I PTPRT/D MUTATION OR PROMOTER METHYLATION: IMPLICATIONS for STAT3 INHIBITION
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Inflammatory Cytokine Signalling by Protein Tyrosine Phosphatases in Pancreatic Β-Cells
59 4 W J STANLEY and others PTPN1 and PTPN6 modulate 59: 4 325–337 Research cytokine signalling in β-cells Differential regulation of pro- inflammatory cytokine signalling by protein tyrosine phosphatases in pancreatic β-cells William J Stanley1,2, Prerak M Trivedi1,2, Andrew P Sutherland1, Helen E Thomas1,2 and Esteban N Gurzov1,2,3 Correspondence should be addressed 1 St. Vincent’s Institute of Medical Research, Melbourne, Australia to E N Gurzov 2 Department of Medicine, St. Vincent’s Hospital, The University of Melbourne, Melbourne, Australia Email 3 ULB Center for Diabetes Research, Universite Libre de Bruxelles (ULB), Brussels, Belgium esteban.gurzov@unimelb. edu.au Abstract Type 1 diabetes (T1D) is characterized by the destruction of insulin-producing β-cells Key Words by immune cells in the pancreas. Pro-inflammatory including TNF-α, IFN-γ and IL-1β f pancreatic β-cells are released in the islet during the autoimmune assault and signal in β-cells through f protein tyrosine phosphorylation cascades, resulting in pro-apoptotic gene expression and eventually phosphatases β-cell death. Protein tyrosine phosphatases (PTPs) are a family of enzymes that regulate f PTPN1 phosphorylative signalling and are associated with the development of T1D. Here, we f PTPN6 observed expression of PTPN6 and PTPN1 in human islets and islets from non-obese f cytokines diabetic (NOD) mice. To clarify the role of these PTPs in β-cells/islets, we took advantage f inflammation Journal of Molecular Endocrinology of CRISPR/Cas9 technology and pharmacological approaches to inactivate both proteins. We identify PTPN6 as a negative regulator of TNF-α-induced β-cell death, through JNK- dependent BCL-2 protein degradation. -

CDH12 Cadherin 12, Type 2 N-Cadherin 2 RPL5 Ribosomal
5 6 6 5 . 4 2 1 1 1 2 4 1 1 1 1 1 1 1 1 1 1 1 1 1 1 1 1 1 1 2 2 A A A A A A A A A A A A A A A A A A A A C C C C C C C C C C C C C C C C C C C C R R R R R R R R R R R R R R R R R R R R B , B B B B B B B B B B B B B B B B B B B , 9 , , , , 4 , , 3 0 , , , , , , , , 6 2 , , 5 , 0 8 6 4 , 7 5 7 0 2 8 9 1 3 3 3 1 1 7 5 0 4 1 4 0 7 1 0 2 0 6 7 8 0 2 5 7 8 0 3 8 5 4 9 0 1 0 8 8 3 5 6 7 4 7 9 5 2 1 1 8 2 2 1 7 9 6 2 1 7 1 1 0 4 5 3 5 8 9 1 0 0 4 2 5 0 8 1 4 1 6 9 0 0 6 3 6 9 1 0 9 0 3 8 1 3 5 6 3 6 0 4 2 6 1 0 1 2 1 9 9 7 9 5 7 1 5 8 9 8 8 2 1 9 9 1 1 1 9 6 9 8 9 7 8 4 5 8 8 6 4 8 1 1 2 8 6 2 7 9 8 3 5 4 3 2 1 7 9 5 3 1 3 2 1 2 9 5 1 1 1 1 1 1 5 9 5 3 2 6 3 4 1 3 1 1 4 1 4 1 7 1 3 4 3 2 7 6 4 2 7 2 1 2 1 5 1 6 3 5 6 1 3 6 4 7 1 6 5 1 1 4 1 6 1 7 6 4 7 e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e e l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l l p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p p m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m m -

The Regulatory Roles of Phosphatases in Cancer
Oncogene (2014) 33, 939–953 & 2014 Macmillan Publishers Limited All rights reserved 0950-9232/14 www.nature.com/onc REVIEW The regulatory roles of phosphatases in cancer J Stebbing1, LC Lit1, H Zhang, RS Darrington, O Melaiu, B Rudraraju and G Giamas The relevance of potentially reversible post-translational modifications required for controlling cellular processes in cancer is one of the most thriving arenas of cellular and molecular biology. Any alteration in the balanced equilibrium between kinases and phosphatases may result in development and progression of various diseases, including different types of cancer, though phosphatases are relatively under-studied. Loss of phosphatases such as PTEN (phosphatase and tensin homologue deleted on chromosome 10), a known tumour suppressor, across tumour types lends credence to the development of phosphatidylinositol 3--kinase inhibitors alongside the use of phosphatase expression as a biomarker, though phase 3 trial data are lacking. In this review, we give an updated report on phosphatase dysregulation linked to organ-specific malignancies. Oncogene (2014) 33, 939–953; doi:10.1038/onc.2013.80; published online 18 March 2013 Keywords: cancer; phosphatases; solid tumours GASTROINTESTINAL MALIGNANCIES abs in sera were significantly associated with poor survival in Oesophageal cancer advanced ESCC, suggesting that they may have a clinical utility in Loss of PTEN (phosphatase and tensin homologue deleted on ESCC screening and diagnosis.5 chromosome 10) expression in oesophageal cancer is frequent, Cao et al.6 investigated the role of protein tyrosine phosphatase, among other gene alterations characterizing this disease. Zhou non-receptor type 12 (PTPN12) in ESCC and showed that PTPN12 et al.1 found that overexpression of PTEN suppresses growth and protein expression is higher in normal para-cancerous tissues than induces apoptosis in oesophageal cancer cell lines, through in 20 ESCC tissues. -

Targeting Protein Tyrosine Phosphatases in Cancer Lakshmi Reddy Bollu, Abhijit Mazumdar, Michelle I
Published OnlineFirst January 13, 2017; DOI: 10.1158/1078-0432.CCR-16-0934 Molecular Pathways Clinical Cancer Research Molecular Pathways: Targeting Protein Tyrosine Phosphatases in Cancer Lakshmi Reddy Bollu, Abhijit Mazumdar, Michelle I. Savage, and Powel H. Brown Abstract The aberrant activation of oncogenic signaling pathways is a act as tumor suppressor genes by terminating signal responses universal phenomenon in cancer and drives tumorigenesis and through the dephosphorylation of oncogenic kinases. More malignant transformation. This abnormal activation of signal- recently, it has become clear that several PTPs overexpressed ing pathways in cancer is due to the altered expression of in human cancers do not suppress tumor growth; instead, they protein kinases and phosphatases. In response to extracellular positively regulate signaling pathways and promote tumor signals, protein kinases activate downstream signaling path- development and progression. In this review, we discuss both ways through a series of protein phosphorylation events, ulti- types of PTPs: those that have tumor suppressor activities as mately producing a signal response. Protein tyrosine phospha- well as those that act as oncogenes. We also discuss the tases (PTP) are a family of enzymes that hydrolytically remove potential of PTP inhibitors for cancer therapy. Clin Cancer Res; phosphate groups from proteins. Initially, PTPs were shown to 23(9); 1–7. Ó2017 AACR. Background in cancer and discuss the current status of PTP inhibitors for cancer therapy. Signal transduction is a complex process that transmits extra- PTPs belong to a superfamily of enzymes that hydrolytically cellular signals effectively through a cascade of events involving remove phosphate groups from proteins (2). -

The PTPRT Pseudo-Phosphatase Domain Is a Denitrase
bioRxiv preprint doi: https://doi.org/10.1101/238980; this version posted December 22, 2017. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. The PTPRT pseudo-phosphatase domain is a denitrase Yiqing Zhao1,2,#, Shuliang Zhao3,1,#, Yujun Hao1,2, Benlian Wang4, Peng Zhang1,2, Xiujing Feng1,2, Yicheng Chen1,2, Jing Song4, John Mieyal5, Sanford Markowitz1,2,6,7, Rob M. Ewing8,4, Ronald A. Conlon1,2, Masaru Miyagi4 and Zhenghe Wang1,2* 1Department of Genetics and Genome Sciences, 2Case Comprehensive Cancer Center, 4Department of Nutrition and Center for Proteomics and Bioinformatics, 5Department of Pharmacology, 6Department of Medicine, Case Western Reserve University, 10900 Euclid Avenue, Cleveland, Ohio 44106. 3Division of Gastroenterology and Hepatology and Shanghai Institution of Digestive Disease; Shanghai Jiao-Tong University School of Medicine Renji Hospital, 145 Middle Shandong Rd, Shanghai 200001, China. 7Seidman Cancer Center, University Hospitals Cleveland Medical Center, Cleveland, OH 44106. 8Computational and Systems Biology, School of Biological Sciences, University of Southampton, Southampton SO171BJ, UK * To whom correspondence should be addressed. Email: [email protected] # These authors contributed equally. bioRxiv preprint doi: https://doi.org/10.1101/238980; this version posted December 22, 2017. The copyright holder for this preprint (which was not certified by peer review) is the author/funder. All rights reserved. No reuse allowed without permission. Abstract Protein tyrosine nitration occurs under both physiological and pathological conditions1. However, enzymes that remove this protein modification have not yet been identified. Here we report that the pseudo-phosphatase domain of protein tyrosine receptor T (PTPRT) is a denitrase that removes nitro-groups from tyrosine residues in paxillin. -

Genetic Alterations of Protein Tyrosine Phosphatases in Human Cancers
Oncogene (2015) 34, 3885–3894 © 2015 Macmillan Publishers Limited All rights reserved 0950-9232/15 www.nature.com/onc REVIEW Genetic alterations of protein tyrosine phosphatases in human cancers S Zhao1,2,3, D Sedwick3,4 and Z Wang2,3 Protein tyrosine phosphatases (PTPs) are enzymes that remove phosphate from tyrosine residues in proteins. Recent whole-exome sequencing of human cancer genomes reveals that many PTPs are frequently mutated in a variety of cancers. Among these mutated PTPs, PTP receptor T (PTPRT) appears to be the most frequently mutated PTP in human cancers. Beside PTPN11, which functions as an oncogene in leukemia, genetic and functional studies indicate that most of mutant PTPs are tumor suppressor genes. Identification of the substrates and corresponding kinases of the mutant PTPs may provide novel therapeutic targets for cancers harboring these mutant PTPs. Oncogene (2015) 34, 3885–3894; doi:10.1038/onc.2014.326; published online 29 September 2014 INTRODUCTION tyrosine/threonine-specific phosphatases. (4) Class IV PTPs include Protein tyrosine phosphorylation has a critical role in virtually all four Drosophila Eya homologs (Eya1, Eya2, Eya3 and Eya4), which human cellular processes that are involved in oncogenesis.1 can dephosphorylate both tyrosine and serine residues. Protein tyrosine phosphorylation is coordinately regulated by protein tyrosine kinases (PTKs) and protein tyrosine phosphatases 1 THE THREE-DIMENSIONAL STRUCTURE AND CATALYTIC (PTPs). Although PTKs add phosphate to tyrosine residues in MECHANISM OF PTPS proteins, PTPs remove it. Many PTKs are well-documented oncogenes.1 Recent cancer genomic studies provided compelling The three-dimensional structures of the catalytic domains of evidence that many PTPs function as tumor suppressor genes, classical PTPs (RPTPs and non-RPTPs) are extremely well because a majority of PTP mutations that have been identified in conserved.5 Even the catalytic domain structures of the dual- human cancers are loss-of-function mutations. -
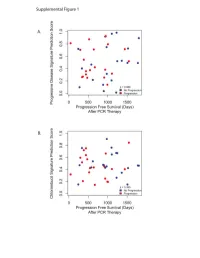
Supplementary Data
Progressive Disease Signature Upregulated probes with progressive disease U133Plus2 ID Gene Symbol Gene Name 239673_at NR3C2 nuclear receptor subfamily 3, group C, member 2 228994_at CCDC24 coiled-coil domain containing 24 1562245_a_at ZNF578 zinc finger protein 578 234224_at PTPRG protein tyrosine phosphatase, receptor type, G 219173_at NA NA 218613_at PSD3 pleckstrin and Sec7 domain containing 3 236167_at TNS3 tensin 3 1562244_at ZNF578 zinc finger protein 578 221909_at RNFT2 ring finger protein, transmembrane 2 1552732_at ABRA actin-binding Rho activating protein 59375_at MYO15B myosin XVB pseudogene 203633_at CPT1A carnitine palmitoyltransferase 1A (liver) 1563120_at NA NA 1560098_at AKR1C2 aldo-keto reductase family 1, member C2 (dihydrodiol dehydrogenase 2; bile acid binding pro 238576_at NA NA 202283_at SERPINF1 serpin peptidase inhibitor, clade F (alpha-2 antiplasmin, pigment epithelium derived factor), m 214248_s_at TRIM2 tripartite motif-containing 2 204766_s_at NUDT1 nudix (nucleoside diphosphate linked moiety X)-type motif 1 242308_at MCOLN3 mucolipin 3 1569154_a_at NA NA 228171_s_at PLEKHG4 pleckstrin homology domain containing, family G (with RhoGef domain) member 4 1552587_at CNBD1 cyclic nucleotide binding domain containing 1 220705_s_at ADAMTS7 ADAM metallopeptidase with thrombospondin type 1 motif, 7 232332_at RP13-347D8.3 KIAA1210 protein 1553618_at TRIM43 tripartite motif-containing 43 209369_at ANXA3 annexin A3 243143_at FAM24A family with sequence similarity 24, member A 234742_at SIRPG signal-regulatory protein gamma -

Comprehensive Protein Tyrosine Phosphatase Mrna Profiling Identifies New Regulators in the Progression of Glioma Annika M
Bourgonje et al. Acta Neuropathologica Communications (2016) 4:96 DOI 10.1186/s40478-016-0372-x RESEARCH Open Access Comprehensive protein tyrosine phosphatase mRNA profiling identifies new regulators in the progression of glioma Annika M. Bourgonje1, Kiek Verrijp2, Jan T. G. Schepens1, Anna C. Navis2, Jolanda A. F. Piepers1, Chantal B. C. Palmen1, Monique van den Eijnden4, Rob Hooft van Huijsduijnen4, Pieter Wesseling2,3, William P. J. Leenders2 and Wiljan J. A. J. Hendriks1* Abstract The infiltrative behavior of diffuse gliomas severely reduces therapeutic potential of surgical resection and radiotherapy, and urges for the identification of new drug-targets affecting glioma growth and migration. To address the potential role of protein tyrosine phosphatases (PTPs), we performed mRNA expression profiling for 91 of the 109 known human PTP genes on a series of clinical diffuse glioma samples of different grades and compared our findings with in silico knowledge from REMBRANDT and TCGA databases. Overall PTP family expression levels appeared independent of characteristic genetic aberrations associated with lower grade or high grade gliomas. Notably, seven PTP genes (DUSP26, MTMR4, PTEN, PTPRM, PTPRN2, PTPRT and PTPRZ1) were differentially expressed between grade II-III gliomas and (grade IV) glioblastomas. For DUSP26, PTEN, PTPRM and PTPRT, lower expression levels correlated with poor prognosis, and overexpression of DUSP26 or PTPRT in E98 glioblastoma cells reduced tumorigenicity. Our study represents the first in-depth analysis of PTP family expression in diffuse glioma subtypes and warrants further investigations into PTP-dependent signaling events as new entry points for improved therapy. Keywords: Glioblastoma, Astrocytoma, EGFR, Oligodendroglioma, IDH1, DUSP26, MTMR4, PTEN, PTP, PTPRM, PTPRN2, PTPRT, PTPRZ1, Malignancy Introduction has slightly improved over the past decades, the prospect Gliomas arise from glial (precursor) cells and represent with current treatment is only a median 15 months fol- the most frequent type of primary brain tumor. -

Activation of Islet Inflammation by Cytokine Signalling in Pancreatic Β
Activation of Islet Inflammation by Cytokine Signalling in Pancreatic b-cells Understanding the Role of Protein Tyrosine Phosphatases William James Stanley ORCID: 0000-0001-8001-2359 Student Number: 515467 Submitted in Total Fulfilment of The Degree of Doctor of Philosophy March 2020 St. Vincent’s Institute of Medical Research Department of Medicine (St. Vincent’s Hospital) The University of Melbourne Abstract: Type 1 diabetes is characterised by the autoimmune destruction of insulin producing β- cells in the islets of Langerhans of the pancreas. Immune cells release pro-inflammatory cytokines such as interferon-g (IFN-g), tumour necrosis factor-a (TNF-a) and interleukin- 1b (IL-1b) into the islet microenvironment which activate phosphorylation cascades and gene expression in b-cells that increase their susceptibility to autoimmune attack and destruction. Protein tyrosine phosphatases (PTPs) regulate phosphorylation based signalling pathways and have previously been shown to negatively regulate IFN-g induced cell death of β-cells in vitro. We previously showed that during immune infiltration to the islet PTPs, including PTPN1 and PTPN6, are rendered catalytically inactive through oxidation resulting in loss of signal regulation. The overall aim of this thesis is to observe if antioxidant treatment can reduce autoimmune development in the NOD/Lt mouse through reduction of oxidised PTPs and dissect the role of PTPN1 and PTPN6 in the regulation of cytotoxic signalling events in the NIT-1 β-cell line and isolated NODPI islets in vitro. Chapter 3 studies the effect of the mitochondrial targeted antioxidant mito-TEMPO on insulitis and diabetes development in the NOD/Lt mouse. Delivery of mito-TEMPO through drinking water reduced levels of oxidised PTPs in the pancreas of NOD/Lt mice but had no effect on the development of insulitis, activity or number of CD8+ and CD4+ T- cells in the periphery in NOD/Lt mice or diabetes development in a diabetes transfer model. -
![RT² Profiler PCR Array (96-Well Format and 384-Well [4 X 96] Format)](https://docslib.b-cdn.net/cover/9005/rt%C2%B2-profiler-pcr-array-96-well-format-and-384-well-4-x-96-format-1459005.webp)
RT² Profiler PCR Array (96-Well Format and 384-Well [4 X 96] Format)
RT² Profiler PCR Array (96-Well Format and 384-Well [4 x 96] Format) Human Protein Phosphatases Cat. no. 330231 PAHS-045ZA For pathway expression analysis Format For use with the following real-time cyclers RT² Profiler PCR Array, Applied Biosystems® models 5700, 7000, 7300, 7500, Format A 7700, 7900HT, ViiA™ 7 (96-well block); Bio-Rad® models iCycler®, iQ™5, MyiQ™, MyiQ2; Bio-Rad/MJ Research Chromo4™; Eppendorf® Mastercycler® ep realplex models 2, 2s, 4, 4s; Stratagene® models Mx3005P®, Mx3000P®; Takara TP-800 RT² Profiler PCR Array, Applied Biosystems models 7500 (Fast block), 7900HT (Fast Format C block), StepOnePlus™, ViiA 7 (Fast block) RT² Profiler PCR Array, Bio-Rad CFX96™; Bio-Rad/MJ Research models DNA Format D Engine Opticon®, DNA Engine Opticon 2; Stratagene Mx4000® RT² Profiler PCR Array, Applied Biosystems models 7900HT (384-well block), ViiA 7 Format E (384-well block); Bio-Rad CFX384™ RT² Profiler PCR Array, Roche® LightCycler® 480 (96-well block) Format F RT² Profiler PCR Array, Roche LightCycler 480 (384-well block) Format G RT² Profiler PCR Array, Fluidigm® BioMark™ Format H Sample & Assay Technologies Description The Human Protein Phosphatases RT² Profiler PCR Array profiles the gene expression of the 84 most important and well-studied phosphatases in the mammalian genome. By reversing the phosphorylation of key regulatory proteins mediated by protein kinases, phosphatases serve as a very important complement to kinases and attenuate activated signal transduction pathways. The gene classes on this array include both receptor and non-receptor tyrosine phosphatases, catalytic subunits of the three major protein phosphatase gene families, the dual specificity phosphatases, as well as cell cycle regulatory and other protein phosphatases. -
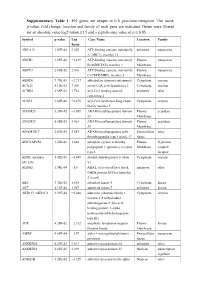
Supplementary Table 1
Supplementary Table 1. 492 genes are unique to 0 h post-heat timepoint. The name, p-value, fold change, location and family of each gene are indicated. Genes were filtered for an absolute value log2 ration 1.5 and a significance value of p ≤ 0.05. Symbol p-value Log Gene Name Location Family Ratio ABCA13 1.87E-02 3.292 ATP-binding cassette, sub-family unknown transporter A (ABC1), member 13 ABCB1 1.93E-02 −1.819 ATP-binding cassette, sub-family Plasma transporter B (MDR/TAP), member 1 Membrane ABCC3 2.83E-02 2.016 ATP-binding cassette, sub-family Plasma transporter C (CFTR/MRP), member 3 Membrane ABHD6 7.79E-03 −2.717 abhydrolase domain containing 6 Cytoplasm enzyme ACAT1 4.10E-02 3.009 acetyl-CoA acetyltransferase 1 Cytoplasm enzyme ACBD4 2.66E-03 1.722 acyl-CoA binding domain unknown other containing 4 ACSL5 1.86E-02 −2.876 acyl-CoA synthetase long-chain Cytoplasm enzyme family member 5 ADAM23 3.33E-02 −3.008 ADAM metallopeptidase domain Plasma peptidase 23 Membrane ADAM29 5.58E-03 3.463 ADAM metallopeptidase domain Plasma peptidase 29 Membrane ADAMTS17 2.67E-04 3.051 ADAM metallopeptidase with Extracellular other thrombospondin type 1 motif, 17 Space ADCYAP1R1 1.20E-02 1.848 adenylate cyclase activating Plasma G-protein polypeptide 1 (pituitary) receptor Membrane coupled type I receptor ADH6 (includes 4.02E-02 −1.845 alcohol dehydrogenase 6 (class Cytoplasm enzyme EG:130) V) AHSA2 1.54E-04 −1.6 AHA1, activator of heat shock unknown other 90kDa protein ATPase homolog 2 (yeast) AK5 3.32E-02 1.658 adenylate kinase 5 Cytoplasm kinase AK7 -

T Cells Deficient in the Tyrosine Phosphatase SHP-1 Resist Suppression by Regulatory T Cells
T Cells Deficient in the Tyrosine Phosphatase SHP-1 Resist Suppression by Regulatory T Cells This information is current as Emily R. Mercadante and Ulrike M. Lorenz of September 29, 2021. J Immunol published online 26 May 2017 http://www.jimmunol.org/content/early/2017/05/26/jimmun ol.1602171 Downloaded from Supplementary http://www.jimmunol.org/content/suppl/2017/05/26/jimmunol.160217 Material 1.DCSupplemental Why The JI? Submit online. http://www.jimmunol.org/ • Rapid Reviews! 30 days* from submission to initial decision • No Triage! Every submission reviewed by practicing scientists • Fast Publication! 4 weeks from acceptance to publication *average by guest on September 29, 2021 Subscription Information about subscribing to The Journal of Immunology is online at: http://jimmunol.org/subscription Permissions Submit copyright permission requests at: http://www.aai.org/About/Publications/JI/copyright.html Email Alerts Receive free email-alerts when new articles cite this article. Sign up at: http://jimmunol.org/alerts The Journal of Immunology is published twice each month by The American Association of Immunologists, Inc., 1451 Rockville Pike, Suite 650, Rockville, MD 20852 Copyright © 2017 by The American Association of Immunologists, Inc. All rights reserved. Print ISSN: 0022-1767 Online ISSN: 1550-6606. Published May 26, 2017, doi:10.4049/jimmunol.1602171 The Journal of Immunology T Cells Deficient in the Tyrosine Phosphatase SHP-1 Resist Suppression by Regulatory T Cells Emily R. Mercadante and Ulrike M. Lorenz The balance between activation of T cells and their suppression by regulatory T cells (Tregs) is dysregulated in autoimmune diseases and cancer. Autoimmune diseases feature T cells that are resistant to suppression by Tregs, whereas in cancer, T cells are unable to mount antitumor responses due to the Treg-enriched suppressive microenvironment.