, Neuroplasticity or Left posterior occipitotemporal sulcus sparing? Authors: Kim Ly, OD, Andrea L. Murphy, OD, FAAO Dorothy L. Hitchmoth, OD, FAAO, ABO, ABCMO Abstract: A patient with complete cortical blindness, as a result of sequential, bilateral occipital strokes, is able to read with occasional accuracy despite no evidence of macular field sparing and no light perception bilaterally. Case History Patient Demographics and Social History: o 58 year-old white male presents to his visit: . Accompanied by his ex-wife . Using sighted guide and a rolling walker for ambulation . Reporting he is in the process of moving in with his son for full-time caregiver support, previously homeless Chief Complaint o Primary complaint of loss of vision: . Started about 1 year ago after a “stroke” . Patient reports loss of vision following: the left half of his visual field in his left eye and "less than one half" in his right eye . A second stroke two months ago caused “complete blindness” . Patient and ex-wife report that patient can still read on occasion, i.e. directions on their car's GPS system or brochures o Secondary Complaint: . Gritty eyes that burn throughout the day Ocular History o Blindness OU o Patient did not report any other ocular history Medical History o Cerebrovascular accident (CVA) of the right occipital lobe secondary to cardiac embolus formation as a result of atrial fibrillation 10/2015 o Cerebrovascular accident affecting the left occipital lobe 6/2016 -

Recurrent Posterior Reversible Encephalopathy Syndrome (PRES)
Journal of Human Hypertension (2004) 18, 287–289 & 2004 Nature Publishing Group All rights reserved 0950-9240/04 $25.00 www.nature.com/jhh CASE REPORT Recurrent posterior reversible encephalopathy syndrome (PRES) G Hagemann1, T Ugur1, OW Witte1 and C Fitzek2 1Department of Neurology, Friedrich-Schiller-University, Jena, Germany; 2Institute of Diagnostic and Interventional Radiology, Friedrich-Schiller-University, Jena, Germany Posterior reversible encephalopathy syndrome is a drome is usually fully reversible. We report a case of proposed cliniconeuroradiological entity characterized recurrent PRES of unknown aetiology following inten- by headache, altered mental status, cortical blindness, sive care unit treatment and only moderately elevated seizures, and other focal neurological signs, and a blood pressure. Clinicians as well as radiologists must diagnostic magnetic resonance imaging picture. A be familiar with this clinically frightening, underdiag- variety of different etiologies have been reported like nosed condition to assure timely diagnosis and treat- hypertension, pre-eclampsia/eclampsia, cyclosporin A ment to prevent persistent deficits. or tacrolimus neurotoxicity, uraemia and porphyria. Journal of Human Hypertension (2004) 18, 287–289. With early diagnosis and prompt treatment, the syn- doi:10.1038/sj.jhh.1001664 Keywords: PRES; reversible encephalopathy; cortical blindness Introduction ferred to a normal ward, she showed a fluctuating agitated confusional state that was accounted for as Posterior reversible encephalopathy syndrome a prolonged alcohol withdrawal syndrome. She was (PRES) is a proposed cliniconeuroradiological entity 1,2 given vitamins, haloperidol and benzodiazepines with a vast spectrum of different aetiologies. The and gradually recovered. After 27 days, she was able clinical hallmark of this syndrome are headache, to walk a few steps without assistance, was fully confusion, seizures, cortical visual disturbances or orientated and did not show any focal neurological blindness and, less common, other focal neurologi- abnormality. -

(12) Patent Application Publication (10) Pub. No.: US 2013/0197002 A1 Staubli Et Al
US 2013 O1970O2A1 (19) United States (12) Patent Application Publication (10) Pub. No.: US 2013/0197002 A1 Staubli et al. (43) Pub. Date: Aug. 1, 2013 (54) BRIMONDINE FOR TREATING VISUAL Publication Classification DSORDERS MEDIATED BY CENTRAL VISUAL PROJECTIONS FROM THE EYE (51) Int. Cl. (71) Applicant: Allergan, Inc., Irvine, CA (US) A613 L/498 (2006.01) (52) U.S. Cl. (72) Inventors: Ursula Staubli, Laguna Beach, CA CPC .................................... A6 IK3I/498 (2013.01) (US); Alan C. Foster, San Diego, CA (US); Daniel W. Gil, Corona Del Mar, USPC .......................................................... S14/249 CA (US); John E. Donello, Dana Point, CA (US) (57) ABSTRACT (73) Assignee: ALLERGAN, INC. Irvine, CA (US) (21) Appl. No.: 13/752,871 The present invention relates to a method for treating visual (22) Filed: Jan. 29, 2013 disorders mediated by lateral geniculate nucleus, Superior Related U.S. Application Data colliculus and the visual cortex by administering to a patient (60) Provisional application No. 61/592,115, filed on Jan. in need of Such treatment, compounds acting at the alpha 2 30, 2012. adrenergic receptor. Patent Application Publication Aug. 1, 2013 Sheet 1 of 3 US 2013/O197002 A1 FIGURE 1 100 8 O 6 O 4. O 2 O Contro O.3 nM 3 nM 30 nM 300 nM 8 O 6 O 4. O 2 O 100 nM Atip 39 gig, 30 nM. Brimo Patent Application Publication Aug. 1, 2013 Sheet 2 of 3 US 2013/O197002 A1 FIGURE 2 p = 0.05 (paired t-test) Patent Application Publication Aug. 1, 2013 Sheet 3 of 3 US 2013/O197002 A1 FIGURE 3 : 22-23 weeks post Blue Light US 2013/O 197002 A1 Aug. -

Sudden Loss of Vision Investigation and Management
THEME VISION AT RISK Lucy Goold Shane Durkin John Crompton MBBS, MMed(OphthSc), is ophthalmology MBBS(Hons), MPHC, MMed(OphthSc), is MBBS, FRANZCO, FRACS, is Associate resident and Associate Clinical Lecturer, South ophthalmology registrar and Associate Professor and Department Head, Australian Institute of Ophthalmology, Royal Clinical Lecturer, South Australian Department of Neurophthalmology, South Adelaide Hospital, South Australia. lgoold@ Institute of Ophthalmology, Royal Australian Institute of Ophthalmology, Royal med.usyd.edu.au Adelaide Hospital, South Australia. Adelaide Hospital, South Australia. Sudden loss of vision Investigation and management Investigation and management should be determined Background depending on the findings from the history and examination. Sudden vision loss usually requires urgent ophthalmic Several of the more common and potentially sight or life assessment. Diagnosis and management requires the judicious threatening aetiologies will be discussed here, although this use of a wide range of serological and imaging investigations to guide appropriate treatment and referral. is not an exhaustive list. Many of the conditions discussed will cause temporary visual loss and several may become Objective permanent, particularly if not promptly managed. This article follows on from the previous discussion of the role of history and examination to discuss the appropriate investigation Giant cell arteritis and management of common causes of sudden visual loss. Suspicion of giant cell arteritis (GCA) in the setting of sudden visual Discussion loss in a patient over 50 years of age should prompt immediate The key historical and examination findings have now been referral for ophthalmic review. Patients should have their erythrocyte extracted and synthesised and these inform the next step. -
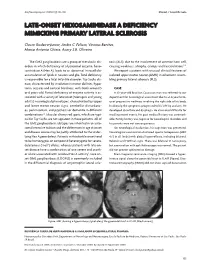
Late-Onset Hexosaminidase a Deficiency Mimicking Primary Lateral Sclerosis
Arq Neuropsiquiatr 2009;67(1):105-106 Clinical / Scientific note late-onSet hexoSaminidaSe a defiCienCy mimiCking primary lateral SCleroSiS Clecio Godeiro-Junior, Andre C. Felicio, Vinicius Benites, Marco Antonio Chieia, Acary S.B. Oliveira The GM2 gangliosidosis are a group of metabolic dis- rosis (ALS), due to the involvement of anterior horn cell, orders in which deficiency of a lysosomal enzyme, hexo- causing weakness, atrophy, cramps and fasciculations3,4. saminidase A (Hex A), leads to an abnormal intracellular We report a patient with unusual clinical features of accumulation of lipids in neurons and glia. Total deficiency isolated upper motor neuron (UMN) involvement, resem- is responsible for a fatal infantile disorder, Tay-Sachs dis- bling primary lateral sclerosis (PLS). ease, characterized by involution in motor abilities, hypo- tonia, seizures and cortical blindness, with death around 5 CaSe or 6 years-old. Partial deficiency of enzyme activity is as- A 30-year-old Brazilian Caucasian man was referred to our sociated with a variety of late-onset (teenagers and young department for neurological assessment due to an 8-year histo- adults) neurological phenotypes, characterized by upper ry of progressive weakness involving the right side of his body. and lower motor neuron signs, cerebellar disturbanc- Insidiously, the symptoms progressed to his left leg and arm. He es, parkinsonism, and psychosis or dementia in different developed dysarthria and dysphagia. He also noted difficulty for combinations1,2. Macular cherry red spots, which are typi- recalling recent events. His past medical history was unremark- cal for Tay-Sachs, are not apparent in these patients. All of able. -

Neuropsychiatry Review Series: Disorders of Visual Perception. Dominic Ffytche, Jan Dirk Blom, Marco Catani
Neuropsychiatry Review series: Disorders of Visual perception. Dominic Ffytche, Jan Dirk Blom, Marco Catani To cite this version: Dominic Ffytche, Jan Dirk Blom, Marco Catani. Neuropsychiatry Review series: Disorders of Visual perception.. Journal of Neurology, Neurosurgery and Psychiatry, BMJ Publishing Group, 2010, 81 (11), pp.1280. 10.1136/jnnp.2008.171348. hal-00587980 HAL Id: hal-00587980 https://hal.archives-ouvertes.fr/hal-00587980 Submitted on 22 Apr 2011 HAL is a multi-disciplinary open access L’archive ouverte pluridisciplinaire HAL, est archive for the deposit and dissemination of sci- destinée au dépôt et à la diffusion de documents entific research documents, whether they are pub- scientifiques de niveau recherche, publiés ou non, lished or not. The documents may come from émanant des établissements d’enseignement et de teaching and research institutions in France or recherche français ou étrangers, des laboratoires abroad, or from public or private research centers. publics ou privés. Disorders of visual perception Dr Dominic H ffytche1,4* Dr JD Blom2,3 4 Dr M Catani 1 Department of Old Age Psychiatry, Institute of Psychiatry, King’s College London, UK 2 Parnassia Bavo Group, The Hague, the Netherlands 3 Department of Psychiatry, University of Groningen, Groningen, the Netherlands 4 Natbrainlab, Department of Forensic and Neurodevelopmental Sciences, Institute of Psychiatry, King’s College London, UK *Address for Correspondence Dr D H ffytche Department of Old Age Psychiatry, Institute of Psychiatry PO70, King’s College