Uroradiology for Medical Students
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Possibilities of Automated Diagnostics of Odontogenic Sinusitis According to the Computer Tomography Data
sensors Article Possibilities of Automated Diagnostics of Odontogenic Sinusitis According to the Computer Tomography Data Oleg G. Avrunin 1, Yana V. Nosova 1 , Ibrahim Younouss Abdelhamid 1, Sergii V. Pavlov 2 , Natalia O. Shushliapina 3, Waldemar Wójcik 4, Piotr Kisała 4,* and Aliya Kalizhanova 5,6 1 Department of Biomedical Engineering, Faculty of Electronic and Biomedical Engineering Kharkiv National University of Radio Electronics, 61166 Kharkiv, Ukraine; [email protected] (O.G.A.); [email protected] (Y.V.N.); [email protected] (I.Y.A.) 2 Department of Biomedical Engineering, Vinnytsia National Technical University, 21021 Vinnytsia, Ukraine; [email protected] 3 Department of Otorhinolaryngology, Stomatological Faculty Kharkiv National Medical University, 61022 Kharkiv, Ukraine; [email protected] 4 Institute of Electronic and Information Technologies, Faculty Electrical Engineering and Computer Science, Lublin University of Technology, 20-618 Lublin, Poland; [email protected] 5 Institute of Information and Computational Technologies CS MES RK, 050010 Almaty, Kazakhstan; [email protected] 6 University of Power Engineering and Telecommunications, 050013 Almaty, Kazakhstan * Correspondence: [email protected]; Tel.: +34-815-384-309 Abstract: Individual anatomical features of the paranasal sinuses and dentoalveolar system, the complexity of physiological and pathophysiological processes in this area, and the absence of actual standards of the norm and typical pathologies lead to the fact that differential diagnosis Citation: Avrunin, O.G.; Nosova, and assessment of the severity of the course of odontogenic sinusitis significantly depend on the Y.V.; Abdelhamid, I.Y.; Pavlov, S.V.; measurement methods of significant indicators and have significant variability. Therefore, an urgent Shushliapina, N.O.; Wójcik, W.; task is to expand the diagnostic capabilities of existing research methods, study the significance of Kisała, P.; Kalizhanova, A. -

CT, MRI and Ultrasound of the Orbit
6/15/2018 CT, MRI and Ultrasound of the Orbit GABRIELA S SEILER DR.MED.VET. DECVDI, DACVR PROFESSOR OF RADIOLOGY NORTH CAROLINA STATE UNIVERSITY 1 6/15/2018 Orbital imaging Principles and Indications of Computed Tomography and Magnetic Resonance Imaging Relevant Imaging Parameters Imaging of Orbital Diseases with Case Examples www.intechopen.com 2 6/15/2018 Tomographic Benefit Exopthalmos, OS Squamous cell carcinoma 148533M 3 6/15/2018 Mixbreed dog, 1 year history of nasal and ocular discharge, initially responded to antibiotics radiograph CT image 4 6/15/2018 5 6/15/2018 Cross‐Sectional Imaging Computed Tomography Magnetic Resonance Imaging Voxel Diagnostic Ultrasound Pixel Pixel ‐ picture element Voxel ‐ volume element 6 6/15/2018 Principles of Cross‐ sectional imaging SPATIAL CONTRAST MODALITY RESOLUTION RESOLUTION Radiography <1 mm Good Ultrasound 1-2mm Better CT 0.4 mm Even better MRI 1-3 mm Best! 7 6/15/2018 Computed Tomography “Cat Scan” 8 6/15/2018 Computed Tomography First CT scanner was built by Sir Godfrey Hounsfield at the EMI Research Laboratories in 1972 9 6/15/2018 Anatomy of a CT scanner X‐ray detectors X‐ray tube 10 6/15/2018 Most CTs are helical or spiral CTs X‐ray tube and an array of receptors rotate around the patient 11 6/15/2018 Image Reconstruction Images acquired by rapid rotation of X‐ray tube 360°around patient as couch moves. The transmitted radiation is then measured by a ring of radiation sensitive ceramic detectors. An image is generated from these measurements 12 6/15/2018 Image Reconstruction Complex mathematical algorithms allow each voxel to be assigned a numerical value based on the x ray attenuation within that volume of tissue. -

ACR Manual on Contrast Media
ACR Manual On Contrast Media 2021 ACR Committee on Drugs and Contrast Media Preface 2 ACR Manual on Contrast Media 2021 ACR Committee on Drugs and Contrast Media © Copyright 2021 American College of Radiology ISBN: 978-1-55903-012-0 TABLE OF CONTENTS Topic Page 1. Preface 1 2. Version History 2 3. Introduction 4 4. Patient Selection and Preparation Strategies Before Contrast 5 Medium Administration 5. Fasting Prior to Intravascular Contrast Media Administration 14 6. Safe Injection of Contrast Media 15 7. Extravasation of Contrast Media 18 8. Allergic-Like And Physiologic Reactions to Intravascular 22 Iodinated Contrast Media 9. Contrast Media Warming 29 10. Contrast-Associated Acute Kidney Injury and Contrast 33 Induced Acute Kidney Injury in Adults 11. Metformin 45 12. Contrast Media in Children 48 13. Gastrointestinal (GI) Contrast Media in Adults: Indications and 57 Guidelines 14. ACR–ASNR Position Statement On the Use of Gadolinium 78 Contrast Agents 15. Adverse Reactions To Gadolinium-Based Contrast Media 79 16. Nephrogenic Systemic Fibrosis (NSF) 83 17. Ultrasound Contrast Media 92 18. Treatment of Contrast Reactions 95 19. Administration of Contrast Media to Pregnant or Potentially 97 Pregnant Patients 20. Administration of Contrast Media to Women Who are Breast- 101 Feeding Table 1 – Categories Of Acute Reactions 103 Table 2 – Treatment Of Acute Reactions To Contrast Media In 105 Children Table 3 – Management Of Acute Reactions To Contrast Media In 114 Adults Table 4 – Equipment For Contrast Reaction Kits In Radiology 122 Appendix A – Contrast Media Specifications 124 PREFACE This edition of the ACR Manual on Contrast Media replaces all earlier editions. -

Diagnosing and Managing Common Adrenal Disorders
Diagnosing and Managing Common Adrenal Disorders Veronica Piziak MD, PhD Emeritus Director of Endocrinology Scott & White Fellowship Director Endocrinology Baylor S&W [email protected] Disclosures: None Objectives Discuss the Management of Incidental Adrenal Masses Discuss the management of common Adrenal Disorders Incidental Adrenal Masses What do you need to know? Is it cancer? What is the a potential for morbidity or mortality? Does it produce hormones that Is it functional? can cause problems? Is it growing? What vital Is there a mass effect? structures could be compromised? About 80+ % of the time the nodules of the adrenal are just warts! Adrenal Mass > 1.0 cm Is it malignant? Very rarely Is it functional? Rarely it can make hormones that cause hypertension, weight gain and diabetes Is there a mass effect? Rarely adrenal tumors can destroy the normal tissue and cause the gland to fail Adrenal Incidentalomas Prevalence of incidentally discovered adrenal Masses: 4.4%- 10% of patients undergoing CT scan Terzolo M et al Eur J Endo 2011;164:851 nonfunctioning benign lesion 82.5% cortisol-secreting adenoma 5.3% pheochromocytoma 5.1% adrenocortical carcinoma 4.7% metastatic lesion 2.5% aldosteronoma 1 % Malignant overall 8% Musella et al. BMC Surgery 2013; 13:57 Goals: Find adrenal carcinoma Identify all adrenal non-functioning lesions suspicious for adrenocortical cancer (imaging) Identify functional pheochromocytomas Identify cortisol or aldosterone secreting lesion Identify benign adenomas You should perform biochemical testing Obtain adequate imaging - CT or MRI adrenal protocol Indications for Surgery Functioning nodules: Unilateral aldosterone producing masses Hormonally active pheochromocytomas Overt Cushing’s Syndrome Non functioning lesions larger than 4 cm 93% of the adrenal carcinomas were >/= 4 cm when found. -

"Fullness" of the Pancreas on CT. Usually Benign, but EUS Plus/Minus FNA Is Warranted to Identify Malignancy
JOP. J Pancreas (Online) 2009 Jan 8; 10(1):37-42. ORIGINAL ARTICLE Focal or Diffuse "Fullness" of the Pancreas on CT. Usually Benign, but EUS Plus/Minus FNA Is Warranted to Identify Malignancy John David Horwhat1, Henning Gerke2, Ruben Daniel Acosta1, Darren A Pavey3, Paul S Jowell3 1Gastroenterology Service, Department of Medicine, Walter Reed Army Medical Center. Washington, DC, USA. 2Division of Gastroenterology, Department of Medicine, University of Iowa Hospitals and Clinics. Iowa City, IA, USA. 3Division of Gastroenterology, Department of Medicine, Duke University Health System. Durham, NC, USA ABSTRACT Context The role of EUS to evaluate subtle radiographic abnormalities of the pancreas is not well defined. Objective To assess the yield of EUS±FNA for focal or diffuse pancreatic enlargement/fullness seen on abdominal CT scan in the absence of discrete mass lesions. Design Retrospective database review. Setting Tertiary referral center. Patients and interventions Six hundred and 91 pancreatic EUS exams were reviewed. Sixty-nine met inclusion criteria of having been performed for focal enlargement or fullness of the pancreas. Known chronic pancreatitis, pancreatic calcifications, acute pancreatitis, discrete mass on imaging, pancreatic duct dilation (greater than 4 mm) and obstructive jaundice were excluded. Main outcome measurement Rate of malignancy found by EUS±FNA. Results FNA was performed in 19/69 (27.5%) with 4 new diagnoses of pancreatic adenocarcinoma, one metastatic renal cell carcinoma, one metastatic colon cancer, one chronic pancreatitis and 12 benign results. Eight patients had discrete mass lesions on EUS; two were cystic. All malignant diagnoses had a discrete solid mass on EUS. Conclusions Pancreatic enlargement/fullness is often a benign finding related to anatomic variation, but was related to malignancy in 8.7% of our patients (6/69). -

X-Ray Computed Tomography 1 X-Ray Computed Tomography
X-ray computed tomography 1 X-ray computed tomography X-ray computed tomography Intervention A patient is receiving a CT scan for cancer. Outside of the scanning room is an imaging computer that reveals a 3D image of the body's interior. ICD-10-PCS B?2 [1] ICD-9-CM 88.38 [2] MeSH D014057 [3] OPS-301 code: 3-20...3-26 X-ray computed tomography, also computed tomography (CT scan) or computed axial tomography (CAT scan), can be used for medical imaging and industrial imaging methods employing tomography created by computer processing.[4] Digital geometry processing is used to generate a three-dimensional image of the inside of an object from a large series of two-dimensional X-ray images taken around a single axis of rotation.[5] CT produces a volume of data that can be manipulated, through a process known as "windowing", in order to demonstrate various bodily structures based on their ability to block the X-ray beam. Although historically the images generated were in the axial or transverse plane, perpendicular to the long axis of the body, modern scanners allow this volume of data to be reformatted in various planes or even as volumetric (3D) representations of structures. Although most common in medicine, CT is also used in other fields, such as nondestructive materials testing. Another example is archaeological uses such as imaging the contents of sarcophagi. Usage of CT has increased dramatically over the last two decades in many countries.[6] An estimated 72 million scans were performed in the United States in 2007.[7] It is estimated that 0.4% of current cancers in the United States are due to CTs performed in the past and that this may increase to as high as 1.5-2% with 2007 rates of CT usage;[8] however, this estimate is disputed.[9] X-ray computed tomography 2 Etymology The word "tomography" is derived from the Greek tomos (slice) and graphein (to write). -

Coronary Artery Calcium Quantification in Contrast-Enhanced Computed Tomography Angiography
Georgia State University ScholarWorks @ Georgia State University Computer Science Dissertations Department of Computer Science 12-18-2013 Coronary Artery Calcium Quantification in Contrast-enhanced Computed Tomography Angiography Abinashi Dhungel Georgia State University Follow this and additional works at: https://scholarworks.gsu.edu/cs_diss Recommended Citation Dhungel, Abinashi, "Coronary Artery Calcium Quantification in Contrast-enhanced Computed Tomography Angiography." Dissertation, Georgia State University, 2013. https://scholarworks.gsu.edu/cs_diss/80 This Dissertation is brought to you for free and open access by the Department of Computer Science at ScholarWorks @ Georgia State University. It has been accepted for inclusion in Computer Science Dissertations by an authorized administrator of ScholarWorks @ Georgia State University. For more information, please contact [email protected]. CORONARY ARTERY CALCIUM QUANTIFICATION IN CONTRAST-ENHANCED COMPUTED TOMOGRAPHY ANGIOGRAPHY by ABINASHI DHUNGEL Under the Direction of Dr. Michael Weeks ABSTRACT Coronary arteries are the blood vessels supplying oxygen-rich blood to the heart muscles. Coronary artery calcium (CAC), which is the total amount of calcium deposited in these arteries, indicates the presence or the future risk of coronary artery diseases. Quantification of CAC is done by using computed tomography (CT) scan which uses attenuation of x- ray by different tissues in the body to generate three-dimensional images. Calcium can be easily spotted in the CT images because of its higher opacity to x-ray compared to that of the surrounding tissue. However, the arteries cannot be identified easily in the CT images. Therefore, a second scan is done after injecting a patient with an x-ray opaque dye known as contrast material which makes different chambers of the heart and the coronary arteries visible in the CT scan. -

In Vivo X-Ray Computed Tomographic Imaging of Soft Tissue with Native, Intravenous, Or Oral Contrast
Sensors 2013, 13, 6957-6980; doi:10.3390/s130606957 OPEN ACCESS sensors ISSN 1424-8220 www.mdpi.com/journal/sensors Review In vivo X-Ray Computed Tomographic Imaging of Soft Tissue with Native, Intravenous, or Oral Contrast Connor A. Wathen 1, Nathan Foje 2, Tony van Avermaete 2,3, Bernadette Miramontes 2,3, Sarah E. Chapaman 4, Todd A. Sasser 2,5, Raghuraman Kannan 6, Steven Gerstler 7 and W. Matthew Leevy 1,4,8,* 1 Department of Biological Sciences, 100 Galvin Life Sciences Center, University of Notre Dame, Notre Dame, IN 46556, USA; E-Mail: [email protected] 2 Department of Chemistry and Biochemistry, 236 Nieuwland Science Hall, University of Notre Dame, Notre Dame, IN 46556, USA; E-Mails: [email protected] (N.F.); [email protected] (T.V.A.); [email protected] (B.M.); [email protected] (T.A.S.) 3 Penn High School, 55900 Bittersweet Road, Mishawaka, IN 46545, USA 4 Notre Dame Integrated Imaging Facility, Notre Dame, IN 46556, USA; E-Mail: [email protected] 5 Bruker-Biospin Corporation, 4 Research Drive, Woodbridge, CT 06525, USA 6 Department of Radiology, University of Missouri, Columbia, MO 65212, USA; E-Mail: [email protected] 7 Saint Joseph Regional Medical Center, Mishawaka, IN 46545, USA; E-Mail: [email protected] 8 Harper Cancer Research Institute, A200 Harper Hall, Notre Dame, IN 46530, USA * Author to whom correspondence should be addressed; E-Mail: [email protected]. Received: 27 March 2013; in revised form: 16 May 2013 / Accepted: 23 May 2013 / Published: 27 May 2013 Abstract: X-ray Computed Tomography (CT) is one of the most commonly utilized anatomical imaging modalities for both research and clinical purposes. -

Computerized Treatment Planning Systems - II CRISTER CEBERG Modern Computerized Treatment Planning Modern Computerized Treatment Planning Generally Available Hardware
Computerized treatment planning systems - II CRISTER CEBERG Modern computerized treatment planning Modern computerized treatment planning Generally available hardware » Network solutions – Servers – Workstations – Citrix clients Dell Precision T5400/T5500 ...not so accessible software » Documentation – Scientific papers – Reference manuals » The implementation is still often a ”black box”! » We will look at general features and examples Types of dose calculation algorithms IAEA TRS 430 Types of dose calculation algorithms IAEA TRS 430 CT for patient information »Diagnostic tools »Target determination »Basis for calculations – Hounsfield units HU 1000 H2O H2O Conversion to electron density The Hounsfield scale +1000 +800 Bone +100 Bonecompact +90 substance compact +80 Coagulated substance +600 blood +70 SD +60 Liver Whole Blood +400 +50 Spleen Muscle +40 Pancreas Fatty Bone +30 Kidney mixed spongy +200 Exudate substance +20 Transudate tissue +100 +10 Ringer solut. 0 Water Fat -100 -10 -20 -200 -30 Fatty -40 mixed tissue -400 -50 -60 -70 -600 -80 Lung tissue -90 Fat -100 -800 -1000 Patients in motion Creating a voxel matrix » Map to each voxel – Tissue type – Composition and density – Interaction properties » sphoto, scompton, spair General components of calculation models » Incident photon fluence » Raytracing » Redistribution of energy Incident fluence Primary and secondary sources RayStation Primary source Beam profile Gaussian Incident primary source primary profile (can also be a wedge profile) Profile slope and source width are -
Contrast CT Take? CT a Contrast CT Will Usually Take 15-20 Minutes
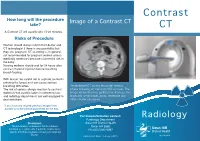
Contrast How long will the procedure Image of a Contrast CT take? CT A Contrast CT will usually take 15-20 minutes. Risks of Procedure Women should always inform their doctor and CT technologist if there is any possibility that they are pregnant. CT scanning is, in general, not recommended for pregnant women unless medically necessary because of potential risk to the baby. Nursing mothers should wait for 24 hours after contrast material injection before resuming breast-feeding. With Ioscan, be careful not to aspirate (contents entering the lungs) as it can cause serious breathing difficulties. An abdomen CT during the portal-venous The risk of serious allergic reaction to contrast phase following an injection of IV contrast. The materials that contain iodine is extremely low, image shows the liver, gallbladder, kidneys, the and radiology departments are well-equipped to large and small bowel, aorta, vertebrae and deal with them. other smaller structures. If you have any related previous images from another provider please bring them on the day. For more information contact: Radiology Radiology Department Disclaimer: Swan Hill District Health The information contained in this brochure is Swan Hill 3585 intended as a guide only. If patients require more Ph: (03) 5033 9287 specific information please contact your referring Doctor. Publication Date: February 2013 What is a Contrast CT? Preparation CT scans of internal organs, bones, soft tissue Women must inform the radiographer if there is If you are over 55 years of age, your doctor will and blood vessels reveal more details than any chance that they are pregnant or if they are give you a pathology slip to have a ‘U & E’ blood regular x-rays. -

Expressing Medical Image Measurements Using the Ontology for Biomedical Investigations Heiner Oberkampf1,2, James A
Expressing Medical Image Measurements using the Ontology for Biomedical Investigations Heiner Oberkampf1,2, James A. Overton3 Sonja Zillner1, Bernhard Bauer2 and Matthias Hammon4 1 Siemens AG, Corporate Technology 2 University of Augsburg, Software Methodologies for Distributed Systems 3 Knocean 4 University Hospital Erlangen, Department of Radiology Agenda 1. Measurements in radiology and pathology 2. Expressing measurements using OBI 1. OBI value specifications 2. Size measurements 3. Density measurements 4. Ratio measurements 3. Normal size, density and ratio specifications 4. Applications 1. Information Extraction 2. Normality Classification 3. Inference of Change 5. Demo Typical Measurements in Radiology Not comprehensive Size length (1D, 2D, 3D), area, volume index (e.g. spleen index = width*height*depth) Density measured in Hounsfield scale (Hu): mainly in CT images minimal, maximal and mean density values for Regions of Interest (ROIs) Angle e.g. bone configurations or fractions Blood flow e.g. PET: myocardial blood flow and blood flow in brain … Measurements in Pathology Not comprehensive Size length (1D, 2D, 3D), area Weight weight of resected tissue, nodule or tumor Ratios immunohistochemical staining of tumor cells Other measurements viscosity of blood, serum, and plasma mitotic rate serum concentration … Expressing Measurements using OBI obi:value specification Shared structure in different contexts The element "1.8cm" can occur in many different parts of a biomedical investigation. It might be part of: • the data resulting from a measurement of one of John's lymph nodes, made on January 12, 2014 in Berlin • a protocol, i.e. a specification of a plan to make some measurement • a prediction of the result a measurement planned for the future • a rule for classifying measurements • many more… OBI uses the "value specification" approach to capture the shared structure across different uses and allow for easy comparison between them. -

Guideline Safe Use of Contrast Media Part 1
Guideline Safe Use of Contrast Media Part 1 This part 1 comprises: 1. Prevention of post-contrast acute kidney injury 2. Use of iodine-containing contrast media in patients with diabetes type 2 who use metformin 3. Use of iodine-containing contrast media in patients undergoing dialysis INITIATED BY Radiological Society of the Netherlands IN ASSOCIATION WITH Netherlands Association of Internal Medicine Dutch Federation for Nephrology Dutch Society of Intensive Care Association of Surgeons of the Netherlands The Netherlands Society of Cardiology Dutch Society for Clinical Chemistry and Laboratory Medicine Netherlands Society of Emergency Physicians Dutch Association of Urology Dutch Society Medical Imaging and Radiotherapy WITH THE ASSISTANCE OF Knowledge Institute of Medical Specialists FINANCED BY Quality Funds of Medical Specialists 1 Guideline Safe Use of Contrast Media – Part 1 Colophon GUIDELINE SAFE USE OF CONTRAST MEDIA – PART 1 ©2017 Radiological Society of the Netherlands Address: Taalstraat 40, 5260 CB Vught 0800 0231 536 / 073 614 1478 [email protected] www.radiologen.nl All rights reserved. The text in this publication can be copied, saved or made public in any manner: electronically, by photocopy or in another way, but only with prior permission of the publisher. Permission for usage of (parts of) the text can be requested by writing or e- mail, only form the publisher. Address and email: see above. 2 Guideline Safe Use of Contrast Media – Part 1 Index Working group ........................................................................................................... 4 Chapter 1 General Introductions ............................................................................. 5 Chapter 2 Justification of this Guideline ................................................................. 10 Chapter 3 PC-AKI: Definitions, Terminology & Clinical Course.….…………….…………… 19 Chapter 4 Risk Stratification and Risk Stratification Tools ......................................