Sensory Thresholds at Different Sites of the Foot: a Valuable Reference for Neurologic Examinations
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Herpes Zoster by Lesia Dropulic, MD
Herpes Zoster Lesia Dropulic Jeffrey Cohen Laboratory of Infectious Diseases, NIAID Varicella (Chickenpox) Centers for Disease Control and Prevention Zoster (Shingles) Centers for Disease Control and Prevention Zoster is Due to Reactivation of Varicella from the Nervous System Blood Adapted from Kimberlin and Whitley NEJM 2007 VZV DNA is Present In Neurons in Ganglia Years After Chickenpox Ganglia latently infected with VZV Subject No. Neurons No. (%) neurons Median VZV DNA Number Tested positive for VZV copies/positive cell Wang et al J Virol 2005 History of Zoster • Zoster: Greek for girdle • Shingles: Latin (cingere) girdle Partial encircling of the trunk with rash First Cell Culture of Varicella-Zoster Virus (March 19, 1949) Thomas Weller in Varicella-Zoster Virus, Cambridge Press 2000 Varicella- Zoster Virus Straus et al. Ann Intern Med 1988 Epidemiology of Zoster • About 99% of adults >40 yo infected with varicella-zoster, thus all older adults at risk • About 1 million cases in the US each year • Rates appear to be increasing • 50% of persons of live to age 85 will develop zoster, 5% may get a second case Risk Factors for Zoster • Age- the major risk factor for healthy persons (long duration since exposure to virus) • Immune compromise- T cell immunity: transplant recipients, leukemia, lymphoma; HIV increases the risk up to 50 fold • Age and immune compromise- reduced VZV-specific T cell immunity Varicella-Zoster Virus: Site of Latency • Varicella-zoster virus is latent in dorsal root ganglia (along the spine) or cranial nerve -

The Neuroanatomy of Female Pelvic Pain
Chapter 2 The Neuroanatomy of Female Pelvic Pain Frank H. Willard and Mark D. Schuenke Introduction The female pelvis is innervated through primary afferent fi bers that course in nerves related to both the somatic and autonomic nervous systems. The somatic pelvis includes the bony pelvis, its ligaments, and its surrounding skeletal muscle of the urogenital and anal triangles, whereas the visceral pelvis includes the endopelvic fascial lining of the levator ani and the organ systems that it surrounds such as the rectum, reproductive organs, and urinary bladder. Uncovering the origin of pelvic pain patterns created by the convergence of these two separate primary afferent fi ber systems – somatic and visceral – on common neuronal circuitry in the sacral and thoracolumbar spinal cord can be a very dif fi cult process. Diagnosing these blended somatovisceral pelvic pain patterns in the female is further complicated by the strong descending signals from the cerebrum and brainstem to the dorsal horn neurons that can signi fi cantly modulate the perception of pain. These descending systems are themselves signi fi cantly in fl uenced by both the physiological (such as hormonal) and psychological (such as emotional) states of the individual further distorting the intensity, quality, and localization of pain from the pelvis. The interpretation of pelvic pain patterns requires a sound knowledge of the innervation of somatic and visceral pelvic structures coupled with an understand- ing of the interactions occurring in the dorsal horn of the lower spinal cord as well as in the brainstem and forebrain. This review will examine the somatic and vis- ceral innervation of the major structures and organ systems in and around the female pelvis. -

Disc Pathology Lumbar Dermatomes
Lumbar Dermatomes: Disc Pathology Lumbar Dermatomes In this example, nerve root pain is due to disc pathology. Dermatomes are regions of altered sensation from irritated or damaged nerve roots. Symptoms that follow a dermatome (numbness, tingling or pain) may indicate a pathology that involves the related nerve root. These symptoms can follow the entire dermatome or just part of it. When symptoms cover more than one dermatome it may suggest more severe pathology and involvement of more than one nerve root. Disc Pathology: Lumbar Disc Pathology has various presentations. 1. Normal Disc 2. Internal Disc Disorder: Small tear at the inner part of the outer third of the disc where the annulus is innervated. 3. Outer Disc Disorder: Larger tear that extends to the outer part of the annulus. Discography is a good way to diagnose the morphology of the disc and establish the disc as a pain generator. 4. Protrusion: Small disc bulge and the outer layers of the annulus are intact 5. Prolapse: Large disc bulge that breaks through the layers of the annulus but not the posterior longitudinal ligament (PLL). 6. Extrusion: Large disc bulge that breaks through the layers of the annulus and the PLL. This often causes pain in a multitude of dermatomes. 7. Sequestration (not shown; rare): Disc fragment breaks away from the rest of the discs. 1. Sizer PS Jr, Phelps V, Matthijs O. Pain generators of the lumbar spine. Pain Pract. 2001;1(3):255‐ 273. 2. Sizer PS Jr, Phelps V, Dedrick G, Matthijs O. Differential diagnosis and management of spinal nerve root‐related pain. -

Unit #2 - Abdomen, Pelvis and Perineum
UNIT #2 - ABDOMEN, PELVIS AND PERINEUM 1 UNIT #2 - ABDOMEN, PELVIS AND PERINEUM Reading Gray’s Anatomy for Students (GAFS), Chapters 4-5 Gray’s Dissection Guide for Human Anatomy (GDGHA), Labs 10-17 Unit #2- Abdomen, Pelvis, and Perineum G08- Overview of the Abdomen and Anterior Abdominal Wall (Dr. Albertine) G09A- Peritoneum, GI System Overview and Foregut (Dr. Albertine) G09B- Arteries, Veins, and Lymphatics of the GI System (Dr. Albertine) G10A- Midgut and Hindgut (Dr. Albertine) G10B- Innervation of the GI Tract and Osteology of the Pelvis (Dr. Albertine) G11- Posterior Abdominal Wall (Dr. Albertine) G12- Gluteal Region, Perineum Related to the Ischioanal Fossa (Dr. Albertine) G13- Urogenital Triangle (Dr. Albertine) G14A- Female Reproductive System (Dr. Albertine) G14B- Male Reproductive System (Dr. Albertine) 2 G08: Overview of the Abdomen and Anterior Abdominal Wall (Dr. Albertine) At the end of this lecture, students should be able to master the following: 1) Overview a) Identify the functions of the anterior abdominal wall b) Describe the boundaries of the anterior abdominal wall 2) Surface Anatomy a) Locate and describe the following surface landmarks: xiphoid process, costal margin, 9th costal cartilage, iliac crest, pubic tubercle, umbilicus 3 3) Planes and Divisions a) Identify and describe the following planes of the abdomen: transpyloric, transumbilical, subcostal, transtu- bercular, and midclavicular b) Describe the 9 zones created by the subcostal, transtubercular, and midclavicular planes c) Describe the 4 quadrants created -

Dermatomal Distribution | Definition of Dermatomal Distribution by Medical
10/13/2016 Dermatomal distribution | definition of dermatomal distribution by Medical dictionary Dermatomal distribution | definition of dermatomal distribution by Medical dictionary http://medicaldictionary.thefreedictionary.com/dermatomal+distribution dermatome (redirected from dermatomal distribution) Also found in: Dictionary, Thesaurus, Encyclopedia, Wikipedia. dermatome [der´mah-tōm] 1. the area of skin supplied with afferent nerve fibers by a single posterior spinal root. 2. the lateral part of an embryonic somite. 3. an instrument for removing splitthickness skin grafts from donor sites; there are many different kinds, divided into three major types: knife, drum, and motordriven. Dermatomes. Segmental dermatome distribution of spinal nerves to the front, back, and side of the body. C, Cervical segments; T, thoracic segments; L, lumbar segments; S, sacral segments; CX, coccygeal segment. Dermatomes are specific skin surface areas innervated by a single spinal nerve or group of spinal nerves. Dermatome assessment is done to determine the level of spinal anesthesia for surgical procedures and postoperative analgesia when epidural local anesthetics are used. From Thibodeau and Patton, 1999. drum dermatome a dermatome consisting of a cylindrical drumlike apparatus coated with adhesive that rolls over the skin while a blade moves across the surface and cuts the graft free. knife dermatome the simplest type of dermatome, which is used to remove grafts by a freehand technique. motordriven dermatome a dermatome driven by a power source; motordriven dermatomes cut with a backandforth blade action. MillerKeane Encyclopedia and Dictionary of Medicine, Nursing, and Allied Health, Seventh Edition. © 2003 by Saunders, an imprint of Elsevier, Inc. -
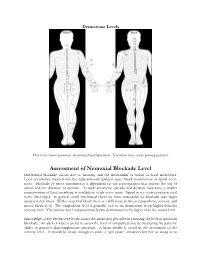
Assessment of Neuraxial Blockade Level Differential Blockade Occurs Due to Anatomy and the Mechanism of Action of Local Anesthetics
Dermatome Levels This is the most common anatomical configuration. Variation may occur among patients. Assessment of Neuraxial Blockade Level Differential blockade occurs due to anatomy and the mechanism of action of local anesthetics. Local anesthetics injected into the subarachnoid/epidural space block transmission at spinal nerve roots. Blockade of nerve transmission is dependent on the concentration that reaches the site of action and the duration of contact. As local anesthetic spreads and distance increases, a smaller concentration of local anesthetic is available to reach nerve roots. Spinal nerve roots contain several nerve fiber types. In general, small myelinated fibers are more susceptible to blockade than larger unmyelinated fibers. With a neuraxial block there is a difference between sympathetic, sensory, and motor block level. The sympathetic level is generally two to six dermatome levels higher than the sensory level. The sensory level is approximately two dermatome levels higher than the motor level. Knowledge of key dermatome levels assists the anesthesia provider in assessing the level of neuraxial blockade. An alcohol wipe is useful to assess the level of sympathectomy by measuring the patients’ ability to perceive skin temperature sensation. A blunt needle is useful in the assessment of the sensory level. It should be sharp enough to cause a “pin prick” sensation but not so sharp as to break the patients skin. The use of the spinal needle stylet can be used. Pinching the patient can also be used. The table below will help determine if the level of blockade achieves the minimum level required for a proposed surgical procedure. When reviewing the required sensory levels, it seems odd that the sensory level is higher than where the surgical procedure actually takes place. -

Assessment of the Sympathetic Level of Lesion in Patients with Spinal Cord Injury
Spinal Cord (2009) 47, 122–127 & 2009 International Spinal Cord Society All rights reserved 1362-4393/09 $32.00 www.nature.com/sc ORIGINAL ARTICLE Assessment of the sympathetic level of lesion in patients with spinal cord injury JG Previnaire1, JM Soler2, W El Masri3 and P Denys4 1Spinal Department, Centre Calve´, Fondation Hopale, Berck sur Mer, France; 2Laboratoire d’urodynamique et de sexologie, Centre Bouffard Vercelli, Cerbe`re, France; 3Midlands Centre for Spinal Injuries, RJ and AH Orthopaedic Hospital, Shropshire, UK and 4Service de Re´e´ducation Neurologique, Hoˆpital Raymond Poincare´, Garches, France Study design: To study the vasomotor responses (skin axon-reflex vasodilatation (SkARV) to stimulation of the skin in spinal cord injury (SCI) patients. Objective: To assess the completeness of the sympathetic injury and to define the sympathetic level of lesion in paraplegic and tetraplegic patients. Setting: Centre Calve, Fondation Hopale and Centre Bouffard-Vercelli, France. Subjects: A total of 81 SCI patients ranging from C2 to L2. Method: A mechanical stimulation was applied to the skin on both sides of the trunk, using a blunt instrument. The presence of an abnormal response below the lesion helped define the sympathetic level. Results: Above the lesion, SkARV was observed in all patients. In patients with a complete sympathetic injury, the response below the lesion was either a vasoconstrictor response in upper motor neuron lesions, or total absence of SkARV in lower motor neuron lesions. There was excellent correspondence between complete somatic (American Spinal Injury Association (ASIA) A) and complete sympathetic lesions (100% of paraplegic and 94% of tetraplegic patients), whereas an incomplete somatic (ASIA B– D) lesion was often associated with a complete sympathetic lesion. -

Entrapment Neuropathy
Limb Weakness: Radiculopathies and Compressive Disorders Spot the brain cell Dr. Theo Mobach PGY-4 Neurology [email protected] Image: Felten, Shetty. Netter’s Atlas of Neuroscience. 2nd Edition. Objectives • Basic neuroanatomy of peripheral nervous system • Physical exam: motor and sensory components • Common entrapment neuropathies – Median Neuropathy at the Wrist – Ulnar Neuropathy at the Elbow – Fibular Neuropathy • Radiculopathies UMN vs LMN Upper Motor Neuron Lower Motor Neuron • Spasticity • Atrophy • Hyperreflexia • Hypotonia • Pyramidal pattern • Decreased or of weakness absent reflexes • Babinski sign • Fasciculation's Motor Unit Motor neuron Skeletal Muscle Fibers Often several motor units work together to coordinate contraction of a single muscle Spinal Roots Image: Olson, Pawlina. Student Atlas of Anatomy. 2nd Edition Image: Olson, Pawlina. Student Atlas of Anatomy. 2nd Edition Dermatome Definition: A sensory region of skin innervated by a nerve root = dermatome Image: Felten, Shetty. Netter’s Atlas of Neuroscience. 2nd Edition. Sensory Innervation Cutaneous Nerve Branches Images: Felten, Shetty. Netter’s Atlas of Neuroscience. 2nd Edition. Nerve Muscle Peripheral Nerve Root Myotome C5 Deltoids Axillary N. Infraspinatus Suprascapular N. Biceps Musculocutaneous Definition: C6 Biceps Musculocutaneous Wrist extensors (ECR) Radial N. C7 Triceps Radial N. Muscles Finger extensors (EDC) PIN (Radial N.) innervated C8 Extensor indicis proprius (EIP) PIN (Radial N.) Median innervated intrinsic Median by a single hand muscles (LOAF) nerve root = L4 Quadriceps Femoral L5 Foot dorsiflexion Fibular N. myotome Foot inversion Fibular N. Foot eversion Tibial N. Hip abduction Gluteal N. S1 Foot plantar flexion, Tibial N. Hip extension Gluteal N. Recall • Write down 2 muscle for each of the following myotomes, the muscles MUST be from different peripheral nerves: – C6 – C8 – L5 – S1 Answer Nerve Muscle Peripheral Nerve Root C6 Biceps Musculocutaneous Wrist extensors (ECR) Radial N. -

The Anatomic and Physiologic Basis of Local, Referred and Radiating Lumbosacral Pain Syndromes Related to Disease of the Spine
J. Neuroradiol., 2004, 31, 163-80 Original article © Masson, Paris, 2004 THE ANATOMIC AND PHYSIOLOGIC BASIS OF LOCAL, REFERRED AND RADIATING LUMBOSACRAL PAIN SYNDROMES RELATED TO DISEASE OF THE SPINE J. RANDY JINKINS Department of Radiology, Downstate Medical Center, State University of New York, 450 Clarkson Avenue, Brooklyn, NY 11203, USA. SUMMARY Conscious perception and unconscious effects originating from the vertebral column and its neural structures, although complex, have definite pathways represented in a network of peripheral and central nervous system (CNS) ramifications. These neural relationships consequently result in superimposed focal and diffuse, local and remote conscious perceptions and unconscious effects. Any one or combination of somatic and autonomic signs and symptoms may potentially be observed in a particular patient. This variety and inconsistency may mislead or confuse both the patient and the physician. A clear understanding of the basic anatomic and physiologic concepts underlying this complexity should accompany clinical consid- erations of the potential significance of spondylogenic and neurogenic syndromes in any disease process affecting the spine. Key words: anatomy, pain, physiology, spine. RÉSUMÉ Bases anatomiques et physiologiques des syndromes douloureux d’origine rachidienne La perception consciente et les effets inconscients provenant du rachis et des structures spinales empruntent un réseau complexe appartenant aux systèmes nerveux central et périphérique. Ces rapports nerveux ont pour conséquence -
Peripheral Nervous System 2: the Autonomic System 16 August 2010
Peripheral Nervous System 2: The Autonomic System 16 August 2010 Handout download: Blackboard or http://www.oucom.ohiou.edu/ dbms-witmer/anatomy_immersion.htm Reading: Moore’s COA6 57–65 Lawrence M. Witmer, PhD Professor of Anatomy Dept of Biomedical Sciences College of Osteopathic Medicine Ohio University Athens, Ohio 45701 [email protected] Somatic vs. Visceral attribute Somatic System Visceral System embryological “body wall:” somatic (parietal) “organs:” splanchnic origin of tissue mesoderm (dermatome, (visceral) mesoderm, myotome) endoderm examples of dermis of skin, skeletal muscles, glands, cardiac muscle, adult tissues connective tissues smooth muscle perception conscious, voluntary unconscious, involuntary Langman’s Embryo 9 2004 Sensory/Motor + Somatic/Visceral Somatic Visceral Sensory somatic sensory visceral sensory (Afferent) [General Somatic [General Visceral Afferent (GSA)] Afferent (GVA)] Motor somatic motor visceral motor (Efferent) [General Somatic [General Visceral Efferent (GSE)] Efferent (GVE)] Somatic Autonomic Nervous Nervous System System (Aug 2) (today) Overview of the Autonomic Nervous System Similarities between Sympathetic & Parasympathetic • Both are efferent (motor) systems: “visceromotor” • Both involve regulation of the “internal” environment generally outside of our conscious control: “autonomous” • Both involve 2 neurons that synapse in a peripheral ganglion • Innervate glands, smooth muscle, cardiac muscle glands CNS ganglion smooth muscle cardiac preganglionic postganglionic muscle neuron neuron Overview -

Observations on the Inconsistency of Dermatome Maps and Its Effect On
Observations on the inconsistency of dermatome maps and its effect on knowledge and confidence in clinical students 1 D. Challoumas, 2 A. Ferro, 1 A. Walker, 1 C. Brassett 1 Department of Physiology, Development and Neuroscience, Downing Site, University of Cambridge, Cambridge, CB2 1DY, +44 1223 3337 78 2 University of Cambridge School of Clinical Medicine, Addenbrooke’s Hospital, Hills Road, Cambridge, CB2 0SP, +44 1223 3367 70 Running title: Dermatomes in medical education Correspondence to: Dimitrios Challoumas, Department of Physiology, Development and Neuroscience, Downing Site, University of Cambridge, Cambridge, CB2 1DY, +44 1223 3337 78 Mail: [email protected] This article has been accepted for publication and undergone full peer review but has not been through the copyediting, typesetting, pagination and proofreading process which may lead to differences between this version and the Version of Record. Please cite this article as an ‘Accepted Article’, doi: 10.1002/ca.23031 This article is protected by copyright. All rights reserved. Page 1 of 26 Clinical Anatomy 1 Observations on the inconsistency of dermatome maps and its effect on knowledge and confidence in clinical students Abstract INTRODUCTION: Dermatomes are an important component of medical curricula and clinical practice. In addition to the intrinsic complexity of dermatome maps, their discrepancies in the literature make their learning among students even more difficult. These discrepancies are particularly evident in the lower deltoid (“regimental badge” area) and upper back. The aims of our study were firstly to identify and compare published versions of the dermatome map focusing on depictions of the “regimental badge” area and upper back, secondly to assess the perceived confidence and knowledge of dermatomes among medical students, and finally to create and introduce a simplified dermatome map. -

Musculo-Skeletal System (Trunk, Limbs, and Head) General Statements: • Mesoderm Gives Rise to Skeletal Muscle, Skin Dermis, Endochondral Bones and Joints
Musculo-Skeletal System (Trunk, Limbs, and Head) General Statements: • Mesoderm gives rise to skeletal muscle, skin dermis, endochondral bones and joints. • Notochord induces paraxial mesoderm to form somites (somitomeres develop rostral to the somitomeres somites notochord in the head). in • Each somite differentiates into three regions: pharyngeal arches — sclerotome (medial): forms most of the axial skeleton (vertebrae, ribs, and base of the skull). heart limb — dermatome (lateral): migrates to form eye bud dermis of the skin head — myotome (middle): migrates to form skeletal Somites & Somitomeres muscles. Individual adult muscles are produced by merger of adjacent myotomes. Note: Early in development, nerves make connections with adjacent myotomes and dermatomes, establishing a segmental innervation pattern. As myotome/dermatome cells migrate to assume adult positions, the segmental nerve supply must follow along to maintain its connection to the innervation target. (Recurrent laryngeal & phrenic nerves travel long distances because their targets migrated far away.) Skin. somite: Consists of dermis and epidermis: ectoderm dermatome Epidermis, including hair follicles & glands, myotome sclerotome is derived from ectoderm. Neural crest cells neural crest intermediate migrate into epidermis and become melanocytes. mesoderm neural tube (Other neural crest cells become tactile disc receptors.) somatic mesoderm Dermis arises from dermatomes of somites. notochord Adjacent dermatomes overlap; thus, each skin endoderm aorta region is innervated by 2 or 3 spinal nerves. coelom Muscle. splanchnic mesoderm All skeletal muscle is derived from paraxial Mesoderm Regions mesoderm which forms somites and, rostrally in the head, somitomeres. (The one exception is iris musculature, derived from optic cup ectoderm.) Cardiac and smooth muscles originate from splanchnic mesoderm.