Blood Donor Variability Is a Modulatory Factor for P. Falciparum Invasion Phenotyping Assays Laty G
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

(CD147) Is Induced by C/Ebpβ and Is Differentially Expressed in ALK+
Laboratory Investigation (2017) 97, 1095–1102 © 2017 USCAP, Inc All rights reserved 0023-6837/17 EMMPRIN (CD147) is induced by C/EBPβ and is differentially expressed in ALK+ and ALK − anaplastic large-cell lymphoma Janine Schmidt1, Irina Bonzheim1, Julia Steinhilber1, Ivonne A Montes-Mojarro1, Carlos Ortiz-Hidalgo2, Wolfram Klapper3, Falko Fend1 and Leticia Quintanilla-Martínez1 Anaplastic lymphoma kinase-positive (ALK+) anaplastic large-cell lymphoma (ALCL) is characterized by expression of oncogenic ALK fusion proteins due to the translocation t(2;5)(p23;q35) or variants. Although genotypically a T-cell lymphoma, ALK+ ALCL cells frequently show loss of T-cell-specific surface antigens and expression of monocytic markers. C/EBPβ, a transcription factor constitutively overexpressed in ALK+ ALCL cells, has been shown to play an important role in the activation and differentiation of macrophages and is furthermore capable of transdifferentiating B-cell and T-cell progenitors to macrophages in vitro. To analyze the role of C/EBPβ for the unusual phenotype of ALK+ ALCL cells, C/EBPβ was knocked down by RNA interference in two ALK+ ALCL cell lines, and surface antigen expression profiles of these cell lines were generated using a Human Cell Surface Marker Screening Panel (BD Biosciences). Interesting candidate antigens were further analyzed by immunohistochemistry in primary ALCL ALK+ and ALK − cases. Antigen expression profiling revealed marked changes in the expression of the activation markers CD25, CD30, CD98, CD147, and CD227 after C/EBPβ knockdown. Immunohistochemical analysis confirmed a strong, membranous CD147 (EMMPRIN) expression in ALK+ ALCL cases. In contrast, ALK − ALCL cases showed a weaker CD147 expression. -

Human and Mouse CD Marker Handbook Human and Mouse CD Marker Key Markers - Human Key Markers - Mouse
Welcome to More Choice CD Marker Handbook For more information, please visit: Human bdbiosciences.com/eu/go/humancdmarkers Mouse bdbiosciences.com/eu/go/mousecdmarkers Human and Mouse CD Marker Handbook Human and Mouse CD Marker Key Markers - Human Key Markers - Mouse CD3 CD3 CD (cluster of differentiation) molecules are cell surface markers T Cell CD4 CD4 useful for the identification and characterization of leukocytes. The CD CD8 CD8 nomenclature was developed and is maintained through the HLDA (Human Leukocyte Differentiation Antigens) workshop started in 1982. CD45R/B220 CD19 CD19 The goal is to provide standardization of monoclonal antibodies to B Cell CD20 CD22 (B cell activation marker) human antigens across laboratories. To characterize or “workshop” the antibodies, multiple laboratories carry out blind analyses of antibodies. These results independently validate antibody specificity. CD11c CD11c Dendritic Cell CD123 CD123 While the CD nomenclature has been developed for use with human antigens, it is applied to corresponding mouse antigens as well as antigens from other species. However, the mouse and other species NK Cell CD56 CD335 (NKp46) antibodies are not tested by HLDA. Human CD markers were reviewed by the HLDA. New CD markers Stem Cell/ CD34 CD34 were established at the HLDA9 meeting held in Barcelona in 2010. For Precursor hematopoetic stem cell only hematopoetic stem cell only additional information and CD markers please visit www.hcdm.org. Macrophage/ CD14 CD11b/ Mac-1 Monocyte CD33 Ly-71 (F4/80) CD66b Granulocyte CD66b Gr-1/Ly6G Ly6C CD41 CD41 CD61 (Integrin b3) CD61 Platelet CD9 CD62 CD62P (activated platelets) CD235a CD235a Erythrocyte Ter-119 CD146 MECA-32 CD106 CD146 Endothelial Cell CD31 CD62E (activated endothelial cells) Epithelial Cell CD236 CD326 (EPCAM1) For Research Use Only. -

Cellular and Molecular Signatures in the Disease Tissue of Early
Cellular and Molecular Signatures in the Disease Tissue of Early Rheumatoid Arthritis Stratify Clinical Response to csDMARD-Therapy and Predict Radiographic Progression Frances Humby1,* Myles Lewis1,* Nandhini Ramamoorthi2, Jason Hackney3, Michael Barnes1, Michele Bombardieri1, Francesca Setiadi2, Stephen Kelly1, Fabiola Bene1, Maria di Cicco1, Sudeh Riahi1, Vidalba Rocher-Ros1, Nora Ng1, Ilias Lazorou1, Rebecca E. Hands1, Desiree van der Heijde4, Robert Landewé5, Annette van der Helm-van Mil4, Alberto Cauli6, Iain B. McInnes7, Christopher D. Buckley8, Ernest Choy9, Peter Taylor10, Michael J. Townsend2 & Costantino Pitzalis1 1Centre for Experimental Medicine and Rheumatology, William Harvey Research Institute, Barts and The London School of Medicine and Dentistry, Queen Mary University of London, Charterhouse Square, London EC1M 6BQ, UK. Departments of 2Biomarker Discovery OMNI, 3Bioinformatics and Computational Biology, Genentech Research and Early Development, South San Francisco, California 94080 USA 4Department of Rheumatology, Leiden University Medical Center, The Netherlands 5Department of Clinical Immunology & Rheumatology, Amsterdam Rheumatology & Immunology Center, Amsterdam, The Netherlands 6Rheumatology Unit, Department of Medical Sciences, Policlinico of the University of Cagliari, Cagliari, Italy 7Institute of Infection, Immunity and Inflammation, University of Glasgow, Glasgow G12 8TA, UK 8Rheumatology Research Group, Institute of Inflammation and Ageing (IIA), University of Birmingham, Birmingham B15 2WB, UK 9Institute of -
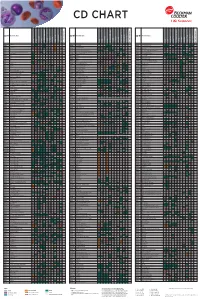
Flow Reagents Single Color Antibodies CD Chart
CD CHART CD N° Alternative Name CD N° Alternative Name CD N° Alternative Name Beckman Coulter Clone Beckman Coulter Clone Beckman Coulter Clone T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells T Cells B Cells Granulocytes NK Cells Macrophages/Monocytes Platelets Erythrocytes Stem Cells Dendritic Cells Endothelial Cells Epithelial Cells CD1a T6, R4, HTA1 Act p n n p n n S l CD99 MIC2 gene product, E2 p p p CD223 LAG-3 (Lymphocyte activation gene 3) Act n Act p n CD1b R1 Act p n n p n n S CD99R restricted CD99 p p CD224 GGT (γ-glutamyl transferase) p p p p p p CD1c R7, M241 Act S n n p n n S l CD100 SEMA4D (semaphorin 4D) p Low p p p n n CD225 Leu13, interferon induced transmembrane protein 1 (IFITM1). p p p p p CD1d R3 Act S n n Low n n S Intest CD101 V7, P126 Act n p n p n n p CD226 DNAM-1, PTA-1 Act n Act Act Act n p n CD1e R2 n n n n S CD102 ICAM-2 (intercellular adhesion molecule-2) p p n p Folli p CD227 MUC1, mucin 1, episialin, PUM, PEM, EMA, DF3, H23 Act p CD2 T11; Tp50; sheep red blood cell (SRBC) receptor; LFA-2 p S n p n n l CD103 HML-1 (human mucosal lymphocytes antigen 1), integrin aE chain S n n n n n n n l CD228 Melanotransferrin (MT), p97 p p CD3 T3, CD3 complex p n n n n n n n n n l CD104 integrin b4 chain; TSP-1180 n n n n n n n p p CD229 Ly9, T-lymphocyte surface antigen p p n p n -

No Evidence for Basigin/CD147 As a Direct SARS-Cov-2 Spike
www.nature.com/scientificreports OPEN No evidence for basigin/CD147 as a direct SARS‑CoV‑2 spike binding receptor Jarrod Shilts 1*, Thomas W. M. Crozier 2, Edward J. D. Greenwood2, Paul J. Lehner 2 & Gavin J. Wright 1,3* The spike protein of SARS‑CoV‑2 is known to enable viral invasion into human cells through direct binding to host receptors including ACE2. An alternate entry receptor for the virus was recently proposed to be basigin/CD147. These early studies have already prompted a clinical trial and multiple published hypotheses speculating on the role of this host receptor in viral infection and pathogenesis. Here, we report that we are unable to fnd evidence supporting the role of basigin as a putative spike binding receptor. Recombinant forms of the SARS‑CoV‑2 spike do not interact with basigin expressed on the surface of human cells, and by using specialized assays tailored to detect receptor interactions as weak or weaker than the proposed basigin‑spike binding, we report no evidence for a direct interaction between the viral spike protein to either of the two common isoforms of basigin. Finally, removing basigin from the surface of human lung epithelial cells by CRISPR/Cas9 results in no change in their susceptibility to SARS‑CoV‑2 infection. Given the pressing need for clarity on which viral targets may lead to promising therapeutics, we present these fndings to allow more informed decisions about the translational relevance of this putative mechanism in the race to understand and treat COVID‑19. Te sudden emergence of SARS-CoV-2 in late 2019 has demanded extensive research be directed to resolve the many uncharted aspects of this previously-unknown virus. -

2021 Code Changes Reference Guide
Boston University Medical Group 2021 CPT Code Changes Reference Guide Page 1 of 51 Background Current Procedural Terminology (CPT) was created by the American Medical Association (AMA) in 1966. It is designed to be a means of effective and dependable communication among physicians, patients, and third-party payers. CPT provides a uniform coding scheme that accurately describes medical, surgical, and diagnostic services. CPT is used for public and private reimbursement systems; development of guidelines for medical care review; as a basis for local, regional, and national utilization comparisons; and medical education and research. CPT Category I codes describe procedures and services that are consistent with contemporary medical practice. Category I codes are five-digit numeric codes. CPT Category II codes facilitate data collection for certain services and test results that contribute to positive health outcomes and quality patient care. These codes are optional and used for performance management. They are alphanumeric five-digit codes with the alpha character F in the last position. CPT Category III codes represent emerging technologies. They are alphanumeric five-digit codes with the alpha character T in the last position. The CPT Editorial Panel, appointed by the AMA Board of Trustees, is responsible for maintaining and updating the CPT code set. Purpose The AMA makes annual updates to the CPT code set, effective January 1. These updates include deleted codes, revised codes, and new codes. It’s important for providers to understand the code changes and the impact those changes will have to systems, workflow, reimbursement, and RVUs. This document is meant to assist you with this by providing a summary of the changes; a detailed breakdown of this year’s CPT changes by specialty, and HCPCS Updates for your reference. -

Whole Exome Sequencing in Families at High Risk for Hodgkin Lymphoma: Identification of a Predisposing Mutation in the KDR Gene
Hodgkin Lymphoma SUPPLEMENTARY APPENDIX Whole exome sequencing in families at high risk for Hodgkin lymphoma: identification of a predisposing mutation in the KDR gene Melissa Rotunno, 1 Mary L. McMaster, 1 Joseph Boland, 2 Sara Bass, 2 Xijun Zhang, 2 Laurie Burdett, 2 Belynda Hicks, 2 Sarangan Ravichandran, 3 Brian T. Luke, 3 Meredith Yeager, 2 Laura Fontaine, 4 Paula L. Hyland, 1 Alisa M. Goldstein, 1 NCI DCEG Cancer Sequencing Working Group, NCI DCEG Cancer Genomics Research Laboratory, Stephen J. Chanock, 5 Neil E. Caporaso, 1 Margaret A. Tucker, 6 and Lynn R. Goldin 1 1Genetic Epidemiology Branch, Division of Cancer Epidemiology and Genetics, National Cancer Institute, NIH, Bethesda, MD; 2Cancer Genomics Research Laboratory, Division of Cancer Epidemiology and Genetics, National Cancer Institute, NIH, Bethesda, MD; 3Ad - vanced Biomedical Computing Center, Leidos Biomedical Research Inc.; Frederick National Laboratory for Cancer Research, Frederick, MD; 4Westat, Inc., Rockville MD; 5Division of Cancer Epidemiology and Genetics, National Cancer Institute, NIH, Bethesda, MD; and 6Human Genetics Program, Division of Cancer Epidemiology and Genetics, National Cancer Institute, NIH, Bethesda, MD, USA ©2016 Ferrata Storti Foundation. This is an open-access paper. doi:10.3324/haematol.2015.135475 Received: August 19, 2015. Accepted: January 7, 2016. Pre-published: June 13, 2016. Correspondence: [email protected] Supplemental Author Information: NCI DCEG Cancer Sequencing Working Group: Mark H. Greene, Allan Hildesheim, Nan Hu, Maria Theresa Landi, Jennifer Loud, Phuong Mai, Lisa Mirabello, Lindsay Morton, Dilys Parry, Anand Pathak, Douglas R. Stewart, Philip R. Taylor, Geoffrey S. Tobias, Xiaohong R. Yang, Guoqin Yu NCI DCEG Cancer Genomics Research Laboratory: Salma Chowdhury, Michael Cullen, Casey Dagnall, Herbert Higson, Amy A. -

Host Genetics and Infectious Disease: New Tools, Insights and Translational Opportunities
REVIEWS Host genetics and infectious disease: new tools, insights and translational opportunities Andrew J. Kwok 1, Alex Mentzer 1,2 and Julian C. Knight 1 ✉ Abstract | Understanding how human genetics influence infectious disease susceptibility offers the opportunity for new insights into pathogenesis, potential drug targets, risk stratification, response to therapy and vaccination. As new infectious diseases continue to emerge, together with growing levels of antimicrobial resistance and an increasing awareness of substantial differences between populations in genetic associations, the need for such work is expanding. In this Review, we illustrate how our understanding of the host–pathogen relationship is advancing through holistic approaches, describing current strategies to investigate the role of host genetic variation in established and emerging infections, including COVID-19, the need for wider application to diverse global populations mirroring the burden of disease, the impact of pathogen and vector genetic diversity and a broad array of immune and inflammation phenotypes that can be mapped as traits in health and disease. Insights from study of inborn errors of immunity and multi-omics profiling together with developments in analytical methods are further advancing our knowledge of this important area. Penetrance Disease syndromes caused by infectious agents have A seminal study of adoptees in the 1980s reported 1 The proportion of individuals occurred throughout the history of modern humans . increased risk of death from infectious disease in chil- with a particular genotype As a result of our continued interactions with patho- dren whose biological parents succumbed to an infec- that also has an associated gens, our genomes have been shaped through processes tious disease7, highlighting the significance of human phenotype. -

Development and Validation of a Protein-Based Risk Score for Cardiovascular Outcomes Among Patients with Stable Coronary Heart Disease
Supplementary Online Content Ganz P, Heidecker B, Hveem K, et al. Development and validation of a protein-based risk score for cardiovascular outcomes among patients with stable coronary heart disease. JAMA. doi: 10.1001/jama.2016.5951 eTable 1. List of 1130 Proteins Measured by Somalogic’s Modified Aptamer-Based Proteomic Assay eTable 2. Coefficients for Weibull Recalibration Model Applied to 9-Protein Model eFigure 1. Median Protein Levels in Derivation and Validation Cohort eTable 3. Coefficients for the Recalibration Model Applied to Refit Framingham eFigure 2. Calibration Plots for the Refit Framingham Model eTable 4. List of 200 Proteins Associated With the Risk of MI, Stroke, Heart Failure, and Death eFigure 3. Hazard Ratios of Lasso Selected Proteins for Primary End Point of MI, Stroke, Heart Failure, and Death eFigure 4. 9-Protein Prognostic Model Hazard Ratios Adjusted for Framingham Variables eFigure 5. 9-Protein Risk Scores by Event Type This supplementary material has been provided by the authors to give readers additional information about their work. Downloaded From: https://jamanetwork.com/ on 10/02/2021 Supplemental Material Table of Contents 1 Study Design and Data Processing ......................................................................................................... 3 2 Table of 1130 Proteins Measured .......................................................................................................... 4 3 Variable Selection and Statistical Modeling ........................................................................................ -

Targets to Watch for SARS-Cov-2 and COVID-19
Drugs of the Future 2020, 45(4): 1-6 (Advanced Publication) Copyright © 2020 Clarivate Analytics CCC: 0377-8282/2020 DOI: 10.1358/dof.2020.45.4.3150676 Targets to Watch Taking aim at a fast-moving target: targets to watch for SARS-CoV-2 and COVID-19 L.A. Sorbera, A.I. Graul and C. Dulsat Clarivate Analytics, Barcelona, Spain Contents six coronaviruses had been known to cause disease in humans: HCoV-229E, HCoV-OC43, HCoV-NL63, HCoV-HKU1, Summary ........................................... 1 severe acute respiratory syndrome coronavirus (SARS-CoV) Introduction ........................................ 1 and Middle East respiratory virus coronavirus (MERS-CoV). SARS-CoV-2 and COVID-19 ............................ 1 The first four are endemic locally; they have been associ- Targets ............................................. 2 ated mainly with mild, self-limiting disease, whereas the latter two—both betacoronaviruses—can cause severe References .......................................... 5 illness (1-3). Given the high prevalence and wide distribution of coro- naviruses, their large genetic diversity as well as the fre- Summary quent recombination of their genomes, and increasing Severe acute respiratory syndrome coronavirus 2 (SARS- activity at the human–animal interface, these viruses CoV-2) is characterized as a betacoronavirus and recog- represent an ongoing threat to human health (4). This fact nized as the seventh discrete coronavirus species capable of recently became starkly evident, with the emergence and causing human disease. This new coronavirus causes febrile rapid spread of a novel coronavirus, first in mainland China respiratory illness and on March 11, 2020, was character- and now globally. The virus—provisionally designated ized as a global pandemic. Investigators have accelerated 2019-nCoV and later given the official name SARS-CoV-2, the search for a vaccine to prevent infection and for agents due to its similarity to SARS-CoV—was quickly isolated to treat it. -

Glycophorins and the MNS Blood Group System: a Narrative Review
16 Review Article Page 1 of 16 Glycophorins and the MNS blood group system: a narrative review Genghis H. Lopez1,2, Catherine A. Hyland1,3, Robert L. Flower1,3 1Clinical Services and Research Division, Australian Red Cross Lifeblood, Kelvin Grove, Queensland, Australia; 2School of Medical Science, Griffith Health, Griffith University, Gold Coast, Queensland, Australia; 3School of Biomedical Sciences, Faculty of Health, Queensland University of Technology, Brisbane, Queensland, Australia Contributions: (I) Conception and design: All authors; (II) Administrative support: None; (III) Provision of study materials or patients: None; (IV) Collection and assembly of data: All authors; (V) Data analysis and interpretation: All authors; (VI) Manuscript writing: All authors; (VII) Final approval of manuscript: All authors. Correspondence to: Genghis H. Lopez, PhD. Clinical Services and Research Division, Australian Red Cross Lifeblood, 44 Musk Avenue, Kelvin Grove, Queensland 4059, Australia. Email: [email protected]. Abstract: The MNS blood group system, International Society of Blood Transfusion (ISBT) 002, is second after the ABO system. GYPA and GYPB genes encode MNS blood group antigens carried on glycophorin A (GPA), glycophorin B (GPB), or on variant glycophorins. A third gene, GYPE, produce glycophorin E (GPE) but is not expressed. MNS antigens arise from several genetic mechanisms. Single nucleotide variants (SNVs) contribute to the diversity of the MNS system. A new antigen SUMI (MNS50), p.Thr31Pro on GPA has been described in the Japanese population. Unequal crossing-over and gene conversion are the mechanisms forming hybrid glycophorins, usually from parent genes GYPA and GYPB. GYPE also contributes to gene recombination previously only described with GYPA. Recently, however, GYPE was shown to recombine with GYPB to form a GYP(B-E-B) hybrid. -
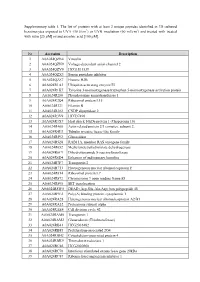
Supplementary Table 1. the List of Proteins with at Least 2 Unique
Supplementary table 1. The list of proteins with at least 2 unique peptides identified in 3D cultured keratinocytes exposed to UVA (30 J/cm2) or UVB irradiation (60 mJ/cm2) and treated with treated with rutin [25 µM] or/and ascorbic acid [100 µM]. Nr Accession Description 1 A0A024QZN4 Vinculin 2 A0A024QZN9 Voltage-dependent anion channel 2 3 A0A024QZV0 HCG1811539 4 A0A024QZX3 Serpin peptidase inhibitor 5 A0A024QZZ7 Histone H2B 6 A0A024R1A3 Ubiquitin-activating enzyme E1 7 A0A024R1K7 Tyrosine 3-monooxygenase/tryptophan 5-monooxygenase activation protein 8 A0A024R280 Phosphoserine aminotransferase 1 9 A0A024R2Q4 Ribosomal protein L15 10 A0A024R321 Filamin B 11 A0A024R382 CNDP dipeptidase 2 12 A0A024R3V9 HCG37498 13 A0A024R3X7 Heat shock 10kDa protein 1 (Chaperonin 10) 14 A0A024R408 Actin related protein 2/3 complex, subunit 2, 15 A0A024R4U3 Tubulin tyrosine ligase-like family 16 A0A024R592 Glucosidase 17 A0A024R5Z8 RAB11A, member RAS oncogene family 18 A0A024R652 Methylenetetrahydrofolate dehydrogenase 19 A0A024R6C9 Dihydrolipoamide S-succinyltransferase 20 A0A024R6D4 Enhancer of rudimentary homolog 21 A0A024R7F7 Transportin 2 22 A0A024R7T3 Heterogeneous nuclear ribonucleoprotein F 23 A0A024R814 Ribosomal protein L7 24 A0A024R872 Chromosome 9 open reading frame 88 25 A0A024R895 SET translocation 26 A0A024R8W0 DEAD (Asp-Glu-Ala-Asp) box polypeptide 48 27 A0A024R9E2 Poly(A) binding protein, cytoplasmic 1 28 A0A024RA28 Heterogeneous nuclear ribonucleoprotein A2/B1 29 A0A024RA52 Proteasome subunit alpha 30 A0A024RAE4 Cell division cycle 42 31