Your Guide to Distal Radius Fracture Surgery Brian J
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Do Fluoroscopic and Radiographic Images Underestimate Pin Protrusion in Paediatric Supracondylar Humerus and Distal Radius Fractures? a Synthetic Bone Model Analysis
Original Clinical Article Do fluoroscopic and radiographic images underestimate pin protrusion in paediatric supracondylar humerus and distal radius fractures? A synthetic bone model analysis S. Kenney Orthopaedic surgeons using fluoroscopy should be aware of J. Schlechter this discrepancy when assessing intraoperative fluoroscopic images to decide on acceptable implant position. Level of Evidence: Level V Abstract Purpose Fluoroscopy is commonly used to confirm accept- Cite this article: Kenney S, Schlechter J. Do fluoroscopic and able position of percutaneously placed pins when treating radiographic images underestimate pin protrusion in pae- paediatric fractures. There is a paucity of literature investigat- diatric supracondylar humerus and distal radius fractures? ing the accuracy of fluoroscopic imaging when determining A synthetic bone model analysis. J Child Orthop 2019;13. DOI: pin position relative to the far cortex of the fixated bone. The 10.1302/1863-2548.13.180173 purpose of this study was to evaluate the accuracy of fluor- oscopic and radiographic imaging in measuring smooth pin Keywords: supracondylar humerus fracture; percutaneous protrusion from the far cortex of a bone model. pinning; fluoroscopic imaging; distal radius fracture; paediatrics Methods Eight bone models were implanted with smooth pins and anteroposterior fluoroscopic and radiographic stud- ies were obtained. All images were evaluated by orthopaedic Introduction attending physicians, residents and medical students. The Paediatric supracondylar humerus and distal radius frac- length of pin protrusion from the model surface was estimat- tures are common injuries making up 17% and 23% of ed on fluoroscopic imaging and measured on radiographs and all paediatric fractures, respectively.1 When these fractures compared with actual lengths measured on the bone models. -

Ultrasound-Assisted Closed Reduction of Distal Radius Fractures
SCIENTIFIC ARTICLE Ultrasound-Assisted Closed Reduction of Distal Radius Fractures Narihito Kodama, MD, PhD, Yoshinori Takemura, MD, PhD, Hiroaki Ueba, MD, Shinji Imai, MD, PhD, Yoshitaka Matsusue, MD, PhD Purpose To assess the accuracy and ability of ultrasound for monitoring closed reduction for distal radius fractures. Methods Consecutive patients undergoing ultrasound-guided closed reduction of acute, dis- placed distal radius fractures between January 2003 and December 2006 at our department were enrolled. The control group was extracted from patients who underwent a closed reduction for similar fractures under fluoroscopy or without any imaging assistance. To confirm the accuracy of the ultrasonography measurements, displacement distance values were compared with those on radiographic imaging before and after reduction. X-ray pa- rameters for pre- and postreduction, reduction time, total cost, and success rate were compared between the ultrasound-guided and the control groups. Results The ultrasound-guided group consisted of 43 patients (mean age, 68 y) and the control group consisted of 57 patients, which included 35 patients (mean age, 74 y) with fluoroscopic reduction and of 22 patients (mean age, 72 y) with reduction unaided by imaging. There were no significant displacement differences between radiographic and ultrasound measurements. In x-ray parameters for pre- and postreduction, there were no significant differences between the 2 groups. Ultrasound-guided reduction took longer than the other 2 methods. The success rate of the ultrasound and the fluoroscopic groups were similar (95% and 94%, respectively). Conclusions Our data suggest that ultrasound assistance can aid reduction of distal radius fractures as well as fluoroscopy. (J Hand Surg Am. -

Bone Mineral Density and Prevalence of Osteoporosis in Postmenopausal Korean Women with Low-Energy Distal Radius Fractures
ORIGINAL ARTICLE Musculoskeletal Disorders http://dx.doi.org/10.3346/jkms.2016.31.6.972 • J Korean Med Sci 2016; 31: 972-975 Bone Mineral Density and Prevalence of Osteoporosis in Postmenopausal Korean Women with Low-Energy Distal Radius Fractures Hong Jun Jung,1 Ho Youn Park,2 The aim of this study was to evaluate the bone mineral density and the prevalence of Jin Sam Kim,1 Jun-O Yoon,1 osteoporosis in postmenopausal Korean women with low-energy distal radius fractures and and In-Ho Jeon1 compared with those of aged-matched normal Korean women. Two hundred and six patients with distal radius fractures between March 2006 and March 2010 were included in 1Department of Orthopaedic Surgery, Asan Medical Center, School of Medicine, University of Ulsan, this study. Patients were divided into three groups by age; group 1 (50-59 years), group 2 Seoul, Korea; 2Department of Orthopedic Surgery, (60-69 years), and group 3 (70-79 years). Controls were age-matched normal Korean Uijeongbu St. Mary’s Hospital, The Catholic women. The bone mineral density values at all measured sites, except for the spine, were University of Korea, Uijeongbu, Korea significantly lower in group 1 than those of control. While the bone mineral density values Received: 3 July 2015 in groups 2 and 3 were lower than those of controls, these differences were not statistically Accepted: 16 March 2016 significant. All groups had significantly higher prevalence of osteoporosis at the Ward’s triangle; however, at the spine, femoral neck and trochanteric area it was not significantly Address for Correspondence: different from those of age-matched controls. -

CS-FFRA-05 – 2005-16 Super Duty Fabricated Radius Arms NOTE
Carli Suspension: 422 Jenks Circle, Corona, CA 92880 Tech Support: (714) 532-2798 CS-FFRA-05 – 2005-16 Super Duty Fabricated Radius Arms NOTE: Please review the product instructions prior to attempting installation to ensure installer is equipped with all tools and capabilities necessary to complete the product installation. We recommend thoroughly reading the instructions at least twice prior to attempting Installation. Before beginning disassembly of the vehicle, check the “What’s Included” section of the instructions to ensure you’ve received all parts necessary to complete installation. Further, verify that the parts received are PROPER TO YOUR application (year range, motor, etc.) to avoid potential down-time in correcting potential discrepancies. Any discrepancies will be handled by Carli Suspension and the correcting products will be shipped UPS Ground. LIFETIME PRODUCT WARRANTY Carli Suspension provides a limited lifetime product warranty against defects in workmanship and materials from date of purchase to the original purchaser for all products produced by Carli Suspension. Parts not manufactured by, but made to Carli Suspension’s specifications by third party manufacturers will carry a warranty through their respective manufacturer. (i.e. King Shocks, Bilstein Shocks, Fox Shocks). Deaver Leaf Spring’s warranty will be processed by Carli Suspension. Proof of purchase (from the original purchaser only) will be required to process any warranty claims. Carli Suspension products must be purchased for the listed Retail Price reflected by the price listed on the Carli Suspension Website at the time of purchase. Carli Suspension reserves the right to refuse warranty claims made by any customer refusing or unable to present proof of purchase, or presenting proof of purchase reflecting a price lower than Carli Suspension’s Retail Price at the time the item was purchased. -

Distal Radius Fractures (Broken Wrist)
DISEASES & CONDITIONS Distal Radius Fractures (Broken Wrist) The radius is the larger of the two bones of the forearm. The end toward the wrist is called the distal end. A fracture of the distal radius occurs when the area of the radius near the wrist breaks. Distal radius fractures are very common. In fact, the radius is the most commonly broken bone in the arm. Description A distal radius fracture almost always occurs about 1 inch from the end of the bone. The break can occur in many different ways, however. One of the most common distal radius fractures is a Colles fracture, in which the broken fragment of the radius tilts upward. This fracture was first described in 1814 by an Irish surgeon and anatomist, Abraham Colles -- hence the name A Colles fracture occurs when the "Colles" fracture. broken end of the radius tilts upward. Other ways the distal radius can break include: Intra-articular fracture. A fracture that extends into the wrist joint. ("Articular" means "joint.") Extra-articular fracture. A fracture that does not extend into the joint is called an extra-articular fracture. Open fracture. When a fractured bone breaks the skin, it is called an open fracture. These types of fractures require immediate medical attention because of the risk for infection. Comminuted fracture. When a bone is broken into more than two pieces, it is called a comminuted fracture. It is important to classify the type of fracture, because some fractures are more difficult to treat than others. Intra-articular fractures, open fractures, comminuted fractures, and displaced fractures (when the broken pieces of bone do not line up straight).are more difficult to treat, for example. -

Bone Limb Upper
Shoulder Pectoral girdle (shoulder girdle) Scapula Acromioclavicular joint proximal end of Humerus Clavicle Sternoclavicular joint Bone: Upper limb - 1 Scapula Coracoid proc. 3 angles Superior Inferior Lateral 3 borders Lateral angle Medial Lateral Superior 2 surfaces 3 processes Posterior view: Acromion Right Scapula Spine Coracoid Bone: Upper limb - 2 Scapula 2 surfaces: Costal (Anterior), Posterior Posterior view: Costal (Anterior) view: Right Scapula Right Scapula Bone: Upper limb - 3 Scapula Glenoid cavity: Glenohumeral joint Lateral view: Infraglenoid tubercle Right Scapula Supraglenoid tubercle posterior anterior Bone: Upper limb - 4 Scapula Supraglenoid tubercle: long head of biceps Anterior view: brachii Right Scapula Bone: Upper limb - 5 Scapula Infraglenoid tubercle: long head of triceps brachii Anterior view: Right Scapula (with biceps brachii removed) Bone: Upper limb - 6 Posterior surface of Scapula, Right Acromion; Spine; Spinoglenoid notch Suprspinatous fossa, Infraspinatous fossa Bone: Upper limb - 7 Costal (Anterior) surface of Scapula, Right Subscapular fossa: Shallow concave surface for subscapularis Bone: Upper limb - 8 Superior border Coracoid process Suprascapular notch Suprascapular nerve Posterior view: Right Scapula Bone: Upper limb - 9 Acromial Clavicle end Sternal end S-shaped Acromial end: smaller, oval facet Sternal end: larger,quadrangular facet, with manubrium, 1st rib Conoid tubercle Trapezoid line Right Clavicle Bone: Upper limb - 10 Clavicle Conoid tubercle: inferior -
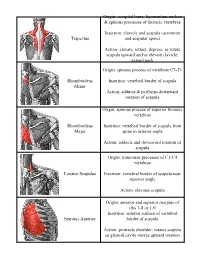
Trapezius Origin: Occipital Bone, Ligamentum Nuchae & Spinous Processes of Thoracic Vertebrae Insertion: Clavicle and Scapul
Origin: occipital bone, ligamentum nuchae & spinous processes of thoracic vertebrae Insertion: clavicle and scapula (acromion Trapezius and scapular spine) Action: elevate, retract, depress, or rotate scapula upward and/or elevate clavicle; extend neck Origin: spinous process of vertebrae C7-T1 Rhomboideus Insertion: vertebral border of scapula Minor Action: adducts & performs downward rotation of scapula Origin: spinous process of superior thoracic vertebrae Rhomboideus Insertion: vertebral border of scapula from Major spine to inferior angle Action: adducts and downward rotation of scapula Origin: transverse precesses of C1-C4 vertebrae Levator Scapulae Insertion: vertebral border of scapula near superior angle Action: elevates scapula Origin: anterior and superior margins of ribs 1-8 or 1-9 Insertion: anterior surface of vertebral Serratus Anterior border of scapula Action: protracts shoulder: rotates scapula so glenoid cavity moves upward rotation Origin: anterior surfaces and superior margins of ribs 3-5 Insertion: coracoid process of scapula Pectoralis Minor Action: depresses & protracts shoulder, rotates scapula (glenoid cavity rotates downward), elevates ribs Origin: supraspinous fossa of scapula Supraspinatus Insertion: greater tuberacle of humerus Action: abduction at the shoulder Origin: infraspinous fossa of scapula Infraspinatus Insertion: greater tubercle of humerus Action: lateral rotation at shoulder Origin: clavicle and scapula (acromion and adjacent scapular spine) Insertion: deltoid tuberosity of humerus Deltoid Action: -

Upper Extremity Fractures
Department of Rehabilitation Services Physical Therapy Standard of Care: Distal Upper Extremity Fractures Case Type / Diagnosis: This standard applies to patients who have sustained upper extremity fractures that require stabilization either surgically or non-surgically. This includes, but is not limited to: Distal Humeral Fracture 812.4 Supracondylar Humeral Fracture 812.41 Elbow Fracture 813.83 Proximal Radius/Ulna Fracture 813.0 Radial Head Fractures 813.05 Olecranon Fracture 813.01 Radial/Ulnar shaft fractures 813.1 Distal Radius Fracture 813.42 Distal Ulna Fracture 813.82 Carpal Fracture 814.01 Metacarpal Fracture 815.0 Phalanx Fractures 816.0 Forearm/Wrist Fractures Radius fractures: • Radial head (may require a prosthesis) • Midshaft radius • Distal radius (most common) Residual deformities following radius fractures include: • Loss of radial tilt (Normal non fracture average is 22-23 degrees of radial tilt.) • Dorsal angulation (normal non fracture average palmar tilt 11-12 degrees.) • Radial shortening • Distal radioulnar (DRUJ) joint involvement • Intra-articular involvement with step-offs. Step-off of as little as 1-2 mm may increase the risk of post-traumatic arthritis. 1 Standard of Care: Distal Upper Extremity Fractures Copyright © 2007 The Brigham and Women's Hospital, Inc. Department of Rehabilitation Services. All rights reserved. Types of distal radius fracture include: • Colle’s (Dinner Fork Deformity) -- Mechanism: fall on an outstretched hand (FOOSH) with radial shortening, dorsal tilt of the distal fragment. The ulnar styloid may or may not be fractured. • Smith’s (Garden Spade Deformity) -- Mechanism: fall backward on a supinated, dorsiflexed wrist, the distal fragment displaces volarly. • Barton’s -- Mechanism: direct blow to the carpus or wrist. -
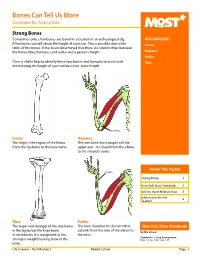
Bones Can Tell Us More Compiled By: Nancy Volk
Bones Can Tell Us More Compiled By: Nancy Volk Strong Bones Sometimes only a few bones are found in a location in an archeological dig. VOCABULARY A few bones can tell about the height of a person. This is possible due to the Femur ratios of the bones. It has been determined that there are relationships between the femur, tibia, humerus, and radius and a person’s height. Humerus Radius Here is a little help to identify these four bones and formulas to assist with Tibia determining the height of a person based on bone length. Humerus Femur: Humerus: The thigh is the region of the femur. The arm bone most people call the From the hip bone to the knee bone. upper arm. It is found from the elbow to the shoulder joints. Inside This Packet Radius Strong Bones 1 New York State Standards 1 Activity: Bone Relationships 2 Information for the Teacher 4 Tibia: Radius: The larger and stronger of the two bones The bone found in the forearm that New York State Standards in the leg below the knee bone. extends from the side of the elbow to Middle School In vertebrates It is recognized as the the wrist. Standard 4: Living Environment strongest weight bearing bone in the Idea 1: 1.2a, 1.2b, 1.2e, 1.2f body. Life Sciences - Post Module 3 Middle School Page 1 Activity: Bone Relationships MATERIALS NEEDED Skeleton Formulas: Tape Measure Bone relationship is represented by the following formulas: Directions and formulas P represents the person’s height. The last letter of each formula stands for the Calculator known length of the bone (femur, tibia, humerus, or radius) through measurement. -

Distal Radius Fracture
Distal Radius Fracture Osteoporosis, a common condition where bones become brittle, increases the risk of a wrist fracture if you fall. How are distal radius fractures diagnosed? Your provider will take a detailed health history and perform a physical evaluation. X-rays will be taken to confirm a fracture and help determine a treatment plan. Sometimes an MRI or CT scan is needed to get better detail of the fracture or to look for associated What is a distal radius fracture? injuries to soft tissues such as ligaments or Distal radius fracture is the medical term for tendons. a “broken wrist.” To fracture a bone means it is broken. A distal radius fracture occurs What is the treatment for distal when a sudden force causes the radius bone, radius fracture? located on the thumb side of the wrist, to break. The wrist joint includes many bones Treatment depends on the severity of your and joints. The most commonly broken bone fracture. Many factors influence treatment in the wrist is the radius bone. – whether the fracture is displaced or non-displaced, stable or unstable. Other Fractures may be closed or open considerations include age, overall health, (compound). An open fracture means a bone hand dominance, work and leisure activities, fragment has broken through the skin. There prior injuries, arthritis, and any other injuries is a risk of infection with an open fracture. associated with the fracture. Your provider will help determine the best treatment plan What causes a distal radius for your specific injury. fracture? Signs and Symptoms The most common cause of distal radius fracture is a fall onto an outstretched hand, • Swelling and/or bruising at the wrist from either slipping or tripping. -

Conservative Vs. Surgical Management of Ulnar Styloid Fractures Associated with Distal Radius Fractures
CLINICAL RESEARCH Conservative vs. surgical management of ulnar styloid fractures associated with distal radius fractures Cristian Robles, Santiago Iglesias, Christian Allende Nores, Pablo Rotella, Martín Caloia, Miguel Capomassi Orthopedics and Traumatology Department, Sanatorio Allende (Córdoba, Argentina) ABSTRACT Objectives: To evaluate potential differences in clinical and radiological outcomes after surgical versus conservative management of ulnar styloid fractures associated with unstable distal radius fractures treated by locked volar plating. Materials and Methods: This was a multicenter, retrospective and descriptive study including surgical patients treated at four different institutions between 2009 and 2012 for ulnar styloid fractures associated with unstable distal radius fractures. Ulnar styloid fractures were treated con- servatively in group I and surgically in group II. Results: The average follow-up was 56 months. The study included 57 patients divided into two groups (group I [29 cases] and group II [28 cases]). Patients in group II had 2.76 times (95% CI: 1.086; 8.80) more chances of achieving bone union than those in group I. DASH and pain scores, both at rest and during activity, did not show significant differences between the two groups (p = 0.276 and p = 0.877). Group I presented milder ulnar deviation and better strength (p = 0.0194 and p = 0.024). Conclusions: Although patients who underwent surgery for ulnar styloid fractures had 2.76 more chances of achieving bone union than those who received conservative management, there were no significant differences between both groups in subjective evaluations (DASH and pain scores) or when considering the degree of ulnar styloid involve- ment. However, the parameters of strength and ulnar deviation were better in the conservative management group. -

Open Reduction and Internal Fixation of a Distal Radius Fracture with a Volar Locking Plate: a Case Report John Wyrick, MD
Special Case Report Series JOT CASE REPORTS www.jorthotrauma.com JOURNALOF ORTHOPAEDIC TRAUMA OFFICIAL JOURNAL OF Orthopaedic Trauma Association AOTrauma North America Belgian Orthopaedic Trauma Association Canadian Orthopaedic Trauma Society Foundation for Orthopedic Trauma International Society for Fracture Repair The Japanese Society for Fracture Repair Open Reduction and Internal Fixation of a Distal Radius Fracture With a Volar Locking Plate: A Case Report John Wyrick, MD Summary: Fractures of the distal radius are one of the most fractures, the American Association of Orthopaedic Surgeons 3 common fractures treated by orthopedists. The case of a 41-year- (AAOS) published the clinical practice guidelines in 2009. This old woman who had initial closed reduction of a distal radius case report of a distal radius fracture treated by ORIF with a volar fracture with subsequent loss of reduction is presented. She was locking plate is presented to highlight current treatment successfully treated by operative stabilization with a distal radius recommendations. volar locking plate. The goal is to emphasize current treatment controversies and the clinical practice guidelines as recommended CASE REPORT by the American Academy of Orthopaedic Surgeons in the A 41-year-old woman fell on her right outstretched hand after treatment of distal radius fractures. falling down 2 or 3 stairs. She was otherwise healthy, and this was her only injury. She presented to the emergency department, and on physical examination, she was noted to have minimal deformity INTRODUCTION about her right wrist, although it was moderately swollen. Her Fracture of the distal radius is the most common fracture of the sensibility to light touch was intact with no deficit in her median upper extremity and one of the most common fractures treated by nerve function, and capillary refill was brisk.