Vemurafenib Inhibits Active PTK6 in PTEN-Null Prostate Tumor Cells
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-
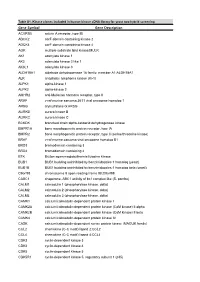

Gene Symbol Gene Description ACVR1B Activin a Receptor, Type IB
Table S1. Kinase clones included in human kinase cDNA library for yeast two-hybrid screening Gene Symbol Gene Description ACVR1B activin A receptor, type IB ADCK2 aarF domain containing kinase 2 ADCK4 aarF domain containing kinase 4 AGK multiple substrate lipid kinase;MULK AK1 adenylate kinase 1 AK3 adenylate kinase 3 like 1 AK3L1 adenylate kinase 3 ALDH18A1 aldehyde dehydrogenase 18 family, member A1;ALDH18A1 ALK anaplastic lymphoma kinase (Ki-1) ALPK1 alpha-kinase 1 ALPK2 alpha-kinase 2 AMHR2 anti-Mullerian hormone receptor, type II ARAF v-raf murine sarcoma 3611 viral oncogene homolog 1 ARSG arylsulfatase G;ARSG AURKB aurora kinase B AURKC aurora kinase C BCKDK branched chain alpha-ketoacid dehydrogenase kinase BMPR1A bone morphogenetic protein receptor, type IA BMPR2 bone morphogenetic protein receptor, type II (serine/threonine kinase) BRAF v-raf murine sarcoma viral oncogene homolog B1 BRD3 bromodomain containing 3 BRD4 bromodomain containing 4 BTK Bruton agammaglobulinemia tyrosine kinase BUB1 BUB1 budding uninhibited by benzimidazoles 1 homolog (yeast) BUB1B BUB1 budding uninhibited by benzimidazoles 1 homolog beta (yeast) C9orf98 chromosome 9 open reading frame 98;C9orf98 CABC1 chaperone, ABC1 activity of bc1 complex like (S. pombe) CALM1 calmodulin 1 (phosphorylase kinase, delta) CALM2 calmodulin 2 (phosphorylase kinase, delta) CALM3 calmodulin 3 (phosphorylase kinase, delta) CAMK1 calcium/calmodulin-dependent protein kinase I CAMK2A calcium/calmodulin-dependent protein kinase (CaM kinase) II alpha CAMK2B calcium/calmodulin-dependent -

Effects of Simultaneous Knockdown of HER2 and PTK6 on Malignancy and Tumor Progression in Human Breast Cancer Cells
Published OnlineFirst January 30, 2013; DOI: 10.1158/1541-7786.MCR-12-0378 Molecular Cancer Oncogenes and Tumor Suppressors Research Effects of Simultaneous Knockdown of HER2 and PTK6 on Malignancy and Tumor Progression in Human Breast Cancer Cells Natalie Ludyga1, Natasa Anastasov2, Michael Rosemann2, Jana Seiler1, Nadine Lohmann1, Herbert Braselmann3, Karin Mengele4, Manfred Schmitt4, Heinz Ho€fler1,5, and Michaela Aubele1 Abstract Breast cancer is the most common malignancy in women of the Western world. One prominent feature of breast cancer is the co- and overexpression of HER2 and protein tyrosine kinase 6 (PTK6). According to the current clinical cancer therapy guidelines, HER2-overexpressing tumors are routinely treated with trastuzumab, a humanized monoclonal antibody targeting HER2. Approximately, 30% of HER2-overexpressing breast tumors at least initially respond to the anti-HER2 therapy, but a subgroup of these tumors develops resistance shortly after the administration of trastuzumab. A PTK6-targeted therapy does not yet exist. Here, we show for the first time that the simultaneous knockdown in vitro, compared with the single knockdown of HER2 and PTK6, in particular in the trastuzumab-resistant JIMT-1 cells, leads to a significantly decreased phosphorylation of crucial signaling proteins: mitogen-activated protein kinase 1/3 (MAPK 1/3, ERK 1/2) and p38 MAPK, and (phosphatase and tensin homologue deleted on chromosome ten) PTEN that are involved in tumorigenesis. In addition, dual knockdown strongly reduced the migration and invasion of the JIMT-1 cells. Moreover, the downregulation of HER2 and PTK6 led to an induction of p27, and the dual knockdown significantly diminished cell proliferation in JIMT-1 and T47D cells. -
Profiling Data
Compound Name DiscoveRx Gene Symbol Entrez Gene Percent Compound Symbol Control Concentration (nM) JNK-IN-8 AAK1 AAK1 69 1000 JNK-IN-8 ABL1(E255K)-phosphorylated ABL1 100 1000 JNK-IN-8 ABL1(F317I)-nonphosphorylated ABL1 87 1000 JNK-IN-8 ABL1(F317I)-phosphorylated ABL1 100 1000 JNK-IN-8 ABL1(F317L)-nonphosphorylated ABL1 65 1000 JNK-IN-8 ABL1(F317L)-phosphorylated ABL1 61 1000 JNK-IN-8 ABL1(H396P)-nonphosphorylated ABL1 42 1000 JNK-IN-8 ABL1(H396P)-phosphorylated ABL1 60 1000 JNK-IN-8 ABL1(M351T)-phosphorylated ABL1 81 1000 JNK-IN-8 ABL1(Q252H)-nonphosphorylated ABL1 100 1000 JNK-IN-8 ABL1(Q252H)-phosphorylated ABL1 56 1000 JNK-IN-8 ABL1(T315I)-nonphosphorylated ABL1 100 1000 JNK-IN-8 ABL1(T315I)-phosphorylated ABL1 92 1000 JNK-IN-8 ABL1(Y253F)-phosphorylated ABL1 71 1000 JNK-IN-8 ABL1-nonphosphorylated ABL1 97 1000 JNK-IN-8 ABL1-phosphorylated ABL1 100 1000 JNK-IN-8 ABL2 ABL2 97 1000 JNK-IN-8 ACVR1 ACVR1 100 1000 JNK-IN-8 ACVR1B ACVR1B 88 1000 JNK-IN-8 ACVR2A ACVR2A 100 1000 JNK-IN-8 ACVR2B ACVR2B 100 1000 JNK-IN-8 ACVRL1 ACVRL1 96 1000 JNK-IN-8 ADCK3 CABC1 100 1000 JNK-IN-8 ADCK4 ADCK4 93 1000 JNK-IN-8 AKT1 AKT1 100 1000 JNK-IN-8 AKT2 AKT2 100 1000 JNK-IN-8 AKT3 AKT3 100 1000 JNK-IN-8 ALK ALK 85 1000 JNK-IN-8 AMPK-alpha1 PRKAA1 100 1000 JNK-IN-8 AMPK-alpha2 PRKAA2 84 1000 JNK-IN-8 ANKK1 ANKK1 75 1000 JNK-IN-8 ARK5 NUAK1 100 1000 JNK-IN-8 ASK1 MAP3K5 100 1000 JNK-IN-8 ASK2 MAP3K6 93 1000 JNK-IN-8 AURKA AURKA 100 1000 JNK-IN-8 AURKA AURKA 84 1000 JNK-IN-8 AURKB AURKB 83 1000 JNK-IN-8 AURKB AURKB 96 1000 JNK-IN-8 AURKC AURKC 95 1000 JNK-IN-8 -

Combined BRAF and MEK Inhibition with Vemurafenib and Cobimetinib for Patients with Advanced Melanoma
Review Melanoma Combined BRAF and MEK Inhibition with Vemurafenib and Cobimetinib for Patients with Advanced Melanoma Antonio M Grimaldi, Ester Simeone, Lucia Festino, Vito Vanella and Paolo A Ascierto Melanoma, Cancer Immunotherapy and Innovative Therapy Unit, Istituto Nazionale Tumori Fondazione “G. Pascale”, Napoli, Italy cquired resistance is the most common cause of BRAF inhibitor monotherapy treatment failure, with the majority of patients experiencing disease progression with a median progression-free survival of 6-8 months. As such, there has been considerable A focus on combined therapy with dual BRAF and MEK inhibition as a means to improve outcomes compared with monotherapy. In the COMBI-d and COMBI-v trials, combined dabrafenib and trametinib was associated with significant improvements in outcomes compared with dabrafenib or vemurafenib monotherapy, in patients with BRAF-mutant metastatic melanoma. The combination of vemurafenib and cobimetinib has also been investigated. In the phase III CoBRIM study in patients with unresectable stage III-IV BRAF-mutant melanoma, treatment with vemurafenib and cobimetinib resulted in significantly longer progression-free survival and overall survival (OS) compared with vemurafenib alone. One-year OS was 74.5% in the vemurafenib and cobimetinib group and 63.8% in the vemurafenib group, while 2-year OS rates were 48.3% and 38.0%, respectively. The combination was also well tolerated, with a lower incidence of cutaneous squamous-cell carcinoma and keratoacanthoma compared with monotherapy. Dual inhibition of both MEK and BRAF appears to provide a more potent and durable anti-tumour effect than BRAF monotherapy, helping to prevent acquired resistance as well as decreasing adverse events related to BRAF inhibitor-induced activation of the MAPK-pathway. -

Dangerous Liaisons: Flirtations Between Oncogenic BRAF and GRP78 in Drug-Resistant Melanomas
Dangerous liaisons: flirtations between oncogenic BRAF and GRP78 in drug-resistant melanomas Shirish Shenolikar J Clin Invest. 2014;124(3):973-976. https://doi.org/10.1172/JCI74609. Commentary BRAF mutations in aggressive melanomas result in kinase activation. BRAF inhibitors reduce BRAFV600E tumors, but rapid resistance follows. In this issue of the JCI, Ma and colleagues report that vemurafenib activates ER stress and autophagy in BRAFV600E melanoma cells, through sequestration of the ER chaperone GRP78 by the mutant BRAF and subsequent PERK activation. In preclinical studies, treating vemurafenib-resistant melanoma with a combination of vemurafenib and an autophagy inhibitor reduced tumor load. Further work is needed to establish clinical relevance of this resistance mechanism and demonstrate efficacy of autophagy and kinase inhibitor combinations in melanoma treatment. Find the latest version: https://jci.me/74609/pdf commentaries F2-2012–279017) and NEUROKINE net- from the brain maintains CNS immune tolerance. 17. Benner EJ, et al. Protective astrogenesis from the J Clin Invest. 2014;124(3):1228–1241. SVZ niche after injury is controlled by Notch mod- work (EU Framework 7 ITN project). 8. Sawamoto K, et al. New neurons follow the flow ulator Thbs4. Nature. 2013;497(7449):369–373. of cerebrospinal fluid in the adult brain. Science. 18. Sabelstrom H, et al. Resident neural stem cells Address correspondence to: Gianvito Mar- 2006;311(5761):629–632. restrict tissue damage and neuronal loss after spinal tino, Neuroimmunology Unit, Institute 9. Butti E, et al. Subventricular zone neural progeni- cord injury in mice. Science. 2013;342(6158):637–640. tors protect striatal neurons from glutamatergic 19. -

Darkening and Eruptive Nevi During Treatment with Erlotinib
CASE LETTER Darkening and Eruptive Nevi During Treatment With Erlotinib Stephen Hemperly, DO; Tanya Ermolovich, DO; Nektarios I. Lountzis, MD; Hina A. Sheikh, MD; Stephen M. Purcell, DO A 70-year-old man with NSCLCA presented with PRACTICE POINTS eruptive nevi and darkening of existing nevi 3 months after • Cutaneous side effects of erlotinib include acneform starting monotherapy with erlotinib. Physical examina- eruption, xerosis, paronychia, and pruritus. tion demonstrated the simultaneous appearance of scat- • Clinicians should monitor patients for darkening tered acneform papules and pustules; diffuse xerosis; and and/or eruptive nevi as well as melanoma during numerous dark copybrown to black nevi on the trunk, arms, treatment with erlotinib. and legs. Compared to prior clinical photographs taken in our office, darkening of existing medium brown nevi was noted, and new nevi developed in areas where no prior nevi had been visible (Figure 1). To the Editor: notThe patient’s medical history included 3 invasive mel- Erlotinib is a small-molecule selective tyrosine kinase anomas, all of which were diagnosed at least 7 years prior inhibitor that functions by blocking the intracellular por- to the initiation of erlotinib and were treated by surgical tion of the epidermal growth factor receptor (EGFR)Do1,2; excision alone. Prior treatment of NSCLCA consisted of a EGFR normally is expressed in the basal layer of the left lower lobectomy followed by docetaxel, carboplatin, epidermis, sweat glands, and hair follicles, and is over- pegfilgrastim, dexamethasone, and pemetrexed. A thor- expressed in some cancers.1,3 Normal activation of ough review of all of the patient’s medications revealed EGFR leads to signal transduction through the mitogen- no associations with changes in nevi. -

FOI Reference: FOI 414 - 2021
FOI Reference: FOI 414 - 2021 Title: Researching the Incidence and Treatment of Melanoma and Breast Cancer Date: February 2021 FOI Category: Pharmacy FOI Request: 1. How many patients are currently (in the past 3 months) undergoing treatment for melanoma, and how many of these are BRAF+? 2. In the past 3 months, how many melanoma patients (any stage) were treated with the following: • Cobimetinib • Dabrafenib • Dabrafenib AND Trametinib • Encorafenib AND Binimetinib • Ipilimumab • Ipilimumab AND Nivolumab • Nivolumab • Pembrolizumab • Trametinib • Vemurafenib • Vemurafenib AND Cobimetinib • Other active systemic anti-cancer therapy • Palliative care only 3. If possible, could you please provide the patients treated in the past 3 months with the following therapies for metastatic melanoma ONLY: • Ipilimumab • Ipilimumab AND Nivolumab • Nivolumab • Pembrolizumab • Any other therapies 4. In the past 3 months how many patients were treated with the following for breast cancer? • Abemaciclib + Anastrozole/Exemestane/Letrozole • Abemaciclib + Fulvestrant • Alpelisib + Fulvestrant • Atezolizumab • Bevacizumab [Type text] • Eribulin • Everolimus + Exemestane • Fulvestrant as a single agent • Gemcitabine + Paclitaxel • Lapatinib • Neratinib • Olaparib • Palbociclib + Anastrozole/Exemestane/Letrozole • Palbociclib + Fulvestrant • Pertuzumab + Trastuzumab + Docetaxel • Ribociclib + Anastrozole/Exemestane/Letrozole • Ribociclib + Fulvestrant • Talazoparib • Transtuzumab + Paclitaxel • Transtuzumab as a single agent • Trastuzumab emtansine • Any other -

Cotellic, INN-Cobimetinib
ANNEX I SUMMARY OF PRODUCT CHARACTERISTICS 1 1. NAME OF THE MEDICINAL PRODUCT Cotellic 20 mg film-coated tablets 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each film-coated tablet contains cobimetinib hemifumarate equivalent to 20 mg cobimetinib. Excipient with known effect Each film-coated tablet contains 36 mg lactose monohydrate. For the full list of excipients, see section 6.1. 3. PHARMACEUTICAL FORM Film-coated tablet. White, round film-coated tablets of approximately 6.6 mm diameter, with “COB” debossed on one side. 4. CLINICAL PARTICULARS 4.1 Therapeutic indications Cotellic is indicated for use in combination with vemurafenib for the treatment of adult patients with unresectable or metastatic melanoma with a BRAF V600 mutation (see sections 4.4 and 5.1). 4.2 Posology and method of administration Treatment with Cotellic in combination with vemurafenib should only be initiated and supervised by a qualified physician experienced in the use of anticancer medicinal products. Before starting this treatment, patients must have BRAF V600 mutation-positive melanoma tumour status confirmed by a validated test (see sections 4.4 and 5.1). Posology The recommended dose of Cotellic is 60 mg (3 tablets of 20 mg) once daily. Cotellic is taken on a 28 day cycle. Each dose consists of three 20 mg tablets (60 mg) and should be taken once daily for 21 consecutive days (Days 1 to 21-treatment period); followed by a 7-day break (Days 22 to 28-treatment break). Each subsequent Cotellic treatment cycle should start after the 7-day treatment break has elapsed. For information on the posology of vemurafenib, please refer to its SmPC. -

Supplementary Table 1. in Vitro Side Effect Profiling Study for LDN/OSU-0212320. Neurotransmitter Related Steroids
Supplementary Table 1. In vitro side effect profiling study for LDN/OSU-0212320. Percent Inhibition Receptor 10 µM Neurotransmitter Related Adenosine, Non-selective 7.29% Adrenergic, Alpha 1, Non-selective 24.98% Adrenergic, Alpha 2, Non-selective 27.18% Adrenergic, Beta, Non-selective -20.94% Dopamine Transporter 8.69% Dopamine, D1 (h) 8.48% Dopamine, D2s (h) 4.06% GABA A, Agonist Site -16.15% GABA A, BDZ, alpha 1 site 12.73% GABA-B 13.60% Glutamate, AMPA Site (Ionotropic) 12.06% Glutamate, Kainate Site (Ionotropic) -1.03% Glutamate, NMDA Agonist Site (Ionotropic) 0.12% Glutamate, NMDA, Glycine (Stry-insens Site) 9.84% (Ionotropic) Glycine, Strychnine-sensitive 0.99% Histamine, H1 -5.54% Histamine, H2 16.54% Histamine, H3 4.80% Melatonin, Non-selective -5.54% Muscarinic, M1 (hr) -1.88% Muscarinic, M2 (h) 0.82% Muscarinic, Non-selective, Central 29.04% Muscarinic, Non-selective, Peripheral 0.29% Nicotinic, Neuronal (-BnTx insensitive) 7.85% Norepinephrine Transporter 2.87% Opioid, Non-selective -0.09% Opioid, Orphanin, ORL1 (h) 11.55% Serotonin Transporter -3.02% Serotonin, Non-selective 26.33% Sigma, Non-Selective 10.19% Steroids Estrogen 11.16% 1 Percent Inhibition Receptor 10 µM Testosterone (cytosolic) (h) 12.50% Ion Channels Calcium Channel, Type L (Dihydropyridine Site) 43.18% Calcium Channel, Type N 4.15% Potassium Channel, ATP-Sensitive -4.05% Potassium Channel, Ca2+ Act., VI 17.80% Potassium Channel, I(Kr) (hERG) (h) -6.44% Sodium, Site 2 -0.39% Second Messengers Nitric Oxide, NOS (Neuronal-Binding) -17.09% Prostaglandins Leukotriene, -

Cobimetinib/Vemurafenib Combination Therapy for Melanoma: a Nursing Tool from the Melanoma Nursing Initiative (MNI)
Cobimetinib/Vemurafenib Combination Therapy for Melanoma: A Nursing Tool From The Melanoma Nursing Initiative (MNI) Cobimetinib (Cotellic®)/vemurafenib (Zelboraf®) combination therapy is indicated for the treatment of patients with unresectable or metastatic melanoma with BRAF V600E or V600K mutations. Cobimetinib is a MEK1 and MEK2 inhibitor, and vemurafenib is an inhibitor of some mutated forms of BRAF kinase, including BRAF V600E. About half of patients with melanoma have a mutated form of the BRAF protein in their tumors. Combination MEK/ BRAF inhibitor therapy is associated with superior tumor response and improved patient survival compared with single-agent BRAF inhibitor therapy. Using the combination also decreases the high rates of secondary cutaneous malignancies associated with single-agent BRAF inhibitory therapy. This document is part of an overall nursing toolkit intended to assist nurses in optimizing care of melanoma patients receiving newer anti-melanoma therapies. © 2017 The Melanoma Nursing Initiative. All rights reserved www.themelanomanurse.org Inspired By Patients . Empowered By Knowledge . Impacting Melanoma DRUG-DOSING/ADMINISTRATION • For advanced melanoma, both cobimetinib and vemurafenib are orally administered drugs. Cobimetinib is administered as 60 mg (three 20-mg tablets) once daily for 3 weeks, followed by a 1-week break, and vemurafenib as 960 mg (four 240-mg tablets) twice daily, for a total daily dosage of 1920 mg, each according to the regimens outlined below. The cobimetinib dose can be taken at the same time as one of the vemurafenib doses. The schedule repeats until disease progression or unacceptable toxicity occurs. • If the patient misses a dose of cobimetinib or vemurafenib, adjust as follows: » Cobimetinib: If ≤4 hours from scheduled dosing time, take the dose. -

New Century Health Policy Changes April 2021
Policy # Drug(s) Type of Change Brief Description of Policy Change new Pepaxto (melphalan flufenamide) n/a n/a new Fotivda (tivozanib) n/a n/a new Cosela (trilaciclib) n/a n/a Add inclusion criteria: NSCLC UM ONC_1089 Libtayo (cemiplimab‐rwlc) Negative change 2.Libtayo (cemiplimab) may be used as montherapy in members with locally advanced, recurrent/metastatic NSCLC, with PD‐L1 ≥ 50%, negative for actionable molecular markers (ALK, EGFR, or ROS‐1) Add inclusion criteria: a.As a part of primary/de�ni�ve/cura�ve‐intent concurrent chemo radia�on (Erbitux + Radia�on) as a single agent for members with a UM ONC_1133 Erbitux (Cetuximab) Positive change contraindication and/or intolerance to cisplatin use OR B.Head and Neck Cancers ‐ For recurrent/metasta�c disease as a single agent, or in combination with chemotherapy. Add inclusion criteria: UM ONC_1133 Erbitux (Cetuximab) Negative change NOTE: Erbitux (cetuximab) + Braftovi (encorafenib) is NCH preferred L1 pathway for second‐line or subsequent therapy in the metastatic setting, for BRAFV600E positive colorectal cancer.. Add inclusion criteria: B.HER‐2 Posi�ve Breast Cancer i.Note #1: For adjuvant (post‐opera�ve) use in members who did not receive neoadjuvant therapy/received neoadjuvant therapy and did not have any residual disease in the breast and/or axillary lymph nodes, Perjeta (pertuzumab) use is restricted to node positive stage II and III disease only. ii.Note #2: Perjeta (pertuzumab) use in the neoadjuvant (pre‐opera�ve) se�ng requires radiographic (e.g., breast MRI, CT) and/or pathologic confirmation of ipsilateral (same side) axillary nodal involvement. -

Trastuzumab Emtansine (T-DM1) and Stereotactic Radiation in the Management of HER2+ Breast Cancer Brain Metastases Matthew N
Mills et al. BMC Cancer (2021) 21:223 https://doi.org/10.1186/s12885-021-07971-w RESEARCH ARTICLE Open Access Trastuzumab Emtansine (T-DM1) and stereotactic radiation in the management of HER2+ breast cancer brain metastases Matthew N. Mills1* , Chelsea Walker2, Chetna Thawani2, Afrin Naz2, Nicholas B. Figura1, Sergiy Kushchayev3, Arnold Etame4, Hsiang-Hsuan Michael Yu1, Timothy J. Robinson1, James Liu4, Michael A. Vogelbaum4, Peter A. Forsyth4, Brian J. Czerniecki5, Hatem H. Soliman5, Hyo S. Han5 and Kamran A. Ahmed1 Abstract Background: Due to recent concerns about the toxicity of trastuzumab emtansine (T-DM1) with stereotactic radiation, we assessed our institutional outcomes treating HER2-positive breast cancer brain metastases (BCBM) with T-DM1 and stereotactic radiation. Methods: This is a single institution series of 16 patients with HER2-positive breast cancer who underwent 18 stereotactic sessions to 40 BCBM from 2013 to 2019 with T-DM1 delivered within 6 months. The Kaplan-Meier method was used to calculate overall survival (OS), local control (LC), distant intracranial control (DIC), and systemic progression-free survival (sPFS) from the date of SRS. A neuro-radiologist independently reviewed follow-up imaging. Results: One patient had invasive lobular carcinoma, and 15 patients had invasive ductal carcinoma. All cases were HER2-positive, while 10 were hormone receptor (HR) positive. Twenty-four lesions were treated with stereotactic radiosurgery (SRS) to a median dose of 21 Gy (14–24 Gy). Sixteen lesions were treated with fractionated stereotactic radiation (FSRT) with a median dose of 25 Gy (20-30Gy) delivered in 3 to 5 fractions. Stereotactic radiation was delivered concurrently with T-DM1 in 19 lesions (48%).