Causes Treatment Of
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Cutaneous Manifestations of HIV Infection Carrie L
Chapter Title Cutaneous Manifestations of HIV Infection Carrie L. Kovarik, MD Addy Kekitiinwa, MB, ChB Heidi Schwarzwald, MD, MPH Objectives Table 1. Cutaneous manifestations of HIV 1. Review the most common cutaneous Cause Manifestations manifestations of human immunodeficiency Neoplasia Kaposi sarcoma virus (HIV) infection. Lymphoma 2. Describe the methods of diagnosis and treatment Squamous cell carcinoma for each cutaneous disease. Infectious Herpes zoster Herpes simplex virus infections Superficial fungal infections Key Points Angular cheilitis 1. Cutaneous lesions are often the first Chancroid manifestation of HIV noted by patients and Cryptococcus Histoplasmosis health professionals. Human papillomavirus (verruca vulgaris, 2. Cutaneous lesions occur frequently in both adults verruca plana, condyloma) and children infected with HIV. Impetigo 3. Diagnosis of several mucocutaneous diseases Lymphogranuloma venereum in the setting of HIV will allow appropriate Molluscum contagiosum treatment and prevention of complications. Syphilis Furunculosis 4. Prompt diagnosis and treatment of cutaneous Folliculitis manifestations can prevent complications and Pyomyositis improve quality of life for HIV-infected persons. Other Pruritic papular eruption Seborrheic dermatitis Overview Drug eruption Vasculitis Many people with human immunodeficiency virus Psoriasis (HIV) infection develop cutaneous lesions. The risk of Hyperpigmentation developing cutaneous manifestations increases with Photodermatitis disease progression. As immunosuppression increases, Atopic Dermatitis patients may develop multiple skin diseases at once, Hair changes atypical-appearing skin lesions, or diseases that are refractory to standard treatment. Skin conditions that have been associated with HIV infection are listed in Clinical staging is useful in the initial assessment of a Table 1. patient, at the time the patient enters into long-term HIV care, and for monitoring a patient’s disease progression. -

WO 2014/134709 Al 12 September 2014 (12.09.2014) P O P C T
(12) INTERNATIONAL APPLICATION PUBLISHED UNDER THE PATENT COOPERATION TREATY (PCT) (19) World Intellectual Property Organization International Bureau (10) International Publication Number (43) International Publication Date WO 2014/134709 Al 12 September 2014 (12.09.2014) P O P C T (51) International Patent Classification: (81) Designated States (unless otherwise indicated, for every A61K 31/05 (2006.01) A61P 31/02 (2006.01) kind of national protection available): AE, AG, AL, AM, AO, AT, AU, AZ, BA, BB, BG, BH, BN, BR, BW, BY, (21) International Application Number: BZ, CA, CH, CL, CN, CO, CR, CU, CZ, DE, DK, DM, PCT/CA20 14/000 174 DO, DZ, EC, EE, EG, ES, FI, GB, GD, GE, GH, GM, GT, (22) International Filing Date: HN, HR, HU, ID, IL, IN, IR, IS, JP, KE, KG, KN, KP, KR, 4 March 2014 (04.03.2014) KZ, LA, LC, LK, LR, LS, LT, LU, LY, MA, MD, ME, MG, MK, MN, MW, MX, MY, MZ, NA, NG, NI, NO, NZ, (25) Filing Language: English OM, PA, PE, PG, PH, PL, PT, QA, RO, RS, RU, RW, SA, (26) Publication Language: English SC, SD, SE, SG, SK, SL, SM, ST, SV, SY, TH, TJ, TM, TN, TR, TT, TZ, UA, UG, US, UZ, VC, VN, ZA, ZM, (30) Priority Data: ZW. 13/790,91 1 8 March 2013 (08.03.2013) US (84) Designated States (unless otherwise indicated, for every (71) Applicant: LABORATOIRE M2 [CA/CA]; 4005-A, rue kind of regional protection available): ARIPO (BW, GH, de la Garlock, Sherbrooke, Quebec J1L 1W9 (CA). GM, KE, LR, LS, MW, MZ, NA, RW, SD, SL, SZ, TZ, UG, ZM, ZW), Eurasian (AM, AZ, BY, KG, KZ, RU, TJ, (72) Inventors: LEMIRE, Gaetan; 6505, rue de la fougere, TM), European (AL, AT, BE, BG, CH, CY, CZ, DE, DK, Sherbrooke, Quebec JIN 3W3 (CA). -

Cutaneous Manifestations of Newborns in Omdurman Maternity Hospital
ﺑﺴﻢ اﷲ اﻟﺮﺣﻤﻦ اﻟﺮﺣﻴﻢ Cutaneous Manifestations of Newborns in Omdurman Maternity Hospital A thesis submitted in the partial fulfillment of the degree of clinical MD in pediatrics and child health University of Khartoum By DR. AMNA ABDEL KHALIG MOHAMED ATTAR MBBS University of Khartoum Supervisor PROF. SALAH AHMED IBRAHIM MD, FRCP, FRCPCH Department of Pediatrics and Child Health University of Khartoum University of Khartoum The Graduate College Medical and Health Studies Board 2008 Dedication I dedicate my study to the Department of Pediatrics University of Khartoum hoping to be a true addition to neonatal care practice in Sudan. i Acknowledgment I would like to express my gratitude to my supervisor Prof. Salah Ahmed Ibrahim, Professor of Peadiatric and Child Health, who encouraged me throughout the study and provided me with advice and support. I am also grateful to Dr. Osman Suleiman Al-Khalifa, the Dermatologist for his support at the start of the study. Special thanks to the staff at Omdurman Maternity Hospital for their support. I am also grateful to all mothers and newborns without their participation and cooperation this study could not be possible. Love and appreciation to my family for their support, drive and kindness. ii Table of contents Dedication i Acknowledgement ii Table of contents iii English Abstract vii Arabic abstract ix List of abbreviations xi List of tables xiii List of figures xiv Chapter One: Introduction & Literature Review 1.1 The skin of NB 1 1.2 Traumatic lesions 5 1.3 Desquamation 8 1.4 Lanugo hair 9 1.5 -
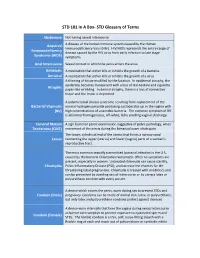
STD Glossary of Terms
STD 101 In A Box- STD Glossary of Terms Abstinence Not having sexual intercourse Acquired A disease of the human immune system caused by the Human Immunodeficiency Virus (HIV). HIV/AIDS represents the entire range of Immunodeficiency disease caused by the HIV virus from early infection to late stage Syndrome (AIDS) symptoms. Anal Intercourse Sexual contact in which the penis enters the anus. Antibiotic A medication that either kills or inhibits the growth of a bacteria. Antiviral A medication that either kills or inhibits the growth of a virus. A thinning of tissue modified by the location. In epidermal atrophy, the epidermis becomes transparent with a loss of skin texture and cigarette Atrophic paper-like wrinkling. In dermal atrophy, there is a loss of connective tissue and the lesion is depressed. A polymicrobial clinical syndrome resulting from replacement of the Bacterial Vaginosis normal hydrogen peroxide producing Lactobacillus sp. in the vagina with (BV) high concentrations of anaerobic bacteria. The common symptom of BV is abnormal homogeneous, off-white, fishy smelling vaginal discharge. Cervical Motion A sign found on pelvic examination suggestive of pelvic pathology; when Tenderness (CMT) movement of the cervix during the bimanual exam elicits pain. The lower, cylindrical end of the uterus that forms a narrow canal Cervix connecting the upper (uterus) and lower (vagina) parts of a woman's reproductive tract. The most common sexually transmitted bacterial infection in the U.S., caused by the bacteria Chlamydia trachomatis. Often no symptoms are present, especially in women. Untreated chlamydia can cause sterility, Chlamydia Pelvic Inflammatory Disease (PID), and increase the chances for life- threatening tubal pregnancies. -

Approach to Elephantiasis Nostra of Unclear Etiology: a Case Report with a Brief Review
Journal of Phebology and Lymphology Approach to Elephantiasis Nostra of Unclear Etiology: A Case Report with a Brief Review Authors: Hamit Serdar BAŞBUĞ, Macit BİTARGİ, Kanat ÖZIŞIK Affiliation: Kafkas University Faculty of Medicine, Department of Cardiovascular Surgery, Kars, TURKEY Adress: 1Physiotherapist, Post Graduate Lato Sensu Course on Lymphovenous Rehabilitation of the Medical School in São José do Rio Preto‐FAMERP‐ Rua Tursa 1442 ,apto 201‐ Barroca ‐ Belo Horizonte‐Minas Gerais‐Brazil‐Cep 30431‐091 E‐mail: [email protected]*corresponding author Published: April 2015 Received: January 2015 Journal Phlebology and Lymphology 2015; 8:1‐5 Accepted: 20 March 2015 Abstract Lower extremity lymphedema is an important clinical condition causing morbidity and is frequently encountered by the phlebologists. Elephantiasis Nostra is the status characterized with the extraordinary massive swelling of one or both legs with subsequent thickening and fibrosis of the overlying skin. It is an exaggerated manifestation of a longstanding chronic lymphedema. Etiologically, secondary lymphedema is caused by an external effect such as a chronic lymphangitis, removal of the lymph nodes, trauma, mechanical obstruction, radiotherapy, venous insufficiency, obesity, heart failure, bacterial or helminthic infection (Lymphatic Filariasis), in contrary to the primary lymphedema in which an inherent malfunction of lymphatic channels exists. A morbidly obese female patient with a bilateral Elephantiasis Nostra and our effort on setting the etiological definition and the treatment approach is presented. Key words: Lymphoedema; obesity; leg ulcers Introduction Elephantiasis is the end result of lymphogranuloma Elephantiasis is a progressive enlargement of an extremity venereum, and lastly the Proteus Syndrome which is an 4 or body part accompanied by a chronic inflammatory genetic disorder widely called as "Elephant Man" . -

Survey of Skin Disorders in Newborns: Clinical Observation in an Egyptian Medical Centre Nursery A.A
املجلة الصحية لرشق املتوسط املجلد الثامن عرش العدد اﻷول Survey of skin disorders in newborns: clinical observation in an Egyptian medical centre nursery A.A. El-Moneim 1 and R.E. El-Dawela 2 مسح لﻻضطرابات اجللدية لدى الولدان: مﻻحظة رسيرية يف حضانة يف مركز طبي يف مرص عبري أمحد عبد املنعم، رهيام عز الدولة الرشقاوي اخلﻻصة:مل َ ْت َظ اﻻضطرابات اجللدية لدى الولدان بدراسات جيدة يف مرص. وقد هدفت الباحثتان إىل دراسة أنامط التغريات اجللدية يف عينة من ِ الولدان املرصيني، وهي دراسة وصفية استباقية أترابية شملت ستة مئة وليد يف َّحضانة يف مستشفى جامعة سوهاج، َّوتضمنت الفحص اجللدي خﻻل اﻷيام اخلمسة اﻷوىل بعد الوﻻدة. وقد تم كشف اﻻضطرابات اجللدية لدى 240 ًوليدا )40%( ولوحظت الومحات لدى 100 وليد )%16.7(، ومعظمها من النمط ذي اخلﻻيا امليﻻنية )لطخات منغولية لدى 11.7% مع ومحات وﻻدية ذات ميﻻنية اخلﻻيا لدى 2.7%(. كام ُك ِش َف ْت العداوى الفطرية اجللدية، ومنها داء َّاملبيضات الفموية، وعدوى الفطريات يف مناطق احلفاظات أو َالـم َذح الناجم عن عدوى َّاملبيضات يف اﻷرفاغ )أصل الفخذ(، وذلك لدى 13.3%، ُوكشفت بعض العداوى اجلرثومية يف 1.3%من الولدان. وتشري املقارنات مع الدراسات اﻷخرى يف أرجاء العامل إىل معدل مرتفع للعدوى بالفطريات مع معدل منخفض للومحات الوﻻدية يف دراستنا للولدان، وتويص الباحثتان بإجراء تقييم روتيني جلدي للولدان، ّوﻻسيام يف ضوء املعدﻻت املرتفعة للعدوى اجللدية بالفطريات. ABSTRACT The frequency of neonatal skin disorders has not been well studied in Egypt. Our aim was to address patterns of dermatological changes in a sample of Egyptian newborns. In a descriptive prospective cohort study 600 newborns in Sohag University hospital nursery were dermatologically examined within the first 5 days of birth. -

Elephantiasis Nostras Verrucosa in Leprosy
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-ISSN: 2279-0853, p-ISSN: 2279-0861. Volume 5, Issue 4 (Mar.- Apr. 2013), PP 35-36 www.iosrjournals.org Elephantiasis Nostras Verrucosa in leprosy. Sonam Goyal1, S.N Mahajan2, Sourya Acharya3, Adarsh Lata Singh4 1. Resident, Dept of Medicine 2. Professor and HOD , Dept of Medicine 3. Professor ,Dept of Medicine 4. Professor and HOD ,Dept of Dermatology and Venereal Diseases. Abstract: We present a case of Elephantiasis Nostras Verrucosa in a patient of leprosy with peripheral neuropathy. Key Words: ENV, Leprosy, peripheral neuropathy I. Introduction: Elephantiasis nostras verrucosa (ENV) is the progressive disfiguring enlargement of a body part caused by recurrent soft tissue bacterial infections in the setting of chronic secondary lymphedema. The basic predisposing factor its development is lymphatic obstruction in any part of the body. This obstruction may be primary or secondary due to long standing non lymphatic edematous conditions that ultimately lead to secondary obstruction to lymph flow. Secondary infections due to poor vascularity, neuropathy and lymphedema further aggravates the clinical situation. II. Case Report: A 70 Years old male patient presented to us with chief complain of swelling and disfigurement, foul smelling discharge in bilateral lower limbs since 1 month. He was diagnosed case of lepromatous leprosy and was on anti leprosy treatment since 8 months .At the time of the diagnosis of leprosy his nerve conduction study had been done which revealed demyelinating -

| Oa Tai Ei Rama Telut Literatur
|OA TAI EI US009750245B2RAMA TELUT LITERATUR (12 ) United States Patent ( 10 ) Patent No. : US 9 ,750 ,245 B2 Lemire et al. ( 45 ) Date of Patent : Sep . 5 , 2017 ( 54 ) TOPICAL USE OF AN ANTIMICROBIAL 2003 /0225003 A1 * 12 / 2003 Ninkov . .. .. 514 / 23 FORMULATION 2009 /0258098 A 10 /2009 Rolling et al. 2009 /0269394 Al 10 /2009 Baker, Jr . et al . 2010 / 0034907 A1 * 2 / 2010 Daigle et al. 424 / 736 (71 ) Applicant : Laboratoire M2, Sherbrooke (CA ) 2010 /0137451 A1 * 6 / 2010 DeMarco et al. .. .. .. 514 / 705 2010 /0272818 Al 10 /2010 Franklin et al . (72 ) Inventors : Gaetan Lemire , Sherbrooke (CA ) ; 2011 / 0206790 AL 8 / 2011 Weiss Ulysse Desranleau Dandurand , 2011 /0223114 AL 9 / 2011 Chakrabortty et al . Sherbrooke (CA ) ; Sylvain Quessy , 2013 /0034618 A1 * 2 / 2013 Swenholt . .. .. 424 /665 Ste - Anne -de - Sorel (CA ) ; Ann Letellier , Massueville (CA ) FOREIGN PATENT DOCUMENTS ( 73 ) Assignee : LABORATOIRE M2, Sherbrooke, AU 2009235913 10 /2009 CA 2567333 12 / 2005 Quebec (CA ) EP 1178736 * 2 / 2004 A23K 1 / 16 WO WO0069277 11 /2000 ( * ) Notice : Subject to any disclaimer, the term of this WO WO 2009132343 10 / 2009 patent is extended or adjusted under 35 WO WO 2010010320 1 / 2010 U . S . C . 154 ( b ) by 37 days . (21 ) Appl. No. : 13 /790 ,911 OTHER PUBLICATIONS Definition of “ Subject ,” Oxford Dictionary - American English , (22 ) Filed : Mar. 8 , 2013 Accessed Dec . 6 , 2013 , pp . 1 - 2 . * Inouye et al , “ Combined Effect of Heat , Essential Oils and Salt on (65 ) Prior Publication Data the Fungicidal Activity against Trichophyton mentagrophytes in US 2014 /0256826 A1 Sep . 11, 2014 Foot Bath ,” Jpn . -

Non-Dermatomal Varicella-Zoster Skin Infection: Disseminated Cutaneous Herpes Zoster Without Dermatome in an Immunosuppressed Woman
Volume 23 Number 10 | October 2017 Dermatology Online Journal || Case Report DOJ 23 (10): 4 Non-dermatomal varicella-zoster skin infection: disseminated cutaneous herpes zoster without dermatome in an immunosuppressed woman Lindsay P Osborn1 BA,, Philip R Cohen2 MD Affiliations: 1Medical College of Georgia, Augusta, Georgia, 2University of California, San Diego, California Corresponding Author: Lindsay P. Osborn, 1 Seventh Street, Suite 1403, Augusta, GA 30901, Email: [email protected] Introduction Abstract Herpes viral infection in humans includes both Disseminated herpes zoster is defined as the presence herpes simplex (HSV) and herpes zoster. The varicella of more than 20 lesions outside the dermatome. zoster virus (VZV) is the etiology of both primary This unusual presentation is more common in varicella and herpes zoster (commonly known as immunosuppressed patients. Complications such chicken pox and shingles, respectively), with herpes as hepatitis, encephalitis, and pneumonitis are more zoster being the re-activated form of the virus. The likely in individuals with disseminated varicella zoster classical presentation of herpes zoster is a unilateral virus infection. distribution of vesicles along a single or adjacent dermatome [1]. Disseminated herpes zoster is A 63-year-old woman being treated for breast cancer defined as having more than 20 lesions outside the developed multiple pustules and vesicles days primary or adjacent dermatome [2]. after starting doxorubicin and cyclophosphamide chemotherapy. Ten individual lesions appeared on Although uncommon among all herpes zoster her chest, abdomen, back, and leg. Non-dermatomal infections, the prevalence of disseminated VZV in disseminated herpes zoster was suspected. She was a setting of immunosuppression is thought to be treated with oral antiviral therapy, as well as with oral anywhere from 10 to 40% [3, 4]. -

Unusual Cause of Saxophone Penis
Letters to the Editor AAddressddress fforor ccorrespondence:orrespondence: Dr. Amar Surjushe, Department of Other causes of genital elephantiasis like infections and Dermatology, Venereology, and Leprology, Grant Medical College and [3,4] Sir JJ Groups of Hospitals, Mumbai - 400 008, India. malignancies are very rare. E-mail: [email protected] A 45-year-old man, father of four, with swelling of scrotum RREFERENCESEFERENCES and penis of about 2 months duration was referred by a surgeon. Onset was sudden and within 2 weeks he developed 1. Wilson B. Necrotizing fasciitis. Am Surg 1952;18:416-31. 2. Weinberg AN, Swartz MN, Tsao H, Johnson RA. Fitzpatrick’s a large swelling of penis and scrotum. He only had a feeling dermatology in general medicine. In: Freedberg IM, Eisen of heaviness and was depressed due to the embarrassing AZ, Wolff K, Austen KF, Goldsmith LA, Katz SI, editors. Soft condition. There was no history of injury, operation, or tissue infections: Erysipelas, cellulitis, gangrenous cellulitis radiation prior to the onset. He had a large number of pus- and myonecrosis. 6th ed. New York: McGraw- Hill Publishing filled eruptions on both legs with fever, about 8 weeks prior Division; 2003. p. 1883-95. to the onset. He was treated by a doctor (non-dermatologist) 3. Melish ME, Bertuch AA. Bacterial skin infections. In: with oral and topical antibiotics. All lesions had healed in Feigin RD, Cherry JD, editors. Textbook of pediatric 10-15 days leaving behind scars. There was no history of infectious diseases. 4th ed. Philadelphia: W.B. Saunders Company; 1998. p. 741-52. extramarital sexual contact or genital ulcer disease. -

Cellulitis: a Review of 62
Clinical Review & Education Review Cellulitis A Review Adam B. Raff, MD, PhD; Daniela Kroshinsky, MD, MPH CME Quiz at IMPORTANCE Cellulitis is an infection of the deep dermis and subcutaneous tissue, presenting jamanetworkcme.com with expanding erythema, warmth, tenderness, and swelling. Cellulitis is a common global health burden, with more than 650 000 admissions per year in the United States alone. OBSERVATIONS In the United States, an estimated 14.5 million cases annually of cellulitis account for $3.7 billion in ambulatory care costs alone. The majority of cases of cellulitis are nonculturable and therefore the causative bacteria are unknown. In the 15% of cellulitis cases in which organisms are identified, most are due to β-hemolytic Streptococcus and Staphylococcus aureus. There are no effective diagnostic modalities, and many clinical conditions appear similar. Treatment of primary and recurrent cellulitis should initially cover Streptococcus and methicillin-sensitive S aureus, with expansion for methicillin-resistant S aureus (MRSA) in cases of cellulitis associated with specific risk factors, such as athletes, children, men who have sex with men, prisoners, military recruits, residents of long-term care facilities, those with prior MRSA exposure, and intravenous drug users. Five days of treatment is sufficient with extension if symptoms are not improved. Addressing predisposing factors can minimize risk of recurrence. CONCLUSIONS AND RELEVANCE The diagnosis of cellulitis is based primarily on history and Author Affiliations: Harvard Medical physical examination. Treatment of uncomplicated cellulitis should be directed against School, Massachusetts General Streptococcus and methicillin-sensitive S aureus. Failure to improve with appropriate first-line Hospital, Boston. antibiotics should prompt consideration for resistant organisms, secondary conditions that Corresponding Author: Daniela mimic cellulitis, or underlying complicating conditions such as immunosuppression, chronic Kroshinsky, MD, MPH, liver disease, or chronic kidney disease. -

Obesity-Associated Abdominal Elephantiasis
Hindawi Publishing Corporation Case Reports in Medicine Volume 2013, Article ID 626739, 3 pages http://dx.doi.org/10.1155/2013/626739 Case Report Obesity-Associated Abdominal Elephantiasis Ritesh Kohli,1 Vivian Argento,2 and Yaw Amoateng-Adjepong3 1 Department of Internal Medicine, Bridgeport Hospital, Yale University School of Medicine, Columbia Tower, Appt. no. 308, 50 Ridgefield Avenue, Bridgeport, CT 06610, USA 2 Geriatric Fellowship, Bridgeport Hospital, Yale University School of Medicine, 267 Grant Street, CT 06610, USA 3 Department of Internal Medicine, Bridgeport Hospital, Yale University School of Medicine, 267 Grant Street, CT 06610, USA Correspondence should be addressed to Ritesh Kohli; [email protected] Received 28 November 2012; Revised 1 March 2013; Accepted 5 March 2013 Academic Editor: Jeffrey M. Weinberg Copyright © 2013 Ritesh Kohli et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Abdominal elephantiasis is a rare entity. Abdominal elephantiasis is an uncommon, but deformative and progressive cutaneous disease caused by chronic lymphedema and recurrent streptococcal or Staphylococcus infections of the abdominal wall. We present 3 cases of patients with morbid obesity who presented to our hospital with abdominal wall swelling, thickening, erythema, and pain. The abdominal wall and legs were edematous, with cobblestone-like, thickened, hyperpigmented, and fissured plaques on the abdomen. Two patients had localised areas of skin erythema, tenderness, and increased warmth. There was purulent drainage from the abdominal wall in one patient. They were managed with antibiotics with some initial improvement.