SHOULDER: Impingement • Rotator Cuff Tendonitis • Subacromial Bursitis
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Iliopsoas Tendonitis/Bursitis Exercises
ILIOPSOAS TENDONITIS / BURSITIS What is the Iliopsoas and Bursa? The iliopsoas is a muscle that runs from your lower back through the pelvis to attach to a small bump (the lesser trochanter) on the top portion of the thighbone near your groin. This muscle has the important job of helping to bend the hip—it helps you to lift your leg when going up and down stairs or to start getting out of a car. A fluid-filled sac (bursa) helps to protect and allow the tendon to glide during these movements. The iliopsoas tendon can become inflamed or overworked during repetitive activities. The tendon can also become irritated after hip replacement surgery. Signs and Symptoms Iliopsoas issues may feel like “a pulled groin muscle”. The main symptom is usually a catch during certain movements such as when trying to put on socks or rising from a seated position. You may find yourself leading with your other leg when going up the stairs to avoid lifting the painful leg. The pain may extend from the groin to the inside of the thigh area. Snapping or clicking within the front of the hip can also be experienced. Do not worry this is not your hip trying to pop out of socket but it is usually the iliopsoas tendon rubbing over the hip joint or pelvis. Treatment Conservative treatment in the form of stretching and strengthening usually helps with the majority of patients with iliopsoas bursitis. This issue is the result of soft tissue inflammation, therefore rest, ice, anti- inflammatory medications, physical therapy exercises, and/or injections are effective treatment options. -

Pes Anserine Bursitis
BRIGHAM AND WOMEN’S HOSPITAL Department of Rehabilitation Services Physical Therapy Standard of Care: Pes Anserine Bursitis ICD 9 Codes: 726.61 Case Type / Diagnosis: The pes anserine bursa lies behind the medial hamstring, which is composed of the tendons of the sartorius, gracilis and semitendinosus (SGT) muscles. Because these 3 tendons splay out on the anterior aspect of the tibia and give the appearance of the foot of a goose, pes anserine bursitis is also known as goosefoot bursitis.1 These muscles provide for medial stabilization of the knee by acting as a restraint to excessive valgus opening. They also provide a counter-rotary torque function to the knee joint. The pes anserine has an eccentric role during the screw-home mechanism that dampens the effect of excessively forceful lateral rotation that may accompany terminal knee extension.2 Pes anserine bursitis presents as pain, tenderness and swelling over the anteromedial aspect of the knee, 4 to 5 cm below the joint line.3 Pain increases with knee flexion, exercise and/or stair climbing. Inflammation of this bursa is common in overweight, middle-aged women, and may be associated with osteoarthritis of the knee. It also occurs in athletes engaged in activities such as running, basketball, and racquet sports.3 Other risk factors include: 1 • Incorrect training techniques, or changes in terrain and/or distanced run • Lack of flexibility in hamstring muscles • Lack of knee extension • Patellar malalignment Indications for Treatment: • Knee Pain • Knee edema • Decreased active and /or passive ROM of lower extremities • Biomechanical dysfunction lower extremities • Muscle imbalances • Impaired muscle performance (focal weakness or general conditioning) • Impaired function Contraindications: • Patients with active signs/symptoms of infection (fever, chills, prolonged and obvious redness or swelling at hip joint). -

Rotator Cuff and Subacromial Impingement Syndrome: Anatomy, Etiology, Screening, and Treatment
Rotator Cuff and Subacromial Impingement Syndrome: Anatomy, Etiology, Screening, and Treatment The glenohumeral joint is the most mobile joint in the human body, but this same characteristic also makes it the least stable joint.1-3 The rotator cuff is a group of muscles that are important in supporting the glenohumeral joint, essential in almost every type of shoulder movement.4 These muscles maintain dynamic joint stability which not only avoids mechanical obstruction but also increases the functional range of motion at the joint.1,2 However, dysfunction of these stabilizers often leads to a complex pattern of degeneration, rotator cuff tear arthropathy that often involves subacromial impingement.2,22 Rotator cuff tear arthropathy is strikingly prevalent and is the most common cause of shoulder pain and dysfunction.3,4 It appears to be age-dependent, affecting 9.7% of patients aged 20 years and younger and increasing to 62% of patients of 80 years and older ( P < .001); odds ratio, 15; 95% CI, 9.6-24; P < .001.4 Etiology for rotator cuff pathology varies but rotator cuff tears and tendinopathy are most common in athletes and the elderly.12 It can be the result of a traumatic event or activity-based deterioration such as from excessive use of arms overhead, but some argue that deterioration of these stabilizers is part of the natural aging process given the trend of increased deterioration even in individuals who do not regularly perform overhead activities.2,4 The factors affecting the rotator cuff and subsequent treatment are wide-ranging. The major objectives of this exposition are to describe rotator cuff anatomy, biomechanics, and subacromial impingement; expound upon diagnosis and assessment; and discuss surgical and conservative interventions. -

Gluteal Tendinopathy
Gluteal Tendinopathy What is a Gluteal Tendinopathy? In lying Up until recently hip bursitis was diagnosed as the main Either on your bad hip or with bad cause of lateral hip pain but recent studies suggest that an hip hanging across body like so irritation of the gluteus muscle tendon is the likeliest cause. The tendon attaches onto a bony prominence (greater trochanter) and it is here that the tendon is subject to All these positions lead to increase friction of the tendon, compressive forces leading to irritation. can cause pain and slow the healing process. This can result in pain over the lateral hip which can refer down the outside For sleeping you might like to try these positions: of the thigh and into the knee. How common is it? Gluteal tendinopathy is relatively common affecting 10-25% of the population. It is 3 times more prevalent in women than men and is most common in women between the ages of 40 and 60. One of the reasons for this is women It is also important to modify your activity. Avoid or reduce tend to have a greater angle at their hip joint increasing things that flare up your pain, this could be climbing stairs compressive forces on the tendon. or hills or those longer walks/runs. Signs and Symptoms Exercise Therapy • Pain on the outside of your hip, can refer down outside of the thigh to the knee This is best administered by a Physiotherapist to suit the • Worse when going up and/or down stairs individual but below is a rough guide to exercises which • Worse lying on affected side (and sometimes on the can help a gluteal tendinopathy. -

The Anatomy of the Deep Infrapatellar Bursa of the Knee Robert F
0363-5465/98/2626-0129$02.00/0 THE AMERICAN JOURNAL OF SPORTS MEDICINE, Vol. 26, No. 1 © 1998 American Orthopaedic Society for Sports Medicine The Anatomy of the Deep Infrapatellar Bursa of the Knee Robert F. LaPrade,* MD Department of Orthopaedic Surgery, University of Minnesota, Minneapolis, Minnesota ABSTRACT knee joint, and to define a consistent surgical approach to the deep infrapatellar bursa. Disorders of the deep infrapatellar bursa are important to include in the differential diagnosis of anterior knee pain. Knowledge regarding its anatomic location can MATERIALS AND METHODS aid the clinician in establishing a proper diagnosis. Fifty cadaveric knees were dissected, and the deep infrapa- Thorough dissections of the anterior aspect of the knee of tellar bursa had a consistent anatomic location in all 50 nonpaired cadaveric knees were performed. There were specimens. The deep infrapatellar bursa was located 27 male and 23 female cadaveric knees with 25 right and directly posterior to the distal 38% of the patellar ten- 25 left knees. The average age of the specimens was 71.8 don, just proximal to its insertion on the tibial tubercle. years (range, 42 to 93). After the skin and subcutaneous There was no communication to the knee joint. Its tissues of the anterior aspect of the knee were carefully average width at the most proximal margin of the tibial dissected away, an approach to the deep infrapatellar tubercle was slightly wider than the average distal bursa of the knee was made through medial and lateral width of the patellar tendon. It was found to be partially arthrotomy incisions along the patella, followed by compartmentalized, with a fat pad apron extending transection of the quadriceps tendon from the patella. -

Spontaneous Septic Subacromial Bursitis Due to Streptococcus
A Case Report: Spontaneous Septic Subacromial Bursitis Due to Streptococcus anginosus Emily McGhee, MD, Mohammad Agha, MD, MHA University of Missouri – Columbia Department of Physical Medicine and Rehabilitation Introduction: Discussion: • 67 year old male presented to clinic with 1-2 weeks • Septic subacromial bursitis is rare due to the nature of right shoulder pain, 8/10 achy, no radiation, of the anatomic location of the deep bursa¹ worse with flexion and extension, improved with ice • It is usually seen in immunocompromised patients, • Gastroenteritis 3 days prior with fever of 102°F and after corticosteroid injections, or if there is a vomiting hematogenous spread from another source² • History is significant for HTN, T2DM, OA, bilateral • Of the cases reported in literature, 80% are caused total knee replacements, previous tobacco user, by Staphylococcus aureus² allergies to penicillin and sulfa • Streptococcus anginosus is part of the normal flora of the oral cavity and gastrointestinal tract • It can spread hematogenously and is known for its Clinical Course: ability to cause abscesses • Physical Exam: Vital signs within normal limits. • Streptococcus anginosus has been seen in pubic Right shoulder active abduction 30°, passive symphysis and sternoclavicular joint infections3,4 abduction 80°, 4/5 external and internal rotation, • There have been no reported cases of remainder of exam deferred due to pain. Normal left Figure 1: T2 weighted MRI Right Shoulder - large Streptococcus anginosus causing septic shoulder exam subacromial bursitis fluid collection in subacromial/subdeltoid bursa, • Diagnosed with rotator cuff tear and started physical appears ruptured with fluid extending laterally therapy Conclusion: • Initial x-ray negative, lab work unremarkable along humeral shaft, synovial thickening and • Pain continued, prompting a clinic visit the next day enhancement. -

Calcific Tendinitis of the Shoulder
CME Further Education Certified Advanced Training Orthopäde 2011 [jvn]:[afp]-[alp] P. Diehl1, 2 L. Gerdesmeyer3, 4 H. Gollwitzer3 W. Sauer2 T. Tischer1 DOI 10.1007/s00132-011-1817-3 1 Orthopaedic Clinic and Polyclinic, Rostock University 2 East Munich Orthopaedic Centre, Grafing 3 Orthopaedics and Sports Orthopaedics Clinic, Klinikum rechts der Isar, Online publication date: [OnlineDate] Munich Technical University Springer-Verlag 2011 4 Oncological and Rheumatological Orthopaedics Section, Schleswig-Holstein University Clinic, Kiel Campus Editors: R. Gradinger, Munich R. Graf, Stolzalpe J. Grifka, Bad Abbach A. Meurer, Friedrichsheim Calcific tendinitis of the shoulder Abstract Calcific tendinitis of the shoulder is a process involving crystal calcium deposition in the rotator cuff tendons, which mainly affects patients between 30 and 50 years of age. The etiology is still a matter of dispute. The diagnosis is made by history and physical examination with specific attention to radiologic and sonographic evidence of calcific deposits. Patients usually describe specific radiation of the pain to the lateral proximal forearm, with tenderness even at rest and during the night. Nonoperative management including rest, nonsteroidal anti-inflammatory drugs, subacromial corticosteroid injections, and shock wave therapy is still the treatment of choice. Nonoperative treatment is successful in up to 90 % of patients. When nonsurgical measures fail, surgical removal of the calcific deposit may be indicated. Arthroscopic treatment provides excellent results in more than 90 % of patients. The recovery process is very time consuming and may take up to several months in some cases. Keywords Rotator cuff Tendons Tendinitis Calcific tendinitis Calcification, pathologic English Translation oft he original article in German „Die Kalkschulter – Tendinosis calcarea“ in: Der Orthopäde 8 2011 733 This article explains the causes and development of calcific tendinitis of the shoulder, with special focus on the diagnosis of the disorder and the existing therapy options. -

Case Report Septic Infrapatellar Bursitis in an Immunocompromised Female
Hindawi Case Reports in Orthopedics Volume 2018, Article ID 9086201, 3 pages https://doi.org/10.1155/2018/9086201 Case Report Septic Infrapatellar Bursitis in an Immunocompromised Female Kenneth Herring , Seth Mathern, and Morteza Khodaee 1Department of Family Medicine, University of Colorado School of Medicine, 3055 Roslyn Street, Denver, CO 80238, USA Correspondence should be addressed to Kenneth Herring; [email protected] Received 8 April 2018; Revised 19 April 2018; Accepted 20 April 2018; Published 6 June 2018 Academic Editor: John Nyland Copyright © 2018 Kenneth Herring et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. Bursitis is a relatively common occurrence that may be caused by traumatic, inflammatory, or infectious processes. Septic bursitis most commonly affects the olecranon and prepatellar bursae. Staphylococcus aureus accounts for 80% of all septic bursitis, and most cases affect men and are associated with preceding trauma. We present a case of an 86-year-old female with an atypical septic bursitis involving the infrapatellar bursa. Not only are there very few reported cases of septic infrapatellar bursitis, but also this patient’s case is particularly unusual in that she is a female with no preceding trauma who had Pseudomonas aeruginosa on aspirate. The case also highlights the diagnostic workup of septic bursitis through imaging modalities and aspiration. This patient had full resolution of her septic bursitis with appropriate IV antibiotics. 1. Introduction and relative superficial location, the olecranon and prepa- tellar bursae are the most common sites of septic bursitis The human body contains upwards of 150 bursae, many [3, 4]. -

Plantar Fasciitis Thomas Trojian, MD, MMB, and Alicia K
Plantar Fasciitis Thomas Trojian, MD, MMB, and Alicia K. Tucker, MD, Drexel University College of Medicine, Philadelphia, Pennsylvania Plantar fasciitis is a common problem that one in 10 people will experience in their lifetime. Plantar fasciopathy is an appro- priate descriptor because the condition is not inflammatory. Risk factors include limited ankle dorsiflexion, increased body mass index, and standing for prolonged periods of time. Plantar fasciitis is common in runners but can also affect sedentary people. With proper treatment, 80% of patients with plantar fasciitis improve within 12 months. Plantar fasciitis is predominantly a clinical diagnosis. Symp- toms are stabbing, nonradiating pain first thing in the morning in the proximal medioplantar surface of the foot; the pain becomes worse at the end of the day. Physical examination findings are often limited to tenderness to palpation of the proximal plantar fascial insertion at the anteromedial calcaneus. Ultrasonogra- phy is a reasonable and inexpensive diagnostic tool for patients with pain that persists beyond three months despite treatment. Treatment should start with stretching of the plantar fascia, ice massage, and nonsteroidal anti-inflamma- tory drugs. Many standard treatments such as night splints and orthoses have not shown benefit over placebo. Recalcitrant plantar fasciitis can be treated with injections, extracorporeal shock wave therapy, or surgical procedures, although evidence is lacking. Endoscopic fasciotomy may be required in patients who continue to have pain that limits activity and function despite exhausting nonoperative treatment options. (Am Fam Physician. 2019; 99(12):744-750. Copyright © 2019 American Academy of Family Physicians.) Illustration by Todd Buck Plantar fasciitis (also called plantar fasciopathy, reflect- than 27 kg per m2 (odds ratio = 3.7), and spending most ing the absence of inflammation) is a common problem of the workday on one’s feet 4,5 (Table 1 6). -

Bursitis of the Knee
Bursitis of the knee What is bursitis? The diagram below shows the position of the Bursitis means inflammation within a bursa. A prepatellar and infrapatellar bursa in the knee. bursa is a small sac of fluid with a thin lining. There are a number of bursae in the body. Bursae are normally found around joints and in places where ligaments and tendons pass over bones and are there to stop the ligaments and bone rubbing together. What is prepatellar bursitis? Prepatellar bursitis is a common bursitis in the knee and can also be known as ‘housemaid’s knee’. There are four bursae located around the knee joint. They are all prone to inflammation. What causes prepatellar bursitis? There are a number of different things that can cause prepatellar bursitis, such as: • A sudden, one-off injury to the knee such as a fall or direct blow on to the knee during sport. People receiving steroid treatment or those on chemotherapy treatment for cancer are also at • Recurrent minor injury to the knee such as an increased risk of developing bursitis. spending long periods of time kneeling down, i.e. at work or whilst cleaning. Prepatellar bursitis is more common in tradesmen who spend long periods of time Infection: the fluid in the prepatellar bursa sac kneeling. For example, carpet fitters, concrete can become infected and cause bursitis. This is finishers and roofers. particularly common in children with prepatellar bursitis and usually follows a cut, scratch or injury to the skin on the surface of the knee. This What are the symptoms of injury allows bacteria (germs) to spread infection prepatellar bursitis? into the bursa. -
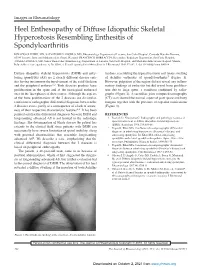
Heel Enthesopathy of Diffuse Idiopathic Skeletal Hyperostosis
Images in Rheumatology Heel Enthesopathy of Diffuse Idiopathic Skeletal Hyperostosis Resembling Enthesitis of Spondyloarthritis IGNAZIO OLIVIERI, MD, SALVATORE D’ANGELO, MD, Rheumatology Department of Lucania, San Carlo Hospital, Contrada Macchia Romana, 85100 Potenza, Italy; and Madonna delle Grazie Hospital; FRANCESCO BORRACCIA, Researcher, Radiology Department, San Carlo Hospital; ANGELA PADULA, MD, Senior Researcher, Rheumatology Department of Lucania, San Carlo Hospital, and Madonna delle Grazie Hospital, Matera, Italy. Address correspondence to Dr. Olivieri; E-mail: [email protected]. J Rheumatol 2010;37:192–3; doi.10.3899/jrheum.090514 Diffuse idiopathic skeletal hyperostosis (DISH) and anky- tendons, resembling the typical fusiform soft tissue swelling losing spondylitis (AS) are 2 clearly different disease enti- of Achilles enthesitis of spondyloarthritis5 (Figure 1). ties having in common the involvement of the axial skeleton However, palpation of the region did not reveal any inflam- and the peripheral entheses1,2. Both diseases produce bone matory findings of enthesitis but did reveal bone prolifera- proliferation in the spine and at the extraspinal entheseal tion due to large spurs, a condition confirmed by radio- sites in the later phases of their course. Although the aspects graphs (Figure 2). A sacroiliac joint computed tomography of the bone proliferations of the 2 diseases are dissimilar, (CT) scan showed the normal aspect of joint space and bony confusion of radiographic differential diagnosis between the margins together with the presence of capsular ossifications 2 diseases exists, partly as a consequence of a lack of aware- (Figure 3). ness of their respective characteristic features2,3. It has been pointed out that the differential diagnosis between DISH and REFERENCES longstanding advanced AS is not limited to the radiologic 1. -

Trochanteric Bursitis in Rheumatoid Arthritis
Images in Rheumatology Trochanteric Bursitis in Rheumatoid Arthritis HIROSHI TANAKA, MD; KENJI KIDO, MD; ATSUHIKO WAKISAKA, MD; TAKATOMO MINE, MD; SHINYA KAWAI, MD, Department of Orthopedic Surgery, Yamaguchi University School of Medicine, 1-1-1 Minamikogushi, Ube, Yamaguchi 755-8505, Japan. Address reprint requests to Dr. Tanaka. We describe a case of giant trochanteric bursitis with bony popliteal cyst, which is frequently found in association with erosion in the great trochanter. A 65-year-old woman with RA of the knee, and that surgical excision of the underlying longstanding rheumatoid arthritis (RA) reported a recurrent bursa is essential to avoid recurrence of the cyst. As in this cyst in the buttock. Her initial pelvic radiograph revealed a case, communication between the trochanteric bursa and the slight erosive change in the left great trochanter (Figure 1). subcutaneous cyst was revealed by Gd enhanced MRI but A contrast medium was injected into the cyst, but it did not not by contrast radiography of the cyst. Gd enhanced MRI pass into the trochanteric bursa or the hip joint (Figure 2). was helpful not only for detecting the extent of the subcuta- Magnetic resonance imaging (MRI) revealed a large neous cyst, but for elucidating the underlying trochanteric trochanteric bursa and a thin walled subcutaneous cyst bursitis communication with the cyst. presumed to arise from the bursa. Following gadolinium (Gd) administration, both the trochanteric bursa and the wall REFERENCES of the subcutaneous cyst with nonenhancing central compo- 1. Palmer DG. Synovial cysts in rheumatoid disease. Ann Intern Med 1969;70:61-8. nent were enhanced, and both communicated with each 2.