Common Extensor Tendon (Elbow) Repair Protocol
Total Page:16
File Type:pdf, Size:1020Kb
Load more
Recommended publications
-

Musculoskeletal Ultrasound Technical Guidelines II. Elbow
European Society of MusculoSkeletal Radiology Musculoskeletal Ultrasound Technical Guidelines II. Elbow Ian Beggs, UK Stefano Bianchi, Switzerland Angel Bueno, Spain Michel Cohen, France Michel Court-Payen, Denmark Andrew Grainger, UK Franz Kainberger, Austria Andrea Klauser, Austria Carlo Martinoli, Italy Eugene McNally, UK Philip J. O’Connor, UK Philippe Peetrons, Belgium Monique Reijnierse, The Netherlands Philipp Remplik, Germany Enzo Silvestri, Italy Elbow Note The systematic scanning technique described below is only theoretical, considering the fact that the examination of the elbow is, for the most, focused to one quadrant only of the joint based on clinical findings. 1 ANTERIOR ELBOW For examination of the anterior elbow, the patient is seated facing the examiner with the elbow in an extension position over the table. The patient is asked to extend the elbow and supinate the fore- arm. A slight bending of the patient’s body toward the examined side makes full supination and as- sessment of the anterior compartment easier. Full elbow extension can be obtained by placing a pillow under the joint. Transverse US images are first obtained by sweeping the probe from approximately 5cm above to 5cm below the trochlea-ulna joint, a Pr perpendicular to the humeral shaft. Cranial US images of the supracondylar region reveal the superficial biceps and the deep brachialis mu- Br scles. Alongside and medial to these muscles, follow the brachial artery and the median nerve: * the nerve lies medially to the artery. * Legend: a, brachial artery; arrow, median nerve; arrowheads, distal biceps tendon; asterisks, articular cartilage of the Humerus humeral trochlea; Br, brachialis muscle; Pr, pronator muscle 2 distal biceps tendon: technique The distal biceps tendon is examined while keeping the patient’s forearm in maximal supination to bring the tendon insertion on the radial tuberosity into view. -

Evaluation and Management of Elbow Tendinopathy
vol. XX • no. X SPORTS HEALTH Evaluation and Management of Elbow Tendinopathy Samuel A. Taylor*† and Jo Hannafin† Context: Elbow tendinopathy is a common cause of pain and disability among patients presenting to orthopaedic sur- geons, primary care physicians, physical therapists, and athletic trainers. Prompt and accurate diagnosis of these conditions facilitates a directed treatment regimen. A thorough understanding of the natural history of these injuries and treatment out- comes will enable the appropriate management of patients and their expectations. Evidence Acquisitions: The PubMed database was searched in December 2011 for English-language articles pertaining to elbow tendinopathy. Results: Epidemiologic data as well as multiple subjective and objective outcome measures were investigated to elucidate the incidence of medial epicondylitis, lateral epicondylitis, distal biceps and triceps ruptures, and the efficacy of various treatments. Conclusions: Medial and lateral epicondylitis are overuse injuries that respond well to nonoperative management. Their etiology is degenerative and related to repetitive overuse and underlying tendinopathy. Nonsteroidal anti-inflammatory drugs and localized corticosteroid injections yield moderate symptomatic relief in short term but do not demonstrate bene- fit on long-term follow-up. Platelet-rich plasma injections may be advantageous in cases of chronic lateral epicondylitis. If 6 to 12 months of nonoperative treatment fails, then surgical intervention can be undertaken. Distal biceps and triceps tendon ruptures, in contrast, have an acute traumatic etiology that may be superimposed on underlying tendinopathy. Prompt diag- nosis and treatment improve outcomes. While partial ruptures confirmed with magnetic resonance imaging can be treated nonoperatively with immobilization, complete ruptures should be addressed with primary repair within 3 to 4 weeks of injury. -

Tennis Elbow Advice and Exercises
Tennis Elbow Advice and Exercises Information for patients What is tennis elbow? Tennis elbow is a problem with the tendons around the elbow joint, known collectively as ‘the common extensor tendon’. This tendon is part of the muscles that lift your hand backwards or up in the air. Upper arm bone (humerus) Tendon Muscle Point of elbow (olecranon) on the ulna bone Wrist joint If you have tennis elbow, you will normally feel pain on the outside of your elbow. This area may be tender to touch. It may also be painful down into your forearm. What causes it? Tennis elbow is thought to occur due to repeated small changes to the tendon. This is often caused by overloading the tendon through doing heavy or repetitive manual work or activities. People most often describe problems with gripping, writing and twisting movements of the forearm, as well as lifting, especially with the palm facing down. Tennis elbow was previously thought to be an inflammatory condition, but recent evidence has shown that this is not the case. page 2 Why does it develop? Tennis elbow can occur at any age, although it most commonly occurs in people aged between 35 and 55. Up to four in ten people may experience it at some point in their life. The majority of people who develop tennis elbow are not actually tennis players. It occurs more often in people who repeatedly use their hand for gripping activities, either at work or through sport. However, sometimes there may not be an obvious cause. Timeline After 1 year eight out of ten people with tennis elbow will have improvement or symptoms that have got better, whether they have treatment or not. -

Johns Hopkins Radiology Anatomy Lecture Spine and Limbs
Johns Hopkins Radiology Anatomy Lecture Spine and Limbs Swa Deshmukh [email protected] 9/22/2001 Upper Extremity Queson: What is the most commonly torn muscle of the rotator cuff? Answer: Supraspinatus hPp://www.handsport.us/ images/sholanat-antview.jpg 1 3 Shoulder 2 4 6 5 1 Acromioclavicular joint 7 2 Clavicle 3 Acromion 4 Coracoid process 5 Spine of the scapula 6 Humeral head 7 Scapula Ref: Moeller 3 2 6 Upper Arm 1 7 (the line) 4 1 Clavicle 5 8 2 Scapula 3 Acromion 4 Greater tubercle of the humerus (supraspinatus, infraspinatus, teres 9 minor) 5 Lesser tubercle of the humerus (subscapularis) 6 Humeral head 7 Bicipital groove (long tendon of biceps) 8 Humerus 9 Deltoid tuberosity (deltoid muscle -> axillary nerve) 10 Lateral epicondyle 12 11 Olecranon/olecranon fossa 10 11 12 Medial epicondyle Ref: Moeller Ref: Mosher Elbow 1 Humerus 2 Coronoid fossa 7 1 (receives coronoid process during flexion of ulna) 3 Coronoid 2 3 5 6 4 Radial head 5 Radial tuberosity 8 4 (biceps tendon) 6 Olecranon fossa 9 7 Medial epicondyle 10 8 Lateral epicondyle 9 Olecranon (into fossa on extension) 10 Ulna Ref: Moeller Epicondylis Medial epicondylis = Lateral epicondylis = common flexor tendon common extensor tendon 4 Forearm 8 1 Radius 1 2 Ulna 3 Radial tuberosity (biceps tendon) 4 Scaphoid 2 5 Trochlea of the humerus (ar<culates with ulna) 1 2 6 Olecranon 7 Olecranon fossa (triangular 3 depression, posterior humerus) 9 6 8 Ulnar styloid 7 9 Capitellum (rounded end of 5 humerus, ar<culates with 6 radius) 7 Ref: Moeller 19 yo Male who was shot in led arm during Labor Day weekend. -

The Region of the Forearm
Thomas Jefferson University Jefferson Digital Commons Regional anatomy McClellan, George 1896 Vol. 1 Jefferson Medical Books and Notebooks November 2009 The Region of the Forearm Follow this and additional works at: https://jdc.jefferson.edu/regional_anatomy Part of the History of Science, Technology, and Medicine Commons Let us know how access to this document benefits ouy Recommended Citation "The Region of the Forearm" (2009). Regional anatomy McClellan, George 1896 Vol. 1. Paper 18. https://jdc.jefferson.edu/regional_anatomy/18 This Article is brought to you for free and open access by the Jefferson Digital Commons. The Jefferson Digital Commons is a service of Thomas Jefferson University's Center for Teaching and Learning (CTL). The Commons is a showcase for Jefferson books and journals, peer-reviewed scholarly publications, unique historical collections from the University archives, and teaching tools. The Jefferson Digital Commons allows researchers and interested readers anywhere in the world to learn about and keep up to date with Jefferson scholarship. This article has been accepted for inclusion in Regional anatomy McClellan, George 1896 Vol. 1 by an authorized administrator of the Jefferson Digital Commons. For more information, please contact: [email protected]. 372 THE REGION OF THE FOREARilI. nerve, owing to its close relation to the internal epicondyle and the difficulty of detaching th e soft structures from that bony prominence. It is very important to preserve the periosteum over the olecranon and the strong fascia over the anconeus muscle, so that the triceps may not be altogether severed from the ulna. The relations of the parts exposed in the procedure by a posterior vertical incision (on the left side) are as follows (Plate 52, Fig. -

Tendinopathies Around the Elbow
14 Tendinopathies Around the Elbow Alan J. Johnstone and Nicola Maffulli Introduction affect males and females equally, and most commonly involve the dominant arm [2]. In most patients, overuse During the last 20 years, there has been a better under- of the limb gives rise to the symptoms with the severity standing of the underlying pathology of upper limb being influenced by the overall intensity and duration of tendinopathies. This knowledge, coupled with a better the activity. Characteristically, individuals, including understanding of the exact location of the pathology, competitive athletes, who place high demands on the has enabled surgeons to rationalize the use of existing upper extremities, are prone to developing epicondy- nonsurgical and surgical management options, and to lopathy,although any task which involves repetitive activ- consider future therapeutic options. Not only has this ities may induce these conditions. Sports commonly approach improved the overall success of management, associated with these conditions include racket sports,and but it has also reduced patient morbidity. Research has sports which involve a throwing action resulting in eccen- also clarified the pathology and clinical presentation of tric loading of the muscles of the forearm. Other less a variety of disorders involving neighboring structures common causes of epicondylopathy include a direct blow that can “mimic” symptoms commonly attributed to to the medial or lateral epicondyle. The symptoms may tendinopathies. These findings should reduce diagnostic also ensue following a sudden extreme effort or activity error and help to identify causes of refractory symptoms. resulting in injury. There also appears to be a group of However, despite the advances made, the management of patients susceptible to generalized tendinopathy: Nirschl a significant proportion of patients with tendinopathies referred to this group of patients as having a “mesenchy- around the elbow remains a clinical challenge. -

The Anatomy of the Forearm Extensor Muscles and the Fascia in The
ogy: iol Cu ys r h re P n t & R y e s Anatomy & Physiology: Current m e o a t Dones III et al., Anatom Physiol 2013, 3:1 r a c n h DOI: 10.4172/2161-0940.1000117 A Research ISSN: 2161-0940 Research Article Open Access The Anatomy of the Forearm Extensor Muscles and the Fascia in the Lateral Aspect of the Elbow Joint Complex Valentin C Dones III1*, Steven Milanese2, David Worth3 and Karen Grimmer-Somers4 1International Centre for Allied Health Evidence, University of South Australia, Adelaide, South Australia 2School of Health Sciences, University of South Australia, Adelaide, South Australia 3Manager Professional at ROSH, Adelaide, South Australia 4International Centre for Allied Health Evidence, University of South Australia, Adelaide, South Australia Abstract Aim: This study aimed to address the lack of detailed information on the fascia, and the potentially diverse attachments of the Extensor Carpi Radialis Brevis and Extensor Digitroum Communis on the lateral epicondyle. Methodology: Twenty cadavers were dissected by layers consisting of the skin, subcutaneous fat, superficial fascia, deep fascia, and muscles. Results/Conclusion: The separable attachment of the Extensor Capri Radialis Brevis and Extensor Digitorum Communis on the lateral epicondyle is best described as the Common Extensor Origin. This Common Extensor Origin is formed by the Extensor Digitorum Communis at its superficial portion (approximately 65-75% of the Common Extensor Origin thickness) and by the Extensor Carpi Radialis Brevis at its deepest quarter (approximately 25-35% of the Common Extensor Origin thickness). Distal to the radiocapitellar joint, the proximal bellies of the Extensor Carpi Radialis Brevis and Extensor Digitorum Communis appear tightly attached to the deep fascia. -

Management of Extensor Tendon Injuries M
36 The Open Orthopaedics Journal, 2012, 6, (Suppl 1: M4) 36-42 Open Access Management of Extensor Tendon Injuries M. Griffin1, S. Hindocha*,2,3, D. Jordan3, M. Saleh4 and W. Khan5 1Academic Foundation Trainee, Kingston Upon Thames, London, UK 2Department of Plastic Surgery, Whiston Hospital, Warrington Road, L355DR, UK 3Department of Plastic Surgery, Countess of Chester Hospital, Liverpool Road, Chester, CH21UL, UK 4Ain Shams University, Khalifa El-Maamon St, Abbasiya Sq, Cairo 11566, Egypt 5University College London Institute of Orthopaedics and Musculoskeletal Sciences, Royal National Orthopaedic Hospital, Stanmore, Middlesex, HA74LP, UK Abstract: Extensor tendon injuries are very common injuries, which inappropriately treated can cause severe lasting impairment for the patient. Assessment and management of flexor tendon injuries has been widely reviewed, unlike extensor injuries. It is clear from the literature that extensor tendon repair should be undertaken immediately but the exact approach depends on the extensor zone. Zone I injuries otherwise known as mallet injuries are often closed and treated with immobilisaton and conservative management where possible. Zone II injuries are again conservatively managed with splinting. Closed Zone III or ‘boutonniere’ injuries are managed conservatively unless there is evidence of displaced avulsion fractures at the base of the middle phalanx, axial and lateral instability of the PIPJ associated with loss of active or passive extension of the joint or failed non-operative treatment. Open zone III injuries are often treated surgically unless splinting enable the tendons to come together. Zone V injuries, are human bites until proven otherwise requires primary tendon repair after irrigation. Zone VI injuries are close to the thin paratendon and thin subcutaneous tissue which strong core type sutures and then splinting should be placed in extension for 4-6 weeks. -
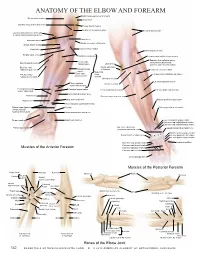
ANATOMY of the ELBOW and FOREARM Medial Cutaneous Nerve of Forearm Biceps Brachii Muscle Ulnar Nerve
ANATOMY OF THE ELBOW AND FOREARM Medial cutaneous nerve of forearm Biceps brachii muscle Ulnar nerve Brachial artery and median nerve Triceps brachii muscle Medial intermuscular septum Triceps brachii muscle Lateral cutaneous nerve of forearm (terminal musculocutaneous nerve) Ulnar artery Brachialis muscle Medial epicondyle of humerus Biceps brachii tendon Radial artery Common flexor tendon Brachioradialis muscle Bicipital aponeurosis Pronator teres muscle Extensor carpi radialis longus muscle Superior ulnar collateral artery Flexor carpi (anastomoses distally with Brachioradialis muscle Ulnar nerve radialis muscle posterior ulnar recurrent artery) Extensor carpi Medial epicondyle radialis longus muscle Palmaris longus of humerus Common extensor tendon muscle Superficial Flexor carpi Extensor carpi flexor Extensor carpi radialis brevis muscle ulnaris muscle radialis brevis muscle muscles Olecranon of ulna Extensor digitorum muscle Flexor digitorum Anconeus muscle superficialis muscle Flexor pollicis longus Palmaris longus tendon Flexor carpi ulnaris muscle Extensor digiti minimi muscle muscle and tendon Dorsal branch of ulnar nerve Radial artery Extensor carpi ulnaris muscle Ulnar artery and nerve Abductor pollicis longus muscle Median nerve Flexor digitorum superficialis tendon Palmar carpal ligament Pisiform Extensor pollicis brevis muscle (continuous with extensor retinaculum) Palmar branch of median nerve Thenar muscles Hypothenar muscles Extensor pollicis longus tendon Extensor carpi radialis brevis tendon Extensor carpi radialis -

Late Surgical Results of Reattachment to Bone in Repair of Chronic Lateral Epicondylitis
An Original Study Late Surgical Results of Reattachment to Bone in Repair of Chronic Lateral Epicondylitis Mark E. Pruzansky, MD, George D. Gantsoudes, MD, and Nathan Watters, BA extensor tendon to bone to more closely approximate nor- Abstract mal anatomy. Strength and proprioception in the forearm All cases of lateral epicondylitis surgically treated in Dr. extensor muscles ought to be maximized through direct Pruzansky’s office practice between October 1986 and reattachment to the lateral epicondyle rather than through December 2005 yielded 24 elbows for this study. Patients adjacent intact musculotendinous units. This concept, were treated with surgical débridement and direct repair which has been in use for more than 20 years, produces to bone through bone tunnels (18 elbows), repair with a predictable return to previous sports and activity level. suture anchors (3 elbows), or augmentation with autolo- gous tendon graft and reattachment to bone via suture This series represents the earliest reattachment cases to anchors (3 elbows). be reported, and with the longest follow-up. One of the This series represents the earliest reattachment cases techniques is an alternative salvage procedure described to be reported, and with the longest follow-up. Mean fol- for use in cases with severe tendon deficiency. low-up (both telephone and office interviews) was 64.7 months. All patients reported satisfaction and graded MATERIALS AND METHODS their outcomes as good or excellent. Mean time to full All cases of lateral epicondylitis surgically treated in Dr. painless preinjury level of use of the elbow was 4.3 Pruzansky’s office practice between October 1986 and months for patients who underwent simple repair and December 2005 yielded 28 elbows in 26 patients. -
Revised 2021 Appendix 1
BMJ Publishing Group Limited (BMJ) disclaims all liability and responsibility arising from any reliance Supplemental material placed on this supplemental material which has been supplied by the author(s) Br J Sports Med Appendix 1 - AMSSM Recommended Sports Ultrasound Scanning Protocols These scanning protocols were developed as educational/instructional tools to assist with familiarization of regional anatomy relevant to the practice of sports medicine. These protocols are not meant to be prescriptive for clinical practice. We recommend each institution develop their own clinical scanning protocols taking into consideration requirements for coding and billing and practice-specific factors. Sports Medicine Fellows should strive to become competent in the scanning techniques and normal anatomy listed below. Recognition and reporting of pathologic findings are addressed in the AMSSM Revised Sports Ultrasound Curriculum for Sports Medicine Fellowships. ACUTE TRAUMA Required 1. Common sites of fracture (should also be reviewed in each of the following musculoskeletal section) a. Rib b. Clavicle c. Distal radius/ulna d. Scaphoid e. Metacarpal f. Fibula g. Metatarsal 2. Common sites of dislocation (should also be reviewed in each MSK section below) a. Glenohumeral joint b. Phalanx 3. eFAST (extended Focused Assessment of Sonography in Trauma) Optional 1. Ocular trauma assessment 2. RUSH (Rapid Ultrasound in Hypotension) 3. Superficial and deep venous thrombosis 4. Pulmonary assessment 5. Limited cardiac assessment for evaluation of pericardial effusion and global systolic function SHOULDER (to include neck, chest, and upper arm as indicated) Required 1. Biceps tendon (long head) and muscle 2. Subscapularis tendon 3. Dynamic assessment of biceps subluxation/dislocation & subcoracoid impingement as indicated Revised 2021 Hall MM, et al. -
Fascial Palpation
Fascial Palpation Thomas Myers Some form of connective tissue matrix is everywhere within the body except the open lumens of the respiratory and digestive tubing, so we cannot palpate anywhere without contacting at least some corner of this unitary body-wide network. (Myers 2008) The same is true of the neural and circulatory syncitia, and epithelia are everywhere as well. With the caveat that no tissue can be truly isolated or separated, this chapter points to some salient and prominent fascial or connective tissue features within this overall net. We will explore these features within the myofasciae of the locomotor system - as opposed to the organic ligaments or meninges within the dorsal and ventral cavities - in terms of the myofasial meridians known nd as the Anatomy Trains (3rd e d. Elsevier, 2014) Before we begin this systematic process, a word about fascial layering: Although the fascial net takes its first form around the end of the second week of embryonic development, as a single three-dimensional cobweb of fine reticular fibers surrounding and investing the entire simple trilaminar embryo, the subsequent origami of embryonic development folds the original fascial net into recognizable layers. (Schultz 1996) ● In the mature phenotype (that would be us), picking up the skin anywhere in the body brings with it the first layer of fascial sheeting, the dermis, a tough but elastic layer that acts as the backing for the carpet of the skin. ● The next layer (although we are at pains to note that each of these layers is incompletely separate from its neighbors as each layer is always connected to the next by variable fuzzy or gluey connections) is known as the areolar or adipose layer.