A Narrative Review on C3 Glomerulopathy: a Rare Renal Disease
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

A Novel CFHR5 Mutation Associated with C3 Glomerulonephritis in a Turkish Girl
A novel CFHR5 mutation associated with C3 glomerulonephritis in a Turkish girl Nesrin Besbas, Bora Gulhan, Safak Gucer, Emine Korkmaz & Fatih Ozaltin Journal of Nephrology ISSN 1121-8428 Volume 27 Number 4 J Nephrol (2014) 27:457-460 DOI 10.1007/s40620-013-0008-1 1 23 Your article is protected by copyright and all rights are held exclusively by Italian Society of Nephrology. This e-offprint is for personal use only and shall not be self- archived in electronic repositories. If you wish to self-archive your article, please use the accepted manuscript version for posting on your own website. You may further deposit the accepted manuscript version in any repository, provided it is only made publicly available 12 months after official publication or later and provided acknowledgement is given to the original source of publication and a link is inserted to the published article on Springer's website. The link must be accompanied by the following text: "The final publication is available at link.springer.com”. 1 23 Author's personal copy J Nephrol (2014) 27:457–460 DOI 10.1007/s40620-013-0008-1 CASE REPORT A novel CFHR5 mutation associated with C3 glomerulonephritis in a Turkish girl Nesrin Besbas • Bora Gulhan • Safak Gucer • Emine Korkmaz • Fatih Ozaltin Received: 17 July 2013 / Accepted: 31 July 2013 / Published online: 5 December 2013 Ó Italian Society of Nephrology 2013 Abstract C3 glomerulopathy defines a subgroup of syndrome and persistently low C3 level, thus expanding the membranoproliferative glomerulonephritis (MPGN) char- genetic and phenotypic spectrum of the disease. Ecu- acterized by complement 3 (C3)-positive, immunoglobu- lizumab seems to be ineffective in this subtype. -

This Thesis Has Been Submitted in Fulfilment of the Requirements for a Postgraduate Degree (E.G
This thesis has been submitted in fulfilment of the requirements for a postgraduate degree (e.g. PhD, MPhil, DClinPsychol) at the University of Edinburgh. Please note the following terms and conditions of use: This work is protected by copyright and other intellectual property rights, which are retained by the thesis author, unless otherwise stated. A copy can be downloaded for personal non-commercial research or study, without prior permission or charge. This thesis cannot be reproduced or quoted extensively from without first obtaining permission in writing from the author. The content must not be changed in any way or sold commercially in any format or medium without the formal permission of the author. When referring to this work, full bibliographic details including the author, title, awarding institution and date of the thesis must be given. Endothelin‐1 antagonism in glomerulonephritis Elizabeth Louise Owen BSc. (Hons), MSc. A thesis submitted towards the degree of PhD The University of Edinburgh 2016 Declaration I declare that the work presented in this thesis is my own and has not previously been published or presented towards another higher degree except where clearly acknowledged as such in the text. ……………………………………… …………. Elizabeth Louise Owen Date Page | 2 Acknowledgements I would like to express my gratitude to my supervisor David Kluth for his support, guidance and efforts during my PhD; Bean, thankyou for your patience and input. Thankyou also to Jeremy Hughes and Simon Brown for your advice and input for the various aspects of labwork, presentations and general how to’s. Jason King, thanks for all your help in the lab, you were always my ‘go‐to‐guy’ for all things technical….and for your many cool pairs of trainers. -

Complement Factor H–Related Hybrid Protein Deregulates Complement in Dense Deposit Disease
Complement factor H–related hybrid protein deregulates complement in dense deposit disease Qian Chen, … , Christine Skerka, Peter F. Zipfel J Clin Invest. 2014;124(1):145-155. https://doi.org/10.1172/JCI71866. Research Article Nephrology The renal disorder C3 glomerulopathy with dense deposit disease (C3G-DDD) pattern results from complement dysfunction and primarily affects children and young adults. There is no effective treatment, and patients often progress to end-stage renal failure. A small fraction of C3G-DDD cases linked to factor H or C3 gene mutations as well as autoantibodies have been reported. Here, we examined an index family with 2 patients with C3G-DDD and identified a chromosomal deletion in the complement factor H–related (CFHR) gene cluster. This deletion resulted in expression of a hybrid CFHR2-CFHR5 plasma protein. The recombinant hybrid protein stabilized the C3 convertase and reduced factor H–mediated convertase decay. One patient was refractory to plasma replacement and exchange therapy, as evidenced by the hybrid protein quickly returning to pretreatment plasma levels. Subsequently, complement inhibitors were tested on serum from the patient for their ability to block activity of CFHR2-CFHR5. Soluble CR1 restored defective C3 convertase regulation; however, neither eculizumab nor tagged compstatin had any effect. Our findings provide insight into the importance of CFHR proteins for C3 convertase regulation and identify a genetic variation in the CFHR gene cluster that promotes C3G-DDD. Monitoring copy number and sequence variations in the CFHR gene cluster in C3G-DDD and kidney patients with C3G-DDD variations will help guide treatment strategies. Find the latest version: https://jci.me/71866/pdf Research article Complement factor H–related hybrid protein deregulates complement in dense deposit disease Qian Chen,1 Michael Wiesener,2 Hannes U. -

Glomerulonephritis Management in General Practice
Renal disease • THEME Glomerulonephritis Management in general practice Nicole M Isbel MBBS, FRACP, is Consultant Nephrologist, Princess Alexandra lomerular disease remains an important cause Hospital, Brisbane, BACKGROUND Glomerulonephritis (GN) is an G and Senior Lecturer in important cause of both acute and chronic kidney of renal impairment (and is the commonest cause Medicine, University disease, however the diagnosis can be difficult of end stage kidney disease [ESKD] in Australia).1 of Queensland. nikky_ due to the variability of presenting features. Early diagnosis is essential as intervention can make [email protected] a significant impact on improving patient outcomes. OBJECTIVE This article aims to develop However, presentation can be variable – from indolent a structured approach to the investigation of patients with markers of kidney disease, and and asymptomatic to explosive with rapid loss of kidney promote the recognition of patients who need function. Pathology may be localised to the kidney or further assessment. Consideration is given to the part of a systemic illness. Therefore diagnosis involves importance of general measures required in the a systematic approach using a combination of clinical care of patients with GN. features, directed laboratory and radiological testing, DISCUSSION Glomerulonephritis is not an and in many (but not all) cases, a kidney biopsy to everyday presentation, however recognition establish the histological diagnosis. Management of and appropriate management is important to glomerulonephritis (GN) involves specific therapies prevent loss of kidney function. Disease specific directed at the underlying, often immunological cause treatment of GN may require specialist care, of the disease and more general strategies aimed at however much of the management involves delaying progression of kidney impairment. -

Diffuse Proliferative Glomerulonephritis and Acute Renal Failure Associated with Acute Staphylococcal Osteomyelitis
Diffuse Proliferative Glomerulonephritis and Acute Renal Failure Associated with Acute Staphylococcal Osteomyelitis MATTHEW D. GRIFFIN,* JOHANNES BJORNSSON,t and STEPHEN B. ERICKSON* *Department of Internal Medicine, Division of Nephrology, and tDepartment of Pathology, Mayo Clinic and Mayo Foundation, Rochester, Minnesota. Abstract. A 72-year-old man developed acute renal failure after peated surgical debridement. Spontaneous recovery of renal coronary bypass surgery that had been complicated by sternal function occurred after eradication of infection and final sur- osteomyelitis caused by the Staphylococcus aureus bacterium. gical wound repair. The relationship between acute bacterial Bacteremia and sepsis were not present. Renal biopsy demon- infections and glomerulonephritis and, in particular, the causal strated a florid, diffuse, proliferative glomerulonephritis with role of staphylococcal antigens in the pathogenesis of such glomerular immune complex deposition. Management in- lesions is discussed. (J Am Soc Nephrol 8: 1633-1639, 1997) cluded hemodialysis, prolonged antibiotic therapy, and re- Coagulase-positive staphylococcus (Staphylococcus aureus) is mg/dl]) and in the immediate postoperative period. Over the the most common causative organism in acute osteomyelitis following days, the patient’s serum creatinine concentration (1). Along with coagulase-negative staphylococcal species, it increased progressively, and hemodialysis was instituted on has also been implicated in the pathogenesis of immune com- day 23 after CABG. There was no past or family history of plex (IC)-mediated diffuse proliferative glomerulonephritis renal disease and no known drug allergies. Prior medical (DPGN) in a variety of infections. These include bacterial history had included degenerative disc disease, stable abdom- endocarditis, ventriculoatrial shunt infections, pneumonia, and inal aortic aneurysm, stable benign prostatic hyperplasia, and visceral abscesses with or without septicemia (2-6). -

FHR5 Binds to Laminins, Uses Separate C3b and Surface-Binding Sites, and Activates Complement on Malondialdehyde-Acetaldehyde Surfaces
Published February 26, 2018, doi:10.4049/jimmunol.1701641 The Journal of Immunology FHR5 Binds to Laminins, Uses Separate C3b and Surface-Binding Sites, and Activates Complement on Malondialdehyde-Acetaldehyde Surfaces Ramona B. Rudnick,* Qian Chen,*,1 Emma Diletta Stea,*,2 Andrea Hartmann,* Nikolina Papac-Milicevic,†,‡ Fermin Person,x Michael Wiesener,{ Christoph J. Binder,†,‡ Thorsten Wiech,x Christine Skerka,* and Peter F. Zipfel*,‖ Factor H related-protein 5 (CFHR5) is a surface-acting complement activator and variations in the CFHR5 gene are linked to CFHR glomerulonephritis. In this study, we show that FHR5 binds to laminin-521, the major constituent of the glomerular base- ment membrane, and to mesangial laminin-211. Furthermore, we identify malondialdehyde-acetaldehyde (MAA) epitopes, which are exposed on the surface of human necrotic cells (Homo sapiens), as new FHR5 ligands. Using a set of novel deletion fragments, we show that FHR5 binds to laminin-521, MAA epitopes, heparin, and human necrotic cells (HUVECs) via the middle region [short consensus repeats (SCRs) 5-7]. In contrast, surface-bound FHR5 contacts C3b via the C-terminal region (SCRs8-9). Thus, FHR5 uses separate domains for C3b binding and cell surface interaction. MAA epitopes serve as a complement-activating surface by recruiting FHR5. The complement activator FHR5 and the complement inhibitor factor H both bind to oxidation- specific MAA epitopes and FHR5 competes with factor H for binding. The C3 glomerulopathy–associated FHR21–2-FHR5 hybrid protein is more potent in MAA epitope binding and activation compared with wild-type FHR5. The implications of these results for pathology of CFHR glomerulonephritis are discussed. -

Comprehensive Genomic Analysis of Rhabdomyosarcoma Reveals a Landscape of Alterations Affecting a Common Genetic Axis in Fusion-Positive and Fusion-Negative Tumors
Published OnlineFirst January 16, 2014; DOI: 10.1158/2159-8290.CD-13-0639 16-CD-13-0639_PAP.indd Page 1 16/01/14 3:10 PM user-f028 ~/Desktop ReseaRch aRticle Comprehensive Genomic Analysis of Rhabdomyosarcoma Reveals a Landscape of Alterations Affecting a Common Genetic Axis in Fusion-Positive and Fusion-Negative Tumors Jack. F Shern1, Li Chen1, Juliann Chmielecki3,4, Jun S. Wei1, Rajesh Patidar1,a Mar Rosenberg3, Lauren Ambrogio3, Daniel Auclair3, Jianjun Wang1, Young K. Song1, Catherine Tolman1,a Laur Hurd1, Hongling Liao1, Shile Zhang1, Dominik Bogen1, Andrew S. Brohl1, Sivasish Sindiri1, Daniel Catchpoole9, Thomas Badgett1, Gad Getz3, Jaume Mora10, James R. Anderson6, Stephen X. Skapek7, Frederic G. Barr2,w Matthe Meyerson3,4,5, Douglas S. Hawkins8, and Javed Khan1 a bstRact Despite gains in survival, outcomes for patients with metastatic or recurrent rhabdomyosarcoma remain dismal. In a collaboration between the National Cancer Institute, Children’s Oncology Group, and Broad Institute, we performed whole-genome, whole-exome, and transcriptome sequencing to characterize the landscape of somatic alterations in 147 tumor/ normal pairs. Two genotypes are evident in rhabdomyosarcoma tumors: those characterized by the PAX3 or PAX7 fusion and those that lack these fusions but harbor mutations in key signaling pathways. The overall burden of somatic mutations in rhabdomyosarcoma is relatively low, especially in tumors that harbor a PAX3/7 gene fusion. In addition to previously reported mutations in NRAS, KRAS, HRAS, FGFR4, PIK3CA, and CTNNB1, we found novel recurrent mutations in FBXW7 and BCOR, providing potential new avenues for therapeutic intervention. Furthermore, alteration of the receptor tyrosine kinase/RAS/PIK3CA axis affects 93% of cases, providing a framework for genomics-directed thera- pies that might improve outcomes for patients with rhabdomyosarcoma. -

Solid Tumour and Glomerulopathy
QJ Med 1996; 89:361-367 Solid tumour and glomerulopathy P. PAI, J.M. BONE, I. McDICKEN and CM. BELL From the Regional Renal Unit, Royal Liverpool University Hospital, Liverpool, UK Received 11 October 1995 and in revised form 31 January 1996 Downloaded from https://academic.oup.com/qjmed/article/89/5/361/1578010 by guest on 01 October 2021 Summary We retrospectively examined the prevalence of solid centic GN and one case of focal segmental GN. tumours in patients with glomerulonephritis (GN) Bronchogenic (6) and gastrointestinal carcinoma followed in our regional renal unit between 1977 (CA) (5) were the commonest tumours encountered. and 1994. We identified 17 cases of what was Other tumours included breast CA (1), renal cell thought to be solid-tumour-related glomerulo- CA (1), prostatic CA (1), an epithelial thymoma and nephritis. Tumours and GN were diagnosed together a leiomyosarcoma of the lung. All MGN and mesang- in six cases, and within a year of each other in ial proliferative GN cases developed nephrotic range another four. In addition, there were seven other proteinuria, whereas all patients with rapidly pro- cases with a weaker temporal relationship (median gressive crescentic GN presented with acute renal duration between GN and cancer diagnosis, two failure. Four cases had received immunosuppressive and a half years) but which nonetheless could be therapy prior to tumour diagnosis. We discuss the tumour-related. In total, there were seven membran- validity of each case as tumour-related glomerulo- ous GN, four mesangial proliferative GN, five cres- nephritis. Introduction Since the first clinicopathological study to present an University Hospital serves a population of 2 million association between cancer and nephrotic syndrome people in the Mersey region of the Northwest of (NS) was suggested by Lee et a\.? the subject of England. -

Glomerulonephritis
Adolesc Med 16 (2005) 67–85 Glomerulonephritis Keith K. Lau, MDa,b, Robert J. Wyatt, MD, MSa,b,* aDivision of Pediatric Nephrology, Department of Pediatrics, University of Tennessee Health Sciences Center, Room 301, WPT, 50 North Dunlap, Memphis, TN 38103, USA bChildren’s Foundation Research Center at the Le Bonheur Children’s Medical Center, Room 301, WPT, 50 North Dunlap, Memphis, TN 38103, USA Early diagnosis of glomerulonephritis (GN) in the adolescent is important in initiating appropriate treatment and controlling chronic glomerular injury that may eventually lead to end-stage renal disease (ESRD). The spectrum of GN in adolescents is more similar to that seen in young and middle-aged adults than to that observed in prepubertal children. In this article, the authors discuss the clinical features associated with GN and the diagnostic evaluation required to determine the specific type of GN. With the exception of hereditary nephritis (Alport’s disease), virtually all types of GN are immunologically mediated with glomerular deposition of immunoglobulins and complement proteins. The inflammatory events leading to GN may be triggered by a number of factors. Most commonly, immune complexes deposit in the glomeruli or are formed in situ with the antigen as a structural component of the glomerulus. The immune complexes then initiate the production of proinflammatory mediators, such as complement proteins and cytokines. Subsequently, the processes of sclerosis within the glomeruli and fibrosis in the tubulointerstitial cells lead to chronic or even irreversible renal injury [1]. Less commonly, these processes occur without involvement of immune complexes—so-called ‘‘pauci-immune GN.’’ * Corresponding author. -

The Impact of Complement Genes on the Risk of Late-Onset Alzheimer's
G C A T T A C G G C A T genes Article The Impact of Complement Genes on the Risk of Late-Onset Alzheimer’s Disease Sarah M. Carpanini 1,2,† , Janet C. Harwood 3,† , Emily Baker 1, Megan Torvell 1,2, The GERAD1 Consortium ‡, Rebecca Sims 3 , Julie Williams 1 and B. Paul Morgan 1,2,* 1 UK Dementia Research Institute at Cardiff University, School of Medicine, Cardiff, CF24 4HQ, UK; [email protected] (S.M.C.); [email protected] (E.B.); [email protected] (M.T.); [email protected] (J.W.) 2 Division of Infection and Immunity, School of Medicine, Systems Immunity Research Institute, Cardiff University, Cardiff, CF14 4XN, UK 3 Division of Psychological Medicine and Clinical Neurosciences, School of Medicine, Cardiff University, Cardiff, CF24 4HQ, UK; [email protected] (J.C.H.); [email protected] (R.S.) * Correspondence: [email protected] † These authors contributed equally to this work. ‡ Data used in the preparation of this article were obtained from the Genetic and Environmental Risk for Alzheimer’s disease (GERAD1) Consortium. As such, the investigators within the GERAD1 consortia contributed to the design and implementation of GERAD1 and/or provided data but did not participate in analysis or writing of this report. A full list of GERAD1 investigators and their affiliations is included in Supplementary File S1. Abstract: Late-onset Alzheimer’s disease (LOAD), the most common cause of dementia, and a huge global health challenge, is a neurodegenerative disease of uncertain aetiology. To deliver Citation: Carpanini, S.M.; Harwood, effective diagnostics and therapeutics, understanding the molecular basis of the disease is essential. -

Chromatin Accessibility Dynamics of Chlamydia-Infected Epithelial Cells
Hayward et al. Epigenetics & Chromatin (2020) 13:45 https://doi.org/10.1186/s13072-020-00368-2 Epigenetics & Chromatin RESEARCH Open Access Chromatin accessibility dynamics of Chlamydia-infected epithelial cells Regan J. Hayward1, James W. Marsh2, Michael S. Humphrys3, Wilhelmina M. Huston4 and Garry S. A. Myers1,4* Abstract Chlamydia are Gram-negative, obligate intracellular bacterial pathogens responsible for a broad spectrum of human and animal diseases. In humans, Chlamydia trachomatis is the most prevalent bacterial sexually transmitted infec- tion worldwide and is the causative agent of trachoma (infectious blindness) in disadvantaged populations. Over the course of its developmental cycle, Chlamydia extensively remodels its intracellular niche and parasitises the host cell for nutrients, with substantial resulting changes to the host cell transcriptome and proteome. However, little infor- mation is available on the impact of chlamydial infection on the host cell epigenome and global gene regulation. Regions of open eukaryotic chromatin correspond to nucleosome-depleted regions, which in turn are associated with regulatory functions and transcription factor binding. We applied formaldehyde-assisted isolation of regulatory elements enrichment followed by sequencing (FAIRE-Seq) to generate temporal chromatin maps of C. trachomatis- infected human epithelial cells in vitro over the chlamydial developmental cycle. We detected both conserved and distinct temporal changes to genome-wide chromatin accessibility associated with C. trachomatis infection. The observed diferentially accessible chromatin regions include temporally-enriched sets of transcription factors, which may help shape the host cell response to infection. These regions and motifs were linked to genomic features and genes associated with immune responses, re-direction of host cell nutrients, intracellular signalling, cell–cell adhesion, extracellular matrix, metabolism and apoptosis. -
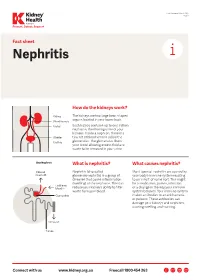
Nephritis Fact Sheet
Last Reviewed March 2017 Page 1 Prevent, Detect, Support. Fact sheet Nephritis How do the kidneys work? The kidneys are two large bean-shaped organs located in your lower back. Each kidney contains up to one million nephrons, the filtering units of your kidneys. Inside a nephron, there is a tiny set of blood vessels called the glomerulus. The glomerulus filters your blood allowing excess fluid and waste to be removed in your urine. What is nephritis? What causes nephritis? Nephritis (also called Most types of nephritis are caused by glomerulonephritis) is a group of your body’s immune system reacting diseases that cause inflammation to an ‘insult’ of some sort. This might (swelling) of the nephrons. This can be a medication, poison, infection reduce your kidney’s ability to filter or a change in the way your immune waste from your blood. system behaves. Your immune system makes antibodies to attack bacteria or poisons. These antibodies can damage your kidneys and nephrons, causing swelling and scarring. Connect with us www.kidney.org.au Freecall 1800 454 363 Kidney Health Australia Nephritis Last Reviewed March 2017 Prevent, Detect, Support. Page 2 What are the different types of nephritis? There are many different types of Different types of nephritis include: Nephrotic syndrome: Damage to the nephritis. It can vary from a mild, nephrons causes them to leak large Focal nephritis: Less than a half of non-damaging condition to a serious amounts of protein into your urine your nephrons have scarring, and problem causing kidney failure. Some but little blood. Losing this protein blood and a small amount of protein types of nephritis appear mild at means your body does not have are found in your urine.