In-Toeing, Out-Toeing, Growing Pains, Bowlegs, Knock-Knees and Flat Feet
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Pierre Robin and the Syndrome That Bears His Name PETER RANDALL
Pierre Robin and the Syndrome That Bears His Name PETER RANDALL, M.D. WILTON M. KROGMAN, Ph.D. SOONA JAHINA, B.D.S., M.Sc. Philadelphia, Pennsylvania The Pierre Robin Syndrome refers to a combination of micrognathia (a small jaw) and glossoptosis (literally, a falling downward or back- ward of the tongue) in the newborn infant (Figure 1). These conditions are likely to cause obstruction of the upper airway, and they are fre- quently associated with an incomplete cleft of the palate. Patients with the Pierre Robin Syndrome may present a real emer- gency in the delivery room because of the obstructed upper airway, or the airway problem may not become manifest for several days or weeks (10, 11, 38). There is frequently a feeding problem, as well as problems associated with the cleft of the palate (if one is present) and also an unusual malocclusion (2, 5, 12, 16). In addition, it presents a fascinating anthropological puzzle (22, 23). This paper will review the work of Dr. Robin, consider some possible etiologies of this syndrome, and report on some work on mandibular bone growth in a group of such patients. History Pierre Robin was far from the first person to recognize this syndrome. One account is recorded in 1822 by St. Hilaire. In 1891 Taruffi men- tioned two subclassifications-hypomicrognatus (small jaw) and hypo- agnathus (absent jaw). In 1891, four cases, two of them having cleft palates, were reported by Lanneloague and Monard (12, 14). Shukow- sky in 1902 described a tongue to lip surgical adhesion to overcome the respiratory obstruction (34). -

Podo Pediatrics Podo Pediatrics
Podo Pediatrics Identifying Biomechanical Pathologies David Lee, D.P.M., D. A.B.P.S. Purpose • Identification of mechanical foot and ankle conditions • Base treatments • Knowing when to refer to a podiatrist Topics • Flatfoot (Pes Plano Valgus) • Equinus • Intoed feet (Cavo-adductor Varus) • Heel pain (Calcaneodynia) • Shin Splints • Various Pedal deformities 1 WHAT IS NORMAL? At birth to ~9 months • Ankle flexible to over 20 deg DF • No “C” shaped foot • No clicking or popping sounds • Babinski sign • Pull up 7-8mo. 9-16 months… • Begin walking • Feet are fat, flat and floppy • Knees are always center or externally rotated, never internal. • Stance is wide and less stable • Stomping gait pattern 2 16-18 months • Able to walk upstairs • Knee never internal • Still wide base and flat and floppy feet • Stomping still 3-7 years • Able toe walk downstairs • Heel-to-toe walk • Watch for – Intoeing – Tripping – Tight ankle joint (equinus) 7 years and up • Arch should be developed • Heel-to-toe walk • Heel is perpendicular to ground • Knees straight ahead 3 Neutral Internal Rotation Early detection is important • Prevent long term adaptation • Joint damage • Adult pathology – Heel pain, bunions, hammertoes, ankle instability, knee pain, shin splints, etc. • Ability to thrive physically and socially 4 THE FLAT FOOT Visual Complaints by the Parent • Tripping or falling • Poor balance- Clumsy • Feet look funny, walks funny • Shoes wearing out quickly Social Complaints by the Parent • Lazy, inactive, “doesn’t like going outside to play or play sports -

Metatarsalgia
just the symptoms. What can I expect from treatment? With a proper diagnosis, and a well-rounded treatment plan including orthotics, the prog- nosis is excellent. With Sole Supports™ foot or- thotics you can expect either a dramatic loss The Truth About . of pain within the first weeks of use or a more gradual reduction of symptoms, depending Metatarsalgia on how long the problem has existed, normal body weight or how well you follow other ther- For more information and a apeutic regimens prescribed by your provider. professional consultation regarding Did you know that, with Sole whether Sole Supports may be Supports, metatarsal pads are rarely helpful for you, please contact the needed? following certified Sole Supports practitioner: What is it? Metatarsalgia is a term used to describe a pain- ful foot condition in the area just before the Arch Flattened small toes (more commonly referred to as the ball of the foot). The condition is characterized by pain and inflammation on the sole in the region of the metatarsal heads, which are the ends of the long bones in your foot. The joint This handout provides a general overview on this capsule or tendons may also be inflamed. topic and may not apply to everyone. To find out if this handout applies to you and to get more infor- mation on this subject, consult with your certified Sole Supports practitioner. Arch Restored The pain is generally aggravated by putting ments but your doctor is likely to recommend pressure off the metatarsals should also be pressure (as in walking) through the ball of a conservative approach first including: followed. -

Wound Classification
Wound Classification Presented by Dr. Karen Zulkowski, D.N.S., RN Montana State University Welcome! Thank you for joining this webinar about how to assess and measure a wound. 2 A Little About Myself… • Associate professor at Montana State University • Executive editor of the Journal of the World Council of Enterstomal Therapists (JWCET) and WCET International Ostomy Guidelines (2014) • Editorial board member of Ostomy Wound Management and Advances in Skin and Wound Care • Legal consultant • Former NPUAP board member 3 Today We Will Talk About • How to assess a wound • How to measure a wound Please make a note of your questions. Your Quality Improvement (QI) Specialists will follow up with you after this webinar to address them. 4 Assessing and Measuring Wounds • You completed a skin assessment and found a wound. • Now you need to determine what type of wound you found. • If it is a pressure ulcer, you need to determine the stage. 5 Assessing and Measuring Wounds This is important because— • Each type of wound has a different etiology. • Treatment may be very different. However— • Not all wounds are clear cut. • The cause may be multifactoral. 6 Types of Wounds • Vascular (arterial, venous, and mixed) • Neuropathic (diabetic) • Moisture-associated dermatitis • Skin tear • Pressure ulcer 7 Mixed Etiologies Many wounds have mixed etiologies. • There may be both venous and arterial insufficiency. • There may be diabetes and pressure characteristics. 8 Moisture-Associated Skin Damage • Also called perineal dermatitis, diaper rash, incontinence-associated dermatitis (often confused with pressure ulcers) • An inflammation of the skin in the perineal area, on and between the buttocks, into the skin folds, and down the inner thighs • Scaling of the skin with papule and vesicle formation: – These may open, with “weeping” of the skin, which exacerbates skin damage. -
Metatarsalgia
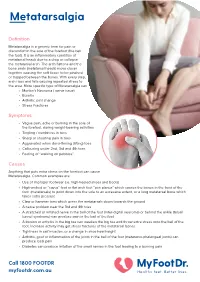
Metatarsalgia Definition Metatarsalgia is a generic term for pain or discomfort in the sole of the forefoot (the ball of the foot). It is an inflammatory condition of the metatarsal heads due to a drop or collapse of the metatarsal arch. The arch flattens and the bone ends (metatarsal heads) move closer together causing the soft tissue to be pinched or trapped between the bones. With every step, the arch rises and falls causing repeated stress to the area. More specific type of Metatarsalgia can be: • Morton’s Neuroma ( nerve issue) • Bursitis • Arthritic joint change • Stress Fractures Symptoms • Vague pain, ache or burning in the sole of the forefoot, during weight-bearing activities • Tingling / numbness in toes • Sharp or shooting pain in toes • Aggravated when dorsi-flexing (lifting) toes • Callousing under 2nd, 3rd and 4th toes • Feeling of “walking on pebbles” Causes Anything that puts extra stress on the forefoot can cause Metatarsalgia. Common examples are: • Use of improper footwear (i.e. high-heeled shoes and boots) • High-arched or “cavus” foot or flat arch feet “pes planus” which causes the bones in the front of the foot (metatarsals) to point down into the sole to an excessive extent, or a long metatarsal bone which takes extra pressure • Claw or hammer toes which press the metatarsals down towards the ground • A nerve problem near the 3rd and 4th toes • A stretched or irritated nerve in the ball of the foot (inter-digital neuroma) or behind the ankle (tarsal tunnel syndrome) can produce pain in the ball of the foot • A bunion or arthritis in the big toe can weaken the big toe and throw extra stress onto the ball of the foot. -

Treatment of Spastic Foot Deformities
TREATMENT OF SPASTIC FOOT DEFORMITIES penn neuro-orthopaedics service Table of Contents OVERVIEW Severe loss of movement is often the result of neurological disorders, Overview .............................................................. 1 such as stroke or brain injury. As a result, ordinary daily activities Treatment ............................................................. 2 such as walking, eating and dressing can be difficult and sometimes impossible to accomplish. Procedures ........................................................... 4 The Penn Neuro-Orthopaedics Service assists patients with Achilles Tendon Lengthening .........................................4 orthopaedic problems caused by certain neurologic disorders. Our Toe Flexor Releases .....................................................5 team successfully treats a wide range of problems affecting the limbs including foot deformities and walking problems due to abnormal Toe Flexor Transfer .......................................................6 postures of the foot. Split Anterior Tibialis Tendon Transfer (SPLATT) ...............7 This booklet focuses on the treatment of spastic foot deformities The Extensor Tendon of the Big Toe (EHL) .......................8 under the supervision of Keith Baldwin, MD, MSPT, MPH. Lengthening the Tibialis Posterior Tendon .......................9 Care After Surgery .................................................10 Notes ..................................................................12 Pre-operative right foot. Post-operative -

The Indications for Toe Transfer After ''Minor
ARTICLE IN PRESS Invited personal view article THE INDICATIONS FOR TOE TRANSFER AFTER ‘‘MINOR’’ FINGER INJURIES F DEL PINAL* From the Institute for Hand and Plastic Surgery, Private Practice, and Mutua Montan*esa, Santander, Spain Toe-to-hand transfer is widely considered to be unjustified for ‘‘minor’’ finger injuries. In this invited personal view article the indications for toe-to-hand transfer for finger amputation and neurocutaneous and major pulp defects are discussed, and a classification of multidigital injury that has both prognostic and decision-making value is presented. In the author’s opinion a toe transfer should always be considered as an option when reconstructing ‘‘minor’’ finger injuries, as it can reproduce significant long-term benefit to the hand and the patient’s sense of well being. The procedure should be carried out in the acute period, not only because it is technically easier and better for hand function, but above all because the surgeon can save structures that will be lost if the transfer is delayed. Journal of Hand Surgery (British and European Volume, 2004) 29B: 2: 120–129 Keywords: microsurgery, toe-to-hand, finger amputation Since the hand is always naked and exposed, even if reconstruction. In this personal view article only the only the fingertip is lost, it presents a very large most ‘‘typical’’ indications will be discussed. The handicap for the patient. (Hirase! et al., 1997) metacarpal hand (Tan et al., 1999; Wei et al., 1997, 1999; Yu and Huang, 2000), congenital reconstruction There was a time when only loss of the thumb was (Kay and Wiberg, 1996; Shibata et al., 1998; Van Holder considered an acceptable indication for toe-to-hand et al., 1999), joint transfer (Dautel and Merle 1997; transfer (Buncke et al., 1973; Cobbett, 1969). -

How to Self-Bandage Your Leg(S) and Feet to Reduce Lymphedema (Swelling)
Form: D-8519 How to Self-Bandage Your Leg(s) and Feet to Reduce Lymphedema (Swelling) For patients with lower body lymphedema who have had treatment for cancer, including: • Removal of lymph nodes in the pelvis • Removal of lymph nodes in the groin, or • Radiation to the pelvis Read this resource to learn: • Who needs self-bandaging • Why self-bandaging is important • How to do self-bandaging Disclaimer: This pamphlet is for patients with lymphedema. It is a guide to help patients manage leg swelling with bandages. It is only to be used after the patient has been taught bandaging by a clinician at the Cancer Rehabilitation and Survivorship (CRS) Clinic at Princess Margaret Cancer Centre. Do not self-bandage if you have an infection in your abdomen, leg(s) or feet. Signs of an infection may include: • Swelling in these areas and redness of the skin (this redness can quickly spread) • Pain in your leg(s) or feet • Tenderness and/or warmth in your leg(s) or feet • Fever, chills or feeling unwell If you have an infection or think you have an infection, go to: • Your Family Doctor • Walk-in Clinic • Urgent Care Clinic If no Walk-in clinic is open, go to the closest hospital Emergency Department. 2 What is the lymphatic system? Your lymphatic system removes extra fluid and waste from your body. It plays an important role in how your immune system works. Your lymphatic system is made up of lymph nodes that are linked by lymph vessels. Your lymph nodes are bean-shaped organs that are found all over your body. -

Flexible Flatfoot
REVIEW ORTHOPEDICS & TRAUMATOLOGY North Clin Istanbul 2014;1(1):57-64 doi: 10.14744/nci.2014.29292 Flexible flatfoot Aziz Atik1, Selahattin Ozyurek2 1Department of Orthopedics and Tarumatology, Balikesir University Faculty of Medicine, Balikesir, Turkey; 2Department of Orthopedics and Traumatology, Aksaz Military Hospital, Marmaris, Mugla, Turkey ABSTRACT While being one of the most frequent parental complained deformities, flatfoot does not have a universally ac- cepted description. The reasons of flexible flatfoot are still on debate, but they must be differentiated from rigid flatfoot which occurs secondary to other pathologies. These children are commonly brought up to a physician without any complaint. It should be kept in mind that the etiology may vary from general soft tissue laxities to intrinsic foot pathologies. Every flexible flatfoot does not require radiological examination or treatment if there is no complaint. Otherwise further investigation and conservative or surgical treatment may necessitate. Key words: Children; flatfoot; flexible; foot problem; pes planus. hough the term flatfoot (pes planus) is gener- forms again (Figure 2). When weight-bearing forces Tally defined as a condition which the longitu- on feet are relieved this arch can be observed. If the dinal arch of the foot collapses, it has not a clinically foot is not bearing any weight, still medial longitu- or radiologically accepted universal definition. Flat- dinal arch is not seen, then it is called rigid (fixed) foot which we frequently encounter in routine out- flatfoot. To differentiate between these two condi- patient practice will be more accurately seen as a re- tions easily, Jack’s test (great toe is dorisflexed as the sult of laxity of ligaments of the foot. -

Hammer Toe Information Sheet
Fitter Feet For Life Hammer toe information sheet. (ref. A15) A hammer toe is a deformity of the first small toe joint with in toes. (proximal inter-phalangeal joint) This deformity can occur in the second, third, fourth or fifth (relatively rare) toes, causing it to be permanently bent, resembling a hammer. This abnormality can create pressure on the foot when wearing shoes and cause discomfort and problems walking. The joints themselves can be arthritic and painful. There is a choice of different procedures to straighten a hammer toe. This information sheet has been written to help you choose which procedure is best for you. Fig 1 Hammer toe . Fig 2 Arthrodesis with K wires . Fig 3. Smart toe implant An arthrodesis is a surgical procedure to treat hammer toes. The deformed joint is fully removed and the apposing bone ends fused together in a corrected position. The joint will no longer move. The joint closer to the end of the toe will still move. The joint where the toe joins the foot will also continue to move. 1 Fitter Feet For life. 34 North Street. London SW40HD 0207 627 4901 Fitter Feet For Life 1. K-Wire Arthrodesis. Traditionally hammer toe correction is performed by arthrodesis surgery using K-Wires. The procedure is successful in most cases and has been performed for many years. The deformed joint is removed and the bone ends are secured together with a K-wire which protrudes though the tip of the toe. The foot must be kept dry, dressed and the k-wire protected in a post operative shoe for six weeks after the operation. -

Comparison of the Upper and Lower Limbs-A Phylogenetic Concept
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-ISSN: 2279-0853, p-ISSN: 2279-0861.Volume 14, Issue 8 Ver. I (Aug. 2015), PP 14-16 www.iosrjournals.org Comparison of the Upper and Lower Limbs-A Phylogenetic Concept Dr.Vandana Sinam1, Dr.Thonthon Daimei2, I Deven Singh3, N Damayanti Devi4 1.Medical officer,2. Senior Resident,3. Assistant Proffessor,4. Professor and Head, Department of Anatomy Regional Institute of Medical Sciences, Imphal, Manipur Abstract: The upper and lower limbs of the human body are phylogenetically homologues of the forelimbs and hind limbs of the quadrupeds. Primates started lifting of the forelimbs off the ground for various functional adaptations as evolution progressed and this led to the deviation of the forelimbs from lower limbs. With the gradual diversification of the functions, morphological evolution of the two limbs follows closely leading to the differences in upper and the lower limbs in the human. Since the inception of the Anatomy as one of the curriculum in medical subjects, the anatomical position has been termed as one that the body stand erect with the eyes looking straight forward and the two upper limbs hanging by the side of the body with the palm facing forward. Therefore in this position the upper limb looked forward with the palm also accordingly faced forward too whilst with the thumb on the lateral side whilst in the lower limb, the big toe which is homologous to the thumb, is placed on the medial side. The anatomical position in the upper limb is not normally a comfortable position as it is kept in this position with effort. -

TRUFORM Classic Medical Closed Toe 20-30 Mmhg Thigh High
TRUFORM Classic Medical Closed Toe 20-30 mmHg Thigh High Stockings Measuring Guide for Compression Stockings Measuring your legs for compression stockings, support socks, support hose, and gradient compression hosiery: • For knee-highs: measure around your ankle and calf. Then, measure the distance from the floor to the back of your knee. • For thigh-high and pantyhose: measure around your ankle, calf, and upper thigh. Then, measure the distance from the floor to your upper thigh (bottom of your buttocks). An Important Measuring Tip... If swelling is an issue with you, measure your legs, first thing in the morning, after you get out of bed. This is when swelling is at a minimum, and the size of your legs should remain once the swelling is eliminated. Each of our compression products has a sizing chart on the product page. ANKLE CALF LENGTH Measure Measure Measure from around the around the the floor to the ankle at the calf muscle bend behind the narrowest at the knee. point, widest part. generally above the ankle bone. THIGH THIGH Measure LENGTH around the Measure thigh the distance approx. 3" from the below the bottom of gluteal fold your (crease of buttocks to buttocks). the floor. Sizes may differ between various brands of support stockings. Keep in mind that each manufacturer of support hose has their own sizing chart. A medium size in one brand of circulation stockings, may not be a medium in another. Some brands of compression stockings offer petite (shorter) lengths, while others do not. Knowing your measurements will ensure you get compression hosiery that fits properly and comfortably.